Beruflich Dokumente
Kultur Dokumente
Chapter 213:: Chemical Peels and Dermabrasion:: Gary Monheit & Bailey Tayebi
Hochgeladen von
Jhauharina RfOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Chapter 213:: Chemical Peels and Dermabrasion:: Gary Monheit & Bailey Tayebi
Hochgeladen von
Jhauharina RfCopyright:
Verfügbare Formate
Chapter 213 :: Chemical Peels and Dermabrasion 31
:: Gary Monheit & Bailey Tayebi
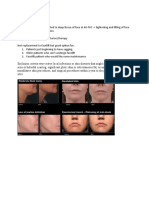
involves the application of a chemical exfoliant aimed
AT-A-GLANCE to wound and subsequently regenerate the epider-
mis and/or dermis to remove superficial skin lesions,
■ Chemexfoliation agents are broadly classified into improve pigmentary abnormalities and photodamage,
superficial, medium, and deep peeling agents and address textural concerns (Table 213-1).1
according to their depth of penetration and
histologic injury.
■
PERIOPERATIVE
Chapter 213 :: Chemical Peels and Dermabrasion
Preoperative evaluation of skin type, degree
of photoaging, and underlying skin disorders
is critical in safeguarding against potential
complications.
CONSIDERATIONS
■ Appropriate patient selection and choice of The perioperative evaluation is a critical component
procedure are critical to success. of every chemical resurfacing procedure. The physi-
■
cian should seek a thorough understanding of patient
Keratocoagulation, evidenced by a white frosting
treatment goals, expectations, and allotted down time
of the skin, is generally regarded as the desired
prior to initiation of the procedure. The physician
clinical end point of chemical peeling with
should also assess the patient’s level of compliance
trichloroacetic acid.
and need for preprocedural and/or postprocedural
■ Mechanical resurfacing, which includes
adjuvant treatments.2 Patients should be instructed
microdermabrasion, manual dermasanding, and
to avoid depilatory procedures, such as waxing and
motorized dermabrasion, is an effective method for
shaving, prior to the procedure, as well as ultraviolet
treatment of scars.
light exposure before and after the date of the chemical
■ Infection, prolonged erythema, pigmentary peel. Lastly, preoperative photographs should be taken
alterations, and scarring are potential to serve as a benchmark with which to grade clinical
complications of resurfacing procedures. results.
BACKGROUND INDICATIONS
Resurfacing procedures, including chemical, mechani-
cal, and laser resurfacing, wound the skin in a con- Chemexfoliation indications can be classified into pig-
trolled and predictable manner so as to promote the mentary (eg, postinflammatory hyperpigmentation,
growth of new skin with improved texture and quality. melasma), photoinduced (eg, actinic keratoses), and
The art of chemical peeling dates back to ancient Egyp- textural abnormalities (eg, epidermal growths, rhyt-
tian times when the use of animal oils, salt, and lactic ides, scarring, acne vulgaris).2
acid in sour milk were used to cosmetically enhance
the appearance of skin. Mechanical exfoliation was
first described in Greek and Roman literature using
compounds containing mustard, sulfur, and limestone. PATIENT SELECTION
In the mid-1800s, Viennese dermatologist Ferdinand
Hebra used various peeling agents to treat pigmentary The perioperative evaluation should assess the
abnormalities. These early exfoliative agents included patient’s skin type, degree of photoaging, and whether
tinctures of iodine and lead, croton oil, cantharides, or not the patient has underlying skin disorders. When
and various acids, including sulfuric, acetic, hydro- evaluating skin type, it is useful to classify patients
chloric, and nitric acids. Tilbury Fox first introduced according to their Fitzpatrick skin phototype (SPT).
phenol to the topical dermatology arena in 1871. A In general, darker skin types (SPT IV to SPT VI) have
decade later, P. G. Unna reported on the use of salicylic an increased risk of pigmentary alterations following
acid, resorcinol, phenol, and trichloroacetic acid (TCA) chemical peels. While superficial peels tend to be well
as peeling agents. Over the next century, several phy- tolerated by all skin types, deep peels are commonly
sicians worked to modify peeling agent formulations, avoided in patients with SPT IV to SPT VI skin because
combinations, and procedures. In the 1980s, Samuel of the higher risks of postprocedural pigmentary
Stegman identified the depth of injury associated with change and scarring (Table 213-2).2-4
various peeling agents, which enabled later categori- The patient’s degree of photodamage assists the phy-
zation into superficial, medium, and deep chemical sician in electing the appropriate rejuvenation proce-
peels. Today, chemexfoliation, or chemical peeling, dure necessary to achieve clinically significant results.
Kang_CH213_p3895-3905.indd 3895 08/12/18 12:03 pm
31 TABLE 213-1
treated with an antiviral agent prior to the procedure.
Common pretreatment regimens include acyclovir 400
Resurfacing Procedures mg thrice daily and valacyclovir 500 mg twice daily
starting on the day of the peel and continued until
PEELING DERMABRASION LASER reepithelialization has occurred (Table 213-3).3,5
Superficial Glycolic Microdermabrasion –
Jessner solution
Salicylic acid
Medium Jessner solution Manual Erbium laser SIDE EFFECTS
depth + 35% dermasanding
trichloroacetic The perioperative consultation is also an appropri-
acid ate time to review the risks and benefits of chemical
Deep Baker phenol Mechanical CO2 laser peeling. Expected intraoperative side effects include
peel dermabrasion stinging, burning, and/or itching. In the immediate
Part 31
postoperative period, erythema, edema, and desqua-
mation may be experienced.2
The Glogau system, which classifies patients into
categories I through IV based on whether the patient
::
has mild, moderate, advanced, or severe photodam-
PERIOPERATIVE
Cosmetic Dermatology
age, is a useful categorization tool for this purpose.
In general, both category I and category II photodam-
age will improve with more superficial peeling agents
PREPARATIONS
(Fig. 213-1). Category III will respond to medium-
depth peels, while category IV will require deep peel- Chemical peeling agents can penetrate to predictable
ing agents possibly in combination with mechanical histologic depths; however, the physician can augment
and/or laser resurfacing procedures3 (Fig. 213-2). this depth with the use of certain preoperative prepa-
Lastly, inquiring about a patient’s underlying skin rations.6-8 Topical pretreatment with retinoic, glycolic,
disorders allows the physician to safeguard against or lactic acid alone, or in combination, will increase the
potentially-devastating complications such as infec- absorption of the wounding agent and promote a more
tion and scarring. The physician should inquire about even penetration of the peel. Pretreatment should
a history of atopy, rosacea, isotretinoin therapy, poor begin 2 to 4 weeks before the procedure and be dis-
wound healing, connective tissue disease, and hyper- continued approximately 2 to 3 days prior to the peel
trophic or keloid scar formation as chemical resur- date.2,6 Pretreatment with a topical retinoid may also
facing may be contraindicated in these patients.4 speed the healing process (Table 213-4).4
Additionally, a history of recurrent infections, includ- Topical medications such as 2% to 5% hydroquinone
ing bacterial, fungal, and viral, should be elicited in may be applied to the skin preoperatively and post-
the preoperative consultation. A patient with recur- operatively to minimize the risk of postinflammatory
rent herpes simplex virus should be prophylactically hyperpigmentation. Pretreatment should be consid-
ered in patients with SPT III to SPT VI, and in those
treated for problems of hyperpigmentation.6 Applica-
tion of hydroquinone, in addition to a ultraviolet A/
TABLE 213-2 ultraviolet B protective sunscreen (sun protection
Fitzpatrick Skin Phototypes and Peel Indications factor 30 or higher), should be initiated 2 to 4 weeks
prior to the date of the peel and resumed once reepi-
PEEL thelialization has occurred postoperatively. As a rule,
SKIN
PHOTOTYPE SKIN REACTION SUPERFICIAL MEDIUM DEEP patients prone to dyschromias should adhere to a pol-
icy of strict sun avoidance in the perioperative period.
