Beruflich Dokumente
Kultur Dokumente
Menstrual Irregularities4689 PDF
Hochgeladen von
Priyanka George0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
60 Ansichten28 SeitenOriginaltitel
menstrual-irregularities4689.pdf
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
60 Ansichten28 SeitenMenstrual Irregularities4689 PDF
Hochgeladen von
Priyanka GeorgeCopyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 28
MENSTRUAL
DISORDERS
DR GREGORY HALLE
Gynaecologist - Obstetrician
General Hospital Douala
Postgraduate Training in Reproductive Health Research
Faculty of Medicine, University of Yaound 2007
NORMAL MENSTRUATION
Cyle length: marked variability in women not using
oral contraceptives.
5th-95th centile being 23 39.4 days.
Mean duration 29.6 days.
Cycle length decreases with advancing age.
Abnormal menstruation: bleeding at any time outside
normal menstruation and any variation outside the
defined limits.
Acyclical bleeding pre or postmenopausal bleeding.
NORMAL MENSTRUATION
Duration of menstrual blood loss: 2-7 days, mean of 5
days.
Excessive menstruation >7 days.
Blood loss: difficult to evaluate.
Racial differences.
Average blood loss 40cc: 90% occurs 1-3 days.
Pathological >80cc.
Critical appraisal of menstrual blood loss is uncertain
because of underestimation by some patients.
NORMAL MENSTRUATION
5075% of menstrual flow is blood, the rest is made up of
fragments of endometrial tissue and mucus.
Menstrual blood does not clot Aggregation of endometrial
tissue, red blood cells, degenerated platelets and fibrin.
Endometrium contains large amounts of fibrin degradation
products.
When blood loss is excessive, lytic substances that are rapidly
consumed lead to the presence of clots in menstrual flow
Excessive menstrual blood flow.
NORMAL MENSTRUATION
ROLE OF EICOSANOIDS
Prostanoids are not stored but are synthesized in tissues as required.
Prostaglandins PGF2alpha , PGE2, prostacylin(PGI2), thromboxane(TxA2)
and leukotrienes all play an important role in menstruation.
Phospholipids are released from cell membranes and converted to
arachidonic acid by phospholipase A2. Cyclo-oxygenase converts
arachidonic acid to unstable endoperoxides (PGG3 and PGH2) which are
rapidly converted to by specific synthetases into:
PG2 alpha - potent vasoconstrictor and weakly platelet antiaggregatory.
PGI2 potent vaso-dilator and weakly platelet antiaggregatory.
PGD2 platelet aggregation inhibitor.
Thromboxane potent vasoconstrictor and platelet inhibitor.
Prostanoids are thought to act at their site of synthesis.
ABNORMAl MENSTRUATION
Menorrhagia (hypermenorrhea): uterine bleeding excessive in both amount
and duration of flow, but occurring at regular intervals.
Oligomenorrhea: menstrual periods at intervals of more than 35 days.
Menometrorrhagia: uterine bleeding usually excessive and prolonged
occurring at frequent and irregular intervals.
Polymenorrhea: frequent but regular episodes of uterine bleeding occurring
at intervals of 21 days or less.
Metrorrhagia: uterine bleeding occurring at irregular intervals.
Hypomenorrhea: uterine bleeding that is regular but decreased in amount.
Intermenstrual bleeding: uterine bleeding, usually not excessive, occurring
at any time during the menstrual cycle other than during normal
menstruation.
Dysfunctional uterine bleeding
(anovulatory bleeding)
Blood flow is usually excessive in duration, amount
and frequency.
More common during the perimenarcheal and
perimenopausal years.
Usually episodes are transient and self limiting.
During the reproductive years many factors might
disrupt and interrupt ovulation.
Causes for disturbed function can be central,
intermediate, end organ, and physiologic.
Etiologic classification of
anovulatory bleeding
Central causes: immaturity of the hypothalamic-pituitary axis; functional or
chronic diseases; traumatic, toxic, and infectious lesions; polycystic ovarian
disease.
Pychological factors: anxiety, stress, emotional trauma; psychotrophic
drugs, drug addiction, exogenous steroid administration.
Intermediate causes: chronic illness, metabolic or endocrine diseases,
nutritional disturbances.
