Beruflich Dokumente
Kultur Dokumente
Nail Disorders and Systemic Disease What The Nails PDF
Hochgeladen von
Trick San AntonioOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Nail Disorders and Systemic Disease What The Nails PDF
Hochgeladen von
Trick San AntonioCopyright:
Verfügbare Formate
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/23156078
Nail disorders and systemic disease: What the nails tell us
Article in The Journal of family practice · September 2008
Source: PubMed
CITATIONS READS
19 3,238
4 authors, including:
Stamatis Gregoriou George Larios
Attikon University Hospital National and Kapodistrian University of Athens
109 PUBLICATIONS 1,744 CITATIONS 28 PUBLICATIONS 421 CITATIONS
SEE PROFILE SEE PROFILE
Dimitris Rigopoulos
Attikon University Hospital
144 PUBLICATIONS 2,203 CITATIONS
SEE PROFILE
Some of the authors of this publication are also working on these related projects:
scars & keloids View project
actinic keratosis View project
All content following this page was uploaded by Dimitris Rigopoulos on 03 June 2014.
The user has requested enhancement of the downloaded file.
THE JOURNAL OF
FAMILY
PRACTICE
Nail disorders and systemic Stamatis Gregoriou, MD,
George Argyriou, MD,
disease: What the nails tell us George Larios, MD, and
Dimitris Rigopoulos, MD,
PhD
University of Athens
Here’s what you’ll see and what to suspect with these Medical School, Dermatology
Department, Nail Clinic, Athens
11 nail disorders drigop@hol.gr
ed ia
lt h M
n H ea y
owd
e nl
t® D
al u se o
h
yrig r person
Cop
Fo
IN THIS ARTICLE
❚ Onycholysis
❚ Clubbing
❚ Can you name these 2 nail conditions? ❚ Koilonychia
❚ What underlying diseases do you suspect ❚ Onychomadesis
are behind these conditions? ❚ Beau’s lines
❚ Pitted nails
If you said onycholysis (left) and red lunula (right), you are correct. As for
❚ Muehrcke’s nails
the underlying diseases: The patient with onycholysis has hyperthyroidism
❚ Terry’s nails
and the patient with red lunula has chronic obstructive pulmonary disease
(COPD). Onycholysis and red lunula are among the more common changes ❚ Half-and-half nails
to the morphology (shape) and color of the nail—the 2 ways by which nail ❚ Red lunula
changes are classified. ❚ Splinter
hemorrhages
ail abnormalities can be a reveal- This review of common—and not so
N ing sign of underlying disease,
and because the nails are readily
examined, a convenient diagnostic tool,
common—nail disorders shows which
changes to the nail are more likely to
occur with which underlying internal
as well. diseases.
CONTINUED
www.jfponline.com VOL 57, NO 8 / AUGUST 2008 509
For mass reproduction, content licensing and permissions contact Dowden Health Media.
509_JFP0808 509 7/18/08 12:11:50 PM
THE JOURNAL OF
FAMILY
PRACTICE
Proximal
Nail anatomy nail fold
Nail changes are classified according Eponychium
to whether they occur in the morphology Nail bed
(shape) or color of the nail. Onycholysis,
clubbing, and koilonychia are some Hyponychium
of the most common changes in the
morphology of the nail. Red lunula is
Nail matrix
one of the most common changes in
the color of the nail.
Distal edge
of nail plate
Nail plate
Lateral
Lunula nail groove
Lateral
nail fold
Eponychium
Distal
phalanx
Epidermis
ILLUSTRATION © ROB FLEWELL
Onycholysis-associated ❚ Onycholysis
systemic diseases1,2 What you’ll see: Distal separation of
• Amyloid and multiple the nail plate from the underlying nail
myeloma bed. Nails with onycholysis are usually
• Anemia smooth, firm, and without nail bed in-
• Bronchiectasis flammation. It is not a disease of the nail
• Carcinoma (lung)
matrix, though nail discoloration may
• Erythropoietic porphyria
• Histiocytosis X
appear underneath the nail as a result of
• Ischemia (peripheral) secondary infection.
• Leprosy What to suspect: Onycholysis is associ-
• Lupus erythematosus ated with many systemic conditions,
• Neuritis including thyroid disease—especially
• Pellagra hyperthyroidism. (See list at left.) The
• Pemphigus vulgaris nail changes seen with hyperthyroidism
• Pleural effusion usually consist of onycholysis beginning
• Porphyria cutanea tarda in the fourth or fifth nail, the so-called
• Psoriatic arthritis
Plummer’s nails.1 Nakatsui and Lin2 have
• Reiter’s syndrome
suggested that patients with unexplained
• Scleroderma
• Syphilis (secondary
onycholysis be screened for asymptom-
and tertiary) atic thyroid disease.