I Always burn, + + −
never tan
PROCEDURAL TECHNIQUE
II Always burn, + + −
sometimes
tan
Following informed consent, instruct the patient to
III Sometimes + + −
burn, always
remove any makeup with a gentle facial cleanser. The
tan patient is then placed in the supine position on the
operating table with the head elevated to a 30-degree
IV Never burn, + + ±
always tan
angle.9 This position minimizes the risk of solution
inadvertently dripping toward the eyes and allows the
V Moderate pig- + ± −
physician to visualize the complete treatment area.
mented skin
In general, more superficial chemical peels do not
VI Darkly pig- + ± − require sedation or other forms of anesthesia. Medium
mented skin
3896 and deep peeling agents, however, are associated
−, no; +, yes; ±, either. with significantly more operative discomfort and may
Kang_CH213_p3895-3905.indd 3896 08/12/18 12:03 pm
31
Chapter 213 :: Chemical Peels and Dermabrasion
Figure 213-1 Glogau photoaging types I and II. Indications for superficial peeling.
3897
Figure 213-2 Glogau photoaging types III and IV. Indications for medium and deep chemical peeling.
Kang_CH213_p3895-3905.indd 3897 08/12/18 12:03 pm
31 TABLE 213-3
This cleansing regimen will remove all oil and debris
and promote even penetration of the wounding agent
Contraindications to Medium and Deep Peels while minimizing the risk of a spotty or ineffective
peel.
RELATIVE CONTRAINDICATIONS ABSOLUTE CONTRAINDICATIONS For medium-depth peeling, an absorbing agent may
Active skin disease Open wounds, excoriations be applied to the skin to increase the effectiveness or
Recent facial surgery Isotretinoin within last 6 months penetration depth of the peeling agent. In 1986, Brody
and Hailey applied solid carbon dioxide (CO2) in com-
History of facial keloids Pregnancy
bination with acetone prior to application of 35% TCA
History of postinflammatory Unrealistic expectations to disrupt the epidermal barrier and achieve a more
hyperpigmentation
even peel at a greater histologic depth.3 Later, in 1989,
Radiation to head and neck Poor patient–physician Monheit described a similar technique using Jessner
relationship solution prior to application of 35% TCA. Acting as
Active skin infection an absorbing agent, Jessner solution removes the stra-
■ Bacterial
Part 31
tum corneum allowing for deeper penetration of TCA.
■ Viral Coleman similarly demonstrated greater wounding
depths with use of 70% glycolic acid prior to applica-
tion of 35% TCA.3,9 Use of absorbing agents such as
::
require sedative and pain medications and/or local these offers improved safety, minimizes the risk of pig-
nerve blocks. Such blocks commonly include anes-
Cosmetic Dermatology
mentary alterations and scarring, and creates clinical
thetizing the supraorbital, infraorbital, temporal, and results comparable to a deep 50% TCA peel.
mental nerves.9 The peeling agent is then applied. This is com-
Once the patient has been positioned and the appro- monly done with cotton-tipped applicators or 4-inch ×
priate level of anesthesia has been undertaken, the 4-inch/2-inch × 2-inch gauze. The face is peeled
skin is vigorously cleansed and degreased. A vari- sequentially by anatomic location starting on the fore-
ety of cleansing agents may be used for this purpose head, followed by the temples, cheeks, and finally the
including hexachlorophene, acetone, rubbing alco- lips and eyelids.3 Feathering of the solution into the
hol, chlorhexidine, or some combination of these hairline, brows, and jawline helps to conceal lines of
agents.3,6,7,9 An even application can be achieved with demarcation between peeled and nonpeeled areas.9
a 4-inch × 4-inch gauze. The skin should then be rinsed Alternatively, a superficial peeling agent may be
and dried prior to application of the chemexfoliant. applied to such areas as neck and décolleté to assist in
blending treated and untreated cosmetic units. Special
care is taken to protect the eyes during a chemical peel.
A semidry applicator should be used to carry the solu-
TABLE 213-4 tion within 2 to 3 mm of the lid margin. Furthermore,
tears are wicked away with a dry cotton-tipped appli-
Preoperative and Postoperative Care for
Chemical Peels cator to prevent peel solution from traveling to the
puncta and eye via capillary action.9 Should peel solu-
Preparation (Weeks to Days Before Peel) tion inadvertently enter the eye, initiate aggressive irri-
■ Topical pretreatment with a retinoid, glycolic or lactic acid solution gation with normal saline flushes immediately.
(begin 2 to 4 weeks prior, discontinue 2 to 3 days before peel date) During the procedure, the physician is able to ensure
■ Consider topical 2% to 5% hydroquinone preoperatively and even application of the peeling agent by the demon-
postoperatively, if postinflammatory hyperpigmentation is a stration of even frosting. Frosting is representative of
concern (2 to 4 weeks prior) underlying keratocoagulation, or denaturation of epi-
■ Sun avoidance, especially in individuals at risk for dyschromias
dermal keratin proteins.9 Although true frosting does
■ Consider pretreatment with acyclovir 400 mg thrice daily or
valacyclovir 500 mg twice daily on the day of peel and until
not occur with each and every peeling agent, frosting
reepithelialization is generally regarded as the desired end point. Level I
frosting is defined as erythema with blotchy or spotty
Preprocedural Care (Immediately Prior to Peel)
frosting. This is often seen with light chemical peels.
■ Cleanse skin with gentle facial cleanser
■ Position patient with head up at a 30-degree angle
Level II frosting is commonly seen in medium-depth
■ Consider sedative/pain medications or local nerve blocks for chemical peels and is achieved when a white coating is
medium to deep peels evident with a slight erythematous background show-
■ Degrease skin with acetone, hexachlorophene, rubbing alcohol, ing through. Level III frosting is attained when a solid
or chlorhexidine white enamel-like frosting is demonstrated on the skin.
