Beruflich Dokumente
Kultur Dokumente
Berkowitz 2009
Hochgeladen von
Gerardo LermaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Berkowitz 2009
Hochgeladen von
Gerardo LermaCopyright:
Verfügbare Formate
The n e w e ng l a n d j o u r na l of m e dic i n e
clinical practice
Molar Pregnancy
Ross S. Berkowitz, M.D., and Donald P. Goldstein, M.D.
This Journal feature begins with a case vignette highlighting a common clinical problem.
Evidence supporting various strategies is then presented, followed by a review of formal guidelines,
when they exist. The article ends with the authors clinical recommendations.
A healthy 37-year-old woman presents at 10 weeks of pregnancy with vaginal bleed-
ing. Physical examination shows that the uterine size is appropriate for gestational
age. The level of serum human chorionic gonadotropin (hCG) is 22,000 mIU per
milliliter. Ultrasonography does not show an identifiable fetal heartbeat. After re-
ceiving a clinical diagnosis of missed abortion, the patient undergoes evacuation of
the uterus; pathological examination indicates a complete molar pregnancy. How
should this case be managed?
The Cl inic a l Probl em
Molar pregnancy comprises two distinct entities, partial and complete mole, which From the New England Trophoblastic Dis-
can be distinguished by means of gross morphologic and histopathological exami- ease Center, Trophoblastic Tumor Regis-
try; the Division of Gynecologic Oncology,
nation and according to chromosomal pattern (Table 1).1-4 Complete moles have no Department of Obstetrics and Gynecolo-
identifiable embryonic or fetal tissues. Classically, the chorionic villi have diffuse gy, Brigham and Womens Hospital; the
trophoblastic hyperplasia and generalized swelling, and the trophoblast at the im- DanaFarber Cancer Institute; and Har-
vard Medical School all in Boston. Ad-
plantation site has diffuse, marked atypia. Complete moles usually have a 46,XX dress reprint requests to Dr. Berkowitz at
karyotype, and the molar chromosomes are derived completely from the father.5 the Division of Gynecologic Oncology,
Most complete moles are homozygous and appear to arise from an anuclear empty Brigham and Womens Hospital, 75 Francis
St., Boston, MA 02115, or at rberkowitz@
ovum that has been fertilized by a haploid (23X) sperm, which then replicates its partners.org.
own chromosomes.6 Whereas chromosomes in the complete mole have a paternal
origin, the mitochondrial DNA has a maternal origin.7 N Engl J Med 2009;360:1639-45.
Copyright 2009 Massachusetts Medical Society.
In contrast to complete moles, partial moles are characterized by the following
pathological features: chorionic villi that vary in size and are characterized by fo-
cal swelling and focal trophoblastic hyperplasia; focal, mild atypia of trophoblasts
at the implantation site; marked villous scalloping and prominent stromal tropho-
blastic inclusions; and identifiable fetal or embryonic tissues.2-4 Partial moles usu-
An audio version
ally have a triploid karyotype that develops after the fertilization of an apparently of this article
normal ovum by two spermatozoa.3 When fetuses with partial moles are identified, is available at
they usually have the congenital anomalies associated with triploidy, such as syndac- NEJM.org
tyly and cleft lip.
Complete moles once were generally diagnosed in the second trimester, and cer-
tain symptoms and signs were common at the time of presentation, including exces-
sive uterine size, anemia, toxemia, hyperemesis, hyperthyroidism, and respiratory
failure.8-11 However, the clinical presentation and pathological features of a complete
mole have changed substantially over the past two decades. In a case series of pa-
tients presenting between 1965 and 1975 at the New England Trophoblastic Disease
Center, at a mean gestational age of 16.5 weeks, the frequency of excessive uterine
size was 51%, anemia 54%, toxemia 27%, hyperemesis 26%, hyperthyroidism 7%,
and respiratory failure 2%.12
With the availability of accurate and sensitive tests for the detection of hCG and
the use of early ultrasonographic examination, the diagnosis is now typically made
n engl j med 360;16 nejm.org april 16, 2009 1639
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Table 1. Chromosomal and Histopathological Features of Complete and Partial Moles.*
Characteristic Complete Mole Partial Mole
Karyotype Diploid; 46,XX (usually), 46,XY Triploid
Results on immunostaining of maternally expressed gene Negative Positive
products (p57, PHLDA2)
Fetal or embryonic tissue Absent Present
Hydropic swelling of villi Diffuse Focal
Trophoblastic hyperplasia Diffuse Focal
Scalloping of chorionic villi Absent Present
Trophoblastic stromal inclusions Absent Present
Trophoblast at implantation site Marked atypia Mild atypia
* Data are from Berkowitz and Goldstein.1
in the first trimester, often before classic clinical ther a complete or partial mole and may require
signs and symptoms develop.12,13 For example, in chemotherapy.