• Thyroid disease
510 VOL 57, NO 8 / AUGUST 2008 THE JOURNAL OF FAMILY PRACTICE
510_JFP0808 510 7/18/08 12:22:24 PM
Nail disorders
▼
❚ Clubbing
What you’ll see: Increased transverse and
longitudinal nail curvature with fibro-
vascular hyperplasia of the soft tissue
proximal to the cuticle. With clubbing,
the Lovibond’s angle, formed between
the dorsal surface of the distal phalanx
and the nail plate, is greater than 180 de-
grees. Schamroth’s sign—the disappear-
ance of the normal window between the
back surfaces of opposite terminal pha-
langes—may also be present.3
What to suspect: Clubbing may be heredi-
tary, idiopathic, or acquired in association
with a variety of disorders. It may also be
unilateral or bilateral. Unilateral clubbing
has been associated with hemiplegia and of nail disorders in HIV-infected patients
vascular lesions, while bilateral clubbing and found that clubbing affects 5.8% of
has been linked to neoplastic, pulmonary, these patients. Moreover, Cribier’s data
cardiac, gastrointestinal, infectious, endo- reinforced the notion that clubbing could
crine, vascular, and multisystem diseases. be an early sign of AIDS in pediatric pa-
Cribier et al4 studied the frequency tients, and thus play a role in diagnosis.
❚ Koilonychia
What you’ll see: Concave thin nails with
everted edges shaped like a spoon and
capable of retaining a drop of water. It
is more common in fingernails, but is oc- FAST TRACK
casionally seen in toenails. Koilonychia is
What to suspect: This nail sign may result
from trauma, constant exposure of hands sometimes
to petroleum-based solvents, or nail-patella a normal variant
syndrome. Koilonychia is most commonly in infants;
associated with iron deficiency anemia
and occasionally occurs in patients with
it usually
hemochromatosis. Other frequent system- koilonychia is sometimes a normal variant disappears in
ic causes of koilonychia include coronary in infants; it usually disappears in the first the first few
disease and hypothyroidism.5 In addition, few years of life. years of life
❚ Onychomadesis
What you’ll see: Proximal separation of
the nail plate from the nail bed. This
typically results in shedding of the nail.
What to suspect: Trauma is the usual
cause. Less common causes include poor
nutritional status, febrile illness, or drug
sensitivity.
Wester et al6 observed the develop-
ment of onychomadesis in a critically
www.jfponline.com VOL 57, NO 8 / AUGUST 2008 511
511_JFP0808 511 7/17/08 2:54:18 PM
THE JOURNAL OF
FAMILY
PRACTICE
ill patient with a large pulmonary ab- It has also been associated with Kawa-
scess. Onychomadesis is often a clinical saki disease8 and hand, foot, and mouth
manifestation of pemphigus vulgaris.7 disease.9
❚ Beau’s lines
What you’ll see: Transverse depressions in
the nail plate that occur as a result of a
temporary cessation in nail growth.
What to suspect: The causes are similar
to those of onychomadesis and include
trauma, poor nutritional status, febrile
illness, and drug sensitivity.
❚ Pitted nails
What you’ll see: Pinpoint (or larger) de-
pressions in an otherwise normal nail.
What to suspect: Pitting is usually associat-
ed with psoriasis and affects 10% to 15%
of patients with the disorder.10 Pitting has
also been reported in patients with Reiter’s
syndrome (and other connective tissue dis-
orders), sarcoidosis, pemphigus, alopecia
areata, and incontinentia pigmenti.5
FAST TRACK
Terry’s nails have
❚ Muehrcke’s nails
been reported What you’ll see: Transverse white bands
in hemodialysis parallel to the lunula. These bands usu-
patients and renal ally occur in pairs and extend all the
way across the nail.
transplant patients This nail disorder is uncommon, and
is 1 of 3 forms of leukonychia caused by
abnormalities in nail bed vascularization.
(The other 2 forms—Terry’s nails and
half-and-half nails—are described on page
513.)
What to suspect: Muehrcke’s nails ap-
pear in patients with hypoalbuminemia
and can improve if serum albumin lev-
els return to normal. They may also oc-
cur in patients with:11,12
• nephrotic syndrome, chemotherapy.
