Beruflich Dokumente
Kultur Dokumente
Fetal Monitoring: Condition Causes Grade
Hochgeladen von
Sachin SinghOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Fetal Monitoring: Condition Causes Grade
Hochgeladen von
Sachin SinghCopyright:
Verfügbare Formate
Fetal Monitoring
Condition Causes Grade
Fetal tachycardia > 160 bpm Fetal tachycardia can be Mild : > 5 bpm from baseline
caused by an infection of the
fetus or the mom, Mod.: 6- 25 bpm from baseline
dehydration, fever, fetal
hypoxemia, anemia, Severe:>25 bpm from baseline
prematurity, drugs to stop
labor such as terbutaline. Absent: no fluctuation in FHR
Drugs such as caffeine,
epinephrine or theophylline.
Illicit street drugs
Fetal Bradycardia Fetal bradycardia can be Mild : > 5 bpm from baseline
caused by maternal
hypotension, supine Mod.: 6- 25 bpm from baseline
hypotensive syndrome,
Severe:>25 bpm from baseline
fetal decompression . late
fetal hypoxia, cord Absent: no fluctuation in FHR
compression. Abruptio
placenta , vagal stimulation
Variability
FHR drops from baseline then recovers, usually jagged and erricatically shaped. Can happen at
anytime during contraction
Nursing interventions : Leftside. IV bolus of fluids, O2 6l mask, Notify HCP
Decreased or absent variability: Non reassuring, acute tx and monitoring are indicated.
Wandering baselines with no variability could indicate
- Congenital defects
- Metabolic acidosis
The nurse should administer 02 and the baby needs to be delivered quickly as possible.
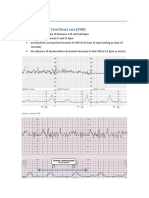
Accelerations: must be 15 BPM above the FHR baseline for 15 seconds ( 15x15 window)
Decelerations : A decrease in FHR during uterine contraction “ U shape” mirrors contractions
Periodic changes : variations that occur during a contraction. “ periodic changes= Period “cramps”
- Reassuring periodic changes : must be 15 BPM above the FHR baseline for 15 seconds ( 15x15
window)
- Benign periodic changes: Early decelerations
Episodic changes: occur in association with medication administration or analgesia “ non uterine”
Decreased or absent variability: medications, narcotics, mag sulfate ( preeclampsia, preterm),
terbutaline, fetal sleep ( normally 20 minute cycles), prematurity, fetal hypoxemia.
Documentation tip : document contractions and FHR q15m
Fetal decelerations
Early decelerations : A decrease in FHR during uterine contraction “ U shape” mirrors uterine
contractions . caused by uterine squeeze ( reassuring “normal’’)
1. FHR slows as the contraction begins
2. Lowest point nadir
coincides with the highest point ACME of the contraction
( FHR should return to normal at this time)
3. Deceleration ends with the contraction
( gradually over 30 seconds or more)
Late deceleration: occurs after the peak of contraction (ACME)
due to
uteroplacental insufficiency, pitocin, HTN, diabetes, placental abruption.
- Too many decelerations will indicate a need for C-section
- Prepare for fetal resuscitation
Variable decelerations: may indicate cord compression. Occur at different times during a
contraction, resulting in fetal HTN that causes the aortic arch to slow the FHR. usually abrupt
and sudden.
