Beruflich Dokumente
Kultur Dokumente
Sevoflurano
Hochgeladen von
Tlao Rodriguez CruzCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Sevoflurano
Hochgeladen von
Tlao Rodriguez CruzCopyright:
Verfügbare Formate
Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
www.ijppp.org /ISSN:1944-8171/IJPPP0018273
Original Article
Sevoflurane enhances neuromuscular blockade by
increasing the sensitivity of skeletal muscle
to neuromuscular blockers
Ling Ye1, Yunxia Zuo2, Peng Zhang2, Pingliang Yang3
Departments of 1Pain Management, 2Anesthesiology, West China Hospital, Sichuan University, Chengdu, Sichuan
610041, P. R. China; 3Department of Anesthesiology, West China Second University Hospital, Sichuan University,
Chengdu, Sichuan 610041, P. R. China
Received October 21, 2015; Accepted December 15, 2015; Epub December 25, 2015; Published December 30,
2015
Abstract: The aim of this study was to investigate the effects of sevoflurane on skeletal muscle contractility. In the
first part, twenty-two American Society of Anesthesiology (ASA I-II) female adult patients undergoing elective hyster-
ectomy surgery inhaled sevoflurane 1.0, 1.5 and 2.0 minimum alveolar concentrations (MAC) in succession. Neu-
romuscular function was assessed at each dose. In the second part, forty-four ASA I-II female adult patients were
randomized into four groups: group 1 (propofol + atracurium, sevoflurane 0 MAC), and groups 2 to 4 (atracurium
+ sevoflurane 1.0, 1.5 and 2.0 MAC, respectively). In group 1, patients were anesthetized by propofol. Then 0.01
mg/kg atracurium was injected into the tested arm intravenously after the arterial blood flow was blocked using a
tourniquet. For the other 3 groups, patients inhaled 1.0 MAC, 1.5 MAC, or 2.0 MAC of sevoflurane. Then 0.01 mg/
kg atracurium was injected. Neuromuscular function was recorded for the 4 groups. Neuromuscular function was
assessed by acceleromyography measurement of evoked responses to train-of four (TOF) stimuli (2 Hz for 2 s ap-
plied every 12 s) at the adductor pollicis using a TOF-GuardTM neuromuscular transmission monitor. Amplitudes of
first response (T1) in each TOF sequence and the ratios of fourth TOF response (T4) to the first were similar at 1.0
MAC, 1.5 MAC, and 2.0 MAC sevoflurane. Compared to baseline, there was no significant change in the TOF value
after inhaling 1.0 MAC, 1.5 MAC, or 2.0 MAC sevoflurane. Compared to group 1, there was no significant difference
in atracurium onset time (time to reach TOF ratio = 0.25) in group 2 ( 5.6 1.8 min vs. 6.5 1.7 min, P>0.05), or
degree of adductor pollicis block (subject number with TOF ratio = 0, 5 vs. 2 subjects, p = 0.3). However, inhaling
1.5 or 2.0 MAC sevoflurane decreased atracurium onset time (4.6 1.5 min and 4.0 1.3 min vs. 6.5 1.7 min,
P<0.01 and P<0.001, respectively), and enhanced the block degree (9 and 10 vs. 2 subjects, P<0.001) compared
with group 1. Sevoflurane has no direct effects on the adductor pollicis contractility, but increased the skeletal
muscle sensitivity to atracurium.
Keywords: Sevoflurane, neuromuscular block, inhaled anesthesia, atracurium, propofol
Introduction thetics [4-6]. Enhancing the action of non-depo-
larizing neuromuscular blocking drugs decreas-
Inhaled anesthetics can induce a variety of es the need for muscle relaxants [7-11].
reversible, clinically important effects including However, the specific sites of action of inhaled
amnesia, hypnosis, immobility (response to anesthetics such as sevoflurane on neuromus-
noxious stimuli) and muscle relaxation. Potent cular blocking are not clear, although some
inhaled anesthetics increase the neuromuscu- believe the spinal cord maybe one of the sites
lar blockade produced by non-depolarizing of action [12-16]. But whether sevoflurane has
drugs in a dose-dependent fashion [1-3] as a direct effect on skeletal muscle contractility is
demonstrated by previous studies showing that unknown. In this study, we aimed to examine
effects of neuromuscular blockade on train-of the effects of sevoflurane on skeletal muscle
four (TOF) values are amplified by inhaled anes- contractility by selectively delivering neuromus-
Sevoflurane enhances neuromuscular blockade
cular blocking drugs to the skeletal muscle Part 2: Administration of sevoflurane or propo-
without affecting in the central nervous fol with neuromuscular blocker
system.
