Beruflich Dokumente
Kultur Dokumente
Cellulitis & Skin Infections
Hochgeladen von
PutriIffahCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Cellulitis & Skin Infections
Hochgeladen von
PutriIffahCopyright:
Verfügbare Formate
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
Skin Infections Antibiotic Choice
Assessment Education
Investigations Recurrent Infections
Cellulitis Management Referral to Community Nursing
Abscess Management References
Infection Control
Skin Infections
Cellulitis is a diffuse inflammation of the soft tissue or connective tissue due to infection. The most
common causes are Staphylococcus aureus and Streptococcus pyogenes (Group A beta-
haemolytic strep). Any break in the skin may lead to infection e.g. insect bites, abrasions,
lacerations, burns and eczema, however the skin often appears intact.
A child with cellulitis will have a red, warm and tender area of skin often with swelling. There may
be signs of local spread: proximal red streaking, regional lymph node involvement, abscess
formation, or systemic symptoms: fever, malaise, chills and sweats.
Abscess an abscess is a cavity containing pus with or without surrounding cellulitis.
Allergic skin reactions may be confused with cellulitis but are usually itchy and non tender.
Impetigo (school sores) is a highly contagious superficial skin infection caused by S.aureus or
S.pyogenes (or both). It is associated with crusting and weeping.
Bullous impetigo is usually caused by a toxin produced by S.aureus. It begins as vesicles which
rapidly enlarge to form flaccid bullae.
Furunculosis (boils) involves infection that is centred on a hair follicle. It may be superficial with
single or multiple red papules or pustules or deeper with abscess formation. It is usually caused by
S.aureus and is associated with excessive sweating, friction or occlusion of hair follicles.
Erysipelas is a distinct infection of skin, subcutaneous tissues & lymphatics, usually caused by
S.pyogenes It is associated with abrupt onset of systemic upset. The skin lesion is a fiery red, hot,
tender indurated plaque that spreads rapidly with a well demarcated raised border. Commonly
occurs on the face or extremities.
Necrotising fasciitis is a life-threatening infection of fascia & sub-cutaneous tissues. It may
initially be mistaken for cellulitis but is associated with disproportionate pain & tenderness, rapidly
advancing soft tissue involvement & signs of sepsis. Necrotising fasciitis is a medical and surgical
emergency that requires prompt surgical exploration & debridement, PICU involvement & broad
spectrum IV antibiotics.
Periorbital cellulitis is swelling and erythema in the soft tissues around the eye. See Eye Infection
guideline
Orbital cellulitis these patients have clinical evidence of exophthalmos, pain on eye movement,
or limitation of eye movement OR radiographic evidence of subperiosteal or orbital abscess.
Urgent ophthalmology review is mandatory for these patients and urgent imaging may be required
See Eye Infection guideline
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 1 of 6
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
Assessment
Remember to ask about:
Systemic upset
Underlying skin disorders (e.g. eczema)
Insect bites
Recent chicken pox infection (in the month prior)
Significant water exposure (e.g. traumatic lesion / cut sustained while in a pond, stream)
Immunisations (H.influenzae is an important causative organism in unimmunised children)
Personal or family history of previous skin sepsis (remember MRSA)
Overseas travel
Past history and family history of cellulitis and other skin sepsis.
Swabs done in the community
Antibiotics & dose given (if any) in the community
Perinatal risks (group B streptococcus may be a causative organism in neonates).
Examine for: signs of sepsis, insect bites, wounds, lymphadenopathy, abscess formation (fluctuant
swelling or overt discharge of pus). Marking the extent of the erythema is useful to assess clinical
progress.
For infections around the eye see Eye Infections guideline
Abscess - If the child has a fluctuant lump, the child is to be referred to the surgical team for
consultation/ incision and drainage.
Investigations
Wound/Pus Swabs: only if pus is present or the skin is broken. A swab for AFB (acid fast bacilli)
should be taken where nontuberculous mycobacteria is suspected.
Blood Culture & FBC: if child has significant systemic upset or an unusual cause of infection is
suspected.