• glomerulonephritis, Muehrcke’s lines have also been de-
• liver disease, scribed in a patient with Peutz-Jeghers
• malnutrition, and syndrome,13 as well as in a heart transplant
• those who have undergone recipient.14
512 VOL 57, NO 8 / AUGUST 2008 THE JOURNAL OF FAMILY PRACTICE
512_JFP0808 512 7/17/08 2:54:22 PM
Nail disorders
▼
❚ Terry’s nails
What you’ll see: Most of the nail plate is
white, with a narrow pink distal band.
All nails tend to be uniformly affected,
with an appearance of ground glass.15
Terry’s nails have been found in 80% of
patients with cirrhosis of the liver.15
What to suspect: One study found Terry’s
nails in 25% of 512 consecutive hospi-
tal inpatients, with researchers linking
the disorder with cirrhosis, chronic CHF,
and adult-onset diabetes mellitus.16 On
rare occasions, Terry’s nails have been re-
ported in hemodialysis patients and renal
transplant recipients.17 Terry’s nails have
also been observed in HIV patients.4
❚ Half-and-half nails (Lindsay’s nails)
What you’ll see: The proximal portion on
the nail bed is white because of edema of
the nail bed and capillary network; the
distal portion is pink or reddish brown.
The nail plate is unaffected.
What to suspect: This nail disorder has
occurred in patients with renal disease as-
sociated with azotemia.18 Half-and-half
nails have also been detected in hemo-
dialysis patients, renal transplant recipi- FAST TRACK
ents,17 and in HIV patients.4 Azure lunula has
occurred in argyria
❚ Red lunula and in patients
What you’ll see: The lunula is red. In ad- taking medications
dition to the red lunula pictured here,
there is also the absence of lunula and
like 5-fluorouracil
azure lunula. and azidothymidine
What to suspect: Red lunula has been
associated with alopecia areata, and
collagen vascular disease. It has also oc-
curred in patients on oral prednisone
for rheumatoid arthritis. Red lunulae
are seen in cardiac failure, COPD, cir-
rhosis, chronic urticaria, psoriasis, and
carbon monoxide poisoning.19
Absence of lunula was the most
common nail disorder in a group of he-
modialysis patients (31.9%) and has also
been reported in renal transplant recipi- occurred in argyria and in patients tak-
ents (17.1%).17 Azure lunula occurs in ing medications like 5-fluorouracil and
patients with Wilson disease. It has also azidothymidine.20
CONTINUED
www.jfponline.com VOL 57, NO 8 / AUGUST 2008 513
513_JFP0808 513 7/17/08 2:54:27 PM
THE JOURNAL OF
FAMILY
PRACTICE
❚ Splinter hemorrhages
What you’ll see: Extravasations of blood
from the longitudinally oriented ves-
sels of the nail bed. These hemorrhages
do not blanch. They form as a result
of the nail plate-dermis structural re-
lationship and tend to be seen in older
patients.
What to suspect: While trauma is the most
common cause, they may also occur with
psoriasis and fungal infection.
Bacterial endocarditis is the most associated with mitral stenosis, vasculi-
common systemic disease associated with tis, cirrhosis, trichinosis, scurvy, chronic
splinter hemorrhages. These hemorrhages glomerulonephritis, and Darier’s disease.
are more common in subacute, rather However, due to the diverse and com-
than acute, infection. Although splinter mon causes of splinter hemorrhages, they
hemorrhages in subacute bacterial endo- cannot be used as an isolated sign of ill-
carditis have been described as proximal- ness, except when they are accompanied
ly located,21 there are no sufficient data to by things like fever, Roth’s spots, Osler’s
confirm this—mainly because splinter le- nodes, Janeway’s lesions, or a heart mur-
sions migrate distally as the nail grows.22 mur, since any of the above would greatly
Splinter hemorrhages may also be increase their significance. ■
Correspondence 11. Muehrcke RC. The fingernails in chronic hypoalbu-
Dimitris Rigopoulos, assistant professor of dermatology, minemia. BMJ. 1956;1:1327.
University of Athens Medical School, 5 Ionos Dragoumi 12. D’Alessandro A, Muzi G, Monaco A, Filiberto S,
Street, 16121 Athens, Greece; drigop@hol.gr Barboni A, Abbritti G. Yellow nail syndrome: does
protein leakage play a role? Eur Respir J. 2001;
87:5435-5441.
Disclosure 13. Skoog S, Boardman L. Muehrcke’s nails in Peutz-
DID YOU KNOW? The authors reported no potential conflict of interest rel-
evant to this article.
