Beruflich Dokumente
Kultur Dokumente
Dyshidrotic Eczema PDF
Hochgeladen von
blacklist16Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Dyshidrotic Eczema PDF
Hochgeladen von
blacklist16Copyright:
Verfügbare Formate
Research Article www.enlivenarchive.
org Enliven: Pediatrics and Neonatal Biology
Dyshidrotic Eczema
Alexander K. C. Leung1*, Benjamin Barankin2, and Kam Lun Hon3
Clinical Professor of Pediatrics, University of Calgary, Pediatric Consultant, Alberta Children’s Hospital
1
Medical Director and Founder, Toronto Dermatology Centre
2
Professor of Pediatrics, Chinese University of Hong Kong
3
*
Corresponding author: Alexander K. C. Leung, MBBS, FRCPC, FRCP Citation: Leung AK, Barankin B, Hon KL (2014) Dyshidrotic Eczema.
(UK & Irel), FRCPCH, FAAP, Clinical Professor of Pediatrics, University Enliven: Pediatr Neonatol Biol 1(1): 002.
of Calgary, Pediatric Consultant, Alberta Children’s Hospital, Canada, Tel:
Copyright:@ 2014 Dr. Alexander K. C. Leung. This is an Open Access
(403) 230-3322; Fax: (403) 230-3322; E-mail: aleung@ucalgary.ca
article published and distributed under the terms of the Creative Commons
Received Date: 14th August 2014 Attribution License, which permits unrestricted use, distribution and
Accepted Date: 10th September 2014 reproduction in any medium, provided the original author and source are
Published Date: 16th September 2014 credited.
Abstract
Dyshidrotic eczema, also known as dyshidrotic dermatitis or pompholyx, is characterized by pruritic, tense, deep-seated vesicles mainly on the
palms and lateral surfaces of the fingers. In the chronic phase, scaling, desquamation, fissuring, and, sometimes, lichenification may be seen. The
peak age of onset is between 20 and 30 years of age. The sex incidence is approximately equal. Most cases are idiopathic. Predisposing factors
include atopy, contact allergens, contact irritants, dermatophyte infection, allergy to ingested metal, hyperhidrosis, prolonged use of protective gloves,
intravenous immunoglobulin, psychological stress, and smoking. Although the disease is benign, it tends to run a chronic and relapsing course.
Successful treatment requires a systemic multipronged approach that consists of avoidance of triggering factors, optimal skin care, pharmacotherapy
during acute exacerbations, and education of patients/caregivers. Ultrapotent topical corticosteroids are the mainstay of pharmacotherapy.
Keywords
Dyshidrotic eczema; Dyshidrotic dermatitis; Pompholyx; Pruritic vesicles; Palms; Fingers; Relapsing; Corticosteroids
Introduction Epidemiology
Dyshidrotic eczema, also known as dyshidrotic dermatitis or pompholyx, The prevalence of hand dermatitis varies from 2 to 8.9% of the general
is characterized by pruritic, tense, deep-seated vesicles mainly on the population [3]. Dyshidrotic eczema accounts for 5 to 20% of all cases of
palms and lateral surfaces of the fingers [1]. The term “dyshidrosis” (Greek, hand dermatitis [4,5]. In one population study, the one-year prevalence
hidrosis meaning sweat) was coined by Fox in 1873 to describe a blistering of dyshidrotic eczema was estimated to be 0.5% [6]. Although dyshidrotic
disease of the palms and soles, presumably due to a disorder of the sweat eczema occurs worldwide, it is less common among Asians [7,8]. The
glands [2]. The term “dyshidrosis” is a misnomer as it is now recognized condition is more common in hot weather [9]. The peak age of onset
that the condition has nothing to do with dysfunction of the sweat glands. is between 20 and 30 years of age [3]. Onset before 10 years of
age is unusual [5]. The sex incidence is approximately equal [5].
