Beruflich Dokumente
Kultur Dokumente
Case 15-2007: A 20-Year-Old Woman With Asthma and Cardiorespiratory Arrest
Hochgeladen von
eliOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Case 15-2007: A 20-Year-Old Woman With Asthma and Cardiorespiratory Arrest
Hochgeladen von
eliCopyright:
Verfügbare Formate
The n e w e ng l a n d j o u r na l of m e dic i n e
case records of the massachusetts general hospital
Founded by Richard C. Cabot
Nancy Lee Harris, m.d., Editor Eric S. Rosenberg, m.d., Associate Editor
Jo-Anne O. Shepard, m.d., Associate Editor Alice M. Cort, m.d., Associate Editor
Sally H. Ebeling, Assistant Editor Christine C. Peters, Assistant Editor
Case 15-2007: A 20-Year-Old Woman
with Asthma and Cardiorespiratory Arrest
Michael E. Wechsler, M.D., M.M.Sc., Jo-Anne O. Shepard, M.D.,
and Eugene J. Mark, M.D.
Pr e sen tat ion of C a se
A 20-year-old woman with asthma was taken to the emergency room of another hos- From the Division of Pulmonary and
pital because of cardiorespiratory arrest. The patient had had severe asthma since Critical Care, Department of Medicine,
Brigham and Women’s Hospital (M.E.W.);
childhood. She was born after a normal pregnancy and delivery to a teenaged, single the Departments of Radiology (J.O.S.) and
mother, who smoked three packs of cigarettes per day during pregnancy and during Pathology (E.J.M.), Massachusetts General
the patient’s childhood. Asthma developed at the age of 4 years, and exacerbations Hospital; and the Departments of Medi-
cine (M.E.W.), Radiology (J.O.S.), and Pa-
occurred frequently thereafter, triggered by cold air, hot humid air, physical activity, thology (E.J.M.), Harvard Medical School
respiratory infections, anxiety, and exposures to paint and to cats and birds that were — all in Boston.
kept in her home or the homes of relatives. Attacks often occurred at night or in the
N Engl J Med 2007;356:2083-91.
early morning. A timeline of medical therapy for asthma is shown in Table 1, and the Copyright © 2007 Massachusetts Medical Society.
results of pulmonary-function tests are shown in Table 2. During testing, the results
improved after bronchodilator therapy. She was followed by pediatricians and spe-
cialists in pulmonary medicine; however, she repeatedly missed outpatient follow-up
appointments and visited emergency rooms on many occasions because of exacer-
bations. She was inconsistent in her use of inhalers and oral medications; she used
inhaled bronchodilators up to 10 times per day when she had symptoms. At the age
of 15 years, she told hospital staff that she rarely took her medications regularly.
Involvement by the Department of Social Services was requested because of non-
compliance with treatment, and the patient’s mother was counseled to stop smok-
ing, but these interventions were unsuccessful. Visiting-nurse assessments of the pa-
tient’s residence for possible allergens were scheduled, but despite multiple attempts,
the assessments were not performed because of the family’s absence from the home.
Oxygen desaturation occurred during some asthma episodes, including an episode
of status asthmaticus at the age of 8 years, with an oxygen saturation of 80% while
the patient was breathing ambient air and had a respiratory rate of more than 50
breaths per minute. She was admitted to this hospital every few months because of
asthma and pneumonia, occasionally to the pediatric intensive care unit. Tracheal
intubation was never required. Peripheral-blood eosinophilia was never documented.
Immunoglobulin E levels were not measured.
Five months before this admission, 1 day after receiving treatment in an emer-
gency room for an asthma flare, the patient was seen at an urgent care facility be-
cause of shortness of breath, cough productive of white sputum, chills, and wheez-
n engl j med 356;20 www.nejm.org may 17, 2007 2083
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Table 1. Timeline of Asthma Therapies.
Medications Administered
on Admission (to Emergency
Age Range Medications Taken at Home Department or Hospital)
4–10 yr Metaproterenol Epinephrine (subcutaneous)
Albuterol by nebulizer and metered-dose inhaler Aminophylline (intravenous)
Theophylline Methylprednisolone (intravenous)
Isoetharine by nebulizer
Cromolyn sodium inhaler
Beclomethasone inhaler
Tapered prednisone (5–14 days)
10–15 yr Albuterol by nebulizer and metered-dose inhaler Epinephrine (subcutaneous)
Ipratropium bromide by nebulizer Terbutaline sulfate (subcutaneous
Salmeterol xinafoate inhaler or intravenous)
Fluticasone propionate metered-dose inhaler
Budesonide inhaler
Tapered prednisone (5–14 days)
Montelukast sodium tablets
Beclomethasone inhaler
15–20 yr Albuterol metered-dose inhaler Epinephrine (subcutaneous or in-
Albuterol and ipratropium bromide by nebulizer travenous)
Theophylline Dexamethasone
Salmeterol xinafoate inhaler Terbutaline (subcutaneous or intra-
Fluticasone propionate metered-dose inhaler venous)
Montelukast sodium tablets Magnesium sulfate (intravenous)
Prednisone (5–60 mg daily)
ing of 2 days’ duration, despite around-the-clock were healthy; her father’s medical history was not
inhalational treatments with nebulized albuterol known.
(2.5 mg) and nebulized ipratropium (0.5 mg). Her On physical examination at the urgent care fa-
other asthma medications were salmeterol (one cility, the patient was in moderate respiratory dis-
puff twice daily), fluticasone propionate delivered tress. The blood pressure was 152/62 mm Hg, the
as an aerosol (220 μg per puff, at a dose of two pulse 120 beats per minute, and the temperature
puffs with a spacer adaptor, twice daily), predni- 37.4°C; the respirations were 28 per minute, and
sone (5 mg every other day), and albuterol with the the oxygen saturation was 90 to 91% while the
use of a metered-dose inhaler (two puffs four times patient was breathing ambient air. At her request,
daily as needed). a peak-flow measurement was not performed. The
The patient had a history of obesity, gastro- body habitus was cushingoid, and there were dif-
esophageal reflux for which she took esomepra- fuse wheezes in both lungs, without rales or rhon-
zole, depression, wrist fractures after a fall, a pari- chi. There was no digital clubbing or cyanosis. The
etal skull fracture after an assault, chickenpox, and remainder of the examination was normal. A chest
pinworms. Childhood vaccinations had been given radiograph revealed consolidation in the right
but had been delayed because of missed appoint- middle lobe and patchy opacity in the left upper
ments. She had no allergies to medications. She lobe. A combination solution of albuterol and ip-
was of South Asian, Scottish, and Dutch ancestry. ratropium was administered by nebulizer twice,
She had missed many months of school because and she was discharged home while receiving
of asthma and had left school after the eighth prednisone (60 mg daily, with instructions to ta-
grade at the age of 15 years. She gave birth to a per the dose), her other medications, and a 5-day
child at the age of 19 years and lived with the course of azithromycin.
