Beruflich Dokumente
Kultur Dokumente
Asdasd
Hochgeladen von
John Paulo RamosOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Asdasd
Hochgeladen von
John Paulo RamosCopyright:
Verfügbare Formate
Lower Respiratory Tract Infections
Dr. Ong
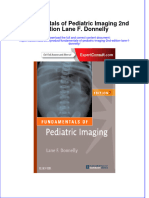
LUNG PHYSIOLOGY AND COUGH
AIRWAY OF ADULT VS PEDIATRICS COUGH RECEPTORS
Narrowest portion of airways Those pink spots would represent the cough receptors, and in
Adult – vocal cords the diagram where do we find it in majority? LARGE AIRWAYS
Pediatrics – Cricoid cartilage from the trachea down to the major bronchi. Notice that the
Airway diameter: pediatric < adult region of the middle ear we have cough receptors, so if we
Significance: Pediatric px will suffer more than adult if there clean our ears getting deeper will stimulate it. The lung
is insult in the airway. parenchyma per se has little cough receptors and most of them
Hypoxemia develops due to increase resistance of the are found in the airways
narrow airways
majority found in the upper or large airways (e.g.
ANATOMY trachea, bronchi)
-Also present in the middle ear, found in the airways but
NOT in the lung parenchyma
Physiology: anatomic, physiologic and immunologic defenses
The body has many anatomic defenses in respiratory tract,
starting with the nose, hair and the terminal bronchioles has
defenses exemplified by the presence of ciliated epithelium
lining the respiratory system
Physiologic defenses of the body:
Cough and sneeze reflex; inhaling an irritant triggers them both,
they serve as important defenses in the body and not meant to
be suppressed.
Immunologic diseases:
Major immunoglobulin in the respiratory tract? IgA
ACUTE VS CHRONIC COUGH
Acute Cough Chronic cough
common feature of LRTI 30 days
diseases e.g. TB, asthma
< 30 days duration
Schematic diagram of the respiratory tract, remember in
anatomy the respiratory tract would start from the nose down to
For every disease, know the:
your terminal bronchioles in the lungs, theoretically you can
most common pathogen
divide the respiratory tract in 2: Upper and Lower respiratory
Age
tract
Clinical manifestations
Diagnostic procedure
Respiratory tract: nose to alveoli
Drug of choice
1st line defense:
There are many diseases in the respiratory system and all of these
vibrissae, ciliated lining epithelium, physiologic
will have one common manifestation which is COUGH. Our task
mechanisms (coughing, sneezing), immunologic
is to find out if a patient is presented with cough, so what are the
mechanisms
underlying cause of the cough? So every disease discussed
throughout the topic we must know the pathogen and the drug
Larynx
of choice to be given. Always consider the age of the patient,
boundary between upper and lower airways
which the specific pathogen would be evident to a patient
consists of 9 cartilages (3 paired and 3 unpaired)
depending on the certain age given the features, even the
Vocal cords, thyroid c, cricoid c, arytenoids, cuneiform, diagnosis would be different if the age of the patient is
corniculate changed.
What are the salient features in combination with cough that we
LOWER RESPIRATORY TRACT
are dealing with the disease? So as we go along we are going
- consists of everything inside the thoracic cavity to identify those salient clinical features of the different diseases.
Then decide if we need laboratory findings, but some diseases
The boundary of the respiratory tract is the larynx, so anything don’t require these procedures and the diagnosis can be
ABOVE the larynx is the UPPER respiratory tract and everything explained by simple history and physical exam.
below is the LOWER respiratory tract
In some literature, respiratory system is divided differently, airways ADVENTITIOUS BREATH SOUNDS
or lung parenchyma; thus from the nose to the terminal
Adventitious Lung Duration Pitch TIming
bronchiole are part of the airways and we have the 2 lungs.
Sounds Sounds
Everything inside is INSIDE the thoracic cavity is THE LOWER
Wheezing Continuous High Inspiratory
RESPIRATORY TRACT and everything outside it is the UPPER
Expiratory
RESPIRATORY TRACT
Rhonchi Continuous Low Inspiratory
Expiratory
Stridor Continuous High Inspiratory
Crackles Discontinuous Inspiratory
the sound is heard during INSPIRATION it is EXTRATHORACIC,
in contrast if EXPIRATION then it is INTRATHORACIC
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 1
Management
PROVEN TO BE EFFECTIVE: In majority of the drugs they relieve the cough but the problem is
Oxygen they do not treat the underlying cause. What is important as
Among all the diseases we are going to talk about, if they have clinicians is to know what causes the cough and manage the
respiratory distress as a salient manifestation, it is understood that underlying problem rather than treating the symptomatic cough
we must give oxygen to the patient. DOB = GIVE OXYGEN per se.
If the patient has difficulty of breathing what happens to the Neozep (phenylephrine + antihistamine)
intake of food, Affected? Yes, so chances are if the patient has antihistamine is only good for cough with allergic etiology
a pulmonary problem in the days preceding the onset of (like asthma) but if it is non-allergic, it will increase the
respiratory distress, this patient may have not been eating well. viscosity of the cough and make it harder to expectorate.
Fever relief: acetaminophen, paracetamol.
Fluids Component of Neozep (Phenylephrine), generally all
but sole water therapy has really not been proven to make decongestants in the market contains phenylephrine; it was
secretions less viscous used to be phenylpropanolamine but it was banded by the US
Misconceptions: If cough, is it not indicated to drink fluids? FDA because of the alleged side –effects seen in adult women
Drinking fluids would not benefit it, but won’t do harm either. taking it as a reducing drug in high doses, side effects noted was
Drinking cold water wont exacerbate the cough nor eating bleeding. But in the usual dose of the decongestant it is rare to
sweets, the problem reflects on what are you drinking or eating. get the side effects. So if a patient asks you a drug for cold, it is
It could be a cause of allergy, recommended to give a drug with a single component with 1
If febrile, the have increased INSENSIBLE water loss. If active drug preparation (over drug combinations)
tachypneic, there will be further increase in SENSIBLE water loss.
So all of these combined together would put the patient at risk If there (+) secretions in colds do we need to give a
of dehydration due to the pulmonary problem it is understood to decongestant? No, but anti – histamine will make the secretions
give fluids either oral or intravenous. If the present with fever then more viscid to lessen it. It contains anti – histamine, noting for its
give paracetamol. side –effects especially 1st generation includes CNS depression
an drowsiness.
COUGH/COLDS MEDICATIONS
RULE OF THUMB: Better to give a drug that only has one 2nd generation: Loratadine and Citirizine, with lesser side – effects.
action. Do not give combination drugs. So whatever benefit the drug has given to the patient for
In the Philippines, patients don’t want to leave the clinic without instance is neozep, the beneficial effect is not secondary to the
a prescription. So it’s important for us to know the cough and anti – histamine properties but to its anti – cholinergic capabilities
cold medicines in the market. Why won’t be discussed in the but not present in NEWER anti – histamines.
topic? Because if you browse the nelson’s book, you’ve noticed
that the cough and cold medicines are not written because If you’re going a drug to treat the cold, your decongestant will
studies show that they do not work particularly the cough try to loosen your secretions, in contrast to anti – histamine will
medicine. But in the Philippines we have to know them. make the secretions more viscid thus opposing each other. So
it’s not therapeutic however people will always ask for advice for
Mucolytics (e.g. Carbocysteine Solmux) cough and colds and give them sound advices.
breaks down the disulfide bonds in the secretions to make
them less viscid and easier to expectorate; however, no STANDARD HOME MEDICATIONS:
clear cut benefit in children Vitamin C
Most important cough medication in the market? Tuseran which shortens the duration of cough and colds but not proven
is the top selling even alone could save the market of the to prevent it
company. Tuseran contains mucolytic which liquefies the Vitamin C: improve body’s defenses, according to belief for
phlegm and anti – histamine if given in a disease not caused by children, reduces the chances of coughs and colds (Ceelin). But
an allergy its effect will make the secretion less. studies have shown that vitamin C will not prevent us from not
If we give an anti-histamine caused by an allergy then the having frequent cough and colds and the proven benefit is to
patient’s condition will improve but if given to a manifestation shorten its duration and lessens severity of the colds.
caused by a viral infection it is going to make the secretions
more viscid (more thick), thus the effects of the drug are Steam inhalation
antagonizing each other. can cause burns especially among infants when not
done correctly; there are safer options!
Expectorants (e.g. Guaifenesin Robitussin) Steam inhalation
it is really not expected for children to be able to Prepare a basin with steaming water while covered in towel to
expectorate; however, justified use when enables child to trap the steam, the water inhaled should preferably be NSS or
sleep restfully at night water mixed with table salt. It works under the effect of the Salt
Expectorants (Guaiafenessin – formerly Glyceryl Guaiaculate) making the secretions less viscid but doesn’t work like that, the
Robitussin, Ventolin process is that the salt serves as an irritant, therefore when we
– it is expected to promote expectoration so the patients would inhale it would stimulate sneezing and coughing that would
be able to cough out phlegm. facilitate evacuation of the phlegm and the nasal secretions for
relief of breathing.
Anti-tussives (e.g Dextromethorphan)
not used in children because cough is a physiologic Lozenges
defense mech and you do not want to suppress Strepsils, decuadin, Fisherman’s friend
Antitussives (dextromethorphan) taken primarily for the sore throat but not for the cough
Anti cough – prevent coughing (remember that cough is a
physiologic mechanism, and not supposed to suppress it) but Saline gargle
there are exemptions in such that the patient can’t sleep well at Primarily for the sore throat.
night due to persistent coughing then the antitussive is indicated. Commercial preparations are available such as bactidol,
Another example when a child during coughing aggravates astring – o – sol, ora care.
abdominal pain when present.