Enliven Archive | www.enlivenarchive.org 1 2014 | Volume 1 | Issue 1
Etiology and Pathogenesis Diagnosis and Differential Diagnosis
The exact etiology is not known. Most cases are idiopathic. Factors The diagnosis is mainly clinical based on a detailed history and the appearance
that may predispose to the development of dyshidrotic eczema in a of the rash. Differential diagnosis includes allergic contact dermatitis (can be
susceptible individual include atopy, contact allergens, contact irritants, determined by patch testing to various contactants), irritant contact dermatitis
dermatophyte infection, allergy to ingested metal (in particular, nickel and (typically over-washing, using harsh soaps and/or insufficient moisturizing) ,
cobalt), hyperhidrosis, prolonged use of protective gloves, intravenous and atopic hand dermatitis (typically a family or personal history of eczema,
immunoglobulin, psychological stress, and smoking [4,8,10-12]. Most cases asthma, and/or hay fever) most commonly; much less commonly, the differential
are sporadic. Rarely, an autosomal dominant mode of inheritance has been would include epidermolysis bullosa simplex, bullous impetigo, herpes
described [5]. A gene locus on chromosome 18q22.1-18q22.3 was identified infection, id reaction, linear IgA disease, dyshidrotic tinea, dyshidrosiform
in a large Chinese family with 14 affected individuals through 4 generations [5]. pemphigoid, pemphigus vulgaris, fixed drug eruption, acropustulosis
of infancy, hand-foot-mouth disease, pustular psoriasis, palmoplantar
pustulosis, secondary syphilis, and acrodermatitis enteropathica [8,12].
Histopathology
In the acute phase, histologic features include intraepidermal spongiosis
with vesicle formation and a superficial perivascular inflammatory infiltrate
Complications
composed mainly of lymphocytes and histiocytes [3,4,11,12]. In the Dyshidrotic eczema has a significant negative impact on the
more chronic phase, there are multiple foci of parakeratosis, acanthosis, quality of life due to the severe pruritus [5,9]. Secondary bacterial
irregular epidermal hyperplasia with minimal or absent spongiosis [3,4,12]. infection, especially with Staphylococcus aureus, is not uncommon
The epidermis is thick and the overlying horny layer is even thicker [8]. [4]. Nail dystrophy may result if the nail matrix is affected [4].
Clinical Manifestations
Clinically, acute dyshidrotic eczema presents with a sudden outbreak of
Prognosis
deep-seated “tapioca-like” vesicles and, less commonly, bullae that affect Although the disease is benign, it tends to run a chronic and relapsing
primarily the palms and lateral surfaces of the fingers [1,9]. The eruption course [3]. The condition tends to be less severe and recurs less often with
may also occur on the soles of the feet. In approximately 80% of cases, age [4]. Most patients eventually outgrow the condition [4].
only the hands are affected [4]. The eruption is usually symmetrical and
pruritic [1]. Some patients experience pain and/or a burning sensation
[1]. In the chronic phase, scaling, desquamation, fissuring, and, Management
sometimes, lichenification may be seen [1]. The condition is typically Dyshidrotic eczema is often difficult to treat, possibly because of the thick
recurrent and both the acute and chronic phases can coexist (Figure 1). epidermis with a compact stratum corneum and richness of the sweat glands
of the affected skin. Successful treatment requires a systemic multipronged
approach that consists of avoidance of triggering factors, optimal skin care,
pharmacotherapy during acute exacerbations, and education of patients/
caregivers.
Soaps and detergents should be avoided as much as possible [13]. The hands
should be washed with lukewarm (not hot) water and soap free cleansers.
Emotional stress often exacerbates the skin lesions of atopic dermatitis.
If avoidance is not possible, coping mechanisms should be tried [13].
Hydration of the skin helps to improve the dryness and pruritus and restore
the disturbed skin’s barrier function. As such, hydration of the skin is of
paramount importance both in the prevention and management of dyshidrotic
eczema. A moisturizer or emollient should be applied as soon as possible after
hand-washing to prevent evaporation of water and to keep the skin soft and
Figure 1: A 3-year-old girl with dyshidrotic eczema presenting with flexible. In general, ointments are most effective but messy; creams are often
vesicles on the palms and scaling patches with crusts and fissures on better tolerated. The type of moisturizer or emollient should be tailored to the
the fingers.
individual skin conditions as well as the child’s needs and preferences [13].
