Beruflich Dokumente
Kultur Dokumente
E435 PDF
Hochgeladen von
M Mas RindaOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
E435 PDF
Hochgeladen von
M Mas RindaCopyright:
Verfügbare Formate
CE
Directed Reading
Diagnosis and Treatment of
Vertebral Compression Fractures
Cherie Dewar, BS
A healthy spine is an integral After completing this article, the reader should be able to:
part of an individual’s overall Describe the causes of most vertebral compression fractures.
well-being. The spinal column’s List risk factors for vertebral compression fractures.
essential role in physiological Discuss psychological and physiological effects of vertebral compression fractures.
and neurological function can Explain the role of medical imaging in diagnosing and treating vertebral compression
be compromised when disease fractures.
or trauma causes a vertebra Discuss medications and treatment options for managing vertebral compression fractures.
Describe complications associated with surgical procedures used to treat vertebral
to compress under the body’s
compression fractures.
weight, producing a vertebral
T
compression fracture. This
he spine’s bony structure, Lateral Spinal Column
is a common ailment among
made up of vertebrae, sup-
adults older than 65 years of ports the core of the body and
age, especially for those with endures the impact of nearly
low bone mass or osteoporosis. every physical movement. The verte-
This article describes vertebral bral column houses the spinal cord
compression fractures, with a and branching nerves that enable
special emphasis on medical movement and supports 80% of the
imaging. body’s weight.1
Osteoporosis, malignancies,
and trauma can affect the vertebral
column, causing vertebral bodies
to collapse. This injury is called a
vertebral compression fracture. Unlike
a traditional traumatic fracture, com-
pression fractures occur when the
bone condenses, much like a crushed
aluminum can.2 Radiographs are
standard diagnostic tools for vertebral
This article is a Directed compression fractures, and medical
Reading. Your access to imaging is used throughout manage-
Directed Reading quizzes ment of such injuries.1
for continuing education
credit is determined by Vertebral Anatomy
your membership status An adult vertebral column is made
and CE preference. up of 33 vertebrae categorized into 5
sections (see Figure 1)3: Figure 1. Sections of the spine.
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 301
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
The cervical section from the base of the head to Overview
the top of the shoulders is made up of 7 vertebrae. A vertebral compression fracture is unique from
These are the smallest, and they bear the least other bone fractures because it is characterized by col-
amount of weight. lapsed trabecular bone rather than a clean break (see
The thoracic section ranges from the shoulders to Figure 4). Trabecular bone can deteriorate because
just above the lower back. The thoracic section is of age or disease processes. A vertebra’s rectangular
the longest, with 12 vertebrae. shape is compressed, and this compression is visible on
The lumbar section is the lower back, with 5 ver- radiographs. 4 The fracture can cause bone fragments
tebrae. to rub against one another, producing pain. 4 Most ver-
Below the lumbar region is the sacral section, tebral compression fractures occur in the thoracolum-
located behind the pelvis. The 5 sacral vertebrae bar region of the spine.5 According to Alexandru and
are fused in adults. So, these compression fractures in the thoracolumbar
The coccygeal section, at the base of spinal column, region have a mechanism of injury related to flexion
comprises 4 vertebrae that fuse after 30 years of age. and compression that typically involves the anterior
A vertebra is composed of a vertebral arch, a vertebral longitudinal ligament and the anterior half of the ver-
body, and projections called processes (see Figure 2).3 tebral body. 6 The authors noted that 60% to 75% of
Each process forms a sort of “W” shape with 2 extra spikes
in either valley, and together they form the vertebral arch.
The oval-shaped vertebral body is attached anteriorly to Superior end plate
the vertebral arch via pedicles and protects the anterior Spinous process
Vertebral body
side of the spinal cord.3 The pedicles originate from the
vertebral body on either side of the spinal cord and con- Inferior end plate
Disk
nect the vertebral body to the vertebral arch. Pedicles
The vertebral body is composed of trabecular bone
Spinal nerve
that has needlelike crossing projections that create vas-
cular, spongy pores within which red marrow produces
red blood cells.3 This trabecular bone is encased in a
thin layer of cortical bone.3 The edges of the top and
bottom of the vertebral body are layered with an end Figure 3. Lateral view of a typical vertebra.
plate (see Figure 3).3
Spinous process
Normal Fracture
Articular process Vertebral arch
Transverse
process
Spinal cord
Pedicles
Vertebral body
Figure 2. Superior view of a typical vertebra. Figure 4. Illustration of a vertebral compression fracture.