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 2
Oil based (in provinces) Misconceptions:
Oil – based preparations in steaming water (may cause If cough, is it not indicated to drink fluids?
Lipoid pneumonia). It causes oil deposits in the lung - Drinking fluids would not benefit it, but won’t do harm either.
parenchyma. Drinking cold water wont exacerbate the cough nor eating
The needed treatment for these is lung transplant so oil – sweets, the problem reflects on what are you drinking or eating.
based is not recommended for a child with a pulmonary It could be a cause of allergy,
problem.
Taking a bath with cough? Yes
Vicks Vaporub - It can be helpful especially with fever (cold shower or tap
oil based and not good for internal application water). Indicated to those also with pneumonia unless not
covers skin pores -> traps heat -> vasodilation ambulatory (do TSB or tepid sponge bath)
Vicks Inhaler: should be used correctly, do not insert inside
the nostrils. Could rain cause colds? No
Vicks vaporub - During rainy seasons, viral infections are common and it is
- For external use only, causes vasodilation for ease of breathing everywhere so it is easily acquired.
ACUTE INFLAMMATORY UPPER AIRWAYS OBSTRUCTION (CROUP SYNDROMES)
characterized by bark-like or brassy cough with stridor (hoarse high pitched inspiratory sound)
EPIGLOTTITIS (SUPRAGLOTTITIS)
Medical emergencies especially in children because of a drooling of saliva. When these problems are present along with
common clinical feature which is STRIDOR. stridor, this will be clue that the patient has epiglottitis. So most
exam questions will give these clinical manifestations
If you ask the patient to open his/ her mouth this is what would
you expect to see, (UVULA, PHARYNGEAL TONSILS) the epiglottis Tripod Position
is not ROUTINELY seen but using a tongue depressor may make it shoulders up,
grossly appear as a flop that is covering your glottic opening leaning forward,
preventing food from entering the airway as we eat. arms used for support,
Located anteriorly, the trachea and posteriorly the esophagus. chin up
ARYTENOIDS -- position assumed to attempt to
TRUE VOCAL CORDS AND FALSE VOCAL CORDS breathe
covered by the epiglottis. The epiglottis could be inflamed
known to be as epiglottitis. Since it is located above the
glottic opening it is termed to as supraglotitis.
Because of respiratory distress, the patient will do certain
CAUSATIVE AGENT maneuvers in order to improve oxygenation, by extending the
H. influenzae (type B), S. pyogenes, S. pneumoniae, S. neck making the airway patent. Another maneuver is the TRIPOD
aureus position, will sit hunched forward with both arms touching the
When you hear the diagnosis of epiglottitis the first organism you knee with a hyperextended neck, usually observed in patients
should consider is H. influenza particularly type B. In the US and with epiglottitis.
other western countries where the vaccines are given for free. Philippine data shows low incidence, probably not recognized
They have very good coverage for Hib vaccine so that the but why do we have to study it? Because its often asked in major
incidence of the diseases cause by H. influenza has markedly examinations and also to prepare us in global competence and
decreased. In the Philippines, some Health centers have Hib diseases that are seen not only in the Philippines but around the
vaccine but cannot sustain it due to the lack of government world.
funds.
DIAGNOSIS
ONSET 1. Clinical with high index of
2-4 y/o (does not preclude adulthood) suspicion
In children 2 – 4 years of age however in literatures would tell 2. Direct Laryngoscopy: insert into
you that the diseases are discovered as young as 1 year old oral cavity to visualize glottis
and as old as 7 years of age markedly inflamed (large, cherry
Features that tells you that this is epiglottitis: Acute onset of fever red, swollen)
that is high, severe throat pain. Because of epiglottis being do with caution because it
swollen being at the top of the glottic opening, then the patient might trigger gag reflex and
would manifest difficulty of breathing due to obstruction of the cause arrest
airway. These in turn would cause air hunger, restlessness, very 3. Lateral Xray of the Neck - THUMB
toxic – looking patient sign
CLINICAL FEATURES How to establish diagnosis:
- History is suggestive, suddenly a patient complained with high
Acute onset: sudden high grade fever, sore throat
fever with pain while swallowing, and if you asked the patient to
Rapidly progresses to air hunger, restlessness, and toxic
open his mouth you would observe the large cherry – red swollen
appearance
epiglottis. This would caution us that this may be epiglottitis but in
Hyperextended neck – attempting to breathe
order to confirm the diagnosis we should do x – ray and note for
Stridor – signals narrowing of airways
the tram sign. Thumb sign
4Ds: Dysphonia, Dyspnea, Dysphagia, Drooling
In x – ray the air is black (lucent) and solid and liquid would
o Considered as EMERGENCY situation
appear as white (opacities) in the x – ray. This is the cervical
When take examinations, patient presenting with stridor and
spine, oral cavity, column of air (pharynx) down to the trachea
explained the 4 clinical manifestations (dyspnea, dysphonia
but appear as narrowing (the lucency off the trachea is getting
(pain while speaking), respiratory distress, dysphagia and
thinner as it goes down) indicating that air flow to the lungs is
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 3
limited because of the swollen epiglottis, if you can see it looks MANAGEMENT
like a thumb (“thumb sign”) so it will give us a hint that it is 1. Medical emergency -> Secure airways - intubation,
epiglottitis and no other disease would give us that impression tracheostomy (puncture cricothyroid membrane)
and its treated as an emergency. 2. Antibiotics
Remember that the priority is to secure the airway or intubate if Ampicillin or Chloramphenicol - DOC for H. influenza
need. Word of caution if the patient is suffering from upper Ceftriaxone - for strains resistant to ampicillin (7 - 9 days)
airway obstruction with stridor (parang umeere ang ingay) that Accdg to Nelson: also Cefotaxime and
the sound appears frightening for the parents considering upper Meropenem
airway obstruction. Rifampicin prophylaxis for other members of household:
Please be advised not to poke the tongue when assessing the once daily for 4 days
mouth using a tongue depressor unless in a facility which CPR The most common cause of epiglottitis is H. influenza so the drug
can be performed. The usual response when being assessed with of choice is ampicillin or chloramphenicol. When you read
a tongue depressor that patient may experience gag and nelson you can also give ceftriaxone and so forth, due to high
stimulation of the vasovagal reflex that may cause reflex resistance to ampicillin but locally still works. For instance all
bradycardia and eventual respiratory arrest. So do not attempt patients who died in Quezon City used Ampicillin as medication,
to look on the throat of the patient without oxygen. henceforth you wouldn’t use it in the first place rather use a
stronger antibiotic. Using a stronger antibiotic won’t make you a
better physician so it’s important why it is necessary to tell the
patient which medication is indicated to be or not to be given.
Epiglotitis is a very virulent and infectious disease, so anyone who
had contact with the child should receive prophylaxis of
rifampicin that is given for 4 weeks.
CROUP (ACUTE LARYNGOTRACHEOBRONCHITIS) - most common
CAUSATIVE AGENT Strictly speaking, this can be establish by history taking and
Parainfluenza, influenza, adenovirus, RSV, measles physical exam. Clinical features are very distinct such as cough,
cold and fever and sudden barking of cough and with stridor will
ONSET serve as a giveaway for diagnosis. In the event that you are not
Older infants and toddlers (< 5 y/o) sure, you can always request an x – ray of the neck.
Most common among diseases causing upper airway Frontal view of the neck; so if you look on the spine, you can see
obstruction is croup or acute laryngotracheobronchitis. The lucency. Spine, vertebral column, with a line of lucency in the
larynx, trachea and bronchi is involved. Caused by usually the middle (represents air in the Trachea). Trace the trachea up,
viruses. Seen in children as early as 3 mos up to 5 yrs of age, most there is a sudden narrowing (Stipple sign; Pencil sign) looks likes a
of the cases in clinical practice that it is seen in children at 2 point of the pencil
years of age. It is very common during the rainy season.
MANAGEMENT
CLINICAL FEATURES NO DOC!
1-3 days: common cough and colds Secure airways
Sneezing, rhinitis, rhinorrhea Racemic Epinephrine - better because hydrophilic
low grade fever - However, this is not available in the Phils. Only the
Barking cough (after 1-2 days) dextrorotatory form in NSS is available, one dose only
Management involves securing the airways, racemic epinephrine,
Hoarseness
and supportive management.
Stridor
Isomers, are mirror image of each other. Can be dextro (Hydrophilic)
Worse sx at night or levo (Hydrophobic). Therefore if a substance is hydrophilic it will
Resolves in a week (viral infxn, so no DOC) dissolve in water, otherwise if hydrophobic it won’t dissolve in water.
Appear as an upper respiratory tract infection, cough, cold and Locally available epinephrine is hydrophobic, so there is no available
fever, sudden barking type of cough, that is very dry and harsh and epinephrine in the Philippines, nearest is in Singapore. The racemic
more painful compared to productive. It is distinguished from epinephrine is effective in just 1 dose as if nothing happened to the
productive aside the fact that children aren’t able to cough phlegm patient and the response is very dramatic so the patient is sent home
properly, so we can tell the differences by the sound it produces. afterwards. However if there are no improvements don’t give a
Children could also either expectorate, vomit or swallow their second dose of it anymore since it won’t work anymore. In
phlegm and goes out with the stool so it’s not unusual for patients socioeconomic concerns, we prefer using epinephrine but not
with pulmonary problems to develop soft stools, so it’s not necessary everyone is recommended to have it because it’s not part of
to scold children who aren’t able to expectorate the phlegm. standard management.
Hoarseness of the voice is clue that there is a problem in the larynx Standard management
and presents as stridor. Symptoms are worse at night. – if this is the diagnosis, these should be the step – wise procedure to
be done to the patient. If the procedure was not followed correctly
DIAGNOSIS and something happened you may be liable for that action.
