Beruflich Dokumente
Kultur Dokumente
Specific Etiologies Associated With The Multiple PARTE 1
Hochgeladen von
darlingcarvajalduqueOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Specific Etiologies Associated With The Multiple PARTE 1
Hochgeladen von
darlingcarvajalduqueCopyright:
Verfügbare Formate
Specific Etiologies Associated With the Multiple
Organ Dysfunction Syndrome in Children: Part 1
Jeffrey S. Upperman, MD1; Jacques Lacroix, MD2; Martha A. Q. Curley, RN, PhD, FAAN3;
Paul A. Checchia, MD, FCCM, FACC4; Daniel W. Lee, MD5; Kenneth R. Cooke, MD6;
Robert F. Tamburro, MD, MSc7
1
Division of Pediatric Surgery, Children’s Hospital Los Angeles, Keck dysfunction although this has not been confirmed in phase II or III trial.
School of Medicine, University of Southern California, Los Angeles, CA. The remaining authors have disclosed that they do not have any potential
conflicts of interest.
2
Division of Pediatric Critical Care Medicine, Department of Pediatrics,
Sainte-Justine Hospital, Université de Montréal, Montreal, QC, Canada. For information regarding this article, E-mail: robert.tamburro@nih.gov
3
School of Nursing, Departments of Anesthesia and Critical Care Medi-
cine, University of Pennsylvania, Philadelphia, PA.
4
Sections of Critical Care and Cardiology, Department of Pediatrics, Objective: To describe a number of the conditions associated
Baylor College of Medicine Texas Children’s Hospital, Houston, TX. with multiple organ dysfunction syndrome presented as part of
5
Division of Pediatric Hematology/Oncology, Department of Pediatrics, the Eunice Kennedy Shriver National Institute of Child Health and
University of Virginia, Charlottesville, VA. Human Development multiple organ dysfunction syndrome work-
6
Department of Oncology, Pediatric Blood and Marrow Transplantation shop (March 26–27, 2015).
Program, Sidney Kimmel Comprehensive Cancer Center, Johns Hopkins
Hospital, The Johns Hopkins University School of Medicine, Baltimore, MD. Data Sources: Literature review, research data, and expert opinion.
7
Pediatric Trauma and Critical Illness Branch, Eunice Kennedy Shriver Study Selection: Not applicable.
National Institute of Child Health and Human Development, National Data Extraction: Moderated by an expert from the field, issues rele-
Institutes of Health, U.S. Department of Health and Human Services, vant to the association of multiple organ dysfunction syndrome with
Bethesda, MD.
a variety of conditions were presented, discussed, and debated
This information or content and conclusions are those of the authors
and should not be construed as the official position or policy of, nor with a focus on identifying knowledge gaps and research priorities.
should any endorsements be inferred by, the National Institutes of Data Synthesis: Summary of presentations and discussion sup-
Health, the U.S. Department of Health and Human Services, or the U.S. ported and supplemented by the relevant literature.
government.
Conclusions: There is a wide range of medical conditions associated
Drs. Upperman, Curley, and Lee received support for this article research
from the National Institutes of Health (NIH). Dr. Curley’s institution with multiple organ dysfunction syndrome in children. Traditionally,
received funding from National Heart, Lung, and Blood Institute and the sepsis and trauma are the two conditions most commonly associ-
National Institute of Nursing Research, NIH (grant U01 HL086622). ated with multiple organ dysfunction syndrome both in children and
Dr. Lee also received support from the St. Baldrick’s Foundation Scholar
Award with generous support from the Hope From Harper Fund. adults. However, there are a number of other pathophysiologic pro-
Dr. Cooke received funding from the NIH (R01 HL111682 and R01 cesses that may result in multiple organ dysfunction syndrome. In this
HD074587) and received funding from Jazz pharmaceuticals, advi- article, we discuss conditions such as cancer, congenital heart dis-
sory board (money paid had no influence on my efforts for this study).
Dr. Tamburro’s former institution received funding from the U.S. Food and ease, and acute respiratory distress syndrome. In addition, the rela-
Drug Administration Office of Orphan Product Development Grant Pro- tionship between multiple organ dysfunction syndrome and clinical
gram and from Ony, LLC (provided the calfactant free of charge for the therapies such as hematopoietic stem cell transplantation and car-
above grant, which assessed the efficacy of surfactant in pediatric hema-
topoietic stem cell transplant patients with acute lung injury). He received diopulmonary bypass is also considered. The purpose of this article
funding from Springer Publishing. Dr. Tamburro disclosed government is to describe the association of multiple organ dysfunction syndrome
work, and he disclosed off-label/unapproved drugs or products: serum with a variety of conditions in an attempt to identify similarities, dif-
interleukin (IL)-6 levels in responding patients have been measured to
be greater than 3,000 pg/mL (normal < 10 pg/mL), and the fever and ferences, and opportunities for therapeutic intervention. (Pediatr Crit
hemodynamic instability reported in cytokine release syndrome (CRS) Care Med 2017; 18:S50–S57)
can be reversed within hours of the administration of the anti–IL-6 recep- Key Words: acute respiratory distress syndrome; congenital heart
tor monoclonal antibody, tocilizumab. Clinical experience suggests that
the timely administration of tocilizumab with or without corticosteroids disease; cytokine release syndrome; graft-versus-host disease;
to the patient with moderate-grade CRS is of paramount importance in hepatic venoocclusive disease/sinusoidal obstruction syndrome;
preventing severe, life-threatening CRS characterized by multiple organ idiopathic pneumonia syndrome; multiple organ dysfunction
Copyright © 2016 by the Society of Critical Care Medicine and the World syndrome; pediatrics; sepsis; thrombotic microangiopathy
Federation of Pediatric Intensive and Critical Care Societies
DOI: 10.1097/PCC.0000000000001048
S50 www.pccmjournal.org March 2017 • Volume 18 • Number 3 (Suppl.)
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
MODS Supplement
T Table 1. Identified Knowledge Gaps and
here are a number of pathophysiologic processes that
may result in the multiple organ dysfunction syndrome Potential Opportunities for Study
(MODS) in children. To begin, certain underlying diag-
noses including, but not limited to cancer, congenital heart dis- An enhanced understanding of the sepsis pathophysiology
ease, inborn errors of metabolism, and rheumatologic diseases that drives MODS needs to be better established and
potential therapeutic targets need to be identified.
have all been associated with a predisposition to the syndrome.