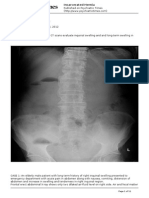
Radiology: X-rays are NOT routine for limb cellulitis and should only be requested if there is:
1. A possible radio-opaque foreign body or,
2. A history of trauma (to exclude an underlying fracture) or,
3. Suspicion of osteomylelitis (including at least 7 days of symptoms)
Ultrasonography: to exclude a non-radio-opaque foreign body (such as wood), or if there is
uncertainty about a drainable collection
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 2 of 6
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
Cellulitis Management
A well child with early & mild cellulitis should be trialed on oral antibiotics with medical review within
24-48 hours by the GP. Treat uncomplicated cellulitis for 5 days. If the child had been on oral
antibiotics prior to presentation consider a trial of a different antibiotic if the child is stable and there
was intolerance or an inappropriate antibiotic used in the first instance. It is also worth checking the
dose of the antibiotic prescribed to see that it was adequate. For infections in or around the eye
please refer to the Eye Infection guideline
Admit ALL children who:
are systemically unwell
neonates
have not responded to appropriate oral antibiotics within 48hrs
have families unable to cope with the illness at home
require IV antibiotic therapy
Admit MOST children who:
have another serious systemic illness (e.g. diabetes)
have facial cellulitis / abscess
are young infants
Managing Teams
Cellulitis +/- abscess of the limbs - orthopedics
Cellulitis of the trunk, head & neck without abscess general paediatrics
Abscess +/- cellulitis of trunk, head or neck surgical or ENT
Other Considerations for Admission
There are certain issues that will influence the decision made whether to discharge or admit a
child. These may not reflect the state of illness but some of the following should be considered:
Social e.g. issues of compliance, coping skills, anxiety etc.
Transport and phone access.
Lack of community services in areas, for example no district nurses.
Discharge on oral antibiotics once systemically well and cellulitis improving.
If the child has had previous skin infections or has been swabbed by their GP look up the swab
results in case of previous MRSA.
Analgesia - Cellulitis is painful. Ensure adequate analgesia. Paracetamol is first line. Avoid
NSAIDs in suspected post-varicella infection & necrotising fasciitis (associated with increased risk
of severe soft tissue infections possibly due to impaired neutrophil function).
All inpatients with cellulitis should be examined at least daily to check for abscess development. If
fluctuance develops referral should be made to the appropriate surgical team (depending on the
location of the infection).
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 3 of 6
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
Abscess Management
Abscesses require incision & drainage if fluctuant. If minimal or no cellulitis is associated with the
abscess and the child is systemically well antibiotic treatment is not necessary. If induration is
present without fluctuance then consider discharge with oral antibiotics and GP follow up. Advise
caregivers that it may still need I&D. I&D may be performed in the Childrens Emergency
Department with appropriate analgesia & sedation in selected cases consult with senior.
Infection Control
The mode of transmission is through direct contact with a person who has a purulent lesion.
Hands are the main vehicle for transmitting infection. Washing and drying your hands is the most
important means of preventing the spread of infection.
Methicillin Resistant Staph Aureus (M.R.S.A.)
If a patient is found to be positive for MRSA from a wound swab, or is known to be MRSA positive
from previous swabs, they should be placed into contact isolation.
Antibiotic Choice
Topical antibiotics
Only useful for uncomplicated localized impetigo ( 3 lesions).
Clean off crusts and apply fusidic acid cream tds to lesions.
Oral antibiotics:
Cephalexin good Staphylococcal & Streptococcal cover, palatable suspension, well tolerated,
funded. Dose 20 mg/kg/dose bd. Max 500 mg/dose.
Flucloxacillin if able to take capsules (suspension unpalatable). Very effective against S.aureus &
has adequate cover for S.pyogenes. Dose 10-25 mg/kg/dose tds (max 500 mg/dose)
Intravenous Antibiotics:
Flucloxacillin - Dose 25-50 mg/kg/dose q6hrly. Max 2g per dose.
For MRSA:
Known or suspected MRSA. (NB: previous MRSA does not necessarily mean this infection is due
to MRSA)
Oral
Co-trimoxazole - Palatable suspension or tablets. Dose 1.5-3 mg/kg/dose bd (trimethoprim
component). Max 80-160 mg/dose.
IV
Antibiotic choices below require approval from the Infectious Diseases tem)
Clindamycin Dose 10 mg/kg/dose q6-8 hourly. Max 600 mg per dose.
