Beruflich Dokumente
Kultur Dokumente
K7121 Leishmania 2016-06-10 GB PDF
Hochgeladen von
Enrique S OcampoOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
K7121 Leishmania 2016-06-10 GB PDF
Hochgeladen von
Enrique S OcampoCopyright:
Verfügbare Formate
RIDASCREEN Leishmania Ab
Article no: K7121
R-Biopharm AG, An der neuen Bergstrae 17, D-64297 Darmstadt, Germany
Phone: +49 (0) 6151 8102-0 / Fax: +49 (0) 6151 8102-20
1. Intended use
For in vitro diagnostic use. The RIDASCREEN Leishmania Ab Test is an enzyme
immunoassay for the qualitative determination of specific IgG antibodies against Leishmania
infantum in human serum.
The test should be used for confirmation purposes when there is a suspected case of
Leishmaniasis.
2. Summary and explanation of the test
After infection with Leishmania, specific antibodies are formed against the pathogen because of
the response from the immune system. By using immunological methods, it is possible to
determine the antibodies in the serum. The test method used and the choice of the pathogen-
specific antigen both have a significant bearing on the meaningfulness of the test.
3. Test principle
Purified antigens are coated to a microwell plate. Antibodies in the patient samples bind to the
antigens and are determined during the second incubation step by using enzyme-labelled anti-
human antibodies (the conjugate). The enzyme converts the colourless substrate (urea
peroxide/TMB) to a blue end product. The enzyme reaction is stopped by adding sulphuric acid
and the colour of the mixture switches from blue to yellow at the same time. The final
measurement is carried out at 450 nm on a photometer using a reference wavelength 620 nm.
RIDASCREEN Leishmania Ab 2016-06-10 2
4. Reagents provided
There are enough reagents in the kit for 96 determinations.
Plate 96 det. Microwell plate, 12 microwell strips (can be divided) in strip holder;
coated with antigens from Leishmania infantum
Diluent 100 ml Sample buffer, phosphate-buffered NaCl solution, ready for use
SeroWP 100 ml Wash buffer, 10-fold concentrate; tris-buffered NaCl solution
Control + 1.2 ml IgG positive control, human serum, ready for use;
red lid
Control - 2.5 ml IgG negative control, human serum, ready for use;
colourless lid
Conjugate 12 ml anti-human IgG conjugate, ready for use;
orange lid peroxidase conjugated anti-human IgG conjugate in stabilized
protein solution
SeroSC 12 ml Substrate
H2O2/tetramethylbenzidine; ready for use
Stop 12 ml Stop reagent
0.5 M sulphuric acid; ready for use
Details of hazardous substances according to labeling obligations. For more details see Material
Safety Data Sheets (MSDS) at www.r-biopharm.com.
5. Storage instructions
The test kit must be stored at 2 8 C and can be used until the expiry date printed on the label.
The diluted wash buffer can be used for a maximum of 4 weeks when stored at 2 8 C or for
5 days when stored at room temperature (20 25 C). After the expiry date, the quality
guarantee is no longer valid.
The aluminium bag containing the microwell plate must be opened in such a way that the clip
seal is not torn off. Any microwell strips which are not required must be stored in the aluminium
bag.
The reagents must not be allowed to become contaminated and the colourless substrate must
be protected from exposure to direct light.
RIDASCREEN Leishmania Ab 2016-06-10 3
6. Materials required but not provided
6.1. Reagents
distilled or deionised water
6.2. Accessories
Test tubes
Vortex mixer
Micropipettes for 10-100 l and 100-1000 l capacities
Measuring cylinder (1000 ml)
Stop clock
Microplate washer or multichannel pipette
Microplate reader (450 nm, reference wavelength 620 nm)
Filter paper (laboratory towels)
Waste container containing 0.5 % hypochlorite solution
7. Precautions for users
For in vitro diagnostic use only.
This test must only be carried out by trained laboratory personnel. The guidelines for working in
medical laboratories have to be followed. The instruction manual for the test procedure has to
be followed. Do not pipet samples or reagents by mouth. Avoid contact with bruised skin or
mucosal membranes. During handling reagents or samples, wear appropriate safety clothing
(appropriate gloves, lab coat, safety goggles) and wash your hands after finishing the test
procedure. Do not smoke, eat or drink in areas where samples or reagents are being used.
