Beruflich Dokumente
Kultur Dokumente
Anterior Decompression Techniques For Thoracic and Lumbar Fractures
Hochgeladen von
metasoniko81Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Anterior Decompression Techniques For Thoracic and Lumbar Fractures
Hochgeladen von
metasoniko81Copyright:
Verfügbare Formate
CHAPTER Davis L.
Reames
D. Kojo Hamilton
133 Toomas Anton
Christopher I. Shaffrey
Anterior Decompression Techniques
for Thoracic and Lumbar Fractures
INTRODUCTION abrasions, swelling, and ecchymoses provides clues about
potential locations and mechanisms and severity of injury. The
The anterior approach for traumatic thoracolumbar fractures presence of deformity or tenderness and the determination of
is used most often for unstable burst fractures when there is coexisting injury are critical in determining if an anterior
severe spinal canal compromise in intact patients or those approach is appropriate. Anterior approaches are most com-
with incomplete neurological deficits or when the surgical monly performed for patients with incomplete neurological
alternative commonly involves a long-segment posterior deficits where posterior-alone approaches are frequently used
fusion. As a general rule, stand-alone anterior approaches with severe injuries with complete neurological deficits. There-
fuse fewer spinal segments with equivalent clinical and radio- fore, a rectal examination should be performed in all cases,
graphic outcomes compared with short-segment posterior with assessment of the bulbocavernosus reflex in patients who
instrumentation and fusion procedures. Although a uniform are suspected to be in spinal shock. The presence of rectal tone
algorithm has not been established, the present literature and sensation in the perineal region may confer functional
describes many relative indications as well as contraindica- neuroanatomical integrity and may change prognosis and thus
tions, which may aid in determining the approach of choice clinical decision making.
for a particular patient. Initial imaging should include anterior/posterior as well as
Approximately 150,000 people sustain spinal column frac- lateral plain films of the entire spine. In almost every case
tures per year, while resultant spinal cord injury occurs in an where surgical intervention is contemplated, computed
estimated 10,000 to 17,000. There is a bimodal age distribution tomography (CT) scan is indicated, which should include sag-
composed of young men and elderly women. Motor vehicle ittal and coronal reconstructed images to better visualize
accidents account for more than 40% of cases of spinal cord osseous abnormalities (Figs. 133.1 and 133.2). Magnetic reso-
injury, and more than half of all spine fractures occur within nance imaging (MRI) is warranted in any patient who has
the thoracolumbar spine. The thoracolumbar spine encom- neurological deficits not explained based on imaging with
passes the transition point from the kyphotic thoracic spine plain film or CT or when the severity of ligamentous injury
supported by the thoracic cage, to the unsupported yet struc- could alter the surgical approach. In these cases, a herniated
turally larger lordotic lumbar spine. The considerable inci- disc, hematoma, or other soft tissue mass may be the cause of
dence of high-velocity trauma such as motor vehicle accidents, injury, potentially only observed with MRI. In addition, if a
together with the susceptibility of the thoracolumbar spine to patients baseline neurological status begins to deteriorate, an
the resultant force vectors, necessitates a comprehensive review MRI may also be indicated.
of the various treatment options when considering these inju- Cobb angle, vertebral body translation percentage, anterior
ries to appropriately select when an anterior surgical treatment vertebral body compression percentage, and percentage canal
of these injuries is appropriate. Severe spinal instability is a rela- occlusion should be determined for each fracture. This allows
tive contraindication for an anterior alone procedure and for sagittal alignment assessment, demonstration of traumatic
appropriate identification of fracture pattern is critical to avoid anterolisthesis, expression of vertebral body compression and
construct failure. total cross-sectional area of the central canal, the sagittal to
transverse canal diameter ratio, and overall canal dimensions,
respectively.
CLINICAL AND RADIOLOGICAL The posterior ligamentous complex (PLC) (interspinous liga-
ASSESSMENT ment, supraspinous ligament, facet capsules, and ligamentum
flavum) is, however, thought to be an important element in deter-
All spinal trauma patients warrant a thorough neurological mining stability in thoracolumbar burst fractures. Some authors
assessment in addition to their full trauma workup. A compre- feel that MRI can help change the surgical approach when the
hensive motor/sensory examination including reflexes, evalua- extent of damage to the anterior and posterior longitudinal liga-
tion for signs of external trauma, including step-offs, lacerations, ments and spinal cord parenchyma are elucidated.3 MRI has been
1439
LWBK836_Ch133_p1439-1448.indd 1439 9/1/11 9:57:12 PM
1440 Section XII Trauma
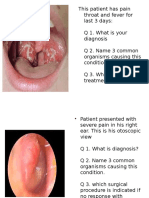
Figure 133.1. Axial computed tomography demonstrating burst Figure 133.2. Sagittal computed tomography demonstrating burst
fracture through L2 with significant canal compromise. fracture through L2 with significant canal compromise and focal
kyphosis.
found to be highly reliable for detecting interspinous and supras-
pinous ligament damage and moderately reliable for posterior
longitudinal ligament damage. The correlation of MRI findings mechanisms of injury, to functionality. In the modern era, the
with neurologic function or severity of fracture has been more concept of the vertebral column as a composite of vertical sup-
difficult, however, and MRI has not been routinely recommended ports has become integral in spinal trauma models. This con-
as necessary for the routine ruling out of occult ligamentous cept, based on anatomical structures, was initially introduced
injury in thoracolumbar burst fractures. Lee et al12 in their Spine by Kelly and Whitesides,9 later to be modified by Denis. Denis5
Trauma Study Group survey analysis for assessing injury to the devised a classification scheme based on a review of radiographs
PLC when plain radiography is normal, found that most respon- of 412 thoracolumbar injuries, CT scans of 53 patients, and
dents preferred a combination of abnormal signal intensity on surgical notes from 120 cases. His goal was to emphasize the
sagittal T1-weighted MRI, diastasis of facet joints on CT, and high pathologic anatomy of different types of spinal injuries, each of
signal intensity on T2/short T1 inversion recovery or fat-saturated which was based on a different mechanism of injury. To accom-
sagittal MRI to be most helpful in determining PLC injury. plish this, Denis introduced the three-column concept of spinal
A common indication for anterior surgical treatment is the stability. This included an anterior (anterior longitudinal liga-
unstable burst fracture. Burst fractures are a heterogenous ment and anterior half of the vertebral body), middle (poste-
group of fractures representing 10% to 20% of all spinal frac- rior longitudinal ligament, posterior annulus fibrosis, and
tures characterized by retropulsion of the middle column into posterior wall of the vertebral body), and posterior column
the vertebral canal with associated loss of anterior vertebral (posterior elements and pedicle). Denis argued that the mode
body height.11 Although stability is not always a straightforward of failure of the middle column correlated to stratified fracture
concept, there are radiographic criteria to assist with diagnosis. types and risk of neurologic injury. Other studies have since
Interspinous widening, increased interlaminar distance, greater reinforced this concept. Ferguson and Allen6 have since modi-
than 2 mm translation, kyphosis measured at greater than 20, fied the Denis classification, and base their classification on
greater than 50% loss of height, dislocations, and fractures of proposed mechanisms of injury.
the articular processes are all demonstrated with burst fractures Compression fractures involve failure of the anterior col-
and taken in clinical context can imply instability. Loss of height umn in compression without injury to the middle column.
of the intervertebral disc proximal to the fracture has been cor- Compression fractures at the thoracolumbar junction typically
related with postoperative dysfunction and pain. The presence are a result of axial loading forces on a flexed spine. As the
of neurological deficits usually is an indicator of spinal instabil- posterior column may remain intact or fail in tension, depend-
ity and when present in burst fractures is the most common ing on the energy level of the injury, the integrity of the poste-
indication for surgical intervention. rior ligamentous structures are the primary determinants of
spinal stability in this fracture pattern. Because of the lack of
spinal canal compromise, and a relatively low risk of progres-
THORACOLUMBAR SPINE sive deformity, anterior decompression is rarely needed for this
FRACTURE CLASSIFICATION fracture type.
