Beruflich Dokumente
Kultur Dokumente
Lumbar Intraosseous Schwannoma: Case Report and Review of The Literature
Hochgeladen von
petrarizkyOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Lumbar Intraosseous Schwannoma: Case Report and Review of The Literature
Hochgeladen von
petrarizkyCopyright:
Verfügbare Formate
Received: 10.12.2013 / Accepted: 06.01.
2014
DOI: 10.5137/1019-5149.JTN.10054-13.0
Case Report
Lumbar Intraosseous Schwannoma:
Case Report and Review of the Literature
Lomber ntraossez vanom: Olgu Sunumu ve Literatr Derlemesi
Deyong Song1, Zhong Chen2, Dewei Song3, Zaixue LI4
1Foshan
Hospital of Traditional Chinese Medicine, Department of Spinal Surgery, Foshan City, China
Hospital of Southern Medical University, Department of Spinal Surgery, Guangzhou City, China
3Mengyin County Hospital, Department of Minimally Invasive Pain Treatment, Linyi City, China
4Shilong Affiliated Hospital of Southern Medical University, Department of Spinal Surgery, Dongguan City, China
2Zhujiang
Corresponding Author: Deyong Song / E-mail: songdeyongss@126.com
ABSTRACT
Intraosseous schwannomas of the mobile spine are extremely rare. To our knowledge, only 21 cases have been reported in the literature. In this
report, we present a case of schwannoma involving the lumbar spine, with a review of the literature and discussion of this rare tumor. A 44-yearold male presented with a 3-year history of intermittent low back pain, with radiation into the right lower extremity during the last 2 years.
Radiographs revealed an approximately 44 cm irregular mass with marginal sclerosis located at the L5 vertebra, involving the right pedicle
and extruding into the spinal canal. The tumor was resected completely and was confirmed as schwannoma by histological examination. At
follow-up after 12 months, the patient was free of pain and with no recurrence. Despite its low incidence, intraosseous schwannomas should
be considered as the differential diagnosis of an extradural mass involving the vertebrae. Surgery is the preferred treatment method and
usually carries a good prognosis.
Keywords: Intraosseous schwannoma, Lumbar vertebra, Surgery
Z
Hareketli omurgann intraossez vanomlar son derece nadirdir. Bildiimiz kadaryla literatrde sadece 21 olgu bildirilmitir. Bu raporda bir
literatr derlemesi ile birlikte lomber omurgayla ilgili bir vanom olgusu sunuyor ve bu nadir tmr tartyoruz. 44 yanda bir erkek hasta
3 yldr devam eden ve son 2 yldr sa alt ekstremiteye yaylan aralkl bel ars yksyle geldi. Radyografiler L5 vertebrada sa pedikl
tutan ve spinal kanal iine ekstrzyon yapan, marjinal sklerozlu yaklak 4x4 cm irregler kitle gsterdi. Tmr rezeksiyonla tamamen karld
ve histolojik incelemede vanom olduu doruland. 12 aylk takipte hastada ar veya nks yoktu. Dk insidansna ramen intraossez
vanomlar vertebralar tutan ekstradural kitlelerin ayrc tansnda dikkate alnmaldr. Tercih edilen tedavi yntemi cerrahidir ve prognoz
genellikle iyidir.
ANAHTAR SZCKLER: ntraossez vanom, Lomber vertebra, Cerrahi
Introduction
Schwannomas are most frequent extramedullary, intradural
spinal tumors arising from the nerve sheath cells. Intraosseous
schwannomas are rare benign tumors that account for less
than 0.2% of primary bone tumors (9). They most commonly
occur in the mandible and sacrum (13). Vertebral involvement
is extremely rare (4). We report a schwannoma involving
the lumbar spine and present the clinical, radiological and
histological ndings, with a review of the literature and
discussion of this rare tumor.
Case Report
A 44-year-old male presented with a 3-year history of
intermittent low back pain, with radiation into the right
lower extremity during the last 2 years. Over the recent few
weeks his pain increased gradually and felt numbness of the
medial aspect of the right foot. He had no previous trauma
and medical problems. On examination there was local pain
982
elicited by percussion of lumbar spine. The range of lumbar
spinal motion was decreased, especially with regard to the
flexion of the lumbar spine. The straight leg test was limited
to 45 on the right side. Motor strength of lower limbs was
normal, patellar and Achilles tendon reflexes were equal
and symmetrical, but he showed paresthesia on the right L5
sensory dermatome. Computed tomography (CT) showed an
approximately 44 cm irregular mass with marginal sclerosis
located at the L5 vertebra, involving the right pedicle with
posterior protrusion compressing the thecal sac (Figure 1A).