Clinical
Neck X- ray (frontal Steroids
view): - Dexamethasone - tablets or parenteral (IM); give
Steeple/Pencil sign then observe for 4-6 hours
- Budesonide – inhalational, one dose
Improvement after 1 week
Other options are available such as steroids, Dexamethasone IV,
Budesonide (Inhalation), there are many showing good response to
drugs because they are available locally. So in the US if diagnose
with croup you won’t be admitted automatically, the patient will be
given a dose of Dexamethasone and observe in ER for 4 to 6 hours. In
How to establish the the Philippines we cannot do that because of the number of patients
occupying the ER which is overcrowding.
diagnosis
Mild cases may not be admitted, it is self – limiting and usually after a
week the patient is okay.
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 4
SPASMODIC CROUP
CAUSATIVE AGENT Another variant: spasmodic croup; the features are similar to
Viral (Parainfluenza); Allergy; Psychological croup but no fever. Has cough, colds, fever in the beginning and
eventually cough becomes hacking or barking. History findings
CLINICAL FEATURES reveal that the child is okay in the morning but once asleep
Presents similar to croup of LTB he/she will walk up due to stridor. In the provinces the most
- barking cough, dyspnea, noisy breathing common mode of transportation used is motorcycles, so usually
How to differentiate: No viral prodome (cough and colds) during the evening the air is cold, so during the travel time the air
or fever flows to the child which is therapeutic for the child so if they
Usually occurs at night arrive to the hospital they would appear okay and set home. So
- How to diff: no symptoms prior to sleeping, unlike history findings could be a giveaway sign that it is spasmodic
in croup croup.
MANAGEMENT
Most cases improve in a few hours
- sometimes on the way to the hospital px improves
d/t exposure to the cold night air
- improvement depends on how soon humidified
air is introduced
BACTERIAL TRACHEITIS
DESCRIPTION Usually it is being though as possible complication of respiratory
Does not involve epiglottitis, but like the others is capable of tract infection. In general, a viral infection would predispose
causing life-threatening airway obstruction secondary to a bacterial infection because cilia is being
Often follows viral RTI denuded caused by viral organisms, when its denuded the
respiratory epithelium is exposed so if the cilia is not there it is
CAUSATIVE AGENT easy for the organism to infect the epithelium.
S. aureus, M. catarrhalis, H. influenzae, anaerobes Distinguishing features of bacterial tracheitis is not that toxic but
there is stridor, no drooling or difficulty in swallowing and the
ONSET usual characteristic is that the patient has a lot of copious
purulent secretions that is yellowish to greenish that will tell us its
5-7 y/o
bacterial (epiglottitis, croup, spasmodic group has less secretions
and will serve as a distinguishing problem of the disease). The
CLINICAL FEATURES
diagnosis is based on clinical, the symptomatology of the
Brassy cough, high fever, stridor disease and the presence of the purulent secretions. Laboratory
With copious, thick, mucopurulent secretions exam is not necessary if clinical impression is bacterial tracheitis.
How to differentiate from other diseases - can lie flat on If we are dealing with staph and increasing incidence of MRSA
bed, NO drooling, NO dysphagia = NOT TOXIC LOOKING so we are considering giving the right antibiotic and if started will
improve 2 – 3 weeks in time. They will manifest difficulty in
DIAGNOSIS breathing. It is a very benign disease, inflammation of the larynx.
based on evidence of bacterial infection (e.g. high grade It is viral in origin and since the larynx is involve it will show voice
fever and purulent phlegm) changes so hoarseness of the voice is present. So if there is
X-ray is unnecessary laryngeal involvement there is voice changes. They don’t usually
manifest difficulty breathing unless we are dealing with very
MANAGEMENT young patients. Since it’s benign, it won’t be a reason to absent
Vancomycin or βlr antibiotics (Cefotaxime, Cefuroxime, from school, work and be excused unless if you’re an
Oxacillin) --- Impt: know your local resistance patterns! announcer. Management is supportive symptomatic, includes
Clinical improvement in 2-3 d gargle, antiseptics, lozenges use in laryngitis.
ACUTE LARYNGITIS
DESCRIPTION Toxic looking that will manifest with DOB. This is an exception. It is
Inflamed larynx -> narrowed lumen -> ↑airway resistance a benign disease – inflammation of the larynx. Viral in origin. If
Main fnc of larynx: Voice box/ Phonation, passage of air the larynx is involved, there will be voice changes – hoarseness of
MoT: Droplet Nuclei voice.
Benign! ---does not cause difficulty of breathing If there is no hoarseness of voice, the larynx is not involved
(Other benign condition: bronchitis) Laryngeal involvement – voice changes; very young patients
presents with difficulty of breathing
CAUSATIVE AGENT It is a benign condition – cannot be used as an excuse sa work
Parainfluenza viruses unless ikaw ay singer. Lol
DIAGNOSIS
ONSET Clinical – Hx and PE
- important to recognize recurrent laryngeal
2-4 y/o infections -> predisposed to develop Rheumatic
Heart Disease
CLINICAL FEATURES Labs not necessary
URTI: Sore throat
(+/-) fever MANAGEMENT
cough DoC: None, it will resolve spontaneously.
(+/-) colds Symptomatic and Supportive Treatment: Lozenges, ginger
hoarse voice (Differentiates it from tonsillitis and pharyngitis Management: supportive, symptomatic
= no hoarseness)
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 5
DIPHTHERIC LARYNGITIS – very infectious
DESCRIPTION DIAGNOSIS
Confirmed by smear (swab pharyngeal area)
extension of the infection to the larynx isolate the organism – swab in pharyngeal study
CAUSATIVE AGENT MANAGEMENT
Corynebacterium diphtheria (incubation period of 2-5 days) Isolate the patient
DOC: (always administer TOGETHER!)
CLINICAL FEATURES - diphtheria antitoxin
fever, sore throat, fetor oris (bad breath) distinguishing - penicillin G or erythromycin -> to neutralize the bound
feature toxins
bull neck appearance
greyish white membrane/plaque on the tonsils In the Philippines we see patients with diphtheria but scarce, it is
common mistake is that they remove it, that results to a communicable disease and most hospitals won’t allow
bleeding admission of these kind of problems even in the private rooms
hoarseness, stridor San lazaro – pavilion with diphtheria
Very communicable diseas; not all hospitals are allow
to admit pts with diphtheria
RETROPHARYNGEAL ABSCESS
DESCRIPTION Hx of prior ENT infection – clue when dealing with retro
infection of deep neck tissue between the pharynx and pharyngeal abscess
cervical spine (posterior to esophageal wall) o Sore throat, took meds, felt a little better, subside
ang symptoms for 1 week, however after few days
ETIOLOGY nag recur ang fever and this time mas severe ang
prior infection in nasopharynx, paranasal sinuses, middle coughing
ear Features – fever - high grade, do not feed, dehydrated,
extension from oropharyngeal infection neck pain, stiffness of the neck (test for neck rigidity – up,
dental infection down; check for suffleness – left to right), muffled voice,
cervical osteomyelitis stridor, bulging of the retropharyngeal wall due to abscess –
cover the glotic opening and the esophagus
At the back of the pharynx Should be differentiated from epiglottitis and foreign body,
- The space that separates the esophagus from the trachea meningitis
- Rich in lymph nodes that is why many microorganism can
easily transfer DIAGNOSIS
o Eg. Dental carries – org can move from one area PE: bulge on pharyngeal wall
to another thru the lymph nodes – usually may - DO NOT use tongue depressor -> can trigger gag
come from tonsillitis, trauma, dental infection, reflex and cause arrest
infection from cervical spine Soft tissue neck films
- shows ↑depth of tissue bet. esophagus and trachea
ONSET - Not required if you can already dx by clinical
3-4 y/o (because nodes involute before 5 y/o) Lateral X-ray or Neck CT scan also possible
- Not seen in children >5y/o bec other lymphoid organs Dx – hx, PE, bulging of the pharyngeal wall, x ray of neck soft
stayed awork? Kaya hindi sila ganun kaimportante tissue (large space between the pharynx and the cervical spine
- <5y/o tonsils, lymph nodes are important due to abscess)
Neck CT scan
CAUSATIVE AGENT
Usually bacterial: group A Strep, Anaerobes S. aureus DIFFERENTIAL DIAGNOSIS
GAS - mc pathogen FBA Foreign Body Aspiration
Abscess – staph Epiglottitis (sore throat, narrowed airway space)
Meningitis (neck pain, stiffness, rigidity)
CLINICAL FEATURES --- If (+) hx of prior ENT infection, think of retropharyngeal
Fever – usu. high grade abscess!!!
Irritability
Dysphagia -> Dec food intake MANAGEMENT
Sore throat, neck pain, torticollis 3rd gen Cephalosporin + ampicillin-sulbactam or
Muffled voice clindamycin
Stridor Drainage ONLY IF: distressed, failure to improve with IV
Distress, cyanosis antibiotics, for culture study on specimen
Mgt – do not drain – can cause aspiration or ingestion – spread
the infection
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 6
FOREIGN BODY ASPIRATION
DESCRIPTION If the object is lucent, not very helpful.
aspiration of small objects (e.g. nuts, beads) CT scan: can be helpful to rule out Bronchoscopy: to investigate
may cause obstruction = MEDICAL EMERGENCY airways with a tube hooked to AV monitor
The child will not tell the parents because they are afraid that they
will be scolded. The only time that they will tell their parents is when
ETIOLOGY
they experience discomfort and difficulty of breathing secondary to
Organic objects (80%) – peanuts, seeds - more problematic the foreign body that is aspirated
if they dissolve -> pneumonitis Then request for an x-ray. Not all foreign bodies will be seen on the x-
Inorganic objects (20%) – earrings, whistle, beads ray. When the foreign body is radio lucent, you will not see it on the
Note if the aspirated object is organic(can cause more damage xray. E.g. X-ray that shows a coin – in frontal view, you cannet tell if it
– can cause tissue breakdown, oils will be released that can is in the esophagus or in the trachea, you need a lateral view xray.
cause pneumonia) or inorganic(earings, wistle) in the xray, you will see that the right lung is darker than the left lung.