Unlike compression fractures, burst fractures result in com-
A variety of classification systems exist for thoracolumbar pression failure of both the anterior and the middle column
trauma, with a basis ranging from anatomical morphology, to following a subaxial loading force. Injury to the middle column
LWBK836_Ch133_p1439-1448.indd 1440 8/26/11 2:34:58 PM
Chapter 133 Anterior Decompression Techniques for Thoracic and Lumbar Fractures 1441
is considered to be a potentially unstable fracture pattern in generated from three major categories, including injury mor-
this classification scheme. Burst fractures most commonly result phology (compression, burst, translational/rotational, and dis-
from high-speed accidents and falls and have a predilection for tractive), neurological status (intact, nerve root, cord/conus
the thoracolumbar junction. Following diagnosis of a burst designated as complete, incomplete, or cauda equina syn-
fracture, a patients spinal stability must be evaluated. In addi- drome), and PLC integrity (intact, injury suspected/indetermi-
tion to the radiological criteria mentioned previously, this com- nate, and injured). The TLISS differs in that it utilizes a mecha-
monly is determined by obtaining upright (dynamic) films with nistic classification scheme rather than fracture morphology.
the patient in a brace. A progressive neurologic deficit, pro- Considering injury morphology, neurological status, and PLC
gressive kyphosis, or radiographic evidence of substantial poste- integrity each impact the decision whether to perform an ante-
rior column injury are indications of instability and may require rior decompression combined with anterior instrumentation
surgical correction. Patients with burst fractures with substan- and fusion or as part of a circumferential procedure, these clas-
tial spinal canal compromise are potential candidates for ante- sifications systems might be an aid in determining the optimal
rior decompression followed by anterior instrumentation and surgical approach.
fusion or posterior instrumentation and fusion. An anterior
approach is almost always indicated in a small subgroup of
patients with a reverse cortical sign. This sign corresponds to TREATMENT ALGORITHM
a fragment of the posterior wall of the vertebral body that has
been flipped 180. The cancellous surface of this fragment Goals of treatment of thoracolumbar burst fractures include
faces posteriorly in the spinal canal and the cortical surface decompression and realignment, stabilization of the fracture,
(posterior wall) facing anteriorly. The identification of such and prevention of further instability, deformity, or neurological
reverse cortical fragment is crucial as ligamentotaxis is classi- injury. Thoracolumbar trauma can be associated with noncon-
cally contraindicated as the posterior longitudinal ligament is tiguous spinal injury in up to 25% of cases and visceral injury
ruptured making posterior-only approaches contraindicated.1 as high as 40% of cases. The surgeon should also bear in mind
A chance fracture and other flexiondistraction injuries the requirements of rehabilitation and strive to maximize the
occur when an anterior force vector acts along the axis of rota- patients recovery by facilitating mobilization and reducing
tion anterior to the spinal column. Consequently, the posterior eventual deformity and pain that can result from inadequate
and middle columns fail in tension, whereas the anterior col- treatment. Morphological considerations include the extent
umn may fail in either tension or compression depending on vertebral body collapse, the severity of kyphosis, and the integ-
the location of the axis of rotation (at or anterior to the ante- rity of the PLC. These are key determinants of spinal stability
rior spinal column). This injury pattern is typically observed and should be considered when deciding between nonopera-
following high-speed motor vehicle accidents in which the lap tive and operative treatments and the surgical approach
belt was used without the shoulder belt (seat belt fracture). selected. Although surgical treatment is generally regarded as
Concomitant abdominal injury as well as spinal epidural hema- standard of care for most two- and three-column injuries, there
toma are common after flexiondistraction injuries fractures has been no definitive support of this management strategy
and should be excluded clinically and radiographically. The with randomized controlled studies (Fig. 133.3).
risk of neurologic injury is higher with this injury type than with Progressive neurological deterioration in the presence of
compression or burst fractures. Anterior-only stabilization of substantial canal compromise is an indication for surgical
these fractures is controversial. Sasso et al18 have reported a decompression and stabilization. The treatment of flexion
large multicenter series of unstable thoracolumbar fracture distraction injuries largely depends on the predominant type of
patients who predominantly had flexiondistraction injuries tissue injury. Pure chance fractures in which disruption occurs
successfully managed with anterior decompression, instrumen- through the bone of the vertebral body, pedicles, laminae, and
tation, and fusion. Other authors have reported higher failure spinous process often will heal reliably if immobilized in a
rates with this approach compared with more traditional hyperextension orthosis, especially in an immature patient. A
posterior-only or circumferential procedures. soft-tissue chance variant, however, with an injury vector pass-
Fracture dislocations are extremely unstable three-column ing through the disc space, facet capsules, and interspinous
injuries that involve translation or rotation through the middle ligament will not heal predictably in the adult and often
column. They commonly involve the thoracolumbar spine and requires operative stabilization. Radiographic evidence of sub-
are often visible on plain radiographs. These injuries are rarely stantial translational or rotational malalignment indicates a
treated with an anterior-only approach. Depending upon neu- highly unstable shear injury or fracturedislocation requiring
rological status and spinal canal compromise, anterior decom- surgical stabilization.
pression and may be required as part of a circumferential pro- The anterior approach can be used to decompress neural
cedure. elements, to restore normal alignment, and to maintain
There have been many attempts at introducing a new system stability.7,8 This technique allows for excellent visualization to
of classification for these fractures. The Spine Trauma Study the ventral spinal anatomy.14 Another advantage is the ability to
Group has developed two systems of classifying thoracolumbar reverse kyphosis by restoring height to the anterior and middle
fractures, called the Thoracolumbar Injury Classification and columns, potentially limiting the number of motion segments
Severity Score (TLICS) and the Thoracolumbar Injury Severity requiring fusion.10 Anterior surgery has demonstrated high
Score (TLISS).19 They recently published a demonstration of rates of neurologic improvement for the treatment of burst
the application of the TLICS through several case studies. The fractures when performed early in patients with incomplete
TLICS system uses fracture morphology rather than mecha- injury.2 However, it is an inherently destabilizing procedure
nism of injury and includes the PLC together with the patients and the resultant vertebral body defect must be replaced with
clinical neurological examination. A numerical grading scale is structural support such as allograft strut, mesh cage, or an
LWBK836_Ch133_p1439-1448.indd 1441 8/26/11 2:34:58 PM
1442 Section XII Trauma
Acute thoracolumbar
fracture
Neurological deficit No neurological deficit
Incomplete injury
Cauda equina
OR Kyphosis >30 Brace
(stabilization and/or Canal compromise >50%
decompression) Upright AP/Lat films
Vertebral loss of height >50%
Neurological deficit Pain control
Anterior instrumentation
Intractable pain
Posterior instrumentation
Non-union of fracture
Combined
Conservative
management
Figure 133.3. Treatment algorithm for the management of thoracolumbar burst fractures.
expandable cage. The anterior approach limits additional dam- decompression is combined with posterior-only short-segment
age to posterior structures such as paraspinal musculature as instrumented fusion.13,16
well as innervation to the area, ligamentous tension bands, and Although the correction of kyphosis and postoperative
bony support. The preservation of these structures may help to maintenance of vertebral body height is a goal of surgery, a
limit the development of posttraumatic kyphosis. clear correlation between postoperative kyphosis from any
Injuries with limited posterior element damage, significant approach and postoperative pain and work status has been
ventral pathology and canal compromise, kyphosis (30), difficult to demonstrate.17
severe anterior comminution, and neurologic impairment have While access as superior as T5 is often attainable, most
been noted as relative indications for the anterior approach.10 authors agree that the anterior approach is most effective from
Using an anterior only approach, Oskouian et al were able T10 to L3.14 As a result of more latitude for compression as a
to spare more lumbar motion segments for selective three- result of a larger canal/nerve root ratio and lack of cord tissue,
column thoracolumbar burst fractures when compared with and difficulty of access due to the location of vascular struc-
traditional posterior approaches.17 Animal models have also tures, the lower lumbar spine (L4 and L5) less often requires an
demonstrated biomechanical advantages and stronger con- anterior approach.
structs when anterior reconstruction is used for anterior and McCullen et al evaluated patients with thoracolumbar injury
middle column injuries. Along these principles, an intact mid- with an incomplete neurological deficit. Fractures that were
dle column (including posterior longitudinal ligament and suboptimally treated by a posterior approach included those
annulus fibrosis) is paramount to deformity correction when with 67% central canal compromise, severe anterior body com-
utilizing a multisegmental posterior instrumented fusion. minution, greater than 30 kyphosis, and those more than
A transpedicular approach has been suggested as an alterna- 4 days from injury. Other patient groups that benefited from
tive approach to provide posterior access to ventral pathology. anterior surgery included those with unsatisfactory results after
However, Lemons et al failed to demonstrate a correlation posterior surgery (residual canal compromise and suboptimal
between neurological recovery and degree of central canal neurologic improvement), flexiondistraction injuries with
reconstruction achieved with this technique, while McLain resultant disc herniation, and planned anterior approaches after
et al, albeit with short follow-up and a limited study, speculated short-segment posterior stabilization are all relative indications
an increase in postoperative kyphosis when transpedicular for anterior surgery.15 Other authors have recommended
LWBK836_Ch133_p1439-1448.indd 1442 8/26/11 2:34:58 PM
Chapter 133 Anterior Decompression Techniques for Thoracic and Lumbar Fractures 1443
additional anterior surgery for residual instability or neural
compression after a posterior approach.10
There is data to support both anterior stabilization and
longer-segment posterior instrumentation and fusion for frac-
tures associated with substantial displacement, kyphosis, and
comminution found in fracturedislocations with at least some
neurological function.10
Contraindications to anterior surgery are severe thoracic or
abdominal concomitant visceral injury. These include concom-
itant cardiorespiratory compromise or reserve, whether acute
or chronic. Patients body habitus and any impairment to
achieving fusion such as osteoporosis or tobacco use would be
expected to compromise either approach.