It also revealed pars defects at L5.The mass was hypointense
on T1-weighted images and hyperintensive on T2-weighted
images (Figure 1B, C). Mild irregular enhancement was
revealed on contrast-enhanced T1-weighted images after the
administration of gadolinium (Figure 1D).
The patient was operated via a posterior approach. After
L5 laminectomy, a well-encapsulated mass was found. The
tumor mass was gray-white and avascular with a clear plane of
Turk Neurosurg 2014, Vol: 24, No: 6, 982-986
Song D. et al: Lumbar Intraosseous Schwannoma
cleavage from the surrounding tissues. No nerves in relation
to the tumor could be identied. Biopsy was taken for frozen
sectioning and the diagnosis was confirmed as schwannoma
without any malignant features. The mass extruding into
the spinal canal was separated and excised. The remaining
tumor inside the L5 vertebral body was carefully removed
using curettes. After excising the entire tumor, transpedicular
screws and intervertebral bone fusion were applied to give
spine stability on L4 to S1.
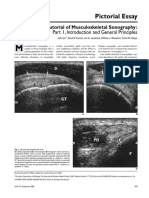
Figure 1: A) Axial CT showing
lytic changes in the L5
vertebra and right pedicle with
intraspinal extension. Isthmic
spondylolysis of L5 can also be
seen. B) MR showing the lesion
is hypointense on T1-weighted,
C) heterointense on T2-weighted
and D) demonstrating mild
irregular enhancement on
postgadolinium T1-weighted
images.
Figure 2: A) Photomicrograph of the tumor specimen reveals hypocellular areas (Antoni A) and hypercellular areas (Antoni B) (H&E,
original magnification 100). B) Immunohistochemical studies for S100 protein is diffusely positive.
Turk Neurosurg 2014, Vol: 24, No: 6, 982-986
983
Song D. et al: Lumbar Intraosseous Schwannoma
The histological examination of the lesion showed Antoni
A and B areas with hypercelular, pallisaded cells alternating
with hypocelular stroma (Figure 2A). Immunohistochemical
testing for S100 protein was diffusely positive, whereas glial
fibrillary acidic protein was negative (Figure 2B).
The postoperative course was uneventful and the patient was
free of preoperative complaints with no neurological decit.
At the latest one-year follow-up, he was asymptomatic. X-rays
showed sound fusion and appearance (Figure 3A, B).
Discussion
Schwannomas are the most frequent extramedullary,
intradural spinal tumors, accounting for up to 25% of all
intradural spinal cord tumors (2, 8). However, intraosseous
schwannomas are rare benign neoplasms that account for
less than 0.2% of primary bone tumors (9). They are most
commonly seen in the third to fourth decade of life, and there
is no gender predilection (6,15).The most frequent sites for
intraosseous schwannomas are in the mandible and sacrum,
other reported sites include ulna, humerus, femur,tibia, ribs,
patella, scapula, maxilla, the small bones of the hands and
vertebral bodies (3-5, 7, 17). The first case of intraosseous
schwannoma was reported by Dickson in 1971 (7). Only 21
cases of intraosseous schwannoma in the mobile spine have
been reported so far. Among these 21 cases, the male-to
female ratio was 13:8. The age of the patients ranged from 10
to 65 years. Nine cases were in the cervical spine, six cases in
the lumbar and six cases in the thoracic spine (TableI).
Three mechanisms have been postulated by which
intraosseous schwannoma arises: (1) extraosseous tumor
causing erosion of the bone, (2) tumor arising centrally within
the bone, (3) tumor arising within the nutrient canal and
growing in a dumbbell conguration (6,11,14). In our case,
like majority of reported cases, the exact origin of the tumor
could not be identified. The surgical findings indicated that
part of the tumor was extraosseous and we speculate that the
third mechanism mentioned above was the probable pattern
of occurrence. Sherman (16) observed nerve fibres existing in
the marrow of the vertebra. However, most of them appeared
to be non-myelinated and myelinated fibres were rare. This
explains why intraosseous schwannomas rare occur in the
vertebral body. Intraosseous schwannomas generally involve
the anterior column of the spine. The tumors chronic pressure
and erosion on the vertebral body and the pedicle can result
in scalloping of the vertebra, pedicle erosion and widening of
the foramen; however, involvement of the posterior column
has also been reported (12).
The radiological findings of intraosseous schwannoma are
non specific. It usually appears as a lytic defect with cortical
A
B
984
Figure 3: A) Anteroposterior and B) lateral
postoperative radiographs showing good bony
fusion.
