Beruflich Dokumente
Kultur Dokumente
Chapter 4: Medication Management: Key Terms & Definitions Drug Monograph
Hochgeladen von
cooole0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
31 Ansichten3 SeitenOriginaltitel
Chap 4 .pdf
Copyright
© © All Rights Reserved
Verfügbare Formate
PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
31 Ansichten3 SeitenChapter 4: Medication Management: Key Terms & Definitions Drug Monograph
Hochgeladen von
coooleCopyright:
© All Rights Reserved
Verfügbare Formate
Als PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 3
Chapter
4: Medication Management • Select medications for inclusion by considering
clinical, quality of life, safety &
Key Terms & Definitions pharmacoeconomic outcomes
• Drug monograph – written, unbiased • Evaluates med use outcomes
evaluation of a specific medication; drug name, • Monitors adverse drug reactions
therapeutic class, pharmacology, indications, • Develops policies & procedures for handling
clinical trials, ADE, drug interactions medications
• Educate health professionals
The Formulary System Formulary System Maintenance
– ongoing process whereby a HCO establishes policies on • Review medication list & guidelines on a regular
the use of drug products & therapies basis
• Drug Formulary – continually updated list of Medication Selection and Review
medications & related info, representing the • Established methods for medication selection &
clinical judgment of RPh, physicians & other review
experts in treatment of disease & promotion of • Med.selection criteria: med efficacy, safety & cost
health • Barriers to optimal formulary decisions
• List of medications routinely stocked o Physician experience w/ drug &
• developed in the 1950s as a management tool ; preference
discourage the use of marginally effective drugs o Detailing by pharmaceutical company
& treatments representatives
• Element of a system that includes med. Use o Unpublished / anecdotal studies
policies, PT&C, med use evaluation, & formulary Medication Use Evaluation ( MUE )
management • Method for evaluating & improving med-use
• Advantage: provides a systematic method to process w/ the goal of optimal patient outcomes
review scientific evidence on clinical • Foundation of med-use process
effectiveness in drug selection decision o Establish a specific criteria for use
• Disadvantage: overly restrictive formulary, o Review for compliance ; Routine review
limited access to medications of data
• Key to process – timely data to review, action
Pharmacy & Therapeutics Committee plan development , follow up
Organization Medication Safety Evaluation
• Committee is a policy recommending body to the • Evaluated through adverse drug reaction reports
medical staff & medication error reports
• Medical executive committee – grp of the Drug Therapy Guidelines
hospital medical staff in charge of institutional • Listing of the indications, dosage regimens,
governance & performance ; w/ primary duration of therapy, mode of administration,
authority for activities related to self governance monitoring parameters & special precautions
& performance improvement • Developed w/ the oversight of practitioners w/
• Health-system board - non-medical staff expertise in the management of disease
advisory committee of hospital members & o Use of pre-printed physician order sheet
community members that governs the affairs of Policy and Procedure Development
hospital • Medication administration process
• Subcommittees / task forces – facilitate meeting • Medications administered in specific locations
efficiency Education
o Medication safety – review of adverse • Newsletter that includes clinical info on drugs
drug events & med errors • Presentation at meetings, health-system website
o Medication use review – performance-
improvement method that focuses on Regulatory & Accrediting Bodies
evaluating & improving med-use • RB: State Dept of Health , Board of Pharmacy
processes for optimal pt outcomes • AB: TJC , AOA, Commission on Accreditation of
o Drug review panels – review drug in an Rehabilitation Facilities ( CARF )
area of specialty ( cardiology )
Pharmacist Role
Committee Membership • Establish P&T committee meeting
• RPh, nurses, physicians, administrators, risk / • Analyze & disseminate scientific, clinical
quality improvement managers information
• Medication management is a multidisciplinary • Conduct drug use evaluation
process • Record & archive P&TC committee actions
• Follow-up w/ research
Responsibilities • Communicate PTC decisions to other health care
• Establish & maintain the formulary system professionals
Formulary Management • Dosage form and cost – table listing comparable
• Open Formularies – generally large, no limitation agents may be useful in formulary addition
to access to a medication • Summary
• Recommendation – formulary addition, restriction,
• Closed formularies – limited list of medications
deletion
to specific physicians, patient care areas, disease
• References –peer-reviewed primary literature
states via formulary restrictions
• Formulary Restrictions –act of limiting the use fo
Therapeutic Class review
specific formulary medications to specific
• Should not be too broad or all inclusive
physicians based on areas of expertise
• New medical info, adverse event profiles,
• Institute of Medicine ( IOM ) evaluated the
purchase or use data
Veterans Administration ( VA ) National
• Objective; have the optimal agents w/in each
Formulary impact on health care costs in six
consideration
closed or preferred class of drugs
• FDS defines the equivalence of indiv chemical
Formulary Changes
entities or generic equivalents
• Process to continually update the formulary
o Approved Drug Products w/
must be established
Therapeutic Equivalence – Orange Book
• Submission of request for making additions &
• Therapeutic Equivalents
deletions ( agent to be added/deleted, rationale
o Drug products w/ diff chemical
for request, alternative agents )
structure but same pharmacologic /
therapeutic class and effects ( ex. 1st gen.