Similarly, acute conditions such as sepsis, acute respiratory dis- A better understanding of the influence that pulmonary and
tress syndrome (ARDS), acute kidney injury, liver failure, and immune system maturation have on the pathophysiology of
ARDS needs to be established with an attempt to explain the
pancreatitis have also been associated with the process. Addi- differences between children and adults in terms of outcomes
tionally, pathophysiologic processes such as hypoxia (of any and the occurrence of MODS associated with ARDS.
source) can be potent triggers of MODS as observed follow-
The impact of age on the occurrence of MODS following
ing cardiopulmonary arrest. Furthermore, acute insults such as cardiac surgery and cardiopulmonary bypass needs to be
multiple trauma and thermal injuries have also been found to better established. Moreover, similarities and differences
result in MODS. Conversely, numerous treatments and thera- between MODS in the setting of cardiac repair and other
peutic regimens such as antineoplastic therapies, blood transfu- etiologies such as sepsis and trauma need to be elucidated;
sions, and hematopoietic and solid organ transplantation have such study may improve outcomes in each of these settings.
all been reported to elicit MODS. Given the breadth of these Established triggers of MODS with well-defined timelines such
various topics, any attempt to provide a comprehensive review as cardiopulmonary bypass and antineoplastic therapy need
of the many etiologies of MODS would be grossly insufficient, to be used as models for studying MODS. The conditions
associated with these interventions such as congenital heart
and thus, that is not the intent of this article. Conditions com- disease and cancer represent opportunities for long-term
monly associated with MODS such as inborn errors of metab- follow-up of MODS and the impact of multiple insults.
olism, brain injury and neurologic insult, and rheumatologic
The role of anticytokine therapy in conditions associated
disorders are not addressed in this or its accompanying article. with MODS needs to be determined. However, to do so,
The available literature contains a host of publications and mediating biomarkers must first be identified that can be
reviews addressing the individual topics and their association assessed in a clinically relevant time frame as has been
with MODS. The purpose of this article is simply to encourage accomplished for the cytokine release syndrome.
investigators to consider the topic from the perspective of other Mortality among pediatric hematopoietic cell patients remains
disciplines to hopefully identify areas of commonality, enhance unacceptably high, and there is a clear association of
the body of knowledge of respective disciplines, and identify mortality with MODS in this patient population. In order to
opportunities for future study (Table 1). advance this field, early predictors of patients at risk need
to be identified. The development of novel strategies that
reduce transplant-related toxicity in combination with the
Sepsis discovery of biomarkers that may predict the development,
Sepsis is a common cause of MODS. It is defined in its simplest severity, and response to therapy of these complications
must be further established.
form as a systemic inflammatory response syndrome (SIRS)
caused by an infection (1). Although sepsis has most recently ARDS = acute respiratory distress syndrome, MODS = multiple organ
dysfunction syndrome.
been redefined for adults (2), those definitions have not been
applied to children to date. Thus, this discussion will continue to
use the definitions initially proposed at the International Pedi- “Septic shock” was defined as sepsis and cardiovascular organ
atric Sepsis Consensus Conference held in 2005. Based on those dysfunction as defined in the MODS diagnostic criteria. Sep-
proceedings, the proposed diagnostic criteria of SIRS include sis may be caused by all forms of microbes including bacteria,
the presence of alterations in at least two of four criteria includ- viruses, protozoans, and fungi. The most frequent causes of
ing temperature, heart rate, respiratory rate, and/or WBC count community- and hospital-acquired infection in the PICU are
(1). This set of diagnostic criteria for SIRS has subsequently in decreasing order: respiratory infections (37%), bacteremia
been found to demonstrate excellent interobserver reliability (25%), urinary tract infections, intra-abdominal infections, soft-
(3). In addition to SIRS, several other definitions were proposed tissue infections, CNS infections, endocarditis, fasciitis, etc (4).
at the International Pediatric Sepsis Consensus Conference. Of the many etiologies of MODS, the association between
For example, “infection” was defined as a suspected or proven MODS and sepsis is perhaps the most studied in children,
infection (by positive culture, tissue stain, or polymerase chain and it is important to understand that relationship (Fig. 1).
reaction test) caused by any pathogen or a clinical syndrome Although not all cases of MODS are caused by an infection,
associated with a high probability of infection (1). Evidence all severe infections can progress to MODS. In addition, sep-
of infection includes positive findings on clinical examination, tic patients must receive antibiotics as soon as possible; even
imaging, or laboratory tests (e.g., WBCs in a normally sterile a delay as short as 30 minutes increases the risk of MODS
body fluid, perforated viscus, chest radiograph consistent with and death (5). The relationship between MODS and sepsis is
pneumonia, petechial or purpuric rash, or purpura fulminans). exemplified by the cumulative effect on mortality of MODS
“Severe sepsis” was defined as sepsis plus cardiovascular organ severity and the septic state. Leclerc et al (6) analyzed the
dysfunction or ARDS or two or more other organ dysfunctions. cumulative influence of organ dysfunctions and the presence
Pediatric Critical Care Medicine www.pccmjournal.org S51
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
Upperman et al
Lung Injury Consensus Conference Group (Fig. 2) (8). In
pediatrics, the occurrence and mortality of ARDS are lower
than published rates for adults. Specifically, pediatric ARDS
(PARDS) occurrence rates range from 2 to 12.8 per 100,000
person-years, whereas mortality rates span from 18 to 27% (9).
However, despite these documented differences with adults,
most of our knowledge related to PARDS is derived from stud-
ies in adult patients or in mature animals with very few studies
performed in children or in young animal models (10). This
void in pediatric-specific inquiry presents a problem because
pulmonary and immune system maturation may impact the
pathophysiology of PARDS and may be significantly different
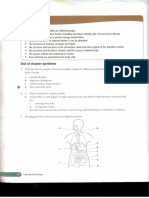
Figure 1. Relationship between the systemic inflammatory response then what has been described in adult ARDS. Differences in the
syndrome (SIRS), the multiple organ dysfunction syndrome (MODS), and innate immunologic response to critical illness may account
three septic states (sepsis, severe sepsis, and septic shock).
for the variation in the rate of multiple organ failure between
critically ill children and adults (11). These fundamental dif-
of sepsis on mortality using the PEdiatric Logistic Organ ferences may impact the diagnosis, severity, and optimal thera-
Dysfunction (PELOD) score among 593 consecutive admis- peutic approach in the management of PARDS.
sions of critically ill children to one of three PICUs. In that PARDS can be associated with MODS either as the precipi-
study, 514 patients had SIRS; 269 of whom had two or more tant of the other organ dysfunctions or as an additional organ
organ dysfunctions (severe sepsis). The hazard ratio (HR) dysfunction incited by another trigger. Either way, MODS at the
of death associated with SIRS or sepsis was similar (9.039) onset of PARDS is an important independent clinical risk factor
and was significantly higher than the risk of death in patients for mortality in children (12–14). In addition, as mortality from
without SIRS or sepsis (p = 0.031). The SIRS/sepsis patients PARDS continues to decrease, rates of new or progressive organ
were grouped together for further analysis. The HR of death system dysfunction and organ failure–free days have been recom-
significantly increased with worsening of the diagnostic cate- mended as alternative endpoints for clinical trials of PARDS (15).
