Beruflich Dokumente
Kultur Dokumente
PCL Reconstruction Protocol
Hochgeladen von
RinainochanOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
PCL Reconstruction Protocol
Hochgeladen von
RinainochanCopyright:
Verfügbare Formate
Department of Rehabilitation Services
Physical Therapy
PCL Reconstruction Protocol
The intent of this protocol is to provide the clinician with a guideline for the post-
operative rehabilitation course of a patient that has undergone a PCL or PCL/ACL
reconstruction. It is by no means intended to be a substitute for one’s clinical decision-
making regarding the progression of a patient’s post-operative course based on their
exam findings, individual progress, and/or presence of post-operative complications. If a
clinician requires assistance in the progression of a post-operative patient, they should
consult with the referring surgeon.
GENERAL GUIDELINES
• No open chain hamstring work.
• Typically it takes 12 weeks for graft to bone healing time.
• Caution against posterior tibial translation (gravity, muscle action).
• Typically no CPM.
• PCL with posterolateral corner or LCL repair follows different post-op care (i.e.
crutches x 3 months).
• Resistance for hip PRE’s should be placed above the knee for hip abduction and
adduction; resistance may be placed distally for hip flexion.
• Supervised physical therapy generally takes place for 3-5 months post-
operatively.
GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING
Patients may begin the following activities at the dates indicated, unless otherwise
specified by the surgeon:
• Bathing/showering without brace (sponge bath only until suture removal)- 1 week
post-op.
• Typically patients can return to driving: 6-8 weeks post-op.
• Typically begin sleeping without brace: 8 weeks post-op.
• Full weight-bearing without assistive devices: 8 weeks post-op (with surgeon’s
clearance based on structural integrity of repair). The exception is PCL with
posterior lateral corner (PLC) or LCL repair, as above.
PCL Reconstruction Protocol 1
Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of
Rehabilitation Services. All rights reserved.
REHABILITATION PROGRESSION
PHASE I: Immediately post-operatively to week 4
Goals:
• Protect healing bony and soft tissue structures.
• Minimize the effects of immobilization:
o Early protected range of motion (protect against posterior tibial sagging).
o PRE’s for quadriceps, hip, and calf with an emphasis on limiting
patellofemoral joint compression and posterior tibial translation.
• Patient education for a clear understanding of limitations and expectations of the
rehabilitation process, and need for supporting proximal tibia/preventing sag.
Brace:
• 0-1 week: post-op brace locked in full extension at all times.
• At 1 week post-op, brace is unlocked for passive ROM performed by a physical
therapist or PT assistant.
• Technique for passive ROM is as follows:
o Patient supine; therapist maintains anterior pressure on proximal tibia as
knee is flexed (force on tibia is from posterior to anterior).
o For patients with combined PCL/ACL reconstructions, the above
technique is modified such that a neutral position of the proximal tibia is
maintained as the knee is flexed.
o It is important to prevent posterior sagging at all times.
Weight-bearing status:
• Weight-bearing as tolerated (WBAT) with crutches, brace locked in extension.
Special considerations:
• Position pillow under proximal posterior tibia at rest to prevent posterior tibial
sag.
Therapeutic exercises:
• Patellar mobilization.
• Quadriceps sets.
• Straight leg raise (SLR).
• Hip abduction and adduction.
• Ankle pumps.
• Hamstring and calf stretching.
• Calf press with exercise bands, progressing to standing calf raise with full knee
extension.
• Standing hip extension from neutral.
PCL Reconstruction Protocol 2
Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of
Rehabilitation Services. All rights reserved.
• Functional electrical stimulation (as needed for trace to poor quadriceps
contraction).
PHASE II: Post-operative weeks 4 to 12
Criteria for progression to Phase II:
• Good quadriceps control (good quad set, no lag with SLR).
• Approximately 60 degrees knee flexion.
• Full knee extension.
• No signs of active inflammation.
Goals:
• Increase ROM (particularly flexion).
• Normalize gait.
• Continue to improve quadriceps strength and hamstring flexibility.
Brace:
• 4-6 weeks: Brace unlocked for gait in controlled environment only (i.e. patient
may walk with brace unlocked while attending PT or when at home).
• 6-8 weeks: Brace unlocked for all activities.
• 8 weeks: Brace discontinued, as allowed by surgeon.
o Note, if PCL or LCL repair, continue brace until cleared by surgeon.
Weight-bearing status:
• 4-8 weeks: WBAT with crutches.
• 8 weeks: May discontinue crutches if patient demonstrates:
o No quadriceps lag with SLR.
o Full knee extension.
o Knee flexion 90-100 degrees.
o Normal gait pattern (May use 1 crutch/cane until gait normalized).
