Beruflich Dokumente
Kultur Dokumente
Evaluation and Treatment of Posterior Neck Pain in Family Practice
Hochgeladen von
danny17phCopyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Evaluation and Treatment of Posterior Neck Pain in Family Practice
Hochgeladen von
danny17phCopyright:
Verfügbare Formate
Evaluation and Treatment of Posterior Neck Pain in
Family Practice
Alan B. Douglass, MD, and Edward T. Bope, MD
Neck pain is almost universal and is a common patient complaint. Although the differential diagnosis is
extensive, most symptoms are from biomechanical sources, such as axial neck pain, whiplash-associated
disorder (WAD), and radiculopathy. Most symptoms abate quickly with little intervention. There is rela-
tively little high-quality treatment evidence available, and no consensus on management of axial neck
pain or radiculopathy. A number of general pain management guidelines are applicable to neck pain,
and specific guidelines are available on the management of WAD. The goal of diagnosis is to identify the
anatomic pain generator(s). Patient history and examination are important in distinguishing potential
causes and identifying red flags. Diagnostic imaging should be ordered only when necessary because of
the high incidence of asymptomatic radiographic abnormalities. First-line drug treatments include acet-
aminophen, cyclo-oxygenase 2–specific inhibitors, or nonsteroidal anti-inflammatory drugs. Short-term
use of muscle relaxants may be considered. Opioids should be used if other treatments are ineffective
and continued if improved function outweighs impairment. Adjuvant antidepressants and anticonvul-
sants should be considered in chronic or neuropathic pain and coincident depression. Epidural steroids
should be considered only in radiculopathy. Physical modalities supported by evidence should be used.
If symptoms have not resolved in 4 to 6 weeks, re-evaluation and additional workup should be consid-
ered. (J Am Board Fam Pract 2004;17:S13–22.)
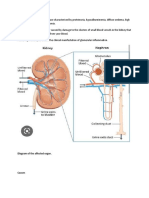
The human neck is a complex structure that is functioning that any disruption in its normal func-
highly susceptible to irritation. In fact, 10% of tion is quickly noticed.
people will have neck pain in any given month.1
Potential pain generators include bones, muscles, Differential Diagnosis
ligaments, facet joints, and intervertebral discs Neck pain has an extensive differential diagnosis
(Figure 1). Almost any injury or disease process (Table 1). By far, the most common causes are
within the neck or adjacent structures will result in biomechanical: axial neck pain, whiplash-associated
reflexive protective muscle spasm and loss of mo- disorder (WAD), and cervical radiculopathy. Much
tion. Gradual collapse of the intervertebral discs less common causes include cervical myelopathy
and degeneration of the facet joints is a universal caused by spinal cord compression, infection, neo-
part of the aging process and, in some people, can plasms, rheumatic causes (ankylosing spondylitis,
lead to nerve or spinal cord impingement. Further, spondyloarthropathies, rheumatoid arthritis, and
neck mobility is so important to normal human diffuse idiopathic skeletal hyperostosis), torticollis,
cervical dystonia, and major trauma, including frac-
tures, dislocations, and cord injuries. Pain also may
From the Family Practice Residency Program, Middlesex be referred to the neck from other sources, such as
Hospital, Middletown, CT (ABD), and Riverside Family
Practice Residency Program, Riverside Methodist Hospital, shoulder disorders, thoracic outlet syndrome,
Columbus, OH (ETB). Address correspondence to Alan B. esophagitis, angina, and vascular dissection. Neck
Douglass, MD, FAAFP, Family Practice Residency Pro- pain may also present as part of complex general-
gram, Middlesex Hospital, 90 South Main Street, Middle-
town, CT 06457 (e-mail: alan_douglass_md@midhosp.org). ized pain syndromes such as fibromyalgia.
The Family Practice Pain Education Project (FP-PEP)
acknowledges an unrestricted educational grant from Pfizer
to Cardinal Health to produce educational materials for Definitions
primary care doctors about pain management. The informa-
tion provided here is the opinions and research of the family This article focuses on the 3 most common sources
physicians who served on FP-PEP. of neck pain that are encountered by primary care
This work was presented in part at the 2003 American
Academy of Family Physicians (AAFP) Scientific Sympo- physicians: axial neck pain, WAD, and cervical ra-
sium. diculopathy. Cervical myelopathy is briefly dis-
http://www.jabfp.org Management of Neck Pain S13
Figure 1. Normal neck anatomy.
cussed as well because of its importance in the Whiplash-associated disorder (WAD) is a special
differential diagnosis of neck pain. case of acute or subacute neck pain resulting from
Axial neck pain (also known as uncomplicated acceleration/deceleration transfer of energy to the
neck pain and cervical strain) is the result of the neck. Multiple pain generators are usually involved,
complex interaction of muscular and ligamentous including myofascial, ligamentous, discogenic, and
factors related to posture, sleep habits, ergonomics facet joint sources. It most commonly occurs in
such as computer monitor and bifocal position, rear-end motor vehicle crashes, but can occur from
stress, chronic muscle fatigue, postural adaptation other causes, such as diving injuries. The Quebec
to other primary pain sources (shoulder, temporo- Classification of Whiplash-Associated Disorders
mandibular joint, craniocervical), or degenerative identifies 4 categories of injury2: grade I comprises
changes of the cervical discs or facet joints. The general, nonspecific complaints regarding the neck,
ICD-9 code is 723.1. such as pain, stiffness, or soreness without objective
physical findings; grade II comprises neck com-
Table 1. Differential Diagnosis of Neck Pain plaints plus signs limited to musculoskeletal struc-
tures; grade III comprises neck complaints plus
Biomechanical causes
neurologic signs; and grade IV comprises neck pain
Axial neck pain
Whiplash associated disorder (WAD)
plus fracture or dislocation and is beyond the scope
Radiculopathy
of this paper. All subsequent discussion of WAD
Cervical myelopathy assumes that fracture, subluxation, and cord injury
Infection have been ruled out. The ICD-9 code is 847.0.