The ideal management of patients with thoracolumbar spi-
nal injuries is controversial. The wide range spectrum of thora-
columbar injury, associated injuries, and neurological status
complicate the ability to provide absolute recommendations.
Even in cases of well-defined injury such as thoracolumbar
burst fractures, the lack of randomized controlled studies has
precluded a generalized consensus on the optimal manage-
ment of pathology in this region. Treatment of trauma in the
thoracolumbar spine should be individualized to each patient
and is based on evaluation of the patients neurologic condi-
tion, radiographic abnormalities, concomitant injuries, and
general medical condition.
SURGICAL OPTIONS AND TECHNIQUE Figure 133.4. Postoperative lateral plain radiograph after left-
sided retroperitoneal approach for L2 vertebrectomy and L1-3 instru-
mented fusion using screwrod construct.
TIMING TO SURGERY
Most investigators have recommended surgery for patients with
progressive neurological loss or a major neurological deficit in
the setting of substantial canal compromise. In these situations,
the goals of surgery are to provide adequate anatomic decom-
pression of the neural elements and rigid stabilization of the
injured segments until biological fusion occurs. The appropri-
ate timing of surgery following spinal cord injury is the subject
of considerable controversy with conflicting information from
animal and clinical studies. Although animal models have sug-
gested that early decompression may improve neurological
recovery, the window of opportunity appears to be very small,
and the limited class one evidence on spinal trauma has dem-
onstrated no substantial difference in outcome between early
and late surgical decompression and stabilization. Various stud-
ies have reported shorter hospitalizations, less time required in
an intensive care unit (ICU), less systemic complications, and
even improved neurologic improvement when early surgical
repair is compared with late surgery (Figs. 133.4 to 133.6).
SURGICAL APPROACH
Anterior and posterior as well as combined anteroposterior
(AP) surgical approaches each have specific advantages and
disadvantages. Familiarity with approach, predictability of
achieving anatomical alignment, spinal stability, and an accept-
able morbidity are often the reasons surgeons prefer the poste-
rior approach. More consistent anterior decompression,
improved postoperative neurological improvement, and fewer
spinal segments fused with comparable morbidity are often the Figure 133.5. Postoperative anteroposterior plain radiograph
explanation for anterior surgery.4 Danisa et al found that pos- after left-sided retroperitoneal approach for L2 vertebrectomy and
terior surgery to be done faster, with less intraoperative blood L1-3 instrumented fusion using screwrod construct.
LWBK836_Ch133_p1439-1448.indd 1443 8/26/11 2:34:58 PM
1444 Section XII Trauma
Although anterior surgery is an effective technique for releas-
ing fixed deformity prior to stabilization, anterior-only recon-
struction also appears to be an adequate treatment of most
burst fractures limited to the anterior and middle columns
(i.e., without severe injury to the posterior column). A posteri-
or-only fusion with instrumentation from two or three levels
cephalad to the injury to two levels caudal to it is an acceptable
alternative in patients who do not require decompression, but
it involves fusing a more extensive portion of the spine. A so-
called posterior short-segment fusion with instrumentation and
utilization of pedicle screw fixation from one level cephalad to
the injury to one level caudal to has generally fallen out of favor
because of a relatively high rate of proximal screw pullout and
loss of correction in the setting of substantial anterior column
compromise. In the presence of considerable anterior collapse
and posterior column disruption, a combined anterior and
posterior fusion often provides the greatest degree of spinal sta-
bility. Because of the nature of instability, flexiondistraction
injuries and fracturedislocations are best approached initially
with posterior stabilization, followed by an anterior decompres-
sion and reconstruction if needed.
Figure 133.6. Axial diagram of anterior instrumentation using EVOLUTION OF MODERN
screw/plate rigid fixation construct.
ANTERIOR APPROACHES
The Harrington rod distraction system was the first instrumen-
loss, and less cost to the patient when compared with anterior tation with consistent clinical results. This allowed restoration
and combined procedures for unstable burst fractures. of vertebral height, reduction of kyphosis, and indirect decom-
Although they could not recommend combined approaches pression of spinal canal. Drawbacks were incomplete decom-
based on their data, they did state an inability to demonstrate a pression of the spinal canal, semirigid construct, high incidence
significant difference in other factors, such as neurological of pseudarthrosis, and a large number of levels needed to be
function, pain, return to work, or kyphotic correction between fixated. The thoracolateral approach was developed in 1950s
anterior and posterior stand-alone procedures.4 Interestingly, for the treatment of scoliosis and tuberculous abscesses. This
three of the senior surgeons from this paper subsequently work led to an anterior single-stage procedure to avoid the
published a second paper describing a significant improvement morbidity of two stages.
over the posterior-alone approach when they modified their There is no universal consensus as to when to operate on
anterior technique by using a titanium mesh interbody patients with a thoracolumbar fracture and no neurologic defi-
cage filled with autologous graft harvested from the corpec- cit. Most surgeons believe that early fusion will help with mobi-
tomy site.20 lization and pain control and may prevent late posttraumatic
In addition to reconstruction of the vertebral body defect kyphosis. Newer literature recommends evaluation of a struc-
with a strut or cage the use of anterior instrumentation has gain tural pattern of the fracture, the integrity of the PLC, and the
popularity. Rigid fixation devices such as transvertebral screws neurological status of the patient. Fracture pattern can be clas-
with plate or rod constructs have reduced the need for com- sified as compression, translation/rotation, or extension. The
bined approaches. The biomechanics of anterior fixation most common fractures are compression and burst fractures.
devices differ from posterior systems in that they do not rely on In case of incomplete neurological injury anterior approach is
long lever arms to resist flexion forces but rather help to dis- chosen, isolated PLC injury is indication for the posterior
tribute the major area of compressive forces located in the approach. In patients presenting with neurologic deficit, most
anterior vertebral body. Some types of constructs have the dual surgeons believe operative decompression and fusion is indi-
role of distribution of axial loading forces while also providing cated in the first 24 hours. There are several formulated indica-
housing for graft material. The less purchase afforded by the tions for surgery. These include thoracolumbar fractures involv-
soft cancellous bone of the vertebral body compared with the ing the anterior and middle columns with neurological deficit
thickness of the pedicles used in posterior fixation and poor and retropulsion of bone fragments into the canal, thoracolum-
resistance to torsional forces are limitations of the anterior bar fracture without neurologic deficit, but with 50% loss of the
fusion technique, although the supplementation of a combined spinal canal, late burst injuries, including those that occur
approach may overcome these inherent difficulties in very 10 days or more postinjury with or without neurologic deficit,
unstable injuries. Lastly, although there are fusion-sparing painful or progressive posttraumatic kyphotic deformities with
devices available, no such motion-preserving implant has suc- or without neurologic involvement, and nonunion of anterior
cessfully replaced rigid fixation as the construct of choice for and middle column fractures. Advantages of anterior decom-
most spine surgeons. pression and instrumentation are restoration of the sagittal and
Most burst fractures are amenable to reconstruction through coronal alignment, complete decompression of the spinal
an anterior thoracoabdominal, a retroperitoneal, or possibly canal, achieving two-column fixation, and vertebral body recon-
an endoscopic approach, depending on the level of the injury. stitution. Short fusion will prevent early degenerative changes
LWBK836_Ch133_p1439-1448.indd 1444 8/26/11 2:34:58 PM
Chapter 133 Anterior Decompression Techniques for Thoracic and Lumbar Fractures 1445
on adjacent levels, which is particularly important in the lum- postoperatively. This gives a direct view to the spine, segmental
bar spine. Restoring sagittal and coronal balance will result in vessels, and sympathetic chain. The segmental vessels at the
better fusion rates. Biomechanically it has been demonstrated level of the fracture and the levels above and below are tied, a
that best results are achieved with rodplate construct with vascular clip is applied for additional verification of hemostasis
superior construct stiffness, stability in screwbone interface, and they are divided individually. Vessels should be divided at
and improved screw pullout strength. the midpoint of the vertebral body about 1 to 2 cm from the
aorta. For the intrapleural exposure, plural flaps are created
and then closed after completion of the surgery.