Vancomycin Dose 15 mg/kg/dose q6 hourly. Max dose 500mg q6h
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 4 of 6
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
For penicillin allergy:
Oral:
Erthyromycin Dose 10 mg/kg/dose qds or 20 mg/kg bd. Max 500 mg/dose.
Roxithromycin Alternative if able to swallow tablets. Dose 4 mg/kg/dose. Twice daily.
Max 150 mg/dose.
Intravenous:
Clindamycin Dose 10 mg/kg/dose q6-8 hourly. Max 600mg/dose.
For animal or human bites:
Amoxycillin & Clavulanic acid
Oral: 15-25 mg/kg/dose tds (amoxycillin component). Max oral dose 500mg/dose.
IV: 25-50 mg/kg/dose. q8h Max IV dose 1g/dose.
Education
Parents should be reminded to;
avoid sharing towels and bedding at home,
wash linen and clothing regularly,
maintain childrens short / clean fingernails to avoid skin breaks from scratching,
examine their childs skin and clean breaks in the skin,
see their GP early if redness develops,
encourage all family members to wash and dry hands properly,
avoid sharing bath, swimming, and cleaning water when the child has an infected wound,
restrict their child from swimming in unclean water when they have an open wound.
Recurrent cellulitis/abscess
Various strategies can be tried to reduce bacterial skin colonisation but requires motivation from
the family. Prevention of infected eczema is best done by proactive management of the eczema
rather than repeated antibiotics alone. The infectious disease team is happy to see these patients
as out-patients. The typical waiting time is a few weeks. If no cultures are available please swab
any lesions plus the nose & groin for bacterial culture.
For children/families who have multiple episodes of skin infection:
Reinforce personal hygiene measures
Encourage early presentation to the GP
Household members are frequently also infected with Staph it is appropriate to ask about
skin infections and examine family members (even adults) to ensure they also receive
treatment.
Some families may find adding Janola to bathwater useful for reducing the bacterial load on
the skin. 5ml Janola per 5L of water twice a week. This is approximately 100ml for a 15cm
deep full sized bath. Babys baths use a capful. Alternatives include antiseptic bath oils (oilatum
plus, QV flare up). If there is no bath then Chlorhexidine washes or even Protex soap (these
two not recommended in eczema).
Family to consider discussion with GP regarding other possible decontamination strategies
(may include short/medium term antibiotics or intranasal mupirocin).
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 5 of 6
Starship Childrens Health Clinical Guideline
Note: The electronic version of this guideline is the version currently in use. Any printed version can
not be assumed to be current. Please remember to read our disclaimer.
CELLULITIS / SKIN INFECTIONS
Referral to Community Nursing
Some children may benefit from follow-up by Paediatric Homecare nurses or Public Health Nurses.
Consdier this if:
Wound has a copious high exudate.
There is a drain in situ.
Dressings are required.
The child has multiple skin infections,
There is a potential for cellulitis to develop into an abscess,
References
Author: Dr Alison Leversha, Dr Kate Anson Service: Community Paediatrics, CED
Editor: Dr Raewyn Gavin Date Reviewed: March 2012
Cellulitis Page: 6 of 6
Das könnte Ihnen auch gefallen