Enliven Archive | www.enlivenarchive.org 2 2014 | Volume 1 | Issue 1
Ultrapotent topical corticosteroids are the mainstay of therapy. Topical 4. Adams DR, Marks JG (2014) Acute palmplantar eczema (dyshidrotic
corticosteroids should not be applied more than twice a day; frequent eczema). In: Post TW, ed. Up To Date. Waltham, MA.
use does not improve efficacy and increase the risk of side effects [14]. 5. Chen JJ, Liang YH, Zhou FS, Yang S, Wang J, et al. (2006) The gene
Topical immunomodulators such as tacrolimus and pimecrolimus are not for a rare autosomal dominant form of pompholyx maps to chromosome
as fast or effective as ultrapotent topical corticosteroids in the treatment of 18q22.1-18q22.3. J Invest Dermatol 126: 300-304.
this skin condition, although they can be considered in the maintenance 6. Meding B, Swanbeck G (1989) Epidemiology of different types of hand
phase of treatment [4]. Both topical steroids and immunomodulators are eczema in an industrial city. Acta Derm Venereol 69: 227-233.
commonly and safely used in children [4]. Systemic corticosteroids should
7. Lee CS, Lim HW (2003) Cutaneous diseases in Asians. Dermatol Clin
be reserved for recalcitrant cases and used for the shortest time possible
21: 668-677.
(typically 1 week or so) while awaiting response to other therapies. Other
immunosuppressants such as cyclosporine, azathioprine, and methrotrexate 8. Wollina U (2010) Pompholyx: a review of clinical features, differential
have occasionally be used for recalcitrant and severe cases unresponsive diagnosis, and management. Am J Clin Dermatol 11: 305-314.
to the above measures, but with variable success, and typically not in 9. Abreu-Velez AM, Pinto FJ Jr, Howard MS (2009) Dyshidrotic eczema:
children [8]. These immunosuppressants all have potential adverse effects, relevance to the immune response in situ. N Am J med Sci 1: 117-120.
requiring careful monitoring and restricting their clinical usefulness [13]. 10. Markantoni V, Kouris A, Armyra K, Vavouli C, Kontochristopoulos G
Psoralen plus ultraviolet A (PUVA), UVA1 and UVB have been shown to be (2014) Remarkable improvement of relapsing dyshidrotic eczema after
effective and may be considered in the treatment of refractory cases in older treatment of coexistant hyperhidrosis with oxybutynin. Dermatol Ther
children [8]. Narrow-band UVB is most commonly used. More recently, oral Doi: 10.1111/dth. 12514.
alitretinoin has been shown to be effective for recurrent and refractory cases 11. Shiraishi T, Yamamoto T (2013) Severe dyshidrotic eczema after
of this condition in adults. The response rate is approximately 50% [15]. intravenous immunoglobulin therapy for Kawasaki syndrome. Pediatr
Dermatol 30: e30-e31.
Intradermal botulinum toxin A has also been tried with some success in 12. Yoon SY, Park HS, Lee JH, Cho S (2013) Histological and differentiation
patients with concomitant hyperhidrosis [16]. The medication has potent between palmplantar pustulosis and pompholyx. J Eur Acad Dermatol
antihidrotic activity [16]. Since hyperhidrosis is an aggravating factor, Venereol 27: 889-893.
treatment of hyperhidrosis may lead to regression of the disorder. The 13. Leung AK, Hon KL (2011) Atopic Dermatitis: A Review for the Primary
drawback is the need for repeated injections approximately every 6 Care Physician. New York: Nova Science Publishers 1-113.
months. This is rarely used in children because of the pain involved. 14. Baumer JH (2008) Atopic eczema in children, NICE. Arch Dis Child
Educ Pract Ed 93: 93-97.
Although pruritus in dyshidrotic eczema does not appear to be mediated by 15. Ruzicka T, Lynde CW, Jemec GB, Diepgen T, Berth-Jones J, et
histamine release, oral antihistamines can provide symptomatic relief because al. (2008) Efficacy and safety of oral alitretinoin (9-cis retinoic acid)
of their sedative properties and may be effective for intense pruritus refractory in patients with severe chronic hand eczema refractory to topical
to moisturizers and conservative measures. Of the H1 antihistamines, corticosteroids: results of a randomized, double-blind, placebo-
hydroxyzine is more effective than diphenhydramine and cyproheptadine [13]. controlled, multicentre trial. Br J Dermatol 158: 808-817.
