Beruflich Dokumente
Kultur Dokumente
Impetigo in Neonatus
Hochgeladen von
asep budiyantoCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Impetigo in Neonatus
Hochgeladen von
asep budiyantoCopyright:
Verfügbare Formate
WJ CC World Journal of
Clinical Cases
Submit a Manuscript: http://www.wjgnet.com/esps/ World J Clin Cases 2016 July 16; 4(7): 191-194
Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx ISSN 2307-8960 (online)
DOI: 10.12998/wjcc.v4.i7.191 2016 Baishideng Publishing Group Inc. All rights reserved.
CASE REPORT
Staphylococcal bullous impetigo in a neonate
Shalini Dewan Duggal, Tanisha Bharara, Pragnya Paramita Jena, Avinash Kumar, Abha Sharma, Renu Gur,
Sanjay Chaudhary
Shalini Dewan Duggal, Tanisha Bharara, Pragnya Paramita Article in press: May 11, 2016
Jena, Avinash Kumar, Abha Sharma, Renu Gur, Department Published online: July 16, 2016
of Microbiology, Dr Baba Saheb Ambedkar Hospital, Rohini,
Delhi 110085, India
Sanjay Chaudhary, Department of Pediatrics, Dr Baba Saheb
Ambedkar Hospital, Rohini, Delhi 110085, India Abstract
An otherwise healthy, full-term neonate presented at day
Author contributions: All authors contributed to the acquisition 15 of life to the pediatric emergency with generalized
of data, writing, and revision of this manuscript. papulo-pustular rash for 2 d. This was finally diagnosed
as bullous impetigo caused by Staphylococcus aureus
Institutional review board statement: This case report was
exempt from the Institutional Review Board standards at Dr Baba (S. aureus ). The skin lesions decreased significantly
Saheb Ambedkar Hospital, Rohini, Delhi, India. after starting antibiotic therapy and drainage of blister
fluid. There was no recurrence of the lesions on follow-
Informed consent statement: Informed Consent from patients up. This case of generalized pustular eruption due to S.
mother (verbal). aureus in a neonate is reported, as it poses a diagnostic
dilemma and can have serious consequences if left
Conflict-of-interest statement: The authors have no conflicts of untreated.
interests to declare.
Key words: Pustular lesions; Staphylococcus aureus ;
Open-Access: This article is an open-access article which was
selected by an in-house editor and fully peer-reviewed by external Bullous impetigo
reviewers. It is distributed in accordance with the Creative
Commons Attribution Non Commercial (CC BY-NC 4.0) license, The Author(s) 2016. Published by Baishideng Publishing
which permits others to distribute, remix, adapt, build upon this Group Inc. All rights reserved.
work non-commercially, and license their derivative works on
different terms, provided the original work is properly cited and Core tip: Pustular disorders are common in neonatal
the use is non-commercial. See: http://creativecommons.org/ period. It is important to distinguish benign physiological
licenses/by-nc/4.0/ rashes from significant pathological eruptions. A case
of generalized pustular eruption due to Staphylococcus
Manuscript source: Invited manuscript
aureus in a neonate is reported. Such lesions can pose
Correspondence to: Dr. Shalini Dewan Duggal, Specialist, a diagnostic dilemma and have serious consequences if
Department of Microbiology, Dr Baba Saheb Ambedkar Hospital, left untreated. Differential diagnosis of neonatal pustular
Sector-6, Rohini, Delhi 110085, lesions has been discussed and main features of each
India. shaliniduggal2005@rediffmail.com have been highlighted here.
Telephone: +91-11-9810921982
Fax: +91-11-27055585
Duggal SD, Bharara T, Jena PP, Kumar A, Sharma A, Gur R,
Received:January 23, 2016 Chaudhary S. Staphylococcal bullous impetigo in a neonate.
Peer-review started: January 26, 2016 World J Clin Cases 2016; 4(7): 191-194 Available from: URL:
First decision: March 1, 2016 http://www.wjgnet.com/2307-8960/full/v4/i7/191.htm DOI:
Revised: March 13, 2016
http://dx.doi.org/10.12998/wjcc.v4.i7.191
Accepted: May 10, 2016
WJCC|www.wjgnet.com 191 July 16, 2016|Volume 4|Issue 7|
Duggal SD et al . Staphylococcal pustular eruptions
INTRODUCTION
Pustular disorders are common in the neonatal period,
[1,2]
most of which are benign and self-limiting . It is
important to distinguish the benign physiological rashes
[3]
from significant pathological pustular eruptions .