Nonformulary Drug Review
cephalosporin , histamine-2 blockers )
• Nonformulary agent – medication not part of
• Therapeutic Interchange
drug formulary ; not considered but P&TC
o Authorized exchange of therapeutic
choosing to add it
alternatives in accordance w/
• Automating medication prescribing process
previously approved guidelines ; must
o Computerized prescriber order entry
include dosage strength, frequency, &
o Order Entry Rules – logic established
route of administration
w/in the hospital info system order
• Guidelines for generic substitution
entry module to notify prescribers of
o RPh is responsible for selecting generic
adverse effects ; include weight based
drugs ; P&TC determines therapeutic
dosing, laboratory tests, allergy checks
equivalents
o Pop-ups – info that appears on a
o Prescribers may specify a specific brand
computer monitor when a specific
if clinically justified
actions are taken ; may contain clinical
• Formulary maintenance – ongoing process of
info about med use, drug interactions
assuring relative safety & efficacy of agents
available for use
Drug Use Evaluation ( DUE )
o New product evaluation
• Systematic process used to assess the
o Therapeutic class review – evaluation of
appropriateness of drug therapy by engaging in
a group of medications w/ an
the evaluation of data on drug use
established therapeutic class ; indication
• Medication Use Evaluation ( MUE ) –
for use, dynamics, ADE, drug
encompasses the goals & objectives of DUE in its
interactions
broadest application
o Formulary changes
• first established in 1980s
o Nonformulary drug use review
• provide an ongoing, structured, organized
approach to ensure that drugs are used
New Product Evaluation ( standard elements )
• Generic name – name of all chemical entities appropriately
• Trade name • Outcome assessment – systematic process of
• Therapeutic / Pharmacologic Class evaluating the appropriateness, safety, & efficacy
• Pharmacology – mechanism of action & of a medication ; review of pt medical records
pharmacologic effects • Multiple performance improvement models
• Pharmacokinetics – how drug is handled by the body, o FOCUS-PDCA ( or PDSA )
onset of effect, serum half-life, metabolic § Find process to improve
considerations, route of excretion § Organize a team that knows
• Indications for use § Clarify current knowledge
• Clinical studies – clinical study data supporting § Understand causes of process
indications for use ( statistical analysis, outcomes, info variation
on patient info ) § Select process improvement
• Adverse effects/ warnings – methods to reduce , risk § Plan ; Do ; Check ( or study ) ; Act
& benefit of drug therapy, precautions in pregnancy
• Drug interactions – drug-drug, drug-food
• Dosage range – dosage range for diff routes, age,
hepatic function
• Medication use criteria • Floor Stock – criteria for selecting agents for floor
o Diagnosis-related DUE –criteria identify stock
indications for w/c select drugs may be • Definition of order interpretation – meaning of
appropriate for a given disease specific types of orders ( sliding scale orders, ranger
orders, needed, tapering, titrating orders)
o Prescriber-related DUE – identify
• Medication Administration times – specific time &
specific physicians whom the P&TC has
rules for interpretation
determined may use certain drugs • Adverse Drug Reactions
o Drug-specific DUE – focus on specific • Medication errors
aspects of select drug such as dose or
frequency Published Formulary
• Data should be collected during the patient visit ( • Should provide info on the medications
concurrent ) rather than retrospectively ( chart approved for use, basic therapeutic information