Measures to clarify NON reassuirng FHR patterns
- Fetal stimulation
- Fetal scalp sampling
- Fetal scalp oxemetry
Das könnte Ihnen auch gefallen
- Fetal Heart TonesDokument1 SeiteFetal Heart TonesChristian Clyde N. JakosalemNoch keine Bewertungen
- Saint Gabriel General Hospital: Root Cause Analysis IfudDokument14 SeitenSaint Gabriel General Hospital: Root Cause Analysis IfuddawitNoch keine Bewertungen
- Assessment of Fetal Well BeingDokument61 SeitenAssessment of Fetal Well Beingsana khan008Noch keine Bewertungen
- Fetal Assessment During LaborDokument3 SeitenFetal Assessment During LaborMariya ZafraniNoch keine Bewertungen
- Cardiotocometer: Baseline Fetal Heart RateDokument4 SeitenCardiotocometer: Baseline Fetal Heart RateAnonymous elSqPhzKNoch keine Bewertungen
- Fetal DistressDokument65 SeitenFetal DistressEdward OledanNoch keine Bewertungen
- How To Read A CTGDokument31 SeitenHow To Read A CTGAbdullah As'ad100% (1)
- Google - Fetal Surveillance During Labor - 天津醫院Dokument56 SeitenGoogle - Fetal Surveillance During Labor - 天津醫院OANoch keine Bewertungen
- Worksheet To Accompany FHR Review Video: Emerald Spangler May 6, 2021Dokument3 SeitenWorksheet To Accompany FHR Review Video: Emerald Spangler May 6, 2021Emerald SpanglerNoch keine Bewertungen
- Google - CTG-O-GDokument54 SeitenGoogle - CTG-O-GOANoch keine Bewertungen
- MCN ReviewerDokument4 SeitenMCN ReviewerMaria Arabella LanacaNoch keine Bewertungen
- Cardiotocography (CTG) Electronic Fetal MonitoringDokument54 SeitenCardiotocography (CTG) Electronic Fetal MonitoringnovrinarNoch keine Bewertungen
- Electronic Fetal MonitoringDokument4 SeitenElectronic Fetal MonitoringMauZungNoch keine Bewertungen
- Intrapartum Fetal AssessmentDokument80 SeitenIntrapartum Fetal Assessmentzgra666Noch keine Bewertungen
- Reduced Fetal MovementsDokument9 SeitenReduced Fetal MovementsLois KankowskiNoch keine Bewertungen
- Pregnancy Induced Hypertension PihDokument17 SeitenPregnancy Induced Hypertension PihRose DeymNoch keine Bewertungen
- Intrapartum AssessmentDokument84 SeitenIntrapartum AssessmentAnne Carlie Bucoy RoldanNoch keine Bewertungen
- CTG Interpretation CmeDokument32 SeitenCTG Interpretation CmeNurshawina KamaludinNoch keine Bewertungen
- CTG ReportingDokument89 SeitenCTG ReportingKevin Marcial AralarNoch keine Bewertungen
- Hypertensive Disorders in Pregnancy (Autosaved)Dokument38 SeitenHypertensive Disorders in Pregnancy (Autosaved)Alex WagnerNoch keine Bewertungen
- Abnormal Cardiotohography in NewbornDokument37 SeitenAbnormal Cardiotohography in NewbornAdityaRahaneNoch keine Bewertungen
- How To Read A CTGDokument11 SeitenHow To Read A CTGiwennieNoch keine Bewertungen
- Fetal Heart Rate MonitoringDokument13 SeitenFetal Heart Rate MonitoringNinaSimone17Noch keine Bewertungen
- Criteria of Normal Fetal Heart Rate (FHR)Dokument14 SeitenCriteria of Normal Fetal Heart Rate (FHR)عمر احمد شاكرNoch keine Bewertungen
- Fetal SurveillanceDokument5 SeitenFetal SurveillanceĶHwola ƏľsHokryNoch keine Bewertungen
- CTG Interpretation: Dr. Areen AlnasanDokument37 SeitenCTG Interpretation: Dr. Areen AlnasanMohammad AlrefaiNoch keine Bewertungen
- CTGDokument38 SeitenCTGfahmiNoch keine Bewertungen
- 5 ExamDokument3 Seiten5 Examjacynda linsanganNoch keine Bewertungen
- Obstetric HaemorrhageDokument34 SeitenObstetric HaemorrhageKosie Soyama NambaNoch keine Bewertungen
- Chapter 14Dokument5 SeitenChapter 14Kelly HeartsillNoch keine Bewertungen
- Partograph and CTG Intrapartum Fetal MonitoringDokument56 SeitenPartograph and CTG Intrapartum Fetal MonitoringPEÑAFLOR, Shealtiel Joy G.Noch keine Bewertungen