Jeghers syndrome with hepatic adenoma. Clin
Gastroenterol Hepatol. 2004;2:XXIV.
❙ Systemic disease 14. Nabai H. Nail changes before and after heart trans-
References plantation: personal observation by a physician.
typically affects more Cutis. 1998;61:31-32.
1. Jabbour SA. Cutaneous manifestations of endo-
than 1 nail.5,23 crine disorders: a guide for dermatologists. Am J 15. Dupont AS, Magy N, Humbert P, Dupond JL. Nail
Clin Dermatol. 2003;4:315-331. manifestations of systemic diseases. Rev Prat.
❙ Fingernails usually 2000;50:2236-2240.
2. Nakatsui T, Lin AN. Onycholysis and thyroid dis-
16. Holzberg M, Walker HK. Terry’s nails: revised defi-
provide more accurate ease: report of three cases. J Cutan Med Surg.
nition and new correlations. Lancet. 1984;2:896.
1998;3:40-42.
information than toenails 3. Spicknall KE, Zirwas, MJ, English, JC III. Club-
17. Saray Y, Seckin D, Gulec AT, Akgun S, Haberal M.
Nail disorders in hemodialysis patients and renal
because clinical signs bing: an update on diagnosis, differential diagno-
transplant recipients: a case-control study. J Am
sis, pathophysiology, and clinical relevance. J Am Acad Dermatol. 2004;50:197-202.
on toenails are often Acad Dermatol. 2005;52:1020-1028.
18. Dyachenko P, Monselise A, Shustak A, et al. Nail
modified by trauma.23 4. Cribier B, Mena ML, Rey D, et al. Nail changes in disorders in patients with chronic renal failure and
patients infected with human immunodeficiency vi- undergoing haemodialysis treatment: a case control
❙ Fingernails grow at a rus. A prospective controlled study. Arch Dermatol. study. J Eur Acad Dermatol Venereol. 2007;21:340-
1998;134:1216-1220. 344.
rate of 0.1 mm/day and 5. Zaiac MN, Daniel CR III. Nails in systemic disease. 19. Cohen PR. Red lunulae: case report and literature
toenails grow at a rate Dermatol Ther. 2002;5:99-106. review. J AM Acad Dermatol. 1992;26:292.
6. Wester JP, van Eps RS, Stouthamer A, Girbes AR.
of 0.03 mm/day.5,23 Thus, Critical illness onychomadesis. Intensive Care Med.
20. Tanner LS, Gross DJ. Generalized argyria. Cutis.
1990;45:237.
you can estimate the time 2000;26:1698-700.
21. Saccente M, Cobbs CG. Clinical approach to infec-
at which an initial insult 7. Engineer L, Norton LA, Ahmed AR. Nail involve- tive endocarditis. Cardio Clin. 1996;14:351-362.
ment in pemphigus vulgaris. J Am Acad Dermatol.
22. Swartz MN, Weiburg AN. Infections due to gram-
occurred by measuring 2000;43:529-535.
positive bacteria. In: Fitzpatrick TB, Elsen AZ, Wolff
the distance between the 8. Ciastko AR. Onychomadesis and Kawasaki dis- K, Freedberg IM, Austen KF, eds. Dermatology in
ease. CMAJ. 2002;166:1069. General Medicine. 4th ed. New York: McGraw-Hill;
cuticle and the leading 9. Clementz GC, Mancini AJ. Nail matrix arrest fol- 1993: 2309-2334.
edge of any pigmentation lowing hand-foot-mouth disease: a report of five 23. Lawry M, Daniel CR. Nails in systemic disease.
children. Pediatr Dermatol. 2000;17(1):7-11. In: Scher RK, Daniel CR III, eds. Nails: Diagnosis,
change. 10. Mayeaux, EJ Jr. Nail disorders. Prim Care. 2000; Therapy, Surgery. 3rd ed. Philadelphia: Elsevier
27:333-351. Saunders; 2005:147-176.