gory of the septic state: 18.8 with severe sepsis (p = 0.007) and
32.6 with septic shock (p < 0.001). Additionally, each increase Congenital Heart Disease/Cardiopulmonary Bypass
of 1 U in the PELOD score multiplied the HR of each septic In the United States alone, there are approximately 400,000 car-
state by 1.096 (p < 0.0001). The formula that can be used to diac surgical operations performed employing cardiopulmo-
estimate the cumulative HR of death is HR (death) = HRPELOD nary bypasses (CPB) each year, of which 10,000 are performed
× (HR septic state). For example, for children with severe on children. In nearly all cases, cardiac surgical operations
sepsis and a PELOD score of 24, the HR of death = 169.7 as performed on children employing CPB induce ischemia with
illustrated below: subsequent reperfusion injury resulting from the reinitiation
HRPELOD score = 1.09624 = 9.025; HRsevere sepsis = 18.8; thus, of flow following circulatory arrest and removal of the cross-
HR (death) = HRPELOD × (HR septic state) clamp. These pathophysiologic processes not only cause injury
HR (death) = 1.09624 × 18.8 themselves through myocardial necrosis, renal injury, and
HR (death) = 9.025 × 18.8 = 169.7. neurologic injury but also activate a systemic inflammatory
Thus, the description of the severity of illness is improved response characterized by multisystem organ dysfunction and
in critically ill children by consideration of both the severity of failure. The sum total of these pathologic processes is postop-
MODS and the status of the septic condition. The predictive erative morbidity and mortality that is significantly worse in
value of this combined evaluation is better than the predictive the infant than compared with that in the adult (16). However,
value of MODS or septic state alone. Although these defini- unlike other triggers associated with whole-body inflamma-
tions of SIRS and sepsis are imperfect and likely to be soon tory reactions such as trauma or sepsis, cardiac surgical teams
revised for children, they add useful information. have the advantage of knowing when the trigger will occur (i.e.,
during CPB) and hence have an opportunity for preemptive
ARDS intervention in an effort to attenuate or minimize the response.
ARDS is a syndrome of inflammation and increased perme- The vast majority of patients undergoing congenital car-
ability in the lungs associated with a pattern of clinical, radio- diac repair with bypass have some degree of MODS. Published
logic, and physiologic abnormalities that cannot be explained reports indicate that this rate varies between 4% and 80% (17).
by, but may coexist with, left atrial or pulmonary capillary If cardiac dysfunction is included, virtually all patients have
hypertension (7). Although there are similarities in the patho- MODS. However, the outcomes in this population are excel-
physiology of ARDS between adults and children, pediatric- lent. This raises the possibility that MODS following this type
specific practice patterns, comorbidities, and differences in of injury is fundamentally different than that in other critical
outcome prompted the recent development of a pediatric- disease processes. It is possible that this population requires
specific operational definition for ARDS by the Pediatric Acute separate definitions of MODS.
S52 www.pccmjournal.org March 2017 • Volume 18 • Number 3 (Suppl.)
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
MODS Supplement
investigations. Because of the
extensive follow-up inherent in
this population, an opportunity
for long-term endpoints exists.
Although MODS and critical
cardiac disease have been tradi-
tionally thought of as an acute
problem; the congenital heart
disease population allows exam-
ination of the chronicity and
long-term outcomes of MODS.
Cancer and Antineoplastic
Therapies
Cancer has long been associated
with multiple organ dysfunction
(21, 22). The organ dysfunc-
tion may not only be a result
of the disease process and its
Figure 2. Pediatric acute respiratory distress definition. 1Use Pao2-based metric when available. If Pao2 is associated comorbidities such
not available, wean Fio2 to maintain Spo2 less than or equal to 97% to calculate the Spo2/Fio2 (SF) ratio or as sepsis, but may also emanate
FIO2 mean airway pressure × 100 2 from the antineoplastic thera-
the oxygen saturation index (OSI), where OSI = . Nonintubated patients
SpO2 pies. As innovative therapies
treated with supplemental oxygen or nasal modes of noninvasive ventilation are categorized using the “at-risk” emerge and are implemented
definition. 3Acute respiratory distress syndrome severity stratification based on OSI or oxygenation index (OI),
for an ever-expanding list of
FIO2 mean airway pressure × 100
where OI = should not be applied to children with chronic lung disease who high-risk patients and refractory
PaO2
disease processes, the ability to
normally receive invasive mechanical ventilation or children with cyanotic congenital heart disease.
CPAP = continuous positive airway pressure, PARDS = pediatric acute respiratory distress syndrome, recognize and address adverse
PF = Pao2/Fio2. Reproduced with permission from Khemani et al (9). organ dysfunction in a prompt
and effective manner will be
The fact that the injury in this population is initiated through necessary to optimize treatment outcomes. When organ dysfunc-
the necessity of performing a cardiac repair provides an oppor- tion is associated with specific antineoplastic regimens, it is simi-
tunity to investigate the mechanisms involved. There are very few lar to congenital heart surgery with CPB, in that both represent
situations in which the timing of the injury can be controlled, scheduled interventions with a known propensity to incite organ
and thus, it is incumbent upon investigators to leverage this fac- injury. Clinical situations such as these in which the known insult
tor. Certainly, there are challenges to such investigations includ- can be anticipated would appear to foster greater opportunity for
ing diverse baseline cardiac diseases and physiologic states, as successful intervention.
well as unique bypass strategies, operative approaches, and anes- Recently, after decades of investigation, effective methods
thetic management. However, this represents an opportunity for of utilizing immune cells to recognize and eliminate cancer are
not only study, but also preemptive intervention. Current inter- becoming reality. Most notably, genetic engineering of autolo-
ventional approaches involve modulation of the inflammatory gous T-cells with chimeric antigen receptors (CARs) and T-cell
response including steroids and nitric oxide (16, 18, 19). In addi- receptors has resulted in unprecedented responses in children
tion, such study also allows investigation into the roles of the and adults with relapsed, refractory pre-B-cell acute lympho-
multiple variables such as preoperative state and age. It is clear blastic leukemia (ALL) (23–25), synovial cell sarcoma, or mela-
that cardiac injury and recovery from inflammation are affected noma (26), respectively. However, this transformative therapy
by the age of the patient (20). This may be particularly true in has also been reported to be associated with a pathophysiologic
the cardiac surgical patient. Within this particular population, process known as the “cytokine release syndrome.”