MC foreign body - peanuts and cornicks (hinahagis tapos Therefore mas madami syang hangin. The foreign body is in the left
sasaluhin ng bibig) lung. All of the heart is in the left. The right lung is over inflated. This is
a case of a child who imitate the chippy commercial wherein they
will open it using their mouth. The small plastic particles can be
ONSET
aspirated and we will not see it on x ray. When it lodges to the main
Older infants and toddlers (< 5 y/o) stem bronchus, it will not totally obstruct because it is small but it can
Very common in toddlers or preschool <5 y/o affect the inflow. The left lung begins to collapse.
CAUSATIVE AGENT CT scan is performed kapag walang Makita sa X-ray
CLINICAL FEATURES
Highly suggestive: Cough and Wwheezing MANAGEMENT
<Right main bronchus – common location; because wider Bronchoscopy
and straighter than Left> 3 stages of symptoms: Antibiotics – not routine unless organic FB
1. Violent paroxysms of coughing, choking, gagging and Steroids – if long-standing and inflammation has set in
possible airway obstruction – easy to dx if seen Surgery – extreme cases, obj cannot be removed by scope
2. Asymptomatic interval – delayed dx Bronchoscopy is performed kapag walang Makita sa x-ray or CT
3. Complications – obstruction, erosion, or infection scan. You can use a rigid or flexible. Inserted to the moth or one
nostril until you see the foreign body and it is corrected to a polymer,
Fever, cough, hemoptysis, atelectasis
makikita mo ang loob.
Once the foreign body is big enough to cause obstruction –
If the foreign body has been there for a long time, it is difficult to do
EMERGENCY
_______ (di ko maintindihan) eg. The pt came from Palawan with a
Clinical feature –depending on size
history of asthma for 5 years and x-ray was not performed. When he
- Violent episodes of coughing, choking or gagging
came to manila we did an xray and it revealed that there is a screw
- The body becomes used to it – became asymptomatic – this is a
in the lung. The history revealed that the child is fond of
potential problem because the physician will not push thru in
disassembling his toys. And because the screw has been there for 5
removing the foreign body
years, nagkaron na ng granulation doon, and when we try to pull it
- Complication when not remove - recurrent pulmonary infection
with forcep, nagkakaroon ng bleeding. So we ended up by
operating the patient, and we open it up, the affected lung is
DIAGNOSIS already necrotic so we remove the entire lung
History Moral of the study, if in the vback of your mind foreign body is a
Chest X-ray: If the object is lucent, not very helpful. possibility, you should do all test to rule it out.
CT scan: can be helpful to rule out If the foreign body has been there for so long and you did a lot of
Bronchoscopy: to investigate airways with a tube hooked to manipulation, you can give the pt antibiotic and steroids. If you still
AV monitor cannot remove it, you must perform surgery.
BRONCHITIS
CAUSATIVE AGENT Bronchitis – auscultation - can be normal/clear. As much as possible
Viral: Parainfluenza and adenoviruses ayaw natin ng harsh breath sounds. Some pts. Will have RONCHI
(characteristic of bronchitis)
o Adenovirus – most common pathogen causing
Ronchi – produced due to the movement of secretions during
inflammation to the major bronchi
airflow.
Bacterial In infants (most common):
Crackles – secretions are in the alveolus, during insp, it will dislodge
o H. influenzae the secretions and it will produce a sound
o S. pneumoniae Wheezing – secretions are in the airway that will narrow down the
lumen of the airway
CLINICAL FEATURES
Starts with rhinitis (URTI sx) -> eventually cough (starts as dry - DIAGNOSIS
> eventually productive) Auscultation often NORMAL -> but may present with
Also vomiting - Young children do not know how to cough wheezing (d/t partial obstruction), crackles, and rhonchi
out phlegm, so they swallow it Normal chest X-ray - In some cases there will be increased
Chest pain, or even abdominal pain - Older children, 2° to bronchial markings (but this is not specific for bronchitis)
excessive coughing and cough receptors It is benign – no resp distress
stretched/stimulated
Presents with ordinary cough and colds, may or may not have fever, MANAGEMENT
vomit as the way to get rid of their phlegm. Older children will
complain of chest pain or abdominal pain secondary to excessive If Viral: Symptomatic and supportive tx, NO DOC, resolves
coughing but they will not have DOB. Sometimes the only spontaneously 2 – 3 wks
manifestation is cough. Bronchitis vs simple upper resp tract inf. If Bacterial: DOC for H. influenzae: ampicillin DOC for S.
Upper resp inf - aside from the cough, usually meron pang iba. Like pneumoniae: penicillin
colds and sore throat and fever Supportive/symptomatic – virus
Misconception that the cough will resolve in 1 week. It should be
lessen after 1 week.
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 7
BRONCHIOLITIS
CAUSATIVE AGENT Look at the arms if it is raised – this will cause false impression
RSV(most common pathogen), parainfluenza, that the clavicle is v shape
adenovirus, no evidence for bacterial cause - Compare the lungs, observe the lucency from apex to
RSV - Respiratory Syncitial Virus / Human Orthopneumovirus
base; on the sample x-ray film the base is more lucent than
ONSET the apices – basal air trapping.
Infancy: 1-2 y/o; peak: 6-12 mos - Normal diaphragm – perfect dome, if it is not, a sign of air
A disease of infancy
trapping . the lung is retaining more air so that it is pushing
CLINICAL FEATURES down the diaphragm
Mild URTI: colds, dec appetite, fever - widened intercostals spaces
TRIAD: tachypnea, chest retractions, wheezing (All 3 MUST Radio review:
be present) --- Supine film: if there is a a gap between diaphragm and
The lumen of bronchioles are smaller than the bronchi, gastric gas bubble
when the airways become inflamed, there will be a --- Upright, PA film: v-shaped clavicle
narrowing of lumen and it will produce a lot of secretions. So
the narrowed lumen will be filled with a lot of secretions. The MANAGEMENT
triad must be present in patient <2y/o. if the triad is present Treatment
in a 5y/o pt, you cannot dx him/her with bronchiolitis Upportive and symptomatic
Wheezing - should rule out asthma Mild cases are managed at home
What are the chances that an infant will develop asthma Mod to severe cases are hospitalized
1. Family hx of asthma Ribavirin – expensive & not routine part of mgmt
2. Get nasal secretion – nasal smear – eosinophil – NASAL Corticosteroids – to decrease inflammation
EOSINOPHILIA Bronchodilators - for wheezing (But remember pathology is
3. If responding to bronchodilator (nebulizer) not bronchoconstriction, so the result of this is not uniform
In some studies, a child who develop bronchiolitis, they will follow hence not part of routine management)
up after 3 years to see if how many of them develop asthma Antibiotics – no role since viral
and it shows that 40% of the cases developed asthma. One - Supportive. Mild cases can be treated at home, only those
differentiating point nila is parental smoking who are severe, who are dehydrated or those who refuse to
feed must be admitted to the hospital
DIAGNOSIS - Ribavirin – antiviral. Routine na naiibibigay sabi ni Nelson kasi
Clinically diagnosed - no laboratory exams daw libre. Whether you give it or not, there will be no
Chest Xray – for confirmation only difference
Since there is wheezing, the most important differential - Inflammation – steroids, however there are some patients
diagnosis would be ASTHMA (In asthma, there should be at that are ______liform, some patients will have relieve after
least 3 episodes of wheezing.) administration of steroisds, some patients are not
Chest radiography findings: Trapped air -> over-aerated - Bronchodilators – some patients improve, some are not.
1) Flattening, imperfect dome diaphragm Theoretically there is no bronchoconstriction. There is
2) Widened intercostal spaces nothing to dilate. But there are some cases that some
patients improved with nebulize bronchodilator
3) Some parts are hyperlucent, i.e, bases more
- Ribavirin, steroid, bronchodilator – not part of the standard
lucent than apices
of care. You may or may not give it to your pt. you can try
History and PE is enough to establish the diagnosis of or you can not at all
bronchiolitis. In the event that you are not sure of the diagnosis,
you can get an x-ray. Prevention
x-ray Alibizumab? – ab against the RSV protein – the problem is it
upright – air/gastric bubble (Magenblast) beneath the is expensive
left hemidiaphragm - the patient must receive it every 2 months or every 2 weeks
supine – no air bubble - 1 vial costs 75k
PA – v shape clavicle - Usually you do not use it because the disease is benign
AP - straight clavicle
PNEUMONIA
Diseases of the Respiratory System that you should master as a 4 stages of Pneumonia
general practitioner: 1. Congestion
1. Common colds 2. Red
2. Pneumonia 3. Gray
3. Asthma 4. Resolution
4. TB Not all pts with pneumonia will undergo the 4 stages
If you are on the stage of hepatization, the lung parenchyma is
DESCRIPTION now filled with secretions.
inflammation of the lung parenchyma, in some instances, Instead of air, secretions now occupy the alveoli.
the airway is also involved but you cannot have a case in Lungs become heavier, hard, assuming the consistency of a
which the lung parenchyma is not involved. Like any other liver.
pulmonary disease, you should know the different In essence that would correspond to CONSOLIDATION and NOT
pathogens depending on the age groups all pts with pneumonia would undergo consolidation.