■ Rinse and dry skin prior to application of chemexfoliant This is seen in deeper chemical peels and is indicative
Postprocedural Care of peel penetration into the papillary dermis.3
■ Cleanse skin up to 4 times/day Immediately following the procedure, cool saline
■ Dilute 0.25% acetic acid (1 tbsp vinegar in 1 pint water) as compresses are applied for 5 to 10 minutes. This is for
cleansing agent comfort as the reaction is complete after frosting. Only
■ Pat dry, apply bland emollient glycolic acid peels require neutralization. A bland
■ Daily sunscreen use
3898 emollient as well as a broad-spectrum sunscreen are
■ Avoidance of excessive sun exposure
then gently massaged into the skin.
Kang_CH213_p3895-3905.indd 3898 08/12/18 12:03 pm
CHEMICAL RESURFACING Superficial chemical peeling chemicals
31
PROCEDURES Phenol Resorcinol Salicylic Acid
OH OH COOH
Chemical peeling involves the application of a chemi-
cal agent that wounds the epidermis and/or dermis OH
and stimulates collagen remodeling and new epider-
mal growth, thus achieving a cosmetic benefit. The OH
degree of penetration, destruction, and inflammation
Trichloracetic Acid
determines the level of peeling.3 Superficial peel- Glycolic Acid C2HCl3 O2
ing agents remove the stratum corneum and wound OH O
the epidermis.8,9 Destruction of the entire epidermis
defines a full superficial peel. Medium-depth peels
penetrate through the papillary dermis to the upper H2C C OH
Chapter 213 :: Chemical Peels and Dermabrasion
reticular dermis.3,8 Deep peeling agents wound a
greater portion of the reticular dermis resulting in Figure 213-4 Superficial chemical peeling chemicals.
production of new collagen and ground substances
(Fig. 213-3).3,8,9
acids such as glycolic acid.2,6 Superficial peeling agents
disrupt corneocyte adhesion and lead to regenera-
tion of a thickened epidermis, normalization of the
SUPERFICIAL CHEMICAL basal cell layer, and dispersal of melanin. Superfi-
cial agents may also enact dermal change including
PEELING increased dermal collagen and improved quality of
elastic fibers.11,12 Complete recovery is expected in 2 to
Superficial chemical peels are indicated for acne, 4 days (Fig. 213-4).4,6
particularly comedonal acne, enlarged pores, postin- Salicylic acid is a naturally occurring β-hydroxy acid
flammatory hyperpigmentation, melasma, mild pho- derived from the bark of the willow tree. It is regarded
todamage, and fine textural concerns.2,4,10 Superficial as a safe peel in all skin types for the treatment of acne,
exfoliants include 10% to 20% TCA (20% to 35% TCA melasma, and postinflammatory hyperpigmentation.
achieves a complete epidermal peel), Jessner solution As described by Grimes, salicylic acid exhibits a lipo-
(14% salicylic acid, 14% lactic acid, and 14% resorcinol philic nature that allows for effective dissolution of the
in ethanol), resorcinol, salicylic acid, and α-hydroxy stratum corneum as well as comedolysis.13 Therefore,
Depth of peels
Hair Peel depth
Stratum corneum
Stratum
granulosum
Stratum Super-
spinosum ficial
wound
Stratum basale (.06 mm)
Papillary
dermis
Upper Medium
reticular depth
dermis (.45-.60 mm) wound
Apocrine Mid. Deep
gland reticular depth
dermis (.60-.80 mm) wound
Lower
reticular
dermis
Fat (2.0 mm)
3899
Figure 213-3 Depth of peels.
Kang_CH213_p3895-3905.indd 3899 08/12/18 12:03 pm
31 treatment of dyschromias. In a pilot study by Grimes,
88% of patients with SPT V and SPT VI demonstrated
improvement in dyschromias, with 4% hydroquinone
pretreatment followed by a graduated series of 20%
and 30% salicylic acid peels.10 Salicylic acid is a pref-
erential peeling agent for dyschromia as it is the least
inflammatory of peeling agents. It has the least risk
of producing postinflammatory hyperpigmentation
(Fig. 213-6).
α-Hydroxy acids include glycolic acid along with
several other naturally, occurring, nontoxic agents
such as lactic, citric, malic, and tartaric acid.2,6 Glycolic
A acid concentrations of 10% to 70% are frequently
used in the treatment of acne, dyschromias, and mild
Part 31
signs of photoaging, and are safe in most skin types.
Unlike other superficial peeling agents, the action of
glycolic acid is time dependent and must be neutral-
ized with normal saline, water, or sodium bicarbonate.
::
α-Hydroxy acids wound the skin via loss of keratino-
Cosmetic Dermatology
cyte cohesion within the epidermis. Peels using 70%
glycolic acid can also result in increased fibroblast
proliferation, collagen and elastic fiber formation, and
melanin dispersion.2,15
MEDIUM-DEPTH
CHEMICAL PEELING
B
Medium-depth chemical peels are indicated for the
treatment of mild to moderate photoaging, pigmen-
tary disorders, lentigines, epidermal growths, rhyt-
ides, and actinic keratoses.9 Peeling agents include
45% to 60% TCA as well as combination peels such
as Jessner solution with 35% TCA (Monheit peel),
70% glycolic acid with 35% TCA (Coleman peel), and
solid CO2 with 35% TCA (Brody peel).3,6,9 Fifty percent
TCA is not used any longer because of the risk of scar
from deeper penetration of the agent in the dermis.
Combination peels are the preferred medium-depth
peels because of their lower risk of postprocedural
dyschromias and scarring.3,9 Histologically, medium-
depth chemical peels are associated with diminished
solar elastosis, fibroblast proliferation, increased col-
lagen formation, and reorganization of elastic fibers
(see Fig. 213-3; Table 213-5).8,12
TCA is a crystalline inorganic compound that results
C in keratocoagulation, or protein denaturation, and
resultant cell death, as indicated by a white frosting on
Figure 213-5 Salicylic acid peel for acne. A, Pretreatment.
the skin. Effects of this self-neutralizing peeling agent
B, Perifollicular frosting. C, After 3 treatments.
are cumulative with each application penetrating
deeper than the last. TCA may be relatively quantitated
salicylic acid proves beneficial in the treatment of with utilization of 1 to 4 cotton-tipped applicators.
comedonal and papular/pustular acne.2,4,13,14 A split- Loose or wrinkled skin should be stretched to achieve
face study by Meguid and colleagues reported that an even application of the solution and prevent pool-
treatment of inflammatory acne lesions with the use ing of the solution in folds. A level II to level III frosting
of 30% salicylic acid was superior to treatment using is generally complete within 30 seconds to 2 minutes of
25% TCA, although an improvement in total lesions, TCA application; however, thicker epidermal growths
including both comedonal and inflammatory, occurred may require additional applications.2,9 Moreover, areas
3900 in 95% of patients on the salicylic acid–treated side of poor frosting may require careful reapplication of
(Fig. 213-5).14 Salicylic acid peels are also effective in the the peeling agent.3 At the completion of the peel, cool
Kang_CH213_p3895-3905.indd 3900 08/12/18 12:03 pm
Spectrum of superficial chemical peeling
31
Inflammatory Noninflammatory
Jessner Resorcinol Glycolic TCA Salicylic Acid
Figure 213-6 Spectrum of superficial chemical peeling. TCA, trichloroacetic acid.
