Beruflich Dokumente
Kultur Dokumente
Chronic Bronchitis
Hochgeladen von
Eimhie Lee Casi0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
21 Ansichten2 Seitenbroncho notes
Copyright
© © All Rights Reserved
Verfügbare Formate
DOC, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenbroncho notes
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOC, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
21 Ansichten2 SeitenChronic Bronchitis
Hochgeladen von
Eimhie Lee Casibroncho notes
Copyright:
© All Rights Reserved
Verfügbare Formate
Als DOC, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 2
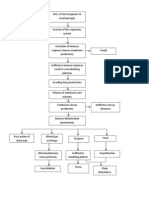
Chronic Bronchitis
Is an inflammation of the lower airways
characterized by excessive secretion of mucus,
hypertrophy of mucous glands, and recurring
infection, progressing to narrowing and
obstruction of airflow.
Assessment:
1. Signs and symptoms of chronic bronchitis
(insidious onset):
Productive cough lasting at least 3 months
during a year for 2 successive years.
Thick, gelatinous sputum (greater amounts produced during superimposed infections).
Dyspnea and wheezing as disease progresses.
Diagnostic Evaluation:
1. Pulmonary function tests, to demonstrate airflow obstruction-reduced forced
expiratory volume in 1 second (FEV1), FEV1 to forced vital capacity ratio; increased
residual volume to total lung capacity (TLC) ration, possibly increased TLC.
2. Chest X-rays to detect hyperinflation, flattened diaphragm, increased retrosternal space,
decreased vascular markings, possible bullae (all in late stages).
3. Arterial blood gases, to detect decreased arterial oxygen pressure (PaO2), pH, and
increased arterial carbon dioxide pressure (Paco2).
4. Sputum smears and cultures to identify pathogens.
Therapeutic and Surgical Interventions:
1. Smoking cessation to stop the progression and preserve lung capacity.
2. Low-flow oxygen to correct severe hypoxemia in a controlled manner and minimize
carbon dioxide retention.
3. Home oxygen therapy, especially at night to prevent turnal oxygen desaturation.
4. Pulmonary rehabilitation to reduce symptoms that limit activity.
5. Chest physical therapy, including postural drainage and breathing retraining.
6. Lung transplant in severe cases of alpha1-antitrypsin deficiency.
Pharmacologic Intervention:
1. Bronchodilators to reduce dyspnea and control bronchospasm delivered by metered-dose
inhaler, other handheld devices, or nebulization.
2. Inhaled corticosteriods may be useful for some with severe airflow limitation and
frequent exacerbations.
3. Corticosteroids by mouth or I.V. in acute exacerbations.
4. Antimicrobials to control secondary bacterial infections in the bronchial tree, thus
clearing the airways.
5. Alpha1-antitrypsin replacement delivered by I.V. infusion.
Nursing Interventions:
1. Monitor for adverse effects of bronchodilators-tremulousness, tachycardia, cardiac
arrhythmias, central nervous system stimulation, hypertension.
2. Monitor oxygen saturation at rest and with activity.
3. Eliminate all pulmonary irritants, particularly cigarette smoke. Smoking cessation usually
reduces pulmonary irritation, sputum production, and cough. Keep the patient’s room as
dust-free as possible.
4. Use postural drainage positions to help clear secretions responsible for airway
obstruction.
5. Teach controlled coughing.
6. Encourage high level of fluid intake (8 to 10 glasses; 2 to 2.5 L daily) within level of
cardiac reserve.
7. Give inhalations of nebulized saline to humidify bronchial tree and liquefy sputum. Add
moisture (humidifier, vaporizer) to indoor air.
8. Avoid dairy products if these increase sputum production.
9. Encourage the patient to assume comfortable position to decrease dyspnea.
10. Use pursed lip breathing at intervals and during periods of dyspnea to control rate and
depth of respiration and improve respiratory muscle coordination.
11. Discuss and demonstrates relaxation exercises to reduce stress, tension, and anxiety.
12. Encourage frequent small meals if the patient is dyspneic; en a small increase in
abdominal contents may press on diaphragm and impede breathing.
13. Offer liquid nutritional supplements to improve caloric intake and counteract weight loss.
14. Avoid foods producing abdominal discomfort.
15. Encourage use of portable oxygen system for ambulation for patients with hypoxemia
and marked disability.