we have the opportunity to examine the response to injury and Cytokine release syndrome (CRS) is a constellation of
progression to MODS across the spectrum of age from the neo- symptoms along a spectrum ranging from mild with only fever
nate to the 90-year-old patient receiving a valve replacement. to severe with very high fever, rigors, headache, flushing, tachy-
Additionally, there exists the potential to examine a single pnea, severe tachycardia, coagulopathy, hypoxia, pulmonary
population, or even a single patient, across multiple surgical expo- edema, hypotension requiring vasopressors, and/or respira-
sures and insults because of the requirement for several staged tory failure (27). Severity of CRS seems to be related to overall
surgical palliative procedures throughout a lifetime. In addition, tumor burden, and almost all patients who respond have some
since complex congenital cardiac disease is now considered a degree of CRS (23). Left unchecked, severe CRS will result
survivable disease, mortality is not an appropriate endpoint for in multiple organ failure typically beginning with the rapid
Pediatric Critical Care Medicine www.pccmjournal.org S53
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
Upperman et al
development of biventricular cardiac dysfunction then failure, (phase 2), and the culmination of target organ damage by soluble
acute pulmonary edema resulting in hypoxemic respiratory and cellular effectors (phase 3). Although components of this
failure, acute kidney injury at times requiring renal replace- paradigm have been challenged and refined (30), the hypothesis
ment therapy, hepatic dysfunction, and severe coagulopathy. identifies areas where novel agents can be explored. The onset of
Neurotoxicities observed in CAR therapy for ALL appear to be acute GVHD typically occurs within the first 2 months after allo-
related to CRS, but often present as an isolated phenomenon geneic HCT, and the classic target organs include the gastrointes-
outside the context of typical multisystem CRS (23, 25). tinal tract, liver, and skin. Historically, the occurrence and severity
Activated CAR T-cells produce massive quantities of of GVHD have correlated with the donor type (related vs unre-
inflammatory cytokines such as interferon-γ, tumor necrosis lated) and the degree of antigenic disparity between the donor
factor-α (TNF-α), and interleukin (IL)-2, which in turn acti- and host. Advanced (grades 3 to 4) GVHD remains life threaten-
vate other aspects of cellular immunity inducing robust pro- ing and often times requires critical care support to manage direct
duction of IL-6 (27). IL-6 clearly drives the symptoms noted in (organ dysfunction) and indirect (opportunistic infection) mani-
CRS. Serum IL-6 levels in responding patients have been mea- festations of disease.
sured to be greater than 3,000 pg/mL (normal < 10 pg/mL), Pulmonary complications in a variety of forms occur in
and the fever and hemodynamic instability reported in CRS 25–55% of HCT recipients and can account for approximately
can be reversed within hours of the administration of the anti– 40% of transplant-related mortality. Historically, approxi-
IL-6 receptor monoclonal antibody, tocilizumab (23–25, 27). mately 50% of cases were determined to be noninfectious in
Clinical experience suggests that the timely administration origin, but the judicious use of broad-spectrum antimicrobial
of tocilizumab with or without corticosteroids to the patient prophylaxis in recent years has tipped the balance of pulmo-
with moderate-grade CRS is of paramount importance in pre- nary complications from infectious to noninfectious causes
venting severe, life-threatening CRS characterized by multiple (31). The idiopathic pneumonia syndrome (IPS) refers to non-
organ dysfunction although this has not been confirmed in infectious lung injury that occurs acutely within the first 120
phase II or III trials. This is one instance where MODS may days following HCT (31–34). Diagnostic criteria of IPS include
actually be prevented. However, early recognition and treat- signs and symptoms of pneumonia, nonlobar radiographic
ment are critical as patients who have already progressed to infiltrates, abnormal pulmonary function, and the absence of
organ failure are rarely rescued even with anticytokine therapy. infectious organisms as determined by bronchoalveolar lavage
In addition, it will be important to assess if such an approach or lung biopsy. IPS has been a frequently fatal complication of
can be successful in other clinical conditions in which cytokine HCT, associated with mortality rates in excess of 70% with a
release drives multiple organ dysfunction. median time from diagnosis to death of only 2 weeks (31–34).
Potential etiologies for IPS include direct toxic effects of HCT
Hematopoietic Cell Transplantation conditioning regimens, occult pulmonary infections, and the
Hematopoietic cell transplantation (HCT) is another antineo- release of inflammatory cytokines that have been implicated in
plastic therapy that has emerged over the past 25 years as the other forms of pulmonary injury (31). Clinically, the diagnosis
only curative therapy for children with a number of malignant, of IPS has been linked to the development of acute GVHD.
as well as nonmalignant, disorders of the blood and immune Although this association suggests the importance of alloreac-
systems. In its more traditional mode, HCT recipients are treated tivity to lung injury that occurs after HCT, a causal relationship
with supralethal doses of anticancer therapy (chemo- and/or between IPS and GVHD is yet to be firmly established.
irradiation therapy) and subsequently “rescued” by the infusion Clinical syndromes presenting with microangiopathic
of hematopoietic stem cells. Despite significant advances in crit- hemolytic anemia, with consumptive thrombocytopenia, and
ical care and transplantation medicine, optimal outcomes fol- often with renal insufficiency and encephalopathy have long
lowing allogeneic HCT continue to be limited by the occurrence been recognized as potentially devastating multisystem compli-
of organ dysfunction as the result of the development of acute cations after HCT (35). Although several terms have been used
graft-versus-host disease (GVHD), acute pulmonary dysfunc- in the literature to describe these microangiopathic processes,
tion, thrombotic microangiopathy, and venoocclusive disease transplant-associated thrombotic microangiopathy (TA-TMA)
(VOD)/sinusoidal obstruction syndrome (SOS) of the liver. is now widely accepted as an umbrella term to cover these disor-
GVHD describes a disease process wherein immune cells in the ders (36).The diagnosis of TA-TMA is based on clinical criteria
donor stem cell “graft” respond to foreign antigens in the “host.” and the classic presentation, which includes the relatively acute
Immunologic dysregulation occurring after allogeneic HCT con- onset of anemia and thrombocytopenia with evidence of RBC
tributes to GVHD. However, donor T-cell activation also enhances fragmentation in the peripheral blood smear (37). Concomitant
the therapeutic potential of HCT through powerful graft versus acute renal dysfunction, often associated with proteinuria and
tumor effects that persist long after the chemo- and irradiation hypertension, occurs in the majority of patients, and neuro-
therapy effects have passed. The pathophysiology of acute GVHD logic deficits, including but not restricted to confusion and
is complex (28–30). Immune dysregulation can be conceptual- seizures, are also commonly observed. The onset of TA-TMA
ized in three distinct phases (29) and involves diffuse damage and usually occurs within the first 100 days after HCT, and the
activation of host tissues by HCT conditioning regimens (phase median time of onset ranged from 44 to 67 days in two large
1), the activation of donor T-cells by host antigen-presenting cells retrospective reports (38, 39). TA-TMA occurs less frequently
S54 www.pccmjournal.org March 2017 • Volume 18 • Number 3 (Suppl.)
