Beruflich Dokumente
Kultur Dokumente
Arbol en Gemacion.
Hochgeladen von
pacho21Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Arbol en Gemacion.
Hochgeladen von
pacho21Copyright:
Verfügbare Formate
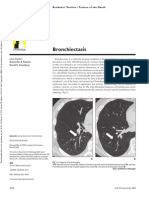
Residents’ Section • Pat tern of the Month
Gosset et al.
Tree-In-Bud Pattern
Residents’ Section
Pattern of the Month
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
Residents
inRadiology Tree-In-Bud Pattern
Natacha Gosset 1 Tree-in-bud (Fig. 1) refers to a pattern seen TABLE 1: Causes of Tree-In-Bud Pattern
Alexander A. Bankier on thin-section chest CT in which centrilobu-
Infections
Ronald L. Eisenberg lar bronchial dilatation and filling by mucus,
pus, or fluid resembles a budding tree (Fig. 2). Bacterial
Gosset N, Bankier AA, Eisenberg RL Usually somewhat nodular in appearance, the Fungal
tree-in-bud pattern is generally most pro- Viral
nounced in the lung periphery and associated
Congenital disorders
with abnormalities of the larger airways.
Normal lobular bronchioles (≤ 1 mm in di- Cystic fibrosis
ameter) cannot be seen on CT scans, which Kartagener syndrome
can only show bronchi more than 2 mm in di- Idiopathic disorders
ameter. However, diseased bronchioles can be
seen. Therefore, the tree-in-bud pattern is in- Obliterative bronchiolitis
dicative of a spectrum of endo- and peribron- Diffuse panbronchiolitis
chiolar disorders with dilatation; bronchiolar Aspiration or inhalation of foreign substances
wall thickening; peribronchiolar inflamma- Immunologic disorders
tion; and bronchiolar luminal impaction with
mucus, pus, fluid, or, as described more re- Allergic bronchopulmonary aspergillosis
cently, tumor emboli. First described in cases Connective tissue disorders
of endobronchial spread of Mycobacterium Rheumatoid arthritis
tuberculosis, the tree-in-bud pattern is now
Sjögren syndrome
recognized as a CT manifestation of such
various entities as infection (bacterial, fungal, Peripheral pulmonary vascular disease
Keywords: bronchial disorders, CT, lung
DOI:10.2214/AJR.09.3401
Received July 28, 2009; accepted after revision
August 18, 2009.
1
All authors: Department of Radiology, Beth Israel
Deaconess Medical Center, Harvard Medical School, 330
Brookline Ave., Boston, MA 02215. Address correspond
ence to R. L. Eisenberg (rleisenb@bidmc.harvard.edu).
WEB
This is a Web exclusive article.
AJR 2009; 193:W472–W477
Fig. 1—Tree-in-bud sign seen in photograph of Fig. 2—Image shows classic CT appearance of tree-
0361–803X/09/1936–W472 magnolia tree just outside of our hospital shows in-bud opacities, consisting of branching structures
typical combination of branching (white arrows) and (black arrows) and buds (white arrows).
© American Roentgen Ray Society buds (black arrows).
W472 AJR:193, December 2009
Tree-In-Bud Pattern
viral, parasitic), congenital disorders (cystic fibrosis, Kartagener syndrome), idiopathic disor-
ders (obliterative bronchiolitis, panbronchiolitis), aspiration or inhalation of foreign substances,
immunologic abnormalities, connective tissue disorders, and peripheral pulmonary vascular
disease (neoplastic pulmonary emboli) (Table 1). Additional imaging findings combined with
history and clinical presentation can suggest the appropriate diagnosis.
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
Infections
Bacterial Infection
The classic cause of the tree-in-bud pattern is postprimary tuberculosis (Fig. 3), a condition
that develops in approximately 5% of patients with primary infection and is frequently associ-
ated with malnutrition and immune suppression. Occasionally, it may reflect reinfection with
new organisms. The tree-in-bud pattern suggests active and contagious disease, especially
when associated with adjacent cavitary disease within the lungs.