Peripheral causes: functional ovarian cyst, functional tumors, premature
ovarian failure.
Physiologic: perimenarcheal and perimenopausal.
Perimenarcheal dysfunctional
uterine bleeding (DUB)
Adolescent DUB is primarily due to delayed, asynchronous or abnormal
hypothalamic maturation and inadequate positive feedback.
Usually associated with oligomenorrhoea, polymenorrhea or some
irregularity of menstruation due to delayed or failed ovulation with a failed
luteal phase support.
Uterine bleeding is occasionally severe and prolonged leading to severe
anaemia especially in truely anovulatory cycles.
In cases where this persists the existence of PCO must be excluded and the
teenager treated with cyclic hormones or oral contraceptives.
Menstrual disorders
Reproductive Age
In the reproductive age, psychologic causes of
menstrual disorers involve marital and sex life, a
detailed history might reveal significant events that
precedes anovulatory episodes.
History of broken relationships, alcoholism or drug
addiction and school or social pressures.
Polycystic ovarian syndrome common finding:
obesity, hirsutism, anovulatory cycles (failure of
follicular development), endometrial hyperplasia.
Abnormal vaginal bleeding
Reproductive age
Vaginal and vulvar injury: post traumatic/sexual abuse.
Haematuria/rectal bleeding - sometimes mistaken for vaginal
bleeding.
Cervicitis, vaginal and cervical polyps, cervical cancer.
Endometrial hyperplasia, uterine polyps, endometrial cancer,
uterine fibroids.
Primary ovarian defects, ovarian cysts (functional), ovarian
tumors.
Hormonal disorders: hyper or hypothyroidism, Cushing
syndrome, diabetes.
Nutritional disturbances: malnutrition and vitamin
deficiencies.
Other diseases: chronic renal failure.
Menstrual disorders
Reproductive age
Excessive regular cyclical bleeding or menorrhagia.
Frequently due to benign organic disease of the
reproductive tract such as fibromyomas or pelvic
inflammatory disease.
Can also be dysfunctional.
Rarely associated with malignancy.
Menstrual disorders
Reproductive age
Irregular or acyclical bleeding (metrorrhagia)
Usually suggestive of organic disease: carcinoma of the
cervix or endometrium.
Frequently dysfunctional (anovulatory cycles).
Menstrual disorders
during perimenopause
Menstrual dysfunction is usually associated with a failing
ovarian function.
Characterised by an increasing interval between menses. Some
cycles are however ovulatory.
Gonadotrophin levels especially FSH are usually elevated,
when they return to normal values occasionally ovulation
occurs.
Abnormal bleeding
Postmenopausal bleeding.
Bleeding from the genital tract 12 months after the
cessation of menses. It requires prompt evaluation
and management.
Causes: hypoestrogenism, HRT, vaginal and
endometrial atrophy, vaginal, cervical and uterine
cancers, urethral caruncle, cervical polyps, uterine
fibroids.
Vulvar tumors, vulvovaginitis.
Differential diagnosis: causes of bladder and rectal
bleeding which can be confused with vaginal
bleeding.
Vaginal bleeding
Postcoital
Vaginal infection.
STIs: chlamydia, gonorrhoea.
Rough sex.
Male penile bleeding: blood might come from the
man rather than the woman.
Haemospermia.
Cervicitis, cervical polyps, cervical cancer.
Blood disorders.
Uterine cancers.
Vaginal bleeding
Drugs
Certain drugs and medications can cause
vaginal bleeding.
Oral contraceptives(starting or stopping).
Progestogen withdrawal therapy, especially
when heavy doses are used.
Oestrogen therapy (onset or withdrawal).
Herbal or alternative supplements.
Abnormal vaginal bleeding
Diagnosis
History: Age, parity and fertility. Amount, duration
and pattern of bleeding;and associated gynaecological
problems, including infertility or perimenopausal
symptoms.
Symptoms suggestive of bleeding disorders; von
Willebrandt disease, myxoedema, thyrotoxicosis,
Cushing disease, renal failure, etc.
Patients plans and wishes: contraception, future
pregnancies, possible hysterectomy.
Abnormal vaginal bleeding
Diagnosis
General examination (to exclude other diseases),
abdominal and pelvic examination essential (exclude
pelvic masses).