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 8
CAUSATIVE AGENT
Neonate Most common pathogen is GBS Tx:
In the Philippines - E. coli and G (-) organism Ampicillin – to cover GBS
Aminoglycosides – E. coli (e.g Genta, Amikacin, Tobramycin)
Preschool 2 most common pathogen that would cause Note:
(2 to <5 yo) pneumonia in this age grp. Eg. Patient, 2 yo, has complete Hib vaccine, what organism to
1. H. influenza – suspect more if pt. is infant to 2yo consider?
2. Strep. pneumonia – more common if pt. is 2 to 5
yo Ans: Strep, even if 1 yo, as long as complete vaccination, NOT Hib.
Im not saying that it is impossible for you to have So, Strep pneumonia is the cause
pneumonia in a child who is 2-5 yo caused by H.
influenza. It is just more common in infant up to 2yo.
3. Staph aureus – 3rd organism to consider in this
age group but not as important as the 2
School Strep. pneumonia Walking Pneumonia
aged Grp Mycoplasma pneumoniae – aka ATYPICAL PNEUMONIA
(>6 yo) – child with full-blown Pneumonia, upon auscultation (+)
crackles, yet pt. seems to be comfortable, has no
difficulty of breathing and can still play
General Rule in pedia
– School age: Mycoplasma pneumonia think if pt. is 6 yo
and above
– INFANT: Chlamydia pneumonia think about this if <1 yo
UPDATE in JOURNAL
– Mycoplasma is not only confined to school-aged grp. It
was isolated even from infants
– Chlamydia also is now found even in older age groups
CLINICAL FEATURES
Clinical Features (Bacterial, Viral, Atypical) are more important in adults. Not so much in pedia.
However, in pedia, the clinical features overlap, there is no set of clinical feature that will strongly tell you with certainty if viral, bacterial.
However, features seen are MC in bacterial or viral pneumonia, so not all manifestations are referable to the RT
BACTERIAL PNEUMONIA VIRAL PNEUMONIA ATYPICAL PNEUMONIA
- sudden onset; fast clinical course - Begins with URTI sx - Called atypical because they do not
(mahihirapan agad huminga) - Gradual onset of respiratory follow the behavior of pneumonia
- Non-specific: fever, chills, headache, distress and cough (child is less caused by TYPICAL pathogens
irritability, GI problems toxic looking vs. bacterial); - Causative agents: Mycoplasma, Chlamydia
(Vomiting/Diarrhea) progressive symptoms (ilang araw (50% of pneumonia caused by
Diarrhea – d/t the swallowed bago mahirapan huminga) Chlamydia: with (+) hx of conjunctivitis)
phlegm capable of making stools - Crackles - Refractory to conventional antibiotics
softer, NOT watery - More appreciated w/viral: - prolonged course and delayed resolution
Vomit – if they don’t swallow their Wheezing – onset trying to - Drug of Choice: Macrolides
phlegm, they vomit it (2 ways expire against a partially 1st gen – e.g. Erythromycin (NOT USED d/t
how the child get rid of their closed glottis, usually in adv effect = GI upset)
plegm) neonates 2nd gen – e.g Clarithromycin
Abdominal pain – referred pain Grunting 3rd gen – e.g. Azithromycin
(R: Lungs and stomach share - more appreciated in viral - If refractory:
some nervous supply. pneumonia, usually seen in Amoxicillin/Ampicillin
Inflammation of the lung infants (6months and below) 2nd gen Cephalosporins
parenchyma manifest also with - Trying to expire against a - X-ray Pattern: Interstitial Pneumonia – diffuse
abdominal pain) closed glottis, parang pulmonary infiltrates
- High grade fever – bacterial cause umeere, everytime the child EXAMPLE:
breathes, you can hear it Pt is 1 yo think Haemophilus DOC:
- Very prominent in neonates Ampicillin (R: Penicillin has NO coverage for
this)
You gave Ampiciilin for 1 week but not
improving
Think either resistance or might be d/t
secondary organism NOT responsive to your
DOC
So, from Ampicillin, now give Cephalosporin
2nd gen – more gram negative coverage
Haemophilus is g (-) give 2nd gen Ceph.
(Cefuroxime, Cefaclor)
If the pt. still did not improve, go to 3rd gen.
(Ceftriaxone, Beta lactamase resistant like Co-
Amoxiclav or Sulbactam)
Pag nakakita ng batang may Pneumonia, di
mo iisipin na atypical pneumonia agad, once
the drug does not work, that’s the time you will
realize that it is ATYPICAL
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 9
PULMONARY MANIFESTATIONS: EXTRAPULMONARY MANIFESTATIONS:
- Cough, always present in pneumonia EXCEPT in neonates - Altered sensorium drowsy (to determine, must be able to
- Pulmonary signs need not be present at the start interact with the patient)
- May have fever first or cold first before the COUGH - Hypoxemic -> drowsy
- Most important manifestation COUGH (R: You cannot dx - Seizures (upward gaze, stunts)
pneumonia w/o cough except if the pt. is a neonate. In
neonate, cough is not so prominent) Can suggest etiologic organisms:
- >1 mo (+) cough - Skin infections (Strep, Staph) --- Maraming sugat sa paa think
- Dyspnea, apnea, cyanosis, bradycardia of staph or strep, pt’s pneumonia might be d/t these organisms
Dyspnea DOB (intercostal retractions, - Ear infections – luga (Strep, H. influenza, Staph)
Periodic respiration cessation of breathing >20 seconds Eye infection + rash (measles)
Apnea: cessation of breathing >20sec or episodic
breathing + cyanosis and bradycardia
- Use of accessory muscles of respiration (SCM, scalene,
trapezius)
- Tachypnea: most important clinical predictor of pneumonia
Neonates – RR > 60 cpm
1-12 mo – RR > 50cpm
13 mo – 5yo – RR > 40cpm
>5y/o – RR > 30cpm
DO A COMPLETE PE OF THE PATIENT
- Inspection
- Palpation
- Percussion: dullness (PE finding to differentiate fluid or gas, GAS
heperresonant, NORMAL resonant)
- Auscultation: crackles, ~diminished breath sounds
(all px with pneumonia present w/ crackles, except those
who are dehydrated)
- Retractions: Subcostal, supraclavicular, infraclavicular,
suprasternal retractions, intercostals
- VOCAL and TACTILE FREMITUS differentiate solid from liquid
(SOLID increased TF, FLUID decreased)
- Chest pain clue that there is pleural involvement
- Simple cases – chest pain is (-)
- Manifestations of respiratory problems need not be referable to
the respiratory tract, you can have manifestations involving
other systems (cardiac DOB results to compensatory
tachycardia, Inc. in VS)
Recurrent pneumonia Persistent/ Non resolving Microbiologic Studies: to identify the pathogens
Pneumonia Culture of lung aspirate – gold standard in the diagnosis of
– paulit ulit - persistence of bacterial pneumonia.