saline compresses are placed on the skin. A bland High concentrations of TCA are used in the treat-
Chapter 213 :: Chemical Peels and Dermabrasion
emollient and sunscreen are then applied. Expected ment of atrophic scars in a procedure known as TCA
side effects include erythema, edema, and desquama- chemical reconstruction of skin scars (TCA CROSS). In
tion. Edema of the eyelids may be severe enough that it this procedure, first described by Lee and colleagues,
closes the lids. As the skin heals, erythema intensifies as TCA is applied with a sharp-tipped wooden applicator
desquamation comes to an end within 3 to 4 days. New pressed firmly against the base of the scar until a white
skin is evident within 6 to 7 days, and healing is com- frost is apparent. Because high concentrations (70% to
plete within 7 to 10 days. At this point, the erythema 100%) of TCA penetrate to the deep dermis, histologic
is reminiscent of a sunburn and is expected to resolve remodeling also occurs at this level. Such remodeling
within 3 to 4 weeks.9 TCA should be used cautiously in consists of dermal expansion with increased collagen
SPT IV to SPT VI. One should never “overcoat” TCA proliferation that results in elevation of depressed,
once the frosting is complete as accumulated TCA will atrophic scars.18,19 Agarwal and colleagues reported
produce a deeper peel (Fig. 213-7). successful use of 70% TCA applied with standard TCA
CROSS technique in the treatment of boxcar, rolling,
and ice pick scars in SPT IV and SPT V. In this study,
postinflammatory hyperpigmentation was reported
DEEP CHEMICAL PEELING but improved with time and use of “depigmenting”
creams; formation of keloids, persistent erythema, and
reactivation of herpes simplex virus were not seen.19
Deep chemical peels are indicated for deep rhytides
Medium-depth and deep peeling agents result in
and severe photoaging (Glogau categories III and IV)
significant inflammation and wounding within the
and include peeling agents such as Baker phenol.9 The
deep reticular dermis and heal with 4 characteristic
phenol is diluted to a concentration of 45% to 55% with
stages, including inflammation, coagulation, reepi-
croton oil, hexachlorophene, and water, and is referred
thelialization, and fibroplasia. Inflammation and
to as the Baker-Gordon phenol peel. Two variations, an
coagulation occur within hours of application of the
occluded and unoccluded, exist in clinical practice. In
peeling agent. Reepithelialization then begins on day
the occluded phenol peel, zinc oxide tape is placed over
3 and continues through days 10 to 14. Fibroplasia is
the skin after the peeling solution has been applied so
the last stage of the healing process and persists for
as to increase absorption. The unoccluded method,
3 to 4 months. This stage includes neoangiogenesis
described by McCollough, requires application of
and collagen proliferation.3 In a histologic and bio-
higher volumes of peeling solution; however, depth of
chemical analysis by Butler and colleagues, reorgani-
penetration is diminished as compared to the occluded
zation of dermal collagen and elastic fiber networks
technique. Both variations of the Baker-Gordon phenol
was prominently seen following 50% TCA and phenol
peel possess inherent risks and require monitoring and
peels.12 These dermal changes allow for the improve-
IV fluid administration because of potential cardiac,
ment in rhytides and other signs of photoaging seen
renal, and hepatic toxicities.3,16,17 Baker-Gordon deep
clinically following deep chemical peels.
chemical peeling is a more aggressive procedure with
inherent risks, but is the most permanent skin rejuve-
nation of all resurfacing procedures.
POSTOPERATIVE CARE
Following a chemical peel, patients are instructed to
cleanse the skin up to 4 times daily to prevent infec-
TABLE 213-5 tion and debride the necrotic exfoliation. Dilute 0.25%
Medium-Depth Wounding acetic acid (1 tablespoon vinegar in 1 pint water) is a
commonly recommended cleansing agent because of
■ Trichloroacetic acid (TCA) 50% its antibacterial action against Pseudomonas and other
■ Liquified phenol USP (U.S. Pharmacopoeia) 88% Gram-negative bacterial organisms.3,5,9 After cleans-
■ Solid carbon dioxide + TCA 35% to 50% ing, the skin is patted dry and a bland emollient is
■ Jessner solution + TCA
3901
applied.
Kang_CH213_p3895-3905.indd 3901 08/12/18 12:03 pm
31 COMPLICATIONS
Complications can occur either intraoperatively or
postoperatively.3 Intraoperative complications include,
but are not limited to, incorrect peel concentrations, use
of expired products, accidental solution misplacement,
and failure to properly neutralize the peel solution.
Such errors may be prevented with care taken to check
concentrations and dates of expiration. As removal of
intact peeling agent crystals from the storage bottle
may lead to higher concentrations placed on the skin,
the physician should pour the peeling solution into a
secondary container prior to initiation of the proce-
dure. Furthermore, solution should never be passed
Part 31
over the face or allowed to actively drip onto the skin.
Neutralizing solutions should be identified properly
(eg, sodium bicarbonate for glycolic acid peels) and
kept at the patient’s bedside for quick placement fol-
::
A
lowing completion of the peel.
Cosmetic Dermatology
Postoperative complications include infection (bac-
terial, viral, fungal), prolonged erythema, pruritus,
pigmentary alterations, contact dermatitis, milia/
acne, exacerbation of an underlying skin disease, and
scarring.3,9 Frequent postoperative visits and early
recognition of complications are critical, especially
for medium and deep chemical peels in which risks of
scarring are inherently higher. Delayed wound heal-
ing and persistent erythema are signs that skin is not
healing normally and are indicative of scarring poten-
tial. Delayed healing is evident with the appearance of
friable, stellate erosions on the skin at the time reepi-
thelialization is expected. As erosions may be indica-
tive of infectious etiologies, all such wounds should
be cultured. Erosions should be treated with artificial
wound dressings and topical or systemic corticoste-
roids.5 Persistent erythema is defined as erythema
lasting longer than 3 to 5 days for a superficial peel,
B
15 to 30 days for a medium-depth peel, and 60 to
90 days for a deep chemical peel.3 Etiologies include
underlying skin disorders such as rosacea and atopy,
contact dermatitis or sensitivity to the peeling agent,
and aggressive peeling techniques.20 Persistent ery-
thema should be treated promptly with topical and/
or systemic corticosteroids (Fig. 213-8).3,5,20
Postinflammatory hyperpigmentation and other
pigmentary dyschromias are more common in
SPT IV to SPT VI with medium and deep chemi-
cal peels presenting a greater risk than superficial
peels. Hyperpigmentation is also more common
Risk of scarring: medium and deep peeling
Intrinsic Operative Postoperative
Skin susceptible Overtreatment Infection
to overinjury with peel Trauma
C
Figure 213-7 Levels of frosting. A, Level I: erythema with Scarring
streaky frosting—superficial epidermal. B, Level II: white
3902 frosting with visible erythema—full-thickness epidermal.