- Pathophysiology AppendicitisDokument3 SeitenPathophysiology AppendicitisIra Krystel ReyesNoch keine Bewertungen
- Drug StudyDokument5 SeitenDrug StudyJanine Erika Julom BrillantesNoch keine Bewertungen
- Pa Tho PhysiologyDokument3 SeitenPa Tho Physiologyaprilkow07Noch keine Bewertungen
- Pa Tho Physiology of RaDokument7 SeitenPa Tho Physiology of Ralisalmar2008Noch keine Bewertungen
- ParacetamolDokument2 SeitenParacetamolsleep whatNoch keine Bewertungen
- Chronic Kidney Disease (CKD) : Diabetes High Blood Pressure Responsible For Up To Two-Thirds GlomerulonephritisDokument6 SeitenChronic Kidney Disease (CKD) : Diabetes High Blood Pressure Responsible For Up To Two-Thirds GlomerulonephritisKyle Ü D. CunanersNoch keine Bewertungen
- What Is Prednisolone?Dokument12 SeitenWhat Is Prednisolone?Chandni SeelochanNoch keine Bewertungen
- Day 2 - Ulcerative Colitis PDFDokument14 SeitenDay 2 - Ulcerative Colitis PDFMaria Charis Anne IndananNoch keine Bewertungen
- Patho of OCDokument1 SeitePatho of OCOrrin D. BarbaNoch keine Bewertungen
- Cholecystectomy (: Laparoscopic GallstonesDokument4 SeitenCholecystectomy (: Laparoscopic GallstonesAlexia BatungbacalNoch keine Bewertungen
- Incarcerated Hernia: Case Studies Sushila Ladumor, MDDokument11 SeitenIncarcerated Hernia: Case Studies Sushila Ladumor, MDbeautifulbeastNoch keine Bewertungen
- Trifluridine and TipiracilDokument3 SeitenTrifluridine and TipiracilKristine AcasioNoch keine Bewertungen
- Ulcerative ColitisDokument9 SeitenUlcerative Colitiskint manlangitNoch keine Bewertungen
- Unit 1 5ADokument7 SeitenUnit 1 5AArvin O-CaféNoch keine Bewertungen
- CellulitisDokument5 SeitenCellulitisaimigdragonNoch keine Bewertungen
- Case 052: Biliary ColicDokument4 SeitenCase 052: Biliary ColicZauzaNoch keine Bewertungen
- Thyroid Papillary Carcinoma CaseDokument6 SeitenThyroid Papillary Carcinoma CaseRandy F BabaoNoch keine Bewertungen
- Kaposi's SarcomaDokument6 SeitenKaposi's SarcomaveremkovichNoch keine Bewertungen
- BARANDINO, Jia Laurice (Gouty Arthritis)Dokument18 SeitenBARANDINO, Jia Laurice (Gouty Arthritis)Deinielle Magdangal RomeroNoch keine Bewertungen
- Chest InjuryDokument4 SeitenChest InjuryFRANCINE EVE ESTRELLANNoch keine Bewertungen
- Final Case Study OutputDokument50 SeitenFinal Case Study Outputudntnid2knwmeNoch keine Bewertungen
- Patophy of PudDokument4 SeitenPatophy of PudClarence BravioNoch keine Bewertungen
- Case UreterolithiasisDokument26 SeitenCase UreterolithiasisPutri Dwi Kartini0% (1)
- CASE STUDY #3 Urinary System (Urninary Tract Infection or UTI)Dokument5 SeitenCASE STUDY #3 Urinary System (Urninary Tract Infection or UTI)Lerma PagcaliwanganNoch keine Bewertungen
- Annotated Group 2 Impetigo Concept Mapping 1Dokument30 SeitenAnnotated Group 2 Impetigo Concept Mapping 1DHANE ANN CAMPOSANONoch keine Bewertungen
- 2.3 HYPOCALCEMIA and HYPERCALCEMIADokument7 Seiten2.3 HYPOCALCEMIA and HYPERCALCEMIABooz Waief CaluzaNoch keine Bewertungen
- UrethritisDokument11 SeitenUrethritismarej143Noch keine Bewertungen
- Review: New Concepts in The Pathophysiology of Inflammatory Bowel DiseaseDokument11 SeitenReview: New Concepts in The Pathophysiology of Inflammatory Bowel DiseaseReynalth Andrew Sinaga100% (1)
- Skin Cancer: I. Overview of The DisorderDokument3 SeitenSkin Cancer: I. Overview of The DisorderSung ChiiNoch keine Bewertungen
- Epidemiology and Pathophysiology of Colonic Diverticular DiseaseDokument8 SeitenEpidemiology and Pathophysiology of Colonic Diverticular DiseaseAnonymous Hz5w55Noch keine Bewertungen