For more details see Material Safety Data Sheets (MSDS) at www.r-biopharm.com.
The control sera (positive control and negative control) in the kit have been tested for HIV- and
HCV-Ab as well as HbsAg with negative results. Nevertheless, they must be treated as poten-
tially infectious in the same way as the patient samples and all other materials with which they
come into contact and they must be handled in accordance with the relevant national safety
regulations.
All reagents and materials used have to be disposed properly after use. Please refer to the
relevant national regulations for disposal.
RIDASCREEN Leishmania Ab 2016-06-10 4
8. Specimen collection and storage
The test has been developed for testing human serum samples. After blood collection, the blood
should be separated from blood clots as soon as possible in order to prevent haemolysis. The
samples must be stored cold or frozen until they are tested. Repeated freezing and thawing of
the samples and microbial contamination must be prevented at all costs. Using heat-inactivated,
lipaemic, haemolytic, icteric or turbid samples can lead to false results.
Table 1: Sample storage
Undiluted serum Diluted serum
2 8 C -20 C 2 8 C
1 week >1 week 7 hours
9. Test procedure
9.1. General information
All reagents and the microwell plate must be brought to room temperature (20 25 C) before
use. The microwell strips must not be removed from the aluminium bag until they have reached
room temperature. The reagents must be thoroughly mixed immediately before use. After use,
the kit must be immediately returned to storage between 2 and 8 C.
Take only the volume of reagents that is needed for test procedure. Do not pour reagents back
into vials as reagent contamination may occur. Do not pour reagents back into vials as this may
lead to reagent contamination.
The microwell strips cannot be used more than once. The reagents and microwell strips must
not be used if the packaging is damaged or the vials are leaking.
The wash buffer, sample buffer, stop reagent and substrate are not test specific; they can also
be used for other RIDASCREEN ELISA for determining antibodies against parasites.
9.2. Preparing the wash buffer
1 part wash buffer concentrate SeroWP is mixed with 9 parts distilled water. In order to do this,
place 100 ml of the concentrate in a 1000 ml measuring cylinder and make up the solution to
1000 ml with distilled water. Any crystals present in the concentrate must be dissolved before-
hand by warming in a water bath at 37 C. The diluted buffer can be used for a maximum of 4
weeks provided it is stored at 2 8 C or for 5 days when stored at room temperature
(20 25 C).
RIDASCREEN Leishmania Ab 2016-06-10 5
9.3. Preparing the samples
Dilute the serum samples to be tested with sample buffer Diluent 1:50 before starting the test.
e.g. 10 l Serum +490 l Diluent
Note:
The negative control and positive control are ready for use and must NOT be diluted.
9.4. First incubation
After inserting a sufficient number of wells in the frame, pipette 100 l diluted sera and ready-to-
use controls Control - and Control + into each of the corresponding wells and incubate at
room temperature (20-25C) for 15 minutes. We recommend that you carry out the negative
control Control - in duplicate.
9.5. Washing
The wells must be emptied into a waste container containing hypochlorite solution for disinfec-
tion. After this, knock out the plate onto absorbent paper in order to remove the residual mois-
ture. After this, wash the plate 5 times using 300 l wash buffer each time. Make sure that the
wells are emptied completely by knocking them out on an unused part of the absorbent paper
after each wash.
When using a microplate washer, make sure that the machine is correctly adjusted to the
type of plate being used. After washing, tap the plate upside down against clean
absorbent paper in order to remove any residual liquid.
9.6. Second incubation
Add 100 l of the anti-human IgG conjugate Conjugate to each well. Then incubate the plate at
room temperature (20 25 C) for 15 minutes.
9.7. Washing
Wash 5 times in accordance with Section 9.5.
9.8. Third incubation
Place 100 l substrate SeroSC to each well. Then incubate the plate at room temperature (20
25 C) for 15 minutes. After this, stop the reaction by adding 50 l stop reagent Stop to each
well.