child, her mother, and her half-siblings. She told Approximately 8 weeks before admission, the
some caregivers that she smoked cigarettes but patient was seen in the emergency room of a local
also told many others that she did not smoke. The hospital because of respiratory symptoms. Cla
patient’s mother and other maternal relatives had rithromycin was prescribed, but the symptoms
asthma and eczema, and there was a family his- worsened; several days later, a chest radiograph
tory of diabetes mellitus. Her two half-siblings revealed a left-upper-lobe and perihilar infiltrate
2084 n engl j med 356;20 www.nejm.org may 17, 2007
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
case records of the massachuset ts gener al hospital
suggestive of pneumonia. Ceftriaxone was pre-
Table 2. Results of Pulmonary-Function Tests.*
scribed and admission to the hospital was recom-
mended, but she left against medical advice to care Measure Age
for her child. One week later, she saw her primary 7 Yr 11 Yr 18 Yr
care physician, who prescribed levofloxacin. Three
actual value (% of predicted value)
days later, she was seen at an urgent care facility
FVC (liters) Normal 2.79 (125)
because of persistent symptoms. At that time, she
was taking prednisone (30 mg) daily and albuterol FEV1 (liters) Normal 2.00 (100) 2.49 (96)
as needed. Prednisone (30 mg) was administered FEF25 of FVC (liters/sec) 3.29 (73)
orally, and a combination of albuterol and ipratro- FEF75 of FVC (liters/sec) — (44) 0.62 (46)
pium was given by nebulizer. She was instructed FEF25–75 of FVC (liters/sec) 1.45 (56) 1.71 (58)
to take prednisone (60 mg) daily, tapering to a
final dose of 10 mg every other day. A follow-up * FVC denotes forced vital capacity in liters, FEV1 forced expiratory volume in
the first second, FEF25 maximum forced expiratory flow rate when 25% of the
visit and an appointment with a pulmonary spe- FVC has been exhaled, FEF75 maximum forced expiratory flow rate when 75%
cialist were scheduled, but the patient did not keep of the FVC has been exhaled, and FEF25–75 maximum forced expiratory flow
the appointments. rate between 25% and 75% of the FVC exhaled.
During the next weeks, the patient visited emer-
gency departments four or five times because of tracking into the neck. On the lateral view (Fig. 1B)
acute symptoms of asthma, and she made numer- there is a tiny anterior pneumothorax. The pneu-
ous phone calls to her primary care physician, re- mothorax results from the Macklin effect, in
questing refills of her medications. The physician which a peripheral alveolus ruptures and the air
became aware that the patient was receiving asth- tracks centrally along the interstitium into the
ma medications from several different providers. mediastinum and soft tissues. These features are
In the early hours of the morning of admission, typical of asthma. Bilateral focal consolidations
the patient’s mother noted that the patient was are present, representing pneumonia.
awake and using a nebulizer, as she did frequently. Dr. Wechsler: This case highlights the problem
When her mother next saw her, approximately of asthma-associated morbidity and mortality,
2 hours later, the patient was lying on the floor, with more than 4000 deaths from asthma occur-
unresponsive, without spontaneous respirations ring annually in the United States.1 This patient’s
or pulse. The patient’s mother called emergency multiple hospitalizations and emergency room
medical services (EMS). visits exemplify the annual 500,000 asthma-related
On examination by EMS providers, the patient hospitalizations and 2 million emergency room
was cold, cyanotic, and in asystole. The trachea visits that account for $16 billion per year spent
was intubated, and cardiopulmonary resuscitation for asthma treatment2 and the millions of asthma-
was initiated. Epinephrine (1 mg) and atropine related lost work and school days. This patient
(1 mg) were administered intravenously; this was dropped out of school because of the hold that
repeated twice without response. The patient was asthma had on her life.
taken to the emergency room of another hospital, There are many possible causes of death in a
arriving 25 minutes later while cardiopulmonary patient with asthma in whom respiratory failure
resuscitation was in progress. She remained in develops. Patients with corticosteroid-induced
asystolic cardiac arrest, despite aggressive resus- chronic immunosuppression are predisposed to
citation attempts. She was pronounced dead 10 life-threatening infections, anaphylaxis, and acute
minutes after arrival. The body was transferred to hypersensitivity reactions; however, this patient did
this hospital, and an autopsy was performed. not have a history or laboratory evidence to suggest
any of these diagnoses, nor did she have any un-
Differ en t i a l Di agnosis derlying cardiac disease. She did not have a history
of eosinophilia or other major clinical manifes-
Dr. Michael E. Wechsler: May we review the imaging tations of eosinophilic pneumonia or the Churg–
studies? Strauss syndrome. She had nearly all the risk fac-
Dr. Jo-Anne O. Shepard: Chest radiographs (Fig. 1A tors for life-threatening asthma and death from
and 1B) obtained 17 months before her death, on asthma (Table 3), except for aspirin sensitivity and
one of the patient’s multiple visits for asthma ex- older age. Although not a consistent cigarette
acerbations, show pneumomediastinum, with air smoker, she had some history of smoking and
n engl j med 356;20 www.nejm.org may 17, 2007 2085
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
A B
33p9
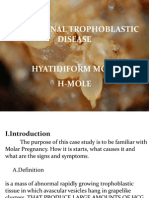
Figure 1. Radiographic Images.
ICM AUTHOR Wechsler RETAKE 1st
Posterior anterior (Panel A) and lateral (Panel B) chest radiographs obtained 17 months
2nd before the patient’s death
REG F FIGURE Fig 1A,B
show pneumomediastinum (Panel A, large arrows) and an anterior pneumothorax (Panel 3rd B, large arrow). Bilateral
CASE TITLE
focal consolidations (Panels A and B,EMail
small arrows) are consistent with pneumonia.
Revised
Line 4-C
Enon ARTIST: mleahy SIZE
H/T H/T 33p9
FILL Combo
exposure to secondhand smoke both in utero and PLEASE
AUTHOR, egories of both moderate and severe persistent
NOTE:
during childhood. She had not requiredFigure mechani-
has been redrawn and type has
disease. been reset.