16. Kontochritopoulos G, Gregoriou S, Agiasofitou G, Nikolakis G,
Rigopoulos D, et al. (2007) Regression of relapsing dyshidrotic eczema
Patient/caregivers education and support are vital in the management of
after treatment of concomitant hyperhidrosis with botulinum toxin-A.
dyshidrotic eczema. Misinformation may be detrimental to disease control.
Dermatol Surg 33:1289-1290.
Steroid fear or phobia among patients/caregivers is common and is a
17. Hon KL, Kam WY, Leung TF, Lam MC, Wong KY, et al. (2006) Steroid
significant factor in suboptimal use or non-compliance to treatment [17]. Poor
compliance is a major reason for treatment failure. Patients and caregivers fears in children with eczema. Acta Paediatr 95: 1451-1455.
should be reassured that topical corticosteroids are safe and effective with
their sensible use and they remain first-line treatment for acute flares [17].
Reference
1. Brazzelli V, Grassi S, Savasta S, Ruffinazzi G, Carugno A, et al. (2014) Submit your manuscript at
Pompholyx of the hands after intravenous immunoglobulin therapy for http://enlivenarchive.org/submit-manuscript.php
clinically isolated syndrome: a paediatric case. Int J Immunopathol New initiative of Enliven Archive
Pharmacol 27: 127-130. Apart from providing HTML, PDF versions; we also provide video
2. Fox T (1873) Clinical lecture on Dyshidrosis: an undescribed eruption. version and deposit the videos in about 15 freely accessible social
Br Med J 2: 365-366. network sites that promote videos which in turn will aid in rapid
circulation of articles published with us.
3. Nezafati KA, Cruz P (2014) Dyshidrotic dermatitis. In: Heyman
WR, Anderson BE, Hivnor C, et al, eds. Clinical Decision Support:
Dermatology. Wilmington, Delaware: Decision Support in Medicine,
LLC, electronic database.
Enliven Archive | www.enlivenarchive.org 3 2014 | Volume 1 | Issue 1
Das könnte Ihnen auch gefallen
- Dyshidrotic Eczema: January 2014Dokument4 SeitenDyshidrotic Eczema: January 2014Strawberry ShortcakeNoch keine Bewertungen
- Canine Demodicosis - TPIDokument3 SeitenCanine Demodicosis - TPIDeepak CNoch keine Bewertungen
- 334-Article Text-1213-1-10-20160514Dokument7 Seiten334-Article Text-1213-1-10-20160514Balakrishna GopinathNoch keine Bewertungen
- EczemaDokument39 SeitenEczemakamardin zakuaniNoch keine Bewertungen
- 1476 ArticleText 6472 1 10 20100118 PDFDokument6 Seiten1476 ArticleText 6472 1 10 20100118 PDFJayantiNoch keine Bewertungen
- A Clinico-Epidemiological Study On Palmoplantar DermatosesDokument8 SeitenA Clinico-Epidemiological Study On Palmoplantar DermatosesIJAR JOURNALNoch keine Bewertungen
- Acral Manifestations of Fungal InfectionsDokument21 SeitenAcral Manifestations of Fungal InfectionsanwarNoch keine Bewertungen
- Hand EczemaDokument12 SeitenHand EczemaMario RodriguezySilvaNoch keine Bewertungen
- Atopic Dermatitis - WikipediaDokument10 SeitenAtopic Dermatitis - WikipediaABHINABA GUPTANoch keine Bewertungen
- D. Diaper 1Dokument4 SeitenD. Diaper 1Merinda Ajeng Arum PratiwiNoch keine Bewertungen
- PDF DocumentDokument4 SeitenPDF DocumentAditya Yudha PratamaNoch keine Bewertungen
- Laporan Pendahuluan DermatitisDokument18 SeitenLaporan Pendahuluan DermatitisIRGZI AULIAHAQNoch keine Bewertungen
- Plants Used To Treat Skin Diseases - ReviewDokument9 SeitenPlants Used To Treat Skin Diseases - ReviewPsicólogo Clinico clinicoNoch keine Bewertungen