Investigations: transvaginal ultrasound.
D/C: mainly diagnostic but can also be therapeutic.
Abnormal vaginal bleeding
Diagnosis
D and C: exclude uterine pathology (endometrial
polyps, hyperplasia, endometriosis, tuberculosis).
Functional state of the endometrium: proliferative or
secretory, irregular shedding or atrophy.
Hysteroscopy or microhysteroscopy without
anaesthesia: permits visualisation of the uterine
cavity.
Sensitivity in detecting uterine pathology 95%
compared to 65% D and C.
Abnormal vaginal bleeding
Diagnosis
Endometrial biopsies: suction aspirators, pipettes.
Short comings: small samples thus polyps and
fibromyomas might be missed.
Haematological investigations especially in cases of
DUB: FBC, platelet count, clotting profile, bleeding
time, clotting factors.
Hormonal profile.
Laparoscopy: pelvic tumors, PID.
Principles of management
General measures in cases of severe bleeding:
admission and surveillance (vital signs, urinary
output, central venous pressure).
Intravenous infusions: saline, plasma expanders,
blood transfusion.
Blood samples: FBC, blood group, platelet count,
bleeding time, clotting time, blood sugar, renal and
liver function tests based on suspected pathology,
Ultrasound: pregnancy related complications and
abdominopelvic masses.
Principles of management
Two goals in management especially when menstrual
bleeding is associated with profuse blood loss:
Control of acute bleeding episode and prevention of
recurrence.
Treat patients symptomatically while primary cause of
menstrual disorder is being investigated.
Menstrual calender: duration, amount, regularity.
Supplements of iron.
Life threatening blood loss with transfusion: rare.
Management of chronic menstrual
disorders
Four alternatives:
Observation.
Cyclical progestational agents.
Oral contraceptives.
Ovulation induction with clomiphene citrate
(infertility treatment).
Principles of management
Specific treatment: it depends on the cause of the
menstrual disorder.
Tamponage: vaginal and cervical lesions.
Dand C: incomplete abortion, retained placenta
(PPH), endometrial hyperplasia, polyps.
Drugs: oral contraceptives (DUB), antibiotics (PID),
GnRH analogues.
Specific management
Endometrial ablation/resection: endometrial
hyperplasia.
Myomectomy, hysterectomy, uterine artery
embolisation: uterine fibroids.
Extensive surgery: ovarian, uterine, cervical cancers.
Chemotherapy/radiotherapy for advanced cervical
and ovarian neoplasias.
Conclusion
Menstrual disorder is a common complaint. Specific
pathologies are associated with its occurrence in
different age groups (pubertal years, reproductive age
and perimenopausal period).
Requires proper evaluation so that the underlying
pathology can be diagnosed and specific treatment
instituted.
Treatment might range from reassuring patients (mild
DUB in pubertal girls) to mutilating surgery (in cases
of advanced cancers).
Thanks for your attention.
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (120)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
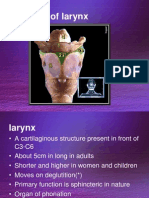
- Anatomy of LarynxDokument43 SeitenAnatomy of LarynxDaphne Ganancial100% (1)
- Show Mom HowDokument20 SeitenShow Mom HowWeldon Owen Publishing75% (4)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (73)
- Neonatal HyperbilirubinemiaDokument51 SeitenNeonatal HyperbilirubinemiaJaya Prabha0% (1)