302 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
vertebral compression fractures occur between T12 and Most patients who have vertebral compression frac-
L2, where the vertebral column transitions from being tures have weakened vertebrae from diseases or condi-
rigid to mobile, which could make these vertebrae more tions such as osteoporosis, cancer, or as sequelae from
vulnerable to compression fractures. 6 infection, hyperparathyroidism, hypogonadism, or
osteomalacia.1,6 Because osteoporosis usually is associ-
Classification ated with older patients, malignancy should be consid-
Vertebral compression fractures are classified into ered as the cause of vertebral compression fracture in
3 types based on the portion of the vertebral body patients who are aged younger than 55 years. 6
affected. The types are wedge, biconcave, and crush. 6 Osteoporosis is the predominant cause of vertebral
Approximately half of all vertebral compression frac- compression fractures. The disease disrupts the struc-
tures are wedge types that involve compression of the ture of the trabecular bones in the vertebrae and chang-
anterior segment of the vertebral body; they typically es the contents of the noncollagenous proteins in the
occur in the midthoracic region. About 17% of ver- bone’s matrix. 6 Approximately 44 million Americans
tebral compression fractures are biconcave, meaning have osteoporosis, and another 34 million have low
the center portion of the vertebral body is compressed bone mass. The high incidence of osteoporosis likely
but its anterior and posterior walls remain unaffected. contributes to the 1.5 million vertebral compression
The rarest type of vertebral compression fracture is fractures diagnosed annually in the United States. 6
a crush fracture, which involves either compression A decrease in bone density begins in both men and
of the entire anterior and posterior portions of the women after they reach 40 years of age, but the process
vertebral body6 or only the posterior portion.1 Crush accelerates in women who have undergone menopause.1
fractures make up about 13% of vertebral compres- A patient’s bone mineral density loss is measured with
sion fractures, and complex fractures—fractures with dual-energy x-ray absorptiometry, or bone densitometry.6
significant soft tissue injury—constitute the remain- The examination generates a T-score that represents the
ing types. 6 standard deviation from the mean peak value of bone
At times, the nature of vertebral compression frac- density in young adults.6 The World Health Organization
tures can be confused with developmental deformities defines osteoporosis as a T-score of less than 2.5, and
such as Scheuermann disease in which the end plates a T-score between 1 to 2.5 is defined as decreased
degenerate and then re-form. The fractures also can be bone density or osteopenia. A T-score of 1 and higher
confused with degeneration from osteoarthritis. 5 is considered normal.6 Low bone mass is a term used for a
T-score between 2.5 and 1.4.1
Symptoms If a patient’s bone density decreases one standard
The onset of mechanical axial back pain caused by deviation below the average vertebral density, the risk
a vertebral compression fracture can surprise a patient of vertebral compression fracture doubles1; if the bone
who has likely experienced no traumatic injury.1 The mineral density falls by 2 standard deviations, the risk
pain can be abrupt and in a single site, but patients have of a compression fracture increases 4 to 6 times. 6
also reported pain that extends anteriorly to their heart Once a patient has one vertebral compression fracture,
or lung area.1 Lying down relieves the pain because it the risk of another fracture, despite the individual’s bone
decreases the effect of gravity on the broken vertebra density, increases 5-fold6; having 2 or more of the frac-
that occurs with sitting and standing.1 tures increases the risk of developing another vertebral
compression fracture by 12-fold.6 Patients who have had
Causes a vertebral compression fracture also have a higher risk
Most vertebral compression fractures are caused by of fracture in other bones, such as the hip.2 Other predic-
diseases, but they also can occur as a result of physical tors of vertebral fracture risk can include an individual’s
trauma. A single compression fracture can lead to sub- bone geometry and the structure of the cortical bone sur-
sequent vertebral fractures. rounding the trabecular bone in the vertebrae.7
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 303
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
Once an individual’s vertebrae are compromised Sequleae
by a bone-weakening condition, the structures cannot Pain is the chief result of a vertebral compres-
withstand normal amounts of pressure or strain.2 As a sion fracture, and pain emanating from the back can
result, the smallest of movements such as bending over, make standing, walking, or even lying down difficult. 6
turning quickly, lifting even light objects, sneezing, and Compression fractures in the lumbar region might
coughing can cause a vertebral compression fracture.2,6 cause greater disability than those in the thoracic
Traumatic injury caused by a fall from a height or a region.5
motor vehicle crash can cause compression fractures, When the vertebrae compress and the spine tilts for-
but up to 30% of vertebral compression fractures can ward, the gap between the ribs and pelvis closes and can
occur while a person is in bed. 6 The reason that trivial impair balance.1 This forward-tilting spinal alignment
motions can lead to injury might be explained by the causes a patient to pull back for counterbalance, which
contraction of the paraspinal muscles. 6 can cause pain.2
Studies have shown that decreased extensor strength Pain from vertebral fractures has additional con-
in the back muscles, reduced spinal mobility, altered sequences, particularly if subsequent compression
trunk muscle control, and balance issues might con- fractures occur. 6 These consequences include loss of
tribute to incidence of vertebral compression fractures stature, fatigued muscles, disproportionate thoracic
in individuals who have osteoporosis. The paraspinal kyphosis (curvature of the thoracic region, resulting in
muscles are responsible for compressive forces in the concave curve of the upper back), and lumbar lordosis
spinal area. Briggs et al showed that a pattern of paraspi- (convex curvature of the lower back). 6 If kyphosis is
nal muscle recruitment occurs in individuals who have severe, as seen in patients with osteoporosis, it can exert
vertebral compression fractures that is different from so much pressure on the pelvis that the individual expe-
the pattern in those who have osteoporosis and do not riences pulmonary impairment, a protruding abdomen,
experience fractures. Motor recruitment is a neuromus- satiety, poor nutrition, and weight loss. 6 Constipation,
cular response that relies on motor, or muscular, units bowel obstruction, and a reduced amount of activity
as resistance increases. The muscle recruitment changes also are possible results of a vertebral compression frac-
occur at the thoracolumbar transition zone in which ture, and reduced activity only expedites weakening of
vertebral fractures are most common.7 the bones and muscles or can cause complications such
as deep vein thrombosis. 6
Risk Factors The sequelae related to vertebral fractures nega-
Several risk factors predispose individuals to ver- tively affects a patient’s quality of life, independence,
tebral compression fractures. These include alcohol self-esteem, emotions, and social life. 6 Approximately
consumption, tobacco use, estrogen deficiency, frailty, 40% of patients with a vertebral compression fracture