The most common CT findings are centrilobular nodules and branching linear and nodular
opacities. This tree-in-bud pattern is due to the presence of caseation necrosis and granuloma-
tous inflammation within and surrounding the terminal and respiratory bronchioles and al-
veolar ducts, reflecting endobronchial spread of tuberculosis. Other common findings include
cavitary nodules, lobular consolidation, interlobular thickening, and bronchovascular distor-
tion. Pleural effusion and enlarged lymph nodes with central low attenuation due to caseous
necrosis also can be seen. After antituberculous therapy is begun, most of the centrilobular
and branching opacities disappear within 5 months. However, bronchovascular distortion, fi-
brosis, emphysema, and bronchiectasis increase on follow-up CT.
Atypical mycobacteria may produce a pattern indistinguishable from that of tuberculosis,
although without any upper lobe predominance (Fig. 4). This is also seen with Mycobacteri-
um avium-intracellulare or M. avium complex, notably in immunologically compromised
individuals with HIV. Bronchiolitis due to Staphylococcus aureus and Haemophilus influen-
zae also may manifest as the peripheral tree-in-bud pattern.
Fungal Infection
Invasive airway aspergillosis causing bronchiolitis occurs most commonly in neutropenic
patients and individuals who are immunologically suppressed with AIDS. Fungal hyphae are
often found in the airway lumen. Other clinical manifestations of this condition are broncho-
pneumonia (peribronchial distribution of consolidation) and tracheobronchitis (bronchiectasis
A B
Fig. 3—Tuberculosis.
A and B, Peripheral tree-in-bud opacities (circle, A) combine to produce more peripheral centrilobular nodules
(circle, B).
AJR:193, December 2009 W473
Gosset et al.
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
A B
Fig. 4—Atypical mycobacterial infection.
A and B, Maximum-intensity-projection images in transverse (A) and coronal (B) planes show generalized tree-
in-bud opacities.
and thickening of the trachea or bronchi), which are often bilateral. Invasive airway aspergil-
losis should be suggested when the tree-in-bud pattern occurs in combination with a consoli-
dation accompanied by a halo of ground-glass opacity in a patient with leukemia.
Viral Infection
Cytomegalovirus infection, which typically occurs in immunologically compromised indi-
viduals, can cause bronchiolitis with centrilobular nodules and thickening of the bronchovas-
cular bundles that produce the tree-in-bud pattern. This pattern may have a patchy and unilat-
eral or bilateral and asymmetric distribution and may progress to areas of ground-glass opac-
ity and consolidation. There may be poorly defined nodules with the CT halo sign. In infants
and young children, the tree-in-bud pattern is most commonly caused by bronchial wall
thickening and dilatation related to respiratory syncytial virus.
Congenital Disorders
Cystic Fibrosis
Cystic fibrosis is an autosomal-recessive hereditary disorder involving the exocrine glands,
resulting in the production of abnormal secretions by the salivary and sweat glands, pancreas,
large bowel, deferent ducts, and tracheobronchial tree. A block in the transport of chloride
into the bronchial lumen and the excessive resorption of sodium leads to the production of
thick and dry mucus, resulting in decreased clearance of mucus and eventually mucous plug-
ging in small and large airways and subsequent bacterial infection.
Chronic infection and inflammatory reactions cause lung damage. The most common CT
findings include bronchial wall thickening, bronchiectasis or bronchiolectasis, mucous plug-
ging, and air trapping on expiratory scanning. Large amounts of bronchiolar secretions can
produce the tree-in-bud pattern, which predominantly tends to affect the upper lobes in the
early stage of the disease.
Kartagener Syndrome
Kartagener syndrome is one of the dyskinetic cilia syndromes, a set of autosomal-recessive
disorders in which inherited abnormalities in ciliary structure and function result in abnormal
mucociliary clearance and chronic infection. It is characterized by the clinical triad of situs
inversus, sinusitis, and bronchiectasis. Symptoms of recurrent bronchitis, pneumonia, and
sinusitis often date from childhood. In men, the syndrome may be associated with immotile
spermatozoa and infertility.