Neoplasm Cervical radiculopathy is motor and/or sensory
Rheumatic causes changes in the neck and arms resulting from ex-
Rheumatoid arthritis trinsic pressure on a cervical nerve root, usually by
Ankylosing spondylitis osteophytes or disk material. The pathology under-
Spondyloarthropathies lying the symptoms is heterogeneous. Seventy to
Diffuse idiopathic skeletal hyperostosis ninety percent of cases are associated with forami-
Dystonia nal encroachment by degenerative bony changes;
Trauma
herniated disk material is present in most of the
Torticollis
remainder.3 An inflammatory response is probably
Referred pain
necessary for the initiation of symptoms.4 The
Fibromyalgia
ICD-9 code is 723.4.
S14 JABFP November–December 2004 Vol. 17 Supplement http://www.jabfp.org
Myelopathy is the manifestation of long tract hand, 85% of people who are symptomatic 3
signs resulting from a decrease in the space avail- months after an accident will remain so after 2
able in the cervical canal for the spinal cord. A years.17
number of factors contribute to extrinsic pressure, A large, population-based study in Rochester,
including the congenital cord diameter, osteo- Minnesota, noted the annual incidence of cervical
phytes, protruding disk material, dynamic changes radicular symptoms to be 83.2 per 100,000 popu-
in canal diameter and the cord itself, and the vas- lation, peaking in the 50- to 54-year age-group.3
cular supply to the cord.4 The ICD-9 code is 721.1. Many patients will have resolution of symptoms
without surgery. In the Rochester study at a mean
follow-up of 5.9 years, 90% of patients were
Prevalence and Natural History asymptomatic or only mildly incapacitated. Refer-
Neck pain is an extremely common but nonspecific ral center-based studies have shown somewhat less
symptom. In a population-specific study, Cote et al positive outcomes.
found that 66% of Saskatchewan adults experi- The overall prevalence of cervical myelopathy is
enced neck pain at some point in their lifetimes, unknown, but it is relatively rare and the natural
54% in the most recent 6 months.5 The prevalence history of the disorder in any one person is unpre-
of neck pain at any point in time is approximately dictable. However, a number of studies have doc-
9%.1 Prevalence increases with age and is higher in umented progressive deterioration without sur-
women than in men.6 Neck pain accounts for al- gery.4 In one recent study of patients who
most 1% of all visits to primary care physicians in underwent laminectomy and posterior fusion, 80%
the United States.7 had good outcomes, 76% had improvement in my-
Axial neck pain is the most common cause of elopathy scores, and no late neurological deterio-
neck pain and has a high rate of spontaneous res- ration in any group was documented at mean
olution. In one study, after 3 months of nonopera- follow-up of 4 years.18
tive care, 70% had complete or partial relief.8 With
time, most patients achieve relief. In another study, Presenting Symptoms
at the 10- to 25-year follow-up, 43% experienced Axial neck pain and WAD typically present as pain
complete resolution, 25% mild residual pain, and or soreness in the posterior paramedian neck mus-
32% moderate or severe residual pain.9 cles, with radiation to the occiput, shoulder, or
In the United States, 1 million cases of WAD parascapular region. Stiffness in one or more direc-
occur annually as a result of motor vehicle acci- tions of motion and headache are common. Axial
dents.10 Prognostic data are variable, but in one neck pain and WAD can be associated with local
large study, 60% of patient symptoms resolved warmth or tingling. Localized areas of muscle ten-
within 1 month.11 The incidence of chronic symp- derness (trigger points) may develop.
toms after acute WAD varies widely among cul- Radicular pain is sharp, tingling, or burning in a
tures and countries,2 and lively medical debate is specific dermatomal distribution in the upper ex-
ongoing about the diagnosis of chronic WAD.12,13 tremity. In clinical practice it is often confused with
There is sparse evidence for a causal link between radiating pain. However, because there are specific
the mechanism of WAD injury and chronic symp- treatments indicated only for radicular pain, an
toms.14 Some authors feel that the symptoms of accurate distinction must be made. True radicular
WAD are often reinforced by legal and social fac- pain follows dermatomal patterns (Figure 2) which
tors.13 It is interesting that in Lithuania, where can be somewhat variable among patients and is
there is little involvement of insurance companies usually, but not always, unilateral. Onset is often
or the legal system in motor vehicle injuries, no insidious but may be abrupt. It is frequently aggra-
difference was found in persistent neck symptoms vated by arm position and extension or lateral ro-
between rear-end-crash victims and uninjured con- tation of the head. In one study of 736 patients,
trols.15 Nonetheless, in 11 high-quality studies, 99% had arm pain, 85% had sensory deficits, 79%
19% to 60% (mean, 33%) of patients with WAD had neck pain, 71% had reflex deficits, 68% had
reported chronic symptoms.16 Overall, 7% of peo- motor deficits, and 52% had scapular pain.19
ple who are asymptomatic 3 months after an acci- Cervical myelopathy has a subtle and varied pre-
dent will have symptoms after 2 years. On the other sentation necessitating a high degree of clinical
http://www.jabfp.org Management of Neck Pain S15
Despite the availability of guidelines, there is no
clear consensus on the management of axial neck
pain or radiculopathy. Clinicians commonly use
multiple medications and modalities empirically,
often without clear evidence supporting their effi-
cacy.