514 VOL 57, NO 8 / AUGUST 2008 THE JOURNAL OF FAMILY PRACTICE
514_JFP0808 514 7/17/08 2:54:31 PM
View publication stats
Das könnte Ihnen auch gefallen
- Nail DisorderDokument6 SeitenNail DisorderMuhammad Luqman Nul HakimNoch keine Bewertungen
- Root Resorption Brezniak II 2002Dokument5 SeitenRoot Resorption Brezniak II 2002Aly OsmanNoch keine Bewertungen
- The Diagnosis and Treatment of Nail DisordersDokument13 SeitenThe Diagnosis and Treatment of Nail DisordersRatih Anindita Rahajeng RipyonoNoch keine Bewertungen
- Introduction: by John AndrewsDokument6 SeitenIntroduction: by John Andrewsbogdit73100% (1)
- Characteristics of Otorhinolaryngological Emergencies in The ElderlyDokument6 SeitenCharacteristics of Otorhinolaryngological Emergencies in The Elderlysibel yıldırımNoch keine Bewertungen
- Jurnal AsliDokument12 SeitenJurnal AslinathanNoch keine Bewertungen
- Therapy Ocular ToxoplasmosisDokument8 SeitenTherapy Ocular ToxoplasmosissitialimahNoch keine Bewertungen
- Seram2012 S-1544Dokument101 SeitenSeram2012 S-1544Cindy AlvarezNoch keine Bewertungen
- Journal of Periodontology - 2018 - Herrera - Acute Periodontal Lesions Periodontal Abscesses and Necrotizing PeriodontalDokument18 SeitenJournal of Periodontology - 2018 - Herrera - Acute Periodontal Lesions Periodontal Abscesses and Necrotizing PeriodontalMonica MartínezNoch keine Bewertungen
- Heterochromic IridocyclitisDokument8 SeitenHeterochromic Iridocyclitisapi-386609393Noch keine Bewertungen
- 10oral Facial Digitalsyndromeofd31 Yearfollow UpmanagementDokument5 Seiten10oral Facial Digitalsyndromeofd31 Yearfollow UpmanagementThế HảiNoch keine Bewertungen
- The Association Between Visual Display Terminal UsDokument19 SeitenThe Association Between Visual Display Terminal Usheni ariniNoch keine Bewertungen
- Hordeolum - Background, Pathophysiology, EpidemiologyDokument6 SeitenHordeolum - Background, Pathophysiology, EpidemiologyKeren SingamNoch keine Bewertungen
- Management of Foreign Bodies in The Ear: A Retrospective Review of 123 Cases in NigeriaDokument5 SeitenManagement of Foreign Bodies in The Ear: A Retrospective Review of 123 Cases in NigeriaElrach CorpNoch keine Bewertungen
- Guidelines For Periodontal Care and Follow-Up During Orthodontic Treatment in Adolescents and Young AdultsDokument6 SeitenGuidelines For Periodontal Care and Follow-Up During Orthodontic Treatment in Adolescents and Young AdultsMonica JohanaNoch keine Bewertungen
- Onychomycosis Caused by Phialophora JeanselmeiDokument9 SeitenOnychomycosis Caused by Phialophora JeanselmeiPande Agung MahariskiNoch keine Bewertungen
- Alveolar OsteitisDokument42 SeitenAlveolar OsteitisBastosTemitayoStephen100% (2)
- Resolution of Pinguecula-Related Dry Eye Disease ADokument4 SeitenResolution of Pinguecula-Related Dry Eye Disease ASylvia MtrianiNoch keine Bewertungen
- Hom M, Demodex - Clinical Cases & Diagnostic Protocol. OVS 2013Dokument8 SeitenHom M, Demodex - Clinical Cases & Diagnostic Protocol. OVS 2013cassie_kuldaNoch keine Bewertungen
- International Nosology Heritable Disorders of Connective Tissue, Berlin, 1986Dokument14 SeitenInternational Nosology Heritable Disorders of Connective Tissue, Berlin, 1986Willy AndersonNoch keine Bewertungen
- Naija Docs Magazine Issue 7Dokument44 SeitenNaija Docs Magazine Issue 7Olumide ElebuteNoch keine Bewertungen
- PlicacionesencirugiaDokument5 SeitenPlicacionesencirugiahelvi fridayaniNoch keine Bewertungen
- Homeo Eye DiseaseDokument15 SeitenHomeo Eye DiseaseAlbena Trifonova100% (3)
- Intra-Aural Tick Induced Facial PalsyDokument2 SeitenIntra-Aural Tick Induced Facial PalsyAssaye NibretNoch keine Bewertungen