RIDASCREEN Leishmania Ab 2016-06-10 6
10. Quality control indications of instability or deterioration
For quality control purposes, the positive control and the negative control (in duplicate) must be
used every time the test is carried out. The test has been carried out correctly if the average
extinction of the negative control at 450 nm is smaller than 0.3. If the two individual
measurements deviate from the average by more than 25 %, the test must be repeated. The
extinction for the positive control at 450 nm must be greater than 0.8.
If the values differ from those required, if the substrate is turbid or has turned blue before adding
to the wells, it may indicate that the reagents have expired.
If the stipulated values are not met, the following points must be checked before repeating the
test:
Expiry date of the reagents used
Functionality of the equipment being used (e.g. calibration)
Correct test procedure
Visual inspection of the kit components for contamination or leaks a substrate solution
which has turned blue must not be used.
If the conditions are still not fulfilled after repeating the test, please contact your local
R-Biopharm distributor.
11. Evaluation and interpretation
11.1. Calculating the sample index
1. The average absorbance is calculated for the negative control.
2. 0.150 is added to the average absorbance. This yields the cut-off for the test.
3. The sample index is obtained by dividing the absorbance for the sample by the cut-off.
For example: Negative control 1 O.D. = 0.115
Negative control 2 O.D. = 0.125
Sample O.D. = 0.508
0.115 + 0.125
cut-off = 2 + 0.150 = 0.270
0.508
Sample index = 0.270 = 1.88
RIDASCREEN Leishmania Ab 2016-06-10 7
11.2. Test result
Table 2: Evaluating the sample index
negative equivocal positive
Sample index < 0.9 0.9 1.1 > 1.1
12. Limitations of the method
The RIDASCREEN Leishmania Ab enzyme immunoassay determines specific IgG antibodies
against Leishmania infantum and should be carried out in cases of suspected Leishmaniasis.
The results obtained must always be interpreted in combination with the clinical picture and
other diagnostic findings.
Antibody signals are dependent on the localisation of the parasitosis and may vary from patient
to patient.
Equivocal and weakly positive results may be produced in the following cases:
- persons who have been stung by infected phlebotomae (sand flies) in regions where the
disease is endemic and produce low antibody titres without manifestation of the infection
- persons, who have recovered from or just recovered from an asymptomatic infection so that
they are still producing low antibody titres
- persons, who have suffered from the illness in the past and still produce residual titres
- persons in the early stages of the disease
- factors which are non-identifiable and non-specific
These cases should be re-examined by testing another sample, by considering the clinical
symptoms and by other diagnostic methods. In the absence of any other exact diagnosis, the
test should be repeated after two to four weeks with a new sample.
Medium and high positive results can be produced with persons who have suffered from the
acute illness or have just recently suffered from the illness. Even higher antibody titres may be
produced after longer infections which have occurred in the past. In cases which are not clear,
the result must be interpreted in the light of the case history, clinical symptoms and other
diagnostic methods.
A negative result does not necessarily rule out Leishmaniasis. During the early stages of the
infection, the number of antibodies may be so small that the test yields a negative result. If
Leishmaniasis is suspected on the basis of the case history, another serum sample should be
tested after four weeks.
RIDASCREEN Leishmania Ab 2016-06-10 8
A cross reaction with serums containing antibodies against T. cruzi (Chagas disease) have
been observed in some cases in South America. This must be taken into consideration when
carrying out the test in areas of South America where Chagas disease is endemic.
A positive result does not rule out the presence of another infectious pathogen.
13. Performance characteristics
Table 3: Inter-assay variation (n = 30)
Inter-assay variation IgG
index CV
Serum 1 4.82 10.7 %
Serum 2 2.13 17.1 %
Serum 3 1.90 22.0 %
Serum 4 0.15 n/a
Table 4: Intra-assay variation (n = 23)
Intra-assay variation IgG
index CV
Serum 1 3.57 11.2 %
Serum 2 2.14 14.0 %
Serum 3 1.27 15.1 %
Serum 4 0.15 n/a
Table 5: Sensitivity and specificity in comparison with one other commercial ELISA
IgG
Sensitivity 87.5%
Specificity 98.5%
RIDASCREEN Leishmania Ab 2016-06-10 9
Table 6: Results from testing 200 blood-donor sera taken from a blood donor centre in Germany
negative equivocal positive
200 blood donor sera 99.5% 0.5% 0.0%
RIDASCREEN Leishmania Ab 2016-06-10 10
References
1. Bray, R.S. and Lainson, R., Trans. Roy. Soc. Trop. Med. Hyg., 60, 605-609 (1966).
2. Bray, R.S. and Lainson, R., Trans. Roy. Soc. Trop. Med. Hyg., 61, 490-505 (1967).
3. Bray, R.S., Ecol. Dis., 4, 257-267 (1982).
4. Hommel, M., Peters, W., Ranque, J., Quilici, M. and Lanotte, G., Ann. Trop. Med.
Parasitol., 72, 213-218 (1978).