Forty-four patients were randomly assigned
Materials and methods into four groups with 11 subjects each: group
1: propofol + atracurium (sevoflurane 0 MAC);
Patients groups 2 to 4: atracurium + sevoflurane 1.0
MAC, 1.5 MAC and 2.0 MAC, respectively. In
This study was approved by the Institutional group 1, general anesthesia was induced by
Research Ethics Committee of West China bolus injection of propofol 2-3 mgkg-1 and fol-
Second University Hospital, Sichuan University, lowed by continuous intravenous propofol 8-10
China, and written informed consent was mgkg-1h-1 during the anesthesia period as
obtained from each patient preoperatively. A measured in the non-tested arm. After loss of
total of sixty-six un-premedicated female adult consciousness and stabilization of the concen-
patients, America Society of Anesthesiology tration, 0.01 mg/kg atracurium (in normal
(ASA) status I and II scheduled for elective saline diluted to 10 ml) was injected to the test-
gynecological surgery were enrolled in the ed arm intravenously after the arterial blood
study. Body weight was within 20% of the nor- flow was blocked by tourniquet (i.e., the same
mal value for the height, and the age range was procedure as is used for intravenous regional
18-65 years. Exclusion criteria included liver or anesthesia (IVRA)), and then the neuromuscu-
renal insufficiency, abnormal plasma electro- lar function was tested.
lytes, obesity, peripheral vessel or neuromus-
cular disease, allergy to atracurium or propofol, In groups 2-4, patients inhaled 1.0 MAC, 1.5
and concomitant medication known to interfere MAC, or 2.0 MAC sevoflurane, respectively for 5
with neuromuscular transmission. min. After loss of consciousness and stabiliza-
tion of the concentration, the arterial blood flow
Upon arrival in the operating room, standard in the tested arms was blocked using a tourni-
monitoring including electrocardiograph, pulse quet and 0.01 mg/kg atracurium (in normal
oximeter, capnograph and noninvasive blood saline diluted to 10 ml) was injected to the
pressure was applied to the patients. Prior to same arm intravenously, and then the neuro-
anesthesia, patients were administered mid- muscular function was recorded.
azolam (<0.05 mg.kg) intravenously followed by
oxygen at 6 liters min-1 via a mask for 3 min- In all the groups, loss of consciousness was
utes. All the tests were done by one skillful defined as loss of the eyelash reflex and lack of
attending anesthesiologist before the surgery. response to verbal stimulation. If undesirable
respiratory depression occurred, a laryngeal
Part 1: Administration of sevoflurane alone mask airway was applied to maintain the par-
under varying concentrations tial pressure of end-tidal carbon dioxide
between 35-40 mmHg. Time for tourniquet was
Twenty-two patients were enrolled in this part less than 30 minutes.