- 5 Pregnancy Induced HypertensionDokument24 Seiten5 Pregnancy Induced HypertensionHyacinth Mae Virtudazo RaganasNoch keine Bewertungen
- Intrapartum Fetal MonitoringDokument15 SeitenIntrapartum Fetal MonitoringAnuradha Maurya100% (1)
- EXTERNAL FETAL MONITORING (NON - INVASIVE) (Autosaved)Dokument54 SeitenEXTERNAL FETAL MONITORING (NON - INVASIVE) (Autosaved)Maria Pina Barbado PonceNoch keine Bewertungen
- Electronic Fetal Monitoring: D. Lata Sharma, MD, FRANZCOG Senior Lecturer, University of Queensland, AustraliaDokument70 SeitenElectronic Fetal Monitoring: D. Lata Sharma, MD, FRANZCOG Senior Lecturer, University of Queensland, AustraliaSiyamak SalehNoch keine Bewertungen
- Interpretation of Abnormal CTG Pattern - 2Dokument17 SeitenInterpretation of Abnormal CTG Pattern - 2Jaspreet Kaur100% (1)
- 2 Obg Seminar at NST J Inal (1) SSTDokument19 Seiten2 Obg Seminar at NST J Inal (1) SSTAmritaNoch keine Bewertungen
- Normal LaborDokument70 SeitenNormal LaborAmlodipine BesylateNoch keine Bewertungen
- Gestational Hypertension-MeDokument32 SeitenGestational Hypertension-Mekurt94764Noch keine Bewertungen
- Antepartum HemorrhageDokument22 SeitenAntepartum HemorrhageGetaneh LiknawNoch keine Bewertungen
- KTG MTGDokument29 SeitenKTG MTGArina fauziyantyNoch keine Bewertungen
- Antenatal Assessment of Fetal WellbeingDokument52 SeitenAntenatal Assessment of Fetal Wellbeing6ixSideCreate MNoch keine Bewertungen
- Ob EfmDokument42 SeitenOb Efmkhaderbasha2020Noch keine Bewertungen
- Azzam Management of PreeclampsiaDokument36 SeitenAzzam Management of PreeclampsiaHezal Zamzuri HudayaNoch keine Bewertungen
- NOTESsDokument5 SeitenNOTESsAhmed Mohammed omarNoch keine Bewertungen
- Bleeding During PregnancyDokument5 SeitenBleeding During PregnancyMaryela Maceda GalozoNoch keine Bewertungen
- PERI Facts Helpful NotesDokument2 SeitenPERI Facts Helpful NotesmunkeeluvdesignsNoch keine Bewertungen
- Intrapartum Fetal Monitoring EditedDokument51 SeitenIntrapartum Fetal Monitoring EditedObgyn DischargesNoch keine Bewertungen
- Lecture-35 Eectronic Fetal MonitoringDokument45 SeitenLecture-35 Eectronic Fetal MonitoringMadhu Sudhan PandeyaNoch keine Bewertungen
- 1 JUSH ObstetricsDokument147 Seiten1 JUSH ObstetricsDaniel Negeri100% (1)
- CTG Interpretation 1Dokument27 SeitenCTG Interpretation 1asri khazaliNoch keine Bewertungen
- Post-Term Labor - NCPDokument8 SeitenPost-Term Labor - NCPCameron De GuzmanNoch keine Bewertungen
- Abnormal Cardiotocography - "CTG"Dokument47 SeitenAbnormal Cardiotocography - "CTG"Ahmad Mustaqim SulaimanNoch keine Bewertungen
- FETAL HEART TRACES 2.0 - CorrDokument9 SeitenFETAL HEART TRACES 2.0 - CorrPatricia SmitNoch keine Bewertungen
- Intrapartum Fetal SurveillanceDokument59 SeitenIntrapartum Fetal SurveillanceGaylinel BongyadNoch keine Bewertungen
- Obstetrics Cases by Caroline de CostaDokument9 SeitenObstetrics Cases by Caroline de CostaJeffrey HingNoch keine Bewertungen
- Case Study 29-APHDokument31 SeitenCase Study 29-APHZarul Naim Mohd TamiziNoch keine Bewertungen
- Pre-eclampsia, (Pregnancy with Hypertension And Proteinuria) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandPre-eclampsia, (Pregnancy with Hypertension And Proteinuria) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Clinical Obstetrics/Gynecology Review 2023: For USMLE Step 2 CK and COMLEX-USA Level 2Von EverandClinical Obstetrics/Gynecology Review 2023: For USMLE Step 2 CK and COMLEX-USA Level 2Bewertung: 4 von 5 Sternen4/5 (1)