a series of cases diagnosed between 1988 and
1993,12 the mean gestational age at diagnosis was S t r ategie s a nd E v idence
11.8 weeks. Excessive uterine size, anemia, tox-
emia, and hyperemesis were detected in only 28%, Diagnosis
5%, 1%, and 8% of the patients, respectively, and Ultrasonographic Examination
no patient had clinical hyperthyroidism or respi- Because a complete molar pregnancy is character-
ratory insufficiency. The incidence of vaginal bleed- ized by marked swelling of the chorionic villi, the
ing as a symptom at presentation also decreased, ultrasonographic finding of a vesicular pattern is
from 97% in the earlier case series to 84% in the strongly suggestive of the diagnosis (Fig. 1). As
later case series. compared with complete moles that are diagnosed
Patients with a partial mole usually present later, complete moles that are diagnosed in the
with the signs and symptoms of missed or incom- first trimester show less cavitation and have small-
plete abortion, including vaginal bleeding and a er villi.18 Nevertheless, ultrasonography can still
uterine size that is small or appropriate for ges- be used to detect most of these cases.19 For ex-
tational age, rather than the classic features of a ample, in one report of 24 cases of complete mole
complete mole.14-16 The symptoms and gestational in the first trimester (mean gestational age, 8.7
age at the diagnosis of a partial mole, unlike those weeks), 17 cases (71%) were correctly diagnosed on
at the diagnosis of a complete mole, have not the basis of the initial ultrasonographic examina-
changed appreciably in recent years.17 tion. Ultrasonographic findings that do not include
The pathological features of complete moles in the characteristics of a molar pregnancy are usu-
the first trimester are also less readily identifiable ally presumed to indicate a missed abortion. An
than those of complete moles in the second tri- elevated hCG level at the time of ultrasonographic
mester. One series compared the pathological examination may help to distinguish an early com-
findings in 23 complete moles diagnosed between plete mole from a missed abortion.20 However,
1994 and 1997, at a mean gestational age of 8.5 a definitive diagnosis requires confirmation by a
weeks, with 20 historic complete moles diagnosed pathologist.
between 1969 and 1975, at a mean gestational age A partial mole is also associated with charac-
of 17 weeks.18 The more recent cases, as compared teristic ultrasonographic findings21,22 (Fig. 2). Such
with the older cases, had a smaller mean maxi- findings that have been shown to be significantly
mal villous diameter (5.7 mm vs. 8.2 mm). The associated with the presence of a partial mole in-
more recent moles were also less likely to have clude focal cystic changes in the placenta and a
circumferential trophoblastic hyperplasia (39% vs. ratio of the transverse to anteroposterior dimen-
75%) and global necrosis (22% vs. 54%) and were sion of the gestational sac that is more than 1.521;
more likely to have primitive villous stroma (70% the latter finding may be related to triploidy. In
vs. 10%). Persistent neoplasia may develop in ei- one study, when both findings were noted, the
1640 n engl j med 360;16 nejm.org april 16, 2009
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
clinical pr actice
positive predictive value for a partial mole was
87%,21 although this finding has not been vali-
dated.
Measurement of hCG
Since trophoblastic cells (which produce hCG) are
hyperplastic in a molar pregnancy, the presence
of a complete mole is strongly suggested by mark-
edly elevated hCG values. Levels of hCG that were
greater than 100,000 mIU per milliliter before
evacuation were observed in 30 of 74 patients with
complete moles (41%) in one series23 and in 70 of
153 patients with complete moles (46%) who were
followed at the New England Trophoblastic Dis-
ease Center.24
As compared with complete moles, partial
moles are characterized by less prominent tropho-
blastic hyperplasia. Accordingly, patients with a Figure 1. Ultrasonographic Scan from a Patient
with a First-Trimester Complete Molar Pregnancy.
partial mole present infrequently with substan-
The scan shows diffuse vesicular changes in the pla-
tially elevated hCG levels. We reported serum hCG centa; the gestational sac is absent. (Image courtesy of
levels greater than 100,000 mIU per milliliter at Carol B. Benson, M.D., Dept. of Radiology, Brigham
presentation in only 2 of 30 patients with partial and Womens Hospital, Boston.)
moles at our center.14 Similarly, only 1 of 17 pa-
tients with a partial mole in another study was
noted to have a urinary hCG level that was greater ucts, whereas all other gestations, including partial
than 300,000 mIU per milliliter.15 moles, are characterized by nuclear immuno
staining in these cells. Thus, a complete mole is
Challenges of Pathological Diagnosis diploid and negative for p57 and PHLDA2, a hy-
The shift to earlier detection and evacuation of dropic abortion is diploid and positive for p57 and
complete moles has made the pathological diag- PHLDA2, and a partial mole is generally triploid
nosis more challenging.25 Early complete moles and positive for p57 and PHLDA2 (Table 1).
have subtle morphologic features that may lead
to their misclassification as partial moles or non- Management
molar hydropic abortions. Patients who receive a diagnosis of molar preg-
Accurate pathological diagnosis can be greatly nancy should be evaluated for potential medical
facilitated through the use of flow cytometry to complications such as anemia, toxemia, or hyper-
determine ploidy (i.e., diploid vs. triploid moles) thyroidism. All patients should undergo a com-
and through assessment of biomarkers of pater- plete physical examination and laboratory testing,
nally imprinted and maternally expressed gene including determination of the blood type and he-
products. Whereas complete moles and hydropic matocrit and evaluation of thyroid, liver, and re-
abortions are both diploid, partial moles are gen- nal function.
