Beruflich Dokumente
Kultur Dokumente
Head Injury - Handout
Hochgeladen von
Mohd Hisyamuddin SaharudinOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Head Injury - Handout
Hochgeladen von
Mohd Hisyamuddin SaharudinCopyright:
Verfügbare Formate
Traumatic Brain Injury
Definition:
Traumatic brain injury (TBI) is physical injury to brain tissue that temporarily or permanently impairs
brain function.
Pathology:
• Injuries are commonly categorized as open or closed.
• Open injuries involve penetration of the scalp and skull (and usually
the meninges and underlying brain tissue).
They typically involve bullets or sharp objects.
• A skull fracture with overlying laceration due to severe blunt force is
also considered an open injury.
• Closed injuries typically occur when the head is struck, strikes an object,
or is shaken violently, causing rapid brain acceleration and deceleration.
• Acceleration or deceleration can injure tissue at the point of impact
(coup), at its opposite pole (contrecoup), or diffusely.
• The frontal and temporal lobes are particularly vulnerable.
• Axons, blood vessels, or both can be sheared or torn.
Common Types of Traumatic Brain Injury
• Concussion:
– Concussion is defined as a transient and reversible posttraumatic
alteration in mental status (eg, loss of consciousness or memory,
confusion) lasting from seconds to minutes and not more than 6 h.
– No gross structural brain lesions and serious neurologic residua.
– Temporary disability can occur due to symptoms, such as nausea,
headache, dizziness, memory disturbance, and difficulty
concentrating (postconcussion syndrome) that usually resolve
within weeks.
• Brain Contusions:
– Contusions (bruises of the brain) can occur with open or closed
injuries.
– Contusions can impair a wide range of brain functions, depending
on contusion size and location.
– Larger contusions may cause brain edema and increased
intracranial pressure (ICP).
– Contusions may enlarge in the hours and days following the initial injury and cause
neurologic deterioration
Azizi KATPM Page 1
• Diffuse axonal injury:
– Diffuse axonal injury (DAI) occurs when there is generalized
disruption of axonal fibers and myelin sheaths.
– No gross structural lesions but small petechial hemorrhages
are present.
– DAI is sometimes defined clinically as a loss of consciousness
lasting > 6 h in the absence of a specific focal lesion.
– Edema from the injury often increases ICP, leading to various manifestations.
• Hematomas:
– Hematomas can occur with open or closed injuries.
– They may be epidural, subdural, or intracerebral.
– Subarachnoid hemorrhage is common
• Subdural hematomas are collections of blood between the dura mater
and the pia-arachnoid mater.
o It arises from laceration of veins.
o They occur from falls and motor vehicle crashes.
o Compression of the brain by the hematoma and swelling of the
brain can increase ICP.
o High ICP increases mortality and morbidity.
o A chronic subdural hematoma cause symptoms gradually over
several weeks after trauma.
These hematomas occur often in alcoholics and elderly
patients (especially in those taking antiplatelet or anticoagulant drugs, or in
those with brain atrophy).
Elderly patients may consider the headinjury relatively trivial or may have even
forgotten it.
Edema and increased ICP are unusual.
• Epidural hematomas are collections of blood between the skull and
dura mater and are less common.
o Epidural hematomas that are large or rapidly expanding are
usually caused by arterial bleeding, from the middle
meningeal artery caused by a temporal bone fracture.
o Without intervention, hematomas may rapidly deteriorate
and cause death.
o Small, venous epidural hematomas are rarely lethal.
• Intracerebral hematomas are collections of blood within the brain itself.
o They result from coalescence of contusions.
o Increased ICP, herniation, and brain stem failure can subsequently
develop, particularly with lesions in the temporal lobes.
Azizi KATPM Page 2
Skull fractures:
• Skull fractures may be linear, depressed, or comminuted.
• The presence of a fracture suggests that significant force was
involved in the injury.
• Patients with any fracture associated with neurologic impairment are
at increased risk of intracranial hematomas.
• Fractures that involve special risks include:
– Depressed fractures can tear the dura and damages the
underlying brain, or both.
– Temporal bone fractures that cross the area of the middle
meningeal artery can caused an epidural hematoma.
– Fractures that cross one of the major dural sinuses cause
significant hemorrhage and venous epidural or venous subdural
hematoma.
– Injured venous sinuses can later thrombose and cause cerebral
infarction.
– Fractures that involve the carotid canal can result in carotid
artery dissection.
– Fractures of the occipital bone and base of the skull (basilar bones).