Whereas all patients with asthma should
Please check carefully.
cal ventilation, but she had been hospitalized many avoid or control factors that trigger attacks, patients
times. Therefore, I believe that this
JOB: patient
35620 had with persistent asthma should also use controller
ISSUE: 5-17-07
status asthmaticus with resultant fatal asthma. medication daily to control airway inflammation
Why did this patient die from asthma? The (e.g., inhaled corticosteroids) and, as the severity
answer may lie with the treatment plan, the com- increases, escalate therapy appropriately. Asthma
pliance of the patient with the plan, and the inher- guidelines from 2006 focus on maintenance of
ent severity of her disease (so severe that no mea- control, reflecting an understanding that asthma
sure taken could have saved her). Each of these severity “involves not only the severity of the un-
factors must be addressed in this case. derlying disease but also its responsiveness to treat-
ment,” and that “severity is not an unvarying fea-
Dis cus sion of M a nage men t ture of an individual patient’s asthma but may
change over months or years.” 4
To address growing concern about increased asth- Inhaled corticosteroids, which had been in-
ma-related morbidity and mortality, in the late cluded in this patient’s regimen early in her care,
1990s the National Institutes of Health (NIH) for- are the cornerstone of these recommendations.
mulated the National Asthma Education and Pre- There is evidence that inhaled corticosteroids not
vention Program, establishing guidelines for the only improve lung function and symptoms but also
management of asthma.3 The NIH recommended may prevent deaths from asthma.5 Short-acting
stratification of patients according to the severity beta-agonists may be used in the short term to
of asthma (mild intermittent, mild persistent, mod- relieve symptoms; however, if there is poor asth-
erate persistent, and severe persistent disease) and ma control despite the use of inhaled corticoste-
implementation of treatment algorithms. At differ- roids, as in this case, other controller therapies,
ent times, this patient’s condition fell into the cat- such as long-acting beta-agonists, leukotriene
2086 n engl j med 356;20 www.nejm.org may 17, 2007
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
case records of the massachuset ts gener al hospital
modifiers, cromolyn, theophylline, or even sys-
Table 3. Risk Factors for Life-Threatening Asthma and Death from Asthma.
temic corticosteroids should be added to the regi-
men. All these medications were prescribed at Long duration of asthma
various times for this patient, but not on a con- Poor control of asthma
sistent basis. When the disease is controlled, the Systemic dependence on corticosteroids
doses or number of controller medications may be Noncompliance with medication regimen
reduced. This patient’s asthma rarely, if ever, ap-
Psychosocial factors
peared to be sufficiently controlled to allow the
tapering of medications. Poor socioeconomic conditions
Patient education is essential at every step of Inconsistent medical follow-up
asthma management, and patients should con- Delayed medical care
tinue to monitor their disease subjectively (i.e., Older age
assessing symptoms) and objectively (using peak- Cigarette smoking
flow meters or spirometry). Although such ap-
Aspirin sensitivity
proaches were attempted in this case, they were
Prior hospitalization for asthma
unsuccessful.
Prior use of mechanical ventilation
Managing Severe Asthma
Both the patient and the physician have responsi- sis, cataracts, glaucoma, and adrenal suppression.
bilities in the management of severe asthma. How- None of these complications were apparent in
ever, a major problem in the control of asthma is this case.
that much of the responsibility lies with the pa-
tient. Consistent Physician Care
Consistency of health care providers was a problem
Adherence to Controller Therapy and Appropriate in this case, because no single physician could ap-
Technique preciate the full scope of this patient’s multiple
Even if a medication is shown to be effective in presentations for worsening asthma. During the
ideal circumstances, as in a clinical trial, its effec- last 5 years of her life, she saw many different pri-
tiveness in practice requires adherence to a pre- mary care doctors, pulmonologists, and allergists.
scribed regimen; for medication to be effective, She went to different clinics and emergency rooms
patients must take it regularly as it is meant to be many times, each time seeing different physicians.
taken. Like this patient, nearly 70% of patients with This fragmentation of care could have resulted in
severe asthma do not refill prescriptions for in- a missed opportunity for one physician to detect
haled corticosteroids,6,7 and many use inhalers in- her clinical deterioration during a period of weeks
correctly. Poor adherence to asthma medications or months and to provide support.
may be due to lack of an immediate benefit, the
patient’s preference for pills rather than inhalers, Education and Warning Signs
suboptimal results because the patient’s technique Education of patients about triggers and warning
of use is suboptimal, cost, inconvenience, and lack signs of severe attacks is critical to the manage-
of education by health care providers. Many pa- ment of severe asthma. This patient knew what
tients, like this one, are children or adolescents provoked her asthma (e.g., cold air and hot, humid
who may have problems accepting the facts of their air), and she avoided going outside in winter. We
illness and the necessity for adhering to an oner- do not know whether she had a peak-flow meter
ous treatment regimen. The cost of the medica- with which to assess the degree of airflow obstruc-
tions may be an issue, since asthma is increasingly tion or whether she was aware of the severity of her
prevalent among economically disadvantaged, in- disease. There was no record of allergy testing.
ner-city children for whom access to medications
is often a difficulty. Physicians clearly worked with Other Medical Options
this patient to maximize adherence and to explain This patient’s physicians had tried virtually all
the importance of taking medications daily. available therapies to control her disease (Table 1),
Adverse effects of medications can also lead to including new treatments such as leukotriene-
poor adherence. For example, inhaled corticoste- receptor antagonists. Novel therapies are now avail-
roids can cause dysphonia, oral thrush, osteoporo- able that might have helped control this patient’s
n engl j med 356;20 www.nejm.org may 17, 2007 2087
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
asthma. For instance, omalizumab, a monoclonal eosinophilia or vasculitis, which are characteristic
antibody against IgE, prevents IgE from binding of the last three disorders. Although IgE levels may
to mast cells and other inflammatory cells, thereby be elevated in these conditions, IgE testing was not
preventing the release of inflammatory mediators. performed.