C, Level III: white enamel frosting—epidermal or dermal. Figure 213-8 Risk of scarring: medium and deep peeling.
Kang_CH213_p3895-3905.indd 3902 08/12/18 12:03 pm
in individuals on hormonal therapies including
oral contraceptive pills and photosensitizing TABLE 213-6
31
medications.5 In general, superficial peels should be Manual vs Motorized Dermabrasion
elected in individuals with darker skin types. The
physician may recommend treatment with hydroqui- MANUAL DERMABRASION MOTORIZED DERMABRASION
none, with or without a retinoid, in the perioperative ■ Minimal cost of equipment, ■ High cost of machine; gas
period to minimize risks of hyperpigmentation.2,4,5 no maintenance, disposable sterilization of burrs and
Hypopigmentation, on the other hand, can be a com- ■ No aerosolization of blood fraises required; face shields,
plication associated with phenol peels. The resulting and infectious particles draping required
coloration of the skin is comparable to the natural ■ Difficult to perform in con- ■ Aerosolization of blood and
cavities (alar groove, nasola- infectious particles
appearance of sun-protected sites, such as the axillae
bial fold) ■ Specialized burr shapes pro-
and postauricular skin, and is directly proportional
■ Longer procedure time vide ease of use in smaller
to the amount of phenol applied.5 Deeper penetra- ■ Depending on material used, units or concavities
tion can efface the papillary dermis creating a much risk for granuloma formation ■ Shorter procedure time
Chapter 213 :: Chemical Peels and Dermabrasion
lighter appearance with an “alabaster” texture. if inadequate postprocedural ■ No risk for granuloma
cleaning formation
MECHANICAL Data from Gillard M, Wang T, Boyd C. Conventional diamond fraise vs
manual spot dermabrasion with drywall sanding screen for scars from
RESURFACING skin cancer surgery. JAMA Dermatol. 2002;138(8):1035-39.
PROCEDURES
MANUAL DERMASANDING
MICRODERMABRASION
Manual dermabrasion (Table 213-6), or dermasand-
Developed by Marini and Lo Brutto in 1985, micro- ing, uses sterile sandpaper of varying grades to
dermabrasion is a closed-system mechanical resur- ablate the epidermis and portions of the dermis.
facing procedure using abrasive aluminum oxide Two hundred or 400 grit-grade sandpaper wrapped
crystals to ablate the superficial epidermis.21-23 around gauze or a cotton-tipped applicator is used
The machine operates by discharging crystals onto to abrade the skin until punctate bleeding is evi-
the skin from a compression source. Crystals wound dent. This cost- and time-effective procedure is fre-
the superficial epidermis, removing keratinocytes quently elected for the treatment of surgical scars. A
and sebum, and are then returned to a waste con- split-scar study by Poulos and colleagues reported
tainer via vacuum suction. The ablative strength of improvement in the appearance of surgical scars,
the procedure is dependent on the strength of the particularly that of scar color and elevation, follow-
vacuum and contact time with the skin. Depth of ing manual dermabrasion performed 6 to 8 weeks
injury and clinical results are generally comparable postoperatively.26 It is important to rinse the abraded
to that of superficial chemical peels. Histologic inves- skin thoroughly to remove the silica-carbide crystals
tigation by Freedman and colleagues demonstrated as they can become imbedded in the skin and create
return of a “basket-weave” stratum corneum, thick- granulomas or tattoos (Fig. 213-9).
ening of the epidermis and dermis, and increased
collagen and elastic fibers following a series of
microdermabrasion treatments.24
Microdermabrasion is regarded as a safe procedure MOTORIZED
in most skin types. The procedure is well tolerated
and does not require anesthesia. Indications include DERMABRASION
enlarged pores, fine rhytides, mild photodamage, and
acne scarring. Multiple treatments are usually neces- Motorized dermabrasion (see Table 213-6) is a mechan-
sary to achieve appreciable clinical results. Side effects ical resurfacing technique in which handheld devices
are minimal and short-lived including erythema, using burrs of varying degrees of coarseness are used
petechiae/purpura, and tenderness. Complications to remove layers of the epidermis and/or dermis.25
such as persistent erythema, telangiectases, and postin- Biopsies of dermabraded skin demonstrate normaliza-
flammatory hyperpigmentation are uncommon; how- tion of the rete ridge pattern, increased type I collagen,
ever, microdermabrasion is best avoided in patients and increased elastic fibers.27,28
with underlying rosacea, and aggressive technique Motorized dermabrasion is indicated for moderate
should be discouraged in patients with SPT V and SPT to severe photodamage, including textural changes,
VI. Rare complications to the technician involve inha- rhinophyma, and scar revision. Patients with SPT IV
lation of the crystals and include pulmonary fibrosis to SPT VI should be treated cautiously because of the
and foreign-body granuloma, which are a result of the potential for postprocedural pigmentary alterations.
aluminum oxide crystals used in the procedure. To To minimize such risks, pretreatment and posttreat-
minimize such risks, eye protection and masks should ment with a topical retinoid or hydroquinone may be 3903
be worn by the operators.23,25 elected.
Kang_CH213_p3895-3905.indd 3903 08/12/18 12:03 pm
31 Manual dermasanding used in conjunction with medium-depth chemical peel
Sterile sandpaper dipped in water
×
l
Part 31
::
Cosmetic Dermatology
Figure 213-9 Manual dermasanding can be used in conjunction with medium-depth chemical peel to provide selective
deeper resurfacing.
Prior to the procedure, the treatment area is injected with wounding to the level of the reticular dermis. To
with local anesthesia. Regional nerve blocks also may be minimize the risk of adverse events including scarring,
done to improve patient comfort. For larger treatment treatment should never extend below the mid-reticular
areas, sedative medications and/or general anesthesia dermis (Fig. 213-10).
may be required. The physician and assistants should At the conclusion of the procedure, cool saline-
wear gowns and eye protection because of aerosoliza- soaked gauze is applied to the skin followed by appli-
tion of skin particles and blood during the procedure. cation of a bland emollient. The patient is instructed
The proper burr should then be selected for the to cleanse the treated skin with 0.25% acetic acid daily
treatment area and desired clinical result. Commonly- and keep the affected skin moist with a bland emollient
used burrs include diamond fraises and wire brushes. until reepithelialization has occurred at approximately
The physician is able to control the depth of destruc- 7 to 10 days. Ultraviolet radiation should be strictly
tion by means of the amount of pressure applied and avoided and broad-spectrum sunscreens should be
the selected speed of the dermabrader. Punctate bleed- applied daily. Healing generally occurs in 2 to 4 weeks
ing is indicative of wounding to the level of the pap- and postprocedural erythema is expected to resolve in
illary dermis while more confluent bleeding is seen 1 to 2 months.25
Surgical landmarks
Papillary dermis/capillary loops
Small red dots-fraise
Corn rows of bleeding-brush
Upper reticular dermis
Large red dots-fraise
White parallel lines in
collagen-brush
Mid-deep reticular dermis
Yellow globules-sebaceous
glands
Frayed collagen bundles
3904
Figure 213-10 Surgical landmarks.
