Beruflich Dokumente
Kultur Dokumente
Anterior Cervical Discectomy
Hochgeladen von
Gabriela MacoveanuOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Anterior Cervical Discectomy
Hochgeladen von
Gabriela MacoveanuCopyright:
Verfügbare Formate
Anterior Cervical Discectomy
Volker K.H. Sonntag, M.D., Patrick P. Han, M.D.,
A. Giancarlo Vishteh, M.D.
Division of Neurological Surgery, Barrow Neurological Institute, St. Joseph’s Hospital
and Medical Center, Phoenix, Arizona
A
nterior cervical discectomy is performed for a variety
of reasons. The most common is a degenerative disease
that induces an osteophyte or a herniated nucleus pul-
posus that then causes radiculopathy or myelopathy (1, 3).
The operation is usually straightforward but has multiple
pitfalls and nuances (2). This article presents the senior au-
thor’s (VKHS’s) surgical technique for anterior cervical disc-
ectomy. Once conservative treatment for cervical radiculopa-
thy, myelopathy, or both, has failed, surgical intervention is
indicated. Depending on the location of the compression, the
amount of axial pain, and the lordosis of the cervical spine, an
anterior or posterior approach is used. The anterior approach
for a single-level discectomy is described below.
In the operating room, the patient must not be hyperex-
tended during intubation. Somatosensory evoked potentials
are routinely monitored. The patient is placed supine with the
neck slightly hyperextended. The head is not turned. The
Caspar operating table attachment is used to help visualize
the lower cervical spine on either plain radiographs or fluo-
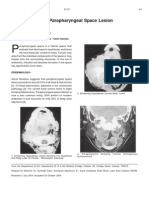
FIGURE 1. Patient positioning with the Caspar headholder.
roscopy. The Caspar table attachment also allows slight hy-
The patient’s head is maintained in a neutral position with an
perextension of the neck. The neck bar is placed under the
elastic chin strap. The cervical spine is maintained in either a
lower cervical and upper thoracic areas to avoid undue pres-
neutral or a minimally extended posture to recreate the cer-
sure on the cervical spine (Fig. 1).
vical lordosis. Adhesive tape is run along the lateral margin
of the shoulder joint and arm and is affixed to the foot of the
SURGICAL APPROACH (see video at web bed to assist with intraoperative fluoroscopic visualization of
site article) the distal cervical spine. To avoid a pressure injury to the
brachial plexus, the tape should not be run directly over the
Superficial landmarks serve as the reference points to de-
clavicle. An intrascapular roll is placed to facilitate operative
termine the level of the skin incision, but intraoperative ra-
access by allowing the shoulders to fall below the coronal
diographs or fluoroscopic studies are obtained to verify the
plane of the cervical spine. The neck bar is placed under the
level. The cervical spine is approached from the right side
upper thoracic spine. Both the scalp leads for evoked poten-
unless the patient has undergone a prior approach from the
tial monitoring and the endotracheal tube (not shown) would
left side. If so, the original incision line is used. If a patient has
be rostral in the operative field. (Courtesy, Barrow Neurolog-
subclinical vocal cord paralysis on the side of the incision,
ical Institute.)
proceeding with an incision on the opposite side is risky. The
potential for recurrent laryngeal nerve palsy is highest on the
right side, although the risk has not been documented in anterior to the sternocleidomastoid muscle, is made if three or
recent reports. The thoracic duct, however, can be injured more interspaces are involved. The angle of the mandible
when the approach is from the left side. tends to correspond to the level of C2, the hyoid bone corre-
A transverse incision is made for a one- or two-level ante- sponds to the level of C2–C3, and the inferior border of the
rior cervical discectomy. A carotid incision, parallel and just thyroid cartilage is estimated to be at C4–C5 (Fig. 2). The skin
Neurosurgery, Vol. 49, No. 4, October 2001 909
910 Sonntag et al.
FIGURE 3. Axial view of the plane of dissection and expo-
sure of the prevertebral space. The carotid sheath and the
jugular vein are retracted laterally, and the trachea and
esophagus are retracted medially. (Courtesy, Barrow Neuro-
logical Institute.)
large pituitary rongeurs, so that the blades can be hooked
under the longus colli muscles (Fig. 4).