a history of falls, impaired eyesight, lack of physical develop depression.2
activity, and a deficiency of calcium and vitamin D.5,6 Even after a vertebral compression fracture has
Chronic obstructive pulmonary disease, seropositive healed, an individual’s loss of height can lead to focal or
rheumatoid arthritis, and Crohn disease are additional sagittal imbalance,1 requiring the use of a cane or walk-
risk factors for vertebral fractures, as is the use of sys- er for mobility or causing difficulty with activities such
tematic glucocorticoids, especially after cumulative as riding in an automobile.2 Patients who have vertebral
exposure to such medications.5 compression fractures have a 15% greater risk of death. 6
Obesity is not considered a risk factor for vertebral The 2005 direct medical economic burden of osteo-
compression fractures but instead decreases risk of bone porosis in the United States is estimated to be between
loss. 6 Obesity causes an increased production of hor- $13.7 billion and $20.3 billion, and vertebral compres-
mones such as estrogen and of insulinlike growth factor sion fractures account for about $1.1 billion of these
binding protein-1, both of which stimulate osteoblast costs.8 It is projected that this cost will increase by 50%
activity and increased bone production. 6 by 2025.9 The long-term morbidities that result from
304 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
vertebral compression fractures are reflected in the fact conditions develop a spinal metastasis that causes
that, in the first year after a painful fracture, the rate of pain.10 Approximately 60% of spinal metastases origi-
patients who require primary care services is 14 times nate from breast or prostate cancer.11 The vertebral
higher than that of the general population.1 The indi- body is more susceptible to invasion by tumor cells
rect costs are difficult to estimate, but they are likely because of its vascular nature as opposed to the avascu-
much higher when patients’ time off work and other lar nature of a disk; about 80% of the time, the cancer
issues like pain, insomnia, and depression are factored invades the vertebral body, followed by the pedicles.11
into the cost of vertebral compression fractures.9
Diagnosis
Epidemiology A patient’s physical examination might reveal hyper-
The risk factors that contribute to vertebral compres- kyphosis, or excessive thoracic spine curvature. The
sion factors also affect incidence, leading to a higher finding indicates likelihood of vertebral compression
number of the fractures among women who have passed fractures.5 The patient’s medical history should provide
menopause. In fact, 25% of postmenopausal women in additional information such as osteoarthritic pain,
the United States experience a vertebral compression pathologic pain from a tumor, or lumbar strain to aid in
fracture. 6 differential diagnosis of vertebral compression fracture.1
Vertebral compression fractures are most preva- A definitive diagnosis of vertebral compression frac-
lent in adults aged 80 years and older, at a rate of 30%. ture usually is accomplished using a number of medical
Nearly 50% of the bone mass in the axial skeleton is lost imaging modalities. However, most vertebral compression
when a woman reaches 80 years of age. Women aged fractures are not diagnosed when they occur. In 2 studies
50 to 69 years have the fractures at a rate of 5% to 10%.1 in the United States, only 25% to 33% of radiographically
The difference in incidence according to sex is nearly identified vertebral fractures were clinically diagnosed.5
double for women, particularly as they age. In general, The same is true in Europe, where nearly 66% of osteopo-
10.7 per 1000 women have a vertebral compression frac- rotic vertebral compression fractures are missed.12
ture annually in the United States, compared with 5.7 Many vertebral compression fractures are identified
fractures per 1000 men. 6 Some reports say that women incidentally on chest radiographs but not addressed by
who are Asian or African American have a lower preva- the treating clinician.5 In addition, vertebral compression
lence of the fractures than do Caucasian women. 5 fractures have been described as insidious and might not
An explanation for incidence might lie in the associa- be visible on a first radiograph.1 Unlike imaging of bone
tion of vertebral compression factors with osteoporosis metastases, nuclear bone scans are used infrequently to
and osteopenia. Nearly 50% of the 1.5 million fractures diagnose vertebral compression fractures. A compression
related to osteoporosis each year in the United States fracture might be revealed incidentally on a bone scan by
are vertebral fractures.2 Likewise, approximately 50% increased uptake of radionuclides.1
of all patients who have a vertebral compression frac- A physician might not order radiography or ver-
ture also have osteoporosis, and 40% have osteopenia.1 tebral fracture assessment, a technology using bone
Approximately 14% to 18% of women who are aged densitometry of the thoracic and lumbar spine, when a
older than 60 years and have low bone mass have a ver- patient has been diagnosed with osteoporosis or has a
tebral compression fracture, 5 and 20% of women who bone density T-score of 1.5 or higher. The reason is
are postmenopausal and have osteoporosis will develop that confirming a vertebral compression fracture likely
a second vertebral fracture within a year of their first will not change the selected course of medical therapy.5
compression fracture.1 An increasingly aging popula- However, if the patient is a postmenopausal woman
tion will lead to higher incidence of the fractures associ- with a T-score of between 1.5 and 2.4 who could
ated with loss of bone mass.2 benefit from drugs such as bisphosphonates to prevent
Cancer also causes vertebral compression fractures. further fractures following an initial vertebral compres-
Approximately 30% of patients with various neoplastic sion fracture, radiography is warranted. In addition,
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 305
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
diagnosis of fractures using radiography or vertebral to Craig St George, R.T.(R)(VI), if a cervical collar has
fracture assessment is justified in terms of cost- been applied, a minimum of anteroposterior and lateral
effectiveness when compared to not treating a vertebral views are performed to rule out fracture before the col-
compression fracture and risking additional fractures or lar is removed (written communication, October 2014).
long-term morbidity.1,5 If a patient has undergone severe trauma, the patient’s
entire spine should be assessed to check all vertebrae
Radiography for injuries. Five percent to 20% of patients who are
A radiograph is the first diagnostic tool used in iden- diagnosed with vertebral compression fracture have
tifying a vertebral compression fracture, 6 with a lateral additional vertebral compression fractures. 6
projection of the thoracic and lumbar spine being the A radiograph provides the following diagnostic
most cost-effective approach (see Figure 5).1 According information1,6:
Identification of a vertebral compression fracture,
including type (wedge, biconcave, or crush).
Measurement of a vertebra’s height loss; a mini-
mum of 20% must be lost compared with normal
portions of the vertebral body for a vertebral com-
pression fracture to be diagnosed.
Measurement of increased distance between the
processes or pedicles, indicating vertebral disrup-
tion.
Estimation of how much a vertebra has moved out
of alignment along its anterior and posterior lines
can be seen on erect projections.