Its use may permit a lower dose of corticosteroids
and may reduce the frequency of exacerbations, Pharmacogenetics and the Efficacy
which, in turn, could reduce the number of outpa- of Asthma Therapies
tient and emergency room visits and hospitaliza- This patient may be one of the many patients whose
tions among patients with moderate-to-severe asth- asthma is unresponsive to current standard ther-
ma.8,9 Tumor-necrosis-factor (TNF) inhibitors have apies. As many as 40% of patients do not have a
also been investigated in asthma. TNF is a proin- response to inhaled corticosteroids,11-13 and per-
flammatory cytokine affecting adhesion, migra- haps even a higher proportion do not have a re-
tion, activation, and proliferation of many types of sponse to leukotriene modifiers. Heterogeneity of
cells. It is increased in the bronchoalveolar-lavage the underlying biology may affect responsiveness
fluid of patients with asthma, and preliminary data to specific therapies. Symptoms may be driven by
suggest that TNF inhibitors may significantly im- perturbations in corticosteroid, leukotriene, IgE, or
prove lung function and symptoms in patients with beta-adrenergic pathways or even in other pathways
severe asthma.10 yet to be identified; each of these pathways may be
modulated by different medications, so therapies
Factors Contributing to Poor Outcomes should ideally be tailored to the underlying patho-
Despite Optimal Medication Regimens genesis. Similarly, asthma may be mediated by eo-
Several factors can result in poor outcomes despite sinophils or, in the case of severe asthma, by neu-
optimized medication regimens. Exposure to en- trophils. TNF may have a role, and natural killer
vironmental exacerbating factors such as dust, cells may be principal effector cells.14 Since it is
smoke, or cockroaches may impair responsiveness currently not possible to identify the specific path-
to specific therapies. Caregivers made attempts to way involved in a given patient’s asthma, we pre-
modify the home environment of this patient when scribe on the basis of trial and error — an approach
she was a child, but they were unsuccessful. We that, as this case shows, is not always successful.
do not know whether the issue of environmental Pharmacogenetics, the study of how genetic
factors had been raised with the patient during re- differences influence variability in therapeutic and
cent years or whether she would have been more adverse responses to drugs, may predict some of
compliant as a young adult than her mother had the heterogeneity of responses to asthma treat-
been during the patient’s childhood. ments. A mutation in a specific pathway may cause
Coexisting diseases can also impair asthma or prevent a response to a medication aimed at that
outcomes despite optimal medication regimens. pathway or cause an adverse reaction. In asthma,
This patient had evidence of gastroesophageal genetic factors may affect responses to beta-ago-
reflux disease, a condition that may provoke or nists, leukotriene modifiers, and inhaled cortico-
worsen symptoms of asthma. She used a proton- steroids.15 In particular, a common variant in the
pump inhibitor, but it would have been important gene coding for the 16th amino acid of the beta-
to ascertain that the reflux was adequately con- adrenergic receptor is associated with a decline in
trolled and was not contributing to asthma exac- lung function and asthma exacerbations in pa-
erbations. Chronic sinusitis and postnasal drip tients receiving either short- or long-acting beta-
may also exacerbate asthma. This patient had a agonists.16-19 Among patients with asthma, this
history of multiple episodes of pneumonia, which polymorphism occurs in one sixth of white pa-
resulted in the exacerbation of symptoms, and in- tients and up to one quarter of black patients.
fection certainly could have contributed to her re- Although genetic testing is not routinely avail-
spiratory failure and death. able, caregivers should be aware of the potential
Some conditions mimic severe asthma. This genotype-specific effects of long-acting beta-ago-
patient’s fleeting pulmonary infiltrates and air- nists and their potential association with bad
flow obstruction could suggest diagnoses such as outcomes, including death, in patients with asth-
cystic fibrosis, allergic bronchopulmonary asper- ma.20 Although these therapies are helpful for the
gillosis, bronchocentric granulomatosis, or the majority of patients with asthma, those taking the
Churg–Strauss syndrome. She had no history of long-acting beta-agonists salmeterol or formoterol
2088 n engl j med 356;20 www.nejm.org may 17, 2007
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
case records of the massachuset ts gener al hospital
have an increased risk of both exacerbations and teristic of fatal asthma.26-31 The gross pathological
asthma-related death, as compared with those not features of fatal asthma may be more dramatic
receiving these medications.21 Although we do not than the microscopical findings. Pneumothorax
have any genotypic information for this patient, may occur as a complication of the disease and is
we know she took salmeterol, and a pharmacoge- a potential cause of death; its documentation at
netically mediated deleterious effect of this long- autopsy requires opening the chest under a water
acting beta-agonist could have played a role in her seal. No pneumothorax was found in this patient.
deteriorating condition and death. A large, pro- The lungs were hyperinflated, with rounded con-
spective, genotype-stratified trial investigating tours when removed from the body (Fig. 2A). Ex-
whether long-acting beta-agonists cause such ad-
verse effects, which is currently being conducted
by the Asthma Clinical Research Network of the A B
NIH, may answer this question.
Use of Biomarkers in Asthma Control
This patient had a normal forced expiratory vol-
ume in 1 second, but she clearly had severe asth-
ma, as shown by the long duration and frequency
of her symptoms, frequent use of quick-relief in-
halers, and missed work and school. An important
area of asthma research is the use of biomarkers
to assess airway inflammation and guide therapy
for patients with asthma. Adjustment of asthma
medications on the basis of assessment of sputum
eosinophils, exhaled nitric oxide, and airway hy-
perreactivity can reduce asthma exacerbations22-25
and also potentially minimize treatment-related C D
side effects.
DR . MICH A EL E . W ECHSL ER’S
DI AGNOSIS
Fatal asthma.
Pathol o gic a l Dis cus sion E
Dr. Eugene J. Mark: The diagnosis of fatal asthma
falls within the purview of both the hospital pa-
thologist and the forensic pathologist, the latter
because of the possibility that asthma may explain
sudden unexpected death. Factors for the forensic
pathologist to consider in determining whether
asthma was the cause of sudden, unwitnessed
Figure 2. Autopsy Findings.
death include a history of severe attacks, the exis-
The right lung is hyperinflated
AUTHOR in Wechsler
this gross photograph taken before the
tence and location of therapeutic drugs and inhal- ICM
lung was removed from the body (Panel A); a depressed
RETAKE 1st
polygonal lobule
REG F FIGURE 2 a_e 2nd
ers that could have been used by the patient, and (arrow) contrasts
CASE with the hyperinflated adjacent lung. Mediastinal 3rd emphy-
TITLE
gross and microscopical evidence of acute and sema is presentEMail Revised
(Panel B), with bubbles of air in the pericardial
Line 4-C
fat (arrows).
chronic asthma. At autopsy, the common differen- A small bronchus
Enonis filled with mucus and sloughed epithelial
ARTIST: mst SIZE cells (Panel
H/T H/T
C, hematoxylinFILL
and eosin). A terminal bronchiole (Panel 22p3
D, hematoxylin
tial diagnosis of the cause of death includes as- Combo
and eosin) contains hypertrophic
AUTHOR, PLEASE NOTE:(arrow). Numerous eosin-
smooth muscle
phyxia from other causes, anaphylactic reaction, ophils are presentFigure
in thehas
pulmonary interstitium
been redrawn and type has(Panel E, hematoxylin and
been reset.
coexistent pulmonary emboli, and coronary artery eosin). (Photographs in Panels Please
A andcheck carefully. of Dr. Pavan Auluck, De-
B courtesy
disease. partment of Pathology, Massachusetts General Hospital.)