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
MODS Supplement
after autologous HCT (up to 2.6%) compared with the alloge- sinusoidal endothelium, hepatocytes, and the central venules
neic setting where the occurrence rate is in the 10–15% range in zone 3 of the liver acinus that ultimately progresses to veno-
and even higher in some recent pediatric reports given the close occlusion and sinusoidal obstruction (51–54). VOD/SOS is
association of TA-TMA with calcineurin inhibitors, GVHD, and characterized clinically by painful hepatomegaly, jaundice, and
infections (38, 40). Recognizing the need to standardize defini- fluid retention as manifested by weight gain and ascites that
tions for toxicity reporting in multicenter clinical trials and to typically occurs within 30 days of HCT. The clinical diagnosis of
facilitate future clinical investigative efforts, U.S. and European VOD/SOS is based on the classical triad of weight gain, painful
working groups have recently proposed specific sets of clinical hepatomegaly, and jaundice as characterized by the Seattle (51)
criteria for reporting TA-TMA (39, 41). and Baltimore (55) transplant groups. Making the diagnosis of
The primary inciting events leading to the development of VOD/SOS can be challenging because the signs and symptoms
TA-TMA remain poorly understood, but evidence suggests that of this condition often overlap those of other processes (54).
damage to the vascular endothelium is central to its pathogen- In this context, the time of onset is often useful in narrowing
esis and may represent a common thread underlying several the differential diagnosis. The severity of VOD/SOS ranges
of the other posttransplant complications (37). In this context, from mild to severe depending on the degree of hyperbilirubi-
TA-TMA is now believed to be a multivisceral disorder and nemia, the amount of fluid retention, and the pace of disease
should be included in the differential diagnosis of usual HCT progression (56–58). When associated with MODS, specifically
complications (36). For example, pulmonary TMA presenting as involving pulmonary and renal impairment, VOD/SOS has
pulmonary hypertension should be considered in patients with historically been associated with unacceptably high mortal-
respiratory failure (42, 43). Recent reports have also found that ity rates that approach 100% despite advances in mechanical
TMA can affect the intestinal tract and present with abdominal ventilation and continuous renal replacement therapy (54, 58).
pain and bloody diarrhea, thereby imitating enteric GVHD or Optimization of care in the immediate post-HCT period
infectious colitis (44, 45). The diagnosis of intestinal TMA relies and minimization of potential organ dysfunction are essential
primarily on histopathologic evaluation, demonstrating hyaline for successful outcomes as the degree of MODS has clearly been
thrombi in the capillaries of intestinal biopsies or the presence associated with survival in the HCT population (21, 59). Indeed,
of thrombonecrotic arteriolar lesions in the intestine on autopsy the development of novel strategies that reduce transplant-
(44, 45). Recent reports have revealed that activation and dysreg- related toxicity, regulate GVHD, preserve graft versus tumor
ulation of the complement alternative pathway may be a major effects, and facilitate engraftment and long-term immune recon-
contributor to endothelial damage incurred during TA-TMA (46, stitution remains the most significant challenge to broadening
47). These findings are significant as they may identify a genetic the scope of allogeneic HCT. The development of novel therapies
susceptibility for disease development and ultimately guide the to treat and prevent acute GVHD, translational research efforts
institution of novel treatment strategies to improve outcomes. underscoring a critical role for TNF inhibitors in the manage-
Approximately 12–18% of patients with TA-TMA will have ment of IPS (60, 61), and the introduction of an endothelial sta-
severe disease affecting their outcome. Proteinuria and acti- bilizing agent (defibrotide) for the management of hepatic VOD/
vated terminal complement at TA-TMA diagnosis are very SOS (62, 63) have represented major advances in the field. These
poor prognostic markers, and prompt clinical interventions breakthroughs in combination with the discovery of biomarkers
should be considered (40). Unfortunately, there is currently no that may predict the development, severity, and response to ther-
standard treatment for TA-TMA, but there is consensus that apy of these complications (64–67) are being considered in the
rapid withdrawal of potential offending drugs such as calci- development of rationally designed, translational research trials
neurin inhibitors or sirolimus should be the primary inter- aimed at identifying patients at risk, limiting the occurrence of
vention. Aggressive management of concurrent GVHD and MODS, and improving patient outcomes after allogeneic HCT.
infections is crucial since these are common causes of mor-
tality in patients with TA-TMA. Although often used, plasma CONCLUSIONS
exchange (PE) has demonstrated limited efficacy and has not In summary, there are a number of medical conditions and ther-
been endorsed as a standard treatment; response rates are apeutic interventions that are associated with multiple organ
generally less than 50%, and mortality rates among patients dysfunction and the MODS. The intent of this article, as with the
treated with PE remain unacceptably high (41). Early imple- accompanying article, is to highlight a handful of those condi-
mentation of PE in pediatric patients may rescue some patients tions and therapies in an attempt to identify areas of commonal-
with renal failure, but outcomes remain poor (48). The fact ity, areas of difference, and opportunities for further study and
that TA-TMA results from direct injury to endothelial cells and intervention; it was not to present an exhaustive list of the many
not from circulating antibody may explain the low response etiologies that may result in MODS. It is hoped that by consider-
rates to PE and supports the use of other agents that inhibit ing this syndrome in relation to a number of disparate condi-
complement (eculizumab) (49) or stabilize vascular endothe- tions, investigators may gain new insight and avenues for study
lial integrity and function (50) to improve outcomes. that will advance our understanding of this process from that
VOD/SOS is recognized as another complication associ- of a syndrome (i.e., simply a collection of related symptoms) to
ated with high-dose chemotherapy and HCT that may result a well-defined clinical entity with established pathophysiologic
in multiple organ dysfunction. It results from direct injury to causes, genetic predispositions, and targeted therapies.
Pediatric Critical Care Medicine www.pccmjournal.org S55
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
Upperman et al
ACKNOWLEDGMENTS 18. Checchia PA, Backer CL, Bronicki RA, et al: Dexamethasone reduces
postoperative troponin levels in children undergoing cardiopulmonary
We thank the Eunice Kennedy Shriver National Institute of bypass. Crit Care Med 2003; 31:1742–1745
Child Health and Human Development and their Office of Sci- 19. Checchia PA, Bronicki RA, Muenzer JT, et al: Nitric oxide delivery
ence Policy, Analysis, and Communications for their support during cardiopulmonary bypass reduces postoperative morbid-
of this workshop. ity in children–a randomized trial. J Thorac Cardiovasc Surg 2013;
146:530–536
20. Checchia PA, Schierding W, Polpitiya A, et al: Myocardial transcrip-
REFERENCES tional profiles in a murine model of sepsis: Evidence for the impor-
1. Goldstein B, Giroir B, Randolph A; International Consensus tance of age. Pediatr Crit Care Med 2008; 9:530–535
Conference on Pediatric Sepsis: International pediatric sepsis con- 21. Dursun O, Hazar V, Karasu GT, et al: Prognostic factors in pediatric
sensus conference: Definitions for sepsis and organ dysfunction in cancer patients admitted to the pediatric intensive care unit. J Pediatr
pediatrics. Pediatr Crit Care Med 2005; 6:2–8 Hematol Oncol 2009; 31:481–484
2. Singer M, Deutschman CS, Seymour CW, et al: The Third International 22. Fiser RT, West NK, Bush AJ, et al: Outcome of severe sepsis in pedi-
Consensus Definitions for Sepsis and Septic Shock (Sepsis-3). atric oncology patients. Pediatr Crit Care Med 2005; 6:531–536
JAMA 2016; 315:801–810
23. Lee DW, Kochenderfer JN, Stetler-Stevenson M, et al: T cells express-
3. Juskewitch JE, Prasad S, Salas CF, et al: Reliability of the identifica- ing CD19 chimeric antigen receptors for acute lymphoblastic leukae-
tion of the systemic inflammatory response syndrome in critically ill mia in children and young adults: A phase 1 dose-escalation trial.