Evaluation of Patients With Neck Pain
History and Physical Examination
A careful history can yield a diagnosis, or at least
categorization of symptoms, in the majority of pa-
tients. History should focus on the mechanism of
injury (if any) and on symptoms. Any prior neck
trauma or symptoms should be noted. Clinicians
should be alert for a number of red flags for poten-
tially serious conditions requiring prompt diagnosis
and management. Morning stiffness that improves
over the course of the day is sometimes indicative
of rheumatic causes. Fever, weight loss, night
sweats, and other systemic symptoms are indicative
Figure 2. Dermatomal pattern of radicular pain. of infection or neoplasm. Unremitting night pain,
especially in the context of a prior history of ma-
lignancy, may be secondary to a bony tumor. Gait
suspicion. Patients may present with subtle findings disturbance, balance problems, sphincter dysfunc-
that have been present for years, or with acute tion, or loss of coordination suggests myelopathy.
paresis. They typically complain of insidious clum- Patients should be carefully questioned about past
siness, weakness, or stiffness in the upper and lower treatment successes and failures.
extremities. Deep, aching pain in the neck, shoul- A careful physical examination is vital for differ-
der, or arm and neck stiffness are common but entiating potential causes. Inspection should focus
occur in less than half of patients. Associated radic- on posture, ease of movement, and visible deformi-
ular symptoms occur in one third of patients. Arm ties. Palpation of soft tissue and bony and other
or leg dysfunction and gait and balance difficulties cervical structures such as thyroid, lymph nodes,
are common. Nonspecific urinary complaints, such and salivary glands should be performed. Cervical
as urgency or hesitancy, can occur, but frank uri- range of motion in flexion, extension, lateral bend-
nary or fecal incontinence is unusual.4,20 ing, and rotation should be noted, along with
shoulder range of motion. Neurologic examination
of sensory and motor function as well as reflexes is
Current Standards of Care vital. Several special maneuvers can be helpful. Ax-
Currently available guidelines specific to neck pain ial loading of the neck while the head is extended
include the Quebec (Canada),2 and New South and rotated (Spurling maneuver) will often provoke
Wales (Australia)21 WAD Guidelines; Prodigy radicular pain. Placing the affected hand on top of
Guidance on Neck Pain (United Kingdom) 22; and the head (abduction relief sign) takes stretch off of
the Philadelphia Panel guidelines on rehabilitation the affected nerve root and may decrease or relieve
interventions (United States).23 A number of gen- radicular symptoms. An electric shock sensation
eral pain diagnostic and management guidelines down the center of the back after neck flexion
applicable to neck pain are also available, including (Lhermitte sign) is indicative of cervical spinal cord
those from the American Geriatrics Society,24 the pathology such as cervical myelopathy.
American Academy of Physical Medicine and Re-
habilitation,25 the American Pain Society,26 the Diagnostic Imaging
American College of Rheumatology,27 and the Diagnostic imaging in neck pain can be misleading,
American Society of Anesthesiologists.28 in that it frequently identifies abnormalities that are
S16 JABFP November–December 2004 Vol. 17 Supplement http://www.jabfp.org
Figure 3. Algorithm for the management of patients with neck pain.
not contributory to current symptoms. One study resolved in 6 to 8 weeks (recommendation strength
of radiographs of asymptomatic persons between B).34
50 and 65 years of age demonstrated that 79% of
subjects had disk space narrowing, endplate sclero-
sis, or osteophytes.29 Another study of magnetic Management of the Patient With Neck Pain
resonance images revealed major abnormalities, Figure 3 displays an algorithmic approach to the
such as bulging or herniated discs, foraminal ste- management of patients with neck pain. The his-
nosis, disk space narrowing, or abnormal cord sig-
tory and physical examination serve as a triage
nal in 14% of asymptomatic subjects younger than
point to divide patients into 5 categories based on
40 years and in 28% older than 40 years.30
the suspected cause of their symptoms. The follow-
Radiographs are recommended in patients with
ing section reviews the evidence underlying the
WAD grade III or suspected grade IV (grade IV
management recommendations for each category
cannot be diagnosed without an radiograph) and in
laid out in the algorithm.
patients with a history of trauma (recommendation
strength A). Detailed guidelines for radiograph se-
lection in patients with blunt neck trauma are avail-
able, including the Canadian C-spine rule, NEXUS Review of the Evidence
decision instruments, and American College of Ra- In the management of neck pain, clinical practice
diology Appropriateness Criteria.31–33 Plain radio- has far outpaced the literature supporting what is
graphs also should be considered in patients with commonly done. There is relatively little high-
axial neck pain unresponsive to 6 to 8 weeks of quality evidence specific to the treatment of neck
conservative treatment; however, no clear guide- pain. In fact, there are almost as many reviews as
lines are available. Magnetic resonance imaging there are controlled trials of therapies; for many
should be performed if myelopathy, infection, or interventions, there is no concordance in the con-
neoplasm is suspected; in patients with radicular clusions drawn by reviewers. Few studies have been
pain associated with motor or reflex deficits; and in made of the long-term effects of treatments for
patients with radicular symptoms that have not neck pain.
http://www.jabfp.org Management of Neck Pain S17
Drug Therapies this class.37 Baclofen and tizanidine may have less
Because of a paucity of high-quality studies of drug potential for addiction than other muscle relaxants.
therapy specific to neck pain, much of the following Muscle relaxants are not recommended for acute
information has been extrapolated from the treat- phase WAD because of limited evidence of effi-
ment of pain from other causes, largely low back cacy.2,21
pain.