JOB: 35620 ISSUE: 05-17-07
In this case, the autopsy findings were charac-
n engl j med 356;20 www.nejm.org may 17, 2007 2089
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
amination of a cut section showed that the pa- the remainder of the autopsy disclosed no evidence
renchyma protruded above the cut edge of the of coronary artery disease or other abnormalities.
visceral pleura. When left lying on a dissecting A Physician: The patient’s mother noted that the
table, the lungs deflated only slowly. In some cases patient was using a nebulizer shortly before she
it may be difficult to inflate the lungs with forma- died. Could that have contributed to her death?
lin through the bronchial tree because of bron- Dr. Wechsler: Frequent use of albuterol was un-
chiolar obstruction, which was the case with this likely to have caused her death unless there was
patient’s lungs. Pneumomediastinum was present, an underlying cardiac abnormality. The frequent
with interstitial emphysema in fibroadipose tissue use of nebulized beta-agonists was an indicator of
(Fig. 2B). Mucus plugs in bronchi are a frequent the poor control of her asthma, which ultimately
finding; the mucus may protrude from the cut end caused her death. We attempted a postmortem
of a bronchus. analysis of tissue from this patient for evidence
Microscopically, bronchi and bronchioles were of the deleterious mutation in the beta-adrener-
distended by mucus (Fig. 2C), and lymphocytes, gic receptor, but we were unable to extract DNA
neutrophils, and mast cells were present in the of sufficient quality.
bronchiolar mucosa. The bronchial basement mem
brane was thickened, and airway smooth-muscle A nat omic a l Di agnosis
hypertrophy caused bronchiolar narrowing or sub-
Status asthmaticus with hyperinflated lungs, pleu-
total occlusion (Fig. 2D).32 Signs of chronic scar-
ral and pericardial interstitial emphysema, mucus
ring, resulting in constrictive bronchiolitis, were
plugging, bronchiolar scarring, and eosinophilic
present, with small focal scars representing oblit-
pneumonitis.
erated bronchioles. Eosinophils are an inconsis- Dr. Wechsler reports receiving consulting fees or advisory-
tent finding in fatal asthma33,34; they may be board fees from Genentech, Merck, Pfizer, Tanox, and Critical
present in the bronchial lumen, in alveoli, or in Therapeutics and lecture fees from Novartis, Genentech, and
Merck, and serving as an investigator in a trial of a bronchial
the pulmonary interstitium, as in this case (Fig. thermoplasty system sponsored by Asthmatx. No other potential
2E).35,36 There were no pulmonary emboli, and conflict of interest relevant to this article was reported.
References
1. Kochanek KD, Murphy SL, Anderson 1999;340:197-206. [Errata, N Engl J Med 12. Tantisira KG, Lake S, Silverman ES, et
RN, Scott C. Deaths: final data for 2002. 1999;340:663, 1999;341:1632.] al. Corticosteroid pharmacogenetics: asso-
Natl Vital Stat Rep 2004;53:1-115. 7. Kelloway JS, Wyatt RA, Adlis SA. Com- ciation of sequence variants in CRHR1 with
2. American Lung Association. Trends parison of patients’ compliance with pre- improved lung function in asthmatics treat-
in asthma morbidity and mortality. New scribed oral and inhaled asthma medica- ed with inhaled corticosteroids. Hum Mol
York: American Lung Association, Epide- tions. Arch Intern Med 1994;154:1349-52. Genet 2004;13:1353-9.
miology & Statistics Unit, Research and 8. Busse W, Corren J, Lanier BQ, et al. 13. Bateman ED, Boushey HA, Bousquet J,
Scientific Affairs, 2004. Omalizumab, anti-IgE recombinant hu- et al. Can guideline-defined asthma con-
3. National Asthma Education and Pre- manized monoclonal antibody, for the trol be achieved? The Gaining Optimal
vention Program: guidelines for the diag- treatment of severe allergic asthma. J Al- Asthma ControL study. Am J Respir Crit
nosis and management of asthma. Expert lergy Clin Immunol 2001;108:184-90. Care Med 2004;170:836-44.
Panel report 2. Bethesda, MD: National 9. Soler M, Matz J, Townley R, et al. The 14. Akbari O, Faul JL, Hoyte EG, et al.
Heart, Lung, and Blood Institute, 1997. anti-IgE antibody omalizumab reduces ex- CD4+ invariant T-cell-receptor+ natural
(NIH publication no. 97-4051.) acerbations and steroid requirement in al- killer T cells in bronchial asthma. N Engl
4. Global Initiative for Asthma. Global lergic asthmatics. Eur Respir J 2001;18:254- J Med 2006;354:1117-29.
strategy for asthma management and pre- 61. [Erratum, Eur Respir J 2001;18:739- 15. Wechsler ME, Israel E. How pharma-
vention. Hamilton, ON, Canada: GINA, No- 40.] cogenomics will play a role in the man-
vember 2006. (Accessed April 20, 2007, at 10. Berry MA, Hargadon B, Shelley M, et al. agement of asthma. Am J Respir Crit Care
http://www.ginasthma.org.) Evidence of a role of tumor necrosis factor Med 2005;172:12-8.
5. Suissa S, Ernst P, Benayoun S, Baltzan α in refractory asthma. N Engl J Med 2006; 16. Israel E, Drazen JM, Liggett SB, et al.
M, Cai B. Low dose inhaled corticosteroids 354:697-708. The effect of polymorphisms of the beta2-
and the prevention of death from asthma. 11. Malmstrom K, Rodriguez-Gomez G, adrenergic receptor on the response to
N Engl J Med 2000;343:332-6. Guerra J, et al. Oral montelukast, inhaled regular use of albuterol in asthma. Am J
6. Drazen JM, Israel E, O’Byrne PM. beclomethasone, and placebo for chronic Respir Crit Care Med 2000;162:75-80.
Treatment of asthma with drugs modify- asthma: a randomized, controlled trial. 17. Israel E, Chinchilli VM, Ford JG, et al.
ing the leukotriene pathway. N Engl J Med Ann Intern Med 1999;130:487-95. Use of regularly scheduled albuterol treat-
2090 n engl j med 356;20 www.nejm.org may 17, 2007
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
case records of the massachuset ts gener al hospital
ment in asthma: genotype-stratified, ran- control after discontinuation of inhaled 30. Rea HH, Scragg R, Jackson R, Beagle-
domized, placebo-controlled cross-over corticosteroids. J Allergy Clin Immunol hole R, Fenwick J, Sutherland DC. A case-
trial. Lancet 2004;364:1505-12. 2005;115:720-7. control study of deaths from asthma. Tho-
18. Wechsler ME, Lehman E, Lazarus SC, 24. Sont JK, Willems LN, Bel EH, van rax 1986;41:833-9.
et al. β-Adrenergic receptor polymorphisms Krieken JH, Vandenbroucke JP, Sterk PJ. 31. Hogg JC. The pathology of asthma.
and response to salmeterol. Am J Respir Clinical control and histopathologic out- Chest 1985;87:Suppl:152S-153S.