review ) about each item
• Technology: Personal Data Assistant ( PDA )
• Task force should develop an action plan & Medication List
criteria • Includes entries for each medication and indexes
• Action plan: devlpt of drug use guidelines,
to facilitate use
preprinted orders, med order entry rules,
• Generic name of Primary active ingredient
formulary changes
• Trade or Synonym name that is commonly used
• Dosage form, strength, & size stocked
Medication Use Policies
• Active ingredients ( formulation )
• Formulary management ; P&T committee ;
• DEA schedule
medication prescribing, dispensing,
administration • Special precautions
• Pediatric / adult dosage ranges
Formulary Management • Cost information
• Should include information on who use a specific • Index arranged alphabetically or generically by
agent ; how a drug is added / deleted, stocked therapeutic class
• Formulary Restriction policy –define how items
are selected for formulary restriction, rationale Medication Use Policy & Procedures
for selecting prescribers, method of managing • Info on prescribing, dispensing, administration
process
• Formulary policy – describe the method for drug Medication Use Guidelines
addition & deletion ( chemical entity , dosage • Detailed guidelines for medication use
forms, strengths ) • Antibiotic use guidelines ; antibiotic use in
surgical prophylaxis
Pharmacy and Therapeutics Committee • Weight-based heparin orders
• Should address the committee membership, • ICU sedation guidelines ; alcohol detox orders
operation and responsibilities • potassium replacement order
• thrombolytic therapy guidelines for stroke
Medication Prescribing, Dispensing, &
Administration Special information
• Writing Medication Orders – defines practitioners that • Health-system specific
may write Rx ; format of Rx • Tailored to the needs of the professional &
• Verbal Orders – defines who may accept a verbal medical staff based on the services
order & the transcription process ; address the
• Nutritional products approved ; equivalent
reading back of the order
dosage tab ; parenteral nutrition formula ;
• Stop Orders – defines the orders that are
pediatric dosage ; antidote list ; serum drug level
automatically terminated, method of reinstatement ;
for medications that require additional evaluation ; antibiograms ; common equations ; advanced
• Investigational Drug Orders –defines how cardiac life support
investigational drugs are managed in the health care
system; include review process & method for
prescribing, dispensing
• Controlled Substances – defines the flow of controlled
substances ; approved prescribers, order process,
distribution & tracking
• Generic & therapeutic Substitution – defines how a
drug is selected for generic substitution ; describe
alternative agent
• Self-administration of medications – conditions &
process for the adminis. of med by the pt.
• Medication Samples – conditions & process for the use
of med samples
Das könnte Ihnen auch gefallen
- Medication Use Evaluation CurrentDokument3 SeitenMedication Use Evaluation CurrentSarahkheridNoch keine Bewertungen
- ACCP - Comprehensive Medication Management in Team-Based CareDokument8 SeitenACCP - Comprehensive Medication Management in Team-Based CareThuane SalesNoch keine Bewertungen
- For Mend PrinciplesDokument4 SeitenFor Mend PrinciplesAndri FerdianNoch keine Bewertungen
- Pharmacy and Therapeutic CommitteeDokument26 SeitenPharmacy and Therapeutic CommitteeRana Ehtisham100% (2)
- 3C DTCDokument40 Seiten3C DTCekramNoch keine Bewertungen
- Clinical Pharmacy PHR 405: Chapter 1: General ConsiderationsDokument24 SeitenClinical Pharmacy PHR 405: Chapter 1: General ConsiderationsSamiul Alam Rajib100% (1)