• If PLC or LCL repair, continue crutches for 12 weeks.
Therapeutic Exercises:
• 4-8 weeks:
o Wall slides/mini-squats (0-45 degrees).
o Leg press (0-60 degrees).
o Standing 4-way hip exercise for flexion, extension, abduction, adduction
(from neutral, knee fully extended).
o Ambulation in pool (work on restoration of normal heel-toe gait pattern in
chest-deep water).
• 8-12 weeks:
o Stationary bike (foot placed forward on pedal without use of toe clips to
minimize hamstring activity; seat set slightly higher than normal).
PCL Reconstruction Protocol 3
Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of
Rehabilitation Services. All rights reserved.
o Closed kinetic chain terminal knee extension using resisted band or weight
machine. Note: important to place point of resistance to minimize tibial
displacement.
o Stairmaster.
o Elliptical trainer.
o Balance and proprioception exercises.
o Seated calf raises.
o Leg press (0-90 degrees).
PHASE III: Post-operative months 3 to 9
Criteria for progression to Phase III:
• Full, painfree ROM. (Note: it is not unusual for flexion to be lacking 10-15
degrees for up to 5 months post-op.)
• Normal gait.
• Good to normal quadriceps control.
• No patellofemoral complaints.
• Clearance by surgeon to begin more concentrated closed kinetic chain
progression.
Goals:
• Restore any residual loss of motion that may prevent functional progression.
• Progress functionally and prevent patellofemoral irritation.
• Improve functional strength and proprioception using close kinetic chain
exercises.
• Continue to maintain quadriceps strength and hamstring flexibility.
Therapeutic exercises:
• Continue closed kinetic chain exercise progression.
• Treadmill walking.
• Jogging in pool with wet vest or belt.
• Swimming (no breaststroke or “frog kick”).
PHASE IV: Post-operative Month 9 until return to full activity
Criteria for progression to Phase IV:
• Clearance by surgeon to resume full or modified/partial activity (i.e. return to
work, recreational, or athletic activity).
• No significant patellofemoral or soft tissue irritation.
• Presence of necessary joint ROM, muscle strength and endurance, and
proprioception to safely return to athletic participation.
o Full, painfree ROM.
o Satisfactory clinical examination.
o Quadriceps strength 85% of uninvolved leg.
PCL Reconstruction Protocol 4
Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of
Rehabilitation Services. All rights reserved.
o Functional testing 85% of uninvolved leg.
o No change in laxity testing.
Goals:
• Safe and gradual return to work or athletic participation.
o This may involve sport-specific training, work hardening, or job
restructuring as needed.
o Patient demonstrates a clear understanding of their possible limitations.
• Maintenance of strength, endurance, and function.
Therapeutic exercises:
• Continue closed kinetic chain exercise progression.
• Cross-country ski machine.
• Sport-specific functional progression, which may include but is not limited to:
o Slide board.
o Jog/Run progression.
o Figure 8, carioca, backward running, cutting.
o Jumping (plyometrics).
• Work hardening program as indicated by physical therapist and/or surgeon
recommendation. Patient will need a referral from surgeon to begin work
hardening.
This protocol has been modified from Brotzman and Wilk, which has been published in
Brotzman SB, Wilk KE, Clinical Orthopaedic Rehabilitation. Philadelphia, PA: Mosby
Inc; 2003: 300-302.
Formatted by: Melissa Flak, PT 7/’06
PCL Reconstruction Protocol 5
Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of
Rehabilitation Services. All rights reserved.