- ChlamydiaDokument37 SeitenChlamydiaElizabeth QuiñonesNoch keine Bewertungen
- OsteomyelitisDokument7 SeitenOsteomyelitis4kscribd100% (1)
- Pathophysiology (Client Base) :: Predisposing Factors: Precipitating FactorsDokument1 SeitePathophysiology (Client Base) :: Predisposing Factors: Precipitating Factorsleslie_macasaetNoch keine Bewertungen
- Gastric CancerDokument7 SeitenGastric CancerMicah PingawanNoch keine Bewertungen
- Medical-Surgical Nursing: St. Paul University Surigao St. Paul University System Surigao City, PhilippinesDokument2 SeitenMedical-Surgical Nursing: St. Paul University Surigao St. Paul University System Surigao City, PhilippinesSelwynVillamorPatente0% (1)
- Osteogenesis ImperfectaDokument52 SeitenOsteogenesis ImperfectaTrias AdnyanaNoch keine Bewertungen
- Pathophysiology of Pressure UlcersDokument1 SeitePathophysiology of Pressure UlcersSTORAGE FILENoch keine Bewertungen
- Or RRLDokument4 SeitenOr RRLAlponce Edal AdagNoch keine Bewertungen
- Case Presentation Second Year 2nd SemesterDokument36 SeitenCase Presentation Second Year 2nd SemesterJohn Robert PescadorNoch keine Bewertungen
- HIV and Its TreatmentDokument24 SeitenHIV and Its Treatmentaathira_kNoch keine Bewertungen
- Cholecystitis Litiasis EctomyDokument23 SeitenCholecystitis Litiasis EctomyTimothy WilliamsNoch keine Bewertungen
- Anorexia NervosaDokument11 SeitenAnorexia NervosaSashMalikNoch keine Bewertungen
- NCP Potts DiseaseDokument2 SeitenNCP Potts Diseasearcitap0% (1)
- Nursing Care Plan Clubfoot or Talipes EquinovarusDokument6 SeitenNursing Care Plan Clubfoot or Talipes EquinovarusMarzie LugtuNoch keine Bewertungen
- A Drug Study On FansidarDokument7 SeitenA Drug Study On FansidarCasey EmellanoNoch keine Bewertungen
- Pathophysiology of Transitional Cell CarcinomaDokument10 SeitenPathophysiology of Transitional Cell CarcinomaJheanAlphonsineT.MeansNoch keine Bewertungen
- Potassium Chloride Injection: Product MonographDokument18 SeitenPotassium Chloride Injection: Product MonographMatthew ParsonsNoch keine Bewertungen
- Anatomy and Phsyiology of MeningococcemiaDokument2 SeitenAnatomy and Phsyiology of MeningococcemiaKevin Comahig100% (1)
- Path o Physiology of SyphilisDokument1 SeitePath o Physiology of Syphilis3S - JOCSON, DENESE NICOLE LEE M.Noch keine Bewertungen
- Communicable DiseaseDokument22 SeitenCommunicable DiseaseheheeheheNoch keine Bewertungen
- LISTERIOSISDokument15 SeitenLISTERIOSISCedric VillalbaNoch keine Bewertungen
- Pathognomonic Signs of Communicable Diseases: JJ8009 Health & NutritionDokument2 SeitenPathognomonic Signs of Communicable Diseases: JJ8009 Health & NutritionMauliza Resky NisaNoch keine Bewertungen
- Fracture at Right Femur Orif Case StudyDokument16 SeitenFracture at Right Femur Orif Case StudyLouie ParillaNoch keine Bewertungen
- Nursing Care PlanDokument2 SeitenNursing Care Planusama_salaymehNoch keine Bewertungen
- Myasthenia Gravis PathophysiologyDokument2 SeitenMyasthenia Gravis PathophysiologyRyan Daet0% (1)
- Anatomy and Physiology DengueDokument5 SeitenAnatomy and Physiology Denguenva226Noch keine Bewertungen
- Abcess CellulitisDokument60 SeitenAbcess CellulitisKirk Kevin PolanteNoch keine Bewertungen