SPECIFIC TECHNIQUES
Upper Thoracic Thoracolumbar Approach
T2-5 High dorsolateral thoracotomy (Usually right sided) The patient is placed in the lateral decubitus position and pres-
T6-12 Dorsolateral thoracotomy (Either left or right sided) sure points are padded. Usually a left-sided approach is used if
Thoracolumbar pathology does not dictate otherwise. A beanbag and wide
Transthoracic/retroperitoneal with division of the diaphragm adhesive tape are used for stabilizing the patient. Intraopera-
T12-L2 Retroperitoneal extracavitary tive monitoring is arranged. The length of the incision is dic-
tated by the number of vertebra to be exposed, and ribs are
Lumbar used for guidance. The skin incision is made in the region of
tenth or eleventh rib. If the T11 or T12 vertebrae need to be
L2-5 Retroperitoneal extracavitary exposed, the T10 or T11 rib should be removed, respectively.
Transabdominal For the T12 exposure T11 rib needs to be notched or removed.
Subperiosteal dissection is carried out to expose the rib or ribs.
Lumbosacral The pleura is stripped from the rib, and rib is cut in appropri-
ate length for the exposure. Again a transpleural or retropleu-
L5-Sacrum Ventral retroperitoneal ral approach can be utilized for the exposure of the thoracic
spine. To facilitate exposure of the thoracolumbar junction, a
Upper Thoracic circumferential incision is made in the medial portion of the
diaphragm adjacent to the costal margin to maximize expo-
The patient is placed in a neutral lateral decubitus position. A sure. A more limited exposure can be achieved by detaching
vacuum deflatable beanbag can be used to maintain position. crural attachment of the diaphragm from the bodies of T12
Throughout the procedure direct lateral position needs to be and L1 without incising the periphery of the diaphragm. With
maintained to not lose the orientation of the spinal canal. The this approach, base of the diaphragm is then retracted superi-
patient should be thoroughly taped or strapped to the opera- orly exposing the thoracolumbar junction. Although this more
tive table to permit table rotation during the course of the pro- limited exposure is associated with decreased morbidity, it is
cedure without losing positioning. The approach is usually difficult to decompress or instrument above the T12 level with
from the right side except when fracture fragments are located this approach.
mainly on the left side, patient has had previous right-sided The rostral retroperitoneal space is exposed by dividing the
surgery or when the surgeon needs to deal with the aortic arch abdominal musculature and blunt dissection of the retroperito-
when operating around levels T4-6. The right-sided approach neal contents is then carried out. The spleen, kidneys, and
reduces the difficulty of manipulating the aortic arch during stomach are retracted medially and caudally. A self-retaining
the surgical approach. Pressure points are carefully padded, retractor system is used to maintain the exposure. The aorta is
axillary rolls are used for the axilla, and a pillow is placed mobilized after the selective ligation and division of segmental
beneath the legs to avoid pressure on the peroneal nerve. A vessels. The iliopsoas is stripped from the lateral aspect of the
double-lumen endotracheal tube is used for the anesthesia. vertebral body recognizing that the lumbar plexus is contained
The skin incision should be overlying the intended level of rib in the posterior half of the muscle. Following the anterior spi-
resection. The incision is typically made two ribs above the cor- nal procedure, repair of the diaphragm is performed and a
pectomy level and one level above the upper instrumented chest tube frequently placed.
level. The incision is started at the lateral border of the paraspi-
nal musculature. The latissimus dorsi and serratus anterior
muscles are divided using monopolar cautery, followed by divi-
Retroperitoneal Approach to L2-5
sion of trapezius and rhomboid muscles for a higher exposure. The patient is placed in the lateral decubitus position and pres-
The scapula is retracted and a plane is developed above the sure points are padded. If possible, the patient should be placed
chest wall. The operative level is confirmed with intraoperative left side up to avoid liver manipulation and retraction of vena
C-arm. The periosteum is elevated using periosteal elevator. A cava. The table is flexed to open up the dissection plane
Doyen periosteal dissector is used to remove the periosteum on between ribs and the iliac crest, this also helps the viscera to fall
the underside of the rib. The rib is cut approximately 5 to 7 cm away. The incision is dictated by necessary level. An oblique
from the rib head. Resected rib can be used later for an inter- flank incision between the lower costal margin and the iliac
body fusion. An extrapleural or intrapleural exposure may be crest is performed. The AP distance of the incision is deter-
performed. For the extrapleural exposure the pleura is dis- mined by the number of the vertebra to be exposed and the
sected off from the ribs and vertebrae to be exposed. The body habitus. The latissimus dorsi, external oblique, internal
authors prefer this approach for younger trauma patients, and oblique, and transverses muscles are incised sequentially. The
it eliminates or reduces the duration of needing a chest tube transversalis fascia is opened and retroperitoneal space is
LWBK836_Ch133_p1439-1448.indd 1445 8/26/11 2:34:58 PM
1446 Section XII Trauma
entered. The peritoneum is bluntly dissected from the abdom- The dissection can be carried out dorsolaterally to decompress
inal walls. Sharp dissection for the adhesions should be used. the nerve root. It is important to remove cartilaginous end
Dissection is carried out behind kidney in the potential place plates from the adjacent vertebral bodies to enhance the fusion
between the renal fascia and quadratus lumborum and psoas rates. The curettes, drill, or osteotome can be used for this pur-
muscles. The retroperitoneal fat and ureter are retracted medi- pose. Interbody fusion is performed using structural autograft
ally. Usually on the surface of psoas genitofemoral nerve is iliac crest, structural allograft, titanium mesh, carbon fiber
noted. A self-retaining retractor is inserted, and abdominal cages, or polyethylethylketone (PEEK) or titanium expandable
blades are used to retract the kidney and abdominal contest. cages. Copious amounts of bone graft are generally required.
The segmental vessels are ligated, and aorta is mobilized. The Bone from the surgical approach (rib) can be mixed with local
sympathetic trunk should be preserved. Appropriate level is bone graft obtained during the course of the anterior decom-
determined radiographically and anterior decompression is pression. Occasionally the size of the defect will require addi-
performed. tional grafting material. Iliac crest bone graft, allograft, and a
variety of osteobiological agents have all been reported to have
been used successfully in these circumstances. A template is
Transperitoneal Approach to L3-S1
used to measure the appropriate length for the structural graft
Exposure of L3-S1 is accomplished through an anterior retro- or cage. A variety of instrumentation systems have been devel-
peritoneal or transperitoneal route. The patient is placed oped for the instrumentation, most maintain similar principles
supine in the Trendelenburg position to move abdominal con- of restoring sagittal balance and achieving biomechanically
tent upwards. Pfannenstiel transverse subumbilical or more solid and lasting fusion. Works by Wenger, Dunn, Zielke, and
commonly a paramedian vertical incision is used. The abdomi- Kaneda have contributed success to stand-alone anterior instru-
nal wall is opened next to the midline at the border of the left mentation and fusion. Most major spinal instrumentation com-
rectus abdominis muscle. At this point, a retroperitoneal or panies have a system designed for treatment of these injuries.
transperitoneal route can be chosen. Transperitoneally perito- Most use two transvertebral bicortical screws placed in the ver-
neum is freed from the abdominal wall and opened in a linear tebra above and below the injured segment. These screws are
fashion. The greater omentum, small bowel, and mesentery are attached to either a plate or rods to maintain stability. Regard-
retracted rostrally. The mesocolon is retracted laterally and sig- less of the system used, the lateral aspects of vertebral bodies
moid caudally. The dorsal peritoneum is opened along the left need to be prepared such that the implant rests flush against
common iliac artery from the bifurcation of the aorta to the the bodies. The plate should sit approximately 5 mm from the
bifurcation of the common iliac arteries. The hypogastric end plates to reduce adjacent-segment degeneration. For bolt
plexus and ureter should be preserved. L3 and L4 can also be insertion an awl is used first to penetrate the outer cortex, fol-
exposed with mobilization of the great vessels. For the retro- lowed by the tap, before screws are inserted using the 0 angle
peritoneal approach, the anterior rectus fascia is opened and for the anterior screw and 10 trajectory away from the spinal
the rectus abdominis muscle is mobilized laterally. The poste- canal for the posterior screw. Monoaxial screws are typically
rior rectus fascia is opened above the arcuate line and the ret- employed but polyaxial screws are available. Instrumentation
roperitoneal space entered. The ureter is retracted with the where rostral and caudal staples are designed for 10 conver-
retroperitoneal contents. Ligation of the segmental vessels gence is also available. If reduction is required prior to inser-
enables vascular mobilization. Repair of the posterior and tion of graft, a parallel distractor can be used, which screws in
anterior rectus fascia is performed at the conclusion of the place. If double rod system is used, a posterior rod is inserted
procedure. first. A French rod bender or in situ benders are available if
contouring of the rod is necessary. Final compression utilizing
a compressor and insertion of cross-link to improve torsional
Instrumentation
rigidity is performed. Prior to closure, lateral and AP radio-
After exposure is achieved, the intervertebral discs above and graphs are taken to verify placement of hardware and correc-
below the fractured vertebra are identified and aggressive dis- tion of the deformity. The wound is closed in standard fashion
cectomy is performed. Identification of the neural foramina utilizing chest tube if necessary. If feasible, closure of the pari-
and ipsilateral pedicle will help for the orientation and position etal pleura over hardware is advisable.