- Management of Tinea Corporis, Tinea Cruris, and Tinea Pedis: A Comprehensive ReviewDokument19 SeitenManagement of Tinea Corporis, Tinea Cruris, and Tinea Pedis: A Comprehensive ReviewYovitaNoch keine Bewertungen
- Topical Treatment of Common Superficial Tinea InfectionsDokument8 SeitenTopical Treatment of Common Superficial Tinea InfectionsColate LocoNoch keine Bewertungen
- Demodicosis in Different Age Groups and AlternativDokument23 SeitenDemodicosis in Different Age Groups and AlternativJuliana FreitasNoch keine Bewertungen
- Contact Dermatitis: Key PointsDokument8 SeitenContact Dermatitis: Key Pointssaimon reyNoch keine Bewertungen
- Penatalaksanaan Dermatitis AtopicDokument13 SeitenPenatalaksanaan Dermatitis AtopicDini MayrisdayaniNoch keine Bewertungen
- Bercak MerahDokument16 SeitenBercak MerahFary SatriadiNoch keine Bewertungen
- Eczema & Psoriasis: Dr. MburuDokument69 SeitenEczema & Psoriasis: Dr. MburuKeith OmwoyoNoch keine Bewertungen
- DermatitisDokument5 SeitenDermatitisAzriatul Farahain Ahmad ZamiliNoch keine Bewertungen
- Dermatitis Clinical Case Presentation OutlineDokument6 SeitenDermatitis Clinical Case Presentation OutlineSamson, Arielle Cate D.Noch keine Bewertungen
- Synopsis of Causation: Dermatitis (Eczema) Including Occupational DermatitisDokument19 SeitenSynopsis of Causation: Dermatitis (Eczema) Including Occupational DermatitisCcNoch keine Bewertungen
- Managing Athlete's FootDokument5 SeitenManaging Athlete's FootCharlesMahonoNoch keine Bewertungen
- Dyshidrotic Eczema: BackgroundDokument5 SeitenDyshidrotic Eczema: BackgroundHiedajatNoch keine Bewertungen
- د. هالة Dermatitis-1 (Muhadharaty)Dokument7 Seitenد. هالة Dermatitis-1 (Muhadharaty)adwNoch keine Bewertungen
- Treatment of Atopic Dermatitis (Eczema) - UpToDateDokument70 SeitenTreatment of Atopic Dermatitis (Eczema) - UpToDateKarla Alejandra BriseñoNoch keine Bewertungen
- 004 - Pyoderma. Scabies. PediculosisDokument33 Seiten004 - Pyoderma. Scabies. PediculosisLucas Victor AlmeidaNoch keine Bewertungen
- Complete Medical Guide for Disease Volume VII; Atopic DermatitisVon EverandComplete Medical Guide for Disease Volume VII; Atopic DermatitisNoch keine Bewertungen
- Dermatographic Urticaria - WikipediaDokument5 SeitenDermatographic Urticaria - WikipediaTeeNoch keine Bewertungen
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraDokument6 SeitenTinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraIsni KhoirunisaNoch keine Bewertungen
- S0733 8635 2803 2900032 920160621 22881 1su0moo With Cover Page v2Dokument33 SeitenS0733 8635 2803 2900032 920160621 22881 1su0moo With Cover Page v2Alfian DjaafaraNoch keine Bewertungen
- Eczema, UrticariaDokument72 SeitenEczema, Urticariaamberwinthrop100% (1)
- Eczema, Psoriasis, Cutaneous Infections, Acne, and Other Common Skin DisordersDokument6 SeitenEczema, Psoriasis, Cutaneous Infections, Acne, and Other Common Skin DisordersElrey InocianNoch keine Bewertungen
- Role of Homoeopathic Medicines in Tinea Corporis: A Case StudyDokument4 SeitenRole of Homoeopathic Medicines in Tinea Corporis: A Case StudySandip VaghelaNoch keine Bewertungen
- AdrianDokument3 SeitenAdrianJohn David ZabalaNoch keine Bewertungen
- Perioral Dermatitis 2011Dokument5 SeitenPerioral Dermatitis 2011Hamza Abu HumaidNoch keine Bewertungen