A Caspar post is placed in what is thought to be one of the
appropriate vertebrae, and a lateral radiograph or fluoro-
scopic study is obtained. A post is preferred to a needle
because it provides a more fixed landmark. If the post is in an
FIGURE 2. Orientation to the vertebral column may be esti- incorrect vertebral body, it easily can be moved and placed in
mated by palpating superficial anatomic structures. The the correct vertebral body. After the correct level is identified,
hyoid bone sits approximately at the level of the C2–C3 disc a second vertebral post is placed. The post spreaders are
space. The top of the thyroid cartilage can be estimated as positioned over the post, and no distraction is performed until
the C3–C4 disc space. The inferior border of the thyroid car- the anterior anulus is incised (Fig. 5). Then vertical traction is
tilage (dotted line) can be estimated as the C4–C5 level. The placed on the vertebral bodies using the post spreaders.
C7–T1 disc space sits approximately one finger’s breadth Removal of the disc begins after the anulus has been cut
above the clavicle. The carotid-type incision (solid line) is (Fig. 6A). The anterior two-thirds of the disc is removed with
made if three or more interspaces are involved. (Courtesy, angled curettes and pituitary rongeurs of various sizes (Fig.
Barrow Neurological Institute © 1993.) 6B). An osseous lip, which is usually present on the superior
vertebral body, is removed with a No. 2 Kerrison rongeur
is incised sharply to the level of the platysma, which also is (Codman/Johnson & Johnson, Raynham, MA) or with a Mi-
divided sharply. When more than one level is exposed, rostral das Rex AM-8 drill (Midas Rex Institute, Fort Worth, TX). The
and caudal subplatysmal dissection is mandatory. superoanterior lip of the inferior vertebral body is drilled until
The plane between the carotid sheath laterally and the it is flush with the endplate. The microscope is brought into
esophagus and trachea medially is dissected sharply and the surgical field, and the rest of the disc is removed.
bluntly (Fig. 3). The omohyoid muscle can be divided if ex- The posterior ligament becomes visible. It is wise to coag-
tensive exposure is required or if it is directly in the route of ulate the posterior ligament to help identify its fibers and to
the approach. The prevertebral tissues are dissected, initially
with a “peanut” and then with low-power monopolar cauter- FIGURE 4. Once the tips of
ization. The longus colli muscles are visible overlying the the self-retaining retractors
anterior longitudinal ligaments and vertebral bodies. With the are positioned beneath the
monopolar cautery device set on low and its tip slightly bent, dissected longus colli mus-
the longus colli muscle is dissected gently from the vertebral cles, the cervical vertebral
body approximately 2 to 3 mm laterally. The teeth of the bodies are exposed anteri-
self-retaining retractor blades, which are placed beneath the orly. (Courtesy, Barrow Neu-
dissected longus colli muscles, often get caught on an osteo- rological Institute.)
phyte. It is best to remove such osteophytes, usually with
Neurosurgery, Vol. 49, No. 4, October 2001
Anterior Cervical Discectomy 911
Once decompression of the symptomatic side is completed,
if no fusion is contemplated, the nonsymptomatic side is
treated just as diligently to prevent postoperative radiculop-
athy related to settling (Fig. 7). If fusion is planned, the Smith-
Robinson fusion technique is preferred. Endplates are rough-
ened with the drill, and bone chips and shavings from the
drilling are saved to place into the middle of the fibula au-
tograft. A posterior shelf of bone (1–1.5 mm) is formed by
drilling the inferior vertebral bodies where the shelf is almost
preformed by the curvature of the vertebral body (Fig. 8). If
plating is not planned, a 1-mm anterior shelf is drilled as well
(Fig. 9). Again, the cortical endplate must not be denuded
completely. At this time, a graft is fashioned to fit the in-
FIGURE 5. Interbody posts and spreader in position. Two- terspace. Distraction of the interspace spreader is increased,
headed arrow, direction of movement of the posts. (Courte- and the fibula graft filled with cancellous bone shavings is
sy, Barrow Neurological Institute.) tapped gently into the interspace (Fig. 10).