of study. The recirculating system of the anes-
thesia machine was primed for 30 s with sevo- Measurement of neuromuscular blockade
flurane in oxygen 6 liters min-1. The face mask
was fitted and the patients were asked to take Neuromuscular function was assessed by the
deep breaths. End-tidal sevoflurane concentra- acceleromyography measurement of evoked
tion was monitored continuously with an anes- responses to train-of four (TOF) stimuli (2 Hz for
thetic gas monitor (Spacelabs Medical, 2 s applied every 12 s) at the adductor pollicis
Issaquah, WA, USA). Each patient was exam- using a TOF-GuardTM neuromuscular transmis-
ined during three different experimental states. sion monitor (Organon Technica, Biometer,
Neuromuscular function was measured at Turnhout, Belgium) according to the recommen-
sevoflurane concentrations of 1.0 MAC, 1.5 dations of Vibymogensen et al. [17]. We record-
MAC and 2.0 MAC with O2. The lowest concen- ed the amplitude of the first response (T1) in
tration was administered first, and highest was each TOF sequence, and calculated the ratio of
administered last. the amplitude of forth TOF response in each
173 Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
Sevoflurane enhances neuromuscular blockade
Table 1. Demographic data for the patients in the study
Part 2 (n = 44)
Characteristics Part 1 (n = 22)
Group 1 (n = 11) Group 2 (n = 11) Group 3 (n = 11) Group 4 (n = 11)
Age (years) 45.8 13.2 44.2 13.6 39.3 14.5 46.9 12.7 47.9 10.8
Height (cm) 158.5 9.0 152.6 7.8 156.3 9.8 158.4 8.0 160.1 7.6
Weight (kg) 56.8 7.2 54.5 6.7 54.6 8.0 60.1 7.8 58.4 7.0
Blood Pressure (mmHg) 113.3 9.1 114.4 7.8 112.9 10.7 112.1 8.7 111.1 9.0
Values are expressed as mean SD. No significant among-group differences (P>0.05). Part 1: Sevoflurane group. Group 1: Pro-
pofol + atracurium group. Group 2: Sevoflurane 1.0 MAC + atracurium group. Group 3: Sevoflurane 1.5 MAC + atracurium group.
Group 4: Sevoflurane 2.0 MAC + atracurium group.
Figure 1. Diagram of the study. First part: 22 subjects were treated in a successive manner was to investigate
whether sevoflurane has direct effects on the adductor pollicis contractility. Second part: 44 subjects were decided
into 4 groups equally to investigate whether sevoflurane would increase the skeletal muscle sensitivity to atracu-
rium, and which concentration of sevoflurane would the effect the sensitivity.
Table 2. Neuromuscular responses during were performed by the attending anesthesi-
sevoflurane anesthesia (n = 22) ologist.
Sevoflurane con- T1 amplitude All measurements were performed 15-20 min
TOF ratio (%)
centration (MAC) (% of control)
after obtaining a stable level of each end-tidal
0 (baseline) 100 100 sevoflurane concentration in 100% O2. All mea-
1.0 103 35 100 2 surements were recorded in duplicate for each
1.5 109 29 96 7 patient.
2.0 106 27 96 8
Mean SD. No significant among-group differences Statistics
(P>0.05).
Data was analyzed with SPSS Version 13.0
(SPSS Inc., Chicago, IL). For part 1, values of
train to that of the first (TOF ratio). A baseline each neuromuscular variable at different con-
was established during the calibration centrations of sevoflurane were compared by
sequence prior to the administration of either repeated measures analysis of variance
the initial atracurium bolus or the volatile anes- (ANOVA). For part 2, demographic data and
thetic agent. Two peripheral nerve stimulators results obtained for each subject in the experi-
which were used for stimulation of the ulnar ment were compared by ANOVA. Differences in
nerves via cutaneous electrodes were applied maximum blockade (number with TOF = 0)
at the wrists. The device was calibrated before between group 1 and groups 2-4 were com-
administration of atracurium. All procedures pared by Fishers exact test. All tests were two-
174 Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
Sevoflurane enhances neuromuscular blockade
ods of the study and the
equilalent experimental data
obtained during the final peri-
od of neuromuscular function
testing. Compared to base-
line, there was no significant
difference in TOF value after
inhalation of 1.0 MAC, 1.5
MAC, or 2.0 MAC sevoflurane
(Table 2).
Sevoflurane or propofol with
atracuriumin
Figure 2. Effects of sevoflurane on atracurium onset time (time to reach TOF
ratio = 0.25). Values are expressed as mean SD. Compared with group 1 (0 Compared group 1 and group
MAC), there was no significant difference in atracurium onset time in group 2, there was no significant dif-
2 (1.0 MAC) (P>0.05). Compared with group 1, group 3 (1.5 MAC) and group ference in atracurium onset
4 (2.0 MAC) did decrease the atracurium onset time (P<0.01 and P<0.001, time (time to reach TOF ratio =
respectively). 0.25; 6.5 1.7 min vs. 5.6
1.8 min, p>0.05) (Figure 2).