– At least 2 episodes in 1 symptoms and o R upper lobe MC affected part of the lung
year radiologic o Get 10cc syringe, gauge 16 or 18
- In between, the x-ray would abnormalities >1 month o Count where’s the center rib
show clearing of the – In between, the x- o E.g rib no. 3, then mark
infiltrates ray DO NOT show o Puncture to aspirate secretions
- > 2 episodes in a year or > 3 clearing of the o Prob: very invasive, mothers won’t consent most of
episodes with radiologic infiltrates the time
clearing between Blood cultures – low yield and may culture something else
occurrences mistakenly
o NOT routine bec:
DIAGNOSIS o the organism in the blood may not necessarily the
CAP Diagnosis organism causing the pneumonia of the patient
History and clinical hx of cough o low yield blood culture in pneumonia <15%
o Fever (+/-) o not routinely requested unless entertaining the
o PE: crackles, Tachypnea (based on WHO) possibility of SEPSIS
Chest radiograph not required especially if the patient is Tracheal aspirates – intubation and section w/in 1hr o/w
NOT toxic looking or your very sure of the dx new colonization will set in
o Only if there are complications solid, liquid or o via ET tube – through the nose/ mouth
gas o Impt: it will enter the trachea, suction the
o Determine severity secretions
o Unsure of dx To confirm o Must be done within the 1st hr of intubation
CBC - not need before giving antibiotics o R: >1 hr. intubated, there will be colonizers in the ET
o To determine ATYPICAL vs VIRAL tube, you might not get the exact pathogen
o Laboratory test to request is CBC causing the Pneumonia
o If lymphocytic predominance VIRAL Sputum culture and gram-stain – only for children >10 y/o
o Sometimes you may need >1 examination to give (capable of expectoration)
you the dx Bacterial and viral antigen detection – kit, results in a few
o Correlate the results minutes, very expensive, done for research purposes
ESR, CRP – acute phase reactants; no roles in pneumonia; Tissue culture and viral antigen – gold standard for viral
not routinely requested pneumonia
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 10
CAP MANAGEMENT CAP Complications
Supportive Management Pleural Effusion liquid
Continued feeding – unless high risk of infection Pneumothorax gas
o do not starve the pt. unless the risk for aspiration is
o Atelectasis solid
very high
Hydration
Oxygen
Antipyretics
Clearing of nasal passages
Chest physiotherapy chest tapping/ clapping
o hand should be cupped, movement should be
from the wrist, do it fast
o if baby use 1 or 2 fingers, put on the chest or
back, then vibrate
o to dislodge the secretions
o can also use the mask of the ambubag
o Percussor – device use by RTs
Antibiotics
CAP PREVENTION
Classification based on the probability that the patient might die
Proper prenatal care
d/t the PNEUMONIA
o poor prenatal care = low birth weight babies risk
NOT classification of severity
factor for pneumonia mortality
Based on MORTALITY
Immunization (Hib, DPT, TB, measles)
Don’t focus on the age
Breast feeding
Important is Tachypneic
Good Nutrition
Vitamin A supplementation - promoting cell mediated
A vs B A (-) co-morbidity and dehydration
immunity and enhance re-epithelialization of airway
B vs C C greater signs of dehydration, other signs of respi
Reduction of pollution and crowding to prevent spread
distress (retractions)
of infx
C vs D D sensorial changes, abN sounds, complications
o ZINC for prevention of pneumonia (NOT
A and B can be managed OPD
treatment)
C admitted – WARD
D admitted – ICU
MC cause of Pneumonia in the Phils MIXED (give antibiotics)
In the US d/t viruses (They do not routinely start antibiotics)
LOBAR PNEUMONIA/ BRONCHOPNEUMONIA INTERSTITIAL PNEUMONIA
LOBAR CONSOLIDATION
Opacity in the R upper lobe Strep, haemophilus, staph, gram (-) think viral or atypical pathogens
Filled with secretions With INFILTRATES described as to: INFILTRATES
CONSOLIDATION 1. Describe (Fine or Course) Course 1. Fine bec. The secretions are
Think or Haemophilus or Strep (NOT virus bec. The secretions are inside outside the alveolus (interstitial
nor atypical) the alveolus spaces)
2. Location Diffuse
With predilection for the hilar area
Alveolus Acinus lobule lobe
The air went to the alveoli, from1
alveolus it went to the surrounding
alveoli
This is d/t the communications between
the alveoli Pores of Kohn and Canals
of Lambert
1 organism transfers from 1 alveoli to
the other passes through the airway,
eventually invade the surrounding lung
parenchyma
= Airway and parenchymal
involvement
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 11
PLEURAL EFFUSION
DESCRIPTION
Pleural fluid is found bet parietal and visceral pleura
Normally 1-2ml per hemi thorax -> prevents adherence of
visceral to parietal pleura
Excess pleural fluid inside the thoracic cavity
Pleural fluid in the fluid cavity N (At least 4 -12 ml)
Old books: 1-2 ml
ETIOLOGY
90% of PF filtered out of arterial end is reabsorbed at venous
end
<10% return to lymphatics Sometimes the Xray result is not classic Pleural Effusion
Starling’s Law = balance between filtration and absorption Still wondering if fluid or solid
Hydrostatic and oncotic Request for thoracic UTZ to differentiate
Normal: Hydrostatic pressure > oncotic pressure net
effect: more fluid outside the blood vessels 3) Ultrasonography
but the difference must be small to maintain the 4-12ml 4) Thoracentesis - Insert a plastic needle with a stylet and
Causes – d/t Pneumonia or secondary to other diseases (TB, aspirate fluid in the chest, submit for analysis
renal, cardiac problems) o Clear/yellow – serous
o Purulent – pus,“nana”
CLINICAL FEATURES o Sanguinous, blood – hemothorax
With history of cough, tachypnea
DIAGNOSIS
1) Hx and PE findings:
o Auscultation: ↓breath sounds since H2O is not a good
Transudates - inflammatory Exudates - infection
conductor of sound, ~retractions
condition
o breath sounds decreased (decreased BS are d/t
Occurs with intact Results from
solid, liquid or gas, that is why you must have a
capillaries inflammation – as in
complete PE to identify what is inside)
Proteins do not leak pneumonia
o Percussion – to differentiate fluid (dull) vs other causes
through Protein-rich fluid leaks
o Fremitus – decreased
↑Hydrostatic pressure or from capillaries
o Retractions - +/- depending on the volume (small
decreased oncotic Local causes
amount of fluid = no retractions)
pressure
2) X-ray
Systemic causes - CHF,
o Necessary and always upright position
kidney dse, tb
(Magenblaze/gas bubble found immediately below
the left hemidiaphragm)
o Demonstrate air fluid level meniscus sign
diagnostic of Pleural Eff.
o Costophrenic Angle – angle form by ribs and
diaphragm, normally sharp, but in effusion disappears,
blunting or loss because it is filled with fluid Rationale: knowing whether exudate or trasudate, to
o Intercostal spaces widen depending on the volume identify possible etiology
of the fluid 5) Microbiologic Studies (underlying cause)
o LLD can also be done – allows you to see air fluid level, Gram stain
even measureable -> Meniscus Sign (Significant is Culture
>1cm) AFB smear (not routine in US, routine in the Phils)
mortal sin thoracentesis but did not get an AFB
smear
MANAGEMENT
SEROUS: PURULENT (NANA): SURGERY
Antibiotics based on age of patient Presumed Staph, unless proven Decortication operate the child,
If pt. did not had Hib vaccine otherwise Oxacillin open the chest, peel off the hard pus,
give Ampicillin o If MRSA, Resistant major procedure, very bloody
If pt. had Hib vaccine expect Vancomycin, but expensive VATS - Video assisted thoracoscopy
Strep. Give Penicillin o Anti-staphylococcal drugs no need to open the chest wall, just
Infant – H. influenzae -> ampicillin Tube drainage/closed-tube make a hole then insert a tube with
Preschool+ - S. pneumoniae until thoracostomy (decide if the fluid should video to see the chest cavity, then
proven otherwise -> penicillin be drained) operate
Also look at immunization status Indicated if fulfills one of the In thoracostomy, when you hit the bone,
following: need only 1 of the 5 slide the needle UP to prevent hitting the
o Gross pus vein artery and nerve
o Serous, do gram stain Evacuate the pus If the pus is left inside
(+) Microorganism on GS the chest antibiotic won’t be able to take
If fulfills neither, wait for effect the pus will harden
chemical analysis: Prevent the lungs from expanding
o PF glucose <40 mg/dL Patient will become dyspneic
o PF LDH >1000 IU (restrictive lung)
o PF pH <7.0
If not purulent, wait for analysis
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 12
TB EFFUSION HEMOTHORAX CHYLOTHORAX
If it is purulent, you can call it empyema or PF hematocrit >50% milky, white or yellow, no smell
pyothorax From the thoracic duct, w/c can be
Char feature: TB effusion: PF protein >5g/dL injured by surgery
(If it coagulates on standing -> it is simply In neonates – most common cause of PF
traumatic; you hit the VAN of the ribs) PF triglycerides >110mg/dL
-> ratio >0.5 -> true Smear: demonstration of fat globules,
hemothorax chylomicrons
PNEUMOTHORAX
DESCRIPTION MANAGEMENT
Inside the thoracic cavity, usually there is no free air Usually 1. If Mild - give 100% oxygen (Green tank –100% O2; Black/
it is in the alveoli and bronchus. Gray tank – 21% O2/room air/ compressed air)
Abnormal accumulation of gas in the pleural cavity -how would you know it is minimal, check the xray, there is a
computation for this.
CAUSATIVE AGENT if pt’s face mask nakasabit sa green tank, receive not exactly
Mostly consist of Nitrogen, O2 only 20% 100% not unless the tube of the tank is connected to the trachea
Adult - the common cause is stab/trauma (Never remove itself. It will be diluted by the room air.
weapon to prevent air from rushing in d/t pressure gradient, Actual conc of O2 received is actually FiO2/ fraction of inspired
suck in of atmospheric air) oxygen.
In pediatrics - the most common is still infection (Pneumonia) No. of %O2 labeled on the tank- it is the actually the FiO2
Alveolar rupture received by the pt
Most abundant gas in room air is nitrogen.
- Principle of denitrogenation or nitrogen wash up – 100% oxygen
CLINICAL FEATURES
readily displaces nitrogen o In PT air is usu nitrogen so if given O2
Types: it will eventually replace it and it will be absorbed by blood
1. Primary spontaneous – “kusang nangyayari” no traumatic, only done in mild pneumothorax
or underlying disease , 2. If massive –
Typical pt: M, adolescent, asthenic, athletic a. chest tube thoracostomy
Usual scenario: Chest pain collapse (rupture of lung) - Usually done by surgeon
2. Secondary spontaneous – in gen. practice MC, d/t -insert a chest tube to remove all of the air out
underlying lung dse but NO trauma Where to place the tube on the chest: fluid- down; air-up
3. Traumatic if you haven’t seen the x-ray of the pt , do not attempt to
4. Iatrogenic - 2° to procedure, careless procedure thoracentesis. Confirm first the location
5. Catamenial – blebs or diaphragmatic defects b. Direct needle aspiration (needling)–emergency
Typical pt: F, adolescent, during their monthly pd procedure
- Fill kidney basin with water, opposite end of butterfly needle in
- because air moves more quickly as compared to fluids water
Mabilis dumami ang air compared sa fluids - Per x-ray place needle, air will be drawn out bubble
- px complains of SUDDEN DYSPNEA AND CHEST PAIN formation
Hx of Pneumothorax: acute tachypnea, acute resp distress - Emergency relief only, until surgeon available
Hx of Pleural Effusion: progressive tachypnea, progressive resp c. Chemical pleurodesis
distress - Recurrent pneumothorax
- severity of symptoms will depend on extent of lung collapsed - chest tube insertion w/ sclerosing agent = talc powder
and pre-existing lung disease Talc will insite sclerosis/ fibrosis so that the leak will be covered up
DIAGNOSIS
History and PE – Diagnostic: hyperresonant lung fields
Confirm by X-ray XRAY!!!