– These bones are thick and strong, so fractures in these areas indicate a high-intensity
impact and so increases the risk of brain injury.
– Basilar skull fractures that extend into the petrous part of the temporal bone often
damage middle and inner ear structures and can impair facial, acoustic, and vestibular
nerve function.
– A linear skull fracture in infants can trapped the meninges with subsequent
development of a leptomeningeal cyst and expansion of the original fracture (growing
fracture)
Pathophysiology :
• Brain function may be immediately impaired by direct damage (eg, crush, laceration) of brain
tissue or occurs shortly thereafter from the cascade of events triggered by the initial injury.
• TBI of any sort can cause cerebral edema and decrease brain blood flow.
• Any swelling from edema or an intracranial hematoma has nowhere to expand and thus
increases ICP.
• The brain becomes ischemic.
• Systemic complications from trauma (eg, hypotension, hypoxia) can also contribute to cerebral
ischemia (secondary brain insults).
• Excessive ICP initially causes global cerebral dysfunction.
• If excessive ICP is unrelieved, it can push brain tissue across the tentorium or through the
foramen magnum, causing herniation and increased morbidity and mortality
Azizi KATPM Page 3
• The Glasgow Coma Scale.
– It is a scoring system used during the initial examination to estimate severity of TBI.
– It is based on eye opening, verbal response, and the best motor response.
– The lowest total score (3) indicates likely fatal damage, especially if both pupils fail to
respond to light and oculovestibular responses are absent.
– Higher initial scores tend to predict better recovery.
– The severity of headinjury is initially defined by the GCS score:
14 or 15 is mild TBI
9 to 13 is moderate TBI
3 to 8 is severe TBI.
– The Glasgow Coma Scale:
Area Assessed Response Points
Eye opening Open spontaneously 4
Open to verbal command 3
Open in response to pain applied to the limbs or sternum 2
None 1
Verbal Oriented 5
Disoriented, but able to answer questions 4
Inappropriate answers to questions; words discernible 3
Incomprehensible speech 2
None 1
Motor Obeys commands 6
Responds to pain with purposeful movement 5
Withdraws from pain stimuli 4
Responds to pain with abnormal flexion (decorticate posture) 3
Responds to pain with abnormal (rigid) extension (decerebrate 2
posture)
None 1
Combined scores < 8 are typically regarded as coma.
Azizi KATPM Page 4
Symptoms of specific types of TBI:
• Symptoms of various types of TBI may overlap considerably.
• Epidural hematoma symptoms usually develop within minutes to several hours after the injury
(the period without symptoms is the so-called lucid interval) and consist of increasing headache,
decreased level of consciousness, and focal neurologic deficits (eg, hemiparesis).
• Pupillary dilation with loss of light reactivity usually indicates herniation.
• Some patients lose consciousness, then have a transient lucid interval, and then gradual
neurologic deterioration.
• Most patients with subdural hematomas have immediate loss of consciousness.
• Intracerebral hematoma and subdural hematoma can cause focal neurologic deficits such as
hemiparesis, progressive decrease in consciousness, or both.
• Progressive decrease in consciousness may result from anything that increases ICP (eg,
hematoma, edema, hyperemia).
• Increased ICP sometimes causes vomiting.
• Classically, it manifests as a combination of hypertension, bradycardia, and respiratory
depression (Cushing triad).
• Severe diffuse brain injury or markedly increased ICP may cause decorticate or decerebrate
posturing.
o Both are poor prognostic signs.
• Transtentorial herniation may result in coma, unilaterally or bilaterally dilated and unreactive
pupils, hemiplegia (usually on the side opposite a unilaterally dilated pupil), and Cushing triad
(hypertension, bradycardia and poor respiration).
• Basilar skull fracture may result in
o leakage of CSF from the nose (CSF rhinorrhea) or ear (CSF otorrhea).
o blood behind the tympanic membrane (hemotympanum) or in the external ear canal if
the tympanic membrane has ruptured.
o ecchymosis behind the ear (Battle sign) or in the periorbital area (raccoon eyes).
• Loss of smell and hearing is usually immediate, usually aware after regain consciousness.
• Facial nerve function may be impaired immediately or after a delay.
• Other fractures of the cranial vault are sometimes palpable, particularly through a scalp
laceration, as a depression or step-off deformity.
• Chronic subdural hematoma may manifest with increasing daily headache, fluctuating
drowsiness or confusion, and mild-to-moderate hemiparesis or other focal neurologic deficits.
Azizi KATPM Page 5
Long-term symptoms:
• Retrograde and anterograde amnesia may persist.