- A Study of the Lack of Hiv/Aids Awareness Among African American Women: a Leadership Perspective: Awareness That All Cultures Should Know AboutVon EverandA Study of the Lack of Hiv/Aids Awareness Among African American Women: a Leadership Perspective: Awareness That All Cultures Should Know AboutBewertung: 5 von 5 Sternen5/5 (1)
- Tao 56 2 106Dokument6 SeitenTao 56 2 106PutriIffahNoch keine Bewertungen
- Toleransi EnteralDokument11 SeitenToleransi EnteralPutriIffahNoch keine Bewertungen
- Jurnal Retinopati DiabetikDokument7 SeitenJurnal Retinopati DiabetikPutriIffahNoch keine Bewertungen
- Manajemen Pemindahan Pasien PDFDokument10 SeitenManajemen Pemindahan Pasien PDFPutriIffahNoch keine Bewertungen
- Presentasi Trauma ToraksDokument22 SeitenPresentasi Trauma ToraksPutriIffahNoch keine Bewertungen
- Jghe v3 Id1043Dokument5 SeitenJghe v3 Id1043PutriIffahNoch keine Bewertungen
- Intestinal Involvement in Kawasaki DiseaseDokument13 SeitenIntestinal Involvement in Kawasaki DiseasePutriIffahNoch keine Bewertungen
- 07 - 260CME-Clinical Manifestations of Ocular TuberculosisDokument5 Seiten07 - 260CME-Clinical Manifestations of Ocular TuberculosisPika LubisNoch keine Bewertungen
- DM Foot CareDokument27 SeitenDM Foot CareKatrina KattNoch keine Bewertungen
- HHS 792 WDokument5 SeitenHHS 792 WPutriIffahNoch keine Bewertungen
- Jurnal - Olopatadine HCL Vs Ketotifen Fumarate Untuk Konjungtivitis AlergiDokument19 SeitenJurnal - Olopatadine HCL Vs Ketotifen Fumarate Untuk Konjungtivitis AlergiPutriIffahNoch keine Bewertungen
- SalerioDokument28 SeitenSalerioRizqaFebrilianyNoch keine Bewertungen
- Klasifikasi WagnerDokument8 SeitenKlasifikasi WagnerNina AmeliaNoch keine Bewertungen
- Physical Activity Promotion Through Primary Health Care in EnglandDokument3 SeitenPhysical Activity Promotion Through Primary Health Care in EnglandPutriIffahNoch keine Bewertungen
- Laporan Bangsal Selasa Rabu KamisDokument10 SeitenLaporan Bangsal Selasa Rabu KamisPutriIffahNoch keine Bewertungen
- Leveling Up Part2Dokument144 SeitenLeveling Up Part2PutriIffahNoch keine Bewertungen
- Laporan Bangsal Selasa Rabu KamisDokument10 SeitenLaporan Bangsal Selasa Rabu KamisPutriIffahNoch keine Bewertungen
- Clayton, 2009Dokument7 SeitenClayton, 2009Anggie AnggriyanaNoch keine Bewertungen
- Health Belief ModelDokument3 SeitenHealth Belief ModelPutri LenggogeniNoch keine Bewertungen
- XSL FO: Original PaperDokument18 SeitenXSL FO: Original PaperPutriIffahNoch keine Bewertungen
- Laporan Bangsal Selasa Rabu KamisDokument10 SeitenLaporan Bangsal Selasa Rabu KamisPutriIffahNoch keine Bewertungen
- 6th Central Pay Commission Salary CalculatorDokument15 Seiten6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- SICH Mgmt2Dokument9 SeitenSICH Mgmt2Lennon Ponta-oyNoch keine Bewertungen
- Dermatology Handbook For Medical Students 2nd Edition 2014 Final2Dokument76 SeitenDermatology Handbook For Medical Students 2nd Edition 2014 Final2Nogra CarlNoch keine Bewertungen
- Ancy Lost OmaDokument5 SeitenAncy Lost OmaPutriIffahNoch keine Bewertungen
- Health Belief ModelDokument3 SeitenHealth Belief ModelPutri LenggogeniNoch keine Bewertungen
- Gizi Phrs PosterDokument3 SeitenGizi Phrs PosterPutriIffahNoch keine Bewertungen
- DifteriDokument34 SeitenDifteriPutriIffahNoch keine Bewertungen
- Health Belief ModelDokument3 SeitenHealth Belief ModelPutri LenggogeniNoch keine Bewertungen
- Hemangioma, Aneurysmal Bone CystDokument59 SeitenHemangioma, Aneurysmal Bone CystPutriIffahNoch keine Bewertungen
- Bomba MedtronicDokument40 SeitenBomba MedtronicrafaelplNoch keine Bewertungen