Turk Neurosurg 2014, Vol: 24, No: 6, 982-986
Song D. et al: Lumbar Intraosseous Schwannoma
Table I: Previously Published Reports of Intraosseous Schwannoma in the Vertebrae (Excluding Sacrum)
No
Year
Series
Age/
Sex
1971
Dickson
51/F
L3
1975
Polkey
34/F
1988
Naidu
50/M
1997
Nooraie
1998
Pathology
Prognosis
complete
benign
2 years no
recurrence
C6,
C7
complete
benign
C3,
C4
complete
benign
46/M
T12
complete
benign
Chang
58/M
L4,
L5
complete
2000
Ramasamy
37/M
T12
complete
2001
Schreuder
38/F
C6
complete
benign
2001
Inoka
9/F
T10
root
T10
complete
benign
2001
Inoka
39/M
L5
operated
benign
10
2005
Nannapaneni
42/M
C5
complete
ancient
schwannoma
11
2005
Gupta
30/F
L2
complete
benign
12
2006
Singrakhia
43/M
C3,
C4
subtotal
benign
13
2006
Singrakhia
45/M
C3
subtotal
benign
14
2007
Choudry
18/M
T12
complete
benign
15
2009
Cetinkal
55/F
T12
complete
benign
16
2009
Park
46/F
L4
complete
ancient
schwannoma
17
2010
Mizutani
44/F
C4
complete
benign
18
2011
Peng
44/M
C3
complete
malignant
transformation
19
2011
Kojima
60/M
T9
complete
benign
20
2012
Youn
65/M
L2
complete
ancient
schwannoma
21
2013
Mohanty
10/M
C4
complete
benign
22
2014
Present Case,
Song
44/M
L5
complete
benign
Turk Neurosurg 2014, Vol: 24, No: 6, 982-986
Origin Level Resection
ancient
schwannoma
Schwannoma
with
proliferation
Symptoms
pain in bilateral lower
limbs
pain and weakness of
limbs
burning paresthesias and
progressive weakness of
limbs
1.5 years no burst fracture caused by
recurrence
trauma
pain and numbness of
lower extremities
back pain, weakness
1.5 years no
and numbness of lower
recurrence
extremities
4 years no neck pain,paraesthesia of
recurrence
right scapula
1 year no
nontender distention of
recurrence
the back
3 years no
lumbar pain
recurrence
1.5 years no
asymptomatic
recurrence
5 months no back, weakness of lower
recurrence
limbs
1 year no numbness and weakness
recurrence
of right shoulder
1 year no
pain and weakness of
recurrence
right upper limb
5 years no back pain, weakness both
recurrence
lower extremities
back pain, pain and
1 year no
numbness of right lower
recurrence
limb
21 months no back pain, weakness in
recurrence
both lower extremities
17 months no
asymptomatic
recurrence
Recurrence at
neck pain
2 years
back pain, weakness and
2 years no
numbness of both lower
recurrence
limbs
back pain, numbness
1 year no
and paresthesias in right
recurrence
lower limb
10 months no
painless mass,
recurrence
dysphagia, stridor
1 year no
back pain, right lower
recurrence
extremity pain
985
Song D. et al: Lumbar Intraosseous Schwannoma
erosion but without periosteal new bone formation, central
calcification or ossification (1,6). These tumors can be easily
mistaken for giant cell tumor, solitary myeloma, aneurysmal
bone cyst, chordoma, osteoblastoma or hemangioma (13,17).
On MR imaging, schwannomas are typically hypointense
relative to the cord on T1-weighted images and hyperintense
on T2-weighted images. They may be heterogeneous on
T2-weighted images with focal areas of hyperintensity and
hypointensity corresponding to cyst formation, hemorrhage,
dense cellularity, or collagen deposition (10). In our case the
postcontrast T1-weighted images were atypical by virtue of
the lack of contrast enhancement. We postulate that this was
due to absent perfusion within the necrotic degeneration of
the tumor.
Surgical excision is the preferred treatment option. Those
tumors are usually well encapsulated without invasion of
the surrounding structures, making complete resection
possible. Complete resection was reported in 19/21 of the
cases. Recurrence is rare following surgical resection. Among
19 reported cases for whom follow-up was available, 18 had
no recurrence ranging from 5 months to 5 years, except one
case recurrence with malignant transformation of a benign
intraosseous schwannoma that was reported 2 years after the
operation (Table I).
It is worth noting that it is important to carry out preoperative
or intraoperative biopsy. This can help surgeons choose
the appropriate treatment option. In our patient, the
histopathological confirmation of benign schwannoma was
obtained by intra-operative frozen section, and the tumor
was therefore removed completely without damage to
the surrounding tissues. Our present patient had both L5
vertebral tumor and isthmic spondylolysis. Surgical treatment
of the isthmic spondylolysis was not necessary at that
time. Considering that spondylolisthesis might occur after
laminectomy and destruction of the vertebral body, internal
fixation and bone graft union were performed from L4 to S1.