• Postconcussion syndrome, commonly after a moderate or severe concussion, includes
headache, dizziness, fatigue, difficulty concentrating, variable amnesia, depression, apathy, and
anxiety.
• Smell and taste, sometimes hearing, or rarely vision is altered or lost.
• Symptoms usually resolve spontaneously over weeks to months.
• Common problems such as amnesia, behavioral changes (eg, agitation, lack of motivation),
emotional laibility, sleep disturbances, and decreased intellectual function can persist.
• Late seizures (> 7 days after the injury) develop in some patients, often weeks, months, or even
years later.
• Spastic motor impairment, gait and balance disturbances, ataxia, and sensory losses may occur.
• A persistent vegetative state can result from a TBI that destroys forebrain cognitive functions
but spares the brain stem.
• The capacity for self-awareness and other mental activity is absent.
• Few patients recover normal neurologic function when a persistent vegetative state lasts for 3
mo after injury, and almost none recover after 6 mo.
• Neurologic function may continue to improve for a few years after TBI, most rapidly during the
initial 6 mo.
Diagnosis:
1. Initial rapid trauma assessment
2. Glasgow coma scale and neurologic examination.
3. CT
• Initial measures:
– Perform a rapid, focused neurologic evaluation.
– Assess adequacy of the airway and breathing.
– Perform pupillary light response.
– Assessed before paralytics and sedatives are given.
– Reassessed at frequent intervals (eg, every 15 to 30 min initially, then every 1 h after
stabilization)
• Complete neurologic examination is done as soon as the patient is sufficiently stable.
• CT scan of the head is indicated for the following:
– Patients with impaired level of consciousness.
– GCS score < 15.
– focal neurologic findings.
– persistent vomiting.
– Seizures.
– a history of loss of consciousness.
– clinically suspected fractures.
• CT can detect hematomas, contusions and skull fractures.
• MRI may be useful later in the clinical course to detect more subtle contusions, DAI, and brain
stem injury.
Azizi KATPM Page 6
Prognosis:
• The vast majority of patients with mild TBI retain good neurologic function.
• With moderate or severe TBI, the prognosis is not good.
• The assessment of TBI outcomes is usually based on the GCS score as follows:
o 14 or 15 - Good recovery (return to previous level of function).
o 9 – 13 - Moderate disability (capable of self-care).
o 3 – 8 - Severe disability (incapable of self-care).
o < 8 - Vegetative (no cognitive function).
• Occurrence and duration of coma after a TBI are strong predictors of disability.
• Of patients whose coma exceeds 24 h, 50% have severe persistent neurologic sequelae, and 2 to
6% remain in a persistent vegetative state at 6 mo.
• Cognitive deficits, with impaired concentration, attention, and memory, and various personality
changes are a more common cause of disability.
• Posttraumatic anosmia and acute traumatic blindness seldom resolve after 3 to 4 mo.
• Hemiparesis and aphasia usually resolve at least partially, except in the elderly.
Treatment:
1. For mild injuries, discharge and home observation
2. For moderate and severe injuries, optimization of ventilation, oxygenation, and brain perfusion;
treatment of complications (eg, increased ICP, seizures, hematomas); and rehabilitation.
At The Scene:
• A clear airway is secured and external bleeding is controlled before the patient is moved.
• Avoid displacement of the spine or other bones to protect the spinal cord and blood vessels.
• Proper immobilization should be maintained with a cervical collar and long spine board.
• After the initial rapid neurologic assessment, pain should be relieved with a short-acting
opioid (eg, fentanyl ).
In the hospital:
• After quick initial evaluation, neurologic findings (GCS and pupillary reaction), BP, pulse, and
temperature should be recorded frequently for several hours because any deterioration
demands prompt attention.
• The cornerstone of management for all patients is -
maintenance of adequate ventilation, oxygenation, and brain perfusion to avoid
secondary brain insult.
aggressive early management of hypoxia, hypercapnia, hypotension, and increased
ICP helps avoid secondary complications.
Bleeding from injuries (external and internal) is rapidly controlled.
intravascular volume is promptly replaced with crystalloid (eg, 0.9% saline) or
sometimes blood transfusion to maintain cerebral perfusion.
Hypotonic fluids (especially 5% D/W) are contraindicated because they contain
excess free water, which can increase brain edema and ICP.
Azizi KATPM Page 7
• Other complications to check for and to prevent include hyperthermia, hyponatremia,
hyperglycemia, and fluid imbalance.
1. Mild injury:
• Injury is mild (GCS score 14-15) in 80% of patients.