- FormularyDokument32 SeitenFormularyAnonymous U4JLHU9e3100% (1)
- M1 Hospital Pharmacy InternshipDokument5 SeitenM1 Hospital Pharmacy InternshipKyle BulloNoch keine Bewertungen
- Drug Utilisation ReviewDokument33 SeitenDrug Utilisation ReviewkeerthanaNoch keine Bewertungen
- Week 7 - PHR514-Pharmacy Law and Regulatory AffairsDokument31 SeitenWeek 7 - PHR514-Pharmacy Law and Regulatory AffairsNeymar ShuvoNoch keine Bewertungen
- Drug Utilisation EvaluationDokument43 SeitenDrug Utilisation Evaluationpavani valluriNoch keine Bewertungen
- Dur and Due - 2016Dokument15 SeitenDur and Due - 2016AriNoch keine Bewertungen
- Oncology Practice Models - Matthews - 6 Slides Per PageDokument9 SeitenOncology Practice Models - Matthews - 6 Slides Per PageMaría Eugenia Martínez MónacoNoch keine Bewertungen
- Chap 3. Drug Utilization EvaluationDokument28 SeitenChap 3. Drug Utilization EvaluationAizaz AhmadNoch keine Bewertungen
- Hospital FormularyDokument18 SeitenHospital Formularyranemabdo22Noch keine Bewertungen
- Introduction To Clinical PharmacyDokument19 SeitenIntroduction To Clinical PharmacyAnisha PandeyNoch keine Bewertungen
- Lec 3 HospitalDokument13 SeitenLec 3 HospitalAya Eid 7asanNoch keine Bewertungen
- ASHP Guidelines On Formulary System Management: PreambleDokument4 SeitenASHP Guidelines On Formulary System Management: Preambleanisa rachmitaNoch keine Bewertungen
- 1-Introduction To Clinical PharmacyDokument25 Seiten1-Introduction To Clinical PharmacyDr-Muhammad Junaid Hassan SharifNoch keine Bewertungen
- Medication SafetyDokument30 SeitenMedication SafetyAprilSenseng100% (1)
- Introduction To Drug Information Services: DR Dzul Azri Mohamed Noor Dzulazri@usm - MyDokument25 SeitenIntroduction To Drug Information Services: DR Dzul Azri Mohamed Noor Dzulazri@usm - MyLakshmanan ValliappanNoch keine Bewertungen
- MODULE 4 PharmacovigilanceDokument20 SeitenMODULE 4 PharmacovigilanceJUDYANN PINEDANoch keine Bewertungen
- Rational Drug Therapy: By: Associate Professor Dept of Pharmacology JSS Medical CollegeDokument36 SeitenRational Drug Therapy: By: Associate Professor Dept of Pharmacology JSS Medical CollegeVenu D DonNoch keine Bewertungen
- Essential Drug Concept & Rational Use of Drugs RDU: The Use of Appropriate, Efficacious, Safe and Cost-Effective Drug Given For The RightDokument9 SeitenEssential Drug Concept & Rational Use of Drugs RDU: The Use of Appropriate, Efficacious, Safe and Cost-Effective Drug Given For The RightParth GandhiNoch keine Bewertungen
- Concept of Clinical PharmacyDokument30 SeitenConcept of Clinical PharmacyKishori Kedia100% (4)
- Medication Use Evaluation CurrentDokument18 SeitenMedication Use Evaluation CurrentintanNoch keine Bewertungen
- Hospital Formulary-Lecture NotesDokument7 SeitenHospital Formulary-Lecture NotesPatras BhattiNoch keine Bewertungen
- Clinical Pharmacy: Definition, Scope and ActivitiesDokument18 SeitenClinical Pharmacy: Definition, Scope and ActivitiesSachin MishraNoch keine Bewertungen
- Daily Activities of A Clinical PharmacistDokument20 SeitenDaily Activities of A Clinical PharmacistAnoop Tandur0% (1)
- ASHP Guidelines On A Standardized Method For Pharmaceutical CareDokument3 SeitenASHP Guidelines On A Standardized Method For Pharmaceutical CareAnonymous hys2qeBRvNoch keine Bewertungen
- Chapter 4Dokument19 SeitenChapter 4EmmaNoch keine Bewertungen
- 3063-20220805085327-PD Pharmacist July 2022Dokument7 Seiten3063-20220805085327-PD Pharmacist July 2022Raheel KhanNoch keine Bewertungen
- Guidelines For The Medicines and Therapeutics CommitteeDokument20 SeitenGuidelines For The Medicines and Therapeutics CommitteeLorezza Miranda Aguilar100% (1)