5. Kager, P.A., Rees, P.H., Wellde, B.T., Hockmeyer, W.T. and Lyerly, W.H., Trans. R. Soc.
Trop. Med. Hyg., 75, 556-559 (1981).
6. Lainson, R., Trans. Roy. Soc. Trop. Med. Hyg., 77, 569-596 (1983).
7. Low-A-Chee, R.M., Rose, P. and Ridley, D.S., Ann. Trop. Med. Parasitol., 77, 255-260
(1986).
8. Ranque, J. and Quilici, M., Journal of Parasitology, 56, 277-278 (1970).
RIDASCREEN Leishmania Ab 2016-06-10 11
Das könnte Ihnen auch gefallen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Ultrasound: Oxford Huntleigh Toco TransducerDokument1 SeiteUltrasound: Oxford Huntleigh Toco TransducerEnrique S OcampoNoch keine Bewertungen
- Equipo Oftalmico A1 PDFDokument188 SeitenEquipo Oftalmico A1 PDFEnrique S OcampoNoch keine Bewertungen
- Bateria PHILIPSDokument1 SeiteBateria PHILIPSEnrique S OcampoNoch keine Bewertungen
- Ecografo Pro PDFDokument174 SeitenEcografo Pro PDFEnrique S Ocampo100% (1)
- Equipo Oftalmico A1 PDFDokument188 SeitenEquipo Oftalmico A1 PDFEnrique S OcampoNoch keine Bewertungen
- Ep - NT: Operator ManualDokument23 SeitenEp - NT: Operator ManualEnrique S OcampoNoch keine Bewertungen
- Ecografo Pro PDFDokument174 SeitenEcografo Pro PDFEnrique S Ocampo100% (1)
- Audio MetroDokument64 SeitenAudio MetroEnrique S OcampoNoch keine Bewertungen
- Safety Data Sheet Eucoclean Organic Insect Spray: IdentificationDokument5 SeitenSafety Data Sheet Eucoclean Organic Insect Spray: IdentificationEnrique S OcampoNoch keine Bewertungen
- Equipo de Signos VitalesDokument2 SeitenEquipo de Signos VitalesEnrique S OcampoNoch keine Bewertungen
- Manual Servicio EcografoDokument59 SeitenManual Servicio EcografoEnrique S OcampoNoch keine Bewertungen
- Papillotomes - 3 Lumen: SliderDokument1 SeitePapillotomes - 3 Lumen: SliderEnrique S OcampoNoch keine Bewertungen
- Chlamydia TrachomatisDokument12 SeitenChlamydia TrachomatisEnrique S OcampoNoch keine Bewertungen
- NP7004 RIDAQUICK Malaria Control 2016-09-02 - GB PDFDokument1 SeiteNP7004 RIDAQUICK Malaria Control 2016-09-02 - GB PDFEnrique S OcampoNoch keine Bewertungen
- Applicator UseDokument2 SeitenApplicator UseEnrique S Ocampo100% (1)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
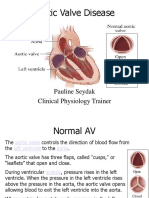
- Aortic Valve DiseaseDokument25 SeitenAortic Valve Diseasesagungw93Noch keine Bewertungen
- Indices / Orthodontic Courses by Indian Dental AcademyDokument77 SeitenIndices / Orthodontic Courses by Indian Dental Academyindian dental academyNoch keine Bewertungen
- Acute BronchitisDokument25 SeitenAcute BronchitisCherish Panopio RoadillaNoch keine Bewertungen
- Hera Factsheet Health-Threat MCMDokument2 SeitenHera Factsheet Health-Threat MCM周一行Noch keine Bewertungen
- Issues and Challenges Encountered Related To Training by The Student-Athletes of Arellano University During Pandemic PeriodDokument4 SeitenIssues and Challenges Encountered Related To Training by The Student-Athletes of Arellano University During Pandemic PeriodCarl LewisNoch keine Bewertungen