Crit Care Med 2006;173:519-26. come of asthma when using airway hy- 32. Hossain S, Heard BE. Hyperplasia of
19. Palmer CNA, Lipworth BJ, Lee S, Is- perresponsiveness as an additional guide bronchial muscle in asthma. J Pathol 1970;
mail T, Macgregor DF, Mukhopadhyay S. to long-term treatment. Am J Respir Crit 101:171-84.
Arginine-16 beta-2 adrenoceptor genotype Care Med 1999;159:1043-51. 33. Saetta M, Di Stefano A, Rosina C,
predisposes to exacerbations in young asth- 25. Green RH, Brightling CE, McKenna S, Thiene G, Fabbri LM. Quantitative struc-
matics taking regular salmeterol. Thorax et al. Asthma exacerbations and sputum tural analysis of peripheral airways and
2006;61:940-4. eosinophil counts: a randomised controlled arteries in sudden fatal asthma. Am Rev
20. Nelson HS, Weiss ST, Bleecker ER, trial. Lancet 2002;360:1715-21. Respir Dis 1991;143:138-43.
Yancey SW, Dorinsky PM. The Salmeterol 26. Mark EJ. Pathology of fatal asthma. 34. Sur S, Crotty TB, Kephart GM, et al.
Multicenter Asthma Research Trial: a com- In: Sheffer AL, ed. Fatal asthma. Vol. 115 Sudden-onset fatal asthma: a distinct en-
parison of usual pharmacotherpay for asth- of Lung biology in health and disease. tity with few eosinophils and relatively
ma or usual pharmacotherapy plus sal- New York: Marcel Dekker, 1998:127-38. more neutrophils in the airway submu-
meterol. Chest 2006;129:15-26. [Erratum, 27. Houston JC, De Navasquez S, Trounce cosa? Am Rev Respir Dis 1993;148:713-9.
Chest 2006;129:1393.] JR. A clinical and pathological study of 35. Carroll N, Elliot J, Morton A, James A.
21. Martinez FD. Safety of long-acting fatal cases of status asthmaticus. Thorax The structure of large and small airways
beta-agonists — an urgent need to clear 1953;8:207-13. in nonfatal and fatal asthma. Am Rev
the air. N Engl J Med 2005;353:2637-9. 28. Dunnill MS. The pathology of asthma, Respir Dis 1993;147:405-10.
22. Smith AD, Cowan JO, Brassett KP, with special reference to changes in the 36. Chetta A, Foresi A, Del Donno M, Ber-
Herbison GP, Taylor DR. Use of exhaled bronchial mucosa. J Clin Pathol 1960;13: torelli G, Pesci A, Olivieri D. Airways re-
nitric oxide measurements to guide treat- 27-33. modeling is a distinctive feature of asth-
ment in chronic asthma. N Engl J Med 29. Messer JW, Peters GA, Bennett WA. ma and is related to severity of disease.
2005;352:2163-73. Causes of death and pathologic findings in Chest 1997;111:852-7.
23. Deykin A, Lazarus SC, Fahy JV, et al. 304 cases of bronchial asthma. Dis Chest Copyright © 2007 Massachusetts Medical Society.
Sputum eosinophil counts predict asthma 1960;38:616-24.
Lantern Slides Updated: Complete PowerPoint Slide Sets from the Clinicopathological Conferences
Any reader of the Journal who uses the Case Records of the Massachusetts General Hospital as a teaching exercise or reference
material is now eligible to receive a complete set of PowerPoint slides, including digital images, with identifying legends,
shown at the live Clinicopathological Conference (CPC) that is the basis of the Case Record. This slide set contains all of the
images from the CPC, not only those published in the Journal. Radiographic, neurologic, and cardiac studies, gross specimens,
and photomicrographs, as well as unpublished text slides, tables, and diagrams, are included. Every year 40 sets are produced,
averaging 50-60 slides per set. Each set is supplied on a compact disc and is mailed to coincide with the publication of the
Case Record.
The cost of an annual subscription is $600, or individual sets may be purchased for $50 each. Application forms for the current
subscription year, which began in January, may be obtained from the Lantern Slides Service, Department of Pathology,
Massachusetts General Hospital, Boston, MA 02114 (telephone 617-726-2974) or e-mail Pathphotoslides@partners.org.
n engl j med 356;20 www.nejm.org may 17, 2007 2091
The New England Journal of Medicine
Downloaded from nejm.org on September 18, 2013. For personal use only. No other uses without permission.
Copyright © 2007 Massachusetts Medical Society. All rights reserved.