of the spinal canal. A corpectomy is performed using the high-
speed drill, curettes, and rongeurs. The anterior longitudinal
Newer Techniques
ligament is left intact to protect the aorta and inferior vena
cava. The vertebra is resected to the opposite pedicle and the Conventional surgical approaches for the thoracolumbar
canal is completely decompressed. The posterior longitudinal trauma are associated with muscle atrophy, scarring, intercostal
ligament must be identified and removed. Diligence is required neuralgia, postthoracotomy syndromes, hemiparesis of the dia-
when removing bone fragments from the spinal canal to pre- phragm, significant blood loss, and pain. Considering all these
vent neurological injury. This may be performed using a curette clinical effects, more minimally invasive techniques have been
and a no 4 Penfield. There are bone fragments frequently developed over the last 10 years. The rational for this is to
retained behind the ipsilateral pedicle and removing the pedi- reduce all the aforementioned complications. In the 1980s
cle will improve the decompression. Reduction is performed video-assisted thoracoscopic surgery (VATS) was developed by
when necessary using manual pressure over the dorsal spine at cardiothoracic surgeons. VATS technique is successfully utilized
the apex of the kyphosis. This can be assisted using laminal by spinal surgeons who report large clinical series.
spreader between end plates or distraction applied through Minimally invasive techniques were first used for the tho-
transvertebral spinal instrumentation. Reduction can be main- racic discectomies, thoracic sympathectomies, and paraspinal
tained using a distractor attached to the transvertebral screws. nerve sheath tumor resections, among other indications. These
LWBK836_Ch133_p1439-1448.indd 1446 8/26/11 2:34:58 PM
Chapter 133 Anterior Decompression Techniques for Thoracic and Lumbar Fractures 1447
techniques were eventually developed to include corpectomies Postoperatively aggressive pulmonary toilet is required to avoid
for trauma. The patients were positioned in standard lateral atelectasis and pneumonia. Drains should be inserted to avoid
position. Working channels were inserted, and decompression postoperative hematoma. Deep venous thrombosis should be
and fusion were performed endoscopically. Fixed landmarks administered immediately postoperatively, and it should be
and screws were routinely placed prior to decompression. A supplemented with thigh high stockings and intermittent com-
steep learning curve is associated with the VATS technique; pressive boots. Early mobilization is a key to avoid prolonged
however, advantages include the significantly minimized injury postoperative ileus. It is strongly recommended using intraop-
to the chest wall, decreased blood loss, improvement in the erative electromyogram (EMG) and somatosensory evoked
postoperative pain, and shorter recovery. potential (SSEP) monitoring to detect any changes in neuro-
Mini approaches have also been described, which avoid vio- logical function. Should any change occur, immediate evalua-
lation of pleural and peritoneal cavities, eliminating the need tion of placed hardware and reduction construct is required.
for a chest tube and avoiding extensive dissection. This Decompression should be started after location of spinal canal
approach is used for accessing thoracolumbar junction using and cord is identified. A careful staged approach to complete
5-cm incision and creating access to the spine through splitting decompression reduces the risk of injury. Decompression needs
the abdominal muscles and retracting diaphragm and to be complete with exposure of the contralateral pedicle. All
peritoneum. the defects to vascular structures, diaphragm, ureter, abdomi-
nal wall, and thoracic duct should be repaired immediately.
Incidental durotomies should be repaired primarily with a non-
ADVANTAGES AND LIMITATIONS OF
absorbable suture. In poorly visualized defects, DuraSeal com-
MINIMALLY INVASIVE TECHNIQUES
bined with Duragen should be used. Intraoperative C-arm
should be used to verify proper placement of instrumentation.
Advantages Limitations In insertion of graft or cage direct visualization confirmed with
Better cosmesis Steep learning curve C-arm should be utilized to avoid violation of spinal canal.
Decrease of intercostal Need for specialized equipment Proper graft placement with appropriate end plate preparation
neuralgia will help with fusion rates. When inserting vertebral screws
Lesser trauma to chest wall Contraindication on multitrauma proper angle away from a spinal canal should be maintained.
patient We use 10 angle away from spinal canal to assure safety on our
Reduced blood loss Difficulties with the redo surgeries posterior screw. In case of breach of any vascular structures
Decrease in postoperative consultation from a vascular surgeon should be obtained imme-
pain diately. Meticulous approach in attention to the detail will help
Early mobilization
to avoid any of these complications.
COMPLICATIONS RELATED TO OPERATIVE
POSTOPERATIVE MANAGEMENT AND PERIOPERATIVE PERIOD
Patients are taken to ICU postoperatively. AP/lateral radio- Perioperative
graphs are obtained immediately after surgery. If a chest tube
is in place daily chest radiographs should be obtained. Early Peripheral nerve injury caused by improper positioning
mobilization and pulmonary toilet are of paramount impor- Bleeding
tance. We continue postoperative antibiotics until drains or Infection
chest tube is discontinued. Early mobilization is also important Anesthesia complications (related to deflation of the lung,
to prevent postoperative ileus. In addition, prophylactic antac- myocardial infarction [MI], etc.)
ids to prevent stomach ulcers are standard. Blood transfusions Postoperative hemo/pneumothorax
are often necessary in the postoperative period. Patients are Deep venous thrombosis
usually ready for discharge 5 to 8 days postoperatively after Pulmonary embolism
detailed physical therapy evaluation. Unless a patient has sus-
tained a three-column injury, we do not generally brace patients Operative
in a postoperative orthosis. If indicated, orthosis is usually con-
tinued for 8 to 12 weeks in an upright position. Wrong level
New neurologic deficit
Inadequate decompression
Cerebrospinal fluid (CSF) leak
COMPLICATION AVOIDANCE Vascular injury
Injury to a lung, liver, spleen, thoracic duct, sympathetic chain
Complication related to the perioperative period include inap- Improper placement of the hardware
propriate positioning or padding, which is necessary to avoid Failure of the hardware
peripheral nerve injury, which is especially important as these Failure to restore sagittal and coronal balance
surgeries may take up to 6 to 8 hours. Preoperative antibiotics
should be administered 30 minutes before the incision and
then redosed accordingly. Having a good anesthesia team is SUMMARY
required considering unilateral ventilation. Blood loss should
be replaced promptly. Adequate blood pressure optimal to spi- The anterolateral approach to the thoracolumbar spine was
nal cord perfusion should be sustained during the procedure. first developed for the drainage of tuberculosis abscesses.
LWBK836_Ch133_p1439-1448.indd 1447 8/26/11 2:34:58 PM
1448 Section XII Trauma
Through advances in the treatment of scoliosis with improved 4. Danisa OA, Shaffrey CI, Jane JA, Whitehill R, Wang GJ, Szabo TA. Surgical approaches for
the correction of unstable thoracolumbar burst fractures: a retrospective analysis of treat-
understanding in spinal biomechanics and improved instru- ment outcomes. J Neurosurg 1995;83:977983.
mentation techniques, anterior approaches have gained popu- 5. Denis F. Spinal instability as defined by the three-column spine concept in acute spinal
trauma. Clin Orthop Relat Res 1984;6576.
larity for the decompression and stabilization of thoracolumbar
6. Ferguson RL, Allen BL Jr. A mechanistic classification of thoracolumbar spine fractures.
fractures. Clin Orthop Relat Res 1984;7788.