- MSF 2020 Annual Report WebDokument62 SeitenMSF 2020 Annual Report WebDoctors Without Borders/Médecins Sans FrontièresNoch keine Bewertungen
- C B C I: Omplete Lood Ount NterpretationsDokument44 SeitenC B C I: Omplete Lood Ount NterpretationsridhoniNoch keine Bewertungen
- ARDS PathophysiologyDokument2 SeitenARDS PathophysiologyIntanAgustiFernandesNoch keine Bewertungen
- Clostridium Botulinum - Ecology and Control in Foods (1993)Dokument762 SeitenClostridium Botulinum - Ecology and Control in Foods (1993)RhynoHD100% (1)
- The Pathophysiology of LabyrinthitisDokument2 SeitenThe Pathophysiology of LabyrinthitisSurya Michael ChanceNoch keine Bewertungen
- Mozart Causes of DeathDokument16 SeitenMozart Causes of DeathlucienkarhausenNoch keine Bewertungen
- The Black Death-SourceworkDokument5 SeitenThe Black Death-SourceworkMartinaNoch keine Bewertungen
- Diseases of NeonatesDokument8 SeitenDiseases of NeonatesSantosh BhandariNoch keine Bewertungen
- NCP To NG PneumoniaDokument3 SeitenNCP To NG PneumoniaGlenn Asuncion PagaduanNoch keine Bewertungen
- A Fascinating Story of Exploding Toads and Clever CrowsDokument2 SeitenA Fascinating Story of Exploding Toads and Clever CrowsDirham RevolusionerNoch keine Bewertungen
- Skin LesionsDokument7 SeitenSkin LesionsAndreitaFernandezNoch keine Bewertungen
- Pen - Udara Dalam RuangDokument26 SeitenPen - Udara Dalam RuangFaradina Shefa AuliaNoch keine Bewertungen
- Aseptic TechniqueDokument3 SeitenAseptic TechniqueAndreea FloryNoch keine Bewertungen
- Fromlackofbeds Toriseinpoverty, Housepanelflags CovidconcernsDokument16 SeitenFromlackofbeds Toriseinpoverty, Housepanelflags Covidconcernsshivam srivastavaNoch keine Bewertungen
- Home Remedies Using Mustard Seeds Prophet666Dokument2 SeitenHome Remedies Using Mustard Seeds Prophet666Hussainz AliNoch keine Bewertungen
- Donovania GranulomatisDokument22 SeitenDonovania Granulomatistummalapalli venkateswara raoNoch keine Bewertungen
- Standard Surgical Attire Surgical ScrubDokument20 SeitenStandard Surgical Attire Surgical ScrubzekkipianoNoch keine Bewertungen
- LKPD Reading New ItemDokument4 SeitenLKPD Reading New ItemM. Feri afriantoNoch keine Bewertungen
- 11Dokument3 Seiten11faresaltaii100% (2)
- Proefschrift Helma RuijsDokument102 SeitenProefschrift Helma RuijsdevijfdedagNoch keine Bewertungen
- Enhanced Strategy: Department of Health, PhilippinesDokument28 SeitenEnhanced Strategy: Department of Health, PhilippinesEduard Espeso Chiong-Gandul Jr.Noch keine Bewertungen
- Health Teaching HygieneDokument6 SeitenHealth Teaching HygieneMonette Abalos MendovaNoch keine Bewertungen
- Automatic Hand Sanitizer MachineDokument6 SeitenAutomatic Hand Sanitizer MachineBhumika J PawarNoch keine Bewertungen
- Bulletin of Animal Health and Production PDFDokument262 SeitenBulletin of Animal Health and Production PDFMarcelo Anibal AlvarezNoch keine Bewertungen
- Organization Sign On Letter Demanding SRHD TransparencyDokument7 SeitenOrganization Sign On Letter Demanding SRHD TransparencyErin RobinsonNoch keine Bewertungen