Das könnte Ihnen auch gefallen
- Case 2Dokument4 SeitenCase 2Patrícia Martins25% (4)
- Anger ManagementDokument174 SeitenAnger ManagementRatna Prasad100% (5)
- Economic Traits For Sheep and GoatDokument18 SeitenEconomic Traits For Sheep and GoatAdarshBijapur89% (9)
- Páginas Desdepharmacotherapy Casebook 10th Ed.Dokument61 SeitenPáginas Desdepharmacotherapy Casebook 10th Ed.Glo VsNoch keine Bewertungen
- Jurnal AsmaDokument12 SeitenJurnal AsmaaulNoch keine Bewertungen
- DR Eric Brestel's Sep 5 2000 Letter To EditorDokument2 SeitenDR Eric Brestel's Sep 5 2000 Letter To EditorRobert Davidson, M.D., Ph.D.Noch keine Bewertungen
- The Effects of Laparoscopic Nissen FundoplicationDokument2 SeitenThe Effects of Laparoscopic Nissen FundoplicationGabriel CassNoch keine Bewertungen
- ACCP Ambulatory CareDokument50 SeitenACCP Ambulatory CareJim DansNoch keine Bewertungen
- Malmstrom Et Al - 1999 - Oral Montelukast, Inhaled Beclomethasone, and Placebo For Chronic AsthmaDokument10 SeitenMalmstrom Et Al - 1999 - Oral Montelukast, Inhaled Beclomethasone, and Placebo For Chronic AsthmaRutvik ShahNoch keine Bewertungen
- PulmonaryDokument54 SeitenPulmonarytheonlinegeekhubNoch keine Bewertungen
- Mepolizumab For Prednisone-Dependent Asthma With Sputum EosinophiliaDokument9 SeitenMepolizumab For Prednisone-Dependent Asthma With Sputum EosinophiliaSurya Perdana SiahaanNoch keine Bewertungen
- Nishant Respiratory SecondDokument10 SeitenNishant Respiratory SecondNishantNoch keine Bewertungen
- Kasus AsmaDokument5 SeitenKasus AsmaHananun Zharfa0% (3)
- 1 s2.0 S1016319010600092 MainDokument5 Seiten1 s2.0 S1016319010600092 MainYasmine MonttNoch keine Bewertungen
- Questions BasedDokument69 SeitenQuestions Baseds007750Noch keine Bewertungen
- Case Report AsliDokument4 SeitenCase Report AsliLidiaNoch keine Bewertungen
- Multidrug Resistant Pneumonia: A Case Study: April 2018Dokument4 SeitenMultidrug Resistant Pneumonia: A Case Study: April 2018ummuNoch keine Bewertungen
- Evaluation of Step-Down Therapy From An Inhaled Steroid To Montelukast in Childhood AsthmaDokument7 SeitenEvaluation of Step-Down Therapy From An Inhaled Steroid To Montelukast in Childhood AsthmaAriNoch keine Bewertungen
- Annotated-Tuberculosis PresentationDokument42 SeitenAnnotated-Tuberculosis PresentationAnna mae AaronNoch keine Bewertungen
- TCRM 7 459 PDFDokument13 SeitenTCRM 7 459 PDFMikhael JHNoch keine Bewertungen
- Pediatric AsthmaDokument63 SeitenPediatric Asthmasrober0565Noch keine Bewertungen
- Pulmonary Medicine - Case StudyDokument9 SeitenPulmonary Medicine - Case StudyFerdinand YuzonNoch keine Bewertungen
- A Comparison of Oral Procaterol and Albuterol in Reversible Airflow ObstructionDokument6 SeitenA Comparison of Oral Procaterol and Albuterol in Reversible Airflow Obstructionparris shanyNoch keine Bewertungen
- Nejmoa 1814917Dokument11 SeitenNejmoa 1814917yasserNoch keine Bewertungen
- Nejm200009073431003 PDFDokument6 SeitenNejm200009073431003 PDFaprid dhawatiNoch keine Bewertungen
- COPD - Drug FormularyDokument32 SeitenCOPD - Drug FormularyCharles BayogNoch keine Bewertungen
- TB MDR Primer Dengan Limfadenitis TB Pada Wanita SLE: Jurnal RespirasiDokument7 SeitenTB MDR Primer Dengan Limfadenitis TB Pada Wanita SLE: Jurnal RespirasiindraNoch keine Bewertungen
- TB MDR Primer Dengan Limfadenitis TB Pada Wanita SLE: Jurnal RespirasiDokument7 SeitenTB MDR Primer Dengan Limfadenitis TB Pada Wanita SLE: Jurnal RespirasiImam SyaifullahNoch keine Bewertungen
- 1 s2.0 S1755001708000109 MainDokument5 Seiten1 s2.0 S1755001708000109 MainRazmi Wulan DiastutiNoch keine Bewertungen
- 2.5 Ethambutol in The Treatment of Patients With Chronic Pulmonary TuberculosisDokument4 Seiten2.5 Ethambutol in The Treatment of Patients With Chronic Pulmonary TuberculosisRara IndrianiNoch keine Bewertungen
- La Eficacia Del Sulfato de Magnesio para El Estado Asmático Fuera Del Entorno de Cuidados IntensivosDokument6 SeitenLa Eficacia Del Sulfato de Magnesio para El Estado Asmático Fuera Del Entorno de Cuidados IntensivosCesar Jesus Jara VargasNoch keine Bewertungen
- Br. J. Anaesth. 2013 Schutte Bja Aet257Dokument4 SeitenBr. J. Anaesth. 2013 Schutte Bja Aet257Mădălina RădulescuNoch keine Bewertungen
- An Extremely Rare and Life Threatening Thyrotoxicosis - FinalDokument12 SeitenAn Extremely Rare and Life Threatening Thyrotoxicosis - FinalChristian PoerniawanNoch keine Bewertungen
- Early Intervention in Childhood AsthmaDokument33 SeitenEarly Intervention in Childhood Asthmadr_reddy_lufyanNoch keine Bewertungen
- Sevoflurane Case ReportDokument0 SeitenSevoflurane Case Reportyvonne_dr72Noch keine Bewertungen
- 1 Sumreen Case ReportDokument4 Seiten1 Sumreen Case ReportNosheen JavedNoch keine Bewertungen
- Epinephrine Medication ErrorDokument3 SeitenEpinephrine Medication ErrorNirwana AshanNoch keine Bewertungen
- Use of Biologics in AsthmaDokument55 SeitenUse of Biologics in Asthmaosama.khalifaNoch keine Bewertungen
- Cardiac Arrest Upon Induction of General AnesthesiaDokument7 SeitenCardiac Arrest Upon Induction of General AnesthesiaIlona HiariejNoch keine Bewertungen
- Jurnal AsthmaDokument11 SeitenJurnal AsthmaNadira Juanti PratiwiNoch keine Bewertungen
- Au Di Major Case Study HistoplasmosisDokument18 SeitenAu Di Major Case Study Histoplasmosisapi-301816885Noch keine Bewertungen
- Mepolizumab For Prednisone-Dependent Asthma With Sputum EosinophiliaDokument9 SeitenMepolizumab For Prednisone-Dependent Asthma With Sputum EosinophiliaKinan BasalimNoch keine Bewertungen
- AsthmaDokument10 SeitenAsthmaWidia Siti SarahNoch keine Bewertungen