- Athlete's Foot (Tinea Pedis) : Dr. Partha Pratim PalDokument2 SeitenAthlete's Foot (Tinea Pedis) : Dr. Partha Pratim PalBear FamilyNoch keine Bewertungen
- Contact Dermatitis in ChildrenDokument6 SeitenContact Dermatitis in ChildrenYogi SanjayaNoch keine Bewertungen
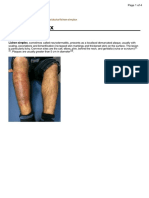
- Lichen Simplex: AppearanceDokument4 SeitenLichen Simplex: AppearanceTripser LockyNoch keine Bewertungen
- Antifungal DrugsDokument16 SeitenAntifungal DrugsAmrinder SagguNoch keine Bewertungen
- Irritant Contact Dermatitis: Practice EssentialsDokument4 SeitenIrritant Contact Dermatitis: Practice EssentialsHiedajatNoch keine Bewertungen
- Ccid 11 175Dokument11 SeitenCcid 11 175Remo Alnovryanda PutraNoch keine Bewertungen
- Atopic Dermatitis: (Infantile and Childhood Eczema)Dokument17 SeitenAtopic Dermatitis: (Infantile and Childhood Eczema)Ageededin HartNoch keine Bewertungen
- 2003, Vol.21, Issues 3, Antifungal TherapyDokument186 Seiten2003, Vol.21, Issues 3, Antifungal TherapyRizweta DestinNoch keine Bewertungen
- Jurnal Reading DADokument18 SeitenJurnal Reading DAWinendy Deo HaryantoNoch keine Bewertungen
- Eczema and DermatitisDokument47 SeitenEczema and DermatitisDeborah ChemutaiNoch keine Bewertungen
- ErythrodermaDokument48 SeitenErythrodermaShwan OmarNoch keine Bewertungen
- Fungal InfectionsDokument9 SeitenFungal InfectionsCoral Srinivasa RamaluNoch keine Bewertungen
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Dokument7 SeitenTinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Dicky KurniawanNoch keine Bewertungen
- Impetigo in Children: A Clinical Guide and Treatment OptionsDokument2 SeitenImpetigo in Children: A Clinical Guide and Treatment OptionsBeuty SavitriNoch keine Bewertungen
- Dermatology Primer: Selected Skin Diseases and Treatment Tailored For The Athletic TrainerDokument64 SeitenDermatology Primer: Selected Skin Diseases and Treatment Tailored For The Athletic TrainerSilviu100% (1)
- Scientific Revolution in Ayurveda!: Dyshidrotic Eczema: A PerspectiveDokument7 SeitenScientific Revolution in Ayurveda!: Dyshidrotic Eczema: A PerspectiveDwitiara SeptianiNoch keine Bewertungen
- Contact DermatitisDokument2 SeitenContact DermatitisMIR SARTAJNoch keine Bewertungen
- Dermatitis Numularis PDFDokument3 SeitenDermatitis Numularis PDFRiska Permata SariNoch keine Bewertungen
- Chronic DermatophytosisDokument4 SeitenChronic DermatophytosisLiana BegNoch keine Bewertungen
- Dermatitis and Eczema: Ailing Zou (邹爱玲) 2021.10.18Dokument31 SeitenDermatitis and Eczema: Ailing Zou (邹爱玲) 2021.10.18AmeliaNoch keine Bewertungen
- Tinea Pedis - An Update: September 2011Dokument6 SeitenTinea Pedis - An Update: September 2011Disty Aldilla WicaksonoNoch keine Bewertungen
- RingwormDokument7 SeitenRingwormSAMSON, MAXZENE ANICKANoch keine Bewertungen
- School: Sta. Maria Integrated School Group No. Names: Energy Forms & Changes Virtual LabDokument3 SeitenSchool: Sta. Maria Integrated School Group No. Names: Energy Forms & Changes Virtual LabNanette Morado0% (1)
- Carotenoids-Birkhäuser Basel (1971)Dokument934 SeitenCarotenoids-Birkhäuser Basel (1971)feghbalibNoch keine Bewertungen
- GEC PE 3 ModuleDokument72 SeitenGEC PE 3 ModuleMercy Anne EcatNoch keine Bewertungen
- Level 9 - Unit 34Dokument7 SeitenLevel 9 - Unit 34Javier RiquelmeNoch keine Bewertungen
- RA 9344 (Juvenile Justice and Welfare Act)Dokument10 SeitenRA 9344 (Juvenile Justice and Welfare Act)Dan RamosNoch keine Bewertungen