16. Encourage the patient in energy conservation techniques.
Das könnte Ihnen auch gefallen
- Woman With PneumoniaDokument9 SeitenWoman With PneumoniaNohaira SADANGNoch keine Bewertungen
- Bronchospasm PR 1Dokument41 SeitenBronchospasm PR 1teklayNoch keine Bewertungen
- Respiratory System MedicationsDokument2 SeitenRespiratory System Medicationsmlbrown8Noch keine Bewertungen
- Acute Bronchitis - StatPearls - NCBI BookshelfDokument7 SeitenAcute Bronchitis - StatPearls - NCBI BookshelfCynthia ChezanNoch keine Bewertungen
- Patho Exam 3: Deficiency in Alpha-1-Antitrypsin-Unchecked Elastase Destruction of The AlveoliDokument5 SeitenPatho Exam 3: Deficiency in Alpha-1-Antitrypsin-Unchecked Elastase Destruction of The AlveoliTaran LuthraNoch keine Bewertungen
- Infectious Disease MedicationsDokument8 SeitenInfectious Disease MedicationsSheril MarekNoch keine Bewertungen
- Ajnr 7 4 2 PDFDokument8 SeitenAjnr 7 4 2 PDFniaNoch keine Bewertungen
- Jurnal GGDokument11 SeitenJurnal GGKanesti KamajayaNoch keine Bewertungen
- Chronic Obstructive Lung Disease (Copd)Dokument32 SeitenChronic Obstructive Lung Disease (Copd)manal at100% (1)
- Chronic BronchitisDokument5 SeitenChronic BronchitisJemalyn M. Saludar100% (2)
- Bronchitis: Week 5 1Dokument5 SeitenBronchitis: Week 5 1jessNoch keine Bewertungen
- Lung Metabolism: Proteolysis and Antioproteolysis Biochemical Pharmacology Handling of Bioactive SubstancesVon EverandLung Metabolism: Proteolysis and Antioproteolysis Biochemical Pharmacology Handling of Bioactive SubstancesAlain JunodNoch keine Bewertungen
- Pathophysiology PneumoniaDokument1 SeitePathophysiology PneumoniaMajkel Benche CustodioNoch keine Bewertungen
- Blue Bloaters and Pink PuffersDokument2 SeitenBlue Bloaters and Pink PuffersAlmir SaraciNoch keine Bewertungen
- Respiration 16 Respiratory FailureDokument31 SeitenRespiration 16 Respiratory Failureapi-19641337Noch keine Bewertungen
- Pulmonary PathoPhysiologyDokument45 SeitenPulmonary PathoPhysiologySuliman Garalleh100% (1)
- Mechanical Ventilation and Intracranial PressureDokument30 SeitenMechanical Ventilation and Intracranial PressureFlavius AnghelNoch keine Bewertungen
- Noninvasive VentilationDokument6 SeitenNoninvasive VentilationEma MagfirahNoch keine Bewertungen
- Ards and RF FileDokument12 SeitenArds and RF FileEdwin Delos Reyes Abu100% (1)
- Respiratory EmergenciesDokument34 SeitenRespiratory EmergenciesRoshana MallawaarachchiNoch keine Bewertungen
- Breathing and Exchange of GasesDokument5 SeitenBreathing and Exchange of Gaseslpc4944Noch keine Bewertungen
- What's New in Respiratory DisordersDokument4 SeitenWhat's New in Respiratory DisorderssobanNoch keine Bewertungen
- Mechanical Ventilation TherapyDokument17 SeitenMechanical Ventilation TherapyFaizal FlNoch keine Bewertungen
- Impaired Gas ExchangeDokument4 SeitenImpaired Gas ExchangeNuraini Hamzah100% (1)
- Midterm Last TopicDokument3 SeitenMidterm Last TopicLynette BalodNoch keine Bewertungen
- Oxygenation NCM 103Dokument10 SeitenOxygenation NCM 103Richmond LacadenNoch keine Bewertungen
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsVon EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsNoch keine Bewertungen
- Asthma and CopdDokument44 SeitenAsthma and CopdBeer Dilacshe100% (1)