- Formoterol, A New Long-Acting Bronchodilator For InhalationDokument6 SeitenFormoterol, A New Long-Acting Bronchodilator For InhalationAlief AkbarNoch keine Bewertungen
- Idiopathic HiccupDokument3 SeitenIdiopathic HiccupSuresh IndiaNoch keine Bewertungen
- Ijopp 6 2 2013 14Dokument3 SeitenIjopp 6 2 2013 14Deepak SharmaNoch keine Bewertungen
- NCM 112 Rle Case Analysis: Care of Client With Alterations in Oxygenation (ASTHMA)Dokument2 SeitenNCM 112 Rle Case Analysis: Care of Client With Alterations in Oxygenation (ASTHMA)Joegie ArioNoch keine Bewertungen
- Bronchial AsthmaDokument3 SeitenBronchial AsthmaSabrina Reyes0% (1)
- Ok O'ByrneDokument12 SeitenOk O'ByrneChristian OliveiraNoch keine Bewertungen
- Midazolam Prevent AgitationDokument13 SeitenMidazolam Prevent AgitationUzZySusFabregasNoch keine Bewertungen
- Nej Mo A 1411481Dokument12 SeitenNej Mo A 1411481Indra PermanaNoch keine Bewertungen
- Treatment of Status Migrainosus by General AnestheDokument3 SeitenTreatment of Status Migrainosus by General AnesthenurulwindianggrainiNoch keine Bewertungen
- 10 1056@NEJMoa1715274Dokument12 Seiten10 1056@NEJMoa1715274Paul ParrasNoch keine Bewertungen
- Treatment of AsthmaDokument22 SeitenTreatment of AsthmaMedranoReyesLuisinNoch keine Bewertungen
- Teofilina Vs AcebrofilinaDokument9 SeitenTeofilina Vs AcebrofilinaAgencia FaroNoch keine Bewertungen
- Antivenom For Critically Ill Children With Neurotoxicity From Scorpion StingsDokument9 SeitenAntivenom For Critically Ill Children With Neurotoxicity From Scorpion StingsBreiner Andres LopezNoch keine Bewertungen
- Sevoflurane Administration in Status Asthmaticus: A Case ReportDokument2 SeitenSevoflurane Administration in Status Asthmaticus: A Case ReportMădălina RădulescuNoch keine Bewertungen
- A Patient With Suspected Diphtheria - Journal of Universitas AirlanggaDokument8 SeitenA Patient With Suspected Diphtheria - Journal of Universitas AirlanggaNur Rahmat WibowoNoch keine Bewertungen
- Remifentanil in The Management of Severe TetanusDokument3 SeitenRemifentanil in The Management of Severe TetanusSitiNoch keine Bewertungen
- Fergie 2Dokument8 SeitenFergie 2RambuNoch keine Bewertungen
- Fast Facts: Asthma: Improve patient self-management and drug use, achieve asthma controlVon EverandFast Facts: Asthma: Improve patient self-management and drug use, achieve asthma controlNoch keine Bewertungen
- Answer All The Following Short Essay Questions: (3 Questions)Dokument4 SeitenAnswer All The Following Short Essay Questions: (3 Questions)Soad ShedeedNoch keine Bewertungen
- JAYPEE Handbook of Blood Banking - Transfusion Medicine, 2006Dokument366 SeitenJAYPEE Handbook of Blood Banking - Transfusion Medicine, 2006Dwi della yaumil qitmiaNoch keine Bewertungen
- Stem CellDokument8 SeitenStem Cellapi-220278259Noch keine Bewertungen
- Test Report: Method: Qualitative Real Time PCR by Quantstudio 5 (ABI) Thermo Scientific, USA Icmr Reg No: PacapalabvgDokument2 SeitenTest Report: Method: Qualitative Real Time PCR by Quantstudio 5 (ABI) Thermo Scientific, USA Icmr Reg No: PacapalabvgDevendra SinghNoch keine Bewertungen
- Study Guide 12 StsDokument9 SeitenStudy Guide 12 StsJovan Marie ElegadoNoch keine Bewertungen
- Phenomenology of Squalor, Hoarding and Self-NeglectDokument5 SeitenPhenomenology of Squalor, Hoarding and Self-NeglectastrogliaNoch keine Bewertungen
- 1.1 IB Cell TheoryDokument32 Seiten1.1 IB Cell TheoryVenya NaiduNoch keine Bewertungen
- Unit 5 Module 12 CombinedDokument9 SeitenUnit 5 Module 12 Combinedapi-293001217Noch keine Bewertungen
- Comportamiento Del Ibuprofeno en La Reparación OseaDokument7 SeitenComportamiento Del Ibuprofeno en La Reparación OseaGilliam SierraNoch keine Bewertungen
- Benefits of MangosteenDokument4 SeitenBenefits of Mangosteenmunj100% (1)
- Koagulasi DarahDokument2 SeitenKoagulasi DarahSekar NugraheniNoch keine Bewertungen
- CH 14 Darwin and EvolutionDokument39 SeitenCH 14 Darwin and EvolutionJane Heidi MomonganNoch keine Bewertungen
- Summary Notes For Wakefulness and SleepDokument4 SeitenSummary Notes For Wakefulness and Sleepbobadilla.sarah19Noch keine Bewertungen
- Gamma Knife1Dokument17 SeitenGamma Knife1api-247561652Noch keine Bewertungen
- Production Recombinant Therapeutics in E. ColiDokument11 SeitenProduction Recombinant Therapeutics in E. ColiStephany Arenas100% (2)
- Allergy 2010Dokument7 SeitenAllergy 2010HAOMSNoch keine Bewertungen
- TTNFF PDFDokument7 SeitenTTNFF PDFHendroNoch keine Bewertungen
- Qualis NovosDokument914 SeitenQualis NovoshgdfdNoch keine Bewertungen
- Muscular DystrophyDokument21 SeitenMuscular DystrophyIqra Iftikhar100% (4)
- Papaya Leaves in Increasing PlateletsDokument25 SeitenPapaya Leaves in Increasing PlateletsRichard BacharNoch keine Bewertungen
- MAF - MednetDokument3 SeitenMAF - MednetMuhammad Siddiuqi100% (1)
- Fundamentals of Microbiological ControlDokument4 SeitenFundamentals of Microbiological Controlsonali tendulkar100% (2)
- Annona SquamosaDokument10 SeitenAnnona SquamosaAlarm GuardiansNoch keine Bewertungen
- Steroid Hormones! Mechanisms of Action!Dokument14 SeitenSteroid Hormones! Mechanisms of Action!leh.mo9315Noch keine Bewertungen
- La Biología de La Cromatina Complejos de Remodelación: FurtherDokument24 SeitenLa Biología de La Cromatina Complejos de Remodelación: FurtherVíc AltamarNoch keine Bewertungen
- History: Pandaemonium 1660 - 1886Dokument3 SeitenHistory: Pandaemonium 1660 - 1886Shoumik DeyNoch keine Bewertungen
- Dna StructureDokument23 SeitenDna StructureAnonymous mHS76aNoch keine Bewertungen
- H MoleDokument23 SeitenH MoleJoel Santos100% (1)