Conclusion
Intraosseous schwannomas are rare tumors and should be
considered in the differential diagnosis of an extradural mass
involving the vertebrae. Surgical excision is the preferred
treatment option. Complete resection can be achieved and
recurrence is uncommon.
References
1. Agha FP, Lilienfeld RM: Roentgen features of osseous
neurilemmoma. Radiology 102(2):325326, 1972
2. Ahn DK, Park Hs, Choi DJ, Kim TW, Park SY: The surgical
treatment for spinal intradural extramedullary tumors. Clin
Orthop Surg 1:165-172, 2009
986
3. Barnowsky L, Dala R: Extradural schwannoma manifested
as an expansile vertebral lesion. AJR Am J Roentgenol 159:
13521353, 1992
4. Chang CJ, Huang JS, Wang YC, Huang SH: Intraosseous
schwannoma of the fourth lumbar vertebrae: Case report.
Neurosurgery 43:12191222, 1998
5. Choudry Q, Younis F, Smith RB: Intraosseous schwannoma of
D12 thoracic vertebra: Diagnosis and surgical management
with 5-year follow-up. Eur Spine J 16(3):283286, 2007
6. De la Monte SM, Dorfman HD, Chandra R, Malawer M:
Intraosseous schwannoma: Histologic features, ultrastructure,
and review of the literature. Hum Pathol 15:551558, 1984
7. Dickson JH, Waltz TA, Fechner RE: Intraosseous neurilemmoma
of the third lumbar vertebra. J Bone Joint Surg Am 53:
347355, 1971
8. Engelhard HH, Villano JL, Porter KR, Stewart AK, Barua M,
Barker FG, Newton HB: Clinical presentation, histology, and
treatment in 430 patients with primary tumors of the spinal
cord, spinal meninges, or cauda equina. J Neurosurg Spine
13:67-77, 2010
9. Fawcett KJ, Dahlin DC: Neurilemmoma of bone. Am J Clin
Pathol 47:759766, 1976
10.
Friedman DP, Tar taglino LM, Flanders AE: Intradural
schwannomas of the spine: MR findings with emphasis on
contrast-enhancement characteristics. AJR Am J Roentgenol
158:13471350, 1992
11. Gordon EJ: Solitary intraosseous neurilemmoma of the tibia
review of intraosseous neurilemmoma and neurobroma.
Clin Orthop 117:271282, 1976
12. Kojima M, Seichi A, Yamamuro K, Inoue H, Kimura A, Hoshino
Y: Intraosseous schwannoma originating from the posterior
column of the thoracic spine. Eur Spine J 20 suppl 2:S153
S156, 2011
13.
Mizutani A, Yokota N, Kawaji H, Yamaguchi-Okada M,
Miyagawa T, Namba H: Intraosseous schwannoma of the
cervical vertebral body: A case report and review of the
literature. Br J Neurosurg 24(5):604-606, 2010
14. Samter TG, Dahlin DC: Neurilemmoma of bone. Report of 3
cases with review of the literature. Radiology 75:215222,
1960
15. Sanado L, Ruiz JL, Laidler L, Polo M: Femoral intraosseous
neurilemmoma. Arch Orthop Trauma Surg 110(4):212213,
1991
16. Sherman SH: The nerve of bone. J Bone Joint Surg Am 45:
522528, 1963
17. Singrakhia MD, Parmar H, Maheshwari M, Fehlings M: Cervical
schwannoma presenting as an expansile vertebral body
lesion, report of two cases with a technical note on the
surgical management. Surg Neurol 66:192196, 2006
Turk Neurosurg 2014, Vol: 24, No: 6, 982-986
Das könnte Ihnen auch gefallen
- Chondrosarcoma of The Thoracic Spine A Rare CaseDokument21 SeitenChondrosarcoma of The Thoracic Spine A Rare CaseTHESSNAVARRONoch keine Bewertungen
- Incidental Findings of The Lumbar Spine at MRI During Herniated Intervertebral Disk Disease EvaluationDokument5 SeitenIncidental Findings of The Lumbar Spine at MRI During Herniated Intervertebral Disk Disease EvaluationDyah Gaby KesumaNoch keine Bewertungen
- Angioleiomyoma in Soft Tissue of Extremities: MRI FindingsDokument4 SeitenAngioleiomyoma in Soft Tissue of Extremities: MRI FindingsLuis Javier del PozoNoch keine Bewertungen
- Meningioma in The Lumbar SpineDokument12 SeitenMeningioma in The Lumbar Spinemex487Noch keine Bewertungen
