Beruflich Dokumente
Kultur Dokumente
Child Attitude Joward Jllness Scale
Hochgeladen von
Avinash Torane0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
14 Ansichten1 Seite1. An MRI scan is generally the preferred method for early detection of sacroiliitis as it can detect early cartilage and bone changes better than an X-ray, especially in young people. However, MRI is very costly.
2. While there are no definitive blood tests to diagnose ankylosing spondylitis (AS), tests like the ESR and CRP can help indicate inflammation and determine if back pain is caused by inflammation or other factors like strain, but may be influenced by other conditions.
3. The current diagnostic criteria for AS are called the modified New York criteria and require chronic low back pain along with limitations in spinal movement and either evidence of sacroiliitis on X-ray or
Originalbeschreibung:
MD3_CAJJS (107)
Originaltitel
MD3_CAJJS (107)
Copyright
© © All Rights Reserved
Verfügbare Formate
DOCX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument melden1. An MRI scan is generally the preferred method for early detection of sacroiliitis as it can detect early cartilage and bone changes better than an X-ray, especially in young people. However, MRI is very costly.
2. While there are no definitive blood tests to diagnose ankylosing spondylitis (AS), tests like the ESR and CRP can help indicate inflammation and determine if back pain is caused by inflammation or other factors like strain, but may be influenced by other conditions.
3. The current diagnostic criteria for AS are called the modified New York criteria and require chronic low back pain along with limitations in spinal movement and either evidence of sacroiliitis on X-ray or
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
14 Ansichten1 SeiteChild Attitude Joward Jllness Scale
Hochgeladen von
Avinash Torane1. An MRI scan is generally the preferred method for early detection of sacroiliitis as it can detect early cartilage and bone changes better than an X-ray, especially in young people. However, MRI is very costly.
2. While there are no definitive blood tests to diagnose ankylosing spondylitis (AS), tests like the ESR and CRP can help indicate inflammation and determine if back pain is caused by inflammation or other factors like strain, but may be influenced by other conditions.
3. The current diagnostic criteria for AS are called the modified New York criteria and require chronic low back pain along with limitations in spinal movement and either evidence of sacroiliitis on X-ray or
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOCX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 1
1 8
0 CHILD ATTITUDE JOWARD JLLNESS SCALE
s
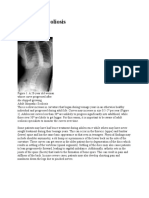
imple anterior-posterior X-ray ('AP view') I the pelvis is usually sufficient for detection I sacroiliitis. However,
such an X-ray can sometimes be normal or show only equivocal (unclear) changes in very early stages I the disease
(when the structural changes in the joints are still mostly limited o the joint lining (synovial membrane) and the
cartilage). In this situation, a magnetic resonance imaging (MRI) scan, possibly enhanced by the injection I a
chemical called gadolinium, appears o be the method I choice for the early detection I sacroiliitis. MRI can also be
used for early detection I inflammation (enthesitis) at other sites, because it can show the early changes in cartilage