Similarity of clinical features, immaturity of neonatal
skin and lack of relevant literature poses diagnostic
[4]
difficulty in cases of neonatal pustular lesions . Another
practical problem relates to the process of ruling out an
infectious etiology.
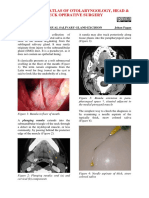
CASE REPORT Figure 1 Flaccid, non-tender bullous lesions on back of the neonate.
An otherwise healthy, full-term neonate presented
at day 15 of life, to the pediatric emergency with
generalized papulo-pustular lesions for 2 d. It was
during the summer of year 2015. The neonate was born
at a primary health centre following a full-term normal
vaginal delivery and had been on breastfeed since birth.
The mother gave no history of sexually transmitted
infections or genital lesions and there was no history
of similar complaints in other siblings. Informed
consent was taken from the mother and the neonate
was examined. On examination his general hygiene
appeared to be poor. He weighed 2600 g, was active,
showed no malaise, or irritability. The pustules were
15-20 in number, generalized in distribution, over scalp,
neck, trunk and extremities sparing palms and soles.
Figure 2 Direct Gram stain of pus showing many polymorphonuclear
These were flaccid, non-tender bullous lesions with an cells and intracellular gram positive cocci.
erythematous base, measuring 1 to 2 cm in diameter
(Figure 1). No scars or sinuses were present. These
were provisionally diagnosed as viral eruptions and a smear was negative. However blood culture of the
call was sent to the Microbiology Department for opinion neonate could not be performed. Human immuno
and necessary investigations. He was afebrile, had no deficiency virus serology and venereal diseases research
lymphadenopathy, the neonatal reflexes and rest of the laboratory test (for syphilis) of mother was negative.
systemic examination was normal. All the pustules were The patient was isolated and treatment was started
punctured and dark yellowish purulent fluid was drained with oral suspension of amoxicillin and clavulanic acid
aseptically. This fluid was inoculated at the bedside on (30 mg/kg body weight divided every 12 h) along with
Chocolate agar, Blood agar and MacConkey agar plates topical mupirocin cream twice daily. The skin lesions
and smears were prepared for direct Gram staining. decreased significantly after starting antibiotic therapy
The plates were streaked and incubated aerobically and drainage of blister fluid. No fresh lesions were seen
overnight at 37. A tube of Brain Heart Infusion broth and there was no recurrence of the lesions during his
and a plate of Mannitol Salt Agar were also inoculated. 7 d hospital stay. He was discharged with an advice to
Antimicrobial susceptibility test was performed by report back in case of recurrence. However, no further
Kirby-Bauer Disc diffusion method and the results were episode was reported.
interpreted as per CLSI 2015 guidelines.
Direct Gram stain showed many pus cells and
intracellular gram-positive cocci in clusters (Figure 2).
DISCUSSION
Pure growth of pin-head, buff coloured, beta hemolytic Pustular eruptions pose a diagnostic dilemma during
colonies appeared on Blood agar after overnight the neonatal period. Diagnosis depends upon clinical
incubation. The case was finally diagnosed as bullous features along with few simple laboratory investigations.