erally triploid. Biomarkers that take advantage of After any medical complications have been ad-
imprinted genes to distinguish complete moles dressed, a decision must be made concerning the
from other gestations have been identified. Be- best method of evacuation. Suction curettage is
cause complete moles generally have no maternal the optimal method of evacuation, regardless of
chromosomes, paternally imprinted gene prod- uterine size, in patients who wish to retain repro-
ucts, which are normally expressed only by ma- ductive function, because it carries a significantly
ternal chromosomes, should be absent.26-28 For lower risk of excessive bleeding, infection, and re-
example, in complete moles, the nuclei of the vil- tained molar tissue than methods involving in-
lous stroma and cytotrophoblastic cells do not ex- duction with oxytocin or prostaglandin.29,30 Be-
press p57 or PHLDA2 (Pleckstrin homology-like cause the RhD antigen is present in trophoblasts,
domain, family A, member 2), which are pater- patients with an Rh-negative blood type should
nally imprinted, maternally expressed gene prod- receive Rh immune globulin at the time of evacu-
n engl j med 360;16 nejm.org april 16, 2009 1641
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
At our center, after evacuation of a complete mole,
local uterine invasion was diagnosed in 15% of
patients, and metastases were diagnosed in 4% of
patients.9 Chemotherapy has been shown to be
highly effective in the treatment of both non-
metastatic and metastatic disease, with cure rates
ranging between 80 and 100%, depending on the
extent of disease.1
Certain clinical features are predictive of tu-
mors after molar pregnancy.8 Among 858 patients
with a complete mole who were followed at our
center, persistent tumor after evacuation was sig-
nificantly more likely among those with signs of
marked trophoblastic proliferation (41% of the
total cohort), including an hCG level greater than
100,000 mIU per milliliter, a uterine size that was
Figure 2. Ultrasonographic Scan from a Patient
with a First-Trimester Partial Molar Pregnancy.
larger than appropriate for gestational age, and
The scan shows focal vesicular changes in the placenta
theca lutein ovarian cysts larger than 6 cm in di-
and a fetus with a gestational sac (bottom). (Image ameter, than among those without these clinical
courtesy of Carol B. Benson, M.D., Dept. of Radiology, findings. The rate of subsequent uterine invasion
Brigham and Womens Hospital, Boston.) among patients with signs of trophoblastic pro-
liferation was 31.0%, as compared with 3.4%
among patients without these signs, and the rate
ation of the uterus. Patients who have completed of metastasis was 8.8% as compared with 0.6%.
or do not have an interest in childbearing may Therefore, patients with a complete mole who
undergo hysterectomy. Although hysterectomy pre- have markedly elevated hCG levels and an abnor-
vents the development of local invasion, it does mally large uterus before evacuation are catego-
not eliminate metastatic disease. Therefore, care- rized as being at high risk for subsequent gesta-
ful monitoring of hCG levels is still required to tional trophoblastic neoplasia.10,36
ensure that persistent neoplasia does not develop. The reported risk of the development of ges-
tational trophoblastic neoplasia after a partial
Persistent Neoplasia after a Molar molar pregnancy ranges from 0 to 11%.9 Gesta-
Pregnancy tional trophoblastic neoplasia was reported in 73
Nonmetastatic or metastatic gestational tropho- of 7155 patients with a partial mole from 10 cen-
blastic neoplasia may develop in a complete or par- ters (1.0%)37 and in 22 of 390 patients at our center
tial molar pregnancy. Nonmetastatic neoplasia (5.6%)17; in our case series, clinical symptoms at
develops when molar tissue or choriocarcinoma presentation did not distinguish patients who were
invades the uterine wall and there is no evidence at risk for persistent tumor from those who were
of disease beyond the uterus, whereas metastatic not at risk.17
disease spreads beyond the uterus. In 2002, the
International Federation of Gynecology and Ob- Monitoring of hCG after Evacuation
stetrics established new criteria for the diagnosis of the Mole
of persistent neoplasia after a molar pregnancy. After evacuation, serial hCG levels should be mon-
These criteria include serum hCG levels that do itored in patients with either a complete or par-
not return to the normal range after evacuation, tial molar pregnancy in order to facilitate the early
evidence of metastasis, and a pathological diag- detection of persistent gestational trophoblastic
nosis of choriocarcinoma, any one of which es- neoplasia. To ensure that the patient has a com-
tablishes the diagnosis of persistent neoplasia.31 plete, sustained remission, hCG tests are often per-
The incidence of gestational trophoblastic neo- formed weekly until levels have been undetectable
plasia after a complete molar pregnancy in the (<5 mIU per milliliter) for 3 weeks, with subse-
United States has been reported to be 18 to quent monthly testing until levels have been un-
29%1,10,32-34 and has not been affected by the ear- detectable for 6 months. Data from multiple cen-
lier diagnosis and treatment of complete moles.12,35 ters for several thousand women with a molar
1642 n engl j med 360;16 nejm.org april 16, 2009
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
clinical pr actice
pregnancy indicate that once the level of hCG be- disease, ultrasonographic examination is recom-
comes undetectable, recurrent elevation of the level mended in the first trimester of a subsequent
occurs in less than 1% of patients. The time of pregnancy to confirm that the pregnancy is nor-
relapse has not been specifically indicated in most mal. It is considered safe for patients to attempt
of these patients.38-46 In one series involving 4754 to conceive as soon as follow-up hCG testing has
patients with a mole, 27 (0.6%) had a relapse after been completed.