• If there is brief or no loss of consciousness, vital signs are stable, a normal head CT scan,
and normal mental and neurologic function, they may be discharged home provided
family members or friends can observe them closely for an additional 24 h.
• The patients are brought back to the hospital if any of the following develop:
– Decreased level of consciousness
– Focal neurologic deficits.
– Worsening headache.
– Vomiting
– Deterioration of mental function (eg, seems confused, cannot recognize people,
behaves abnormally)
– Seizures.
2. Moderate and severe injury:
• Injury is moderate in 10% of patients.
• Because deterioration is possible, these patients should be admitted and observed even
if head CT is normal.
• Because airway protective reflexes are usually impaired and ICP may be increased,
patients are intubated endotracheally.
• Close monitoring using the GCS and pupillary response should continue.
• CT is repeated, particularly if there is an unexplained ICP rise
3. Increased intracranial pressure :
• Treatment principles for patients with increased ICP include
– Rapid sequence orotracheal intubation.
– Mechanical ventilation.
– Monitoring of ICP and Cerebral Perfusion Pressure (CPP)
– Ongoing sedation as needed
– Maintaining euvolemia and serum osmolality of 295 to
320 mOsm/kg
– For intractable increased ICP, possibly CSF drainage,
temporary hyperventilation, decompressive craniotomy,
or pentobarbital coma.
• Patients who require airway support or mechanical ventilation need rapid sequence
intubation (RSI) orally rather than awake nasotracheal intubation, which can cause
coughing and gagging and thereby raise the ICP.
– RSI requires an induction agent (eg. IV etomidate 0.3mg/kg for adult) and a
muscle relaxant (eg. IV succinylcholine 1.5mg/kg).
• Pulse oximetry and ABGs (if possible, end-tidal CO2) should be used to assess adequacy
of oxygenation and ventilation.
– The goal is a normal Paco2 level (38 to 42 mm Hg).
Azizi KATPM Page 8
• Cerebral venous drainage can be enhanced (thus lowering ICP) by elevating the head of
the bed to 30° and by keeping the patient's head in a midline position.
– The goal is to maintain ICP at < 20 mm Hg.
• Preventing agitation, excessive muscular activity (eg, due to delirium), and pain can also
help prevent increases in ICP.
– For sedation, inj propofol is often used in adults because it has quick onset and
very brief duration of action; dose is 0.3 mg/kg/h continuous IV infusion,
titrated gradually upward as needed (up to 3 mg/kg/h).
– Opioids are often needed for adequate pain control.
• Patients should be kept euvolemic and iso-osmolar or slightly hyperosmolar (target
serum osmolality 295 to 320 mOsm/kg).
• To control ICP, hypertonic saline solution (usually 2% to 3%) is more effective as
osmotic agent compared to mannitol. It is given as a bolus of 2 to 3 mL/kg IV as needed
or as a continuous infusion of 1 mL/kg/h.
• Serum Na level is monitored and kept ≤ 155 mEq/L.
• When increased ICP is refractory to other interventions,
decompressive craniotomy is considered. A bone flap is removed
(to be replaced later), and duraplasty is done to allow outward
brain swelling.
• Next option for intractable increased ICP is pentobarbital coma.
• Coma is induced by giving pentobarbital 10 mg/kg IV over 30 min,
5 mg/kg/h for 3 h, then 1 mg/kg/h maintenance infusion. This will
suppress bursts of EEG activity.
4. Seizures:
• Seizures can worsen brain damage and increase ICP and therefore should be treated
promptly.
• In patients with significant structural injury (eg, larger contusions or hematomas, brain
laceration, depressed skull fracture) or a GCS score < 10, a prophylactic anticonvulsant
should be considered.
• Inj phenytoin is commonly used. A loading dose of 20 mg/kg IV is given followed by
maintenance dose of 2 to 2.7 mg/kg tid for adult.
5. Skull fractures:
• Aligned closed fractures require no specific treatment.
• Depressed fractures sometimes require surgery to elevate fragments, manage lacerated
cortical vessels, repair dura mater, and debride injured brain.
• Open fractures may require surgical debridement unless there is no CSF leak and the
fracture is not depressed by greater than the thickness of the skull.
6. Surgery:
• Intracranial hematomas may require urgent surgical evacuation to prevent or treat brain
shift, compression, and herniation.
• Small intracerebral and subdural hematomas rarely require surgery.
• Factors that suggest a need for surgery include -
a midline brain shift of > 5 mm.
Azizi KATPM Page 9
compression of the basal cisterns.
worsening neurologic examination findings.