A patient who has osteopenia could be more prone
to vertebral compression fractures, and certain charac-
teristics on radiographs suggest osteopenia, including
increased radiolucence and loss of horizontal trabecu-
lae. Wong and McGirt also list decreased cortical thick-
ness accompanied by increased relative opacity of the
end plates and vertical trabeculae as signs of osteope-
nia.1 The authors also noted that the age of a fracture
can be estimated if prior radiographs with no signs
of fracture are available for comparison. In addition,
radiologists also measure the kyphotic angle, or the
angle between the superior end plate one level above
the injured segment and the inferior end plate one level
below the injured segment, to reach a diagnosis of verte-
bral compression fracture (see Figure 6). 6
In 2013, Cho et al published the results of their
study comparing the usefulness of the prone cross-table
lateral projection to the standing extension lateral pro-
jection in preoperative and postoperative radiographs
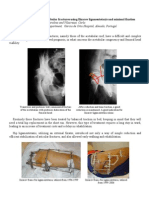
Figure 5. Lateral radiograph of a vertebral compression fracture
showing anterior wedging (arrow). Reprinted with permission of 62 patients with vertebral compression fractures
from Alexandru D, So W. Evaluation and management of verte- (see Figure 7).13 The authors measured the degree of
bral compression fractures. Perm J. 2012;16(4):46-51. patients’ pain associated with each position and the
306 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
accuracy with which each position and projection could
display the restoration of the postoperative wedge angle
and vertebral heights. The authors found that the prone
cross-table lateral radiographs were more accurate than
the erect images in helping radiologists determine the
degree of restoration of vertebral heights and wedge
b angles following surgery. In addition, the prone cross-
table positioning caused less pain during the examina-
tion. The authors also noted that the prone cross-table
lateral radiograph can be used effectively in diagnosing
Line 1 intravertebral clefts or intravertebral dynamic mobil-
a ity.13 Intravertebral clefts are a radiographic sign of avas-
cular necrosis in the vertebral body. When intraverte-
bral clefts are present, a delay of fracture healing called
Line 2 dynamic mobility can occur.14 Eventually, dynamic
mobility can result in nonunion of the fractured verte-
brae, called Kümmel disease.13
c Computed Tomography
Computed tomography (CT) scanning requires a
deeper inspection by the radiologist to diagnose a ver-
tebral compression fracture or to clearly examine the
Figure 6. Parameters and calculating methods from lateral radio- bones and loss of height (see Figure 8).1,6 CT scans can
graphs. Vertebral wedge angle = Cobb angle between line 1 and help physicians determine whether an anterior wedge is
line 2. Vertebral height ratio = a / (b + c) × 2. Reprinted with unstable, and they are ideal for imaging complex verte-
permission from Cho JH, Shin SI, Lee JH, Yeom JS, Chang BS, bral compression fractures. 6 A CT myelogram typically
Lee CK. Usefulness of prone cross-table lateral radiographs in ver- is not necessary to diagnose a vertebral compression
tebral compression fractures. Clin Orthop Surg. 2013;5(3):195- fracture but is useful for assessing whether a vertebral
201. Creative Commons Attribution Noncommercial License.
fracture has resulted in cord compression and as an
alternative when magnetic resonance (MR) imaging is
unavailable or contraindicated. 6
Magnetic Resonance Imaging
MR imaging also is not usually needed to diagnose
vertebral compression fractures, with a few exceptions,
including imaging of a patient who has a neurological
deficit. MR also might be indicated when physicians
need to assess ligament damage or the age of a vertebral
compression fracture. MR also could be used with a
postcontrast technique if physicians need to examine a
fracture that might have been caused by an infection or
cancer (see Figure 9).1,6
Figure 7. This position allows for prone cross-table lateral radio-
Increased MR signal intensity is seen with spinal
graphs to aid in diagnosing vertebral compression fractures. The cord injuries, and recent fractures display a higher
arrow indicates the direction of the x-ray beam. T2-weighted signal intensity compared with normal
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 307
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
Figure 8. Computed tomography scan of a biconcave vertebral Figure 9. T2-weighted magnetic resonance (MR) images of wedge
compression fracture (arrow). Reprinted with permission from vertebral compression fracture (white arrow) and biconcave verte-
Alexandru D, So W. Evaluation and management of vertebral bral compression fracture (blue arrow). Reprinted with permission
compression fractures. Perm J. 2012;16(4):46-51. from Alexandru D, So W. Evaluation and management of verte-
bral compression fractures. Perm J. 2012;16(4):46-51.
vertebrae because the fractures have more water in
their vertebral body. 6 MR images also reveal whether (PET-CT) scans could be specific and sensitive
a vertebral compression fracture is causing damage to enough to distinguish between benign and malignant
nerves by pressing on nerve roots or the spinal cord.1 lesions that contributed to a vertebral compression
MR short tau inversion recovery can help determine fracture.15 Lesions that cause vertebral compression
the condition of a patient’s spinal ligamentous com- fractures typically are evaluated with fine-needle aspi-
plex, which can inform an interventional team of a ration cytology, but the researchers wanted to know
fracture’s stability.1 whether biopsy could be avoided with use of imaging
In 2013, Aggarwal et al published results from a techniques alone or whether advanced imaging could
study that sought to determine whether MR and posi- be used as a tool to confirm evaluation when cytology
tron emission tomography–computed tomography results were inconclusive.
308 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
Imaging was conducted on 24 sub- A B C
jects with vertebral compression fractures
and no history of osteoporosis, degen-
erative disease, or disk herniations. MR
images were acquired with a 1.5T Siemens
MAGNETOM with and without gadolini-
um contrast (0.1 mmol/kg). CT scans were
acquired at 140 kV 10 mA, followed by
PET scans on GE Discovery PET-CT equip-
ment after the injection of 10 mCi to 20 mCi
of fluorodeoxyglucose F 10.15 All patients
also underwent fine-needle aspiration biopsy
of primary lesions or of other sites noted by
PET-CT if the initial cytology results were
uncertain.