- R115Patients PDFDokument14 SeitenR115Patients PDFcarneoliaNoch keine Bewertungen
- Get Big Diet by Jacob WilsonDokument5 SeitenGet Big Diet by Jacob WilsonYoel OrueNoch keine Bewertungen
- Diklofenac DietilaminDokument12 SeitenDiklofenac DietilaminAnnisa FitrianaNoch keine Bewertungen
- Ucrete MFDokument3 SeitenUcrete MFMohiuddin MuhinNoch keine Bewertungen
- Module 2 Personality Traits 3Dokument6 SeitenModule 2 Personality Traits 3Angelica BautistaNoch keine Bewertungen
- Tray Line PresentationDokument22 SeitenTray Line Presentationapi-235273578100% (1)
- Deborah Falla The Role of Motor Learning and Neuroplasticity in Designing RehabilitationDokument5 SeitenDeborah Falla The Role of Motor Learning and Neuroplasticity in Designing RehabilitationDago Angel Prieto PalavecinoNoch keine Bewertungen
- Journal of Food Composition and AnalysisDokument11 SeitenJournal of Food Composition and AnalysisJessica WeaverNoch keine Bewertungen
- 07 Emergency and Critical CareDokument20 Seiten07 Emergency and Critical CareDenise BuckleyNoch keine Bewertungen
- Vanrobaeys Catalog 2016Dokument40 SeitenVanrobaeys Catalog 2016Alexandru Sandor Szabo100% (1)
- Confidentiality - A Case ScenarioDokument4 SeitenConfidentiality - A Case ScenarioimmaNoch keine Bewertungen
- Peel Instruction BookletDokument16 SeitenPeel Instruction BookletMariana HernandezNoch keine Bewertungen
- Drug Study - CaDokument3 SeitenDrug Study - Casaint_ronald8Noch keine Bewertungen
- Skin Diseases of GoatsDokument8 SeitenSkin Diseases of GoatsmadheshvetNoch keine Bewertungen
- 002-Trauma & BurnsDokument36 Seiten002-Trauma & BurnsAhmed Zaghw100% (2)
- Open Reduction and Internal Fixation of The.17Dokument2 SeitenOpen Reduction and Internal Fixation of The.17Rakesh KumarNoch keine Bewertungen
- Hot Tips For Master Plumber Boards2Dokument8 SeitenHot Tips For Master Plumber Boards2jcedricaquino100% (1)
- Norton Mental Health Annual Catalog 2016Dokument84 SeitenNorton Mental Health Annual Catalog 2016NortonMentalHealthNoch keine Bewertungen
- Angels in The NurseryDokument17 SeitenAngels in The NurseryRoxana DincaNoch keine Bewertungen
- Unit 4 Humanistic and Self Theory (Maslow and Rogers) : StructureDokument19 SeitenUnit 4 Humanistic and Self Theory (Maslow and Rogers) : StructuremustafaNoch keine Bewertungen
- The Psychological AspectsDokument7 SeitenThe Psychological AspectsInvisible_TouchNoch keine Bewertungen
- HNELHD CG 12 04 Warfarin Age Adjusted Dosing in AdultsDokument5 SeitenHNELHD CG 12 04 Warfarin Age Adjusted Dosing in AdultsAnonymous 4txA8N8etNoch keine Bewertungen
- Rebekah Wilson PT ResumeDokument3 SeitenRebekah Wilson PT Resumeapi-487211279Noch keine Bewertungen
- Lupus NephritisDokument15 SeitenLupus NephritisVilza maharaniNoch keine Bewertungen
- Primal Kitchen Cookbook ReviewDokument338 SeitenPrimal Kitchen Cookbook ReviewPrimalBlueprint100% (21)
- Hydroxychloroquine PDFDokument2 SeitenHydroxychloroquine PDFsbsreddy100% (1)
- Document 105Dokument14 SeitenDocument 105Marie JhoanaNoch keine Bewertungen
- What Is Peripheral Arterial Disease (PAD) ?: Blood VesselsDokument6 SeitenWhat Is Peripheral Arterial Disease (PAD) ?: Blood VesselsmainehoonaNoch keine Bewertungen
- Adam B. Galla: Independent Consultant (July 2016) ManniondanielsDokument4 SeitenAdam B. Galla: Independent Consultant (July 2016) ManniondanielsAnonymous G4aIQ7aHNoch keine Bewertungen