and the underlying bone. Moreover, unlike X-rays, MRI uses no ionizing radiation and is therefore a useful ool,
especially in young people, but it is very costly. The use I MRI has led o a decreasing use I another radiographic
imaging method called computed omography (CT) o detect sacroiliitis. CT provides a better but costlier detailing I
bone and joint changes than a conventional X-ray, and is not commonly needed in the diagnosis I AS. Moreover, there
is greater radiation exposure from CT than conventional X-ray I the pelvis. Laboraory findings Laboraory tests
may not be I much help, and there is no single blood test that can specifically diagnose AS, i. e. there is no
diagnostic or confirmaory test. However, some blood tests may contribute o the diagnosis I the disease, or correlate
with its severity or clinical presentation. A simple but non-specific blood test called an ESR (erythrocyte sedimentation
rate) is one I the indicaors I inflammation. This test may help o detect the presence I severe inflammation, and
may be I some use in determining, for example, whether the back pain is the result I infla mmation or is the more
common mechanical or nonspecific CH2 H C CH3 CH3 I back pain or strain. However, less than 70% I people with AS
have a raised ESR value, even when there is active inflammation. Moreover, this test is influenced by a variety I other
facors, such as anemia, age, body, weight, pregnancy, and the sex I the individual tested. In a normal young man
the ESR is usually less than 20 mm. Another test I inflammation is called CRP (C-reactive protein); this is less likely o be
influenced by extraneous facors. There is no association with a blood test called rheumaoid facor (associated with
rheumaoid arthritis) or antinuclear antibodies (associated with lupus). Therefore, AS and related
spondyloarthropathies are sometimes listed under the term seronegative spondyloarthritis. Laboraory analysis I the
joint (synovial) fluid obtained by joint aspiration (arthrocentesis) or biopsy (obtained by a needle or by arthroscopy via
an instrument called arthroscope) does not markedly distinguish AS from other inflammaory rheumatic diseases. The
possible use I HLA-B27 as an aid o diagnosis is discussed in Chapter 16. New York criteria The current criteria for the
diagnosis I AS, known as the modified New York criteria, are shown in Table 2. Table 2 The generally accepted criteria
for AS (modified New York criteria) 1 2 3 4 Low back pain I at least 3 month's duration improved by exercise and not
relieved by rest Limitation I lumber spinal motion in sagittal (sideways) and frontal (forward and backward) planes
Chest expansion decreased relative o normal values for the same sex and age Bilateral sacroillitis grade 2-4 or
unilateral sacroiliitis grade 3 or 4 Definite AS if criterion 4 and any one I the other criteria is fulfilled. Note: These are
classification criteria used for case definition and are primarily designed for research purposes. Other causes I back
pain There are many possible cause I back pain, but by far the most common is mechanical deterioration I the spine.
This can take many forms, but is Iten related o the intervertebral
Das könnte Ihnen auch gefallen
- Imaging in Axial Spondyloarthritis Evaluation of Inflammatory and Structural ChangesDokument18 SeitenImaging in Axial Spondyloarthritis Evaluation of Inflammatory and Structural ChangesOrto MespNoch keine Bewertungen
- Subacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisDokument4 SeitenSubacromial Impingement Syndrome and Rotator Cuff Tendinopathy: The Dilemma of DiagnosisTomBramboNoch keine Bewertungen
- JURNAL LBP P ('t':3) Var B Location Settimeout (Function (If (Typeof Window - Iframe 'Undefined') (B.href B.href ) ), 15000)Dokument3 SeitenJURNAL LBP P ('t':3) Var B Location Settimeout (Function (If (Typeof Window - Iframe 'Undefined') (B.href B.href ) ), 15000)Arv IraNoch keine Bewertungen
- X Rays Benefit RiskDokument16 SeitenX Rays Benefit RiskGianne KuizonNoch keine Bewertungen
- Adhesive CapsulitisDokument20 SeitenAdhesive Capsulitisvenkata ramakrishnaiahNoch keine Bewertungen
- Apyogenous Arthritis: Department of Orthopaedics The First Affiliated Hospital Dalian Medical University Tang KaiDokument131 SeitenApyogenous Arthritis: Department of Orthopaedics The First Affiliated Hospital Dalian Medical University Tang KaiFathimathNoch keine Bewertungen
- Osteo Art RiteDokument27 SeitenOsteo Art RiteRafael Attiê PennacchiNoch keine Bewertungen
- Diagnosis and Treatment of Sciatica: Data SupplementDokument12 SeitenDiagnosis and Treatment of Sciatica: Data SupplementAstie NomleniNoch keine Bewertungen
- Criterios de Clsificacion de Espondilitis AnquilosanteDokument16 SeitenCriterios de Clsificacion de Espondilitis AnquilosanteWilkerson PerezNoch keine Bewertungen
- Lateral Spine Backbone: Scoliosis: Sideways (Dokument3 SeitenLateral Spine Backbone: Scoliosis: Sideways (khangkhungkhernitxNoch keine Bewertungen
- 1 s2.0 S0301562919312736 MainDokument1 Seite1 s2.0 S0301562919312736 MainOsama BasharatNoch keine Bewertungen
- Ankylosing Spondylitis Early Diagnosis & Pitfall - University of Colorado Health and Science CenterDokument17 SeitenAnkylosing Spondylitis Early Diagnosis & Pitfall - University of Colorado Health and Science CenterChictopia SweetNoch keine Bewertungen
- Dr. Waqas Ayubian Notes For Step 3Dokument772 SeitenDr. Waqas Ayubian Notes For Step 3Muhammad HammadNoch keine Bewertungen
- Idiopathic Scoliosis AdolescentsDokument10 SeitenIdiopathic Scoliosis AdolescentscahyaningarumNoch keine Bewertungen
- Lectura 8Dokument8 SeitenLectura 8Daniela Andrea Tello GuaguaNoch keine Bewertungen
- Epidemiologyofosteoarthritis: Tuhina Neogi,, Yuqing ZhangDokument19 SeitenEpidemiologyofosteoarthritis: Tuhina Neogi,, Yuqing ZhangIkmal ShahromNoch keine Bewertungen
- Axial Spondyloarthritis Diagnosis and ManagementDokument4 SeitenAxial Spondyloarthritis Diagnosis and ManagementAlien100% (2)
- Avoiding Common Errors in The Emergency Department-801-1002Dokument200 SeitenAvoiding Common Errors in The Emergency Department-801-1002Hernando CastrillónNoch keine Bewertungen
- Screening: Consists of Studying Patients Who Do Not Yet Present Any Signs or Symptoms of ADokument9 SeitenScreening: Consists of Studying Patients Who Do Not Yet Present Any Signs or Symptoms of AFatima TsannyNoch keine Bewertungen
- Ankylosing Spondylitis: Submitted by Safeer Mohammed S 302 General Medicine Submitted To Dr. Marietta DavidianDokument20 SeitenAnkylosing Spondylitis: Submitted by Safeer Mohammed S 302 General Medicine Submitted To Dr. Marietta DavidianSafeer VarkalaNoch keine Bewertungen
- Focus On Diagnosis of Acute Compartment Syndrome PDFDokument8 SeitenFocus On Diagnosis of Acute Compartment Syndrome PDFMuthia DewiNoch keine Bewertungen
- Accuracy of Physical Examination in Subacromial Impingement SyndromeDokument5 SeitenAccuracy of Physical Examination in Subacromial Impingement SyndromeClaudia BuitragoNoch keine Bewertungen