• Chronic subdural hematomas may require surgical drainage but much less urgently than
acute subdural hematomas.
• Large or arterial epidural hematomas are treated surgically.
Small epidural hematomas that are thought to be venous in origin can be
followed with serial CT.
7. Rehabilitation:
• When neurologic deficits persist, rehabilitation is needed.
• Rehabilitation is best provided through a team approach that combines physical,
occupational, and speech therapy, skill-building activities, and counseling to meet the
patient's social and emotional needs.
• Brain injury support groups may provide assistance to the families of brain-injured
patients.
Azizi KATPM Page 10
Das könnte Ihnen auch gefallen
- CS Lecture1 TBI Introduction 202122 1Dokument68 SeitenCS Lecture1 TBI Introduction 202122 1Vicky TangNoch keine Bewertungen
- Traumatic Lesions: Head Injuries: Delano, Alexandra Julianne Duran, Fatima MedrizaDokument31 SeitenTraumatic Lesions: Head Injuries: Delano, Alexandra Julianne Duran, Fatima MedrizaFatima Medriza Duran100% (1)
- Spinal InjuriesDokument22 SeitenSpinal InjuriesPak Budi warsonoNoch keine Bewertungen
- Head Injury ManagementDokument11 SeitenHead Injury Managementrajan kumar100% (1)
- Neurologic EmergenciesDokument194 SeitenNeurologic Emergenciesapi-205902640Noch keine Bewertungen
- Head Trauma: Khamim Thohari Rsud DR Muhammad Soewandhie SurabayaDokument33 SeitenHead Trauma: Khamim Thohari Rsud DR Muhammad Soewandhie SurabayaJessica Alexandria WuNoch keine Bewertungen
- Coma Dfiferential DiagnosisDokument23 SeitenComa Dfiferential DiagnosisGeorge GeorgeNoch keine Bewertungen
- Slide Head Injury ZickyDokument41 SeitenSlide Head Injury ZickyShabrina Ghassani RozaNoch keine Bewertungen
- Traumatic Brain InjuryDokument40 SeitenTraumatic Brain InjuryRed DevilNoch keine Bewertungen
- Tbi Case PresentationDokument22 SeitenTbi Case PresentationNinaNoch keine Bewertungen
- Neurosurgical Emergencies NeuroupdateDokument29 SeitenNeurosurgical Emergencies NeuroupdateAdi SulistyantoNoch keine Bewertungen
- Approach To Unconsious PTDokument62 SeitenApproach To Unconsious PTHussain AzharNoch keine Bewertungen
- CP Angle TumorsDokument65 SeitenCP Angle TumorsDiah VerawatiNoch keine Bewertungen
- Slides For SeizureDokument15 SeitenSlides For SeizureBryan Mae H. Degorio100% (3)
- Brain InjuryDokument35 SeitenBrain InjuryAkhil Adhithyan RamNoch keine Bewertungen
- Cerebellopontine Angle TumoursDokument11 SeitenCerebellopontine Angle TumoursIsmail Sholeh Bahrun MakkaratteNoch keine Bewertungen
- Gullaine-Barré SyndromeDokument13 SeitenGullaine-Barré SyndromeOnieBoy CurayagNoch keine Bewertungen
- Anatomy of Cerebral Blood Supply & Cerebral PhysiologyDokument32 SeitenAnatomy of Cerebral Blood Supply & Cerebral Physiologykiran kizhakkiniNoch keine Bewertungen
- Types of Skull FractureDokument5 SeitenTypes of Skull FractureKhor Hui DiNoch keine Bewertungen
- CRANIOVETEBRALJUNCTIONDokument130 SeitenCRANIOVETEBRALJUNCTIONdrarunrao100% (1)
- Ppt. Patho Head InjuryDokument56 SeitenPpt. Patho Head Injurybermejomelody6877100% (3)
- Traumatic Brain Injury: Shantaveer Gangu Mentor-Dr - Baldauf MDDokument53 SeitenTraumatic Brain Injury: Shantaveer Gangu Mentor-Dr - Baldauf MDRio AlexanderNoch keine Bewertungen
- Head and Spinal Cord InjuryDokument68 SeitenHead and Spinal Cord Injuryiam jessNoch keine Bewertungen
- Head Trauma: Yoon Seung-Hwan, M.DDokument53 SeitenHead Trauma: Yoon Seung-Hwan, M.DAhmed ZahranNoch keine Bewertungen
- Hydrocephalus: I Dewa Ketut Gede Herry Oka Pembimbing: Dr. Dr. I Wayan Niryana, Sp. BS (K)Dokument40 SeitenHydrocephalus: I Dewa Ketut Gede Herry Oka Pembimbing: Dr. Dr. I Wayan Niryana, Sp. BS (K)Dewa Oka100% (1)
- Classification of StrokeDokument3 SeitenClassification of StrokeafhamazmanNoch keine Bewertungen
- HemiplegiaDokument30 SeitenHemiplegiasarguss14100% (1)