Opioids
Acetaminophen
An extensive body of literature documents the
The use of full-dose (2 to 4 g per day) acetamino-
short-term effectiveness of opioids in a variety of
phen as a first-line therapy is supported by strong
pain syndromes (recommendation strength A).
evidence and several major sets of guidelines (rec-
However, no high-quality, randomized, controlled
ommendation strength A).24,26 It should be recog-
trials of sufficient length exist to demonstrate long-
nized that in alcoholism, fasting states, hepatic dis-
term efficacy and safety for any indication.25 The
ease, the presence of certain medications (especially
usefulness of opioids in neck pain must be balanced
anticonvulsants), or in the frail elderly, liver toxicity
against adverse effects such as constipation, seda-
can occur at recommended doses.35 Furthermore,
tion, and physiologic dependence. Several major
acetaminophen toxicity increases substantially
recommending bodies support the use of opioids in
when it is taken in conjunction with a cyclo-oxy-
a variety of pain syndromes when other strategies
genase (COX-2)-specific inhibitor or nonsteroidal
do not provide adequate pain relief, and there is
anti-inflammatory drug (NSAID).36
clear evidence that they do not impair the patient
and produce significant and sustained improve-
NSAIDs
ment.25,28
There is strong evidence of efficacy in acute pain
and moderate evidence in chronic pain (recommen-
dation strength A). NSAIDs are recommended by Adjuvant Antidepressants and Anticonvulsants
most major sets of guidelines. The efficacy of all Although there are no good quality randomized,
NSAIDs seems to be roughly equivalent.37 Weigh- controlled trials of the use of these agents specifi-
ing efficacy versus adverse effects, the American cally in neck pain, their use, especially in chronic
Geriatrics Society recommends COX-2 inhibitors and neuropathic pain, is widely supported by the
as first-line therapy over traditional NSAIDs.24 literature (recommendation strength A) and all
Nonacetylated salicylates (choline magnesium major sets of general pain management guide-
trisalicylate, salsalate) are effective and may have lines.24 –26,28 It should also be noted that in chronic
fewer gastrointestinal side effects than traditional pain syndromes, coincident depression is frequent,
NSAIDs at a lower cost than more selective and aggressive treatment of depression can often be
agents.24,26 If traditional NSAIDs are chosen, gas- of benefit.
tric cytoprotection should be considered based on
the patient’s risk profile. NSAIDs should be par-
Sedative Hypnotics
ticularly considered when inflammation is believed
No high-quality randomized, controlled trials of
to be playing a substantial role in the production of
sufficient length exist to demonstrate long-term
the pain process.
efficacy and safety in any pain syndrome.25 Other
than relieving pain specifically caused by muscle
Muscle Relaxants
spasm, they are otherwise not effective analgesics.26
Evidence supporting the use of muscle relaxants is
mixed (evidence strength B). A review of 14
moderate-quality randomized, controlled trials Trigger Point Injections
showed that cyclobenzaprine was more effective Although widely used, evidence of efficacy is cur-
than placebo in the management of neck and back rently lacking.25,37 A single randomized trial, albeit
pain. However, the effect was modest and came at for low back pain, showed no difference in pain
the price of greater adverse effects. The effect was response between saline injection, anesthetic injec-
greatest in the first 4 days of therapy.38 Similar tion, needle insertion without injection, and vapo-
conclusions have been reached for other drugs in coolant spray with acupressure.39
S18 JABFP November–December 2004 Vol. 17 Supplement http://www.jabfp.org
Steroids been reported.23,26 Exercise is recommended in
Epidural injection of steroids is a commonly per- WAD.2,21
formed procedure for radicular neck and lower
back pain. Trial results are roughly divided be-
Manipulation and Mobilization
tween positive and negative results37 Variability in
Manipulation of the spine directs a high-velocity
response may be a result, at least in part, of heter-
thrust at one or more joints of the cervical spine.
ogeneous pathology in this group of patients and
Mobilization includes all manual therapies directed
differences in technique. Recent trials with more
at cervical joint dysfunction that do not involve
careful patient selection and standardized tech-
high-velocity thrusts. Both modalities probably
niques have shown more positive results. The de-
provide at least short-term benefit in patients
cision to consider epidural steroids in any given
with neck pain, but more high-quality research is
patient is therefore an exercise in clinical judgment.
needed before definitive recommendations can be
There exists no clear rationale for epidural steroid
made.43,45,46 Both manipulation and mobilization
injection in nonradicular pain. Their use should be
are recommended in grades II and III WAD.2
reserved for clear radicular pain (recommendation
strength B).37,40 Some recommending bodies sup-
port the use of epidural steroid injections,28 Pulsed Electromagnetic Field Therapy
whereas others do not.25 Small trials of the clinical Significant reductions in pain and increases in cer-
efficacy of systemic steroids have been inconclu- vical range of motion in studies of high method-
sive,37 and clinical trials comparing oral and epi- ologic quality were found in 4 reviews.43,44,46,47
dural steroids have not been performed. Intra-
articular injection of steroids has not been shown to Physical Modalities With No Evidence of Effect
provide effective long-term pain relief,37,41 and The following physical modalities may be helpful
they are not recommended in chronic WAD.2,21 in individual patients, but their use is not currently
supported by a reasonable quantity of high-quality
Percutaneous Radio Frequency Neurotomy scientific evidence.