- Hyperlucent = matches background lucency, blackness
- Absence of lung markings (pathognomonic)
ibig sabihin hangin lng eto outside of the lungs
Heart moves to the right meaning there is something occupying
the left side
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 13
ATELECTASIS
DESCRIPTION
lungs collapse or not properly expanded
Imperfect expansion/collapse of a segment or lobe of a
lung
ETIOLOGY
1. External pressure
a. External compression w/in thoracic cavity– effusion,
enlarged LN, tumor causes impingment collapse
b. Direct interference w/ expansion
2. Intrabronchial (airway) obstruction - MC
a. Most important
b. Usu mucus plug- MC secretions
3. Reduced amplitude of expansion
a. Common in surgery pts
b. Shallow breathing -> lung collapse
usually advice the pt to deep breath Wedge or fan shaped - typical finding
because it is painful to breathe, the pt will tend to do shallow - Triangular Shape/Wedge Shape/Fan Shape/ Pyramidal of
breathing instead opacity
- Apex is in middle part
PATHOPHYSIOLOGY - Only atelectasis causes shift (trachea, etc.) to the same side, all
- Incomplete: air passes in but cannot be expired other chest lesions push it opposite (by palpation, you can also
- Complete: air cannot even pass in appreciate tracheal deviation to the ipsilateral side of the lesion)
If there is an obstruction in the airway, whch will collapse - Asymmetrical lung expansion, lag on right o PMI deviated to
proximal or distal? distal right
Nitrogen - absorbed in 2-3h
O2 – absorbed = 6-10 mins MANAGEMENT
Eventually nitrogen will be absorbed + obstruction (no new - Depends on cause, duration and severity
air) -> atelectasis - Antibiotics – pneumonia secretions
- Occluded airway -> trapped air - Bronchodilator – asthma
The more segments of the lung that is occluded, the more - Bronchoscopy –remove FB (critical period – 8 weeks)
symptoms the patient will present -> fibrotic or necrotic lungs
All distal to occluded airway will be collapsed
hospital
CLINICAL FEATURES AND DIAGNOSIS
for another
PE findings similar to Consolidation x-ray
- Parenchyma compressed together, solidified - Chest physiotherapy- secretions
- RLL and LLL most frequently collapsed - Corticosteroids – asthma
- But in pts w/ PTB, RML are the ones usually collapsed - Tb – anti-tb drugs
Chest X-ray
-establish the diagnosis PROGNOSIS
Horizontal fissure –division separating RUL and RML
- Benign
- Normal - forms right angle w/ vertebral column
- Prone to infection if remains to become atelectatic
CONSOLIDATION ATELECTASIS - If persistent -> bronchiectasis, lung abscess
Lung the lung is filled with the lung is reduced
appearance secretions in size because of no
air
Angle of lungs filled w/mucous less volume,
Horizontal and secretions -> becomes smaller,
fissure ↑volume -> more acute angle
increased/obtuse or
same angle
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 14
SAMPLE CASES
A 9 mo old infant bought to the opd with a hx of 1 day 5 y.o. boy brought to the ER because of DOB. Productive cough
productive cough, watery nasal discharge, low to moderate for 1 week, high grade fever for 2 days. On PE, the RR was 50, he
grade fever. On the day of consultation the infant is breathing had symmetrical chest expansion, intercostal retractions
fast, hence he brought to the ER. bilateral, decreased breath sounds on the right, decreased
1. Where is the pathology? Upper or lower RT? vocal and tactile fremitus on the right, dull percussion.
Lower –the patient is presenting difficulty of breathing
Upper – will not present with respiratory distress, they What condition should we consider? Pleural Effusion
are benign
Any problem invoving the larynx, there is What is your next step? X-ray to confirm the presence of pleural
hoarseness of voice, signs of obstruction – stridor effusion.
2. Airways or lung parenchyma? What if there is a homogenous opacity on the right the heart is
Airway – very acute. 1 day hx of cough then progress midline the entire right lung. Is it a clear case of pleural effusion?
to DOB. Very fast, very short, nahirapan huminga, think No coz of the normal position of the heart. In pleural effusion,
of airway problem heart should deviate to the opposite side.
UTZ should be done to differentiate if solid or liquid
Parenchymal – 2 lungs; pneumonia - coughing for few
days before DOB
A 5 y.o. boy was admitted to the hospital due to respiratory
DIAGNOSIS: distress. X-ray coarse infiltrates on both fields. The patient was
Bronchiolitis – age- 9 mos, tachypnic, retractions. started on IV pen. After 3 days, the patient’s condition was
But if I will give you a case in which the pt’s RR is 62bpm, improved. He was more comfortable at room air, was eating
symmetrical chest expansion, intercostals retraction, crackles and was just waiting for the completion of medicines. On the 6th
and wheezes on both lung fields. Pat medical history had 2 hospital day, he suddenly complained of dyspnea and was
similar episodes at 3 months and 5 months of age. What would noted to be irritable.
be your diagnosis – bronchial asthma
Cannot be bronchitis – because bronchitis is a benign What condition should we consider? Pneumothorax
condition. You are not suppose to manifest respiratory The patient was stable or previously well then suddenly dyspneic,
distress. if the patient can verbalize will complain of chest pain
2 benign diseases pneumothorax chest xray
1. Bronchitis
2. Laryngitis
Happy happy birthday Nikko Jay and Hannah!! <3
EVANGELISTA, FALCON, MARQUEZ, MIRASOL (3B) 15
Das könnte Ihnen auch gefallen
- Acute Respiratory InfectionsDokument145 SeitenAcute Respiratory InfectionsManuel VIc O. Lacaya100% (1)
- A Modern Approach To Cough ManagementDokument4 SeitenA Modern Approach To Cough ManagementSorin PalcuNoch keine Bewertungen
- Cough: Group - 10Dokument41 SeitenCough: Group - 10AradhanaRamchandaniNoch keine Bewertungen
- Bailey & Scott's Diagnostic Microbiology, 13th Edition-Pages-1011-1034Dokument24 SeitenBailey & Scott's Diagnostic Microbiology, 13th Edition-Pages-1011-1034JhanKarloFloresFlores0% (2)
- RespDokument23 SeitenRespAyessa D. RosalitaNoch keine Bewertungen
- The Respiratory SystemDokument61 SeitenThe Respiratory SystemLuna JadeNoch keine Bewertungen
- Respiratory Disorders & TB in Children (Part I and Ii) - Dr. MendozaDokument17 SeitenRespiratory Disorders & TB in Children (Part I and Ii) - Dr. MendozaRea Dominique CabanillaNoch keine Bewertungen
- Thesis On Respiratory SystemDokument96 SeitenThesis On Respiratory SystemDr Nimit ShahNoch keine Bewertungen
- Asthma Lesson PlanDokument26 SeitenAsthma Lesson PlanBharat Singh BanshiwalNoch keine Bewertungen
- Lec 3 PTDokument12 SeitenLec 3 PTBassam AlgalalyNoch keine Bewertungen
- 50 Diseases: Respiratory System: 1. Emphysema Nursing ManagementDokument26 Seiten50 Diseases: Respiratory System: 1. Emphysema Nursing ManagementJewenson SalvadorNoch keine Bewertungen
- RespiDokument27 SeitenRespierisha.cadagNoch keine Bewertungen
- Approach To The Patient With Disease of The Respiratory SystemDokument3 SeitenApproach To The Patient With Disease of The Respiratory SystemIsabel CastilloNoch keine Bewertungen
- Chronic Cough in Children: Dwi Wastoro DadiyantoDokument57 SeitenChronic Cough in Children: Dwi Wastoro DadiyantoirenaNoch keine Bewertungen
- Nursing Care Management - 112Dokument67 SeitenNursing Care Management - 112Ong KarlNoch keine Bewertungen
- NCM 112 N LECTURE MidtermDokument42 SeitenNCM 112 N LECTURE MidtermVivien IgnacioNoch keine Bewertungen
- Respiratory System: Larynx EpiglottisDokument12 SeitenRespiratory System: Larynx Epiglottisangel sychingNoch keine Bewertungen
- Diseases of Respiratory SystemDokument23 SeitenDiseases of Respiratory SystemMarchelle Fae EsmallaNoch keine Bewertungen
- Respiratory SystemDokument2 SeitenRespiratory SystemDearly Niña OsinsaoNoch keine Bewertungen
- Respiratory SystemDokument38 SeitenRespiratory Systemjsreyes.402Noch keine Bewertungen
- W1 L4 Asthma in ChildrenDokument61 SeitenW1 L4 Asthma in ChildrenAnas FikriNoch keine Bewertungen
- UNIT 1 (MS 1) Care of Clients With Problems in OxygenationDokument10 SeitenUNIT 1 (MS 1) Care of Clients With Problems in OxygenationElle MirandaNoch keine Bewertungen
- Im B4.9 CopdDokument9 SeitenIm B4.9 CopdCC Samson, Caesar AnthonyNoch keine Bewertungen
- Asthma 2 (LP)Dokument14 SeitenAsthma 2 (LP)Abi NairaNoch keine Bewertungen