Das könnte Ihnen auch gefallen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Entity-Level Controls Fraud QuestionnaireDokument8 SeitenEntity-Level Controls Fraud QuestionnaireKirby C. LoberizaNoch keine Bewertungen
- Plastique: Art and EducationDokument7 SeitenPlastique: Art and EducationJackStevensonNoch keine Bewertungen
- Elementary SurveyingDokument19 SeitenElementary SurveyingJefferson EscobidoNoch keine Bewertungen
- Attery: User Guide Dict Release 2020Dokument47 SeitenAttery: User Guide Dict Release 2020diegoNoch keine Bewertungen
- Johns Hopkins University Press Is Collaborating With JSTOR To Digitize, Preserve and Extend Access To ELHDokument13 SeitenJohns Hopkins University Press Is Collaborating With JSTOR To Digitize, Preserve and Extend Access To ELHAttila Lébényi-PalkovicsNoch keine Bewertungen
- Ministry of Truth Big Brother Watch 290123Dokument106 SeitenMinistry of Truth Big Brother Watch 290123Valentin ChirilaNoch keine Bewertungen
- Storey Publishing Fall 2017 CatalogDokument108 SeitenStorey Publishing Fall 2017 CatalogStorey PublishingNoch keine Bewertungen
- Southeast Asian Fabrics and AttireDokument5 SeitenSoutheast Asian Fabrics and AttireShmaira Ghulam RejanoNoch keine Bewertungen
- Ylarde vs. Aquino, GR 33722 (DIGEST)Dokument1 SeiteYlarde vs. Aquino, GR 33722 (DIGEST)Lourdes Loren Cruz67% (3)
- PED100 Mod2Dokument3 SeitenPED100 Mod2Risa BarritaNoch keine Bewertungen
- Parwati DeviDokument25 SeitenParwati DevikvntpcsktprNoch keine Bewertungen
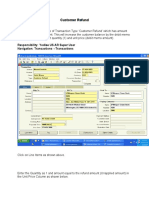
- Customer Refund: Responsibility: Yodlee US AR Super User Navigation: Transactions TransactionsDokument12 SeitenCustomer Refund: Responsibility: Yodlee US AR Super User Navigation: Transactions TransactionsAziz KhanNoch keine Bewertungen
- Rediscovering The True Self Through TheDokument20 SeitenRediscovering The True Self Through TheManuel Ortiz100% (1)
- Defending A Dogma: Between Grice, Strawson and Quine: Elvis ImafidonDokument10 SeitenDefending A Dogma: Between Grice, Strawson and Quine: Elvis ImafidonYang Wen-LiNoch keine Bewertungen
- International Conference On Basic Science (ICBS)Dokument22 SeitenInternational Conference On Basic Science (ICBS)repositoryIPBNoch keine Bewertungen
- TLS FinalDokument69 SeitenTLS FinalGrace Arthur100% (1)
- Modelling of Short Duration Isopluvial Map For Raichur District KarnatakaDokument4 SeitenModelling of Short Duration Isopluvial Map For Raichur District KarnatakaMohammed Badiuddin ParvezNoch keine Bewertungen
- Bossa Nova Book PDFDokument5 SeitenBossa Nova Book PDFschmimiNoch keine Bewertungen
- Full Download Social Animal 14th Edition Aronson Test BankDokument35 SeitenFull Download Social Animal 14th Edition Aronson Test Banknaeensiyev100% (32)
- SAP CRM Tax ConfigurationDokument18 SeitenSAP CRM Tax Configurationtushar_kansaraNoch keine Bewertungen
- Different Departments Required in A HospitalDokument11 SeitenDifferent Departments Required in A HospitalEdsel Dudes AbanteNoch keine Bewertungen
- Registration - No Candidate Gender Category Rank/Percentage Allotment - Seat Base - Seat Course CollegeDokument166 SeitenRegistration - No Candidate Gender Category Rank/Percentage Allotment - Seat Base - Seat Course CollegeCyber ParkNoch keine Bewertungen
- Oedogonium: Class: Chlorophyceae Order: Oedogoniales Family: OedogoniaceaeDokument28 SeitenOedogonium: Class: Chlorophyceae Order: Oedogoniales Family: OedogoniaceaeA SASIKALANoch keine Bewertungen
- Introduction To Sociology ProjectDokument2 SeitenIntroduction To Sociology Projectapi-590915498Noch keine Bewertungen
- Strategi Pencegahan Kecelakaan Di PT VALE Indonesia Presentation To FPP Workshop - APKPI - 12102019Dokument35 SeitenStrategi Pencegahan Kecelakaan Di PT VALE Indonesia Presentation To FPP Workshop - APKPI - 12102019Eko Maulia MahardikaNoch keine Bewertungen
- Donna Claire B. Cañeza: Central Bicol State University of AgricultureDokument8 SeitenDonna Claire B. Cañeza: Central Bicol State University of AgricultureDanavie AbergosNoch keine Bewertungen
- Radiography Safety ProcedureDokument9 SeitenRadiography Safety ProcedureأحمدآلزهوNoch keine Bewertungen
- OrthoDokument22 SeitenOrthosivaleela gNoch keine Bewertungen
- Challenges Faced by Freight Forwarders in Their Operations in Chennai City, Tamil NaduDokument3 SeitenChallenges Faced by Freight Forwarders in Their Operations in Chennai City, Tamil NaduNiraj KasbeNoch keine Bewertungen
- Su Jok, Twist Therapy AND Smile MeditationDokument7 SeitenSu Jok, Twist Therapy AND Smile MeditationprateekNoch keine Bewertungen