Researchers found that the diagnosing
specificity for MR and PET-CT combined Figure 10. A. Vertebral fracture assessment that has a low resolution compared with
was 100% for benign lesions, and the sensi- standard lateral radiographs of the spine with projection distortion. The vertebral
tivity of the 2 imaging modalities combined cortices and end plates are less distinct (arrow) and the vertebral fracture assessment
was 100% for malignant tumors. The speci- does not display the thoracic spine well at a level superior to T7. B.-C. Standard
lateral spinal radiographs with projection distortion (parallax). From N Engl J
ficity for MR and PET-CT combined was not Medicine. Ensrud KE, Schousboe JT. Vertebral Fractures. Vol. 364, page 1634.
100% for malignant tumors. The researchers Copyright © 2011 Massachusetts Medical Society. Reprinted with permission from
found that PET-CT scans were helpful in Massachussetts Medical Society.
determining additional biopsy locations.15
Vertebral Fracture Assessment currently consists primarily of 2 procedures: percu-
A vertebral fracture assessment can divulge an occult taneous vertebroplasty or percutaneous kyphoplasty.
fracture between vertebrae T4 and L4 and is a conve- Decisions regarding treatment approaches for each
nient imaging examination for many patients at risk patient can be difficult and controversial. Typically,
for fractures because the assessment can be performed physicians first recommend that a patient allow a ver-
during a bone density scan. A vertebral fracture assess- tebral compression fracture to heal with a conservative
ment uses less radiation than lateral lumbar spine radi- approach, or with medical therapy. Vertebral augmenta-
ography, 5 and the images have less parallax than when tion options are considered if the patient’s pain persists.2
vertebrae are imaged with a cone-beam method (see
Figure 10). The bone densitometry method of fracture Medical Therapy
assessment, combined with careful measurements to Medical therapy is a safe first choice for managing
determine which area of the vertebra is compressed, a vertebral compression fracture and associated pain2
can be 90% sensitive and specific to diagnose moderate but does not restore vertebral height or realignment.
to severe fractures, but it is less sensitive in diagnosing Without vertebral height restoration, a patient can expe-
mild fractures.5 rience deteriorating kyphosis and consequences such as
further kyphotic deformity and its sequleae. 6 A typical
Treatment first-line regimen of nonsurgical management entails
Vertebral compression fractures can be treated inva- analgesics, some bed rest, avoidance of motion that
sively or more conservatively with medical therapy. could bend the spine, bracing, medication to improve
The invasive treatment, called vertebral augmentation, bone health, and physical therapy.1,16
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 309
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
Medications strength and balance training, with stabilization of the
A combination of medications can be recommended lumbar area, twice a week. Bennell et al emphasized
for patients who have vertebral compression fractures once-a-week soft tissue massage therapy and exercises
to treat the pain. The type and level of analgesic chosen such as standing wall pushups.21,22 Both programs
might depend on pain level, potential adverse effects, led to reduced back pain from compression fractures
and the medication’s effects on a patient’s comorbidi- and improved the patients’ quality-of-life scores. A
ties. Pain relief options range from nonsteroidal anti- third research group led by Papaioannou conducted a
inflammatory drugs to opiates.1,2 Patients on opiates randomized controlled trial that lasted 6 months and
should be monitored carefully for addiction to these included stretching, strength training, and aerobics.
drugs. Other medication options to treat vertebral Although participants in the Papaioannou study had
compression fracture pain include muscle relaxants and improved quality-of-life scores and better balance, their
local analgesic patches.1 Tricyclic antidepressants also bone mineral density remained unchanged.23
are commonly prescribed for patients with vertebral
compression fractures and neuropathic pain.5 Nonmedication Pain Relief Methods
If a vertebral compression fracture leads to the diagno- Physicians might recommend applying ice packs or
sis of osteoporosis, a patient could receive one of several heat packs over the area of the vertebral compression
drugs that have been vetted in large, randomized trials fracture to help relieve pain.2 Other pain relief methods
to treat osteoporosis, reduce pain from the fracture, and include intercostal nerve blocks and use of transcutane-
prevent further fractures.5 Other drugs have even been ous nerve stimulation units.1 Radiation therapy can help
shown to prevent additional nonvertebral fractures such relieve pain for patients whose vertebral compression
as hip fractures. Table 1 lists several medications used to fracture is caused by cancer. Radiation therapy has
manage pain, osteoporosis, and fractures. been shown to provide pain relief for half of the patients
whose fractures were caused by myeloma, prostate can-
Physical Activity cer, or breast cancer. 6
Often, a physician orders bed rest for a patient with
a new vertebral compression fracture but only for a Back Bracing
limited period. Long periods of immobility can increase A back brace can help reduce the amount of pres-
bone mineral density loss (0.25%-1.0% per week of bed sure on a patient’s compression fracture.2 Braces hold
rest) and the risk of other health issues such as venous the spine straight, stabilize the fracture, and prevent
thrombosis, pulmonary embolism, pressure ulcers, and further compression.2 A patient could require use of a
urinary tract infections.2,6 brace for up to 3 months, but using a brace beyond 3
When a patient is ready, performing gentle exercises months is not recommended because it can weaken the
such as swimming or walking, perhaps with a walking core muscles.2 A prospective randomized study with
aid, is recommended.2,20 Patients also may be referred patients using thoracolumbar orthotic braces found that
to physical therapy and rehabilitation programs to patients’ core strength, posture, and height improved,
improve recovery from a vertebral compression frac- leading to a better quality of life for the patients.1
ture.20 Physical therapy should strengthen a patient’s Another study with bracing found that patients’ core
axial musculature, including the spinal extensors, and muscles were actually more active with a brace, though
educate the patient how to improve posture and gait to the brace should have been limiting their flexion.1 Yet
avoid falls.1 another small, randomized, unblinded study involved
Strengthening spinal extensors also reduces verte- 2 groups, one with patients who wore a rigid brace dur-
bral compression fracture pain.1 Randomized trials led ing their waking hours for 6 weeks and a second group
by Malmros et al and Bennell et al followed patients of patients who wore a nonrigid brace for only 2 hours
who participated in the authors’ respective 10-week a day for 24 weeks. Participants in both groups experi-
physical therapy programs. Malmros et al emphasized enced less self-reported pain.5
310 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
Table 1
Medications Used to Manage Vertebral Compression Fractures
Medication Adverse Effects Notes
1,17-19
To Treat Osteoporosis
Bisphosphonates Nausea, GI problems such as stomach pain and The FDA expressed concerns in 2011 about risk of
bloating, dizziness, joint swelling. Serious effects such bisphosphonates in increasing risk of renal failure but
as chest pain, hives, difficulty swallowing. has stated that benefit outweighs risks overall.