- Epidural Hematoma: Kurniasari Armayana AhmadDokument10 SeitenEpidural Hematoma: Kurniasari Armayana AhmadSuci AlimaNoch keine Bewertungen
- Myasthenia Gravis. SURYADokument41 SeitenMyasthenia Gravis. SURYANofilia Citra CandraNoch keine Bewertungen
- Traumatic Brain Injury (TBI) : Epidural Hematoma Subdural HematomaDokument62 SeitenTraumatic Brain Injury (TBI) : Epidural Hematoma Subdural HematomaRey AlwiwikhNoch keine Bewertungen
- Dandy-Walker SyndromeDokument12 SeitenDandy-Walker SyndromeHarshita bansalNoch keine Bewertungen
- TraumaDokument10 SeitenTraumaNur Liyana Ahmad ZakiNoch keine Bewertungen
- Head TraumaDokument22 SeitenHead TraumaEllsay AliceNoch keine Bewertungen
- Spinal Cord InjuryDokument17 SeitenSpinal Cord InjuryTom MallinsonNoch keine Bewertungen
- Neurology - Headache NotesDokument3 SeitenNeurology - Headache NotessarahNoch keine Bewertungen
- StrokeDokument17 SeitenStrokeSathias SundariNoch keine Bewertungen
- Approach To ComaDokument33 SeitenApproach To ComaDương Đình ThuậnNoch keine Bewertungen
- Disorders of Autonomic Nervous System: Chair PersonsDokument37 SeitenDisorders of Autonomic Nervous System: Chair PersonswarunkumarNoch keine Bewertungen
- Head InjuryDokument27 SeitenHead InjuryAmanda100% (1)
- Neuroscience I - Neurologic History Taking and Examination (POBLETE)Dokument9 SeitenNeuroscience I - Neurologic History Taking and Examination (POBLETE)Johanna Hamnia PobleteNoch keine Bewertungen
- ANA 6.01 General Somatic Afferents Dr. EsguerraDokument22 SeitenANA 6.01 General Somatic Afferents Dr. EsguerraNinna Ricci San JuanNoch keine Bewertungen
- 3.1.3.2 - HeadacheDokument40 Seiten3.1.3.2 - HeadacheaddinaNoch keine Bewertungen
- F - Proximal Ulnar Nerve Injury Correct AnswerDokument26 SeitenF - Proximal Ulnar Nerve Injury Correct AnswerMehdi Hasan MazumderNoch keine Bewertungen
- Diseases of The Spinal CordDokument89 SeitenDiseases of The Spinal CordLolla SinwarNoch keine Bewertungen
- Traumatic Brain Injury 1Dokument33 SeitenTraumatic Brain Injury 1Bright SunshinenNoch keine Bewertungen
- Potassium ParticipantsDokument21 SeitenPotassium ParticipantsSkylar IvyNoch keine Bewertungen
- PARAQUAT POISIONING 3rd Block Imed COMPLIEDDokument15 SeitenPARAQUAT POISIONING 3rd Block Imed COMPLIEDMohil PratapNoch keine Bewertungen
- Introduction To Intervertebral Disc Anatomy, Pivd (Lumbar) and Its ManagementDokument104 SeitenIntroduction To Intervertebral Disc Anatomy, Pivd (Lumbar) and Its ManagementVivek SaxenaNoch keine Bewertungen
- Spinal Cord Injury, DisordersDokument54 SeitenSpinal Cord Injury, DisordersChananNoch keine Bewertungen
- HSF Stroke Assessment Pocket Guide PDFDokument24 SeitenHSF Stroke Assessment Pocket Guide PDFPeter FritzNoch keine Bewertungen
- HydrocephalusDokument39 SeitenHydrocephalusAjeng Aristiany Rahawarin100% (1)
- Altered States of AwarenessDokument7 SeitenAltered States of AwarenessCharlene FernándezNoch keine Bewertungen
- Physiology of BalanceDokument45 SeitenPhysiology of BalanceThadei MrumaNoch keine Bewertungen
- Febrile Seizure: Satanun Charoencholvanich, MDDokument10 SeitenFebrile Seizure: Satanun Charoencholvanich, MDAPETT WichaiyoNoch keine Bewertungen
- Spine Fractures and Spinal Cord InjuryDokument54 SeitenSpine Fractures and Spinal Cord InjuryAloy PudeNoch keine Bewertungen
- Diffuse Axonal InjuryDokument3 SeitenDiffuse Axonal InjuryAnirban GhoshNoch keine Bewertungen
- Cerebellar DisordersDokument12 SeitenCerebellar DisordersAnn SamNoch keine Bewertungen
- Post Trauma EpilepsyDokument42 SeitenPost Trauma Epilepsyminerva_fowlNoch keine Bewertungen
- PE-TBI Brain InjuryDokument7 SeitenPE-TBI Brain InjuryjordaoNoch keine Bewertungen
- 3 - Head Injured PatientDokument94 Seiten3 - Head Injured PatientAmmarNoch keine Bewertungen
- Spinal Cord CompressionDokument7 SeitenSpinal Cord CompressionMarius Clifford BilledoNoch keine Bewertungen
- Psychosurgery A Historical Overview.41Dokument13 SeitenPsychosurgery A Historical Overview.41lore.vanbaelNoch keine Bewertungen