Though the degree of adduc-
tor pollicis block was higher in
group 2 at 1.0 MAC servoflu-
roane but it did not reach sig-
nificance (TOF ratio = 0, 2 vs.
5 subjects, P = 0.36) (Figure
3). Compared group 3 or 4
with group 1, inhaling 1.5 or
2.0 MAC sevoflurane did
decrease the atracurium
onset time (4.6 1.5 min and
4.0 1.3 min vs. 6.5 1.7
min, P<0.01 and P<0.001,
Figure 3. Effects of sevoflurane on atracurium block degree. Numbers of sub- respectively; Figure 2) and
jects (of 11 per group) with TOF ratio of 0. Compared with group 1 (0 MAC), significantly enhanced the
there was no significant difference significance in group 2 (1.0 MAC) (2 vs. 5 degree of adductor pollicis
subjects, P =0.36). Compared with group 1 (0 MACA), group 3 (1.5 MAC) or 4
(2.0 MAC) significantly enhanced the degree of adductor pollicis block (9 and
block (Figure 3, TOF ratio = 0,
10 vs. 2 subjects, P<0.001). 9 and 10 vs. 2 subjects,
P<0.001).
sided, with p<0.05 considered significant. Discussion
Levels of significance are indicated by the num-
ber of symbols, e.g., *P = .01 to <.05; **P = .001 Sevoflurane alone had no significant direct
to .01; ***P<.001. Data are presented as effect on muscle relaxation, however, sevoflu-
average SD. rane, but not propofol, increased the sensitivity
to muscle relaxant atracurium.
Results
In this study, a procedure as IVRA was obtained
All groups did not differ significantly with regard by local injection to avoid exposure of spinal
to age, height or weight and blood pressure cord or supraspinal cord to neuromuscular
(Table 1). Figure 1 showed the diagram of the blockers, and the administered drugs will selec-
whole study and the purpose of the two parts. tively target skeletal muscle only in the affected
Sevoflurane alone under varying concentra- region. When a drug is given systematically, it is
tions difficult to determine whether the effect is gen-
erated by acting on the muscle, spinal cord, or
Values for T1 and TOF ratio were similar at 1.0, brain. Yang et al. devised a technique to admin-
1.5, and 2.0 MAC sevoflurane. No significant ister anesthetics only into the spinal cord in
differences were found between the initial peri- experimental animals, and showed that the spi-
175 Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
Sevoflurane enhances neuromuscular blockade
nal cord was an important site of anesthetic Conclusions
action [18]. We were interested in determining
possible anesthetic effects in skeletal muscle. In conclusion, we used a regional anesthesia
So we administered the neuromuscular block method to develop a model to preferentially
drugs locally, to affect only the tested skeletal deliver neuromuscular blocking drugs to the
muscles, using IVRA. In 1908 Bier described skeletal muscle. Using this model, we con-
the use of tourniquets and injected agents to firmed that sevoflurane has no direct effects on
induce localized anesthesia [19, 20]. We used the adductor pollicis contractility, but can
this principle to allow preferential delivery of increase the skeletal muscle sensitivity to neu-
neuromuscular blocking drug to the skeletal romuscular blocker.
muscle by injecting the drug into the upper test
arm blood vessel. This method allowed us to Disclosure of conflict of interest
study the effects of sevoflurane on muscle
relaxation without the interference of the cen- None.
tral nervous system clearly demonstrate the Address correspondence to: Dr. Pingliang Yang,
direct effects of sevoflurane at the level of the Department of Anesthesiology, West China Second
skeletal muscle. This method may contribute to University Hospital, Sichuan University, Chengdu,
a better understanding of their neuromuscular Sichuan 610041, P. R. China. Tel: 86-28-85422997;
mechanisms of action. Fax: 86-28-85422997; E-mail: pingliangyang@163.