- EV-H-A1R 54C - M - EN - 2014 - D - Heat Detector SalwicoDokument2 SeitenEV-H-A1R 54C - M - EN - 2014 - D - Heat Detector SalwicoCarolinaNoch keine Bewertungen
- Eim s2000 Series Brochure PDFDokument16 SeitenEim s2000 Series Brochure PDFHumbertoOtaloraNoch keine Bewertungen
- Air Pollution Emissions 2008-2018 From Australian Coal Mining: Implications For Public and Occupational HealthDokument11 SeitenAir Pollution Emissions 2008-2018 From Australian Coal Mining: Implications For Public and Occupational HealthMaria Stephany CalisayaNoch keine Bewertungen
- Meyer-Andersen - Buddhism and Death Brain Centered CriteriaDokument25 SeitenMeyer-Andersen - Buddhism and Death Brain Centered Criteriautube forNoch keine Bewertungen
- Chem Sba 2019-2020Dokument36 SeitenChem Sba 2019-2020Amma MissigherNoch keine Bewertungen
- 03 - Air Ticket Request & Claim Form 2018Dokument1 Seite03 - Air Ticket Request & Claim Form 2018Danny SolvanNoch keine Bewertungen
- Audio AmplifierDokument8 SeitenAudio AmplifierYuda Aditama100% (2)
- Energies: Numerical Simulations On The Application of A Closed-Loop Lake Water Heat Pump System in The Lake Soyang, KoreaDokument16 SeitenEnergies: Numerical Simulations On The Application of A Closed-Loop Lake Water Heat Pump System in The Lake Soyang, KoreaMvikeli DlaminiNoch keine Bewertungen
- Passive ROMDokument3 SeitenPassive ROMCzarina FayeNoch keine Bewertungen
- Anesthesia 3Dokument24 SeitenAnesthesia 3PM Basiloy - AloNoch keine Bewertungen
- Midyear Budget ReportDokument402 SeitenMidyear Budget Reportcbs6albanyNoch keine Bewertungen
- Hijama Cupping A Review of The EvidenceDokument5 SeitenHijama Cupping A Review of The EvidenceDharma Yoga Ayurveda MassageNoch keine Bewertungen
- Fundamental Unit of Life 1-25Dokument25 SeitenFundamental Unit of Life 1-25Anisha PanditNoch keine Bewertungen
- Questions To Client On SAP HCMDokument19 SeitenQuestions To Client On SAP HCMeurofighterNoch keine Bewertungen
- Adjectives Comparative and Superlative FormDokument5 SeitenAdjectives Comparative and Superlative FormOrlando MiguelNoch keine Bewertungen
- Complete Denture TechniquesDokument6 SeitenComplete Denture TechniquesJohn Hyunuk ChoNoch keine Bewertungen
- ANNEX I of Machinery Directive 2006 - 42 - EC - Summary - Machinery Directive 2006 - 42 - CE - Functional Safety & ATEX Directive 2014 - 34 - EUDokument6 SeitenANNEX I of Machinery Directive 2006 - 42 - EC - Summary - Machinery Directive 2006 - 42 - CE - Functional Safety & ATEX Directive 2014 - 34 - EUAnandababuNoch keine Bewertungen
- The Nursing ShortageDokument6 SeitenThe Nursing Shortageapi-455495817Noch keine Bewertungen
- Voca-Book (This Must Be The Place)Dokument13 SeitenVoca-Book (This Must Be The Place)Анастасия ВознесенскаяNoch keine Bewertungen
- Republic Act No. 10070Dokument3 SeitenRepublic Act No. 10070Ganiela MCNoch keine Bewertungen
- Diagnostic Test 12Dokument3 SeitenDiagnostic Test 12Honorato BugayongNoch keine Bewertungen
- Unit Plan Adult Health Nursing Unit IIDokument7 SeitenUnit Plan Adult Health Nursing Unit IIDelphy VargheseNoch keine Bewertungen
- Cardiovascular SystemDokument47 SeitenCardiovascular SystemAtnasiya GadisaNoch keine Bewertungen
- Upper Gi f1 Survival GuideDokument1 SeiteUpper Gi f1 Survival GuideNathan Hovis JeffreysNoch keine Bewertungen
- EarthmattersDokument7 SeitenEarthmattersfeafvaevsNoch keine Bewertungen