The typical chest CT findings in Kartagener syndrome include bilateral bronchiectasis
with a basal predominance. Airway damage can extend to the smaller airways, causing bron-
chiolectasis, air trapping, and centrilobular opacities producing the tree-in-bud pattern.
W474 AJR:193, December 2009
Tree-In-Bud Pattern
Idiopathic Disorders
Obliterative Bronchiolitis
Obliterative bronchiolitis, also known as constrictive bronchiolitis, is an irreversible fibro-
sis of small airway walls that narrows or obliterates the lumen, leading to chronic airway
obstruction. The most common causes include infection (viral, bacterial, mycoplasma), inha-
lation of toxic fumes, drug treatment (penicillamine or gold), collagen vascular disease (rheu-
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
matoid arthritis, especially after the therapies mentioned), chronic lung transplant rejection,
and bone marrow transplantation with chronic graft-versus-host disease. Nevertheless, oblit-
erative bronchiolitis is often idiopathic. Patients usually present with shortness of breath and
evidence of airway obstruction. CT findings include bronchial wall thickening, central and
peripheral bronchiectasis, mosaic perfusion, and air trapping on expiratory CT scans (the
most sensitive sign). Centrilobular nodules from luminal impaction produce the tree-in-bud
pattern (Fig. 5).
Fig. 5—Obliterative bronchiolitis. CT image shows
extensive right lower lobe area of peripheral tree-
in-bud opacities (arrows). Nodular component of
opacities is smaller but well defined.
Diffuse Panbronchiolitis
Diffuse panbronchiolitis is a progressive inflammatory disease of unknown cause that has
been reported almost exclusively in Japan and Eastern Asia. It represents a transmural infil-
tration of lymphocytes and plasma cells, with mucus and neutrophils filling the lumen of af-
fected bronchioles. Most affected individuals are nonsmokers and have chronic sinusitis. The
natural history of the disease is progressive respiratory failure leading to cor pulmonale and
ultimately death. In addition to thick-walled bronchioles filled with mucus and producing the
tree-in-bud pattern, there may be nodules, bronchiectasis, large cystic opacities accompanied
by dilated proximal bronchi, and mosaic perfusion or air trapping.
Aspiration or Inhalation of Foreign Substances
Aspiration of infected oral secretions or other irritant material into the bronchioles can
lead to a chronic inflammatory reaction. Predisposing factors include structural abnormali-
ties of the pharynx, esophageal disorders (achalasia, Zenker diverticulum, hiatal hernia and
reflux, esophageal carcinoma), neurologic defects, and chronic illness. In acute cases, exten-
sive exudative bronchiolar disease may develop and result in centrilobular nodules and the
tree-in-bud pattern in a distribution characteristic of aspirated material.
Inhalation of toxic fumes and gases can cause pulmonary damage. Acutely, it leads to al-
veolocapillary damage with subsequent pulmonary edema, bronchitis, and bronchiolitis and
AJR:193, December 2009 W475
Gosset et al.
Fig. 6—Chronic aspiration. Tree-in-bud opacities
(arrows) in right lower lobe. Note hiatal hernia.
Nodular component of changes may later coalesce
and create ground-glass appearance.
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
may be complicated by atelectasis and pneumonia. Chronically, it can result in obliterative
bronchiolitis. CT findings include bronchial wall thickening, bilateral consolidation, bron-
chiectasis, and the tree-in-bud pattern (Fig. 6).
Immunologic Disorders
Allergic bronchopulmonary aspergillosis is a hyperimmune response to airway coloniza-
tion with Aspergillus species commonly seen in patients with asthma and cystic fibrosis. The
fungus proliferates in the proximal bronchi, acting as an antigenic stimulus for the production
of IgE and IgG antibodies. The inflammatory reaction results in damage to the bronchial wall,
central bronchiectasis, and the formation of mucous plugs that contain fungus and inflamma-
tory cells, producing the finger-in-glove sign of large airway impaction that tends to have
upper lobe predominance and can be seen on chest radiographs. Involvement of the small
airways causes the tree-in-bud pattern (Fig. 7). Indirect signs of small airways disease include
a mosaic pattern of lung attenuation and air trapping on expiratory scanning.