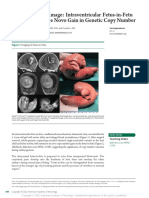
- Teaching Neuroimage: Intraventricular Fetus-In-Fetu With Extensive de Novo Gain in Genetic Copy NumberDokument3 SeitenTeaching Neuroimage: Intraventricular Fetus-In-Fetu With Extensive de Novo Gain in Genetic Copy NumberStancu Oana RuxandraNoch keine Bewertungen
- Badie 2004Dokument11 SeitenBadie 2004Bhayu Rizallinoor BhayuNoch keine Bewertungen
- Neurotrauma & Critical CareDokument10 SeitenNeurotrauma & Critical CareyohanesNoch keine Bewertungen
- Clinical Neurology and NeurosurgeryDokument4 SeitenClinical Neurology and NeurosurgeryGissela AlvaradoNoch keine Bewertungen
- Neurosurgery Syllabus - AustralasiaDokument77 SeitenNeurosurgery Syllabus - AustralasiaRaenette DavidNoch keine Bewertungen
- Oral & Maxillofacial Facial Surgery: SyllabusDokument12 SeitenOral & Maxillofacial Facial Surgery: Syllabussherani999Noch keine Bewertungen
- CghsDokument6 SeitenCghsFACTS- WORLDNoch keine Bewertungen
- JR131870 - Position Description - Unaccredited Neurosurgery RegistrarDokument5 SeitenJR131870 - Position Description - Unaccredited Neurosurgery RegistrarVick VenkateshNoch keine Bewertungen
- List of Hospitals/Diagnostic Centres Empanelled Under Cghs Delhi &Dokument29 SeitenList of Hospitals/Diagnostic Centres Empanelled Under Cghs Delhi &Varun MehrotraNoch keine Bewertungen
- Prof - Dr.Stefan Mindea CV OFFICIAL PDFDokument28 SeitenProf - Dr.Stefan Mindea CV OFFICIAL PDFAndrei BuzutNoch keine Bewertungen
- Personalities of Hillcrest - HuntersDokument101 SeitenPersonalities of Hillcrest - HuntersJames FickbohmNoch keine Bewertungen
- Neuro-Radiology For Final YearDokument150 SeitenNeuro-Radiology For Final YearR DNoch keine Bewertungen
- DR - Raja S Vignesh (Thoothukudi Medical College) in Hospital Care of Patient by NeurosurgeonDokument25 SeitenDR - Raja S Vignesh (Thoothukudi Medical College) in Hospital Care of Patient by NeurosurgeonBrunoNoch keine Bewertungen
- Value To Strategic PartnersDokument23 SeitenValue To Strategic PartnersScottAndrewJordanNoch keine Bewertungen
- Failure of Endoscopic Spine SurgeryDokument6 SeitenFailure of Endoscopic Spine SurgeryKaustubh KeskarNoch keine Bewertungen
- Introduction: What Is Neurosurgery?: Essential Neurosurgery For Medical StudentsDokument2 SeitenIntroduction: What Is Neurosurgery?: Essential Neurosurgery For Medical Studentsakmal shahzadNoch keine Bewertungen
- An Introduction To Neurosurgical Approaches 2010 SCURT FINALDokument153 SeitenAn Introduction To Neurosurgical Approaches 2010 SCURT FINALEcaterina Ignat100% (1)
- SGH Paediatrics Guide 2020 08Dokument44 SeitenSGH Paediatrics Guide 2020 08Yoseph SeleshiNoch keine Bewertungen
- Samer S. Hoz (Auth.) - Vascular Neurosurgery - in Multiple-Choice Questions (2017, Springer International Publishing) PDFDokument223 SeitenSamer S. Hoz (Auth.) - Vascular Neurosurgery - in Multiple-Choice Questions (2017, Springer International Publishing) PDFdedi100% (1)
- Career Forecast Ism AssignmentDokument3 SeitenCareer Forecast Ism Assignmentapi-371078596Noch keine Bewertungen
- List of Empanelled Hospitals/Diagnostic Centres, and Cghs RatesDokument2 SeitenList of Empanelled Hospitals/Diagnostic Centres, and Cghs RatesBabita KumariNoch keine Bewertungen
- Healthcare Knowledge Management: Incorporating The Tools Technologies Strategies and Process of KM To Effect Superior Healthcare DeliveryDokument19 SeitenHealthcare Knowledge Management: Incorporating The Tools Technologies Strategies and Process of KM To Effect Superior Healthcare DeliveryEndris MamoNoch keine Bewertungen
- Thermo TomesDokument5 SeitenThermo Tomesaaronjdriver2248Noch keine Bewertungen
- Clinical Pathway in Emergency MedicineDokument648 SeitenClinical Pathway in Emergency MedicineUtari100% (1)
- ATLS - Head Trauma ImodifiedDokument39 SeitenATLS - Head Trauma ImodifiedSammon TareenNoch keine Bewertungen