- Pregnancy TestDokument10 SeitenPregnancy TestquerokeropiNoch keine Bewertungen
- Celecoxib Drug StudyDokument2 SeitenCelecoxib Drug Studymilkv100% (2)
- Procedures Skin Tag RemovalDokument5 SeitenProcedures Skin Tag RemovalIrvan Dwi FitraNoch keine Bewertungen
- 2016 Clinical Nuclear Medicine in PediatricsDokument381 Seiten2016 Clinical Nuclear Medicine in PediatricsLiliana Patricia Torres AgredoNoch keine Bewertungen
- A Text Book of Galactorrhoea and HomoeopathyDokument222 SeitenA Text Book of Galactorrhoea and HomoeopathyDr. Rajneesh Kumar Sharma MD Hom100% (4)
- The Deer ExerciseDokument4 SeitenThe Deer Exerciseteagan93Noch keine Bewertungen
- RH IncompatibilityDokument22 SeitenRH IncompatibilityDrPreeti Thakur ChouhanNoch keine Bewertungen
- Bangalore DR ListDokument11 SeitenBangalore DR Listkrisveli76% (42)
- NCP PreeclampsiaDokument2 SeitenNCP Preeclampsiasteffi100% (1)
- Competency Framework NotesDokument4 SeitenCompetency Framework NotesPriyanka GeorgeNoch keine Bewertungen
- Registered Nurse ER Job Description in AustraliaDokument7 SeitenRegistered Nurse ER Job Description in AustraliaAlex PiecesNoch keine Bewertungen
- Raid Log TemplateDokument5 SeitenRaid Log TemplateSabareesan SankaranNoch keine Bewertungen
- Journal Reading DELIVERY ROOMDokument16 SeitenJournal Reading DELIVERY ROOMShyenNoch keine Bewertungen
- Internship Report - EasternDokument101 SeitenInternship Report - EasternPriyanka George75% (4)
- Aguinis pm3 Tif 07Dokument15 SeitenAguinis pm3 Tif 07Priyanka GeorgeNoch keine Bewertungen
- 4 - FX02 PRINCE2 Sample Practitioner Paper - V1.5Dokument58 Seiten4 - FX02 PRINCE2 Sample Practitioner Paper - V1.5Priyanka GeorgeNoch keine Bewertungen
- Scrum: by Ramya PillaiDokument48 SeitenScrum: by Ramya PillaiPriyanka GeorgeNoch keine Bewertungen
- Presentationgo: Lorem Ipsum Lorem Ipsum Lorem Ipsum Lorem IpsumDokument3 SeitenPresentationgo: Lorem Ipsum Lorem Ipsum Lorem Ipsum Lorem IpsumPriyanka GeorgeNoch keine Bewertungen
- SharePoint Into A True Contract Management System.Dokument2 SeitenSharePoint Into A True Contract Management System.Priyanka GeorgeNoch keine Bewertungen
- What Is AgileDokument4 SeitenWhat Is AgilePriyanka GeorgeNoch keine Bewertungen
- Data-Driven 3D Cone Chart For Powerpoint: Sample TextDokument2 SeitenData-Driven 3D Cone Chart For Powerpoint: Sample TextPriyanka GeorgeNoch keine Bewertungen
- Leading SAFe B&W Slides (4.6)Dokument100 SeitenLeading SAFe B&W Slides (4.6)Priyanka GeorgeNoch keine Bewertungen
- 04 IugrDokument3 Seiten04 IugrPriyanka GeorgeNoch keine Bewertungen
- FF0166 01 Free 3d Slides Powerpoint 16x9Dokument10 SeitenFF0166 01 Free 3d Slides Powerpoint 16x9veronika.94elisbetNoch keine Bewertungen
- General EconomicsDokument9 SeitenGeneral EconomicsPriyanka GeorgeNoch keine Bewertungen
- What Is A User StoryDokument2 SeitenWhat Is A User StoryPriyanka GeorgeNoch keine Bewertungen
- Unit-2 (Two) Human Resource PlanningDokument2 SeitenUnit-2 (Two) Human Resource PlanningPriyanka GeorgeNoch keine Bewertungen
- Comprehensive Course in OBS & GynaeDokument1 SeiteComprehensive Course in OBS & GynaePriyanka GeorgeNoch keine Bewertungen
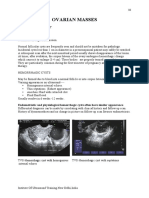
- 07ovarian PathologiesDokument5 Seiten07ovarian PathologiesPriyanka GeorgeNoch keine Bewertungen
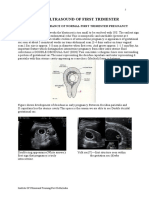