- BroshureDokument3 SeitenBroshuretarikeopsNoch keine Bewertungen
- 1 s2.0 S1542012417301349 MainextDokument75 Seiten1 s2.0 S1542012417301349 MainextWagner de AvizNoch keine Bewertungen
- EctrodactylyDokument2 SeitenEctrodactylyFrianne LuxNoch keine Bewertungen
- Elbow Orthoses: A Review of Literature: Prosthetics and Orthotics International January 2005Dokument11 SeitenElbow Orthoses: A Review of Literature: Prosthetics and Orthotics International January 2005Calugareanu MadalinaNoch keine Bewertungen
- Chessa2020 Article PathogenesisClinicalSignsAndTrDokument13 SeitenChessa2020 Article PathogenesisClinicalSignsAndTrvieeveeNoch keine Bewertungen
- Tessier 1972Dokument22 SeitenTessier 1972Dhila SafirinaNoch keine Bewertungen
- Clinical Concepts of Dry SocketDokument12 SeitenClinical Concepts of Dry SocketSyifa Al QushoyyiNoch keine Bewertungen
- Periorbital Edema: A Puzzle No More?: ReviewDokument10 SeitenPeriorbital Edema: A Puzzle No More?: ReviewJavier Infantes MolinaNoch keine Bewertungen
- Bron 2017Dokument73 SeitenBron 2017Anggia BungaNoch keine Bewertungen
- Osteomyelitis: A Descriptive Study: Clinics in Orthopedic Surgery March 2014Dokument7 SeitenOsteomyelitis: A Descriptive Study: Clinics in Orthopedic Surgery March 2014Gabriel KlemensNoch keine Bewertungen
- Primary Empty Sella A Comprehensive Review 2017Dokument11 SeitenPrimary Empty Sella A Comprehensive Review 2017Paúl Otañez MolinaNoch keine Bewertungen
- Onychogryphosis: Case Report and Review of The Literature: Novel Insights From Clinical PracticeDokument5 SeitenOnychogryphosis: Case Report and Review of The Literature: Novel Insights From Clinical PracticeGabriela VillafañezNoch keine Bewertungen
- Pattern of Ocular Diseases Among Patients Attending Ophthalmic Outpatient Department - A Cross-Sectional StudyDokument11 SeitenPattern of Ocular Diseases Among Patients Attending Ophthalmic Outpatient Department - A Cross-Sectional StudyDr. Abhishek OnkarNoch keine Bewertungen
- Course Overview: American Heart Association, Heart Saver First Aid, CPR/AED G2015Dokument3 SeitenCourse Overview: American Heart Association, Heart Saver First Aid, CPR/AED G2015Ronald AranhaNoch keine Bewertungen
- Homeopathy Advanced Eye HealthDokument21 SeitenHomeopathy Advanced Eye Healthumair_siddiqui8475100% (3)
- Ocular Complications Following Dental Local Anaesthesia (2011)Dokument7 SeitenOcular Complications Following Dental Local Anaesthesia (2011)JohnNoch keine Bewertungen
- Polydactyly - Surgical Strategy and Clinical Experience With 40 CasesDokument14 SeitenPolydactyly - Surgical Strategy and Clinical Experience With 40 CasesAnonymous LnWIBo1G100% (1)
- Mol S Poveda - Et - Al 2019 Pediatric - DermatologyDokument2 SeitenMol S Poveda - Et - Al 2019 Pediatric - DermatologyMaria TebiesNoch keine Bewertungen
- Osteoma Cutis As The Presenting Feature of AlbrighDokument6 SeitenOsteoma Cutis As The Presenting Feature of AlbrighAntonia MariaNoch keine Bewertungen
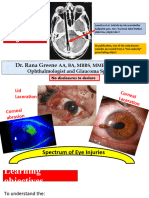
- Trauma Rana GreeneDokument29 SeitenTrauma Rana GreeneGG INoch keine Bewertungen
- Forensic OdontologyDokument10 SeitenForensic OdontologyJeyr UrbanoNoch keine Bewertungen
- Odontoma Compound 1Dokument4 SeitenOdontoma Compound 1ashariNoch keine Bewertungen
- Contact Lens and Anterior Eye: Dayron F. Martínez-Pulgarín, Marcel Y. Avila, Alfonso J. Rodríguez-MoralesDokument8 SeitenContact Lens and Anterior Eye: Dayron F. Martínez-Pulgarín, Marcel Y. Avila, Alfonso J. Rodríguez-MoralesAndi SilpiaNoch keine Bewertungen
- Thecontralateralear 500 PatientsDokument3 SeitenThecontralateralear 500 PatientsDwi Aji HerdianNoch keine Bewertungen