at least one hCG test indicating an undetectable
level (<5 mIU per milliliter in serum or <25 mIU A r e a s of Uncer ta in t y
per milliliter in urine).47 In eight clinical series
published since 2004, only 2 of more than 2000 The necessary period of follow-up hCG testing
patients with a molar pregnancy had persistent after evacuation of the mole remains uncertain.
tumor after serum hCG levels had become unde- The use of prophylactic chemotherapy at the time
tectable. These data suggest that it may be possible of evacuation also remains uncertain. In two ran-
to shorten the period of follow-up hCG testing domized trials, chemoprophylaxis in patients with
after evacuation of the mole without compromis- high-risk complete molar pregnancies resulted in
ing a patients safety. a significant reduction in the incidence of persis-
Because the occurrence of a new gestation tent gestational trophoblastic neoplasia (14% for
would interfere with follow-up testing of hCG both studies, vs. 47% and 50% among patients
levels, patients with a molar pregnancy are strong- who did not receive chemoprophylaxis).54,55 The
ly advised to use reliable contraception during the use of chemoprophylaxis in patients with high-
entire interval of hCG monitoring. An intrauter- risk complete moles is generally considered in cir-
ine device should not be inserted before gonado- cumstances in which follow-up hCG testing is un-
tropin remission because of the risk of perforat- available or patient compliance is a concern.
ing the uterus if tumor is present. The use of either
barrier methods of contraception or oral contra- Guidel ine s
ceptives should be recommended after evacuation.
Although limited data have suggested that the use The American College of Obstetricians and Gy-
of oral contraceptives before gonadotropin remis- necologists (ACOG) has recommended that after
sion may be associated with an increase by a fac- evacuation of a mole, serum hCG levels should be
tor of two to three in the frequency of tumor after
monitored every 1 to 2 weeks in all patients while
a molar pregnancy, as compared with the fre- the levels are elevated and then at monthly inter-
quency among women who do not use oral con vals for an additional 6 months once the levels
traceptives,48 a more recent randomized trial become undetectable (<5 mIU per milliliter).56 The
showed no increase in the risk of gestational tro-International Federation of Gynecology and Ob-
phoblastic neoplasia after molar pregnancy with stetrics has established the following guidelines
the use of these contraceptives.49 Moreover, several
for the diagnosis of persistent tumor after molar
other observational studies have likewise shown pregnancy: four or more measurements of the
no significant association between the use of oralhCG level that show a plateau in the values over
contraception and the risk of persistent tumor a period of at least 3 weeks, an increase in the
after molar pregnancy.50,51 hCG level of 10% or more in three or more mea-
surements over a period of at least 2 weeks, the
Subsequent Pregnancy presence of choriocarcinoma on histologic analy-
After a molar pregnancy, patients and their part- sis, and the persistence of detectable hCG levels
ners commonly express concern about the poten- 6 months after evacuation of a mole.33
tial for a molar pregnancy in the future.52 Case
series indicate that most patients with a molar C onclusions a nd
pregnancy who subsequently conceive will have a R ec om mendat ions
normal pregnancy, but there is an increased risk
of another molar pregnancy.53 The absolute risk The woman described in the vignette presented
that a subsequent pregnancy will be a molar preg- with signs and symptoms of first-trimester missed
nancy is about 1% after one mole and about 15 to abortion. She did not have the classic features of
18% after two moles.47,53 molar pregnancy (e.g., a uterus that is larger than
Because of the increased risk of later molar appropriate for gestational age, a marked eleva-
n engl j med 360;16 nejm.org april 16, 2009 1643
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
tion of the hCG level, and a characteristic appear- ACOG currently recommends continuation of fol-
ance of a mole on ultrasonographic examination); low-up testing for 6 months after the levels be-
this absence of findings is common now that mo- come undetectable, but the risk of recurrence once
lar pregnancy is typically diagnosed in the first the levels are undetectable is extremely low (<1%),
trimester. In cases in which the histologic findings and it is possible that this duration of follow-up
are nondiagnostic, the use of flow cytometry to could be safely abbreviated. Patients should be in-
determine ploidy (a partial mole is generally trip- structed to use reliable contraception during the
loid) and immunostaining for maternally expressed entire interval of hCG monitoring; data indicate
gene products (complete moles are negative for that the use of oral contraceptives is safe during
p57 and PHLDA2) can facilitate an accurate patho- this period. Patients should be reassured that, al-
logical diagnosis. though there is a slightly increased risk of a sub-
Suction curettage is recommended for evacu- sequent molar pregnancy after one molar preg-
ation, after which serial hCG levels should be nancy, in most cases, a subsequent pregnancy will
measured in all patients with molar pregnancy in be normal.
order to ensure a return to undetectable levels, No potential conflict of interest relevant to this article was
which are indicative of complete remission. The reported.