Although a uniform standard for the use of anterior 7. Ghanayem AJ, Zdeblick TA. Anterior instrumentation in the management of thoracolum-
bar burst fractures. Clin Orthop Relat Res 1997;89100.
approach spinal decompression and fusion in thoracolumbar 8. Haas N, Blauth M, Tscherne H. Anterior plating in thoracolumbar spine injuries. Indica-
spinal trauma has not been developed, ideal candidates for this tion, technique, and results. Spine 1991;16:S100S111.
technique are likely those patients suffering from a burst frac- 9. Kelly RP, Whitesides TE Jr. Treatment of lumbodorsal fracture-dislocations. Ann Surg
1968;167:705717.
ture with a limited involvement of the posterior complex and in 10. Kirkpatrick JS. Thoracolumbar fracture management: anterior approach. J Am Acad
whom ventral pathology primarily accounts for the resultant Orthop Surg 2003;11:355363.
11. Korovessis P, Baikousis A, Zacharatos S, Petsinis G, Koureas G, Iliopoulos P. Combined
incomplete neurological deficit. The excellent visualization of
anterior plus posterior stabilization versus posterior short-segment instrumentation and
the ventral dura mater and ability to directly decompress neu- fusion for mid-lumbar (L2-L4) burst fractures [see comment]. Spine 2006;31:859868.
ral elements and reconstruct the anterior and middle columns 12. Lee JY, Vaccaro AR, Schweitzer KM Jr, et al. Assessment of injury to the thoracolumbar
posterior ligamentous complex in the setting of normal-appearing plain radiography.
are a major advantage of this technique. There are a multitude Spine J 2007;7:422427.
of various constructs, materials, techniques, and patient factors 13. Lemons VR, Wagner FC Jr, Montesano PX. Management of thoracolumbar fractures with
to consider in the treatment of complex thoracolumbar spinal accompanying neurological injury. Neurosurgery 1992;30:667671.
14. McAfee PC, Bohlman HH, Yuan HA. Anterior decompression of traumatic thoracolumbar
trauma. More prospective randomized controlled trials are fractures with incomplete neurological deficit using a retroperitoneal approach. J Bone
needed to standardize a reproducible treatment algorithm. Joint Surg Am 1985;67:89104.
15. McCullen G, Vaccaro AR, Garfin SR. Thoracic and lumbar trauma: rationale for selecting
the appropriate fusion technique. Orthop Clin North Am 1998;29:813828.
16. McLain RF, Sparling E, Benson DR. Early failure of short-segment pedicle instrumentation
for thoracolumbar fractures. A preliminary report [see comment]. J Bone Joint Surg Am
REFERENCES 1993;75:162167.
17. Oskouian RJ Jr, Shaffrey CI, Whitehill R, et al. Anterior stabilization of three-column tho-
1. Arlet V, Orndorff DG, Jagannathan J, Dumont A. Reverse and pseudoreverse cortical sign racolumbar spinal trauma. J Neurosurg Spine 2006;5:1825.
in thoracolumbar burst fracture: radiologic description and distinctiona propos of three 18. Sasso RC, Best NM, Reilly TM, McGuire RA Jr. Anterior-only stabilization of three-column
cases. Eur Spine J 2009;18:282287. thoracolumbar injuries. J Spinal Disord Tech 2005;18(Suppl):S7S14.
2. Bradford DS, McBride GG. Surgical management of thoracolumbar spine fractures with 19. Vaccaro AR, Zeiller SC, Hulbert RJ, et al. The Thoracolumbar Injury Severity Score: a
incomplete neurologic deficits. Clin Orthop Relat Res 1987;201216. proposed treatment algorithm. J Spinal Disord Tech 2005;18:209215.
3. Brightman RP, Miller CA, Rea GL, Chakeres DW, Hunt WE. Magnetic resonance imaging 20. Wiggins GC, Rauzzino MJ, Shaffrey CI, et al. A new technique for the surgical management
of trauma to the thoracic and lumbar spine. The importance of the posterior longitudinal of unstable thoracolumbar burst fractures: a modification of the anterior approach and an
ligament. Spine 1992;17:541550. outcome comparison to traditional models. Neurosurg Focus 1999;7(1).
LWBK836_Ch133_p1439-1448.indd 1448 8/26/11 2:34:58 PM
Das könnte Ihnen auch gefallen
- Distal Humerus Fractures: Roongsak Limthongthang, MD, and Jesse B. Jupiter, MDDokument10 SeitenDistal Humerus Fractures: Roongsak Limthongthang, MD, and Jesse B. Jupiter, MDRadu UrcanNoch keine Bewertungen
- Surgery of the Cranio-Vertebral JunctionVon EverandSurgery of the Cranio-Vertebral JunctionEnrico TessitoreNoch keine Bewertungen
- Imaging of Spine Trauma: Neuroradiology Review Series Neuroradiology Review SeriesDokument17 SeitenImaging of Spine Trauma: Neuroradiology Review Series Neuroradiology Review SeriesSalman Alfarisy GaulNoch keine Bewertungen
- MRI of the Spine: A Guide for Orthopedic SurgeonsVon EverandMRI of the Spine: A Guide for Orthopedic SurgeonsNoch keine Bewertungen
- A Clinical Approach To Diagnosing Wrist Pain: Los Angeles, CaliforniaDokument6 SeitenA Clinical Approach To Diagnosing Wrist Pain: Los Angeles, CaliforniaOtnil DNoch keine Bewertungen
- Decision en FX CervicalesDokument7 SeitenDecision en FX CervicalesM Joaquin Robles OrtizNoch keine Bewertungen
- MRI Craniocervical LigamentsDokument9 SeitenMRI Craniocervical Ligamentsintan aryantiNoch keine Bewertungen
- Subaxial Cervical Spine Trauma: Cervical Injuries and Treatment (HJ Kim, Section Editor)Dokument9 SeitenSubaxial Cervical Spine Trauma: Cervical Injuries and Treatment (HJ Kim, Section Editor)renonauvalNoch keine Bewertungen
- Abordagem Lateral ExtracavitáriaDokument9 SeitenAbordagem Lateral ExtracavitáriaMarcelo MudoNoch keine Bewertungen
- Displaced Acetabular FracturesDokument11 SeitenDisplaced Acetabular FracturesJayNoch keine Bewertungen
- Classification of Pelvic Fractures and Its Clinical RelevanceDokument6 SeitenClassification of Pelvic Fractures and Its Clinical RelevanceMohamed AzeemNoch keine Bewertungen
- Stav SoucasnyDokument14 SeitenStav SoucasnyTommysNoch keine Bewertungen
- Giacalone 2015Dokument7 SeitenGiacalone 2015Joseval FilhoNoch keine Bewertungen
- ZJ 4852Dokument10 SeitenZJ 4852Christopher BermeoNoch keine Bewertungen
- The Knee - Breaking The MR ReflexDokument20 SeitenThe Knee - Breaking The MR ReflexManiDeep ReddyNoch keine Bewertungen
- Solla 2020Dokument7 SeitenSolla 2020AURORA BADIALINoch keine Bewertungen
- New Symptomatic Compression Fracture After Percutaneous Vertebroplasty at The Thoracolumbar JunctionDokument4 SeitenNew Symptomatic Compression Fracture After Percutaneous Vertebroplasty at The Thoracolumbar JunctionRamy ElmasryNoch keine Bewertungen
- OTA Highlight Paper Predicting Future Displacement of Nonoperatively Managed Lateral Compression Sacral Fractures - Can It Be DoneDokument6 SeitenOTA Highlight Paper Predicting Future Displacement of Nonoperatively Managed Lateral Compression Sacral Fractures - Can It Be Doneakb601Noch keine Bewertungen
- TFCC InjuriesDokument5 SeitenTFCC InjuriesLaineyNoch keine Bewertungen
- Coronal Alignment: After Total Knee ReplacementDokument6 SeitenCoronal Alignment: After Total Knee ReplacementSahithya MNoch keine Bewertungen
- Initial Management of Acute Spinal Cord Injury: Stephen Bonner MRCP FRCA FFICM Caroline Smith FRCADokument8 SeitenInitial Management of Acute Spinal Cord Injury: Stephen Bonner MRCP FRCA FFICM Caroline Smith FRCAMinaz PatelNoch keine Bewertungen
- Temporal Bone TraumaDokument16 SeitenTemporal Bone Traumadafita4661Noch keine Bewertungen
- Rockwood and Green's Fractures in Adultes: Chapter 37 Scapular FracturesDokument23 SeitenRockwood and Green's Fractures in Adultes: Chapter 37 Scapular FracturesPermata GBKP Runggun SurabayaNoch keine Bewertungen
- Transradial Amputation With Pedicled Pronator QuadDokument8 SeitenTransradial Amputation With Pedicled Pronator QuadDeborah SalinasNoch keine Bewertungen