Alternatively, an autograft can be obtained from the iliac
crest. An incision is made 2 cm posterior to the anterior iliac
spine. Soft tissue is dissected down to the iliac crest, and the
FIGURE 6. A, the discec- periosteum is dissected sharply with a knife or a monopolar
tomy is initiated by incising cauterization device. An appropriate-sized tricortical piece of
the anulus with a No. 11 iliac crest is obtained to fit the interspace. In a patient with a
blade. B, after the anulus large iliac crest, a bicortical autograft can be obtained. After
fibrosus has been opened the autograft or allograft is placed, the distracting posts are
initially, a small amount of removed. If no plating is pursued, the graft should be placed
distraction is applied across just below the formed anterior lip. If plating is considered, the
the vertebral bodies by using anterior lip is unnecessary, and the graft is tapped flush with
the post spreaders. A curette the vertebral bodies. The microscope is then removed from
is used to “scrape” the carti- the surgical field.
laginous endplate to remove When an anterior plate is placed, an appropriate-sized plate
additional disc material. is chosen. The vertebral bodies must be void of osteophytes
(Courtesy, Barrow Neurolog- and soft tissue before the plate is applied. The two superior
ical Institute.) screws should be placed just above the interspace 6 degrees
medially and 12 degrees rostrally, and the inferior screws are
placed 12 degrees caudally and 6 degrees medially. The
screws are fastened to the plate with the appropriate locking
coagulate the veins running through it. Coagulation also mechanisms.
seems to make entering the ligament easier with the micro- After copious irrigation, the wound is closed. It is inspected
curette. The posterior ligament is incised with the curette or once more by placing two self-retaining Cloward retractors in
with the No. 1 Kerrison rongeur. the wound, keeping one self-retaining retractor deep in the
The symptomatic site is decompressed first. That is, if the wound. The walls of the wound are checked for any bleeding,
patient has a left radiculopathy, the patient is turned 10 to 20 which is then controlled, and the opposite retractor is re-
degrees away from the surgeon, who is on the right side so moved slowly. The same maneuver is performed on the other
that the left foramen is easily seen. With microcurettes and a side. The platysma layer is closed with interrupted 3-0 Vicryl
micro-Kerrison rongeur, the foraminotomy is performed by suture (Ethicon, Inc., Somerville, NJ), and the skin is closed
removing the osteophytes and disc material. Often the herni- with a running subcuticular 4-0 Vicryl suture. The suture line
ated disc is posterior to the ligament and is identified at this
time. It is often difficult to determine how far lateral to carry
the dissection. Helpful landmarks are the origin of the nerve FIGURE 7. Axial view of the
root, fat in the axilla, the curvature of the uncovertebral joint, operative site after discec-
or extensive venous bleeding from the laterally positioned tomy. The disc space has a
veins. Bipolar coagulation and Avitene (Davol, Inc., Cranston, keystone configuration after
RI) are used to control these epidural veins. The uncovertebral the disc and the posterior
joint is best identified at the beginning of the curvature of the longitudinal ligaments have
endplate. When the osteophyte is removed, the surgeon al- been resected and the
ways must bite bone with the Kerrison rongeur, an angled foramina have been decom-
curette, or both. The surgeon should never bite into “air” for pressed. (Courtesy, Barrow
fear of injuring the vertebral artery. Neurological Institute.)
Neurosurgery, Vol. 49, No. 4, October 2001
912 Sonntag et al.
FIGURE 10. Sagittal view of
the operative site after disc-
FIGURE 8. A shelf drilled
ectomy or osteophytectomy
along the superior aspect of
and spinal canal decompres-
the inferior vertebral body
sion with fusion. (Courtesy,
prevents retromigration of
the Barrow Neurological
the bone graft. (Courtesy,
Institute.)
Barrow Neurological
Institute.)
days of discharge, patients are seen in the office for a “wound
check.” Flexion-extension radiographs are obtained 6 weeks
after the operation in patients with a fusion construct. If
evidence of fusion is present and there are no signs of
FIGURE 9. Sagittal view of
pseudarthrosis, patients are started on exercise therapy at that
the anterior and posterior
time. Patients who do not undergo a fusion procedure can
vertebral body shelves. Dot-
start exercise 2 to 3 weeks after surgery.
ted line defines posterior
vertebral body shelf. (Cour-
Received, January 24, 2001.
tesy, Barrow Neurological
Accepted, April 20, 2001.