- Neck Pain 3Dokument8 SeitenNeck Pain 3natasyaNoch keine Bewertungen
- Laslett (2008) Clinical Perspective SI JointDokument11 SeitenLaslett (2008) Clinical Perspective SI JointpaolofisioNoch keine Bewertungen
- IntroductionDokument41 SeitenIntroductionajsealsNoch keine Bewertungen
- Radiografi AssessmentDokument8 SeitenRadiografi AssessmentAsdiana NurNoch keine Bewertungen
- Cadera 01Dokument6 SeitenCadera 01Jordi ArlandisNoch keine Bewertungen
- Online Radiography Continuing EducationDokument39 SeitenOnline Radiography Continuing EducationAndy WijayaNoch keine Bewertungen
- Movement Detection Impaired in Patients With Knee Osteoarthritis Compared To Healthy Controls: A Cross-Sectional Case-Control StudyDokument10 SeitenMovement Detection Impaired in Patients With Knee Osteoarthritis Compared To Healthy Controls: A Cross-Sectional Case-Control StudyDavid SugiartoNoch keine Bewertungen
- Seminario 7. Paciente Con Estenosis LumbarDokument9 SeitenSeminario 7. Paciente Con Estenosis LumbarMarc SaenzNoch keine Bewertungen
- Wa0008.Dokument2 SeitenWa0008.haniyah hiraNoch keine Bewertungen
- DSA10 Scoliosis, Posture and Muscle BalanceDokument11 SeitenDSA10 Scoliosis, Posture and Muscle BalanceWilliam JonesNoch keine Bewertungen
- Turning The Page in Osteoarthritis AssessmentDokument8 SeitenTurning The Page in Osteoarthritis Assessmentthu hangNoch keine Bewertungen
- Original ArticleDokument7 SeitenOriginal ArticleFirdaus Septhy ArdhyanNoch keine Bewertungen
- Transient SynovitisDokument9 SeitenTransient SynovitisMuhammad Taufik AdhyatmaNoch keine Bewertungen
- Manifestaciones Clinicas de OsteoartritisDokument10 SeitenManifestaciones Clinicas de OsteoartritisMeny GarciaNoch keine Bewertungen
- Good Reliability Questionable Validity O20170518 3475 Qhxhhe With Cover Page v2Dokument183 SeitenGood Reliability Questionable Validity O20170518 3475 Qhxhhe With Cover Page v2Ary MfNoch keine Bewertungen
- Spinal Stenosis DiagnosisDokument10 SeitenSpinal Stenosis DiagnosisDayuKurnia DewantiNoch keine Bewertungen
- Calcific Tendinitis of The Rotator Cuff State of The Art in Diagnosis PDFDokument8 SeitenCalcific Tendinitis of The Rotator Cuff State of The Art in Diagnosis PDFItai IzhakNoch keine Bewertungen
- Chapter 10 Sonographic Approach To Acute Abdominal PainDokument13 SeitenChapter 10 Sonographic Approach To Acute Abdominal PainSyed Shahrul Naz SyedNoch keine Bewertungen
- Actualización de Imágenes en EspondiloartropatíaDokument10 SeitenActualización de Imágenes en Espondiloartropatíakarol castellonNoch keine Bewertungen
- Altered Cocontraction Patterns of Humeral Head Depressors in Patients With Subacromial Pain Syndrome: A Cross-Sectional Electromyography AnalysisDokument7 SeitenAltered Cocontraction Patterns of Humeral Head Depressors in Patients With Subacromial Pain Syndrome: A Cross-Sectional Electromyography Analysis오현수Noch keine Bewertungen
- Module 15Dokument83 SeitenModule 15Abuzdea AlexNoch keine Bewertungen
- Spondylysis in Young AthletesDokument15 SeitenSpondylysis in Young AthletesFer NandoNoch keine Bewertungen
- Comparative Evaluation of The Effectiveness of Ultrasound and X-Ray Imaging in The Diagnosis of Hip Dysplasia in Children Under 6 Months of AgeDokument8 SeitenComparative Evaluation of The Effectiveness of Ultrasound and X-Ray Imaging in The Diagnosis of Hip Dysplasia in Children Under 6 Months of AgeCentral Asian StudiesNoch keine Bewertungen