infants and children. Pediatr Crit Care Med 2012; 13:e55–e57 Lancet 2015; 385:517–528
4. Watson RS, Carcillo JA, Linde-Zwirble WT, et al: The epidemiology of 24. Maude SL, Frey N, Shaw PA, et al: Chimeric antigen receptor
severe sepsis in children in the United States. Am J Respir Crit Care T cells for sustained remissions in leukemia. N Engl J Med 2014;
Med 2003; 167:695–701 371:1507–1517
5. Kumar A, Roberts D, Wood KE, et al: Duration of hypotension before 25. Davila ML, Riviere I, Wang X, et al: Efficacy and toxicity management
initiation of effective antimicrobial therapy is the critical determinant of of 19-28z CAR T cell therapy in B cell acute lymphoblastic leukemia.
survival in human septic shock. Crit Care Med 2006; 34:1589–1596 Sci Transl Med 2014; 6:224ra25
6. Leclerc F, Leteurtre S, Duhamel A, et al: Cumulative influence of organ 26. Robbins PF, Kassim SH, Tran TL, et al: A pilot trial using lymphocytes
dysfunctions and septic state on mortality of critically ill children. Am J genetically engineered with an NY-ESO-1-reactive T-cell receptor:
Respir Crit Care Med 2005; 171:348–353 Long-term follow-up and correlates with response. Clin Cancer Res
7. Bernard GR, Artigas A, Brigham KL, et al: The American-European 2015; 21:1019–1027
Consensus Conference on ARDS. Definitions, mechanisms, relevant 27. Lee DW, Gardner R, Porter DL, et al: Current concepts in the diag-
outcomes, and clinical trial coordination. Am J Respir Crit Care Med nosis and management of cytokine release syndrome. Blood 2014;
1994; 149:818–824 124:188–195
8. Pediatric Acute Lung Injury Consensus Conference Group: Pediatric 28. Blazar BR, Murphy WJ, Abedi M: Advances in graft-versus-host dis-
acute respiratory distress syndrome: Consensus recommendations ease biology and therapy. Nat Rev Immunol 2012; 12:443–458
from the Pediatric Acute Lung Injury Consensus Conference. Pediatr
Crit Care Med 2015;16:428–439 29. Ferrara JL, Cooke KR, Teshima T: The pathophysiology of graft-vs-
host disease. In: Graft-vs-Host Disease. Third Edition. Ferrara J,
9. Khemani RG, Smith LS, Zimmerman JJ, et al; Pediatric Acute Lung Cooke K, Degg HJ (Eds). New York, Marcel Dekker, Inc., 2005, pp
Injury Consensus Conference Group: Pediatric acute respiratory dis- 1–34
tress syndrome: Definition, incidence, and epidemiology: Proceedings
from the Pediatric Acute Lung Injury Consensus Conference. Pediatr 30. Shlomchik WD: Graft-versus-host disease. Nat Rev Immunol 2007;
Crit Care Med 2015;16:S23–S40 7:340–352
10. Sapru A, Flori H, Quasney MW, et al; Pediatric Acute Lung Injury 31. Panoskaltsis-Mortari A, Griese M, Madtes DK, et al; American Thoracic
Consensus Conference Group: Pathobiology of acute respiratory dis- Society Committee on Idiopathic Pneumonia Syndrome: An official
tress syndrome. Pediatr Crit Care Med 2015;16:S6–S22 American Thoracic Society research statement: Noninfectious lung
injury after hematopoietic stem cell transplantation: Idiopathic pneu-
11. Wood JH, Partrick DA, Johnston RB Jr: The inflammatory response to monia syndrome. Am J Respir Crit Care Med 2011; 183:1262–1279
injury in children. Curr Opin Pediatr 2010; 22:315–320
32. Clark JG, Hansen JA, Hertz MI, et al: NHLBI workshop summary.
12. Flori H, Dahmer MK, Sapru A, et al; Pediatric Acute Lung Injury Idiopathic pneumonia syndrome after bone marrow transplantation.
Consensus Conference Group: Comorbidities and assessment of Am Rev Respir Dis 1993; 147:1601–1606
severity of pediatric acute respiratory distress syndrome: Proceedings
from the Pediatric Acute Lung Injury Consensus Conference. Pediatr 33. Crawford SW, Hackman RC: Clinical course of idiopathic pneumo-
Crit Care Med 2015;16:S41–S50 nia after bone marrow transplantation. Am Rev Respir Dis 1993;
147:1393–1400
13. López-Fernández Y, Azagra AM, de la Oliva P, et al; Pediatric Acute
Lung Injury Epidemiology and Natural History (PED-ALIEN) Network: 34. Kantrow SP, Hackman RC, Boeckh M, et al: Idiopathic pneumonia
Pediatric Acute Lung Injury Epidemiology and Natural History study: syndrome: Changing spectrum of lung injury after marrow transplan-
Incidence and outcome of the acute respiratory distress syndrome in tation. Transplantation 1997; 63:1079–1086
children. Crit Care Med 2012; 40:3238–3245 35. Cooke KR, Jannin A, Ho V: The contribution of endothelial activa-
14. Leclerc F, Duhamel A, Deken V, et al; Groupe Francophone de tion and injury to end-organ toxicity following allogeneic hematopoi-
Réanimation et d’Urgences Pédiatriques: Nonrespiratory pediatric logis- etic stem cell transplantation. Biol Blood Marrow Transplant 2008;
tic organ dysfunction-2 score is a good predictor of mortality in children 14:23–32
with acute respiratory failure. Pediatr Crit Care Med 2014; 15:590–593 36. Jodele S, Laskin BL, Dandoy CE, et al: A new paradigm: Diagnosis
15. Quasney MW, López-Fernández YM, Santschi M, et al; Pediatric Acute and management of HSCT-associated thrombotic microangiopathy
Lung Injury Consensus Conference Group: The outcomes of children as multi-system endothelial injury. Blood Rev 2015; 29:191–204
with pediatric acute respiratory distress syndrome: Proceedings from 37. Fuge R, Bird JM, Fraser A, et al: The clinical features, risk factors
the Pediatric Acute Lung Injury Consensus Conference. Pediatr Crit and outcome of thrombotic thrombocytopenic purpura occurring after
Care Med 2015;16:S118–S131 bone marrow transplantation. Br J Haematol 2001;113:58–64
16. Checchia PA, Gandhi SK: Defining vasodilatory shock following car- 38. George JN, Li X, McMinn JR, et al: Thrombotic thrombocytopenic
diac surgery in children: When, where, how often? Pediatr Crit Care purpura-hemolytic uremic syndrome following allogeneic HPC trans-
Med 2009; 10:409–410 plantation: A diagnostic dilemma. Transfusion 2004;44:294–304
17. Taggart DP, Hadjinikolas L, Hooper J, et al: Effects of age and ischemic 39. Ruutu T, Barosi G, Benjamin RJ, et al; European Group for Blood and
times on biochemical evidence of myocardial injury after pediatric car- Marrow Transplantation; European LeukemiaNet: Diagnostic criteria
diac operations. J Thorac Cardiovasc Surg 1997; 113:728–735 for hematopoietic stem cell transplant-associated microangiopathy:
S56 www.pccmjournal.org March 2017 • Volume 18 • Number 3 (Suppl.)