References
1. Berkowitz RS, Goldstein DP. Chorionic Creasman WT, Parker RT. Hydatidiform 20. Romero R, Horgan JG, Kohorn EI, Ka-
tumors. N Engl J Med 1996;335:1740-8. mole: diagnosis, management and long- dar N, Taylor KJW, Hobbins JC. New crite-
2. Szulman AE, Surti U. The syndromes term follow-up of 347 patients. Obstet ria for the diagnosis of gestational tro-
of hydatidiform mole. II. Morphologic Gynecol 1975;45:1-8. phoblastic disease. Obstet Gynecol 1985;
evolution of the complete and partial mole. 11. Kohorn EI. Molar pregnancy: presen- 66:553-8.
Am J Obstet Gynecol 1978;132:20-7. tation and diagnosis. Clin Obstet Gynecol 21. Fine C, Bundy AL, Berkowitz RS, Bos
3. Idem. The syndromes of hydatidiform 1984;27:181-91. well SB, Berezin AF, Doubilet PM. Sono-
mole. I. Cytogenetic and morphologic cor- 12. Soto-Wright V, Bernstein MR, Gold- graphic diagnosis of partial hydatidiform
relations. Am J Obstet Gynecol 1978;131: stein DP, Berkowitz RS. The changing mole. Obstet Gynecol 1989;73:414-8.
665-71. clinical presentation of complete molar 22. Naumoff P, Szulman AE, Weinstein B,
4. Montes M, Roberts D, Berkowitz RS, pregnancy. Obstet Gynecol 1995;86: Mazer J, Surti U. Ultrasonography of par-
Genest DR. Prevalence and significance 775-9. tial hydatidiform mole. Radiology 1981;
of implantation site trophoblast atypia in 13. Felemban AA, Bakri YN, Alkharif HA, 140:467-70.
hydatidiform moles and in spontaneous Altuwaijri SM, Shalhoub J, Berkowitz RS. 23. Menczer J, Modan M, Serr DM. Pro-
abortions. Am J Clin Pathol 1996;105: Complete molar pregnancy: clinical trends spective follow-up of patients with hyda-
411-6. at King Fahad Hospital, Riyadh, Kingdom tidiform mole. Obstet Gynecol 1980;55:
5. Kajii T, Ohama K. Androgenetic ori- of Saudi Arabia. J Reprod Med 1998; 346-9.
gin of hydatidiform mole. Nature 1977; 43:11-3. 24. Genest DR, Laborde O, Berkowitz RS,
268:633-4. 14. Berkowitz RS, Goldstein DP, Bern- Goldstein DP, Bernstein MR, Lage J.
6. Yamashita K, Wake N, Araki T, Ichi- stein MR. Natural history of partial molar A clinicopathologic study of 153 cases of
noe R, Makoto K. Human lymphocyte pregnancy. Obstet Gynecol 1985;66:677- complete hydatidiform mole (1980-1990):
antigen expression in hydatidiform mole: 81. histologic grade lacks prognostic signifi-
androgenesis following fertilization by a 15. Czernobilsky B, Barash A, Lancet M. cance. Obstet Gynecol 1991;78:402-9.
haploid sperm. Am J Obstet Gynecol 1979; Partial moles: a clinicopathologic study of 25. Sebire NJ, Fisher RA, Rees HC. Histo-
135:597-600. 25 cases. Obstet Gynecol 1982;59:75-7. pathological diagnosis of partial and com-
7. Azuma C, Saji F, Tokugawa Y, et al. 16. Szulman AE, Surti U. The clinico- plete hydatidiform mole in the first tri-
Application of gene amplification by poly- pathological profile of the partial hyda- mester of pregnancy. Pediatr Dev Pathol
merase chain reaction to genetic analysis tidiform mole. Obstet Gynecol 1982;59: 2003;6:69-77.
of molar mitochondrial DNA: the detec- 597-602. 26. Fukunaga M. Immunohistochemical
tion of anuclear empty ovum as the cause 17. Feltmate CM, Growdon WB, Wolfberg characterization of p57 (KIP2) expression
of complete mole. Gynecol Oncol 1991; AJ, et al. Clinical characteristics of persis- in early hydatidiform moles. Hum Pathol
40:29-33. tent gestational trophoblastic neoplasia 2002;33:1188-92.
8. The diagnosis and management of after partial hydatidiform molar preg- 27. Genest DR, Dorfman DM, Castrillon
molar pregnancy. In: Goldstein DP, Berkow- nancy. J Reprod Med 2006;51:902-6. DH. Ploidy and imprinting in hydatidi-
itz RS. Gestational trophoblastic neo- 18. Mosher R, Goldstein DP, Berkowitz form moles: complementary use of flow
plasms: clinical principles of diagnosis and RS, Bernstein MR, Genest DR. Complete cytometry and immunohistochemistry of
management. Philadelphia: Saunders, 1982: hydatidiform mole: comparison of clini- the imprinted gene product p57KIP2 to
143-75. copathologic features, current and past. assist molar classification. J Reprod Med
9. Berkowitz RS, Goldstein DP. Presen- J Reprod Med 1998;43:21-7. 2002;47:342-6.
tation and management of molar preg- 19. Benson CB, Genest DR, Bernstein 28. Thaker HM, Berlin A, Tycko B, et al.