- Onychomadesis: Literature ReviewDokument19 SeitenOnychomadesis: Literature Reviewtaufik perdanaNoch keine Bewertungen
- Ehlers Danlos Syndrome Associated With Cleft Lip and PalateDokument3 SeitenEhlers Danlos Syndrome Associated With Cleft Lip and PalateelmancuernoNoch keine Bewertungen
- Ehz 620Dokument13 SeitenEhz 620Solitary YamantakaNoch keine Bewertungen
- A Rare Complication of Combined Oral Contraceptives (Cocs) : Optic NeuritisDokument3 SeitenA Rare Complication of Combined Oral Contraceptives (Cocs) : Optic NeuritisGufront MustofaNoch keine Bewertungen
- Hypoglossal Nerve Paralysis in A Child After A Dental ProcedureDokument5 SeitenHypoglossal Nerve Paralysis in A Child After A Dental ProcedureMadalinaNoch keine Bewertungen
- Jan'22RQ - PDF Version 1Dokument5 SeitenJan'22RQ - PDF Version 1Rabab BuKhamseenNoch keine Bewertungen
- Journal of Dental Research: The Odontogenic Keratocyst: A Cyst, or A Cystic Neoplasm?Dokument11 SeitenJournal of Dental Research: The Odontogenic Keratocyst: A Cyst, or A Cystic Neoplasm?cedo7Noch keine Bewertungen
- Sudah JPER.16 0642Dokument18 SeitenSudah JPER.16 0642Rabiatul AdawiyahNoch keine Bewertungen
- The Geriatric Patient Use of Acute Geriatrics UnitDokument7 SeitenThe Geriatric Patient Use of Acute Geriatrics Unitlee suk moNoch keine Bewertungen
- (8, 43) Ethmoidectomy-Balkan32017Dokument6 Seiten(8, 43) Ethmoidectomy-Balkan32017ChiNdy AfiSaNoch keine Bewertungen
- The Foundations of Iridology: The Eyes as the Key to Your Genetic Health ProfileVon EverandThe Foundations of Iridology: The Eyes as the Key to Your Genetic Health ProfileNoch keine Bewertungen
- Dental Update 2002. Trismus - Aetiology Differential Diagnosis and TreatmentDokument5 SeitenDental Update 2002. Trismus - Aetiology Differential Diagnosis and TreatmentMNur AshraNoch keine Bewertungen
- Dokumen - Tips Montano Vs Insular GovernmentDokument1 SeiteDokumen - Tips Montano Vs Insular GovernmentTrick San AntonioNoch keine Bewertungen
- IN WITNESS THEREOF, I Have Hereunto Set My Hand This 4: Hereto Attached As AnnexDokument2 SeitenIN WITNESS THEREOF, I Have Hereunto Set My Hand This 4: Hereto Attached As AnnexTrick San AntonioNoch keine Bewertungen
- Bar Questions and Answers Criminal Law 1Dokument86 SeitenBar Questions and Answers Criminal Law 1Trick San AntonioNoch keine Bewertungen
- General Nature and Definition of Human Rights: Top of Form Bottom of FormDokument27 SeitenGeneral Nature and Definition of Human Rights: Top of Form Bottom of FormTrick San AntonioNoch keine Bewertungen
- OJT Complaint Sum of Money Activity 3Dokument5 SeitenOJT Complaint Sum of Money Activity 3Trick San AntonioNoch keine Bewertungen
- Text Readings: Entire Procedure in Land RegistrationDokument12 SeitenText Readings: Entire Procedure in Land RegistrationTrick San AntonioNoch keine Bewertungen
- Legal Forms PatricksDokument12 SeitenLegal Forms PatricksTrick San AntonioNoch keine Bewertungen
- CASE DIGEST Michael C. Guy vs. Atty. Glenn C. Gacot (Partnership)Dokument4 SeitenCASE DIGEST Michael C. Guy vs. Atty. Glenn C. Gacot (Partnership)Bo Dist100% (1)
- Avaliaç So Satisfação Prof Saude Polonia CPDokument6 SeitenAvaliaç So Satisfação Prof Saude Polonia CPJoana Brazão CachuloNoch keine Bewertungen
- Conivaptan MedicalDokument38 SeitenConivaptan MedicalSanjay NavaleNoch keine Bewertungen
- Positional Plagiocephaly: An Analysis of The Literature On The Effectiveness of Current GuidelinesDokument9 SeitenPositional Plagiocephaly: An Analysis of The Literature On The Effectiveness of Current GuidelinesManjunath VaddambalNoch keine Bewertungen
- NMB MyDokument91 SeitenNMB MyGirish Bk B KNoch keine Bewertungen
- Neuraxial ProceduresDokument2 SeitenNeuraxial ProceduresRessy HastoprajaNoch keine Bewertungen