- 05 Developing Standards ofDokument8 Seiten05 Developing Standards ofSachin SinghNoch keine Bewertungen
- Assigmnt. On MRIDokument8 SeitenAssigmnt. On MRISachin SinghNoch keine Bewertungen
- Sample PBBSCDokument1 SeiteSample PBBSCSachin SinghNoch keine Bewertungen
- Comman Sign and SymptomsDokument3 SeitenComman Sign and SymptomsSachin SinghNoch keine Bewertungen
- Dites Nursing Wifi3Dokument4 SeitenDites Nursing Wifi3Sachin SinghNoch keine Bewertungen
- 14 Reports and Duty RoasterDokument17 Seiten14 Reports and Duty RoasterSachin Singh100% (1)
- Assigmnt. On DefribillaterDokument9 SeitenAssigmnt. On DefribillaterSachin SinghNoch keine Bewertungen
- Models of CollaborationDokument1 SeiteModels of CollaborationSachin SinghNoch keine Bewertungen
- Assigmnt. On Cardiac RehabilitationDokument15 SeitenAssigmnt. On Cardiac RehabilitationSachin Singh100% (1)
- Planning Purpose: Experimental GroupDokument1 SeitePlanning Purpose: Experimental GroupSachin SinghNoch keine Bewertungen
- Models of CollaborationDokument1 SeiteModels of CollaborationSachin SinghNoch keine Bewertungen
- DialysisDokument19 SeitenDialysisSachin Singh100% (2)
- Bones PDFDokument9 SeitenBones PDFSachin SinghNoch keine Bewertungen
- 123 PDFDokument14 Seiten123 PDFSachin SinghNoch keine Bewertungen
- Panna Dhai Maa Subharti Nursing College Anecdotal Recording FormDokument1 SeitePanna Dhai Maa Subharti Nursing College Anecdotal Recording FormSachin SinghNoch keine Bewertungen
- Burn Injury: Burn Injury Is The Result of Heat Transfer From One Site To AnotherDokument10 SeitenBurn Injury: Burn Injury Is The Result of Heat Transfer From One Site To AnotherSachin SinghNoch keine Bewertungen
- Tracheotomy CareDokument20 SeitenTracheotomy CareSachin SinghNoch keine Bewertungen
- Models of CollaborationDokument1 SeiteModels of CollaborationSachin SinghNoch keine Bewertungen
- Chatarpati Shivaji Subharti Hospital Anecdotal Recording FormDokument1 SeiteChatarpati Shivaji Subharti Hospital Anecdotal Recording FormSachin SinghNoch keine Bewertungen
- Av AidsDokument19 SeitenAv AidsSachin SinghNoch keine Bewertungen
- Anemia Nursing Care Management - A Study GuideDokument8 SeitenAnemia Nursing Care Management - A Study GuideSachin Singh100% (1)
- Av AidsDokument19 SeitenAv AidsSachin SinghNoch keine Bewertungen
- Check List For Cardiopulmonary Resuscitation: Skill The Participant Yes NoDokument1 SeiteCheck List For Cardiopulmonary Resuscitation: Skill The Participant Yes NoSachin SinghNoch keine Bewertungen
- Angina Pectoris (Stable Angina) Nursing Care Management - Study GuideDokument8 SeitenAngina Pectoris (Stable Angina) Nursing Care Management - Study GuideSachin Singh100% (1)
- Acute Respiratory Distress Syndrome Nursing Management and Interventions - NurseslabsDokument2 SeitenAcute Respiratory Distress Syndrome Nursing Management and Interventions - NurseslabsSachin SinghNoch keine Bewertungen
- Unit Plan: TOPIC: Care in Hospital Setting. SUBJECT: Medical-Surgical Nursing Class: MSC (N) 1 ObjectivesDokument2 SeitenUnit Plan: TOPIC: Care in Hospital Setting. SUBJECT: Medical-Surgical Nursing Class: MSC (N) 1 ObjectivesSachin SinghNoch keine Bewertungen
- Chatarpati Shivaji Subharti Hospital Anecdotal Recording FormDokument1 SeiteChatarpati Shivaji Subharti Hospital Anecdotal Recording FormSachin SinghNoch keine Bewertungen
- Panna Dhai Maa Subharti Nursing College Anecdotal Recording FormDokument1 SeitePanna Dhai Maa Subharti Nursing College Anecdotal Recording FormSachin SinghNoch keine Bewertungen
- MCQsDokument4 SeitenMCQsSachin Singh100% (2)