- List of Super Speciality Treatment Hospitals in Maharashtra Region As On 30.06.2023Dokument54 SeitenList of Super Speciality Treatment Hospitals in Maharashtra Region As On 30.06.2023Chris PresleyNoch keine Bewertungen
- T20 Operating Table BrochureDokument12 SeitenT20 Operating Table BrochureCatur SetiawanNoch keine Bewertungen
- No. 27 PDFDokument7 SeitenNo. 27 PDFAdilah Zatil KurniaNoch keine Bewertungen
- The Age of Magical Overthinking: Notes on Modern IrrationalityVon EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityBewertung: 4 von 5 Sternen4/5 (24)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisVon EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisBewertung: 4.5 von 5 Sternen4.5/5 (42)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsVon EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNoch keine Bewertungen
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedVon EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedBewertung: 5 von 5 Sternen5/5 (80)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsVon EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsBewertung: 5 von 5 Sternen5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaVon EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeVon EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeBewertung: 2 von 5 Sternen2/5 (1)
- The Obesity Code: Unlocking the Secrets of Weight LossVon EverandThe Obesity Code: Unlocking the Secrets of Weight LossBewertung: 4 von 5 Sternen4/5 (5)
- The Comfort of Crows: A Backyard YearVon EverandThe Comfort of Crows: A Backyard YearBewertung: 4.5 von 5 Sternen4.5/5 (23)
- Why We Die: The New Science of Aging and the Quest for ImmortalityVon EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityBewertung: 4 von 5 Sternen4/5 (3)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningVon EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningBewertung: 4 von 5 Sternen4/5 (3)
- Gut: the new and revised Sunday Times bestsellerVon EverandGut: the new and revised Sunday Times bestsellerBewertung: 4 von 5 Sternen4/5 (392)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Von EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Bewertung: 4.5 von 5 Sternen4.5/5 (110)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsVon EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsBewertung: 3.5 von 5 Sternen3.5/5 (3)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDVon EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDBewertung: 5 von 5 Sternen5/5 (1)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisVon EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisBewertung: 3.5 von 5 Sternen3.5/5 (2)
- An Autobiography of Trauma: A Healing JourneyVon EverandAn Autobiography of Trauma: A Healing JourneyBewertung: 5 von 5 Sternen5/5 (2)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsVon EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsBewertung: 4.5 von 5 Sternen4.5/5 (169)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessVon EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessBewertung: 4.5 von 5 Sternen4.5/5 (328)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisVon EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisBewertung: 4 von 5 Sternen4/5 (1)
- Summary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisVon EverandSummary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisBewertung: 4 von 5 Sternen4/5 (9)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosVon Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosBewertung: 4.5 von 5 Sternen4.5/5 (207)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryVon EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryBewertung: 4 von 5 Sternen4/5 (44)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeVon EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeBewertung: 4.5 von 5 Sternen4.5/5 (253)