- Anatomy and Physiology of The Respiratory System: Basco, Kimberly BSN-2Dokument5 SeitenAnatomy and Physiology of The Respiratory System: Basco, Kimberly BSN-2Cxazandra Kaith CasasNoch keine Bewertungen
- Hippokratia 13 187Dokument5 SeitenHippokratia 13 187A.h.MuradNoch keine Bewertungen
- 6 RESPI - Bronchopneumonia.Dokument11 Seiten6 RESPI - Bronchopneumonia.Putri NoviyantiNoch keine Bewertungen
- Pneumonia: DR - Dr. Tahan P.H.,Spp.,Dtce.,Mars Fk-Uwk, 1 April 2011Dokument35 SeitenPneumonia: DR - Dr. Tahan P.H.,Spp.,Dtce.,Mars Fk-Uwk, 1 April 2011IqbalRazifNoch keine Bewertungen
- Medical Mnemonic Sketches : Pulmonary DiseasesVon EverandMedical Mnemonic Sketches : Pulmonary DiseasesNoch keine Bewertungen
- Ca - MS (Respiratory)Dokument4 SeitenCa - MS (Respiratory)kyleNoch keine Bewertungen
- Respiratory 2 of 2Dokument31 SeitenRespiratory 2 of 2glenn johnstonNoch keine Bewertungen
- Pneumonia PathoDokument38 SeitenPneumonia PathoIvan Michael IcaoNoch keine Bewertungen
- 5 MED II 1 - PneumoniaDokument11 Seiten5 MED II 1 - PneumoniaDeann RoscomNoch keine Bewertungen
- Approach To CoughDokument5 SeitenApproach To CoughZulaikha HattaNoch keine Bewertungen
- Laracas Lezel M. BSN3B - Medical SurgicalDokument14 SeitenLaracas Lezel M. BSN3B - Medical SurgicalLezel LaracasNoch keine Bewertungen
- Asthma OpdDokument59 SeitenAsthma OpdJb TlntinoNoch keine Bewertungen
- 5485 Jurnal Edit - Fix.2pptxDokument36 Seiten5485 Jurnal Edit - Fix.2pptxAdita AyuNoch keine Bewertungen
- Respiratory SystemDokument15 SeitenRespiratory SystemMichelle Gambol100% (2)
- 1 CopdDokument37 Seiten1 CopdnaturehalwestNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD)Dokument16 SeitenChronic Obstructive Pulmonary Disease (COPD)Kimberly Abella CabreraNoch keine Bewertungen
- J Resp 2008 09 012Dokument7 SeitenJ Resp 2008 09 012Ariel Badillo BustamanteNoch keine Bewertungen
- Dr. H. I. Dr. H. I. Boediman Boediman,, Sp.A Sp.A (K) (K) : B Fdiii FR IlDokument49 SeitenDr. H. I. Dr. H. I. Boediman Boediman,, Sp.A Sp.A (K) (K) : B Fdiii FR IlPrissilmaTaniaNoch keine Bewertungen
- "Year of Universalization of Health": I.S.T.P: Course: Especiality: Cycle: Topic: Teacher: StudentDokument8 Seiten"Year of Universalization of Health": I.S.T.P: Course: Especiality: Cycle: Topic: Teacher: StudentKarina DiazNoch keine Bewertungen
- Respiratory DisordersDokument48 SeitenRespiratory DisordersJean Cabigao100% (1)
- Case Study: Neonatal PneumoniaDokument47 SeitenCase Study: Neonatal PneumoniaJay Villasoto100% (1)
- Causes and Possible Prevention of Asthma and AllergiesVon EverandCauses and Possible Prevention of Asthma and AllergiesNoch keine Bewertungen
- Case 3 - Anatomy and Physiology - SalimbagatDokument4 SeitenCase 3 - Anatomy and Physiology - SalimbagatChristine Pialan SalimbagatNoch keine Bewertungen
- Recent Developments in United Airways DiseaseDokument7 SeitenRecent Developments in United Airways DiseaseStanislaus Stanley SuhermanNoch keine Bewertungen
- Childhood Asthma: DR - Rodman Tarigan, Spa.,MkesDokument35 SeitenChildhood Asthma: DR - Rodman Tarigan, Spa.,MkesBambang IrwansyahNoch keine Bewertungen
- Vital Signs:: Case Scenario: AsthmaDokument9 SeitenVital Signs:: Case Scenario: AsthmaCherry CayabyabNoch keine Bewertungen
- Week 1 Respiratory SystemDokument9 SeitenWeek 1 Respiratory SystemCarl Brian L. MonteverdeNoch keine Bewertungen
- Respiratory System To Be ContinueDokument5 SeitenRespiratory System To Be ContinueRose Ann CammagayNoch keine Bewertungen
- Update in Airway Obstuction DiseaseDokument42 SeitenUpdate in Airway Obstuction DiseaseTiyaTyraSidoraNoch keine Bewertungen
- 50 DiseasesDokument44 Seiten50 DiseasesJewenson SalvadorNoch keine Bewertungen
- ICD Pulmo Session 3Dokument4 SeitenICD Pulmo Session 3Mary Christine IlangaNoch keine Bewertungen
- Prologue 1.1 BackgroundDokument9 SeitenPrologue 1.1 BackgroundWulan Yulia DintasariNoch keine Bewertungen
- 03 Diagnostic Approach To Cough PDFDokument1 Seite03 Diagnostic Approach To Cough PDFSindujaNoch keine Bewertungen
- Acute Respiratory Infection: Pediatrics of Guangxi Medical University Nong GuangminDokument62 SeitenAcute Respiratory Infection: Pediatrics of Guangxi Medical University Nong GuangminSecret AgentNoch keine Bewertungen
- Rhinitis and Asthma United Airway DiseaseDokument7 SeitenRhinitis and Asthma United Airway DiseaseStanislaus Stanley SuhermanNoch keine Bewertungen
- NCM 112 LEC Topic 2 Oxygenation Current Health History Physical Examination Normal Abnormal Breath Sounds Breathing PatternsDokument7 SeitenNCM 112 LEC Topic 2 Oxygenation Current Health History Physical Examination Normal Abnormal Breath Sounds Breathing PatternsViviene Faye FombuenaNoch keine Bewertungen
- Approch To StridorDokument27 SeitenApproch To Stridoraltabeb hasoon67% (3)
- Mark Klimek Blue BookDokument200 SeitenMark Klimek Blue Bookbeatris100% (7)
- TracheitisDokument7 SeitenTracheitisÁlvaro DezaNoch keine Bewertungen
- (Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Dokument43 Seiten(Ped-W1) (Dr. Zuhair M. Al Musawi) Repiratory 2Haider Nadhem AL-rubaiNoch keine Bewertungen
- Croup: Straight To The Point of CareDokument36 SeitenCroup: Straight To The Point of CareNana OkujavaNoch keine Bewertungen
- Airway Foreign Body: Mohd Nasiruddin MansorDokument25 SeitenAirway Foreign Body: Mohd Nasiruddin MansorZunairaNoch keine Bewertungen
- Inpatient Management of Acute Asthma ExacerbationDokument10 SeitenInpatient Management of Acute Asthma ExacerbationMonika JonesNoch keine Bewertungen
- Lesser Writing BogerDokument51 SeitenLesser Writing BogerAtit Sheth100% (1)
- Croup Diagnosis and Management 2018Dokument6 SeitenCroup Diagnosis and Management 2018Jose Fernando DiezNoch keine Bewertungen
- Acute Upper Airway Obstruction (Power Point)Dokument21 SeitenAcute Upper Airway Obstruction (Power Point)Sawsan Z. Jwaied100% (2)
- Vocal Cord ParalysisDokument74 SeitenVocal Cord ParalysisWaqas KhanNoch keine Bewertungen
- Fundamentals of Pediatric Imaging 2Nd Edition Lane F Donnelly Full ChapterDokument51 SeitenFundamentals of Pediatric Imaging 2Nd Edition Lane F Donnelly Full Chapterbetty.tavares510100% (12)
- Acute Management of Croup in The Emergency - Canadian Paediatric SocietyDokument6 SeitenAcute Management of Croup in The Emergency - Canadian Paediatric SocietyHarrisNoch keine Bewertungen
- ENT NoseDokument18 SeitenENT NosevkNoch keine Bewertungen
- Pediatric Nursing: PilliteriDokument16 SeitenPediatric Nursing: PilliteriLeiNoch keine Bewertungen
- Review: Ediatric NursingDokument142 SeitenReview: Ediatric NursingBuRiO03Noch keine Bewertungen
- Acute Upper Airway ObstructionDokument3 SeitenAcute Upper Airway ObstructionGilbertLiemNoch keine Bewertungen
- Disorders of Skin in ChildrenDokument47 SeitenDisorders of Skin in Childrensmriti boraNoch keine Bewertungen
- Normal PediaDokument13 SeitenNormal PediaChelsea GulfanNoch keine Bewertungen
- Lecture 8, Nursing Care of The Child With Respiratory Dysfunction and Renal Disorders 2Dokument48 SeitenLecture 8, Nursing Care of The Child With Respiratory Dysfunction and Renal Disorders 2مهند الرحيليNoch keine Bewertungen
- Oral RevalidaDokument98 SeitenOral RevalidaJay ArNoch keine Bewertungen
- Understanding Airway Disease in InfantsDokument17 SeitenUnderstanding Airway Disease in InfantsGabrielaNoch keine Bewertungen
- Problem - Solving - Collected 2Dokument64 SeitenProblem - Solving - Collected 2mulyadiNoch keine Bewertungen
- Common Pediatric ED Presentations: Dr. Okon, MD, MRCSDokument6 SeitenCommon Pediatric ED Presentations: Dr. Okon, MD, MRCSEdwin OkonNoch keine Bewertungen
- Boger The Homoepathic TherapeuticsDokument96 SeitenBoger The Homoepathic TherapeuticsKumar100% (2)
- Pain & SympDokument4 SeitenPain & SympxxdissuNoch keine Bewertungen
- Upper Airway Obstruction: Ref.: Nelson Essentials of Pediatrics 7 - Edit. Nelson's Textbook of Pediatrics 20 - EditDokument5 SeitenUpper Airway Obstruction: Ref.: Nelson Essentials of Pediatrics 7 - Edit. Nelson's Textbook of Pediatrics 20 - EditAli Abd AlrezaqNoch keine Bewertungen
- Pediatrics RemarksDokument62 SeitenPediatrics RemarksGÖKSU SAYGILINoch keine Bewertungen
- Im - Disorders of The LarynxDokument11 SeitenIm - Disorders of The LarynxChristine MendozaNoch keine Bewertungen
- Acute Epiglottitis: DR Eric El HittiDokument5 SeitenAcute Epiglottitis: DR Eric El HittinoviNoch keine Bewertungen