com
Our findings using atracurium in are consistent
with previous studies showing that sevoflurane
References
did not significantly affect the magnitude and
recovery time of another nondepolarizing block- [1] Eger II E, Eisenkraft J and Weiskopf R. Neuro-
er, rocuronium [21]. In that study, isoflurane muscular effects of inhaled anesthetics. In:
and sevoflurane both augmented the intensity Eger II E, ed. The Pharmacology of Inhaled An-
of rocuronium-induced NMB to a similar extent esthetics. Sponsored by the Danmiller Memo-
rial Educational Foundation, Educational Grant
Previous studies [21, 22] demonstrated the from Baxter Healthcare Corporation; 2003. p.
lack of potentiation of neuromuscular blockade 133-145.
when NMBs were combined with propofol, simi- [2] Kelly RE, Lien CA, Savarese JJ, Belmont MR,
lar to what we have found in this study. The pro- Hartman GS, Russo JR and Hollmann C. De-
pofol group showed no increased sensitivity to pression of neuromuscular function in a pa-
atracurium. Beaussier et al. showed sevoflu- tient during desflurane anesthesia. Anesth
rane at 1 MAC decreases accelerometric Analg 1993; 76: 868-871.
responses of the adductor pollicis to atracuri- [3] Miller RD, Way WL, Dolan WM, Stevens WC and
um [23]. The findings were supported by an ani- Eger EI. The dependence of pancuronium and
mal study in which they showed that 1.0 MAC d-tubocurarine induced neuromuscular block-
sevoflurane did not alter responses to periph- ades on alveolar concentrations of halothane
and forane. Anesthesiology 1972; 37: 573-81.
eral nerve stimulation [24]. Our study confirmed
[4] Fogdall RP and Miller RD. Neuromuscular ef-
that inhaled anesthetics can provide a dose-
fects of enflurane, alone and combined with
related muscle relaxation as reported in the
d-Tubocurarine, pancuronium and succinylcho-
previous studies [1-3] and also showed sevoflu- line, in man. Anesthesiology 1975; 42: 173-8.
rane increased sensitivity to muscle relaxants [5] Cannon JE, Fahey MR, Castagnoli KP, Furuta T,
but no direct muscle relaxation. Canfell PC, Sharma M and Miller RD. Continu-
ous infusion of vecuronium: the effect of anes-
Further studies are necessary to determine the thetic agents. Anesthesiology 1987; 67: 503-
mechanisms underlying the enhancement of 6.
the sensitivity of skeletal muscles to neuro- [6] Caldwell JE, Laster MJ, Magorian T, Heier T, Ya-
muscular blockers, and to assess the effects of suda N, Lynam DP, Eger EI and Weiskopf RB.
inhaled anesthetics on neuromuscular block- The neuromuscular effects of desflurane,
age in male patients. In addition, it would also alone and combined with pancuronium or suc-
be interesting to test using different neuromus- cinylcholine in humans. Anesthesiology 1991;
cular blockers. 74: 412-8.
176 Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
Sevoflurane enhances neuromuscular blockade
[7] Morita T, Tsukagoshi H, Sugaya T, Yoshhikawa [16] Yang J, Chai YF, Gong CY, Li GH, Luo N, Luo NF
D and Fujita T. The effects of sevoflurane are and Liu J. Further proof that the spinal cord,
similar to those of isoflurane on the neuromus- and not the brain, mediates the immobility pro-
cular block produced by vecuronium. Br J An- duced by inhaled anesthetics. Anesthesiology
aesth 1994; 72: 465-7. 2009; 110: 591-5.
[8] Wulf H, Ledowski T, Linstedt U, Proppe D and [17] Viby-Mogensen J, Engbaek J, Eriksson LI,
Sitzlack D. Neuromuscular blocking effects of Gramstad L, Jensen E, Jensen FS, Koscielniak-
rocuronium during desflurane, isoflurane, and Nielsen Z, Skovgaard LT and Ostergaard D.
sevoflurane anaesthesia. Can J Anaesth 1998; Good clinical research practice (GCRP) in phar-
45: 526-32. macodynamic studies of neuromuscular block-
[9] Kastrup MR, Marsico FF, Ascoli FO, Becker T, ing agents. Acta Anaesthesiol Scand 1996;
Soares JH and Gomez de Segura IA. Neuro- 40: 59-74.