nancy. In: Hancock BW, Newlands ES, MR, Soto-Wright V, Goldstein DP, Berkow- Immunohistochemistry for the imprinted
Berkowitz RS, eds. Gestational tropho- itz RS. Sonographic appearance of first gene product IPL/PHLDA2 for facilitating
blastic disease. London: Chapman & Hall, trimester complete hydatidiform moles. the differential diagnosis of complete hy-
1997:127-42. Ultrasound Obstet Gynecol 2000;16:188- datidiform mole. J Reprod Med 2004;
10. Curry SL, Hammond CB, Tyrey L, 91. 49:630-6.
1644 n engl j med 360;16 nejm.org april 16, 2009
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
clinical pr actice
29. Hancock BW, Tidy JA. Current man- Recurrent gestational trophoblastic dis- tional age, contraceptive method, and the
agement of molar pregnancy. J Reprod ease after hCG normalization following mode of primary treatment of patients
Med 2002;47:347-54. hydatidiform mole in The Netherlands. with hydatidiform moles on the incidence
30. Berkowitz RS, Goldstein DP, Bernstein Gynecol Oncol 2007;106:142-6. of subsequent chemotherapy. Br J Obstet
MR. Evolving concepts of molar pregnan- 40. Kerkmeijer L, Wielsma S, Bekkers R, Gynaecol 1979;86:782-92.
cy. J Reprod Med 1991;36:40-4. Pyman J, Tan J, Quinn M. Guidelines fol- 49. Curry SL, Schlareth JB, Kohorn EI, et
31. Kohorn EI. Negotiating a staging and lowing hydatidiform mole: a reappraisal. al. Hormonal contraception and tropho-
risk factor scoring system for gestational Aust N Z J Obstet Gynaecol 2006;46: blastic sequelae after hydatidiform mole
trophoblastic neoplasia: a progress report. 112-8. (a Gynecologic Oncology Group study).
J Reprod Med 2002;47:445-50. 41. Pisal N, Tidy J, Hancock B. Gestation- Am J Obstet Gynecol 1989;160:805-11.
32. Idem. Hydatidiform mole and gesta- al trophoblastic disease: is intensive fol- 50. Berkowitz RS, Goldstein DP, Marean
tional trophoblastic disease in Southern low up essential in all women? BJOG AR, Bernstein M. Oral contraceptives and
Connecticut. Obstet Gynecol 1982;59:78- 2004;111:1449-51. postmolar trophoblastic disease. Obstet
84. 42. Wielsma S, Kerkmeijer L, Bekkers R, Gynecol 1981;58:474-7.
33. Lurain JR, Brewer JI, Torok EE, Hal Pyman J, Tan J, Quinn M. Persistent tro- 51. Costa HLFF, Doyle P. Influence of oral
pern B. Natural history of hydatidiform phoblastic disease following partial mo- contraceptives in the development of post-
mole after primary evacuation. Am J Ob- lar pregnancy. Aust N Z J Obstet Gynaecol molar trophoblastic neoplasia a system-
stet Gynecol 1983;145:591-5. 2006;46:119-23. atic review. Gynecol Oncol 2006;100:579-
34. Morrow CP, Kletzky OA, DiSaia PJ, 43. Batorfi J, Vegh G, Szepesi J, Szigetvari 85.
Townsend DE, Mishell DR, Nakamura RM. I, Doszpod J, Fulop V. How long should 52. Wenzel L, Berkowitz R, Robinson S,
Clinical and laboratory correlates of mo- patients be followed after molar pregnan- Bernstein MR, Goldstein D. The psycho-
lar pregnancy and trophoblastic disease. cy? Analysis of serum hCG follow-up data. logical, social, and sexual consequences
Am J Obstet Gynecol 1977;128:424-30. Eur J Obstet Gynecol Reprod Biol 2004; of gestational trophoblastic disease. Gy-
35. Paradinas FJ, Browne P, Fisher RA, 112:95-7. necol Oncol 1992;46:74-81.
Foskett M, Bagshawe KD, Newlands E. 44. Wolfberg AJ, Feltmate C, Goldstein 53. Garrett LA, Garner EI, Feltmate CM,
A clinical, histopathologic and flow cyto- DP, Berkowitz RS, Lieberman E. Low risk Goldstein DP, Berkowitz RS. Subsequent
metric study of 149 complete moles, 146 of relapse after achieving undetectable pregnancy outcomes in patients with mo-
partial moles and 107 non-molar hydropic hCG levels in women with complete mo- lar pregnancy and persistent gestational
abortions. Histopathology 1996;28:101-10. lar pregnancy. Obstet Gynecol 2004;104: trophoblastic neoplasia. J Reprod Med
36. Morrow CP. Postmolar trophoblastic 551-4. 2008;53:481-6.
disease: diagnosis, management, and prog- 45. Wolfberg AJ, Growdon WB, Feltmate 54. Kim DS, Moon H, Kim KT, Moon YJ,
nosis. Clin Obstet Gynecol 1984;27:211-20. CM, et al. Low risk of relapse after achiev- Hwang YY. Effects of prophylactic chemo-
37. Hancock BW, Nazir K, Everard JE. ing undetectable hCG levels in women therapy for persistent trophoblastic disease
Persistent gestational trophoblastic neo- with partial molar pregnancy. Obstet Gy- in patients with complete hydatidiform
plasia after partial hydatidiform mole: in- necol 2006;108:393-6. mole. Obstet Gynecol 1986;67:690-4.
cidence and outcome. J Reprod Med 2006; 46. Lavie I, Rao GG, Castrillon DH, Miller 55. Limpongsanurak S. Prophylactic ac-
51:764-6. DS, Schorge JO. Duration of human chori- tinomycin D for high-risk complete hyda-
38. Feltmate CM, Bartorfi J, Fulop V, onic gonadotropin surveillance for partial tidiform mole. J Reprod Med 2001;46:
Goldstein DP, Doszpod J, Berkowitz RS. hydatidiform moles. Am J Obstet Gynecol 110-6.