- Deep-Breathing Exercises Reduce PDFDokument9 SeitenDeep-Breathing Exercises Reduce PDFAde PayNoch keine Bewertungen
- 406 - Respiratory Therapy Consult Service HandbookDokument28 Seiten406 - Respiratory Therapy Consult Service HandbookIkhsan JohnsonNoch keine Bewertungen
- RT 220 B C AirwaystudyguideDokument25 SeitenRT 220 B C Airwaystudyguiderpebdani0% (2)
- Airway Skills 2 - Bag Valve MaskDokument4 SeitenAirway Skills 2 - Bag Valve MaskRinna MauLiddaNoch keine Bewertungen
- COPD Acute Management ABCDEDokument11 SeitenCOPD Acute Management ABCDESSNoch keine Bewertungen
- Mechanical Ventilation: Standard Weaning Criteria (Respiratory Therapy)Dokument6 SeitenMechanical Ventilation: Standard Weaning Criteria (Respiratory Therapy)S3DOSHA osmanNoch keine Bewertungen
- Discussion QuestionsDokument2 SeitenDiscussion QuestionsMary RiasNoch keine Bewertungen
- ICU Scoring Systems A Complete Guide - 2020 EditionVon EverandICU Scoring Systems A Complete Guide - 2020 EditionNoch keine Bewertungen
- Riding The WavesDokument76 SeitenRiding The WavesMedic03431Noch keine Bewertungen
- Types of InhalersDokument23 SeitenTypes of Inhalersshamie1110Noch keine Bewertungen
- Effects of HypoxiaDokument6 SeitenEffects of HypoxiaMaria TelloNoch keine Bewertungen
- #6 Copd 11 PDFDokument11 Seiten#6 Copd 11 PDFOmar BasimNoch keine Bewertungen
- NURSING CARE OF ADULTS II: Passbooks Study GuideVon EverandNURSING CARE OF ADULTS II: Passbooks Study GuideNoch keine Bewertungen
- Tracheostomy SuctioningDokument10 SeitenTracheostomy SuctioningJANIEZA ANGEL RA�ISES BALTAZARNoch keine Bewertungen
- Suctioning Artificial Airways - AdultsDokument27 SeitenSuctioning Artificial Airways - AdultssdaNoch keine Bewertungen
- Acuterespiratorydistress Syndrome: Ventilator Management and Rescue TherapiesDokument16 SeitenAcuterespiratorydistress Syndrome: Ventilator Management and Rescue TherapiessamuelNoch keine Bewertungen
- What Is Respiratory Alkalosis?Dokument3 SeitenWhat Is Respiratory Alkalosis?Lorenn AdarnaNoch keine Bewertungen
- Pneumonia: DefinitionDokument5 SeitenPneumonia: DefinitionhemaanandhyNoch keine Bewertungen
- Suctioning TracheaDokument24 SeitenSuctioning Trachealuis_chubee100% (1)
- PepDokument18 SeitenPepAdrian DedicNoch keine Bewertungen
- CopdDokument14 SeitenCopdMohd Farid Bin RosliNoch keine Bewertungen
- Walking Pneumonia, (Mycoplasma Pneumonia) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandWalking Pneumonia, (Mycoplasma Pneumonia) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Registered Respiratory TherapistDokument3 SeitenRegistered Respiratory Therapistapi-76909521Noch keine Bewertungen
- Aerosoltherapy Nebu 120503115712 Phpapp01Dokument65 SeitenAerosoltherapy Nebu 120503115712 Phpapp01Aan Ika SugathotNoch keine Bewertungen
- ARDSDokument27 SeitenARDSChloie Marie RosalejosNoch keine Bewertungen
- Vascular Responses to PathogensVon EverandVascular Responses to PathogensFelicity N.E. GavinsNoch keine Bewertungen
- Nursing DiagnosisDokument4 SeitenNursing DiagnosisKrizzia CarlosNoch keine Bewertungen
- Lung AuscultationDokument62 SeitenLung AuscultationOlea CroitorNoch keine Bewertungen
- Rapid Sequence InductionDokument8 SeitenRapid Sequence InductionAngela Mitchelle NyanganNoch keine Bewertungen