impetigo caused by Staphylococcus aureus (S. aureus). There are many different causes of neonatal pustular
The isolate was identified on the basis of Gram stain, dermatosis including noninfectious and infectious
[3-5]
golden yellow pigment, catalase test, coagulase (slide, causes (Table 1). Ruling out an infective etiology
tube) test and yellow colonies on Mannitol Salt Agar. remains the corner stone of any diagnostic approach
It was found to be sensitive to penicillin, cefoxitin, in neonatal pustular eruptions. Early and accurate
clindamycin, gentamicin, and chloramphenicol but diagnosis can spare a healthy neonate with a benign
resistant to erythromycin and ciprofloxacin. Tzanck treatable condition from unnecessary investigations and
WJCC|www.wjgnet.com 192 July 16, 2016|Volume 4|Issue 7|
Duggal SD et al . Staphylococcal pustular eruptions
Table 1 Differential diagnosis of Staphylococcal bullous impetigo in neonates
Causes Characteristic features
Infectious causes
Herpes simplex virus Grouped vesicles on an erythematous base that rupture to become erosions covered by crusts; may have
prodromal symptoms
Varicella zoster virus Lesions of different stages are present at the same time in a given body area as new crops develop
Streptococcus spp. Similar lesions with Gram stain showing Gram positive cocci in chains. Further differentiated on the basis of
culture characteristics and biochemical tests
Treponema pallidum Diffuse erythematous lesions containing large number of treponemes. Associated systemic involvement
Staphylococcal scalded skin Cutaneous tenderness, positive Nikolsky sign, large areas of desquamation or exfoliation. Infection spreads
syndrome hematogenously because of absence of protective antitoxin antibodies. Culture of bullae is negative
Cutaneous candidiasis Generalized skin eruptions at birth, characterized by erythematous macules and papules
Candida albicans demonstrated on direct KOH smear, skin biopsy
Listeriosis Presents with systemic signs and symptoms of sepsis
Pseudomonas skin infection These may present as localized cutaneous folliculitis or as necrotising infection, ecthyma gangrenosum. Lesions
are painful and systemic involvement may be seen. Diagnosis is confirmed by isolation of Pseudomonas aeruginosa
from lesions
Noninfectious causes
Bullous erythema multiforme Usually involves extensor surfaces of extremities
Bullous lupus erythematosus May be pruritic; tends to favor the upper part of the trunk and proximal upper extremities
Bullous pemphigoid Vesicles and bullae appear rapidly on widespread pruritic, urticarial plaques
Pemphigus vulgaris Healing with hyperpigmentation
Stevens-Johnson syndrome Vesiculo-bullous disease of the skin, mouth, eyes, and genitalia; ulcerative stomatitis with hemorrhagic crusting is
most characteristic feature
Toxic epidermal necrolysis Stevens-Johnsonlike mucous membrane disease followed by diffuse generalized detachment of the epidermis
Insect bites Bullae seen with pruritic papules grouped mainly in exposed parts of body
Thermal burns History of burn with blistering in second-degree burns
Neonatal pustular psoriasis Sterile widespread pustules on an erythematous background
Erythema toxicum neonatorum Benign self-limited eruption occurring in early neonatal period in healthy neonates. Macular erythema, papules,
vesicles or pustules
Neonatal acne Acneform eruptions in newborn often seen on nose and adjacent portions of cheek
also prevent the occurrence of severe complications. Rarely these skin and soft tissue infections may
Incubation period of Staphylococcal skin and soft invade dermal and fascial barriers to cause S. aureus
[10]
tissue infections vary from 2-10 d, thus, ruling out bacteremia . Blebs should be punctured as soon as
[11]
iatrogenic causes at the time of delivery in this case. In formed and topical ointment/lotion should be applied .
the present case probable source of S. aureus infection Full recovery usually occurs in 2-3 wk. Isolation of the
could be mother/other family members/fomites like patient is recommended as an infection control measure
dirty linen/clothes. The pathogenicity of S. aureus skin otherwise it may rapidly spread to other patients,
and soft tissue infections is related to various bacterial attendants and health care workers.
[6]
surface components and to extracellular proteins . The main objective of this article was to emphasize
S. aureus can disrupt the skin barrier by secreting a systematic approach in evaluation of pustular eru
exfoliative toxins A and B. These act as superantigens ptions in the neonate. A detailed perinatal history;
to promote massive release of T-lymphocytes and complete physical examination; and careful assessment
[7]
lymphokines like IL-1, IL-6 and TNF- . The exfoliative of the morphology and distribution of the lesions form
toxin A causes proteolytic cleavage of desmoglein-1 the cornerstone for diagnosis. Targeted therapy can
which is present in desmosomes and is responsible for reduce the morbidity and mortality; and associated
cell-cell adhesion. This leads to blister formation just hospitalization costs.
below the stratum corneum allowing bacteria in the
[8]
blister fluid to proliferate and spread . Depending on
the immune status of the host, it may lead to formation COMMENTS
COMMENTS
of exfoliative cutaneous eruptions, vomiting, fall in
Case characteristics
blood pressure and shock as in staphylococcal scalded
A full-term neonate presented at day 15 of life, to the pediatric emergency with
skin syndrome or may be localized to skin as bullous generalized papulo-pustular lesions for 2 d.
impetigo, as seen in the present case. There have been
several case reports suggesting role of Panton Valentine
Clinical diagnosis
leukocidin toxin in Staphylococcal skin infections; Neonatal pustulosis.
associated more commonly with MSSA than MRSA,
[9]
particularly in community isolates . Differential diagnosis
In full-term newborns, S. aureus infection usually Infectious causes like Herpes simplex virus, Varicella zoster virus, Streptococcus
first appears as a skin and soft tissue infection, but may spp., non-infectious causes include bullous erythema multiforme, bullous lupus
[4]
rapidly progress to osteomyelitis and pneumonia . erythematosus, bullous pemphigoid.