Human chorionic gonadotropin follow-up 2005;192:1362-4. 56. Soper JT, Mutch DG, Schink JC. Diag-
in patients with molar pregnancy: a time 47. Bagshawe KD, Dent J, Webb J. Hyda- nosis and treatment of gestational tropho-
for reevaluation. Obstet Gynecol 2003; tidiform mole in England and Wales blastic disease: ACOG Practice Bulletin
101:732-6. 1973-1983. Lancet 1986;2:673-7. No. 53. Gynecol Oncol 2004;93:575-85.
39. Kerkmeijer LGW, Wielsma S, Mas- 48. Stone M, Bagshawe KD. An analysis Copyright 2009 Massachusetts Medical Society.
suger LFAG, Sweep FCGJ, Thomas CMG. of the influences of maternal age, gesta-
personal archives in the journal online
Individual subscribers can store articles and searches using a feature
on the Journals Web site (NEJM.org) called Personal Archive.
Each article and search result links to this feature. Users can create
personal folders and move articles into them for convenient retrieval later.
n engl j med 360;16 nejm.org april 16, 2009 1645
The New England Journal of Medicine
Downloaded from nejm.org at Arizona Health Sciences Center and UMC on May 15, 2013. For personal use only. No other uses without permission.
Copyright 2009 Massachusetts Medical Society. All rights reserved.
Das könnte Ihnen auch gefallen
- Fenotipos Sepsis 5 PDFDokument16 SeitenFenotipos Sepsis 5 PDFGerardo LermaNoch keine Bewertungen
- Treatment Implications of Novel Clinical Phenotypes For Sepsis PDFDokument2 SeitenTreatment Implications of Novel Clinical Phenotypes For Sepsis PDFGerardo LermaNoch keine Bewertungen
- Fenotipos Sepsis 3Dokument5 SeitenFenotipos Sepsis 3Gerardo LermaNoch keine Bewertungen
- Gibson 2018Dokument10 SeitenGibson 2018Gerardo LermaNoch keine Bewertungen
- s13054 019 2655 7 PDFDokument9 Seitens13054 019 2655 7 PDFjenaro heli Ardila CortesNoch keine Bewertungen
- Sepsis and ShockDokument13 SeitenSepsis and ShockUther Pendragon100% (2)
- Fenotipos Sepsis 1 PDFDokument2 SeitenFenotipos Sepsis 1 PDFGerardo LermaNoch keine Bewertungen
- 10 1001@jama 2019Dokument15 Seiten10 1001@jama 2019Liliam GonzalezNoch keine Bewertungen
- Fenotipos Sepsis 3Dokument5 SeitenFenotipos Sepsis 3Gerardo LermaNoch keine Bewertungen
- AOAStudy 2018Dokument26 SeitenAOAStudy 2018Gerardo Lerma100% (1)
- Acute Respiratory Distress Syndrome NEJM 2018Dokument11 SeitenAcute Respiratory Distress Syndrome NEJM 2018darlingcarvajalduqueNoch keine Bewertungen
- Anxiety LancetDokument12 SeitenAnxiety LancetAnonymous B9zv0Y100% (1)
- 13958054684195Dokument13 Seiten13958054684195Chairul Nurdin AzaliNoch keine Bewertungen
- ARDSnet Ventilation Protocol SummaryDokument2 SeitenARDSnet Ventilation Protocol SummaryvbfisioNoch keine Bewertungen
- Enfermedades de Transmision SexualDokument45 SeitenEnfermedades de Transmision SexualGerardo LermaNoch keine Bewertungen
- Pas PDFDokument8 SeitenPas PDFRoxi_137Noch keine Bewertungen
- Artritis ReumatoideDokument9 SeitenArtritis ReumatoideGerardo Lerma BurciagaNoch keine Bewertungen
- Trombotic MicroangyopathyDokument13 SeitenTrombotic MicroangyopathyGerardo LermaNoch keine Bewertungen
- Study Guide PlannerDokument6 SeitenStudy Guide PlannerGerardo LermaNoch keine Bewertungen
- ABIM DetalladoDokument52 SeitenABIM DetalladoGerardo LermaNoch keine Bewertungen
- Abim Certificacion Examination BlueprintDokument28 SeitenAbim Certificacion Examination BlueprintGerardo LermaNoch keine Bewertungen
- Picmonic Step 1 Study Guide 2016Dokument32 SeitenPicmonic Step 1 Study Guide 2016bisharat50% (2)
- FIGO Clasificación HUA 2011Dokument11 SeitenFIGO Clasificación HUA 2011dickenskevinNoch keine Bewertungen
- UnderstandingPathophysiology2E 9780729541602 CraftGordon Samplechapter Web PDFDokument38 SeitenUnderstandingPathophysiology2E 9780729541602 CraftGordon Samplechapter Web PDFGerardo Lerma0% (4)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (119)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- HL Topic 11.4 ReproductionDokument6 SeitenHL Topic 11.4 ReproductionAnonymous iIj7YGNoch keine Bewertungen