- Copd HandoutDokument6 SeitenCopd Handoutapi-272951876Noch keine Bewertungen
- Prognosis MGDokument7 SeitenPrognosis MGPutri Cindy Claudia PandoyoNoch keine Bewertungen
- Pulmo GuideDokument1 SeitePulmo GuideEimhie Lee CasiNoch keine Bewertungen
- Sample 2Dokument2 SeitenSample 2Eimhie Lee CasiNoch keine Bewertungen
- Pain ManagementDokument18 SeitenPain ManagementEimhie Lee CasiNoch keine Bewertungen
- Emergency Drugs Used in Different CasesDokument60 SeitenEmergency Drugs Used in Different CasesEimhie Lee CasiNoch keine Bewertungen
- Lab Test SampleDokument2 SeitenLab Test SampleEimhie Lee CasiNoch keine Bewertungen
- Cardiovascular Agent: Prof. Clement Belvis RN, RM, MPHDokument86 SeitenCardiovascular Agent: Prof. Clement Belvis RN, RM, MPHEimhie Lee CasiNoch keine Bewertungen
- GIT AgentsDokument51 SeitenGIT AgentsEimhie Lee CasiNoch keine Bewertungen
- Clinic 1-Materilas: Materials Brand Quantity Expirartion DateDokument3 SeitenClinic 1-Materilas: Materials Brand Quantity Expirartion DateEimhie Lee CasiNoch keine Bewertungen
- Definition:: GingivitisDokument6 SeitenDefinition:: GingivitisEimhie Lee CasiNoch keine Bewertungen
- ComputationDokument3 SeitenComputationEimhie Lee CasiNoch keine Bewertungen
- Lower Respiratory Tract Upper Respiratory Tract Infection Bacterial InfectionDokument2 SeitenLower Respiratory Tract Upper Respiratory Tract Infection Bacterial InfectionEimhie Lee CasiNoch keine Bewertungen
- Clinic Report FormDokument1 SeiteClinic Report FormEimhie Lee CasiNoch keine Bewertungen
- Completion FormDokument2 SeitenCompletion FormEimhie Lee CasiNoch keine Bewertungen
- Focus ChartingDokument2 SeitenFocus ChartingIrvin John Diao Capistrano100% (1)
- Abdul Aziz Albalood (1240) : Sinus Lifting and Implant For ToothDokument1 SeiteAbdul Aziz Albalood (1240) : Sinus Lifting and Implant For ToothEimhie Lee CasiNoch keine Bewertungen
- Patient Consent Form ARABICDokument2 SeitenPatient Consent Form ARABICEimhie Lee CasiNoch keine Bewertungen
- Restoration of Endodontically Treated Tooth 97Dokument43 SeitenRestoration of Endodontically Treated Tooth 97Eimhie Lee CasiNoch keine Bewertungen
- 3M Monophase 3M STD PuttyDokument3 Seiten3M Monophase 3M STD PuttyEimhie Lee CasiNoch keine Bewertungen
- PRINt DrugsDokument1 SeitePRINt DrugsEimhie Lee CasiNoch keine Bewertungen
- BudgetDokument4 SeitenBudgetEimhie Lee CasiNoch keine Bewertungen
- Evidence Based Nursing: Musculoskeletal DisorderDokument8 SeitenEvidence Based Nursing: Musculoskeletal DisorderEimhie Lee CasiNoch keine Bewertungen
- Evidence Based Nursing: Batch 2011Dokument7 SeitenEvidence Based Nursing: Batch 2011Eimhie Lee CasiNoch keine Bewertungen
- Binder 1Dokument107 SeitenBinder 1Ana Maria Gálvez Velasquez0% (1)
- PlsqldocDokument21 SeitenPlsqldocAbhishekNoch keine Bewertungen
- SC-Rape-Sole Testimony of Prosecutrix If Reliable, Is Sufficient For Conviction. 12.08.2021Dokument5 SeitenSC-Rape-Sole Testimony of Prosecutrix If Reliable, Is Sufficient For Conviction. 12.08.2021Sanjeev kumarNoch keine Bewertungen
- Petitioner's Response To Show CauseDokument95 SeitenPetitioner's Response To Show CauseNeil GillespieNoch keine Bewertungen
- CNG Fabrication Certificate16217Dokument1 SeiteCNG Fabrication Certificate16217pune2019officeNoch keine Bewertungen