Kang_CH213_p3895-3905.indd 3904 08/12/18 12:04 pm
CONCLUSIONS 12. Butler PE, Gonzalez S, Randolph MA, et al. Quantitative
and qualitative effects of chemical peeling on photo-
31
aged skin: an experimental study. Plast Reconstr Surg.
Chemical and mechanical resurfacing procedures
2001;107:222-228.
serve as effective treatments for a multitude of pig- 13. Grimes PE. The safety and efficacy of salicylic acid
mentary, textural, and photodamage-related concerns. chemical peels in darker racial-ethnic groups. Derma-
A vast variety of procedures exist, each targeting a spe- tol Surg. 1999;25:18.
cific depth of wounding and repair and each with its 14. Abdel Meguid AM, Elaziz Ahmed Attallah DA, Omar
own inherent risks and benefits. It is prudent for the H. Trichloroacetic acid versus salicylic acid in the
physician to have a broad knowledge base regarding treatment of acne vulgaris in dark-skinned patients.
these procedures so as to ensure treatment success and Dermatol Surg. 2015;41:1398-1404.
safeguard against untoward complications. Likewise, 15. Kubiak M, Mucha P, Debowska R, et al. Evaluation of
the proper selection of patients and choice of proce- 70% glycolic peels versus 15% trichloroacetic peels for
the treatment of photodamaged facial skin in aging
dure are critical. With appropriate usage, resurfacing
women. Dermatol Surg. 2014;40:883-891.
procedures can be a gratifying part of dermatologic 16. Alt TH. Occluded Baker-Gordon chemical peel: review
Chapter 213 :: Chemical Peels and Dermabrasion
practice. and update. J Dermatol Surg Oncol. 1989;15(9):980-993.
17. Landau M. Cardiac complications in deep chemical
peels. Dermatol Surg. 2007;33:190-193.
REFERENCES 18. Lee JB, Chung WG, Kwahck H, et al. Focal treatment of acne
scars with trichloroacetic acid: chemical reconstruction of
skin scars method. Dermatol Surg. 2002:28:1017-1021.
1. Brody HJ, Monheit GD, Resnik SS, et al. A history of 19. Agarwal N, Gupta LK, Khare AK, et al. Therapeutic
chemical peeling. Dermatol Surg. 2000;26:405-409. response of 70% trichloroacetic acid CROSS in atro-
2. Salam A, Dadzie OE, Galadari H. Chemical peeling in phic acne scars. Dermatol Surg. 2015;41:597-604.
ethnic skin: an update. Br J Dermatol. 2013;169:82-90. 20. Maloney BP, Millman B, Monheit G, et al. The etiology
3. Monheit GD. Chemical peels. Skin Therapy Lett. of prolonged erythema after chemical peel. Dermatol
2004;9(2):6-11. Surg. 1998;24:337-341.
4. Berson DS, Cohen JL, Rendon MI, et al. Clinical role and 21. Tsai R, Wang C, Chan H. Aluminum oxide crystal
application of superficial chemical peels in today’s microdermabrasion: a new technique for treating
practice. J Drugs Dermatol. 2009;8(9):803-811. facial scarring. Dermatol Surg. 1995;21:539-542.
5. Brody HJ. Complications of chemical resurfacing. 22. Bhalla M, Thami GP. Microdermabrasion: reappraisal
Dermatol Clin. 2001;19(3):427-438. and brief review of literature. Dermatol Surg. 2006;32:
6. Coleman WP III, Brody HJ. Advances in chemical peel- 809-814.
ing. Dermatol Clin. 1997;15(1):19-26. 23. Shim EK, Barnette D, Hughes K, et al. Microdermabra-
7. Brody HJ. Trichloroacetic acid application in chemical sion: a clinical and histopathologic study. Dermatol
peeling. Oper Tech Plast Reconstr Surg. 1995;2(2): Surg. 2001;27:524-530.
127-128. https://www.sciencedirect.com/science/ 24. Freedman BM, Rueda-Pedraza E, Waddell SP. The
article/pii/S1071094905800071 epidermal and dermal changes associated with micro-
8. Nelson BR, Fader DJ, Gillard M, et al. Pilot histologic and dermabrasion. Dermatol Surg. 2001;27:1031-1034.
ultrastructural study of the effects of medium-depth 25. Kim EK, Hovsepian RV, Mathew P, et al. Dermabrasion.
chemical facial peels on dermal collagen in patients Clin Plast Surg. 2011;38:391-395.
with actinically damaged skin. J Am Acad Dermatol. 26. Poulos E, Taylor C, Solish N. Effectiveness of derma-
1995;32(3):472-478. sanding (manual dermabrasion) on the appearance
9. Monheit GD. The Jessner’s + TCA peel: a medium- of surgical scars: a prospective, randomized, blinded
depth chemical peel. J Dermatol Surg Oncol. 1989;15(9): study. J Am Acad Dermatol. 2003;48:897-900.
945-950. 27. Benedetto AV, Griffin TD, Benedetto EA, et al.
10. Grimes PE. The safety and efficacy of salicylic acid Dermabrasion: therapy and prophylaxis of the photo-
peels in darker racial-ethnic groups. Dermatol Surg. aged face. J Am Acad Dermatol. 1992;27(3):439-447.
1999;25(1):18-22. 28. Nelson BR, Metz RD, Majmudar G, et al. A comparison
11. Ditre CM, Griffin TD, Murphy GF, et al. Effects of of wire brush and diamond fraise superficial
α-hydroxy acids on photoaged skin: a pilot clini- dermabrasion for photoaged skin. J Am Acad Derma-
cal, histological, and ultrastructural study. J Am Acad tol. 1996;34(2):235-243.
Dermatol. 1996;34:187-195.