One randomized controlled trail in patients with
chronic WAD-related neck pain demonstrated a
Thermotherapy
significant increase in the number of patients who
Systematic reviews found no demonstrated benefit
were pain-free at 27 weeks after percutaneous radio
for neck pain.23,43
frequency neurotomy of the facet joints compared
with sham procedure. In those patients who were
not pain-free, the median time to return to 50% of Immobilization
the preoperative level of pain was markedly longer Cervical collars have little effect on cervical range
in the treatment group.42 This technique is cur- of motion in healthy adults. Inconclusive or no
rently available only in research centers. evidence of benefit in neck pain was found in 3
reviews.43,44,47 The New South Wales WAD
Physical Modalities Likely to be Beneficial guidelines recommended the use of soft collars for
The use of the following physical modalities is no more than 3 days in grades II and III WAD,21
supported by a reasonable quantity of high-quality whereas the Quebec guidelines do not recom-
scientific evidence (recommendation strength B). mended them and state that they should be discour-
aged. Their use beyond 72 hours probably prolongs
disability.2
Early Return to Usual Activities
Good evidence supports its recommendation in
WAD.2,21,43 Transcutaneous Electrical Nerve Stimulation
Good-quality studies show no evidence of ef-
fect.2,23
Supervised Exercise
Good evidence of positive effect on acute traumatic
neck injuries44 and clinically important benefit on Therapeutic Ultrasound
pain and function in chronic neck pain have Good-quality evidence shows no benefit.2,23
http://www.jabfp.org Management of Neck Pain S19
Educational Advice on Posture cervical radiographic abnormalities in asymptom-
One review found positive effect on acute traumatic atic persons.
neck injuries,44 but 2 others found insufficient ev- Recommended first-line drug treatment should
idence to make a recommendation.2,43 be with acetaminophen, COX-2–specific inhibi-
tors, or NSAIDs. Short-term muscle relaxants may
be considered, but their sedative properties and
Traction addictive potential must be taken into account.
Available high-quality studies do not allow clear Opioids should be used if other treatments have
conclusions about the effectiveness of cervical been insufficiently effective and continued if there
traction.46 – 48 No major recommending body has is evidence of improved function that outweighs
found convincing evidence of positive effect for any impairment caused by adverse effects. Adjuvant
traction in either acute or chronic neck pain, and antidepressants and anticonvulsants should be con-
none recommends it.2,23 sidered, especially in chronic or neuropathic pain
and when coincident depression is suspected. Epi-
Acupuncture dural steroid injections should be considered only
No reviews show clear demonstration of effective- in cervical radiculopathy. Physical modalities sup-
ness. A review of the outcomes of 14 randomized, ported by evidence of benefit should be used, in-
controlled trials were equally balanced between cluding early return to usual activities, supervised
positive and negative outcomes.6 Another review exercise, electromagnetic therapy, manipulation,
found high methodologic quality of studies, but and mobilization. If symptoms have not resolved
interventions had either no effect or negative ef- within 4- to 6-weeks, re-evaluation and additional
fect.46 Acupuncture treatment is not currently rec- diagnostic workup should be considered.
ommended for any form of neck pain by any major
recommending body.2,25 We acknowledge the contributions of the other members of the
Family Practice Pain Education Project: Gail Cawkwell, MD,
Alan Gibovsky, MD, Deborah Haynes, MD, Tanya Jones,
Conclusions MD, Laeth Nasir, MBBS, Trish Palmer, MD, Sunil Panchal,
MD, Francine Rainone, MD, PhD, Peter Rives, MD, Knox
Neck pain is an almost universal human condition
Todd, MD, and James Toombs, MD.
and is among the most common complaints pre-
sented to family physicians. Although the differen-
References
tial diagnosis of neck pain is extensive, most symp-
1. Lawrence JS. Disc degeneration. Its frequency and
toms are produced by biomechanical sources, such relationship to symptoms. Ann Rheum Dis 1969
as axial neck pain, WAD, and cervical radiculopa- Mar;28:121–38
thy. Most symptoms will abate in a timely fashion 2. Quebec Task Force on Whiplash-associated disor-
with little intervention. ders cohort study. Spine 1995;20 Suppl 8:125– 65.
There is relatively little high-quality evidence 3. Radhakrishnan K, Litchy WJ, O’Fallon WM, Kur-
available that is specific to the treatment of neck land LT. Epidemiology of cervical radiculopathy. A
pain, and there is a dearth of long-term outcomes population-based study from Rochester, Minnesota,
1976 –1990. Brain 1994;117:325–35.
data. This article presents a consensus on the man-
4. Rao R. Neck pain, cervical radiculopathy, and cervi-
agement of axial neck pain and cervical radiculop- cal myelopathy: pathophysiology, natural history,
athy. Straightforward guidelines are available on and clinical evaluation. J Bone Joint Surg Am 2002;
the management of WAD, and a number of general 84:1872– 81.
pain management guidelines that are applicable to 5. Cote P, Cassidy J, Carroll L. The Saskatchewan
neck pain are also available. health and back pain survey. The prevalence of neck
Patient history and physical examination are im- pain and associated disability in Saskatchewan adults.
Spine 1998;23:1689 –98.
portant in distinguishing potential etiologies and
6. White AR, Ernst E. A systematic review of random-
immediately identifying red flags for more serious
ized controlled trials of acupuncture for neck pain.
conditions. Distinguishing between radicular and Rheumatology 1999;38:143–7.
nonradicular neck pain is particularly important. 7. Green LA, Phillips RL, Fryer, GE. The nature of
Diagnostic imaging should be ordered only when primary medical vare. In: Jones R, Britten N,
truly necessary because of the high incidence of Culpepper L, Gass D, Grol R, Mont D, editors.