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
MODS Supplement
Results of a consensus process by an International Working Group. 53. Bearman SI: The syndrome of hepatic veno-occlusive disease after
Haematologica 2007; 92:95–100 marrow transplantation. Blood 1995; 85:3005–3020
40. Jodele S, Davies SM, Lane A, et al: Diagnostic and risk criteria for 54. Coppell JA, Richardson PG, Soiffer R, et al: Hepatic veno-occlusive
HSCT-associated thrombotic microangiopathy: A study in children disease following stem cell transplantation: Incidence, clinical course,
and young adults. Blood 2014; 124:645–653 and outcome. Biol Blood Marrow Transplant 2010; 16:157–168
41. Ho VT, Cutler C, Carter S, et al: Blood and marrow transplant clini- 55. Jones RJ, Lee KS, Beschorner WE, et al: Venoocclusive disease
cal trials network toxicity committee consensus summary: Thrombotic of the liver following bone marrow transplantation. Transplantation
microangiopathy after hematopoietic stem cell transplantation. Biol 1987;44:778–783
Blood Marrow Transplant 2005; 11:571–575 56. Blostein MD, Paltiel OB, Thibault A, Rybka WB: A comparison of
42. Dandoy CE, Hirsch R, Chima R, et al: Pulmonary hypertension clinical criteria for the diagnosis of veno-occlusive disease of the
after hematopoietic stem cell transplantation. Biol Blood Marrow liver after bone marrow transplantation. Bone Marrow Transplant
Transplant 2013; 19:1546–1556 1992;10:439–443
43. Jodele S, Hirsch R, Laskin B, et al: Pulmonary arterial hypertension in 57. Bearman SI, Anderson GL, Mori M, et al: Venoocclusive disease of
pediatric patients with hematopoietic stem cell transplant-associated the liver: Development of a model for predicting fatal outcome after
thrombotic microangiopathy. Biol Blood Marrow Transplant 2013; marrow transplantation. J Clin Oncol 1993; 11:1729–1736
19:202–207 58. Carreras E: How I manage sinusoidal obstruction syndrome after hae-
44. Nishida T, Hamaguchi M, Hirabayashi N, et al: Intestinal thrombotic matopoietic cell transplantation. Br J Haematol 2015; 168:481–491
microangiopathy after allogeneic bone marrow transplantation: A clin- 59. Tamburro RF, Barfield RC, Shaffer ML, et al: Changes in outcomes
ical imitator of acute enteric graft-versus-host disease. Bone Marrow (1996-2004) for pediatric oncology and hematopoietic stem cell
Transplant 2004; 33:1143–1150 transplant patients requiring invasive mechanical ventilation. Pediatr
45. El-Bietar J, Warren M, Dandoy C, et al: Histologic features of intesti- Crit Care Med 2008; 9:270–277
nal thrombotic microangiopathy in pediatric and young adult patients 60. Yanik GA, Grupp SA, Pulsipher MA, et al: TNF-receptor inhibitor
after hematopoietic stem cell transplantation. Biol Blood Marrow therapy for the treatment of children with idiopathic pneumonia syn-
Transplant 2015; 21:1994–2001 drome. A joint Pediatric Blood and Marrow Transplant Consortium
46. Jodele S, Licht C, Goebel J, et al: Abnormalities in the alterna- and Children’s Oncology Group Study (ASCT0521). Biol Blood
tive pathway of complement in children with hematopoietic stem Marrow Transplant 2015; 21:67–73
cell transplant-associated thrombotic microangiopathy. Blood 61. Klein O, Cooke KR: Idiopathic pneumonia syndrome following
2013;122:2003–2007 hematopoietic stem cell transplantation. J Ped Intensive Care
47. Jodele S, Zhang K, Zou F, et al: The genetic fingerprint of suscep- 2014;3:147–157
tibility for transplant-associated thrombotic microangiopathy. Blood 62. Richardson PG, Ho VT, Giralt S, et al: Safety and efficacy of defi-
2016; 127:989–996 brotide for the treatment of severe hepatic veno-occlusive disease.
48. Jodele S, Laskin BL, Goebel J, et al: Does early initiation of therapeu- Ther Adv Hematol 2012; 3:253–265
tic plasma exchange improve outcome in pediatric stem cell trans- 63. Corbacioglu S, Cesaro S, Faraci M, et al: Defibrotide for prophylaxis
plant-associated thrombotic microangiopathy? Transfusion 2013; of hepatic veno-occlusive disease in paediatric haemopoietic stem-
53:661–667 cell transplantation: An open-label, phase 3, randomised controlled
49. Jodele S, Fukuda T, Vinks A, et al: Eculizumab therapy in children with trial. Lancet 2012; 379:1301–1309
severe hematopoietic stem cell transplantation-associated thrombotic 64. Schlatzer DM, Dazard JE, Ewing RM, et al: Human biomarker dis-
microangiopathy. Biol Blood Marrow Transplant 2014; 20:518–525 covery and predictive models for disease progression for idiopathic
50. Corti P, Uderzo C, Tagliabue A, et al: Defibrotide as a promising treat- pneumonia syndrome following allogeneic stem cell transplantation.
ment for thrombotic thrombocytopenic purpura in patients undergo- Mol Cell Proteomics 2012; 11:M111.015479
ing bone marrow transplantation. Bone Marrow Transplant 2002; 65. Paczesny S, Krijanovski OI, Braun TM, et al: A biomarker panel for
29:542–543 acute graft-versus-host disease. Blood 2009; 113:273–278
51. McDonald GB, Sharma P, Matthews DE, et al: Venocclusive disease 66. Vander Lugt MT, Braun TM, Hanash S, et al: ST2 as a marker for
of the liver after bone marrow transplantation: Diagnosis, incidence, risk of therapy-resistant graft-versus-host disease and death. N Engl
and predisposing factors. Hepatology 1984;4:116–122 J Med 2013; 369:529–539
52. McDonald GB, Hinds MS, Fisher LD, et al: Veno-occlusive dis- 67. Levine JE, Braun TM, Harris AC, et al; Blood and Marrow Transplant
ease of the liver and multiorgan failure after bone marrow trans- Clinical Trials Network: A prognostic score for acute graft-versus-host
plantation: A cohort study of 355 patients. Ann Intern Med 1993; disease based on biomarkers: A multicentre study. Lancet Haematol
118:255–267 2015; 2:e21–e29
Pediatric Critical Care Medicine www.pccmjournal.org S57
Copyright © 2016 by the Society of Critical Care Medicine and the World Federation of Pediatric Intensive and Critical Care Societies.