muscular blocking properties of atracurium [18] Yang J, Li Z, Gong CY, Chai YF, Li T, Li GH, Luo N,
during sevoflurane or propofol anaesthesia in Luo NF, Zhu L and Liu J. A model for the prefer-
dogs. Vet Anaesth Analg 2005; 32: 222-7. ential delivery of isoflurane to the spinal cord
[10] Caldwell JE, Laster MJ, Magorian T, Heier T, Ya- of the goat. Vet J 2011; 187: 239-44.
suda N, Lynam DP, Eger EI and Weiskopf RB. [19] Holmes CM. The history and development of
The neuromuscular effects of desflurane, intravenous regional anaesthesia. Acta Anaes-
alone and combined with pancuronium or suc- thesiol Scand Suppl 1969; 36: 11-8.
cinylcholine in humans. Anesthesiology 1991; [20] Brown EM, McGriff JT and Malinowski RW. In-
74: 412-8. travenous regional anaesthesia (Bier block):
[11] Miller RD, Eger EI II, Way WL, Stevens WC and review of 20 years experience. Can J Anesth
Dolan WM. Comparative neuromuscular ef- 1989; 36: 307-10.
fects of forane and halothane alone in combi- [21] Wulf H, Ledowski T, Linstedt U, Proppe D and
nation with d-tubocurarine in man. Anesthesi- Sitzlack D. Neuromuscular blocking effects of
ology 1971; 35: 38-42. rocuronium during desflurane, isoflurane, and
[12] Pron Y, Bernard JM, Nguyen The Tich S, Gen- sevoflurane anaesthesia. Can J Anaesth 1998;
et R, Petitfaux F and Guihneuc P. The effects 45: 526-32.
of desflurane on the nervous system: from spi- [22] McCarthy GJ, Mirakhur RK and Pandit SK.
nal cord to muscles. Anesth Analg 1999; 89: Lack of interaction between propofol and ve-
490-5. curonium. Anesth Analg 1992;75: 536-8.
[13] Hicks RG, Woodforth IJ, Crawford MR, Stephen [23] Beaussier M, Boughaba A, Schiffer E, Debaene
JP and Burke DJ. Some effects of isoflurane on B, Lienhart A and dHollander A. Acute desflu-
I waves of the motor evoked potential. Br J An- rane or sevoflurane exposure on a previously
aesth 1992; 69: 130-6. stabilized atracurium-induced neuromuscular
[14] Rampil IJ, Mason P and Singh H. Anesthetic block. Eur J Anaesthesiol 2006; 23: 755-9.
potency (MAC) is independent of forebrain [24] Kastrup MR, Marsico FF, Ascoli FO, Becker T,
structures in the rat. Anesthesiology 1993; 78: Soares JH and Gomez de Segura IA. Neuro-
707-12. muscular blocking properties of atracurium
[15] Antognini JF and Schwartz K. Exaggerated an- during sevoflurane or propofol anaesthesia in
esthetic requirements in the preferentially dogs. Vet Anaesth Analg 2005; 32: 222-7.
anesthetized brain. Anesthesiology 1993; 79:
1244-9.