A B
Fig. 7—Allergic bronchopulmonary aspergillosis.
A and B, Peripheral tree-in-bud opacities (arrows, A) can often be accompanied by more proximal airway
abnormalities, such as mucous plugging (arrows, B).
Connective Tissue Disorders
Rheumatoid Arthritis
Rheumatoid arthritis is twice as common in women, although extraarticular manifesta-
tions (including lung disease) are more common in men. About 90% of patients have a posi-
tive serum rheumatoid factor and show clinical evidence of arthritis before developing pul-
monary or pleural disease. The most common thoracic abnormalities include interstitial
pneumonia and fibrosis, pleural effusion or pleural thickening, necrobiotic nodules, organiz-
ing pneumonia, bronchiectasis, and obliterative bronchiolitis.
W476 AJR:193, December 2009
Tree-In-Bud Pattern
Fig. 8—Rheumatoid arthritis. Axial CT image shows
tree-in-bud opacities (arrows) in lingula.
Downloaded from www.ajronline.org by 181.57.244.244 on 07/07/18 from IP address 181.57.244.244. Copyright ARRS. For personal use only; all rights reserved
A lymphoid interstitial infiltrate in the walls of the small airways (follicular bronchiolitis) may
cause small centrilobular nodules and the tree-in-bud pattern (Fig. 8). More extensive lympho-
cytic infiltrations may be associated with lymphoid interstitial pneumonia (LIP), with ground-
glass opacities, consolidation, septal thickening mimicking the lymphangitic spread of carcinoma,
and cystic air spaces. This condition progresses to fibrosis in about one third of patients.
Sjögren Syndrome
Sjögren syndrome consists of the clinical triad of keratoconjunctivitis sicca, xerostomia,
and recurrent swelling of the parotid gland. The most common thoracic manifestations in-
clude LIP (more common than in rheumatoid arthritis), follicular bronchiolitis, interstitial
pneumonia, organized pneumonia, tracheobronchial gland inflammation, and pleuritis with
or without effusion. As with rheumatoid arthritis, lymphoid interstitial infiltrate in the walls
of the small airways may produce the tree-in-bud pattern.
Peripheral Pulmonary Vascular Disease
The lung is a frequent site of tumor embolism, most commonly from choriocarcinoma and
primary malignancies of the liver, breast, kidney, stomach, and prostate. Filling of the centri-
lobular arteries with tumor cells or a rare widespread fibrocellular intimal hyperplasia of
small pulmonary arteries (carcinomatous endarteritis) may produce the tree-in-bud pattern.
Affected patients present with progressive dyspnea and cough and signs of hypoxia and pul-
monary hypertension (due to increased pulmonary vascular resistance).