WJCC|www.wjgnet.com 193 July 16, 2016|Volume 4|Issue 7|
Duggal SD et al . Staphylococcal pustular eruptions
Laboratory diagnosis
All the pustules were punctured and fluid was cultured. Antimicrobial
REFERENCES
susceptibility test was performed by Kirby-Bauer Disc diffusion method and the 1 Van Praag MC, Van Rooij RW, Folkers E, Spritzer R, Menke HE,
results were interpreted as per CLSI 2015 guidelines. Oranje AP. Diagnosis and treatment of pustular disorders in the
neonate. Pediatr Dermatol 1997; 14: 131-143 [PMID: 9144701
DOI: 10.1111/j.1525-1470.1997.tb00221.x]
Microbiological diagnosis 2 Baruah CM, Bhat V, Bhargava R, Garg RB, Kumar V. Prevalence
Direct Gram stain showed many pus cells and intracellular gram-positive cocci in
of dermatoses in the neonates in Pondichery. Indian J Der Ven Lepl
clusters. Culture grew Staphylococcus aureus (S. aureus).
1991; 57: 25-28
3 Ghosh S. Neonatal pustular dermatosis: an overview. Indian J
Treatment Dermatol 2015; 60: 211 [PMID: 25814724 DOI: 10.4103/0019-515
Complete resolution of lesions after treatment with oral amoxicillin and clavulanic 4.152558]
acid along with topical mupirocin cream. 4 Nanda S, Reddy BS, Ramji S, Pandhi D. Analytical study of
pustular eruptions in neonates. Pediatr Dermatol 2002; 19: 210-215
[PMID: 12047639 DOI: 10.1046/j.1525-1470.2002.00061.x]
Related reports 5 Cole C, Gazewood J. Diagnosis and treatment of impetigo. Am
In full-term newborns, S. aureus infection usually first appears as a skin and
Fam Physician 2007; 75: 859-864 [PMID: 17390597]
soft tissue infection, but may rapidly progress to osteomyelitis and pneumonia
6 Archer GL. Staphylococcus aureus: a well-armed pathogen.
or cause bacteremia. Blebs should be punctured as soon as formed and topical
Clin Infect Dis 1998; 26: 1179-1181 [PMID: 9597249 DOI:
ointment/lotion should be applied. Full recovery usually occurs in 2-3 wk.
10.1086/520289]
Isolation of the patient is recommended as an infection control measure.
7 Manders SM. Toxin-mediated streptococcal and staphylococcal
disease. J Am Acad Dermatol 1998; 39: 383-398; quiz 399-400
Term explanation [PMID: 9738772 DOI: 10.1016/S0190-9622(98)70314-7]
Pustules are small pus filled blisters in the superficial layers of skin. 8 Amagai M, Matsuyoshi N, Wang ZH, Andl C, Stanley JR. Toxin in
bullous impetigo and staphylococcal scalded-skin syndrome targets
desmoglein 1. Nat Med 2000; 6: 1275-1277 [PMID: 11062541
Experiences and lessons DOI: 10.1038/81385]
(1) Pustular eruptions in neonates pose a diagnostic dilemma; (2) Diagnosis
9 Lina G, Pimont Y, Godail-Gamot F, Bes M, Peter MO, Gauduchon
depends upon clinical features along with few simple laboratory investigations;
V, Vandenesch F, Etienne J. Involvement of Panton-Valentine
(3) A detailed perinatal history; complete physical examination; and careful
leukocidin-producing Staphylococcus aureus in primary skin
assessment of the morphology and distribution of the lesions form the corners
infections and pneumonia. Clin Infect Dis 1999; 29: 1128-1132
tone for diagnosis; (4) Targeted therapy can reduce the morbidity and mortality;
[PMID: 10524952 DOI: 10.1086/313461]
and associated hospitalization costs.