3905
Kang_CH213_p3895-3905.indd 3905 08/12/18 12:04 pm
Das könnte Ihnen auch gefallen
- Textbook of Chemical PeelsDokument402 SeitenTextbook of Chemical PeelsHENDRIK20110% (1)
- Acne Scars Nu PDFDokument315 SeitenAcne Scars Nu PDFCristina Pop100% (2)
- Resurface and Peel Treatment TrainingDokument22 SeitenResurface and Peel Treatment Trainingamymonuskin100% (6)
- Electrical Units of MeasureDokument36 SeitenElectrical Units of MeasureHyung BaeNoch keine Bewertungen
- Aesthetic Injection: Dr. Ersje Retnowati, M.BiomedDokument53 SeitenAesthetic Injection: Dr. Ersje Retnowati, M.Biomedmohammad.irfanNoch keine Bewertungen
- Chemical Peels and Microdermabrasion PDFDokument9 SeitenChemical Peels and Microdermabrasion PDFKhiem Tran DuyNoch keine Bewertungen
- FOTONA New Skin Treatment Possibilities With Piano Mode On An Nd-YAGDokument11 SeitenFOTONA New Skin Treatment Possibilities With Piano Mode On An Nd-YAGLucia Regina Cavalcanti TeixeiraNoch keine Bewertungen
- The Art of Skin Peels Rhonda AllisonDokument182 SeitenThe Art of Skin Peels Rhonda Allisonmiichaz80% (5)
- Perioral RejuvenationDokument11 SeitenPerioral RejuvenationjuliemonneypennyNoch keine Bewertungen
- Systematic Approach to Non-Surgical Facial RejuvenationDokument4 SeitenSystematic Approach to Non-Surgical Facial RejuvenationEvieYoung67% (3)
- Acne Scars Classification and Treatment PDFDokument191 SeitenAcne Scars Classification and Treatment PDFMai Anh0% (1)
- CanulaDokument3 SeitenCanulaCatalina Soler Lioi100% (1)
- Understanding Thread Lifting (History)Dokument5 SeitenUnderstanding Thread Lifting (History)Anonymous LnWIBo1G100% (1)
- Melasma TreatmentDokument78 SeitenMelasma TreatmentRendy Adhitya PratamaNoch keine Bewertungen
- Illustrated Guide To Aesthetic BTX Injections - CH 4 - Estetik - Kort VariantDokument16 SeitenIllustrated Guide To Aesthetic BTX Injections - CH 4 - Estetik - Kort Variantbobocmihail0% (1)
- Aesthetic Treatments Around The EyesDokument6 SeitenAesthetic Treatments Around The Eyessavvy_as_98Noch keine Bewertungen
- TreadliftDokument39 SeitenTreadliftanggraini100% (4)
- Treatmentofageingskin 150319073717 Conversion Gate01Dokument85 SeitenTreatmentofageingskin 150319073717 Conversion Gate01Chyntia Giska100% (1)
- Complications of Thread Lift and How To Manage - Thread Protrusion, Infection, Dimpling and BruisingDokument4 SeitenComplications of Thread Lift and How To Manage - Thread Protrusion, Infection, Dimpling and BruisingAnonymous LnWIBo1G0% (1)
- Introductory Botulinum PresentationDokument113 SeitenIntroductory Botulinum Presentationprontaprintpottersbar100% (5)
- Rejuvenation MesotherapyDokument40 SeitenRejuvenation MesotherapyerlanggawidyaputriNoch keine Bewertungen
- Intense Pulsed Light (IPL) Treatment For The SkinDokument20 SeitenIntense Pulsed Light (IPL) Treatment For The SkinElaine MedeirosNoch keine Bewertungen
- Ulthera Facial Tightening Without SurgeryDokument3 SeitenUlthera Facial Tightening Without SurgeryChaojaNoch keine Bewertungen
- Vascular Complication of Injectable FillerDokument17 SeitenVascular Complication of Injectable Fillerahmed100% (1)
- Minimally Invasive Cosmetic Uses of Botulinum ToxinDokument28 SeitenMinimally Invasive Cosmetic Uses of Botulinum Toxineby_3tamaNoch keine Bewertungen
- A Practical Approach To Chemical PeelsDokument8 SeitenA Practical Approach To Chemical Peelsleenatalia93100% (2)
- Presentación Gama Mesohyal - en v1.1Dokument26 SeitenPresentación Gama Mesohyal - en v1.1Niculae Bogdan DimitrieNoch keine Bewertungen
- Mesotherapy by Institute BCN EnesfrDokument32 SeitenMesotherapy by Institute BCN Enesfrmarketing4558Noch keine Bewertungen
- Radiofrequency in Aesthetic MedicineDokument13 SeitenRadiofrequency in Aesthetic MedicineChristopher Schaa Gonzalez100% (1)
- Beautification and Rejuvenation With Botulinum Toxin InjectionDokument80 SeitenBeautification and Rejuvenation With Botulinum Toxin InjectionViniFortunata100% (1)
- Dermatrix - Radiofrequency Facial Rejuvenation Evidence-Based Effect IraildesDokument12 SeitenDermatrix - Radiofrequency Facial Rejuvenation Evidence-Based Effect IraildesTatiane MouraNoch keine Bewertungen
- Facial Lifting With Aptos ThreadsDokument9 SeitenFacial Lifting With Aptos ThreadsAlejandro Saldarriaga OchoaNoch keine Bewertungen
- Avoiding Dermal Filler Complications PDFDokument10 SeitenAvoiding Dermal Filler Complications PDFAndreas DilipidiNoch keine Bewertungen
- Skin Aging Fitz 9Dokument13 SeitenSkin Aging Fitz 9Jhauharina RfNoch keine Bewertungen
- Radiofrequency in Cosmetic DermatologyDokument12 SeitenRadiofrequency in Cosmetic DermatologyThe Vancouver Sun100% (2)
- Aubrey Debut ScriptDokument5 SeitenAubrey Debut ScriptKevin Jones CalumpangNoch keine Bewertungen
- Basic Model User'S ManualDokument4 SeitenBasic Model User'S ManualDokterYolanda100% (1)
- Superficial and Medium-Depth Chemical PeelsDokument10 SeitenSuperficial and Medium-Depth Chemical PeelsFenni Oktoberry100% (1)
- Microneedling Plus PRP Effective for Acne ScarsDokument7 SeitenMicroneedling Plus PRP Effective for Acne ScarsAcengHamudin100% (1)
- Chemical and Physical Peelings - Almeida Issa - 2017Dokument183 SeitenChemical and Physical Peelings - Almeida Issa - 2017sattwikaNoch keine Bewertungen
- Anti-Aging Therapeutics Volume XIVVon EverandAnti-Aging Therapeutics Volume XIVBewertung: 3 von 5 Sternen3/5 (1)
- Aesthetic 2Dokument100 SeitenAesthetic 2davidwee1987100% (1)
- Facial MesotherapyDokument3 SeitenFacial Mesotherapydanielagonzalezt5Noch keine Bewertungen
- Advanced Chemical Peels - Notes of InterstDokument4 SeitenAdvanced Chemical Peels - Notes of Interstgeraffe100% (3)
- MESOTHERAPYDokument39 SeitenMESOTHERAPYAtid Amanda100% (2)