- Practical GAD (1-32) Roll No.20IF227Dokument97 SeitenPractical GAD (1-32) Roll No.20IF22720IF135 Anant PatilNoch keine Bewertungen
- Human Resource Management by John Ivancevich PDFDokument656 SeitenHuman Resource Management by John Ivancevich PDFHaroldM.MagallanesNoch keine Bewertungen
- Active Directory FactsDokument171 SeitenActive Directory FactsVincent HiltonNoch keine Bewertungen
- Descriptive Statistics - SPSS Annotated OutputDokument13 SeitenDescriptive Statistics - SPSS Annotated OutputLAM NGUYEN VO PHINoch keine Bewertungen
- A Winning Formula: Debrief For The Asda Case (Chapter 14, Shaping Implementation Strategies) The Asda CaseDokument6 SeitenA Winning Formula: Debrief For The Asda Case (Chapter 14, Shaping Implementation Strategies) The Asda CaseSpend ThriftNoch keine Bewertungen
- Gmo EssayDokument4 SeitenGmo Essayapi-270707439Noch keine Bewertungen
- Week 7 Apple Case Study FinalDokument18 SeitenWeek 7 Apple Case Study Finalgopika surendranathNoch keine Bewertungen
- IEEE Conference Template ExampleDokument14 SeitenIEEE Conference Template ExampleEmilyNoch keine Bewertungen
- Data Mining - Exercise 2Dokument30 SeitenData Mining - Exercise 2Kiều Trần Nguyễn DiễmNoch keine Bewertungen
- Scope: Provisional Method - 1994 © 1984 TAPPIDokument3 SeitenScope: Provisional Method - 1994 © 1984 TAPPIМаркус СилваNoch keine Bewertungen
- The Concept of ElasticityDokument19 SeitenThe Concept of ElasticityVienRiveraNoch keine Bewertungen
- An Over View of Andhra Pradesh Water Sector Improvement Project (APWSIP)Dokument18 SeitenAn Over View of Andhra Pradesh Water Sector Improvement Project (APWSIP)gurumurthy38Noch keine Bewertungen
- Ms Microsoft Office - WordDokument3 SeitenMs Microsoft Office - WordFarisha NasirNoch keine Bewertungen
- Hitt PPT 12e ch08-SMDokument32 SeitenHitt PPT 12e ch08-SMHananie NanieNoch keine Bewertungen
- Rs 422Dokument1 SeiteRs 422rezakaihaniNoch keine Bewertungen
- A Survey On Multicarrier Communications Prototype PDFDokument28 SeitenA Survey On Multicarrier Communications Prototype PDFDrAbdallah NasserNoch keine Bewertungen
- Economies and Diseconomies of ScaleDokument7 SeitenEconomies and Diseconomies of Scale2154 taibakhatunNoch keine Bewertungen
- Majalah Remaja Islam Drise #09 by Majalah Drise - Issuu PDFDokument1 SeiteMajalah Remaja Islam Drise #09 by Majalah Drise - Issuu PDFBalqis Ar-Rubayyi' Binti HasanNoch keine Bewertungen
- Projects: Term ProjectDokument2 SeitenProjects: Term ProjectCoursePinNoch keine Bewertungen
- The "Solid Mount": Installation InstructionsDokument1 SeiteThe "Solid Mount": Installation InstructionsCraig MathenyNoch keine Bewertungen
- Lexington School District Two Return To School GuideDokument20 SeitenLexington School District Two Return To School GuideWLTXNoch keine Bewertungen
- Agreement Deed BangladeshDokument8 SeitenAgreement Deed BangladeshVabna EnterpriseNoch keine Bewertungen
- Random Variable N N Mean or Expected Value: Number of Ducks Type of Duck AmountDokument2 SeitenRandom Variable N N Mean or Expected Value: Number of Ducks Type of Duck AmountAngie PastorNoch keine Bewertungen
- YeetDokument8 SeitenYeetBeLoopersNoch keine Bewertungen
- Assessment 21GES1475Dokument4 SeitenAssessment 21GES1475kavindupunsara02Noch keine Bewertungen