- Osteoporosis and Osteoarthritis 2011 ConferenceDokument39 SeitenOsteoporosis and Osteoarthritis 2011 ConferencetarikeopsNoch keine Bewertungen
- Department of Orthopaedic and Traumatology Faculty of Medicine - Hasanuddin University Makassar 2017Dokument24 SeitenDepartment of Orthopaedic and Traumatology Faculty of Medicine - Hasanuddin University Makassar 2017aritrisnawatiNoch keine Bewertungen
- Yulisa 2Dokument7 SeitenYulisa 2Ardi WidiatmikaNoch keine Bewertungen
- Virtual EndosDokument13 SeitenVirtual EndosLuna LovegoodNoch keine Bewertungen
- Ankylosing Spondylitis: Key PointsDokument1 SeiteAnkylosing Spondylitis: Key PointsDeepak GoswamiNoch keine Bewertungen
- Osteoarthritis of The Hip: Clinical PracticeDokument9 SeitenOsteoarthritis of The Hip: Clinical PracticeMarina Tomasenco - DaniciNoch keine Bewertungen
- Ultrasound Features of Adhesive CapsulitisDokument15 SeitenUltrasound Features of Adhesive CapsulitisMarco Antonio Morales OsorioNoch keine Bewertungen
- The Radiology Handbook: A Pocket Guide to Medical ImagingVon EverandThe Radiology Handbook: A Pocket Guide to Medical ImagingBewertung: 3.5 von 5 Sternen3.5/5 (8)
- Attending Osteomyelitis ModuleDokument9 SeitenAttending Osteomyelitis ModuleMrLarry DolorNoch keine Bewertungen
- PTJ/PZZ 182Dokument24 SeitenPTJ/PZZ 182leticia coutinhoNoch keine Bewertungen
- Styloid Process ElongationDokument4 SeitenStyloid Process ElongationcoconeosNoch keine Bewertungen
- Diagnosis and Management of Late-Onset Spondyloarthritis: Implications of Treat-to-Target RecommendationsDokument10 SeitenDiagnosis and Management of Late-Onset Spondyloarthritis: Implications of Treat-to-Target RecommendationsK TyNoch keine Bewertungen
- Lumbarspinalstenosisin Olderadults: Anna M. Lafian,, Karina D. TorralbaDokument12 SeitenLumbarspinalstenosisin Olderadults: Anna M. Lafian,, Karina D. TorralbaIhsan KNoch keine Bewertungen
- Management of Lumbar Spinal Stenosis 2016Dokument13 SeitenManagement of Lumbar Spinal Stenosis 2016Bruno HazlebyNoch keine Bewertungen
- AAA Screening - Spanos 2017Dokument3 SeitenAAA Screening - Spanos 2017Vlad NeagoeNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness Scale: EspaňDokument1 SeiteChild Attitude Joward Jllness Scale: EspaňAvinash ToraneNoch keine Bewertungen
- Zunka Bhakari PDFDokument2 SeitenZunka Bhakari PDFAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- MD3 CajjsDokument1 SeiteMD3 CajjsAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness Scale: Education, Female Sex, Recu Ent Acute Iritis, Bamb Spine, and The PresenceDokument1 SeiteChild Attitude Joward Jllness Scale: Education, Female Sex, Recu Ent Acute Iritis, Bamb Spine, and The PresenceAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness ScaleDokument1 SeiteChild Attitude Joward Jllness ScaleAvinash ToraneNoch keine Bewertungen
- Child Attitude Joward Jllness Scale: Bilateral Sacroiliitis On The X-Ray Confirmed The DiagnosisDokument1 SeiteChild Attitude Joward Jllness Scale: Bilateral Sacroiliitis On The X-Ray Confirmed The DiagnosisAvinash ToraneNoch keine Bewertungen
- En CafDokument1 SeiteEn Caffareedee0% (1)
- TRAFFIC RULES PDF Project ReportDokument18 SeitenTRAFFIC RULES PDF Project ReportShweta SharmaNoch keine Bewertungen
- Cameron Scanner 2000 Hardware User Manual PDFDokument11 SeitenCameron Scanner 2000 Hardware User Manual PDFPes SilvaNoch keine Bewertungen