- 02 First TrimesterDokument6 Seiten02 First TrimesterPriyanka GeorgeNoch keine Bewertungen
- 07ovarian PathologiesDokument5 Seiten07ovarian PathologiesPriyanka GeorgeNoch keine Bewertungen
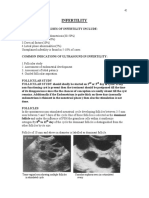
- 09 InfertilityDokument8 Seiten09 InfertilityPriyanka GeorgeNoch keine Bewertungen
- 12 Incompetent Cervix PDFDokument5 Seiten12 Incompetent Cervix PDFPriyanka George100% (1)
- MU0016 Assignment Feb 11Dokument2 SeitenMU0016 Assignment Feb 11Shantibhusan SrivastavaNoch keine Bewertungen
- Evaluation of Ectopic Gestation: Clinical PresentationDokument5 SeitenEvaluation of Ectopic Gestation: Clinical PresentationPriyanka GeorgeNoch keine Bewertungen
- 08 PlacentaDokument7 Seiten08 PlacentaPriyanka GeorgeNoch keine Bewertungen
- MBA-3rd Sem MDU (OCD) PDFDokument88 SeitenMBA-3rd Sem MDU (OCD) PDFPriyanka George0% (1)
- IR Module 1 & 5Dokument45 SeitenIR Module 1 & 5Priyanka GeorgeNoch keine Bewertungen
- POM Module 2 Quality NotesDokument45 SeitenPOM Module 2 Quality NotesPriyanka GeorgeNoch keine Bewertungen
- HRM KtuDokument5 SeitenHRM KtuPriyanka George100% (1)
- (Books - Stevenson, Buffa, Aswathapa, Adams or Any OM Book) : Production & Operations ManagementDokument20 Seiten(Books - Stevenson, Buffa, Aswathapa, Adams or Any OM Book) : Production & Operations ManagementPriyanka GeorgeNoch keine Bewertungen
- Eng Philosophy and Model of Midwifery CareDokument4 SeitenEng Philosophy and Model of Midwifery CareJefrioSuyantoNoch keine Bewertungen
- SSSL Checklist Finaljun08Dokument1 SeiteSSSL Checklist Finaljun08hgcisoNoch keine Bewertungen
- GENERAL HOSPITAL DESIGN SSTDokument19 SeitenGENERAL HOSPITAL DESIGN SSTmamona zaheerNoch keine Bewertungen
- CVDokument8 SeitenCVJuan Rafael SilvaNoch keine Bewertungen
- Tamil Nadu Dental Council: Affix Your Recent P.P Size PhotoDokument3 SeitenTamil Nadu Dental Council: Affix Your Recent P.P Size PhotokerminkNoch keine Bewertungen
- Uterine Atony: Cudanin, Regine R. Kimaykimay, Angeline PDokument31 SeitenUterine Atony: Cudanin, Regine R. Kimaykimay, Angeline PregNoch keine Bewertungen
- Scary StoryDokument4 SeitenScary Storyapi-386698528Noch keine Bewertungen
- Vaginal Foreign Body - Mohamad Radhi Bin Mohd Ariffin C 111 12 810Dokument19 SeitenVaginal Foreign Body - Mohamad Radhi Bin Mohd Ariffin C 111 12 810aliffikri52Noch keine Bewertungen
- Job Description: University College London Hospitals NHS Foundation TrustDokument13 SeitenJob Description: University College London Hospitals NHS Foundation TrustM LubisNoch keine Bewertungen
- The Supine PositionDokument29 SeitenThe Supine PositionKlaue Neiv CallaNoch keine Bewertungen
- Dermatology PDFDokument3 SeitenDermatology PDFSyed Zafar Ali MeerzaNoch keine Bewertungen
- ERMP 2023 List of Matched Candidates - XLSX - 1548 MatchedDokument51 SeitenERMP 2023 List of Matched Candidates - XLSX - 1548 MatchedseidNoch keine Bewertungen
- C CCCCCCCCCCCC C C C CDokument20 SeitenC CCCCCCCCCCCC C C C CZandra Kiamco MillezaNoch keine Bewertungen
- Catalogo Ancla GiiDokument2 SeitenCatalogo Ancla GiiLUCIA SOLISNoch keine Bewertungen
- Chandka Medical CollegeDokument120 SeitenChandka Medical CollegeMuhammadObaidullahNoch keine Bewertungen
- Management of Liver Trauma in Adults: Nasim Ahmed, Jerome J VernickDokument7 SeitenManagement of Liver Trauma in Adults: Nasim Ahmed, Jerome J VernickwiraNoch keine Bewertungen