S20 JABFP November–December 2004 Vol. 17 Supplement http://www.jabfp.org
Oxford textbook of primary medical care. London: management of persistent pain in older persons.
Oxford University Press; 2003. J Am Geriatr Soc 2002;50(6 Suppl):S205–24.
8. DePalma AF, Rothman RH, Liwinnek GE, Canale 25. Sanders S, Harden N, Benson SE, Vincente
ST. Anterior interbody fusion for severe cervical disc PJ. Clinical Practice Guidelines for chronic non-
degeneration. Surg Gynecol Obstet 1972;134: malignant pain syndrome patients II: an evidence-
755– 8. based approach. J Back Musculoskel Rehabil 1999;
9. Gore DR, Sepic SB, Gardner GM, Murray MP. 13:47–58.
Neck pain: a long-term follow-up of 205 patients. 26. American Pain Society. Principles of analgesic use in
Spine 1987;12:1–5. the treatment of acute pain and cancer pain. 4th ed.
10. Evans RW. Some observations of whiplash injuries. Glenview (IL): American Pain Society; 1999.
Neurol Clin 1992;10:975–97. 27. Guidelines for the initial evaluation of the adult
11. Ferrari R, Russell AS. Epidemiology of whiplash: patient with acute musculoskeletal symptoms. Amer-
an international dilemma. Ann Rheum Dis 1999; ican College of Rheumatology Ad Hoc Committee
58:1–5. on Clinical Guidelines. Arthritis Rheum 1996;39:
1– 8.
12. Hammacher ER, van der Werken C. Acute neck
sprain: “whiplash” revisited. Injury 1996;27:463– 66. 28. Practice guidelines for chronic pain management. A
report by the American Society of Anesthesiologists
13. Pawl RP. Chronic neck syndromes: an update. Task Force on Pain Management, Chronic Pain Sec-
Comp Ther 1999;25:278 – 82. tion. Anesthesiology 1997;86:995–1004.
14. Stovner LJ. The nosologic status of the whiplash 29. Gore DR, Sepic SB, Gardner GM. Roentgeno-
syndrome: a critical review based on a methodologic graphic findings of the cervical spine in asymptom-
approach. Spine 1996;21:2735– 46. atic people. Spine 1986;11:521–24.
15. Schrader H, Obelieniene D, Bovim G, et al. Natural 30. Boden SD, McCowin PR, Davis DO, Dina TS,
evolution of late whiplash syndrome outside the Mark AS, Weisel S. Abnormal magnetic resonance
medicolegal context. Lancet 1996;347:1207–11. scans of the cervical spine in asymptomatic subjects:
16. Freeman MD, Croft AC, Rossignol AM. Whiplash a prospective investigation. J Bone Joint Surg Am
associated disorders: redefining whiplash and its 1990;72:1178 – 84.
management, by the Quebec task force. A critical 31. Stiell IG, Wells GA, Vandemheen KL, et al. The
evaluation. Spine 1998;23:1043– 49. Canadian c-spine rule for radiography in alert and
17. Gargan MF and Bannister GC. The rate of recovery stable trauma patients. JAMA 2001;286:1841– 8.
following whiplash injury. Eur Spine J 1994;3: 32. Hoffman JR, Mower WR, Wolfson AB, Todd KH,
162– 4. Zucker MI. Validity of a set of clinical criteria to rule
18. Kumar VG, Rea GL, Mervis LJ, McGregor JM. out injury to the cervical spine in patients with blunt
Cervical spondylotic myopathy: functional and ra- trauma. N Engl J Med 2000;343:94 –9.
diographic long-term outcome after laminectomy 33. Keats TE, Dalinka MK, Alazraki N, et al. Cervical
and posterior fusion. Neurosurgery 1999;44:771–7. spine trauma. American College of Radiology. ACR
19. Henderson CM, Hennessy RG, Shuey HM Jr, appropriateness criteria. Radiology 2000;215 Suppl:
Shackelford EG. Posterior-lateral foramenectomy as 243– 6.
an exclusive operative technique for cervical radicu- 34. Seidenwurm D, Drayer BP, Anderson RE, Braffman
lopathy: a review of 846 consecutively operated B, Davis PC, Deck MD. Myelopathy. American Col-
cases. Neurosurgery 1983;13:504 –12. lege of Radiology appropriateness criteria. Radiol-
20. Young WF. Cervical spondylotic myopathy: a com- ogy 2000;215 Suppl:495–505.
mon cause of spinal cord dysfunction in older pa- 35. Fry SW, Seeff LB. Hepatotoxicity of analgesics and
tients. Am Fam Physician 2000;62:1064 –70. anti-inflammatory agents. Gastroenterol Clin North
21. Guidelines for the management of whiplash-associ- Am 1995;24:875–905.
ated disorders. Sydney, Australia: New South Wales 36. Garcia-Rodriguez LA, Hernandez-Diaz S. The risk
Motor Accidents Authority; 2001. Available at: of upper gastrointestinal complications associated
http://www.maa.nsw.gov.au/pdfs/whip_mgt_summary_ with nonsteroidal anti-inflammatory drugs, glu-
guide.pdf cocorticoids, acetaminophen, and combinations of
22. Prodigy.nhs.uk [homepage on the Internet]. New- these agents. Arthritis Res 2001;3:98 –101.
castle upon Tyne: Sowerby Centre for Health Infor- 37. Deyo RA. Drug therapy for back pain: which drugs
matics at Newcastle; c2003 [cited 2003 Jun 6]. Avail- help which patients? Spine 1996;24:2840 –50.