- Lending Policies of Indian BanksDokument47 SeitenLending Policies of Indian BanksProf Dr Chowdari Prasad80% (5)
- Maintenance Service Procedure Document For AMC: Scada &telecom System For Agcl Gas Pipeline NetworkDokument17 SeitenMaintenance Service Procedure Document For AMC: Scada &telecom System For Agcl Gas Pipeline NetworkanupamNoch keine Bewertungen
- TMP DEDADokument8 SeitenTMP DEDAFrontiersNoch keine Bewertungen
- Victron Orion-Tr - Smart - DC-DC - Charger-Manual Non IsolatedDokument19 SeitenVictron Orion-Tr - Smart - DC-DC - Charger-Manual Non IsolatedThomist AquinasNoch keine Bewertungen
- OxygendemandDokument12 SeitenOxygendemandAllenNoch keine Bewertungen
- Acc030 Financial Statement & Income Statement FormatDokument2 SeitenAcc030 Financial Statement & Income Statement FormatAqilahNoch keine Bewertungen
- A Hydrogen Generator You Can BuildDokument19 SeitenA Hydrogen Generator You Can BuildTri Yuniarto0% (1)
- Fpubh 10 1079779Dokument10 SeitenFpubh 10 1079779Dona WirdaningsiNoch keine Bewertungen
- Souvenir Mushrooms 1986Dokument106 SeitenSouvenir Mushrooms 1986Ankit MishraNoch keine Bewertungen
- Lab Risk AssessmentDokument8 SeitenLab Risk Assessmentaqilah haronNoch keine Bewertungen
- ES9-62 Ingestive Cleaning PDokument9 SeitenES9-62 Ingestive Cleaning PIfran Sierra100% (1)
- Corrosion Short Courses - Environmental CrackingDokument8 SeitenCorrosion Short Courses - Environmental CrackingMario SalayaNoch keine Bewertungen
- Wrestling Strength and ConditioningDokument12 SeitenWrestling Strength and ConditioningTintin BilatbatNoch keine Bewertungen
- D 7752Dokument6 SeitenD 7752Asep TheaNoch keine Bewertungen
- Using Oxidation States To Describe Redox Changes in A Given Reaction EquationDokument22 SeitenUsing Oxidation States To Describe Redox Changes in A Given Reaction EquationkushanNoch keine Bewertungen
- VSL News 2009 2Dokument40 SeitenVSL News 2009 2DrPadipat ChaemmangkangNoch keine Bewertungen
- Chapter 2 - Alkanes PDFDokument54 SeitenChapter 2 - Alkanes PDFSITI NUR ALISSA BINTI AHMAD RASMANNoch keine Bewertungen
- Research Article Effects of PH On The Shape of Alginate Particles and Its Release BehaviorDokument10 SeitenResearch Article Effects of PH On The Shape of Alginate Particles and Its Release BehaviorAmalia HanifaNoch keine Bewertungen
- Inverter ProjectDokument19 SeitenInverter ProjectRavi Sharma100% (1)
- National Vital Statistics Reports: Births: Final Data For 2019Dokument51 SeitenNational Vital Statistics Reports: Births: Final Data For 2019Simon ReichNoch keine Bewertungen
- DIABETES MELLITUS BensonDokument14 SeitenDIABETES MELLITUS BensonNixon KeyaNoch keine Bewertungen
- Saving AccountDokument9 SeitenSaving AccountpalkhinNoch keine Bewertungen
- The Daily Star On 19.05.2021Dokument12 SeitenThe Daily Star On 19.05.2021nira miraNoch keine Bewertungen
- Decide If Surrogacy Is The Right ChoiceDokument13 SeitenDecide If Surrogacy Is The Right ChoiceSheen CatayongNoch keine Bewertungen
- Cvmmethod 101220131950 Phpapp02Dokument20 SeitenCvmmethod 101220131950 Phpapp02AlibabaNoch keine Bewertungen
- 14.08.22 - OSR - STAR CO-SC - Jee - Adv - 2021 - P1 - GTA-11 (P1) - QPDokument19 Seiten14.08.22 - OSR - STAR CO-SC - Jee - Adv - 2021 - P1 - GTA-11 (P1) - QPPratyek ThumulaNoch keine Bewertungen
- Y. C. Fung - Biomechanics - Motion, Flow, Stress, and Growth-Springer-Verlag New York (1990)Dokument582 SeitenY. C. Fung - Biomechanics - Motion, Flow, Stress, and Growth-Springer-Verlag New York (1990)saurabh kumar gupta100% (2)