177 Int J Physiol Pathophysiol Pharmacol 2015;7(4):172-177
Das könnte Ihnen auch gefallen
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- ObamaDeception SupplementalBookletDokument34 SeitenObamaDeception SupplementalBookletAccurateHistorian100% (4)
- Ansi+asse+z359 13-2013Dokument54 SeitenAnsi+asse+z359 13-2013Oscar Casso100% (1)
- MyLabX5 160000160 V04 LRDokument5 SeitenMyLabX5 160000160 V04 LRVishnu0049Noch keine Bewertungen
- Summary of Non Sexist CityDokument2 SeitenSummary of Non Sexist CityIMY KARDAS100% (3)
- Referat Limba Engleză-Zidaroiu Ionuț-EduardDokument6 SeitenReferat Limba Engleză-Zidaroiu Ionuț-EduardEduard IonutNoch keine Bewertungen
- Union Carbide Corporation and Others v. Union of India and OthersDokument73 SeitenUnion Carbide Corporation and Others v. Union of India and OthersUrviNoch keine Bewertungen
- Drug Study (FINAL)Dokument31 SeitenDrug Study (FINAL)iamjenivicNoch keine Bewertungen
- Uses of Isotopes in Our Daily LivesDokument3 SeitenUses of Isotopes in Our Daily LivesVibhor Mathur70% (10)
- THE Center: Anxiety DisordersDokument13 SeitenTHE Center: Anxiety DisordersOti VuraNoch keine Bewertungen
- Post-Exercise Recovery Strategies in Basketball: Practical Applications Based On Scientific EvidenceDokument17 SeitenPost-Exercise Recovery Strategies in Basketball: Practical Applications Based On Scientific EvidenceMari PaoNoch keine Bewertungen
- Jumpstart: Name: Angel E. PicazoDokument2 SeitenJumpstart: Name: Angel E. PicazoAngel PicazoNoch keine Bewertungen
- Nordic Business Forum 2023 ExecutiveSummaryDokument71 SeitenNordic Business Forum 2023 ExecutiveSummaryveda.norwayNoch keine Bewertungen
- BP HSE Action PLanDokument6 SeitenBP HSE Action PLanbesongNoch keine Bewertungen
- Lung Contusion & Traumatic AsphyxiaDokument17 SeitenLung Contusion & Traumatic AsphyxiaLady KeshiaNoch keine Bewertungen
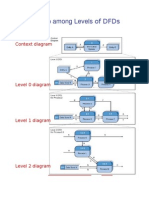
- Relationship Among Levels of DFDsDokument8 SeitenRelationship Among Levels of DFDssunny_242574Noch keine Bewertungen
- Poverty Is General Scarcity or The State of One Who Lacks A Certain Amount of Material Possessions or MoneyDokument41 SeitenPoverty Is General Scarcity or The State of One Who Lacks A Certain Amount of Material Possessions or MoneyChristian Cañon GenterolaNoch keine Bewertungen
- Mini Project Report On Heart Disease PreDokument23 SeitenMini Project Report On Heart Disease PregayuNoch keine Bewertungen
- DNAlysis MygeneRx Sample ReportDokument13 SeitenDNAlysis MygeneRx Sample ReportTrustNoch keine Bewertungen
- A. Differential Diagnosis:: Bone MetastasisDokument3 SeitenA. Differential Diagnosis:: Bone MetastasisDonna DumaliangNoch keine Bewertungen
- Slu Brochure Ay 2014-2015Dokument2 SeitenSlu Brochure Ay 2014-2015Michael BermudoNoch keine Bewertungen
- Health & Illness FinalDokument16 SeitenHealth & Illness FinalAJNoch keine Bewertungen
- SavedrecsDokument1.440 SeitenSavedrecsAshish AhirwalNoch keine Bewertungen
- MMG 301 Study Guide For Exam 1Dokument14 SeitenMMG 301 Study Guide For Exam 1Juyeon CheongNoch keine Bewertungen
- Tranexamic Acid MouthwashDokument1 SeiteTranexamic Acid MouthwashTalal MazharNoch keine Bewertungen
- CertificateDokument1 SeiteCertificateriteshNoch keine Bewertungen
- Filipino Research Paper Kabanata 4Dokument8 SeitenFilipino Research Paper Kabanata 4nynodok1pup3100% (1)
- Clase 1-Fisiopatología de La Artritis ReumatoideaDokument45 SeitenClase 1-Fisiopatología de La Artritis ReumatoideaPercy Williams Mendoza EscobarNoch keine Bewertungen
- Achristian,+JAFSCD COVID Commentary Disruptions Malaysia August 2020Dokument3 SeitenAchristian,+JAFSCD COVID Commentary Disruptions Malaysia August 2020Siew LeongNoch keine Bewertungen
- REPORTDokument1 SeiteREPORTFoamy Cloth BlueNoch keine Bewertungen
- Personal Finance Canadian 2nd Edition Madura Test BankDokument48 SeitenPersonal Finance Canadian 2nd Edition Madura Test Bankannabellaauroravb5cf100% (22)