- A Three-Dimensional Method of Visualizing The Temporomandibular Joint Based On Magnetic Resonance Imaging in A Case of Juvenile Chronic ArthritisDokument7 SeitenA Three-Dimensional Method of Visualizing The Temporomandibular Joint Based On Magnetic Resonance Imaging in A Case of Juvenile Chronic ArthritisNAGARAJNoch keine Bewertungen
- A Guide On: Faculties and Institutes of Higher Education in The Arab Republic of EgyptDokument587 SeitenA Guide On: Faculties and Institutes of Higher Education in The Arab Republic of EgyptEgyptian ResearcherNoch keine Bewertungen
- Anatomy of The Larynx: General DescriptionDokument38 SeitenAnatomy of The Larynx: General DescriptionDr-Firas Nayf Al-ThawabiaNoch keine Bewertungen
- WEEK 6 ECHN Case StudyDokument7 SeitenWEEK 6 ECHN Case StudybevNoch keine Bewertungen
- Vilep 3 Jusmitha NoviDokument5 SeitenVilep 3 Jusmitha NoviChocolovaNoch keine Bewertungen
- New List of Skilled Occupations - Skilled Occupation List (SOL)Dokument4 SeitenNew List of Skilled Occupations - Skilled Occupation List (SOL)Dok Aidz Cruz AsinasNoch keine Bewertungen
- Ear, Nose and Throat EmergenciesDokument3 SeitenEar, Nose and Throat Emergenciesfmta100% (1)
- FINALE - ResearchDokument14 SeitenFINALE - ResearchDarryle Clven Ace BorjaNoch keine Bewertungen
- Maternal Midterm Reviewer Common ProblemsDokument58 SeitenMaternal Midterm Reviewer Common ProblemsEya BaldostamonNoch keine Bewertungen
- Pediatric Endocrinology A Practical Clinical Guide, 2E 2013 (PDF) (DR - Carson) VRGDokument263 SeitenPediatric Endocrinology A Practical Clinical Guide, 2E 2013 (PDF) (DR - Carson) VRGIonela RobertaNoch keine Bewertungen
- NTLS Brouchure-3Dokument1 SeiteNTLS Brouchure-3Sanjay100% (1)
- The Healing Rituals of MandayaDokument3 SeitenThe Healing Rituals of MandayaKatrina BuhianNoch keine Bewertungen
- Surgical Count Instrument, Needles & SpongesDokument2 SeitenSurgical Count Instrument, Needles & Spongeserwin kurniawanNoch keine Bewertungen
- The Brooklyn Cancer Center Announces New Chief of Hematology-OncologyDokument3 SeitenThe Brooklyn Cancer Center Announces New Chief of Hematology-OncologyPR.comNoch keine Bewertungen
- Basic Physician Training (BPT Year 1 and 2) at The Royal Hobart Hospital: Information Sheet 2022Dokument1 SeiteBasic Physician Training (BPT Year 1 and 2) at The Royal Hobart Hospital: Information Sheet 2022nevermore11Noch keine Bewertungen
- Orchitis Vs Testicular Torsion Urology ReportDokument13 SeitenOrchitis Vs Testicular Torsion Urology ReportRem AlfelorNoch keine Bewertungen
- Hospitals That Offer ObservershipsDokument6 SeitenHospitals That Offer ObservershipsNisarg DaveNoch keine Bewertungen
- E-Books For Dental PGsDokument13 SeitenE-Books For Dental PGsArchitNoch keine Bewertungen
- AAOGUDokument6 SeitenAAOGUGoran JosipovićNoch keine Bewertungen
- Textbook For Mrcog 1 by Richa Saxena 9385891286Dokument5 SeitenTextbook For Mrcog 1 by Richa Saxena 9385891286DrMuhammad Hassan50% (2)
- Ncma 219 Rle ReviewerDokument7 SeitenNcma 219 Rle ReviewerAngelica AdlawanNoch keine Bewertungen
- Guide To Read HarrisonDokument3 SeitenGuide To Read HarrisonSheikhEras100% (1)
- Biomechanical Effects of Double or Wide Implants For Single Molar Replacement in The Posterior Mandibular RegionDokument4 SeitenBiomechanical Effects of Double or Wide Implants For Single Molar Replacement in The Posterior Mandibular RegiondwinugrohojuandaNoch keine Bewertungen
- Ecpe Preliminary Test 12Dokument5 SeitenEcpe Preliminary Test 12lilalilakNoch keine Bewertungen
- Kelly Morrison Edited ResumeDokument2 SeitenKelly Morrison Edited Resumeapi-355985174Noch keine Bewertungen