Institute.) Reprint requests: Volker K.H. Sonntag, M.D., c/o Neuroscience Pub-
lications, Barrow Neurological Institute, 350 W. Thomas Road, Phoe-
is reinforced with Steri-Strips (3M Healthcare, St. Paul, MN) nix, AZ 85013-4496. Email: neuropub@chw.edu
or Dermabond (Closure Medical Corp., Raleigh, NC).
For patients who undergo a fusion procedure, anterior and REFERENCES
lateral radiographs are obtained in the recovery room to ver-
ify the position of the graft, the plate, and the screws. Patients 1. Cloward RB: The anterior approach for removal of ruptured cer-
vical disks. J Neurosurg 15:602–617, 1958.
without an internal fixation device wear a rigid collar for 4 to
2. Golfinos JG, Dickman CA, Zabramski JM, Sonntag VKH, Spetzler
6 weeks. In patients who receive internal fixation and in those RF: Repair of vertebral artery injury during anterior cervical de-
who undergo no fusion, external orthosis is not applied rou- compression. Spine 19:2552–2556, 1994.
tinely, except to control pain. Patients are discharged the day 3. Robinson RA, Smith GW: Anterolateral cervical disc removal and
after surgery. A problem with swallowing is the usual reason interbody fusion for cervical disc syndrome. Bull John Hopkins
why patients are kept longer in the hospital. Within 7 to 10 Hosp 96:223–224, 1955.
Instructions for Contributors:
Email Address Needed for All Submissions
In preparation for moving to an online submission and review process and electronic
proofs, we emphasize the following, found in the Instructions for Contributors:
Author Contact Information Page—Include a separate page with the
name, address, telephone and fax numbers, and email address of the
author responsible for correspondence and galley proofs. Clearly indi-
cate if changes of address are anticipated, and include forwarding ad-
dresses. It is the corresponding author’s responsibility to notify the Edi-
torial Office of changes of address.
Thank you for your cooperation in providing us with all of your contact infor-
mation, including your email address.
Neurosurgery, Vol. 49, No. 4, October 2001
Das könnte Ihnen auch gefallen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Areview of Analogies Between Some Neuroanatomical Termsand Roman Household Objects PDFDokument7 SeitenAreview of Analogies Between Some Neuroanatomical Termsand Roman Household Objects PDFGabriela MacoveanuNoch keine Bewertungen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Pictorial Essay - Parapharyngeal Space LesionDokument0 SeitenPictorial Essay - Parapharyngeal Space LesionGabriela MacoveanuNoch keine Bewertungen
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Anatomy and Development of Oral Cavity and PharynxDokument14 SeitenAnatomy and Development of Oral Cavity and PharynxGabriela MacoveanuNoch keine Bewertungen
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Parapharyngeal Synovial SarcomaDokument8 SeitenParapharyngeal Synovial SarcomaGabriela MacoveanuNoch keine Bewertungen
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Anterior Cervical VertebrectomyDokument4 SeitenAnterior Cervical VertebrectomyGabriela MacoveanuNoch keine Bewertungen
- Head and Neck CancerDokument48 SeitenHead and Neck CancerGabriela MacoveanuNoch keine Bewertungen
- Antimicrobial DrugsDokument21 SeitenAntimicrobial DrugsfikeNoch keine Bewertungen
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Anatomy and Surgical Approaches of TheDokument2 SeitenAnatomy and Surgical Approaches of TheGabriela MacoveanuNoch keine Bewertungen
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- AI LabDokument17 SeitenAI LabTripti JainNoch keine Bewertungen
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Ed508-5e-Lesson-Plan-Severe Weather EventsDokument3 SeitenEd508-5e-Lesson-Plan-Severe Weather Eventsapi-526575993Noch keine Bewertungen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- 3500 Ha027988 7Dokument384 Seiten3500 Ha027988 7Gigi ZitoNoch keine Bewertungen