Selective estrogen Breathing problems, chest pain, lower leg pain and Use of raloxifene helps preserve bone density with-
receptor modulators edema, severe headache. out introducing risk of breast and uterine cancer.
1
Hormone replacement Increased risk of cancer, stroke, and myocardial For younger postmenopausal women.
therapy infarction in postmenopausal women.
5
Supplemental vitamin Vitamin D can cause toxic effects such as weakness, Recommendations vary ;
D and calcium muscle and bone pain, and elevated liver enzymes Vitamin D – 600-800 IU/d
if taken at high doses. Calcium can cause nausea, Calcium – 1000-1200 mg/d
vomiting, and constipation; people with kidney stones
should use caution.
1,2,5
To Reduce Pain, Prevent Additional VCFs
Bisphosphonates Upper GI irritation. Administered orally or by injection.
Calcitonin Stuffy nose (nasal administration), nausea, injection Should not be taken in place of analgesics.
site reactions, red hands and face (subcutaneous
administration).
Teriparatide Nausea, arthralgia, leg cramps, hypercalcemia, Injectable recombinant parathyroid hormone.
hypercalciuria.
5
To Prevent Additional VCFs, Non-VCFs
Lasofoxifene Leg cramps, hot flashes. N/A
Strontium ranelate Diarrhea, nausea, eczema, headaches. N/A
5
To Prevent Additional VCFs, Non-VCFs, Hip Fractures
Alendronate Upper GI irritation. A bisphosphonate; reduces risk of VCF by 50% in
6
postmenopausal women.
Risedronate Upper GI irritation. A bisphosphonate with delayed release action.
Zoledronic acid Bone pain (first dose), flulike symptoms. Injectable bisphosphonate.
Denosumab Eczema, nausea, injection-site reactions. Alternative to bisphosphonate called a RANK ligand
inhibitor.
Abbreviations: FDA, U.S. Food and Drug Administration; GI, gastrointestinal; N/A, not applicable; VCF, vertebral compression fracture.
The type of brace recommended depends on the sacral orthosis.1 A compression fracture in the lumbar
location of a vertebral compression fracture. Thoracic area can be braced by a lumbosacral orthosis, which
fractures can be braced with a thoracolumbar orthosis does not always immobilize the entire spine but instead
(such as a Jewett, cruciform anterior spinal hyperexten- can increase motion between vertebrae L4 and S1 and
sion, or Taylor brace), and a vertebral compression frac- confine sagittal plane motion between vertebrae L1
ture in the sacrum can be braced by a thoracolumbar and L3.1,13
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 311
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
Complications with bracing include discomfort, called a tamp) into the fractured area to push the end
skin irritation, and breathing interference. Softer, light- plates out. This created a cavity into which partially
weight braces could reduce these complications and cured cement was injected, under less pressure, after
improve compliance, but a more stringent brace might the balloon was removed (see Figure 11). Reiley’s tech-
be needed if a patient’s spine is severely deformed.1 nique formed the basis for kyphoplasty.25,27
Both vertebroplasty and kyphoplasty are minimally
Vertebral Augmentation invasive, can be performed with local anesthesia, take
Typically, the augmentation options from which a approximately one hour, and do not require stitches.
patient can choose are percutaneous vertebroplasty Both use image guidance and can be performed in an
(also called acrylic vertebroplasty) and percutaneous interventional radiology or neuroradiology suite and on
kyphoplasty (also called balloon-assisted vertebro- an outpatient basis.4 The following detailed steps apply
plasty).23 Kyphoplasty is a type of vertebroplasty, and to both vertebroplasty and kyphoplasty:
both procedures can potentially stabilize the vertebra, An MR scan is likely to be performed before the
prevent further loss of vertebral height, correct kyphotic procedure to check for the fracture-confirming
deformity, and reduce pain. Between 85% and 95% of presence of bone edema; to see if there is disk,
patients who have undergone one of the procedures spinal cord, or soft tissue involved with the verte-
have experienced immediate pain relief. A study of 1309 bral compression fracture; and to verify the level
patients reported that both techniques reduced patients’ of the spine to be treated.2,25 A technologist also
pain by half.2 As with any invasive procedure, risks are will evaluate the patient’s spinal level under fluo-
involved with both options, and augmentation should roscopic guidance to prepare for the procedure,
be carefully considered for use in elderly patients, who and the interventional physician will use fluoros-
have a higher incidence of comorbidities. 6,25 The proce- copy to evaluate the treatment level prior to the
dures for vertebral compression fractures are conducted procedure (St George, written communication,
by interventional radiologists, anesthesiologists and October 2014).