Suggested Reading
1. Collins J, Blankenbaker D, Stern EJ. CT patterns of bronchiolar disease: what is “tree-in-bud”? AJR 1998;
171:365–370
2. Eisenhuber E. The tree-in-bud sign. Radiology 2002; 222:771–772
3. Hansell DM. Small airways diseases: detection and insights with computed tomography. Eur Respir J 2001;
17:1294–1313
4. Bankier AA, Van Muylem A, Knoop C, et al. Bronchiolitis obliterans syndrome in heart–lung transplant
recipients: diagnosis with expiratory CT. Radiology 2001; 218:533–539
5. Franquet T, Giménez A, Prats R, Rodríguez-Arias JM, Rodríguez C. Thrombotic microangiopathy of pul-
monary tumors: a vascular cause of tree-in-bud pattern on CT. AJR 2002; 179:897–899
6. Hansell DM, Bankier AA, MacMahon H, McLoud TC, Müller NL, Remy J. Fleischner Society: glossary of
terms for thoracic imaging. Radiology 2008; 246:697–722
7. Müller NL, Silva CIS. Imaging of the chest: expert radiology series. New York, NY: Saunders, 2008
8. Rossi SE, Franquet T, Volpacchio M, et al. Tree-in-bud pattern at thin-section CT of the lungs: radiologic–
pathologic overview. RadioGraphics 2005; 25:789–801
9. Webb WR, Higgins CB. Thoracic imaging: pulmonary and cardiovascular radiology. Philadelphia, PA:
Lippincott Williams & Wilkins, 2005
AJR:193, December 2009 W477
Das könnte Ihnen auch gefallen
- Bronkiektasis PDFDokument14 SeitenBronkiektasis PDFHalida Batik AlunaNoch keine Bewertungen
- Ajr 161 6 8249719Dokument7 SeitenAjr 161 6 8249719hotmart ventasNoch keine Bewertungen
- Tuberculosis of The Spine - Imaging FeaturesDokument11 SeitenTuberculosis of The Spine - Imaging FeaturesSetyo Budi Premiaji WidodoNoch keine Bewertungen
- Pa Tho Physiology of Spinal Cord InjuryDokument1 SeitePa Tho Physiology of Spinal Cord InjuryGenel Joseph Jacildo Peñaflor100% (2)
- NCERT Zhatka Final - PDF Biology02Dokument3 SeitenNCERT Zhatka Final - PDF Biology02Babarav DaradeNoch keine Bewertungen
- NCERT Zhatka Final - PDF BiologyDokument24 SeitenNCERT Zhatka Final - PDF BiologyKunal Dattatray SapateNoch keine Bewertungen
- Aleksa Obradović, Tamara Popović, Jelena Adamović, Anđelka Prokić, Milan IvanovićDokument1 SeiteAleksa Obradović, Tamara Popović, Jelena Adamović, Anđelka Prokić, Milan IvanovićMirko PetrićNoch keine Bewertungen
- Small-Bowel Obstruction From Adhesive Bands and Matted Adhesions: CT DifferentiationDokument5 SeitenSmall-Bowel Obstruction From Adhesive Bands and Matted Adhesions: CT DifferentiationOlga DianaNoch keine Bewertungen
- 03 - Diffuse Pulmonary NodulesDokument13 Seiten03 - Diffuse Pulmonary NodulesOmar Guerrero Soto100% (1)
- Ajr 12 10386Dokument12 SeitenAjr 12 10386CuauhtémocNoch keine Bewertungen
- Excavatum 3Dokument6 SeitenExcavatum 3nadiaNoch keine Bewertungen
- Congenital Heart Disease For The Adult Cardiologist: Ventricular Septal DefectsDokument8 SeitenCongenital Heart Disease For The Adult Cardiologist: Ventricular Septal DefectsMuliana DatuNoch keine Bewertungen
- Sciencedirect: © 2019, Ifac (International Federation of Automatic Control) Hosting by Elsevier Ltd. All Rights ReservedDokument6 SeitenSciencedirect: © 2019, Ifac (International Federation of Automatic Control) Hosting by Elsevier Ltd. All Rights ReservedheryuanoNoch keine Bewertungen