able from: http://www.prodigy.nhs.uk. 38. Browning R, Jackson JL, O’Malley PG. Cycloben-
23. Philadelphia panel evidence-based clinical practice zaprine and back pain: a meta-analysis. Arch Intern
guidelines on selected rehabilitation interventions Med 2001;161:1613–20.
for neck pain. Phys Ther 2001;81:1701–17. 39. Garvey TA, Marks MF, Weisel SW. A prospective
24. AGS Panel on Persistent Pain in Older Persons. The randomized double-blind evaluation of trigger point
http://www.jabfp.org Management of Neck Pain S21
injection therapy for low back pain. Spine 1989;14: therapy intervention on soft tissue neck injury fol-
962– 4. lowing trauma. Physiother Canada 2000;52:111–30.
40. Ferrante FM, Wilson SP, Iacoabo C, Orav EJ, 45. Hurwitz EL, Aker PD, Adams AH, Meeker WC,
Rocco AG, Lipson S. Clinical classification as a pre- Shekelle PG. Manipulation and mobilization of the
dictor of therapeutic outcome after cervical epidural cervical spine: a systematic review of the literature.
Spine 1996;21:1746 –59.
steroid injection. Spine 1993;18:730 – 6.
46. Kjellman GV, Skargren EI, Oberg BE. A critical
41. Barnsley L, Lord SM, Wallis BJ, Bogduk N. Lack of analysis of randomised clinical trials on neck pain
effect of intraarticular corticosteroids for chronic and treatment efficacy. A review of the literature.
pain in the cervical zygapophyseal joints. N Engl Scand J Rehabil Med 1999;31:139 –52.
J Med 1994;330:1047–50. 47. Hoving JL, Gross AR, Gasner D, et al. A critical
42. Lord SM, Barnsley L, Wallis BJ, McDonald GJ, appraisal of review articles on the effectiveness of
Bogduk N. Percutaneous radio-frequency neurot- conservative treatment for neck pain. Spine 2001;26:
omy for chronic cervical zygapophyseal joint pain. 196 –205.
N Engl J Med 1996;335:1721– 6. 48. Van der heijden GJ, Beurskens AJ, Koes BW, As-
sendelft WJ, de Vet HC, Bouter LM. The efficacy of
43. Binder A. Neck pain. Clin Evid 2002;8:232–34.
traction for back and neck pain: a systematic, blinded
44. Magee DJ, Oborn-Barrett E, Turner S, Fenning N. review of randomized clinical trial methods. Phys
A systematic overview of the effectiveness of physical Ther 1995;75:93–104.
S22 JABFP November–December 2004 Vol. 17 Supplement http://www.jabfp.org
Das könnte Ihnen auch gefallen
- Rehab in The Time of Drug WarDokument5 SeitenRehab in The Time of Drug Wardanny17phNoch keine Bewertungen
- The Ongoing Evolution of Rotaract Is Redefining Its Place Within RotaryDokument6 SeitenThe Ongoing Evolution of Rotaract Is Redefining Its Place Within Rotarydanny17phNoch keine Bewertungen
- Molave Hotel: Carlitos HostelDokument2 SeitenMolave Hotel: Carlitos Hosteldanny17phNoch keine Bewertungen
- Philippine Eagles HymnDokument2 SeitenPhilippine Eagles Hymndanny17ph100% (8)
- Bond Investing Guide 1 To 3Dokument4 SeitenBond Investing Guide 1 To 3danny17phNoch keine Bewertungen
- Hormone Replacement Therapy The Right Choice For Your PatientDokument9 SeitenHormone Replacement Therapy The Right Choice For Your Patientdanny17phNoch keine Bewertungen
- How Should We Diagnose and Treat Osteoarthritis of The KneeDokument3 SeitenHow Should We Diagnose and Treat Osteoarthritis of The Kneedanny17phNoch keine Bewertungen
- Foreign Body in The Eye: Unit No. 3ADokument2 SeitenForeign Body in The Eye: Unit No. 3Adanny17phNoch keine Bewertungen
- Dyspnea, PancytopeniaDokument4 SeitenDyspnea, Pancytopeniadanny17phNoch keine Bewertungen
- How Should We Evaluate Constipation in Infants and ChildrenDokument3 SeitenHow Should We Evaluate Constipation in Infants and Childrendanny17phNoch keine Bewertungen
- Rosa History RevisedDokument2 SeitenRosa History Reviseddanny17ph100% (1)
- Neck Mass How Would You TreatDokument5 SeitenNeck Mass How Would You Treatdanny17phNoch keine Bewertungen
- Facilitators Meeting Agenda For The Training On The ImplementationDokument1 SeiteFacilitators Meeting Agenda For The Training On The Implementationdanny17phNoch keine Bewertungen
- The Pharmacotherapy of Chronic Obstructive Pulmonary Disease in The ElderlyDokument14 SeitenThe Pharmacotherapy of Chronic Obstructive Pulmonary Disease in The Elderlydanny17phNoch keine Bewertungen
- Correlation Between Glycated Haemoglobin and GlucoseDokument6 SeitenCorrelation Between Glycated Haemoglobin and Glucosedanny17phNoch keine Bewertungen