- Primary Extraskeletal Ewing Sarcoma of The Sinonasal Tract - A Rare Case Report and Review of The LiteratureDokument7 SeitenPrimary Extraskeletal Ewing Sarcoma of The Sinonasal Tract - A Rare Case Report and Review of The LiteraturemohammadsayfooNoch keine Bewertungen
- Intradural Primary Chondroblastic Osteosarcoma: Case ReportDokument3 SeitenIntradural Primary Chondroblastic Osteosarcoma: Case ReportSulistyawati WrimunNoch keine Bewertungen
- JournalDokument6 SeitenJournalYessi PerlitasariNoch keine Bewertungen
- Giant Cell Tumor of The Tendon Sheath: A Rare Case in The Left Knee of A 15-Year-Old BoyDokument3 SeitenGiant Cell Tumor of The Tendon Sheath: A Rare Case in The Left Knee of A 15-Year-Old BoyFriadi NataNoch keine Bewertungen
- Askin TumorDokument6 SeitenAskin TumorGaluh Kresna BayuNoch keine Bewertungen
- A Giant Plexiform Schwannoma of The Brachial Plexus: Case ReportDokument6 SeitenA Giant Plexiform Schwannoma of The Brachial Plexus: Case ReportpetrarizkyNoch keine Bewertungen
- BJR 20140771Dokument10 SeitenBJR 20140771DanaAmaranducaiNoch keine Bewertungen
- Content ServerDokument5 SeitenContent ServerEverProfesionallNurseNoch keine Bewertungen
- Spinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SDokument3 SeitenSpinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SRonald QuezadaNoch keine Bewertungen
- Jurnal 5Dokument3 SeitenJurnal 5Centia PicalNoch keine Bewertungen
- 2008 TWPRMLinDokument8 Seiten2008 TWPRMLinVictor_id077Noch keine Bewertungen
- Spinal Tuberculosis: Imaging Features On MRIDokument6 SeitenSpinal Tuberculosis: Imaging Features On MRIEster JuanitaNoch keine Bewertungen
- Ghost Cell TumourDokument5 SeitenGhost Cell TumourrgrthhnNoch keine Bewertungen
- Primary Tumours of The Synovium: A Report of Four Cases of Malignant TumourDokument5 SeitenPrimary Tumours of The Synovium: A Report of Four Cases of Malignant TumourpompompompompomNoch keine Bewertungen
- Chondrosarcoma of The Temporomandibular Joint: A Case Report and Review of The LiteratureDokument9 SeitenChondrosarcoma of The Temporomandibular Joint: A Case Report and Review of The LiteratureCatalina Soler LioiNoch keine Bewertungen
- MRI Findings in Proven Mycobacterium: Case Report Original Article Original ArticleDokument7 SeitenMRI Findings in Proven Mycobacterium: Case Report Original Article Original ArticleWenny EudensiaNoch keine Bewertungen
- Fibrous Dysplasia of The Thoracic Spine: SciencedirectDokument5 SeitenFibrous Dysplasia of The Thoracic Spine: SciencedirectRisang Nur WigunaNoch keine Bewertungen
- Spinal Chordoma: Radiologic Features: in 14 CasesDokument3 SeitenSpinal Chordoma: Radiologic Features: in 14 Casesselvie87Noch keine Bewertungen
- Spinal Cystic SchwannomaDokument3 SeitenSpinal Cystic SchwannomahelenNoch keine Bewertungen
- Surgery of the Cranio-Vertebral JunctionVon EverandSurgery of the Cranio-Vertebral JunctionEnrico TessitoreNoch keine Bewertungen
- Medicine: Brachial Plexus Schwannoma Mimicking Cervical LymphadenopathyDokument4 SeitenMedicine: Brachial Plexus Schwannoma Mimicking Cervical LymphadenopathykalixinNoch keine Bewertungen
- A Case of Synovial Hemangioma of The KneeDokument5 SeitenA Case of Synovial Hemangioma of The KneeAnjana g rNoch keine Bewertungen
- Europeanjournalof Radiologyopen: Longitudinal Stress Fracture of The Femur: A Rare PresentationDokument4 SeitenEuropeanjournalof Radiologyopen: Longitudinal Stress Fracture of The Femur: A Rare PresentationYusfaIndahNoch keine Bewertungen
- Case 8391: A Case Report of Thoracic Outlet Syndrome (TOS)Dokument7 SeitenCase 8391: A Case Report of Thoracic Outlet Syndrome (TOS)Mudassar SattarNoch keine Bewertungen