Unauthorized reproduction of this article is prohibited
Das könnte Ihnen auch gefallen
- Httpswatermark Silverchair Com - Ezproxy.unbosque - edu.Copedsinreview.2022005642.Pdftoken AQECAHi208BE49Ooan9kkhW Ercy7Dm3ZL 9Dokument10 SeitenHttpswatermark Silverchair Com - Ezproxy.unbosque - edu.Copedsinreview.2022005642.Pdftoken AQECAHi208BE49Ooan9kkhW Ercy7Dm3ZL 9darlingcarvajalduqueNoch keine Bewertungen
- Early Progressive Mobility Protocol: Step 1: Screen For SafetyDokument2 SeitenEarly Progressive Mobility Protocol: Step 1: Screen For SafetydarlingcarvajalduqueNoch keine Bewertungen
- Nihms 1646158Dokument30 SeitenNihms 1646158darlingcarvajalduqueNoch keine Bewertungen
- Pediatric Pain AssessmentDokument10 SeitenPediatric Pain AssessmentdarlingcarvajalduqueNoch keine Bewertungen
- Post-Intensive Care Syndrome: Its Pathophysiology, Prevention, and Future DirectionsDokument14 SeitenPost-Intensive Care Syndrome: Its Pathophysiology, Prevention, and Future DirectionsdarlingcarvajalduqueNoch keine Bewertungen
- Early Progressive Mobility Protocol: Step 1: Screen For SafetyDokument2 SeitenEarly Progressive Mobility Protocol: Step 1: Screen For SafetydarlingcarvajalduqueNoch keine Bewertungen
- De-Escalation of Critical Care and Prevention of Iatrogenicity Through PICU Liberation Rounding Process and A Daily Rounding ChecklistDokument1 SeiteDe-Escalation of Critical Care and Prevention of Iatrogenicity Through PICU Liberation Rounding Process and A Daily Rounding ChecklistdarlingcarvajalduqueNoch keine Bewertungen
- Acutebrainfailure: Pathophysiology, Diagnosis, Management, and Sequelae of DeliriumDokument59 SeitenAcutebrainfailure: Pathophysiology, Diagnosis, Management, and Sequelae of DeliriumdarlingcarvajalduqueNoch keine Bewertungen
- PALS Algorithms 2019 (Pediatric Advanced Life Support)Dokument1 SeitePALS Algorithms 2019 (Pediatric Advanced Life Support)darlingcarvajalduqueNoch keine Bewertungen
- Protocolo FATE (Eco TT)Dokument4 SeitenProtocolo FATE (Eco TT)darlingcarvajalduqueNoch keine Bewertungen
- Pals TachycardiaDokument1 SeitePals TachycardiadarlingcarvajalduqueNoch keine Bewertungen
- Pals Pediatric BradycardiaDokument1 SeitePals Pediatric BradycardiadarlingcarvajalduqueNoch keine Bewertungen
- Pediatric ShockDokument19 SeitenPediatric ShockdarlingcarvajalduqueNoch keine Bewertungen
- SDOM Promising TherapiesDokument16 SeitenSDOM Promising TherapiesdarlingcarvajalduqueNoch keine Bewertungen
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Soal Materi 1 KLS X IntroductionDokument2 SeitenSoal Materi 1 KLS X IntroductionFira AnandaNoch keine Bewertungen
- Shyla Jennings Ebook FinalDokument17 SeitenShyla Jennings Ebook FinalChye Yong HockNoch keine Bewertungen
- PP Planning Workshop SAPDokument36 SeitenPP Planning Workshop SAPDavid100% (1)
- Ksiidc and KssidcDokument13 SeitenKsiidc and KssidckasperNoch keine Bewertungen
- Wavoo Wajeeha Women's College - Annual Report - 2013-14Dokument29 SeitenWavoo Wajeeha Women's College - Annual Report - 2013-14kayalonthewebNoch keine Bewertungen
- New Rich Text DocumentDokument12 SeitenNew Rich Text Documentsonam dorjiNoch keine Bewertungen
- Name: - Date: - Week/s: - 2 - Topic: Examining Trends and FadsDokument3 SeitenName: - Date: - Week/s: - 2 - Topic: Examining Trends and FadsRojelyn Conturno100% (1)
- University of Physician V CIRDokument24 SeitenUniversity of Physician V CIROlivia JaneNoch keine Bewertungen
- 3 Social Policy and Social Welfare AdministrationDokument284 Seiten3 Social Policy and Social Welfare AdministrationJoseph Kennedy100% (5)
- Priya - Rachna Kumari PrasadDokument17 SeitenPriya - Rachna Kumari PrasadSumant priyadarshiNoch keine Bewertungen
- A Crude Awakening Video NotesDokument3 SeitenA Crude Awakening Video NotesTai NguyenNoch keine Bewertungen
- Founders' ShareDokument2 SeitenFounders' ShareHenry BerlangaNoch keine Bewertungen
- ABC LTD ProposalDokument4 SeitenABC LTD ProposalAbhishek JurianiNoch keine Bewertungen
- End-Of-Chapter Questions: CambridgeDokument17 SeitenEnd-Of-Chapter Questions: CambridgeMido MidoNoch keine Bewertungen
- Effectives of e Wallets NewDokument15 SeitenEffectives of e Wallets NewRicardo SantosNoch keine Bewertungen
- GnatusDokument36 SeitenGnatusNacer Mezghiche100% (1)
- Catherine Davies - Modernity, Masculinity, and Imperfect Cinema in CubaDokument16 SeitenCatherine Davies - Modernity, Masculinity, and Imperfect Cinema in CubakahlilchaarNoch keine Bewertungen
- Hitachi Zx330 3 Series Hydraulic ExcavatorDokument15 SeitenHitachi Zx330 3 Series Hydraulic ExcavatorAgung ArdhanaNoch keine Bewertungen
- Bang Thong Ke Phep NamDokument16 SeitenBang Thong Ke Phep NamTiến Tươi TỉnhNoch keine Bewertungen
- Pico Power: A Boon For Rural Electrification: Rajat KapoorDokument8 SeitenPico Power: A Boon For Rural Electrification: Rajat KapoorBamNoch keine Bewertungen
- UNIX Introduction 1Dokument18 SeitenUNIX Introduction 1Akash SavaliyaNoch keine Bewertungen
- ReflectionDokument2 SeitenReflectionBảo HàNoch keine Bewertungen
- VIETTELDokument20 SeitenVIETTELSolgrynNoch keine Bewertungen
- Region XiDokument2 SeitenRegion XiGarcia, Rafael Rico O.Noch keine Bewertungen
- Uplifting Hauora Maori RealDokument32 SeitenUplifting Hauora Maori RealFano AsiataNoch keine Bewertungen
- Acd 1Dokument3 SeitenAcd 1Kath LeynesNoch keine Bewertungen
- Floline Size eDokument4 SeitenFloline Size eNikesh ShahNoch keine Bewertungen
- Hazardous Location Division Listed LED Light: Model 191XLDokument2 SeitenHazardous Location Division Listed LED Light: Model 191XLBernardo Damas EspinozaNoch keine Bewertungen
- Case Study of AmoebiasisDokument16 SeitenCase Study of AmoebiasisGlorielle ElvambuenaNoch keine Bewertungen
- 1.2 Introduction To PHP - PHP KeywordsDokument12 Seiten1.2 Introduction To PHP - PHP KeywordsOvie Nur FaizahNoch keine Bewertungen