other pain management specialists, and orthopedic At the time of the procedure, a patient lies prone
surgeons.26 Medical imaging is used before, during, and with the arms above the head on a Jackson table, a
after vertebroplasty and kyphoplasty.2 table made for back surgery that allows for the use
A vertebroplasty involves a small incision that allows of high-resolution fluoroscopic imaging in orthog-
a needle, guided by real-time CT or fluoroscopy, to onal planes and permanent image recording.
inject liquid cement into a compressed vertebra. The
cement is injected under pressure into the vertebra’s
A B
spaces and crevices.2,25,27 Two interventional neuroradi-
ologists in Amiens, France, performed the first percuta-
neous vertebroplasty procedure in 1984.25 The doctors,
Galibert and Deramond, performed the procedure on a
patient who had a C2 vertebra compromised by a verte-
bral hemangioma. The patient’s pain subsided for a long
period following the injection.25
After vertebroplasty gained notice, an orthopedic
surgeon named Reiley developed a new vertebroplasty
technique in an effort to reduce the risk of cement leak-
age during the procedure and to reinstate vertebral Figure 11. Kyphoplasty process. A. Balloon tamp is inserted into
height to the damaged vertebra.25 Instead of squeezing the collapsed vertebra and the balloon is inflated to create a cav-
liquid cement between the cracks of a compressed ver- ity. B. The balloon is withdrawn, and the physician injects cement
tebra, Reiley first inserted and inflated a balloon (also to fill the cavity.
312 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
Using the Jackson table minimizes repositioning location. The length of observation time deemed
and potential infection of the injection site.1,24 appropriate varies for each patient. Rarely, a
A patient’s vital signs such as heart rate, blood patient is admitted as an inpatient. 4
pressure, and pulse are reviewed and recorded Pain relief can be immediate or take up to 48 hours.2,4
before the procedure begins, and the incision area The cement’s mechanism of action for pain relief is not
is cleaned and shaved. 4 totally understood, but the hypothesis is that it immobi-
A patient’s vital signs are checked regularly during lizes the end plates and the tiny trabecular fractures that
the procedure, and a facility performing vertebral caused pain during movement. Kyphoplasty is consider-
augmentation should ensure access to CT or rapid ably more expensive than vertebroplasty.25
MR within 30 to 45 minutes in the event of com-
plications. Most patients receive local anesthesia Vertebral Augmentation Cement
under the skin and in the deep tissues near the Most cement used for vertebroplasty is polymethyl
fracture, but patients who are in poor health or of methacrylate, which was approved by the U.S. Food
advanced age, who cannot tolerate lying prone, and Drug Administration (FDA) in 2004.25 Polymethyl
or who have multiple vertebral compression frac- methacrylate usually is shipped as 2 components, a
tures requiring treatment might receive anesthe- powder and a liquid, and then mixed in the operating
sia intravenously.2,4 room or interventional suite just before injecting the
The physician makes a small incision near the cement into a patient.25 The cement hardens slowly and
fracture and inserts a trocar (hollow needle) has proved its compatibility with the human body in
through the patient’s muscles and into the frac- dentistry, hip and joint replacements, and filling gaps
tured vertebra under fluoroscopic guidance. 4,25 between prostheses and bone.25
The lateral and anteroposterior fluoroscopic The powder portion of polymethyl methacrylate is
images should display the pedicles clearly for tro- made up of beads or a similar acrylic polymer, along
car position. Patients who are awake might feel a with a filler that includes a contrast agent, most often
tapping sensation when the trocar is inserted into barium sulfate. Other contrast agents that can be used
the vertebra. 4 The procedure occasionally is per- are tantalum powder, tungsten, or zirconium dioxide.25
formed under CT guidance. The liquid part is made of methyl methacrylate mono-
Some physicians perform venography before mer (concentration 95% weight).25
injecting the cement mixed with a contrast mate- When the 2 parts are mixed together, the polymer-
rial. Fewer physicians are performing venography ization is initiated by a chemical in the liquid, but some
and some debate whether venography is effective, hardening inhibitors such as hydroquinine might be
but its use might minimize cement leakage and added if necessary.25 The person mixing the cement
display the venous channels near the trocar.25 should carefully calculate the ratio, which typically is
In vertebroplasty, cement is injected into the verte- 2.18 parts solid to 1 part liquid. If a staff person makes
bra.4,25 In kyphoplasty, the physician inserts a bal- an error in the ratio and the mixture is not properly bal-
loon tamp through the trocar, and the balloon is anced, the cement could harden prematurely or insuf-
inflated to create a cavity, then deflated and with- ficiently, leading to inadequate strength in the final
drawn before cement is injected into the cavity.4,25 compound, or an irregularity in the time required for
After the injection, the trocar is removed, and a hardening, all of which could lead to serious adverse
bandage is placed over the incision. 4 effects in a patient.25
The cement takes approximately 15 to 20 minutes It is recommended that a vertebroplasty cement
to harden and will be at 90% of its strength within have a longer liquid phase working time than that used
24 hours.2,25 for kyphoplasty. The cement used in vertebroplasty
After the procedure, a radiograph or CT scan must be squeezed into the tight spaces of a fracture
might be performed to check the cement’s while under high pressure, but a cement used during
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 313
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
kyphoplasty should have a shorter liquid phase and take (4-6 mL) and the appearance of the balloon on fluoros-
on a more doughy appearance to fill the cavity under copy.1 Sequential images are acquired during inflation
less pressure.25 to ensure that the end plates are not disturbed by the
After the procedure, the hardened cement is vis- balloon.1 Multiple images also are acquired during the
ible on diagnostic imaging. Some practices have added cement injection process to assess when the cavity is
antibiotics to the cement to minimize infection risk, but properly filled and whether the cement has leaked into
antibiotics such as gentamicin might compromise the the spinal cavity.1 The mean volume of cement injected