- An Unusual Cause of "Appendicular Pain" in A Young Girl: Mesenteric Cystic LymphangiomaDokument3 SeitenAn Unusual Cause of "Appendicular Pain" in A Young Girl: Mesenteric Cystic LymphangiomaSherif Abou BakrNoch keine Bewertungen
- Collagenous Fibroma (Desmoplastic Fibroblastoma) : Clinical, Pathological and Imaging FindingsDokument41 SeitenCollagenous Fibroma (Desmoplastic Fibroblastoma) : Clinical, Pathological and Imaging FindingsAnonymous bE4VegCcNoch keine Bewertungen
- Five Cases of Lymphangioma of The Mediastinum in AdultDokument3 SeitenFive Cases of Lymphangioma of The Mediastinum in AdultIman SyahNoch keine Bewertungen
- 143 FullDokument8 Seiten143 FullDokdem AjaNoch keine Bewertungen
- Surgical Management of Cervical Ossified Posterior Longitudinal LigamentDokument13 SeitenSurgical Management of Cervical Ossified Posterior Longitudinal Ligamentinfobusiness2010Noch keine Bewertungen
- Exercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509Dokument4 SeitenExercise-Associated Numbness and Tingling in The Legs: For Editorial Comment See Page 1509herpthederpNoch keine Bewertungen
- Melanocit CaseDokument5 SeitenMelanocit CaseDelfi AnggrainiNoch keine Bewertungen
- Vasc Lesions H & NDokument6 SeitenVasc Lesions H & Nإسلام الجزيريNoch keine Bewertungen
- Suh 2009Dokument4 SeitenSuh 2009al qurtubi al andalusiNoch keine Bewertungen
- Ewing'S Sarcoma: Imaging FeaturesDokument9 SeitenEwing'S Sarcoma: Imaging FeaturesRachelMayaMalauNoch keine Bewertungen
- Surgical Management of Sacral Chordomas - Illustrative Cases and Current Management ParadigmsDokument7 SeitenSurgical Management of Sacral Chordomas - Illustrative Cases and Current Management ParadigmsHugo JBNoch keine Bewertungen
- Medi 97 E11210Dokument6 SeitenMedi 97 E11210فرجني موغNoch keine Bewertungen
- 2002 17 3 181 185 EngDokument5 Seiten2002 17 3 181 185 EngMortezaNoch keine Bewertungen
- tmp8916 TMPDokument3 Seitentmp8916 TMPFrontiersNoch keine Bewertungen
- Cystic Echinococcosis in The ThighDokument10 SeitenCystic Echinococcosis in The ThighShakti pawadiaNoch keine Bewertungen
- Cervical MyelopathyDokument5 SeitenCervical MyelopathyagisagitaNoch keine Bewertungen
- Rodilla Inervación Tran2018 PDFDokument8 SeitenRodilla Inervación Tran2018 PDFLore BarreraNoch keine Bewertungen
- Metanephric Adenoma in An 8-Year-Old Child: Case Report and Review of The LiteratureDokument4 SeitenMetanephric Adenoma in An 8-Year-Old Child: Case Report and Review of The LiteratureNGUYEN QUYNHNoch keine Bewertungen
- TMP BCFFDokument3 SeitenTMP BCFFFrontiersNoch keine Bewertungen
- Telaah 1Dokument3 SeitenTelaah 1anri albarruNoch keine Bewertungen
- PicsDokument8 SeitenPicsShoaib KhanNoch keine Bewertungen
- Bladder Pecoma Dynamic CT and MRI Presentation of 2 Cases With 2yr Follow Up and Review of The LiteratureDokument7 SeitenBladder Pecoma Dynamic CT and MRI Presentation of 2 Cases With 2yr Follow Up and Review of The LiteratureJanetNoch keine Bewertungen
- AsianJNeurosurg102126-4310714 115827 PDFDokument3 SeitenAsianJNeurosurg102126-4310714 115827 PDFSucipto HartonoNoch keine Bewertungen
- Idiopathic Cervical Spinal Subdural Haematoma: A Case Report and Literature ReviewDokument10 SeitenIdiopathic Cervical Spinal Subdural Haematoma: A Case Report and Literature ReviewSelfa YunitaNoch keine Bewertungen
- Minimally Invasive Approach For Extraforaminal Synovial Cyst L5-S1Dokument7 SeitenMinimally Invasive Approach For Extraforaminal Synovial Cyst L5-S1Tatiana RoaNoch keine Bewertungen