- K12 Rational Drugs Selection Based On EBMDokument49 SeitenK12 Rational Drugs Selection Based On EBMdinda annisaNoch keine Bewertungen
- ASHP Medication Use EvaluationDokument3 SeitenASHP Medication Use EvaluationArslan BashirNoch keine Bewertungen
- Pharma Lesson 1Dokument3 SeitenPharma Lesson 1BabyJane GRomeroNoch keine Bewertungen
- DISPENSINGDokument1 SeiteDISPENSINGJENSEL CLOUIE C. REGLOSNoch keine Bewertungen
- Introduction To Drug Supply ManagementDokument39 SeitenIntroduction To Drug Supply ManagementfikebatuNoch keine Bewertungen
- Pharmacy and Therapeutics Committee Policies and ProceduresDokument11 SeitenPharmacy and Therapeutics Committee Policies and ProceduresJedDesabille67% (3)
- A Guide To Patient Medication Review: September 2003Dokument33 SeitenA Guide To Patient Medication Review: September 2003Muhamad GunturNoch keine Bewertungen
- Medication Management: Abcede - Azurin.Bautista - Borromeo.Chica - Cinconiegue 2C-PHDokument73 SeitenMedication Management: Abcede - Azurin.Bautista - Borromeo.Chica - Cinconiegue 2C-PHbambamborromeoNoch keine Bewertungen
- Drug Utilization Evaluation FinalDokument13 SeitenDrug Utilization Evaluation FinalNikkiiNoch keine Bewertungen
- Prescribing Competencies: Mrs. Satyapriya M.Sc. Nursing (Community Health Nursing) Lecturer Government College of NursingDokument16 SeitenPrescribing Competencies: Mrs. Satyapriya M.Sc. Nursing (Community Health Nursing) Lecturer Government College of Nursingvani reddyNoch keine Bewertungen
- Preceptor Development: Patient Care Process: The Pharmacy Care PlanDokument11 SeitenPreceptor Development: Patient Care Process: The Pharmacy Care PlantyaNoch keine Bewertungen
- Minimum Standards For Pharmacies in HospitalsDokument10 SeitenMinimum Standards For Pharmacies in HospitalsharibinnocentNoch keine Bewertungen
- Slid CH01Dokument20 SeitenSlid CH01Susan EllisNoch keine Bewertungen
- Standards of PracticeDokument4 SeitenStandards of PracticealzafaNoch keine Bewertungen
- 5 Role of Pharmacist in PHDokument20 Seiten5 Role of Pharmacist in PHمحمد العمريNoch keine Bewertungen
- Week4 PTC Formulary DispensingDokument7 SeitenWeek4 PTC Formulary DispensingChunnie JakosalemNoch keine Bewertungen
- Chapter 1 Institutional Pharmacy PracticeDokument2 SeitenChapter 1 Institutional Pharmacy PracticecoooleNoch keine Bewertungen
- Pharmaceutical Care ConceptDokument38 SeitenPharmaceutical Care ConceptTiti SulistiowatiNoch keine Bewertungen
- 3B - Clinical PharmacyDokument35 Seiten3B - Clinical PharmacyekramNoch keine Bewertungen
- 3B - Clinical PharmacyDokument35 Seiten3B - Clinical PharmacyekramNoch keine Bewertungen
- p2371 Sample Chapter 4Dokument22 Seitenp2371 Sample Chapter 4Kayla Andrea CalibaNoch keine Bewertungen
- Ward Round ParticipationDokument19 SeitenWard Round ParticipationAnisha PandeyNoch keine Bewertungen
- Introduction To Acute and Ambulatory Care Pharmacy PracticeDokument100 SeitenIntroduction To Acute and Ambulatory Care Pharmacy PracticeDanielle De GuzmanNoch keine Bewertungen
- Quality Control and Drug AnalysisDokument57 SeitenQuality Control and Drug AnalysisIhab AdelNoch keine Bewertungen
- Medication Use Evaluation (MUE)Dokument16 SeitenMedication Use Evaluation (MUE)tsedaleNoch keine Bewertungen
- A Textbook of Clinical Research and PharmacovigilanceVon EverandA Textbook of Clinical Research and PharmacovigilanceBewertung: 3.5 von 5 Sternen3.5/5 (3)
- Renal Pharmacotherapy: Dosage Adjustment of Medications Eliminated by the KidneysVon EverandRenal Pharmacotherapy: Dosage Adjustment of Medications Eliminated by the KidneysNoch keine Bewertungen
- Mumps S/diseases/mumps - HTML: Why Should My Child Get The MMR Shot?Dokument3 SeitenMumps S/diseases/mumps - HTML: Why Should My Child Get The MMR Shot?coooleNoch keine Bewertungen