- PDO&PCL Lifting Thread of Shandong Haidike PDFDokument8 SeitenPDO&PCL Lifting Thread of Shandong Haidike PDFhuyenthanh1807Noch keine Bewertungen
- Mesoglow y MesoliftDokument2 SeitenMesoglow y MesoliftPablo BaudinoNoch keine Bewertungen
- Tratment Melasma PDFDokument18 SeitenTratment Melasma PDFGheavita Chandra DewiNoch keine Bewertungen
- PDO Thread LiftsDokument2 SeitenPDO Thread LiftsDrekka Hanibal Putra33% (3)
- MESOTHERAPYDokument11 SeitenMESOTHERAPYimec_coordinator7353100% (3)
- Restylane Enhancing Natural BeautyDokument24 SeitenRestylane Enhancing Natural Beautympiegypt100% (2)
- Hair LaserDokument10 SeitenHair Laseriship pkmkenangaNoch keine Bewertungen
- State of The Art Penelitian - Chat GPT 2023Dokument137 SeitenState of The Art Penelitian - Chat GPT 2023restyNoch keine Bewertungen
- NitrocelluloseDokument7 SeitenNitrocellulosejumpupdnbdjNoch keine Bewertungen
- PepsicoDokument18 SeitenPepsicorahil virani0% (1)
- Dermapen Treatment Area GuideDokument2 SeitenDermapen Treatment Area GuideQiuyu ChenNoch keine Bewertungen
- Holistic Microneedling: The Manual of Natural Skin Needing and Derma Roller UseVon EverandHolistic Microneedling: The Manual of Natural Skin Needing and Derma Roller UseBewertung: 4.5 von 5 Sternen4.5/5 (3)
- 4D Ultrasonic Beauty Machine ManualDokument16 Seiten4D Ultrasonic Beauty Machine ManualAnam Ali75% (8)
- User Manual: (High Intensity Focused Ultrasound)Dokument11 SeitenUser Manual: (High Intensity Focused Ultrasound)Agha SoroushNoch keine Bewertungen
- Chemical Peeling IIDokument8 SeitenChemical Peeling IIAkindele O AdigunNoch keine Bewertungen
- Versant ModifiedDokument57 SeitenVersant ModifiedAryan Kharadkar100% (3)
- Poultry Disease Prevention and ControlDokument64 SeitenPoultry Disease Prevention and Controlsigra100% (3)
- Manual of Skin Surgery: A Practical Guide to Dermatologic ProceduresVon EverandManual of Skin Surgery: A Practical Guide to Dermatologic ProceduresBewertung: 1 von 5 Sternen1/5 (1)
- ACE Group Patient Leaflet Dermal FillersDokument9 SeitenACE Group Patient Leaflet Dermal FillersJim MackieNoch keine Bewertungen
- Phend Pharmaceuticals Double Blind Study Shows NATOX Cream Reduces Wrinkles Without Side EffectsDokument2 SeitenPhend Pharmaceuticals Double Blind Study Shows NATOX Cream Reduces Wrinkles Without Side EffectsLiliana LesuNoch keine Bewertungen
- Add A HeadingDokument3 SeitenAdd A HeadingJhauharina RfNoch keine Bewertungen
- Chapter 147:: Vascular Malformations:: Laurence M. Boon, Fanny BallieuxDokument33 SeitenChapter 147:: Vascular Malformations:: Laurence M. Boon, Fanny BallieuxJhauharina RfNoch keine Bewertungen
- Chapter 116:: Melanoma:: Jessica C. Hassel & Alexander H. EnkDokument36 SeitenChapter 116:: Melanoma:: Jessica C. Hassel & Alexander H. EnkJhauharina RfNoch keine Bewertungen
- Timeline ObatDokument2 SeitenTimeline ObatJhauharina RfNoch keine Bewertungen
- Versi Print Adaptive Immunity Dr. HannyDokument19 SeitenVersi Print Adaptive Immunity Dr. HannyJhauharina RfNoch keine Bewertungen
- Presentation 1Dokument1 SeitePresentation 1Jhauharina RfNoch keine Bewertungen
- GMsetDokument8 SeitenGMsetdilo001Noch keine Bewertungen
- Fatigue Life Prediction of A320-200 Aileron Lever Structure of A Transport AircraftDokument4 SeitenFatigue Life Prediction of A320-200 Aileron Lever Structure of A Transport AircraftMohamed IbrahimNoch keine Bewertungen
- Kerala Electricity Regulatory Commission Schedule of TariffDokument36 SeitenKerala Electricity Regulatory Commission Schedule of TariffvjtheeeNoch keine Bewertungen
- Ampersand MenuDokument5 SeitenAmpersand MenuJozefNoch keine Bewertungen
- Arta Fridei Kahlo A Fost Intotdeauna o ReactieDokument13 SeitenArta Fridei Kahlo A Fost Intotdeauna o ReactieAlta DaianNoch keine Bewertungen
- Termites and Microbial Biological Control StrategiesDokument30 SeitenTermites and Microbial Biological Control StrategiesMuhammad QasimNoch keine Bewertungen
- Nitocote WP DDokument4 SeitenNitocote WP DdaragNoch keine Bewertungen
- BiologyDokument21 SeitenBiologyHrituraj banikNoch keine Bewertungen
- 4 Ideal Models of Engine CyclesDokument23 Seiten4 Ideal Models of Engine CyclesSyedNoch keine Bewertungen
- MUCLecture 2021 10311889Dokument11 SeitenMUCLecture 2021 10311889Ramon Angelo MendezNoch keine Bewertungen
- Progressing Cavity Pump Overhaul GuideDokument5 SeitenProgressing Cavity Pump Overhaul Guidesdsds-54Noch keine Bewertungen
- Print Date:: Container No NO Size Seal No Seal Party Supplier Status Movement TypeDokument3 SeitenPrint Date:: Container No NO Size Seal No Seal Party Supplier Status Movement TypeYudha PermanaNoch keine Bewertungen
- Poultry DiseasesDokument5 SeitenPoultry DiseasesAnjum IslamNoch keine Bewertungen
- Khasi Community of MeghalayaDokument3 SeitenKhasi Community of MeghalayaMidhat FatimaNoch keine Bewertungen
- Shanidham - In-Shanidham Pacify Lord ShaniDokument3 SeitenShanidham - In-Shanidham Pacify Lord ShanisubramanyaNoch keine Bewertungen
- Is Revalida ExamDokument11 SeitenIs Revalida ExamRodriguez, Jhe-ann M.Noch keine Bewertungen
- Qand ADokument5 SeitenQand AJoshua PascasioNoch keine Bewertungen
- Abundance BlocksDokument1 SeiteAbundance BlockssunnyNoch keine Bewertungen
- Advanced Composite Materials Design EngineeringDokument19 SeitenAdvanced Composite Materials Design EngineeringpanyamnrNoch keine Bewertungen
- Palm Wine SpecificationDokument10 SeitenPalm Wine SpecificationUday ChaudhariNoch keine Bewertungen
- Cricothyroidotomy and Needle CricothyrotomyDokument10 SeitenCricothyroidotomy and Needle CricothyrotomykityamuwesiNoch keine Bewertungen
- True/False/Not Given Exercise 5: It Rains On The SunDokument2 SeitenTrue/False/Not Given Exercise 5: It Rains On The Sunyuvrajsinh jadejaNoch keine Bewertungen