- Specific Objective of MsDokument1 SeiteSpecific Objective of MsSachin SinghNoch keine Bewertungen
- Electronic Devices and Electronic Circuits: QuestionsDokument51 SeitenElectronic Devices and Electronic Circuits: QuestionsRohit SahuNoch keine Bewertungen
- ENG101 Final Term NOTES by VU LearningDokument15 SeitenENG101 Final Term NOTES by VU LearningAbdul WahabNoch keine Bewertungen
- Reading Listening 2Dokument5 SeitenReading Listening 2Lisbet GomezNoch keine Bewertungen
- Case Study On TQMDokument20 SeitenCase Study On TQMshinyshani850% (1)
- Math 10 Module - Q2, WK 8Dokument5 SeitenMath 10 Module - Q2, WK 8Reygie FabrigaNoch keine Bewertungen
- Baccarat StrategyDokument7 SeitenBaccarat StrategyRenz Mervin Rivera100% (3)
- Presentation (AJ)Dokument28 SeitenPresentation (AJ)ronaldNoch keine Bewertungen
- Customer AnalysisDokument6 SeitenCustomer AnalysisLina LambotNoch keine Bewertungen
- LITERATURE MATRIX PLAN LastimosaDokument2 SeitenLITERATURE MATRIX PLAN LastimosaJoebelle LastimosaNoch keine Bewertungen
- 211 N. Bacalso Avenue, Cebu City: Competencies in Elderly CareDokument2 Seiten211 N. Bacalso Avenue, Cebu City: Competencies in Elderly CareScsit College of NursingNoch keine Bewertungen
- A Management and Leadership TheoriesDokument43 SeitenA Management and Leadership TheoriesKrezielDulosEscobarNoch keine Bewertungen
- Skin DseDokument9 SeitenSkin DsePapitas FritasNoch keine Bewertungen
- Introduction To Computational Fluid DynamicsDokument3 SeitenIntroduction To Computational Fluid DynamicsJonyzhitop TenorioNoch keine Bewertungen
- Types of CostsDokument9 SeitenTypes of CostsPrathna AminNoch keine Bewertungen
- Endogenic Processes (Erosion and Deposition) : Group 3Dokument12 SeitenEndogenic Processes (Erosion and Deposition) : Group 3Ralph Lawrence C. PagaranNoch keine Bewertungen
- Verbal Reasoning TestDokument3 SeitenVerbal Reasoning TesttagawoNoch keine Bewertungen
- MU151 Group Assignment 6Dokument3 SeitenMU151 Group Assignment 6Jay CadienteNoch keine Bewertungen
- Chapter 3 SIP MethodologyDokument43 SeitenChapter 3 SIP MethodologyMáxyne NalúalNoch keine Bewertungen
- MC2 Sewing Patterns: Dressmaking Learning ModuleDokument91 SeitenMC2 Sewing Patterns: Dressmaking Learning ModuleMargie JariñoNoch keine Bewertungen
- FORTRESS EUROPE by Ryan BartekDokument358 SeitenFORTRESS EUROPE by Ryan BartekRyan Bartek100% (1)
- Adventures in Parenting RevDokument67 SeitenAdventures in Parenting Revmakj_828049Noch keine Bewertungen
- Native Americans - Clothing & Head DressesDokument28 SeitenNative Americans - Clothing & Head DressesThe 18th Century Material Culture Resource Center100% (15)
- Darshan Institute of Engineering & Technology Unit: 7Dokument9 SeitenDarshan Institute of Engineering & Technology Unit: 7AarshenaNoch keine Bewertungen
- English 7 Compare Contrast The People Could Fly Harriet TubmanDokument3 SeitenEnglish 7 Compare Contrast The People Could Fly Harriet Tubmanapi-508729334Noch keine Bewertungen
- CardiologyDokument83 SeitenCardiologyAshutosh SinghNoch keine Bewertungen
- PDF Document 2Dokument12 SeitenPDF Document 2Nhey VergaraNoch keine Bewertungen
- Activity 2Dokument2 SeitenActivity 2cesar jimenezNoch keine Bewertungen
- Massage Format..Dokument2 SeitenMassage Format..Anahita Malhan100% (2)
- Lesson Plan in Science III ObservationDokument2 SeitenLesson Plan in Science III ObservationTrishaAnnSantiagoFidelNoch keine Bewertungen
- CB Insights Venture Report 2021Dokument273 SeitenCB Insights Venture Report 2021vulture212Noch keine Bewertungen