Beruflich Dokumente
Kultur Dokumente
Ischemic Cardiomiopati
Hochgeladen von
u_dhani0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
70 Ansichten2 SeitenManifestations of congestive heart failure are common in patients with chronic CAD. Heart failure may be dominant clinical feature in some patients. Ischemic cardiomyopathy is often confused with dilated cardiomyopathy.
Originalbeschreibung:
Originaltitel
ischemic cardiomiopati
Copyright
© Attribution Non-Commercial (BY-NC)
Verfügbare Formate
DOC, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenManifestations of congestive heart failure are common in patients with chronic CAD. Heart failure may be dominant clinical feature in some patients. Ischemic cardiomyopathy is often confused with dilated cardiomyopathy.
Copyright:
Attribution Non-Commercial (BY-NC)
Verfügbare Formate
Als DOC, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
70 Ansichten2 SeitenIschemic Cardiomiopati
Hochgeladen von
u_dhaniManifestations of congestive heart failure are common in patients with chronic CAD. Heart failure may be dominant clinical feature in some patients. Ischemic cardiomyopathy is often confused with dilated cardiomyopathy.
Copyright:
Attribution Non-Commercial (BY-NC)
Verfügbare Formate
Als DOC, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 2
HEART FAILURE
Manifestations of congestive heart failure are common in patients
with chronic CAD. Heart failure may be the dominant clinical feature
in some patients, especially those who have sustained prior
myocardial infarction(s), in whom ischemic areas have become
replaced with a fibrous scar, leading to disappearance or reduction
of the angina. The three most common causes of congestive heart
failure are (1) an inadequate quantity of normally contracting
myocardium, (2) left ventricular aneurysm, and (3) mitral
regurgitation due to papillary muscle dysfunction. The first is the
most common of the three.
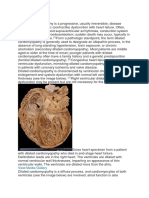
Ischemic Cardiomyopathy
In 1970 Burch and colleagues first used the term ischemic
cardiomyopathy to describe the condition in which CAD results in
severe myocardial dysfunction, with clinical manifestations often
indistinguishable from those of primary dilated cardiomyopathy (see
[For More Information] ). Symptoms of heart failure, caused by
ischemic myocardial dysfunction (hibernation), diffuse fibrosis, and
multiple infarctions, alone or in combination, may dominate the
clinical picture of CAD. In some patients with chronic CAD, angina
may be the principal clinical manifestation at one time, but later this
symptom diminishes or even disappears as heart failure becomes
more prominent. Other patients with ischemic cardiomyopathy have
no history of angina or myocardial infarction (type I silent ischemia),
and it is in this subgroup that ischemic cardiomyopathy is often
confused with dilated cardiomyopathy.
As discussed earlier in this chapter (see [For More Information]
), in patients with CAD and stable angina, left ventricular
dysfunction and overt heart failure may be due to a localized infarct,
scattered fibrosis, ischemic noncontractile (hibernating)
myocardium, or some combination of these. A similar situation
exists in patients without angina who present with heart failure and
little or no angina as their primary manifestation of CAD. It is
important to recognize hibernating myocardium in patients with
ischemic cardiomyopathy because symptoms resulting from chronic
left ventricular dysfunction may be incorrectly thought to result
from necrotic and scarred myocardium rather than from a reversible
ischemic process. Hibernating myocardium may be present in
patients with known or suspected CAD with a degree of cardiac
dysfunction or heart failure not readily accounted for by prior
myocardial infarctions.
The outlook for patients with ischemic cardiomyopathy treated
medically is quite poor, and revascularization or cardiac
transplantation may be considered. The prognosis is particularly
poor in patients in whom the ischemic cardiomyopathy is secondary
to multiple myocardial infarctions and in those with associated
ventricular arrhythmias. On the other hand, patients whose heart
failure, even if severe, is secondary to large segments of reversibly
injured but viable (hibernating) myocardium have a better prognosis
following revascularization. Thus, the key to the management of
patients with ischemic cardiomyopathy is to assess the extent of
residual viable myocardium with a view to coronary
revascularization. Techniques for detecting hibernating myocardium
are described on .