- Civil Engineering Construction Manager in ST Louis MO Resume Mark JensenDokument3 SeitenCivil Engineering Construction Manager in ST Louis MO Resume Mark JensenMark JensenNoch keine Bewertungen
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- IHRM Midterm ASHUVANI 201903040007Dokument9 SeitenIHRM Midterm ASHUVANI 201903040007ashu vaniNoch keine Bewertungen
- Comparative ApproachDokument12 SeitenComparative ApproachSara WongNoch keine Bewertungen
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- Recruitment of Officers in Grade B' (General) - DR - By-2019Dokument2 SeitenRecruitment of Officers in Grade B' (General) - DR - By-2019Shalom NaikNoch keine Bewertungen
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Sample Barista Offer LetterDokument2 SeitenSample Barista Offer LetterMohammed Albalushi100% (2)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- Alma Matter SpeechDokument1 SeiteAlma Matter Speechlariza gallegoNoch keine Bewertungen
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- A Guide To Energy Efficiency ComplianceDokument16 SeitenA Guide To Energy Efficiency ComplianceOARIASCONoch keine Bewertungen
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Maruti FinalDokument23 SeitenMaruti FinalYash MangeNoch keine Bewertungen
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Marketing Plan Potato Food TruckDokument25 SeitenMarketing Plan Potato Food TruckAhasan h. ShuvoNoch keine Bewertungen
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Contemporary Philippine MusicDokument11 SeitenContemporary Philippine MusicmattyuuNoch keine Bewertungen
- Shakespeare Ubd Unit PlanDokument16 SeitenShakespeare Ubd Unit Planapi-239477809Noch keine Bewertungen
- Ventilation WorksheetDokument1 SeiteVentilation WorksheetIskandar 'muda' AdeNoch keine Bewertungen
- Research InstrumentsDokument28 SeitenResearch InstrumentsAnjeneatte Amarille AlforqueNoch keine Bewertungen
- Management of Odontogenic Infection of Primary Teeth in Child That Extends To The Submandibular and Submental Space Case ReportDokument5 SeitenManagement of Odontogenic Infection of Primary Teeth in Child That Extends To The Submandibular and Submental Space Case ReportMel FANoch keine Bewertungen
- WP Seagull Open Source Tool For IMS TestingDokument7 SeitenWP Seagull Open Source Tool For IMS Testingsourchhabs25Noch keine Bewertungen
- Monster Energy v. Jing - Counterfeit OpinionDokument9 SeitenMonster Energy v. Jing - Counterfeit OpinionMark JaffeNoch keine Bewertungen
- Four Quartets: T.S. EliotDokument32 SeitenFour Quartets: T.S. Eliotschwarzgerat00000100% (1)
- Pressuremeter TestDokument33 SeitenPressuremeter TestHo100% (1)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Legal NoticeDokument3 SeitenLegal NoticeT Jayant JaisooryaNoch keine Bewertungen
- Harmonica IntroDokument5 SeitenHarmonica Introapi-26593142100% (1)
- ShowimgDokument76 SeitenShowimgROSHAN ROBERTNoch keine Bewertungen
- Sri Anjaneya Cotton Mills LimitedDokument63 SeitenSri Anjaneya Cotton Mills LimitedPrashanth PB50% (2)
- 1 - CV - SwarupaGhosh-Solutions Account ManagerDokument2 Seiten1 - CV - SwarupaGhosh-Solutions Account ManagerprabhujainNoch keine Bewertungen
- Lagundi/Dangla (Vitex Negundo)Dokument2 SeitenLagundi/Dangla (Vitex Negundo)Derrick Yson (Mangga Han)Noch keine Bewertungen
- Differentialequations, Dynamicalsystemsandlinearalgebra Hirsch, Smale2Dokument186 SeitenDifferentialequations, Dynamicalsystemsandlinearalgebra Hirsch, Smale2integrationbyparths671Noch keine Bewertungen
- Ecological Pyramids WorksheetDokument3 SeitenEcological Pyramids Worksheetapi-26236818833% (3)
- Generic NdaDokument2 SeitenGeneric NdalataminvestmentsNoch keine Bewertungen
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)