10 Rongpharpi SR, Duggal S, Kalita H, Duggal AK. Staphylococcus
aureus bacteremia: targeting the source. Postgrad Med 2014; 126:
Peer-review 167-175 [PMID: 25295661 DOI: 10.3810/pgm.2014.09.2811]
The paper is well written. The case is interesting and clearly reported. 11 Soellner CH. Pemphigus neonatorum. Ame J Nurs 1922; 23: 94-98
P- Reviewer: Gao SH, Hu SCS, Negosanti L S- Editor: Qiu S
L- Editor: A E- Editor: Wu HL
WJCC|www.wjgnet.com 194 July 16, 2016|Volume 4|Issue 7|
Published by Baishideng Publishing Group Inc
8226 Regency Drive, Pleasanton, CA 94588, USA
Telephone: +1-925-223-8242
Fax: +1-925-223-8243
E-mail: bpgoffice@wjgnet.com
Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx
http://www.wjgnet.com
2016 Baishideng Publishing Group Inc. All rights reserved.
Das könnte Ihnen auch gefallen
- ImpetigoDokument24 SeitenImpetigoIvan Sitohang100% (2)
- ChancroidDokument6 SeitenChancroidSukmasari TNoch keine Bewertungen
- Short Atlas in Pediatrics Spot Diagnosis of The Most Common Pediatric Diseases 2nd EditionDokument113 SeitenShort Atlas in Pediatrics Spot Diagnosis of The Most Common Pediatric Diseases 2nd Editiondeycallmebud100% (2)
- Bacterial Skin InfectionsDokument9 SeitenBacterial Skin InfectionskateverdadNoch keine Bewertungen
- @MedicalBooksStore 2016 AntibioticDokument349 Seiten@MedicalBooksStore 2016 Antibioticant bee100% (1)
- Pathophysiology ImpetigoDokument3 SeitenPathophysiology ImpetigoAnne de VeraNoch keine Bewertungen
- Covid-19 Infection and PregnancyVon EverandCovid-19 Infection and PregnancyAhmed M. Maged El-GolyNoch keine Bewertungen
- ImpetigoDokument16 SeitenImpetigokikimasyhurNoch keine Bewertungen
- (Libribook - Com) Introduction To Clinical Infectious Diseases A Problem-Based Approach 1st EditionDokument465 Seiten(Libribook - Com) Introduction To Clinical Infectious Diseases A Problem-Based Approach 1st EditionDaoud IssaNoch keine Bewertungen
- 1 s2Dokument3 Seiten1 s2RyanNoch keine Bewertungen
- Screening of Infertile Females For Lower Genital Tract InfectionsDokument6 SeitenScreening of Infertile Females For Lower Genital Tract InfectionsIJAR JOURNALNoch keine Bewertungen
- Worl Journal of Pediatrics 2016Dokument8 SeitenWorl Journal of Pediatrics 2016Maria Emilia MenendezNoch keine Bewertungen
- 2010 Swidsinski GV Involves Females and Male and Is Transmitted SexuallyDokument8 Seiten2010 Swidsinski GV Involves Females and Male and Is Transmitted SexuallyClau RiveraNoch keine Bewertungen
- Doctor Who Identified SARS Becomes Its Victim - Intermediate PDFDokument5 SeitenDoctor Who Identified SARS Becomes Its Victim - Intermediate PDFhahahapsu100% (1)
- Appropriateness of Use of An AntimicrobialDokument3 SeitenAppropriateness of Use of An AntimicrobialKurt Maverick De LeonNoch keine Bewertungen
- Sarcoma Botryoides A Management Dilemma: A Review of Two CasesDokument8 SeitenSarcoma Botryoides A Management Dilemma: A Review of Two CasesPhn StanleyNoch keine Bewertungen
- Sarcoma Botryoides A Management Dilemma: A Review of Two CasesDokument8 SeitenSarcoma Botryoides A Management Dilemma: A Review of Two CasesPhn StanleyNoch keine Bewertungen
- International Journal of Recent Scientific ResearchDokument5 SeitenInternational Journal of Recent Scientific ResearchifahInayahNoch keine Bewertungen
- Reevaluating The FDA's Warning Against The Use of Probiotics inDokument6 SeitenReevaluating The FDA's Warning Against The Use of Probiotics inhosnameskarNoch keine Bewertungen
- Far Eastern University: Evidence Based NursingDokument4 SeitenFar Eastern University: Evidence Based NursingKhaye MendozaNoch keine Bewertungen
- Chikungunya FinalDokument23 SeitenChikungunya FinalMaruf HossainNoch keine Bewertungen