Das könnte Ihnen auch gefallen
- View Media GalleryDokument9 SeitenView Media Galleryjenrimz33Noch keine Bewertungen
- Cardiomyopathies: Cardiomyopathy Is A Heart Muscle Disease Associated With CardiacDokument10 SeitenCardiomyopathies: Cardiomyopathy Is A Heart Muscle Disease Associated With Cardiacmerin sunilNoch keine Bewertungen
- Heart DiseasesDokument73 SeitenHeart DiseasesturbomurboNoch keine Bewertungen
- Patofisiologi CHFDokument7 SeitenPatofisiologi CHFHafiz Idul FitranulNoch keine Bewertungen
- CHF PathDokument7 SeitenCHF PathGeraldine Gallaron - CasipongNoch keine Bewertungen
- Seminar ON: Cardiomyopat HYDokument43 SeitenSeminar ON: Cardiomyopat HYmerin sunilNoch keine Bewertungen
- USMLE General CardiologyDokument72 SeitenUSMLE General CardiologyWidyo MahargoNoch keine Bewertungen
- Differentiating Constrictive Pericarditis and Restrictive Cardiomyopathy - UpToDateDokument3 SeitenDifferentiating Constrictive Pericarditis and Restrictive Cardiomyopathy - UpToDateAnca StanNoch keine Bewertungen
- ACS HandoutDokument19 SeitenACS HandoutGloriana Julia TeopeNoch keine Bewertungen
- Cardio Myopathy.Dokument17 SeitenCardio Myopathy.Salman Khan100% (1)
- Diagnostico HF 2004Dokument8 SeitenDiagnostico HF 2004Carlos Alan Lopez100% (1)
- CardiomyopathyDokument93 SeitenCardiomyopathyAbnet WondimuNoch keine Bewertungen
- Ischemic Heart Disease (IHD)Dokument35 SeitenIschemic Heart Disease (IHD)Ali Akand AsifNoch keine Bewertungen
- Hypertrophic CardiomyopathyDokument10 SeitenHypertrophic CardiomyopathySam SonNoch keine Bewertungen
- Extrinsic Cardiomyopathies: CardiomyopathyDokument3 SeitenExtrinsic Cardiomyopathies: CardiomyopathyJoshua ObrienNoch keine Bewertungen
- Minoca INOCA HFDokument12 SeitenMinoca INOCA HFDaniel MelendezNoch keine Bewertungen
- 125 002 PDFDokument6 Seiten125 002 PDFgrahapuspa17Noch keine Bewertungen
- Myocardial Ischemia: Dr. Wael H. Mansy, MDDokument37 SeitenMyocardial Ischemia: Dr. Wael H. Mansy, MDHaleema SultanNoch keine Bewertungen
- Heart Failure Differential DiagnosesDokument3 SeitenHeart Failure Differential DiagnosesAizel ManiagoNoch keine Bewertungen
- Myocardial Infarction: BackgroundDokument9 SeitenMyocardial Infarction: BackgroundNor Faizah Ahmad SadriNoch keine Bewertungen
- Approach and ECGDokument35 SeitenApproach and ECGShaira Aquino VerzosaNoch keine Bewertungen
- IntroductionDokument13 SeitenIntroductionSiyara AntonyNoch keine Bewertungen
- Cardio MyopathiesDokument39 SeitenCardio Myopathiesinyanji.barasaNoch keine Bewertungen
- CardiologyDokument4 SeitenCardiologyShatha AlgahtaniNoch keine Bewertungen
- Background: Congestive Heart FailureDokument5 SeitenBackground: Congestive Heart FailureyasayyasayNoch keine Bewertungen
- Myocardial Infarction AssignmentDokument23 SeitenMyocardial Infarction AssignmentPums100% (6)
- Pathology of Acute Myocardial InfarctionDokument13 SeitenPathology of Acute Myocardial InfarctionNaily Nuzulur RohmahNoch keine Bewertungen
- Introduction - MIDokument10 SeitenIntroduction - MIkhimiiiNoch keine Bewertungen
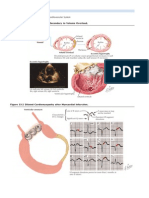
- Figure 33-1 Cardiac Remodeling Secondary To Volume OverloadDokument5 SeitenFigure 33-1 Cardiac Remodeling Secondary To Volume OverloadGiuseppe SerenaNoch keine Bewertungen
- Casos Cardiológicos 1Dokument12 SeitenCasos Cardiológicos 1Larissa SeabraNoch keine Bewertungen
- Lemone 6e Chapter 31Dokument47 SeitenLemone 6e Chapter 31Husein Fatih ArafatNoch keine Bewertungen