- Preface: Dendrocalamus Asper Gigantochloa Apus Gigantochloa AtterDokument1 SeitePreface: Dendrocalamus Asper Gigantochloa Apus Gigantochloa AtterbabakaroNoch keine Bewertungen
- Ductus ProminentDokument4 SeitenDuctus ProminentEvaristo GomesNoch keine Bewertungen
- Apical Fenestration in Endodontically Treated.20Dokument4 SeitenApical Fenestration in Endodontically Treated.20Mohd NazrinNoch keine Bewertungen
- Chapter 4 Bio 110Dokument1 SeiteChapter 4 Bio 110Sir Majid the 21stNoch keine Bewertungen
- Bot010.Exercise 07Dokument3 SeitenBot010.Exercise 07KimNoch keine Bewertungen
- Pictorial Essay: Cavernous Sinus SyndromeDokument8 SeitenPictorial Essay: Cavernous Sinus SyndromeDian DestriyanahNoch keine Bewertungen
- UG 2022 Lecture ScheduleDokument16 SeitenUG 2022 Lecture ScheduleSaurabh LamkhadeNoch keine Bewertungen
- Assessment Diagnosis Explanation of The Problem Planning Intervention Rationale Evaluation Subjective: Sto: StoDokument5 SeitenAssessment Diagnosis Explanation of The Problem Planning Intervention Rationale Evaluation Subjective: Sto: StoMaria Francheska OsiNoch keine Bewertungen
- Case 046Dokument2 SeitenCase 046Emayavaramban MNoch keine Bewertungen
- Rita Barros - Wrist - And.hand - EULAR TTT 2022Dokument17 SeitenRita Barros - Wrist - And.hand - EULAR TTT 2022Rita BarrosNoch keine Bewertungen
- Silva Et Al 2012 Asthma and Associated Conditions High Resolution CT and Pathologic FindingsDokument8 SeitenSilva Et Al 2012 Asthma and Associated Conditions High Resolution CT and Pathologic FindingsMilton Nogueira da Silva JuniorNoch keine Bewertungen
- Ajr 163 6 7992738Dokument6 SeitenAjr 163 6 7992738qrscentralNoch keine Bewertungen
- Swensen Et Al 2013 High Resolution CT of The Lungs Findings in Various Pulmonary DiseasesDokument9 SeitenSwensen Et Al 2013 High Resolution CT of The Lungs Findings in Various Pulmonary Diseasesjeetchoudhary7890Noch keine Bewertungen
- Auditory Auditory: HearingDokument3 SeitenAuditory Auditory: HearingEdward XiamNoch keine Bewertungen
- Cone Beam Computed Tomography Evaluation of The.9Dokument5 SeitenCone Beam Computed Tomography Evaluation of The.9francisco EscorciaNoch keine Bewertungen
- Anatomical Features of Bougainvillea (Nyctaginaceae) : Sarah ChewDokument7 SeitenAnatomical Features of Bougainvillea (Nyctaginaceae) : Sarah ChewPratistha ShauryaNoch keine Bewertungen
- Adobe Scan 31 May 2023Dokument5 SeitenAdobe Scan 31 May 2023GauravNoch keine Bewertungen
- Jurnal 8Dokument13 SeitenJurnal 8sriwahyuutamiNoch keine Bewertungen
- Injury To The Inferior Alveolar and Lingual Nerves in Successful and Failed Coronectomies - Systematic ReviewDokument7 SeitenInjury To The Inferior Alveolar and Lingual Nerves in Successful and Failed Coronectomies - Systematic ReviewBelen AntoniaNoch keine Bewertungen
- PTB NCPDokument3 SeitenPTB NCPناديه المعمريNoch keine Bewertungen
- Ajr-Mucocele AppendixDokument4 SeitenAjr-Mucocele AppendixOrlin Zlatarski100% (1)
- Solitary Intra-Osseous Myofibroma of The Jaw - A Case Report and Review of LiteratureDokument8 SeitenSolitary Intra-Osseous Myofibroma of The Jaw - A Case Report and Review of LiteratureJean Carlos Barbosa FerreiraNoch keine Bewertungen
- Kazerooni ScoreDokument7 SeitenKazerooni ScoreAndiie ResminNoch keine Bewertungen