- Tibial Plateau Fractures: A Review: P Fenton and K PorterDokument7 SeitenTibial Plateau Fractures: A Review: P Fenton and K PorterDot DitNoch keine Bewertungen
- Acute Posterior Cruciate Ligament Injuries: Effect of Location, Severity, and Associated Injuries On Surgical ManagementDokument10 SeitenAcute Posterior Cruciate Ligament Injuries: Effect of Location, Severity, and Associated Injuries On Surgical Managementshabrina nurafiatiNoch keine Bewertungen
- Mayne 2016Dokument11 SeitenMayne 2016Ozergio rjksNoch keine Bewertungen
- 2008 - Elbow Dislocation - OCNADokument7 Seiten2008 - Elbow Dislocation - OCNAharpreet singhNoch keine Bewertungen
- J Langford. Pelvic Fractures Part 1, Evaluation, Calssification and Resucitation. 2013Dokument10 SeitenJ Langford. Pelvic Fractures Part 1, Evaluation, Calssification and Resucitation. 2013Bruno HazlebyNoch keine Bewertungen
- Subaxial Cervical Spine Trauma: Evaluation and Surgical Decision-MakingDokument8 SeitenSubaxial Cervical Spine Trauma: Evaluation and Surgical Decision-Makingvicky174Noch keine Bewertungen
- The Use of A Transolecranon Pin in The Treatment of Flexion-Type SCFsDokument6 SeitenThe Use of A Transolecranon Pin in The Treatment of Flexion-Type SCFsBariša KiršnerNoch keine Bewertungen
- Acute Distal Radioulnar Joint InstabilityDokument13 SeitenAcute Distal Radioulnar Joint Instabilityyerson fernando tarazona tolozaNoch keine Bewertungen
- 09.20-09.35 - DR - Dr.heri Suroto - When To OperateDokument80 Seiten09.20-09.35 - DR - Dr.heri Suroto - When To OperateJoseph WilsonNoch keine Bewertungen
- Imaging of Chopart (Midtarsal) Joint Complex: Normal Anatomy and Posttraumatic FindingsDokument10 SeitenImaging of Chopart (Midtarsal) Joint Complex: Normal Anatomy and Posttraumatic FindingsEdgar Bonifacio Chay ChayNoch keine Bewertungen
- European Journal of Radiology: R. Siemund, M. Thurnher, P.C. SundgrenDokument8 SeitenEuropean Journal of Radiology: R. Siemund, M. Thurnher, P.C. SundgrenMasithaNoch keine Bewertungen
- Subaxial Cervical Spine Trauma: Evaluation and Surgical Decision-MakingDokument7 SeitenSubaxial Cervical Spine Trauma: Evaluation and Surgical Decision-Makingvicky174Noch keine Bewertungen
- Fractura Muñeca RevisionDokument13 SeitenFractura Muñeca RevisionwilhelmNoch keine Bewertungen
- Cervical Spine InjuryDokument18 SeitenCervical Spine InjuryGabriel KlemensNoch keine Bewertungen
- Ajr 21 25606Dokument11 SeitenAjr 21 25606ecavalcantiNoch keine Bewertungen
- Fractura de MuñecaDokument13 SeitenFractura de MuñecawilhelmNoch keine Bewertungen
- Surgical Removal of Spinal Tumors: Article by James Willey, Cst/Cfa, and Mark V. Iarkins, M DDokument8 SeitenSurgical Removal of Spinal Tumors: Article by James Willey, Cst/Cfa, and Mark V. Iarkins, M DLuwiNoch keine Bewertungen
- Daftar 23Dokument4 SeitenDaftar 23pratamayossi41Noch keine Bewertungen
- Carroll 2012Dokument11 SeitenCarroll 2012Yuri Chiclayo CubasNoch keine Bewertungen
- Review Article: Radiographically Occult and Subtle Fractures: A Pictorial ReviewDokument11 SeitenReview Article: Radiographically Occult and Subtle Fractures: A Pictorial ReviewPutri Wahyuni AllfazmyNoch keine Bewertungen
- Exogenous Spinal Trauma-Surgical Therapy and AftercareDokument8 SeitenExogenous Spinal Trauma-Surgical Therapy and Aftercaretaner_soysurenNoch keine Bewertungen
- Dai 2001Dokument5 SeitenDai 2001Sri MahadhanaNoch keine Bewertungen
- Laminar Fractures As A Severity Marker in Burst Fractures of The Thoracolumbar SpineDokument4 SeitenLaminar Fractures As A Severity Marker in Burst Fractures of The Thoracolumbar Spinenovera wardaliaNoch keine Bewertungen
- Artigo Image Dogs DOIDokument4 SeitenArtigo Image Dogs DOIrebsbvetNoch keine Bewertungen
- Adult Traumatic Brachial Plexus Injury: J.J. RankineDokument8 SeitenAdult Traumatic Brachial Plexus Injury: J.J. RankineSuhartiniNoch keine Bewertungen
- Distal Radius Fractures 2009Dokument10 SeitenDistal Radius Fractures 2009Un SerNoch keine Bewertungen
- Zygomatic Fractures: Classification and Complications: TveterasDokument7 SeitenZygomatic Fractures: Classification and Complications: TveterasBriando Stevano LinelejanNoch keine Bewertungen
- Yar Boro 2016Dokument13 SeitenYar Boro 2016saimanojkosuriNoch keine Bewertungen
- Jsa 0000000000000162Dokument8 SeitenJsa 0000000000000162Mohammed AliNoch keine Bewertungen
- Comminuted Patella FracturesDokument8 SeitenComminuted Patella FracturesKirana lupitaNoch keine Bewertungen
- Intracranial NeoplasiaDokument12 SeitenIntracranial NeoplasiaJamille OliveiraNoch keine Bewertungen
- Fracturas PatologicasDokument20 SeitenFracturas PatologicasSamantha AriasNoch keine Bewertungen
- Fractura Cadera 1Dokument22 SeitenFractura Cadera 1Júlia LedesmaNoch keine Bewertungen
- PJR 85 41637Dokument20 SeitenPJR 85 41637Rakesh JhaNoch keine Bewertungen
- Acromioclavicular Joint Injuries: Diagnosis, Classification and Ligamentoplasty ProceduresDokument8 SeitenAcromioclavicular Joint Injuries: Diagnosis, Classification and Ligamentoplasty ProceduresMiguel Angel Lamas RamirezNoch keine Bewertungen
- LWBK836 Ch146 p1575-1580Dokument6 SeitenLWBK836 Ch146 p1575-1580metasoniko81Noch keine Bewertungen
- LWBK836 Ch154 p1633-1648Dokument16 SeitenLWBK836 Ch154 p1633-1648metasoniko81Noch keine Bewertungen
- LWBK836 Ch147 p1581-1583Dokument3 SeitenLWBK836 Ch147 p1581-1583metasoniko81Noch keine Bewertungen
- Intradural, Extramedullary Spinal Tumors: BackgroundDokument9 SeitenIntradural, Extramedullary Spinal Tumors: Backgroundmetasoniko81Noch keine Bewertungen
- LWBK836 Ch150 p1598-1607Dokument10 SeitenLWBK836 Ch150 p1598-1607metasoniko81Noch keine Bewertungen
- LWBK836 Ch137 p1485-1486Dokument2 SeitenLWBK836 Ch137 p1485-1486metasoniko81Noch keine Bewertungen
- Intramedullary Spinal Cord Tumors: Clinical PresentationDokument15 SeitenIntramedullary Spinal Cord Tumors: Clinical Presentationmetasoniko81Noch keine Bewertungen
- LWBK836 Ch144 p1553-1559Dokument7 SeitenLWBK836 Ch144 p1553-1559metasoniko81Noch keine Bewertungen
- LWBK836 Ch148 p1584-1590Dokument7 SeitenLWBK836 Ch148 p1584-1590metasoniko81Noch keine Bewertungen
- Primary Malignant Tumors of The Spine: Gregory S. Mcloughlin Daniel M. Sciubba Jean-Paul WolinskyDokument12 SeitenPrimary Malignant Tumors of The Spine: Gregory S. Mcloughlin Daniel M. Sciubba Jean-Paul Wolinskymetasoniko81Noch keine Bewertungen
- Spinal Vascular Malformations: Michelle J. Clarke William E. Krauss Mark A. PichelmannDokument9 SeitenSpinal Vascular Malformations: Michelle J. Clarke William E. Krauss Mark A. Pichelmannmetasoniko81Noch keine Bewertungen
- LWBK836 Ch135 p1460-1473Dokument14 SeitenLWBK836 Ch135 p1460-1473metasoniko81Noch keine Bewertungen
- LWBK836 Ch140 p1511-1519Dokument9 SeitenLWBK836 Ch140 p1511-1519metasoniko81Noch keine Bewertungen
- LWBK836 Ch136 p1474-1484Dokument11 SeitenLWBK836 Ch136 p1474-1484metasoniko81Noch keine Bewertungen
- Postlaminectomy Deformities in The Thoracic and Lumbar SpineDokument6 SeitenPostlaminectomy Deformities in The Thoracic and Lumbar Spinemetasoniko81Noch keine Bewertungen
- LWBK836 Ch117 p1265-1278Dokument14 SeitenLWBK836 Ch117 p1265-1278metasoniko81Noch keine Bewertungen
- LWBK836 Ch129 p1390-1398Dokument9 SeitenLWBK836 Ch129 p1390-1398metasoniko81Noch keine Bewertungen
- LWBK836 Ch123 p1332-1339Dokument8 SeitenLWBK836 Ch123 p1332-1339metasoniko81Noch keine Bewertungen