- The Management of Perianal Abscess With An Udumber Ksheer Pichu - A Case ReportDokument4 SeitenThe Management of Perianal Abscess With An Udumber Ksheer Pichu - A Case ReportInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Paediatrica Indonesiana: Andi Dwi Bahagia Febriani, Nilam Sartika Putri, Ema Alasiry, Dasril DaudDokument6 SeitenPaediatrica Indonesiana: Andi Dwi Bahagia Febriani, Nilam Sartika Putri, Ema Alasiry, Dasril DaudingridNoch keine Bewertungen
- A Case Report of Spontaneous Abortion Caused by Brucella Melitensis Biovar 3Dokument4 SeitenA Case Report of Spontaneous Abortion Caused by Brucella Melitensis Biovar 3lidwina143Noch keine Bewertungen
- The Diagnosis of Scabies by Non-Expert Examiners: A Study of Diagnostic AccuracyDokument13 SeitenThe Diagnosis of Scabies by Non-Expert Examiners: A Study of Diagnostic AccuracyAnisa Rifkia ZSNoch keine Bewertungen
- Zoon's Vulvitis: A Case Report: March 2020Dokument3 SeitenZoon's Vulvitis: A Case Report: March 2020perussi pranadiptaNoch keine Bewertungen
- TBM Checklist2Dokument9 SeitenTBM Checklist2SapNoch keine Bewertungen
- Tuse convulsiva-TNOAJOphthalmicSciRes563185-8109162 - 223131Dokument3 SeitenTuse convulsiva-TNOAJOphthalmicSciRes563185-8109162 - 223131Cosmin RăileanuNoch keine Bewertungen
- Counselling: Pamela FrancoDokument34 SeitenCounselling: Pamela FrancoKevin kovossNoch keine Bewertungen
- BV DiagnostikDokument20 SeitenBV DiagnostikCindy AgustinNoch keine Bewertungen
- Ulcer Outbreak ReportDokument11 SeitenUlcer Outbreak ReportEpie marcNoch keine Bewertungen
- Antimicrobial Blue Light Inactivation of Neisseria GonorrhoeaeDokument8 SeitenAntimicrobial Blue Light Inactivation of Neisseria GonorrhoeaeCristian PonceNoch keine Bewertungen
- Meningitis, Bali, Indonesia, 2014-2017: Streptococcus Suis-AssociatedDokument8 SeitenMeningitis, Bali, Indonesia, 2014-2017: Streptococcus Suis-AssociatedRinaRastutiNoch keine Bewertungen
- Robert Proposal 4Dokument26 SeitenRobert Proposal 4Brian RuttoNoch keine Bewertungen
- International Journal of Infectious DiseasesDokument9 SeitenInternational Journal of Infectious DiseasesHope ChrisNoch keine Bewertungen
- Letter To The Editor: Neonatal Coronavirus Disease-2019: Presentation and ManagementDokument3 SeitenLetter To The Editor: Neonatal Coronavirus Disease-2019: Presentation and ManagementadeNoch keine Bewertungen
- Newborn Umbilical Cord Care - An Evidence Based Quality ImprovemenDokument45 SeitenNewborn Umbilical Cord Care - An Evidence Based Quality ImprovemenNuridha FauziyahNoch keine Bewertungen
- Fcimb 11 694093Dokument12 SeitenFcimb 11 694093Marketable StudioNoch keine Bewertungen
- Scabies With Secondary Infection Resembling KerionDokument5 SeitenScabies With Secondary Infection Resembling KerionDwi PutriNoch keine Bewertungen
- Ihac 077Dokument7 SeitenIhac 077CONSTANTIUS AUGUSTONoch keine Bewertungen
- Newborn Umbilical Cord Care in Parakou in 2013: Practices and RisksDokument12 SeitenNewborn Umbilical Cord Care in Parakou in 2013: Practices and RisksFatma ElzaytNoch keine Bewertungen
- Title: Coronavirus Disease 2019 (COVID-19) During Pregnancy: A Case SeriesDokument28 SeitenTitle: Coronavirus Disease 2019 (COVID-19) During Pregnancy: A Case Seriesbrenda elielNoch keine Bewertungen
- Piaa 065Dokument15 SeitenPiaa 065Yulius DonyNoch keine Bewertungen
- Reproductive Assistance in HIV Serodiscordant CoupDokument16 SeitenReproductive Assistance in HIV Serodiscordant CoupDrAstha GuptaNoch keine Bewertungen
- Journal Reading AnakDokument19 SeitenJournal Reading AnakPutra Priambodo WibowoNoch keine Bewertungen