- Diagnostic Testing - Yellow FeverDokument2 SeitenDiagnostic Testing - Yellow FevercoooleNoch keine Bewertungen
- Transmission of Yellow Fever VirusDokument1 SeiteTransmission of Yellow Fever ViruscoooleNoch keine Bewertungen
- Symptoms, Diagnosis, & Treatment of Yellow Fever VirusDokument3 SeitenSymptoms, Diagnosis, & Treatment of Yellow Fever ViruscoooleNoch keine Bewertungen
- Yellow Fever VaccinationDokument2 SeitenYellow Fever VaccinationcoooleNoch keine Bewertungen
- Frequently Asked Questions About Yellow FeverDokument6 SeitenFrequently Asked Questions About Yellow FevercoooleNoch keine Bewertungen
- Diphtheria, Tetanus, and Whooping Cough Vaccination - What Everyone Should KnowDokument20 SeitenDiphtheria, Tetanus, and Whooping Cough Vaccination - What Everyone Should KnowcoooleNoch keine Bewertungen
- Vaccine (Shot) For MeaslesDokument3 SeitenVaccine (Shot) For MeaslescoooleNoch keine Bewertungen
- Rotavirus: When Should My Baby Get The Drops?Dokument2 SeitenRotavirus: When Should My Baby Get The Drops?coooleNoch keine Bewertungen
- Polio Vaccination: at A GlanceDokument7 SeitenPolio Vaccination: at A GlancecoooleNoch keine Bewertungen
- Vaccine (Shot) For Pneumococcal DiseaseDokument7 SeitenVaccine (Shot) For Pneumococcal DiseasecoooleNoch keine Bewertungen
- NCCN Pain ManagementDokument14 SeitenNCCN Pain ManagementcoooleNoch keine Bewertungen
- Whooping Cough (Pertussis)Dokument5 SeitenWhooping Cough (Pertussis)coooleNoch keine Bewertungen
- Hepatitis A Questions and Answers For The PublicDokument8 SeitenHepatitis A Questions and Answers For The PubliccoooleNoch keine Bewertungen
- The History of PharmacyDokument2 SeitenThe History of PharmacycoooleNoch keine Bewertungen
- Human Papillomavirus (HPV) Vaccination - What Everyone Should KnowDokument4 SeitenHuman Papillomavirus (HPV) Vaccination - What Everyone Should KnowcoooleNoch keine Bewertungen
- Chickenpox - Varicella VaccinationDokument2 SeitenChickenpox - Varicella VaccinationcoooleNoch keine Bewertungen
- Capsule Manufacturing TechnologyDokument2 SeitenCapsule Manufacturing TechnologycoooleNoch keine Bewertungen
- Formulation and Physical Properties of Soft Capsules (Gabriele Reich)Dokument13 SeitenFormulation and Physical Properties of Soft Capsules (Gabriele Reich)coooleNoch keine Bewertungen
- Standard Manufacturing Procedure For Syrup and Tablet Forms of Jwarahara DashemaniDokument1 SeiteStandard Manufacturing Procedure For Syrup and Tablet Forms of Jwarahara DashemanicoooleNoch keine Bewertungen
- McDonald's - Early HistoryDokument2 SeitenMcDonald's - Early HistorycoooleNoch keine Bewertungen
- Henry Ford - Founder, Ford Motor CompanyDokument4 SeitenHenry Ford - Founder, Ford Motor CompanycoooleNoch keine Bewertungen
- Introduction of Tablet Manufacturing ProcessDokument5 SeitenIntroduction of Tablet Manufacturing ProcesscoooleNoch keine Bewertungen
- Key Facts About Seasonal Flu VaccineDokument14 SeitenKey Facts About Seasonal Flu VaccinecoooleNoch keine Bewertungen
- JNC8 HTNDokument2 SeitenJNC8 HTNTaradifaNurInsi0% (1)
- Chapter 1 Institutional Pharmacy PracticeDokument2 SeitenChapter 1 Institutional Pharmacy PracticecoooleNoch keine Bewertungen
- Chap 2 - History PDFDokument3 SeitenChap 2 - History PDFcoooleNoch keine Bewertungen
- Chap 2 - History PDFDokument3 SeitenChap 2 - History PDFcoooleNoch keine Bewertungen
- Chapter 15: Parenteral TherapyDokument3 SeitenChapter 15: Parenteral TherapycoooleNoch keine Bewertungen
- Health - Very Very Important Tips: WaterDokument8 SeitenHealth - Very Very Important Tips: WaterLohidas PailaNoch keine Bewertungen