- An Illustrated Tutorial of Musculoskeletal Sonography Part 1, Introduction - and - General - PrinciplesDokument9 SeitenAn Illustrated Tutorial of Musculoskeletal Sonography Part 1, Introduction - and - General - PrinciplesNovitaNoch keine Bewertungen
- 17 OmerhodzicDokument9 Seiten17 OmerhodzicFederico MinghinelliNoch keine Bewertungen
- An Investigation of The Relationship Between Thoracic Outlet Syndrome and The Dimensions of The First Rib and ClavicleDokument7 SeitenAn Investigation of The Relationship Between Thoracic Outlet Syndrome and The Dimensions of The First Rib and ClavicleFrancisco Javier Flores IzarNoch keine Bewertungen
- Sleeve Fracture of The Adult PatellaDokument3 SeitenSleeve Fracture of The Adult PatellaRadenMasKaerNoch keine Bewertungen
- Endometriosis of The Vastus Lateralis Muscle: CasereportDokument4 SeitenEndometriosis of The Vastus Lateralis Muscle: CasereporttabareeNoch keine Bewertungen
- Translated Laporan Kasus Meningioma Spinal en Plaque IDEM Dengan KalsifikasiDokument7 SeitenTranslated Laporan Kasus Meningioma Spinal en Plaque IDEM Dengan KalsifikasiArif Susilo RahadiNoch keine Bewertungen
- Ewing Sarcoma, Anatomie NR 1Dokument5 SeitenEwing Sarcoma, Anatomie NR 1Ioana PelinNoch keine Bewertungen
- Zika: Protecting Children From Mosquito Bites at CampDokument2 SeitenZika: Protecting Children From Mosquito Bites at CamppetrarizkyNoch keine Bewertungen
- Facial Nerve Schwannoma Arising From The Cerebellopontine AngleDokument3 SeitenFacial Nerve Schwannoma Arising From The Cerebellopontine AnglepetrarizkyNoch keine Bewertungen
- 09 2003 Dec Designing-BalancedDokument8 Seiten09 2003 Dec Designing-BalancedpetrarizkyNoch keine Bewertungen
- Evolution of Haemodynamics and Outcome of Fluid Refractory Septic Shock in ChildrenDokument8 SeitenEvolution of Haemodynamics and Outcome of Fluid Refractory Septic Shock in ChildrenpetrarizkyNoch keine Bewertungen
- 1 s2.0 S0720048X00001479 MainDokument6 Seiten1 s2.0 S0720048X00001479 MainpetrarizkyNoch keine Bewertungen
- Ballard ChartsDokument1 SeiteBallard ChartsSyamsu RizaliNoch keine Bewertungen
- Ijmcmed v2n1p34 enDokument7 SeitenIjmcmed v2n1p34 enpetrarizkyNoch keine Bewertungen
- Journal of Surgery April2014Dokument62 SeitenJournal of Surgery April2014petrarizkyNoch keine Bewertungen
- Familial Occurrence of Unilateral Vestibular Schwannoma: K. K. H. EDokument5 SeitenFamilial Occurrence of Unilateral Vestibular Schwannoma: K. K. H. EpetrarizkyNoch keine Bewertungen
- Critical Review: The Triple Threat of Aspiration PneumoniaDokument7 SeitenCritical Review: The Triple Threat of Aspiration PneumoniapetrarizkyNoch keine Bewertungen
- Ajr 142 5 897Dokument6 SeitenAjr 142 5 897petrarizkyNoch keine Bewertungen
- Simple Apparatus THE Recording Of: A FOR Diagnosis and DiplopiaDokument6 SeitenSimple Apparatus THE Recording Of: A FOR Diagnosis and DiplopiapetrarizkyNoch keine Bewertungen
- Clin. Microbiol. Rev. 2016 Musso 487 524Dokument38 SeitenClin. Microbiol. Rev. 2016 Musso 487 524petrarizkyNoch keine Bewertungen
- Opth 9 1041Dokument7 SeitenOpth 9 1041petrarizkyNoch keine Bewertungen
- Zika Transmission InfographicDokument1 SeiteZika Transmission InfographicpetrarizkyNoch keine Bewertungen
- Journal of Oral and Maxillofacial Surgery, Medicine, and PathologyDokument5 SeitenJournal of Oral and Maxillofacial Surgery, Medicine, and PathologypetrarizkyNoch keine Bewertungen
- All About The SpineDokument3 SeitenAll About The SpineSapoCacoNoch keine Bewertungen
- Sistem RangkaDokument165 SeitenSistem RangkaNadzirah ZukriNoch keine Bewertungen