- The Potential For A Blood Test For Scabies: BackgroundDokument12 SeitenThe Potential For A Blood Test For Scabies: BackgroundMaya QadrianiNoch keine Bewertungen
- FFHGDDGHCSFGDokument2 SeitenFFHGDDGHCSFGनटराज नचिकेताNoch keine Bewertungen
- Rapid Diagnosis of Diarrhea Caused by Shigella Sonnei Using Dipsticks Comparison of Rectal Swabs, Direct Stool and Stool CultureDokument9 SeitenRapid Diagnosis of Diarrhea Caused by Shigella Sonnei Using Dipsticks Comparison of Rectal Swabs, Direct Stool and Stool CultureSuci IrianiNoch keine Bewertungen
- Chikungunya Final Draft 16052017finalDokument24 SeitenChikungunya Final Draft 16052017finalvishnupgiNoch keine Bewertungen
- Infectious Mononucleosis Due To Epstein-Barr Virus Infection in Children - A Profile From Eastern IndiaDokument7 SeitenInfectious Mononucleosis Due To Epstein-Barr Virus Infection in Children - A Profile From Eastern IndiaEmilia LunguNoch keine Bewertungen
- 21 NattaDokument6 Seiten21 NattaLidwina ApyakaNoch keine Bewertungen
- Pinworms (E.vermicularis) Mimicking Acute AppendicitisDokument2 SeitenPinworms (E.vermicularis) Mimicking Acute AppendicitisMedtext PublicationsNoch keine Bewertungen
- 1 s2.0 S1201971219304229 MainDokument10 Seiten1 s2.0 S1201971219304229 MainAlleidya SalsabiillaNoch keine Bewertungen
- D1 PDFDokument26 SeitenD1 PDFpopov357Noch keine Bewertungen
- The Stethoscope As A Vector of Infectious Diseases in The Paediatric DivisionDokument3 SeitenThe Stethoscope As A Vector of Infectious Diseases in The Paediatric DivisionAlagarsamy GNoch keine Bewertungen
- Diagnosis, Treatment, and Prevention of Typhoid Fever (WHO)Dokument48 SeitenDiagnosis, Treatment, and Prevention of Typhoid Fever (WHO)Nina KharimaNoch keine Bewertungen
- AcneDokument12 SeitenAcneWilhelmina DhNoch keine Bewertungen
- Beneficial Effects of A Mouthwash Containing An Antiviral Phthalocyanine Derivative On The Length of Hospital Stay For COVID 19: Randomised TrialDokument10 SeitenBeneficial Effects of A Mouthwash Containing An Antiviral Phthalocyanine Derivative On The Length of Hospital Stay For COVID 19: Randomised TrialtvinteNoch keine Bewertungen
- International Journal of Infectious DiseasesDokument3 SeitenInternational Journal of Infectious DiseasesPendidikan Dokter Unsyiah 2015Noch keine Bewertungen
- Identification of Microbial Contaminants in Sinus Rinse Squeeze Bottles Used by Allergic Rhinitis PatientsDokument4 SeitenIdentification of Microbial Contaminants in Sinus Rinse Squeeze Bottles Used by Allergic Rhinitis PatientsRiaNoch keine Bewertungen
- Saxena 2019Dokument4 SeitenSaxena 2019Fitri Kasmita SariNoch keine Bewertungen
- Literature Review Puerperal SepsisDokument5 SeitenLiterature Review Puerperal Sepsisgatewivojez3100% (1)
- Histoplasma Capsulatum Caused A Localized Tongue Ulcer in A Non-HIV Patient - A Case From Nonendemic CountryDokument3 SeitenHistoplasma Capsulatum Caused A Localized Tongue Ulcer in A Non-HIV Patient - A Case From Nonendemic CountryJohny SimatupangNoch keine Bewertungen
- PUERPERAL SEPSIS CoverDokument9 SeitenPUERPERAL SEPSIS CoverKerpersky LogNoch keine Bewertungen
- Acne: Current Concepts and ManagementVon EverandAcne: Current Concepts and ManagementDae Hun SuhNoch keine Bewertungen
- Coronavirus Crisis: Information and Help in the 2020 Pandemic - What Everyone Should KnowVon EverandCoronavirus Crisis: Information and Help in the 2020 Pandemic - What Everyone Should KnowNoch keine Bewertungen
- Corona Virus: Information You Need and How to Protect Yourself and Your Fellow Human BeingsVon EverandCorona Virus: Information You Need and How to Protect Yourself and Your Fellow Human BeingsNoch keine Bewertungen
- Jurnal AcneDokument10 SeitenJurnal Acneasep budiyantoNoch keine Bewertungen