- Cardiogenic ShockDokument26 SeitenCardiogenic ShockAnggun V. M SitumorangNoch keine Bewertungen
- Neacsu Aurelia EssayDokument3 SeitenNeacsu Aurelia EssaySimona NeacsuNoch keine Bewertungen
- Clinical Epidemiology of Heart Failure: Arend Mosterd, Arno W HoesDokument11 SeitenClinical Epidemiology of Heart Failure: Arend Mosterd, Arno W HoesCAMILO ANDRES TOVAR DAZANoch keine Bewertungen
- CARDIO (PBL3) - Mohamad Arbian Karim - FMUI20Dokument10 SeitenCARDIO (PBL3) - Mohamad Arbian Karim - FMUI20Mohamad Arbian KarimNoch keine Bewertungen
- Heart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart Failure PDFDokument11 SeitenHeart Failure Clinical Presentation - History, Physical Examination, Predominant Right-Sided Heart Failure PDFislamiah 89Noch keine Bewertungen
- Ischaemic Heart Disease: EtiopathogenesisDokument12 SeitenIschaemic Heart Disease: Etiopathogenesisritika shakkarwalNoch keine Bewertungen
- CARDIOMYOPATHYDokument67 SeitenCARDIOMYOPATHYJoanna RachelNoch keine Bewertungen
- Cardiomyopathy: Restrictive Heart DiseaseDokument18 SeitenCardiomyopathy: Restrictive Heart DiseaseMitch GabuyaNoch keine Bewertungen
- Aortic StenosisDokument20 SeitenAortic Stenosisvasarhely imolaNoch keine Bewertungen
- Study Guide 4Dokument21 SeitenStudy Guide 4cNoch keine Bewertungen
- Lecture 2 Ischemic Heart DiseasesDokument19 SeitenLecture 2 Ischemic Heart DiseasesOsama MalikNoch keine Bewertungen
- Bonagura 4Dokument20 SeitenBonagura 4job88264629Noch keine Bewertungen
- Shock With Jugular Venous Distention: Clinical Review ArticleDokument9 SeitenShock With Jugular Venous Distention: Clinical Review ArticlenevmerkaNoch keine Bewertungen
- Heart Guide 2022Dokument13 SeitenHeart Guide 2022AnuNoch keine Bewertungen
- Angina Pectoris Myocardial Infarction: Bahuguna, Nimisha Imd-Batch 3Dokument19 SeitenAngina Pectoris Myocardial Infarction: Bahuguna, Nimisha Imd-Batch 3Nimisha BahugunaNoch keine Bewertungen
- Myocardial Infarction: "Heart Attack" Redirects Here. For Other Uses, See - Not To Be Confused WithDokument2 SeitenMyocardial Infarction: "Heart Attack" Redirects Here. For Other Uses, See - Not To Be Confused WithButchick De Leon BernabeNoch keine Bewertungen
- Cardiac ArrestDokument7 SeitenCardiac ArrestDiana MuañaNoch keine Bewertungen
- SINCOPE Journal of Internal MedicineDokument9 SeitenSINCOPE Journal of Internal MedicineIlse MarquezNoch keine Bewertungen
- Gagal JantungDokument69 SeitenGagal JantungKota Tako100% (1)
- Internal Medicine Lecture 6 Cardiomyopathies and MyocarditidesDokument98 SeitenInternal Medicine Lecture 6 Cardiomyopathies and MyocarditidesDaily MedicineNoch keine Bewertungen
- Cardiac EmergencyDokument56 SeitenCardiac Emergency21rayhanf100% (1)
- Coronary Artery DisaeseDokument48 SeitenCoronary Artery DisaeseAzkaZulfiqarNoch keine Bewertungen
- Heart Failure & Cor PulmunaleDokument12 SeitenHeart Failure & Cor PulmunaleShrestha AnjivNoch keine Bewertungen
- Pathologt of The HeartDokument40 SeitenPathologt of The HeartJudithNoch keine Bewertungen
- Myocardial InfarctionDokument25 SeitenMyocardial Infarctionfam111222Noch keine Bewertungen
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtVon EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtBewertung: 5 von 5 Sternen5/5 (1)
- GlomerulonephritisDokument1 SeiteGlomerulonephritismaleskunNoch keine Bewertungen
- BM 9303 - Diagnostic and Therapeutic Equipment IDokument1 SeiteBM 9303 - Diagnostic and Therapeutic Equipment IMythily VedhagiriNoch keine Bewertungen