- Total HIP Replacement : Roentgen Appearance OF Current DevicesDokument6 SeitenTotal HIP Replacement : Roentgen Appearance OF Current DevicesIsti NisaNoch keine Bewertungen
- Detolla 2000Dokument5 SeitenDetolla 2000guptaamitalwNoch keine Bewertungen
- Does Talking To Plants Help Their Grwoth?Dokument4 SeitenDoes Talking To Plants Help Their Grwoth?John OsborneNoch keine Bewertungen
- Cancers: Pineal Gland Tumors: A ReviewDokument18 SeitenCancers: Pineal Gland Tumors: A ReviewwinnerfromparisNoch keine Bewertungen
- Gettingto Know Plants BookDokument14 SeitenGettingto Know Plants BookSOMEONE OUT Of your knowledgeNoch keine Bewertungen
- Root Reshaping: An Integral Component of Periodontal SurgeryDokument9 SeitenRoot Reshaping: An Integral Component of Periodontal SurgeryANDREANoch keine Bewertungen
- Bcs Article RoleDokument15 SeitenBcs Article RoleSowmya ANoch keine Bewertungen
- Radiological Aspects of Apical Periodontitis: Sisko Huumonen & Dag ØrstavikDokument23 SeitenRadiological Aspects of Apical Periodontitis: Sisko Huumonen & Dag ØrstavikAsadulla KhanNoch keine Bewertungen
- Nodal AnatomyDokument7 SeitenNodal Anatomymeet ChaudharyNoch keine Bewertungen
- The Coronavirus: in A Tiny DropDokument4 SeitenThe Coronavirus: in A Tiny DropARAVIND KANTHNoch keine Bewertungen
- Cervical Burnout and Mach Band: Two Shadows of Doubt in Radiologic Interpretation of Carious LesionsDokument4 SeitenCervical Burnout and Mach Band: Two Shadows of Doubt in Radiologic Interpretation of Carious LesionsNishtha KumarNoch keine Bewertungen
- AtlasRespiratorioPorcino IngDokument6 SeitenAtlasRespiratorioPorcino IngEduardo ViolaNoch keine Bewertungen
- Discussion of Clinical Anatomy of The Lingual Nerves: Haruyuki SHINOHARA, Izumi MATAGA and Ikuo KAGEYAMADokument6 SeitenDiscussion of Clinical Anatomy of The Lingual Nerves: Haruyuki SHINOHARA, Izumi MATAGA and Ikuo KAGEYAMAmNoch keine Bewertungen
- Synthesis Grid 4of4Dokument5 SeitenSynthesis Grid 4of4api-550375558Noch keine Bewertungen
- Femoral Acetabular Impingement ImportantDokument43 SeitenFemoral Acetabular Impingement ImportantAjeetalbertNoch keine Bewertungen
- Renal Papillary Necrosis 16 PDFDokument9 SeitenRenal Papillary Necrosis 16 PDFAdrian ZapataNoch keine Bewertungen
- Optimizing Imaging Parameters For MR Evaluation of The SpineDokument11 SeitenOptimizing Imaging Parameters For MR Evaluation of The SpineDimas PramujaNoch keine Bewertungen
- Maxillary Sinus Disease Diagnosis and TreatmentDokument7 SeitenMaxillary Sinus Disease Diagnosis and Treatmentsadia Gul - Oral and Maxilofacial SurgeryNoch keine Bewertungen
- Lung-Cancer 3Dokument1 SeiteLung-Cancer 3Aphrill Pearl PacisNoch keine Bewertungen
- Format NCPDokument2 SeitenFormat NCPFranz goNoch keine Bewertungen
- Format NCPDokument2 SeitenFormat NCPFranz goNoch keine Bewertungen
- WARD Et Al 2011 Whats New in The Nitrogen CycleDokument9 SeitenWARD Et Al 2011 Whats New in The Nitrogen Cyclesafira143Noch keine Bewertungen
- Controlo Optimo Aplicado ADokument21 SeitenControlo Optimo Aplicado AVivaldo BilaNoch keine Bewertungen
- Medicina Africana Yorubic Medicine - The Art of Divine HerbologyDokument34 SeitenMedicina Africana Yorubic Medicine - The Art of Divine HerbologyJosé Laerton100% (1)