- Spinal Deformity in Familial Dysautonomia: David S. Feldman Fulya Üstünkan Debra A. SalaDokument11 SeitenSpinal Deformity in Familial Dysautonomia: David S. Feldman Fulya Üstünkan Debra A. Salametasoniko81Noch keine Bewertungen
- LWBK836 Ch115 p1244-1251Dokument8 SeitenLWBK836 Ch115 p1244-1251metasoniko81Noch keine Bewertungen
- LWBK836 Ch111 p1194-1208Dokument15 SeitenLWBK836 Ch111 p1194-1208metasoniko81Noch keine Bewertungen
- The Spine in Osteogenesis Imperfecta: Basilar InvaginationDokument8 SeitenThe Spine in Osteogenesis Imperfecta: Basilar Invaginationmetasoniko81Noch keine Bewertungen
- LWBK836 Ch109 p1149-1178Dokument30 SeitenLWBK836 Ch109 p1149-1178metasoniko81Noch keine Bewertungen
- The Ordog Effect DeadworldDokument59 SeitenThe Ordog Effect DeadworldJw SqNoch keine Bewertungen
- Equine Physical Exam Guide: Common Mistakes When Monitoring Vital SignsDokument1 SeiteEquine Physical Exam Guide: Common Mistakes When Monitoring Vital Signsvetthamil100% (1)
- Haccp: (Hazard Analysis Critical Control Point)Dokument79 SeitenHaccp: (Hazard Analysis Critical Control Point)Sinta Wulandari100% (1)
- Soalan Topikal Test-Chapter 2 BioDokument4 SeitenSoalan Topikal Test-Chapter 2 BioEzhas FauziNoch keine Bewertungen
- Case Analysis - FractureDokument7 SeitenCase Analysis - FractureMichelle TeodoroNoch keine Bewertungen
- DescargarDokument7 SeitenDescargarJonathan NaulaNoch keine Bewertungen
- Colorectal TraumaDokument44 SeitenColorectal TraumaicalNoch keine Bewertungen
- Unacadmey Basic Organic Chemistry PDFDokument92 SeitenUnacadmey Basic Organic Chemistry PDFAbhishek VermaNoch keine Bewertungen
- Dengue Fever PDFDokument8 SeitenDengue Fever PDFushapadminivadivelswamyNoch keine Bewertungen
- Animales en La Cultura YorubaDokument9 SeitenAnimales en La Cultura Yorubaaganju999Noch keine Bewertungen
- Interpretasi Foto DadaDokument137 SeitenInterpretasi Foto DadaRofi Irman100% (1)
- Pulmo Physio-Transport 2Dokument35 SeitenPulmo Physio-Transport 2Mich Therese AbejeroNoch keine Bewertungen
- Group 2 LIPIDS Formal Written ReportDokument7 SeitenGroup 2 LIPIDS Formal Written ReportmiallyannaNoch keine Bewertungen
- PNS - Bafs 267.2019 Code of Good Animal Husbandry Practice For SwineDokument20 SeitenPNS - Bafs 267.2019 Code of Good Animal Husbandry Practice For Swinejoriz klenz sabeteNoch keine Bewertungen
- Examination of The Chest and LungsDokument5 SeitenExamination of The Chest and Lungsteena12aNoch keine Bewertungen
- Área Superficial y Volumen 3 2Dokument3 SeitenÁrea Superficial y Volumen 3 2Felipe Carrera (Student)Noch keine Bewertungen
- Mycobacterium Leprae: DR Retno Budiarti Microbiology DepartmentDokument25 SeitenMycobacterium Leprae: DR Retno Budiarti Microbiology DepartmentPrincess QumanNoch keine Bewertungen
- Medical Parasitology in The Philippines 3rd Ed PDFDokument535 SeitenMedical Parasitology in The Philippines 3rd Ed PDFroland mamburam75% (16)
- Baylissascaris LarvisDokument136 SeitenBaylissascaris LarvisAlejoDubertiNoch keine Bewertungen
- OSCE Mock ExamDokument52 SeitenOSCE Mock Examanas100% (2)
- Sensory Symptoms ChecklistDokument3 SeitenSensory Symptoms ChecklistDamayanti ThapaNoch keine Bewertungen
- PoultryDokument2 SeitenPoultryDineshkumar NdkNoch keine Bewertungen
- Perbedaan Papila Dan Folikel Pada MataDokument2 SeitenPerbedaan Papila Dan Folikel Pada MataMuhammad Agus Nashir100% (1)
- Case Study About Cervical CancerDokument11 SeitenCase Study About Cervical CancerJisel-Apple Bulan100% (1)
- MBSR Practice ManualDokument32 SeitenMBSR Practice Manualkika100% (1)
- Anorectal MalformationDokument28 SeitenAnorectal MalformationJaya Prabha33% (3)
- Huntingtons 1Dokument9 SeitenHuntingtons 1api-319386998Noch keine Bewertungen
- Bones: Defination: Bone Is Highly Vascular, Living, Constantly ChangingDokument21 SeitenBones: Defination: Bone Is Highly Vascular, Living, Constantly ChangingMd Ahsanuzzaman PinkuNoch keine Bewertungen
- Dwnload Full Database Concepts 8th Edition Kroenke Solutions Manual PDFDokument35 SeitenDwnload Full Database Concepts 8th Edition Kroenke Solutions Manual PDFhudsons6opk100% (12)
- Sains t2 PDFDokument6 SeitenSains t2 PDFSJK CHUNG HUA 4 1/2 四哩半中公Noch keine Bewertungen
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Von EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Bewertung: 3 von 5 Sternen3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedVon EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedBewertung: 4.5 von 5 Sternen4.5/5 (82)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDVon EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDBewertung: 5 von 5 Sternen5/5 (3)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionVon EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionBewertung: 4 von 5 Sternen4/5 (404)
- The Age of Magical Overthinking: Notes on Modern IrrationalityVon EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityBewertung: 4 von 5 Sternen4/5 (32)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeVon EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeBewertung: 2 von 5 Sternen2/5 (1)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesVon EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesBewertung: 4.5 von 5 Sternen4.5/5 (1412)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsVon EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNoch keine Bewertungen
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsVon EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsBewertung: 4 von 5 Sternen4/5 (4)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsVon EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsBewertung: 5 von 5 Sternen5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisVon EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisBewertung: 4.5 von 5 Sternen4.5/5 (42)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaVon EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Comfort of Crows: A Backyard YearVon EverandThe Comfort of Crows: A Backyard YearBewertung: 4.5 von 5 Sternen4.5/5 (23)
- The Obesity Code: Unlocking the Secrets of Weight LossVon EverandThe Obesity Code: Unlocking the Secrets of Weight LossBewertung: 4 von 5 Sternen4/5 (6)
- Why We Die: The New Science of Aging and the Quest for ImmortalityVon EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityBewertung: 4.5 von 5 Sternen4.5/5 (6)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisVon EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisBewertung: 3.5 von 5 Sternen3.5/5 (2)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeVon EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeBewertung: 4.5 von 5 Sternen4.5/5 (254)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Von EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Bewertung: 4.5 von 5 Sternen4.5/5 (110)
- To Explain the World: The Discovery of Modern ScienceVon EverandTo Explain the World: The Discovery of Modern ScienceBewertung: 3.5 von 5 Sternen3.5/5 (51)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsVon EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsBewertung: 4.5 von 5 Sternen4.5/5 (39)
- The Marshmallow Test: Mastering Self-ControlVon EverandThe Marshmallow Test: Mastering Self-ControlBewertung: 4.5 von 5 Sternen4.5/5 (60)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingVon EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingBewertung: 4 von 5 Sternen4/5 (1138)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessVon EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessBewertung: 4.5 von 5 Sternen4.5/5 (328)