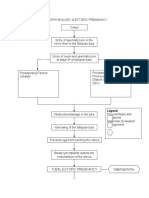
- PATHOPHYSIOLOGY of ECTOPIC PREGNANCYDokument2 SeitenPATHOPHYSIOLOGY of ECTOPIC PREGNANCYrye100% (1)
- The Occult Forces of Sexual UnionDokument6 SeitenThe Occult Forces of Sexual Unionimmortality2045_841960% (5)
- Plant Propagation Lab ActivityDokument2 SeitenPlant Propagation Lab ActivityClint Jhun TabugocNoch keine Bewertungen
- Characteristics of Living Things Guided NotesDokument3 SeitenCharacteristics of Living Things Guided NotesErica HartNoch keine Bewertungen
- NCERT Biology Reproductive Health FactsDokument5 SeitenNCERT Biology Reproductive Health FactsNishtha Jain100% (1)
- Assessing Male Genitalia and InguinalDokument51 SeitenAssessing Male Genitalia and InguinalJellaiza QuiozonNoch keine Bewertungen
- Introduction To Life ScienceDokument24 SeitenIntroduction To Life ScienceCharlize Marie Dula-ogonNoch keine Bewertungen
- R1 Symptoms and Diagnosis of PregnancyDokument49 SeitenR1 Symptoms and Diagnosis of PregnancyMoges desaleNoch keine Bewertungen
- Sexual Reproduction in Flowering Plants QuestionsDokument11 SeitenSexual Reproduction in Flowering Plants QuestionsAjayNoch keine Bewertungen
- 9700 m16 QP 42 PDFDokument28 Seiten9700 m16 QP 42 PDFAtef Ibrahim KhalifaNoch keine Bewertungen
- Veterinaria Medika Vol 7, No. 2, Juli 2014Dokument8 SeitenVeterinaria Medika Vol 7, No. 2, Juli 2014Ergha TriadyNoch keine Bewertungen
- Floral Formula: BotanyDokument7 SeitenFloral Formula: BotanyzedoksNoch keine Bewertungen
- 57-1-1 BiologyDokument15 Seiten57-1-1 BiologyRavneet KaurNoch keine Bewertungen
- BIO 3:plant ClassificationDokument5 SeitenBIO 3:plant ClassificationTers MedinaNoch keine Bewertungen
- Reproductive Character of The Ricefield EelDokument14 SeitenReproductive Character of The Ricefield EelnesaNoch keine Bewertungen
- Mode of ReproductionDokument33 SeitenMode of ReproductionMd. Rayhan Ali RejviNoch keine Bewertungen
- National Public School: SUBJECT-Science (10 (Pre Board Examination)Dokument2 SeitenNational Public School: SUBJECT-Science (10 (Pre Board Examination)amit kumarNoch keine Bewertungen
- J5-6 Lesson 10 - Meiosis StudentDokument3 SeitenJ5-6 Lesson 10 - Meiosis Studentkristhel ann caringal reyes0% (1)
- Week 5 Worksheet AnswersDokument5 SeitenWeek 5 Worksheet AnswersaskldhfdasjkNoch keine Bewertungen
- Question Paper Unit A161 02 Modules b1 b2 b3 Higher TierDokument16 SeitenQuestion Paper Unit A161 02 Modules b1 b2 b3 Higher TierAnonymous QFkCS837bNoch keine Bewertungen
- Teaching and Learning Module KSSR (Semakan 2017) Science Year 6Dokument116 SeitenTeaching and Learning Module KSSR (Semakan 2017) Science Year 6LING KUOK LIMNoch keine Bewertungen
- 1-Embryonic-Stem-Cells 1ST LECDokument31 Seiten1-Embryonic-Stem-Cells 1ST LECrihamazim2018Noch keine Bewertungen
- Bio 10th - How Do Organism Reproduce - Revision WorksheetDokument10 SeitenBio 10th - How Do Organism Reproduce - Revision WorksheetDharmendra SinghNoch keine Bewertungen
- A Quick Overview of Genetic Engineering and EctoDokument1 SeiteA Quick Overview of Genetic Engineering and EctoHannah Grace AquinoNoch keine Bewertungen
- Contoh PDFDokument12 SeitenContoh PDFGratiano TelaumbanuaNoch keine Bewertungen
- Lesson Plan For Final DemoDokument9 SeitenLesson Plan For Final DemoJunjun Caoli50% (2)
- Hydatidiform MoleDokument2 SeitenHydatidiform MoleIrfan HardiNoch keine Bewertungen
- Revision Notes Class 8 Science Chapter 10 - Reaching The Age of AdolescenceDokument2 SeitenRevision Notes Class 8 Science Chapter 10 - Reaching The Age of AdolescenceArpit SharmaNoch keine Bewertungen
- Pregnancy - Anatomy and PhysiologyDokument5 SeitenPregnancy - Anatomy and PhysiologyNiSCHENoch keine Bewertungen