- Discuss Man's Transition in Diets As This Country Has Progressed From From An Agricultural Economy To A Technological EconomyDokument2 SeitenDiscuss Man's Transition in Diets As This Country Has Progressed From From An Agricultural Economy To A Technological Economyselenita2909Noch keine Bewertungen
- Bees in DeclineDokument48 SeitenBees in DeclineFitzcarl ReidNoch keine Bewertungen
- BPRC SlideshowDokument28 SeitenBPRC Slideshowapi-3036345000% (1)
- Esophagus QuesDokument8 SeitenEsophagus QuesnehaNoch keine Bewertungen
- Endoftalmus PDFDokument7 SeitenEndoftalmus PDFArmayaniNoch keine Bewertungen
- COVID-19 Disease - Acute Respiratory Distress Syndrome and Prone PositionDokument5 SeitenCOVID-19 Disease - Acute Respiratory Distress Syndrome and Prone PositionlacundekkengNoch keine Bewertungen
- Drying Methods and Packaging MaterialsDokument95 SeitenDrying Methods and Packaging MaterialsAbubakar Ahmad100% (1)
- Medical Surgical Nursing ReviewerDokument8 SeitenMedical Surgical Nursing ReviewerDavid Brillo0% (1)
- Dexamethasone Suppression TestDokument2 SeitenDexamethasone Suppression Testjbeans92Noch keine Bewertungen
- FCR Capsula Xl2 Brochure 01Dokument3 SeitenFCR Capsula Xl2 Brochure 01Zhandra50% (2)
- Hospital Practice & Patient CareDokument14 SeitenHospital Practice & Patient CareAkinsola Ayomidotun100% (1)
- Health Claim FormDokument4 SeitenHealth Claim Formpandya hemangNoch keine Bewertungen
- Discourse Community AutorecoveredDokument6 SeitenDiscourse Community Autorecoveredapi-360616493Noch keine Bewertungen
- Dwnload Full Nutrition Exercise and Behavior An Integrated Approach To Weight Management 3rd Edition Summerfield Solutions Manual PDFDokument36 SeitenDwnload Full Nutrition Exercise and Behavior An Integrated Approach To Weight Management 3rd Edition Summerfield Solutions Manual PDFbokcardera100% (12)
- Module 1Dokument13 SeitenModule 1MaseaNoch keine Bewertungen
- Ent RevisionDokument104 SeitenEnt RevisionNano BaddourNoch keine Bewertungen
- Maggio 2003Dokument18 SeitenMaggio 2003Mădălina MitroiuNoch keine Bewertungen
- GRE FlashcardDokument304 SeitenGRE FlashcardAjayNoch keine Bewertungen
- Seed Coating) Damping OffDokument11 SeitenSeed Coating) Damping OffOlivia SimanungkalitNoch keine Bewertungen
- BacteDokument210 SeitenBacteEricsson CarabbacanNoch keine Bewertungen
- PG Syllabus - PLANT PATHOLOGYDokument18 SeitenPG Syllabus - PLANT PATHOLOGYAnitharaj AlaguvelNoch keine Bewertungen
- How To Write A Discharge SummaryDokument8 SeitenHow To Write A Discharge Summaryمحمد حسنNoch keine Bewertungen
- Antineoplastic Agents ReportDokument3 SeitenAntineoplastic Agents ReportMegan Rose MontillaNoch keine Bewertungen
- 15 Plural FormsDokument17 Seiten15 Plural FormsRamuguhaNoch keine Bewertungen
- Nemeroff Et Al. 2013 - Dsm-5 2013 Collection Psychiatrist Views (Word Drop)Dokument19 SeitenNemeroff Et Al. 2013 - Dsm-5 2013 Collection Psychiatrist Views (Word Drop)DestriNoch keine Bewertungen
- MRCP Part 1 (1)Dokument23 SeitenMRCP Part 1 (1)ChloeNoch keine Bewertungen
- Guardian Health & Life Insurance FormDokument2 SeitenGuardian Health & Life Insurance Formsmbdy tbhhhNoch keine Bewertungen
- 17A. Immune ToleranceDokument8 Seiten17A. Immune ToleranceEssington BeloNoch keine Bewertungen