- Rosa AwardeesDokument1 SeiteRosa Awardeesdanny17phNoch keine Bewertungen
- Order Set: Abdominal Pain OrdersDokument3 SeitenOrder Set: Abdominal Pain Ordersdanny17phNoch keine Bewertungen
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Oral and Maxillofacial Medicine The Basi PDFDokument436 SeitenOral and Maxillofacial Medicine The Basi PDFNimas Putri100% (2)
- AECOADDokument7 SeitenAECOADAiman Arifin100% (1)
- Brain-Restoring Impact of Magnesium L-Threonate by Susan GoldscheinDokument7 SeitenBrain-Restoring Impact of Magnesium L-Threonate by Susan GoldscheingstrohlNoch keine Bewertungen
- EmpiemaDokument19 SeitenEmpiemaArrol Iswahyudi100% (1)
- 2005 FRACP Written Examination Paediatrics & ChildDokument30 Seiten2005 FRACP Written Examination Paediatrics & ChildMedicEdNoch keine Bewertungen
- GBS Case StudyDokument2 SeitenGBS Case Studyjperry107Noch keine Bewertungen
- Neurophysiologic Basis of EEG: Piotr OlejniczakDokument4 SeitenNeurophysiologic Basis of EEG: Piotr OlejniczakioanviNoch keine Bewertungen
- Nejmcpc 1909624Dokument10 SeitenNejmcpc 1909624SrivarrdhiniNoch keine Bewertungen
- I've got very little energy У мене дуже мало енергіїDokument3 SeitenI've got very little energy У мене дуже мало енергіїvictoriaNoch keine Bewertungen
- Genito-Urinary TB: Jean Marie Niyonkuru, PGY III Florence Umurangwa, UrologistDokument49 SeitenGenito-Urinary TB: Jean Marie Niyonkuru, PGY III Florence Umurangwa, UrologistRwabugili ChrisNoch keine Bewertungen
- Adults and Adolescents (12 Years of Age and Over)Dokument6 SeitenAdults and Adolescents (12 Years of Age and Over)ddandan_2Noch keine Bewertungen
- Nephrotic Syndrome TP 2Dokument5 SeitenNephrotic Syndrome TP 2Ajibola OlamideNoch keine Bewertungen
- Flame TestDokument1 SeiteFlame TestNur'Izzah JuarahNoch keine Bewertungen
- HEMOPTYSISDokument37 SeitenHEMOPTYSISVarun B RenukappaNoch keine Bewertungen
- Dr. Arun Aggarwal Gastroenterologist Explains The Electrogastrogram (EGG) Which Is The Graphic Producer of StomachDokument45 SeitenDr. Arun Aggarwal Gastroenterologist Explains The Electrogastrogram (EGG) Which Is The Graphic Producer of StomachDr. Arun Aggarwal GastroenterologistNoch keine Bewertungen
- Asthma & COPDDokument9 SeitenAsthma & COPDRobert L G MabongaNoch keine Bewertungen
- Antiepileptic Drugs: Presenter: DR Sanjeev Sharma Guide: DR Komal PrasadDokument50 SeitenAntiepileptic Drugs: Presenter: DR Sanjeev Sharma Guide: DR Komal PrasadSanjeev SharmaNoch keine Bewertungen
- The Milk's in The OvenDokument36 SeitenThe Milk's in The Ovenkarthikv_79Noch keine Bewertungen
- Oxidative Stress2 Test DescriptionDokument2 SeitenOxidative Stress2 Test DescriptionAravind ChowdaryNoch keine Bewertungen
- Pathophysiology of Diabetic Ketoacidosis and Hyperglycemic Hyperosmolar Nonketotic Syndrome EtiologyDokument2 SeitenPathophysiology of Diabetic Ketoacidosis and Hyperglycemic Hyperosmolar Nonketotic Syndrome EtiologyJaylord VerazonNoch keine Bewertungen
- CriteriaDokument8 SeitenCriteriaJohn100% (1)
- Drug-Study (Open Glaucoma)Dokument4 SeitenDrug-Study (Open Glaucoma)aliannaNoch keine Bewertungen
- Moore Et Al-2018-Clinical Liver DiseaseDokument4 SeitenMoore Et Al-2018-Clinical Liver DiseaseCarlos Francisco Enciso MartinezNoch keine Bewertungen
- 2.10 (IM) Liver FailureDokument12 Seiten2.10 (IM) Liver FailureMohammad Amoran SampalNoch keine Bewertungen
- Government of Nunavut EHB Policy GuidelinesDokument5 SeitenGovernment of Nunavut EHB Policy GuidelinesNunatsiaqNewsNoch keine Bewertungen
- Theme 5. Gallstone Disease-1Dokument18 SeitenTheme 5. Gallstone Disease-1HashmithaNoch keine Bewertungen
- Kent Materia MedicaDokument694 SeitenKent Materia MedicaIlyas78692110100% (6)
- Disseminated Intravascular Coagulation in Paediatrics: Revathi Rajagopal, Jecko Thachil, Paul MonagleDokument8 SeitenDisseminated Intravascular Coagulation in Paediatrics: Revathi Rajagopal, Jecko Thachil, Paul MonagleRizky LumalessilNoch keine Bewertungen
- Journal Reading Acute Spinal Cord InjuryDokument14 SeitenJournal Reading Acute Spinal Cord InjuryamandaNoch keine Bewertungen
- When Learning and Remembering Compete: A Functional MRI StudyDokument5 SeitenWhen Learning and Remembering Compete: A Functional MRI Studyclaire_thixtonNoch keine Bewertungen