- Jurnal Gangguan Bipolar PDFDokument7 SeitenJurnal Gangguan Bipolar PDFasep budiyantoNoch keine Bewertungen
- Ranula and Sublingual Salivary Gland ExcisionDokument5 SeitenRanula and Sublingual Salivary Gland Excisionasep budiyantoNoch keine Bewertungen
- Original Paper: Lumbar Disk Herniations - Clinical Status, Diagnosis, Imaging, Surgical Treatment and Global OutcomeDokument6 SeitenOriginal Paper: Lumbar Disk Herniations - Clinical Status, Diagnosis, Imaging, Surgical Treatment and Global Outcomeasep budiyantoNoch keine Bewertungen
- Chlorphenamine MaleateDokument2 SeitenChlorphenamine Maleateasep budiyantoNoch keine Bewertungen
- Presentasi JurnalDokument27 SeitenPresentasi Jurnalasep budiyantoNoch keine Bewertungen
- Presentasi Jurnal Interna: Hubungan PPOK Dengan Gagal JantungDokument19 SeitenPresentasi Jurnal Interna: Hubungan PPOK Dengan Gagal Jantungasep budiyantoNoch keine Bewertungen
- Impetigo in NeonatusDokument5 SeitenImpetigo in Neonatusasep budiyantoNoch keine Bewertungen
- Arch Dis Child 1998 Ladhani 85 8Dokument5 SeitenArch Dis Child 1998 Ladhani 85 8Dian Ayu Permata SandiNoch keine Bewertungen
- IZZ - PiodermaDokument51 SeitenIZZ - PiodermavivilmNoch keine Bewertungen
- Inflammatory DermatologyDokument64 SeitenInflammatory DermatologyDragonNoch keine Bewertungen
- Koningstein M 12Dokument14 SeitenKoningstein M 12pataraauliaNoch keine Bewertungen
- Staphylococcus LectureDokument27 SeitenStaphylococcus LectureRalt MedNoch keine Bewertungen
- 1) Bacterial Skin InfDokument32 Seiten1) Bacterial Skin InfsmrutuNoch keine Bewertungen
- Dermatology Training ManualDokument338 SeitenDermatology Training ManualTewodros Demeke100% (2)
- Bacterial and Rickettsial InfectionsDokument51 SeitenBacterial and Rickettsial Infectionslilis lestariNoch keine Bewertungen
- IMPETIGODokument10 SeitenIMPETIGOafifulichwan18Noch keine Bewertungen
- Staphylococcus Scalded Skin SyndromeDokument2 SeitenStaphylococcus Scalded Skin SyndromenikesecaNoch keine Bewertungen
- Dermatopathology For The Surgical Pathologist A Pattern-Based Approach To The Diagnosis of Inflammatory Skin Disorders Part IDokument21 SeitenDermatopathology For The Surgical Pathologist A Pattern-Based Approach To The Diagnosis of Inflammatory Skin Disorders Part IkarigargiuloNoch keine Bewertungen
- Diagnosis and Treatment of ImpetigoDokument9 SeitenDiagnosis and Treatment of Impetigonisha_furiNoch keine Bewertungen
- Impetigo: Author: Sadegh Amini, MD, Senior Clinical Research Fellow, Skin Research GroupDokument12 SeitenImpetigo: Author: Sadegh Amini, MD, Senior Clinical Research Fellow, Skin Research GroupDanoe Setyo SNoch keine Bewertungen
- Impetigo: Referat Makassar - 2016Dokument19 SeitenImpetigo: Referat Makassar - 2016keluargacendanaNoch keine Bewertungen
- ScienceDokument1 SeiteScienceni putu.comsurya dianaNoch keine Bewertungen
- INFECTIONS Staphylococcal InfectionsDokument48 SeitenINFECTIONS Staphylococcal InfectionsDr.P.NatarajanNoch keine Bewertungen
- Bacterial InfectionsDokument47 SeitenBacterial InfectionsSNoch keine Bewertungen
- Chapter 176. Superficial Cutaneous Infections and Pyodermas PDFDokument36 SeitenChapter 176. Superficial Cutaneous Infections and Pyodermas PDFTresia SimalangoNoch keine Bewertungen
- Clinical Review: Common Skin Infections in ChildrenDokument5 SeitenClinical Review: Common Skin Infections in ChildrenkhairaniNoch keine Bewertungen
- ImpetigoDokument34 SeitenImpetigoSarang LeeNoch keine Bewertungen
- Infectious Dermatosis (Bacterial Skin Infections)Dokument31 SeitenInfectious Dermatosis (Bacterial Skin Infections)Melch PintacNoch keine Bewertungen
- PiodermaDokument43 SeitenPiodermashlprtNoch keine Bewertungen