- Renal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarDokument15 SeitenRenal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarSuhas IngaleNoch keine Bewertungen
- PricelistDokument71 SeitenPricelistBugar Wahyu PNoch keine Bewertungen
- Sample of Essay - The FluDokument2 SeitenSample of Essay - The FluMerisa WahyuningtiyasNoch keine Bewertungen
- Above Knee AmputationDokument8 SeitenAbove Knee AmputationAbdul Ghafoor SajjadNoch keine Bewertungen
- Daftar PustakaDokument2 SeitenDaftar PustakaS R PanggabeanNoch keine Bewertungen
- NIV - Past, Present and FutureDokument9 SeitenNIV - Past, Present and FutureDejan ŽujovićNoch keine Bewertungen
- 2015 To 2019 Super Speciality Dissertation Topics PDFDokument35 Seiten2015 To 2019 Super Speciality Dissertation Topics PDFJoseph John Crasto100% (4)
- Lidocaine Infusion A Promising Therapeutic Approach For Chronic PainDokument14 SeitenLidocaine Infusion A Promising Therapeutic Approach For Chronic PaingabhekNoch keine Bewertungen
- SodiumDokument1 SeiteSodiumyoyoyoNoch keine Bewertungen
- Jurnal 3Dokument4 SeitenJurnal 3Arum RaniNoch keine Bewertungen
- Surgical Site MarkingDokument12 SeitenSurgical Site Markingh1m4w4nNoch keine Bewertungen
- High Salivary Soluble L-Selectin and Interleukin-7 Levels in Asian Indian Patients With Primary Sjögren's SyndromeDokument5 SeitenHigh Salivary Soluble L-Selectin and Interleukin-7 Levels in Asian Indian Patients With Primary Sjögren's SyndromeMaite Fernanda CuturrufoNoch keine Bewertungen
- Lesson 2 - Administrative Order No. 2021-0037Dokument10 SeitenLesson 2 - Administrative Order No. 2021-0037Marjan CalzadoNoch keine Bewertungen
- Jtptunimus GDL Handayanig 5251 2 Bab2Dokument42 SeitenJtptunimus GDL Handayanig 5251 2 Bab2Rendra Syani Ulya FitriNoch keine Bewertungen
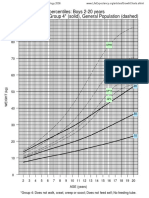
- Weight-For-Age Percentiles: Boys 2-20 Years Cerebral Palsy Group 4 (Solid), General Population (Dashed)Dokument3 SeitenWeight-For-Age Percentiles: Boys 2-20 Years Cerebral Palsy Group 4 (Solid), General Population (Dashed)Feny GoenNoch keine Bewertungen
- Types of AnaesthesiaDokument1 SeiteTypes of AnaesthesiaElaine BriososNoch keine Bewertungen
- Penerapan PMKP RS Arjaty Daud 2022 UPDATEDokument15 SeitenPenerapan PMKP RS Arjaty Daud 2022 UPDATERUNI DARYANTI100% (1)
- TIFF X DAN 6 Week Shred III Workout Program Schedule v2Dokument9 SeitenTIFF X DAN 6 Week Shred III Workout Program Schedule v2808ricksmithNoch keine Bewertungen
- Histopath Unit 1Dokument36 SeitenHistopath Unit 1Kervy PedrazaNoch keine Bewertungen
- Wurzel 2016Dokument8 SeitenWurzel 2016prolanis pkmmulyoharjoNoch keine Bewertungen
- 2010 Bandelow ExtendedDokument16 Seiten2010 Bandelow ExtendedRian YupitaNoch keine Bewertungen
- Pricelist 13 Juli 2020Dokument21 SeitenPricelist 13 Juli 2020Achmad Sya'idNoch keine Bewertungen
- PTSD - Diagnostic CriteriaDokument5 SeitenPTSD - Diagnostic Criteriagreg sNoch keine Bewertungen
- DR - Monobina Sarker (Moic, Ccu) : Howrah District HospitalDokument56 SeitenDR - Monobina Sarker (Moic, Ccu) : Howrah District HospitalDeepa BhattacharjeeNoch keine Bewertungen
- BRO-ZEDEX RANGE Knowledge ExpressDokument7 SeitenBRO-ZEDEX RANGE Knowledge Expressamit khairnarNoch keine Bewertungen
- Drug Information of SilodosinDokument8 SeitenDrug Information of SilodosinSomanath BagalakotNoch keine Bewertungen
- AERGDokument12 SeitenAERGsupaidi97Noch keine Bewertungen
- Adenitis Mesenterica Vs Apendicitis Aguda PDFDokument7 SeitenAdenitis Mesenterica Vs Apendicitis Aguda PDFPaty Alatorre IcazaNoch keine Bewertungen
- Description:: Dance Therapy "In The Mood of Dancing"Dokument2 SeitenDescription:: Dance Therapy "In The Mood of Dancing"kristine_silangNoch keine Bewertungen