- Effects On Inadvertent Endplate Fracture Following Lateral Cage Placement On Range of Motion and Indirect Spine Decompression in Lumbar Spine Fusion Constructs: A Cadaveric StudyDokument8 SeitenEffects On Inadvertent Endplate Fracture Following Lateral Cage Placement On Range of Motion and Indirect Spine Decompression in Lumbar Spine Fusion Constructs: A Cadaveric Studysiti hanifahNoch keine Bewertungen
- Conditions Affecting The Back and The Upper ExtremityDokument19 SeitenConditions Affecting The Back and The Upper Extremityjed larsen capulong gavinoNoch keine Bewertungen
- Scoliosis Charper12Dokument122 SeitenScoliosis Charper12Simón Pérez LópezNoch keine Bewertungen
- Make A Model of The Human Body: Science ProjectDokument5 SeitenMake A Model of The Human Body: Science ProjectEris Putra SulaemanNoch keine Bewertungen
- Journal of Sound and Vibration 1997 - v200 83-103Dokument21 SeitenJournal of Sound and Vibration 1997 - v200 83-103Franco VillanuevaNoch keine Bewertungen
- SpineDokument7 SeitenSpineayyappakrishnadasNoch keine Bewertungen
- 6.S, R, U Systems of Female PelvisDokument2 Seiten6.S, R, U Systems of Female Pelvisahmned A DOCTORNoch keine Bewertungen
- LAMA-Protein-Energy Malnutrition in AlpacasDokument7 SeitenLAMA-Protein-Energy Malnutrition in Alpacastaner_soysuren100% (2)
- 210921-303368305 MR Iqbal 56Y 21-Sep-2021 IMG-3014226035 MaleDokument1 Seite210921-303368305 MR Iqbal 56Y 21-Sep-2021 IMG-3014226035 MaleRizwan khanNoch keine Bewertungen
- ANPH-M1-CU4. Skeletal SystemDokument26 SeitenANPH-M1-CU4. Skeletal SystemajdNoch keine Bewertungen
- Hospital Corpsman ManualDokument574 SeitenHospital Corpsman ManualNes Navarro100% (1)
- Anatomy and Biomechanics of SpineDokument69 SeitenAnatomy and Biomechanics of SpinehisslNoch keine Bewertungen
- How To Look A Posture Doug KellerDokument9 SeitenHow To Look A Posture Doug KelleryogatonNoch keine Bewertungen
- The Thorax - An Integrated ApproachDokument141 SeitenThe Thorax - An Integrated ApproachElin TaopanNoch keine Bewertungen
- Collagen Medical Device Lumbar in The Combined Treatment of Lumbar Instability Induced PainDokument6 SeitenCollagen Medical Device Lumbar in The Combined Treatment of Lumbar Instability Induced PainHoang Anh BuiNoch keine Bewertungen
- Natural History of AISDokument42 SeitenNatural History of AISJosh JoshiNoch keine Bewertungen
- EMG Analysis of Latissimus Dorsi Erector Spinae and Middle TrapDokument68 SeitenEMG Analysis of Latissimus Dorsi Erector Spinae and Middle TrapYuNoch keine Bewertungen
- PostureDokument72 SeitenPosture69016100% (1)
- Biomechanics of The Spine (Cervical and Lumbar Only) - Kinematics - 20 Questions-1Dokument3 SeitenBiomechanics of The Spine (Cervical and Lumbar Only) - Kinematics - 20 Questions-1rehab aymanNoch keine Bewertungen
- Hadzic - Ch22 - Neuraxial AnatomyDokument11 SeitenHadzic - Ch22 - Neuraxial AnatomyGulsahNoch keine Bewertungen
- Dr. S.N. Kedia Mri Report of 9.05.18 MayDokument9 SeitenDr. S.N. Kedia Mri Report of 9.05.18 Mayrt.pcr.pdplNoch keine Bewertungen
- Biomechanics of SpineDokument22 SeitenBiomechanics of Spineyuvraj100% (1)
- Small Animal Spinal Disorders (Second Edition)Dokument369 SeitenSmall Animal Spinal Disorders (Second Edition)Aline Constantino100% (3)
- Anatomy and Physiology 1st Edition McKinley Test Bank 1Dokument98 SeitenAnatomy and Physiology 1st Edition McKinley Test Bank 1anne100% (31)
- Bio Mechanics of Spinal ColumnDokument59 SeitenBio Mechanics of Spinal ColumnOnwaree Ing100% (4)
- Mcem Anatomy MCQDokument37 SeitenMcem Anatomy MCQMOHAMMED ANEEZNoch keine Bewertungen
- Usui Reiki Ryoho Level 2 - Okuden - ManualDokument24 SeitenUsui Reiki Ryoho Level 2 - Okuden - Manualkenseido100% (2)
- C Biomechanics and AdvantageDokument18 SeitenC Biomechanics and Advantageno thanksNoch keine Bewertungen