- Acute Coronary SyndromeDokument48 SeitenAcute Coronary SyndromeAchmad ulil Albab100% (1)
- MCQ On Heart DiseaseDokument10 SeitenMCQ On Heart DiseaseSucheta Ghosh ChowdhuriNoch keine Bewertungen
- Fan 2018Dokument4 SeitenFan 2018Илија РадосављевићNoch keine Bewertungen
- CPC PowerpointDokument36 SeitenCPC Powerpointapi-277377339Noch keine Bewertungen
- TPSVDokument28 SeitenTPSVGeraldine CortesNoch keine Bewertungen
- Electrical Axis of HeartDokument19 SeitenElectrical Axis of Heartrera_avisNoch keine Bewertungen
- Result A Do 138660Dokument5 SeitenResult A Do 138660Kitt Shop ComunicacionesNoch keine Bewertungen
- Atrial Fibrillation 1Dokument15 SeitenAtrial Fibrillation 1api-595122187Noch keine Bewertungen
- Cardiogenic Shock Pathogenesis, Classification, and ManagementDokument20 SeitenCardiogenic Shock Pathogenesis, Classification, and Managementjosh FaducNoch keine Bewertungen
- ECG .DR Ayalew EthiopiaDokument60 SeitenECG .DR Ayalew EthiopiaAyalew Zewdie100% (2)
- Medmastery Handbook ACHD 0Dokument127 SeitenMedmastery Handbook ACHD 0Vladlena Cucoș-Caraiman100% (1)
- Full Programme 9Dokument18 SeitenFull Programme 9Borneo CTVSNoch keine Bewertungen
- Renal FailureDokument23 SeitenRenal FailurerjfeeleyNoch keine Bewertungen
- Clinical Application of The EchocardiogtamDokument39 SeitenClinical Application of The EchocardiogtamStella CooKeyNoch keine Bewertungen
- Aki NephrosapDokument82 SeitenAki NephrosapMARCELO DE ROSA100% (1)
- Acute Exacerbation of Congestive Heart Failure: History & ExamDokument76 SeitenAcute Exacerbation of Congestive Heart Failure: History & ExamMicija CucuNoch keine Bewertungen
- End Stage Renal Disease (ESRD)Dokument21 SeitenEnd Stage Renal Disease (ESRD)Dani DanyNoch keine Bewertungen
- ECG at A GlanceDokument53 SeitenECG at A Glancenurliah armandNoch keine Bewertungen
- Chronic Kidney Disease of Undiagnosed EtiologyDokument14 SeitenChronic Kidney Disease of Undiagnosed EtiologyGreenThumbNoch keine Bewertungen
- Coronary Artery DiseaseDokument10 SeitenCoronary Artery DiseaseStephanie ValerioNoch keine Bewertungen
- Eec Prague 2017 Program, European Echocardiography Course On Congenital Heart Disease, October 2017Dokument7 SeitenEec Prague 2017 Program, European Echocardiography Course On Congenital Heart Disease, October 2017Navojit ChowdhuryNoch keine Bewertungen
- YFT IM Notes 2Dokument81 SeitenYFT IM Notes 2AHMAD ALROWAILYNoch keine Bewertungen
- European J of Heart Fail - 2020 - Chioncel - Epidemiology Pathophysiology and Contemporary Management of Cardiogenic ShockDokument27 SeitenEuropean J of Heart Fail - 2020 - Chioncel - Epidemiology Pathophysiology and Contemporary Management of Cardiogenic ShockRui FonteNoch keine Bewertungen
- IJGMP - RV Function Assessment Pre and Post PTMC in Patients With Severe - AutosavedDokument8 SeitenIJGMP - RV Function Assessment Pre and Post PTMC in Patients With Severe - AutosavedImpact JournalsNoch keine Bewertungen
- The American Journal of Cardiology Vol 107 Issue 4 February 2011Dokument153 SeitenThe American Journal of Cardiology Vol 107 Issue 4 February 2011ppappi12Noch keine Bewertungen
- BIOLOGY PROJECT (Class 12)Dokument21 SeitenBIOLOGY PROJECT (Class 12)Manoghna MaheshNoch keine Bewertungen
- Cardiac ArrestDokument19 SeitenCardiac ArrestHaimelien De LimosNoch keine Bewertungen
- Drug of ChoiceDokument2 SeitenDrug of ChoiceRia Tiglao Fortugaliza100% (1)