mechanical strength of the cement.25 To avoid this, anti- into patients undergoing kyphoplasty has been reported
biotics can be administered intravenously to a patient at 3.9 mL, compared with 2.2 mL for vertebroplasty
before the procedure. injection.16
An early study of kyphoplasty reported that 95%
Vertebroplasty of patients experienced considerable pain relief.27 A
The use of vertebroplasty to manage osteoporotic review article mentioned that kyphoplasty can restore
vertebral compression fractures increased rapidly after vertebral height by 50% to 70% and improve segmental
the first vertebroplasty was performed in the United kyphosis by 6° to 10°. 6 The chances of restoring the
States in the 1990s.2 Claims for Medicare Part B fee- vertebral height are best when kyphoplasty is per-
for-service enrollees nearly doubled for vertebroplasty formed within 3 months of the vertebral compression
procedures between 2001 and 2005.26 fracture occurrence. 6
Typically, 2 trocars are needed for a bipedicular
approach to a vertebral compression fracture for a verte- Complications of Vertebroplasty and Kyphoplasty
broplasty; this allows more cement to be evenly spread Because both procedures use plastic cement to fill
into the fracture.1 The upper region’s vertebral pedicles a vertebral body, both vertebroplasty and kyphoplasty
are smaller, which might necessitate an extrapedicular can put patients at risk for symptomatic cement leakage,
approach between the medial rib head and lateral edge or extravasation. In 2002, the FDA warned that extrav-
of the pedicle.1 asation can occur from both procedures.27
The procedure can relieve a patient’s pain,25 with up Extravasation of the cement material can cause an
to 75% to 100% of patients reporting good to moder- embolism, neurological deficits, spinal cord compres-
ate pain relief shortly after vertebroplasty. 6 A 2006 sion, osteomyelitis, hematoma, infection, digestive
literature review identified 4 studies that reported track bleeding, and adjacent vertebral compression.25
reduction in pain lasting up to one year.28 As many as Extravasation could cause radiculopathy (a disorder
75% of patients have regained their mobility following of the spinal nerve roots) if the cement leaks into the
vertebroplasty. 4 spinal canal or neural foramina of the spine, leading to
weakness.1 The cement’s seepage through the venous
Kyphoplasty channel in the vertebral body could cause an embolism
Kyphoplasty differs from vertebroplasty in the use of in the lungs, kidneys, or heart.2,25,29
a balloon tamp to first create a cavity in the broken ver- Fortunately, a physician can observe the cement
tebra, which compacts the spongy bone and pushes the entering a vertebra with the use of real-time fluoroscopy
end plates as close as possible into their original posi- so extravasation can be avoided.25 A number of studies
tions.1 During a kyphoplasty procedure, the physician have found statistical differences for complication risk
can insert the needle using an extrapedicular approach between vertebroplasty and kyphoplasty techniques.
or use 2 needles.25 Some of these statistics are reviewed in Table 2.25
A pressure gauge informs the physician when to stop The force of high pressure on the slowly filling
inflating the balloon during the procedure. This point cement required for vertebroplasty is a problematic
normally occurs at about 220 psi, not to exceed 300 psi. aspect of the procedure compared with kyphoplasty,
The physician also gauges the balloon’s inflation volume which does not require the same degree of pressure
314 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
Table 2 A B
Complication Rates in Vertebroplasty
25
and Kyphoplasty
Complication Vertebroplasty Kyphoplasty
Neurological effects 0.6% 0.3%
Embolism 0.6% 0.01%
Adjacent vertebral fractures 8%-52% 3%-29%
to fill an empty cavity.25 Extravasation rates have been
reported as higher in osteoporotic-associated vertebral
Figure 12. T2-weighted MR image in the sagittal plane.
compression fractures compared with those associated
A. Preoperative image of vertebral compression fracture at L3.
with malignant tumors. The overall complication rate B. Postoperative image of grade II adjacent disk degeneration
for both vertebral augmentation procedures is less than above the treated vertebra. Reprinted with permission from Qian
2% for fractures caused by osteoporosis and 10% for J, Yang H, Jing J, et al. The early stage adjacent disc degenera-
fractures caused by malignant tumors.25 tion after percutaneous vertebroplasty and kyphoplasty in the
As shown in Table 2, a wide range of adjacent verte- treatment of osteoporotic VCFs. PLoS One. 2012;7(10):e46323.
bral fracture rates are observed with vertebroplasty and Creative Commons Attribution License.
kyphoplasty.25 Yimin et al noted that science has not
determined whether the cement, which is stiffer than their vertebral augmentation. The vertebroplasty group
vertebral bone, affects neighboring vertebrae, or wheth- had a higher incidence of disk degeneration compared
er the subsequent fractures are simply part of the natu- with the kyphoplasty group, but the findings were not
ral progression of osteoporosis.25 A subsequent vertebral statistically significant. The researchers conjectured that
compression fracture rate of 10% has been reported for adjacent disk compression was caused by the cement’s
both procedures. 4 increased pressure on the adjacent disks or because of
In 2012, Qian et al published the results of a study that alterations in spinal loading caused by the cement.16
examined early-stage adjacent disk degeneration follow-
ing vertebroplasty (n 9) and kyphoplasty (n 53), Indications for Vertebral Augmentation
compared with a control group (n 35).16 There were The use of vertebral augmentation procedures
no significant differences between age, sex, body weight, for compression fractures has increased markedly in
or smoking status among the patient groups selected for the United States. Early studies demonstrated the
the study. Those who remained in the study (90.7%) had procedures’ benefits, but results of clinical trials in
MR imaging performed to evaluate the condition of their 2009 began to initiate considerable debate regarding
disks at baseline, or during their first appointment, and at effectiveness of augmentation vs more conservative
their last appointment 2 years later. approaches to managing the fractures, along with con-
The incidence of disk degeneration was significantly cerns about appropriate utilization of augmentation. 30
higher in the group having augmentation (52.6%) than In 2012, the American College of Radiology collabo-
in the control group (29.0%) (see Figure 12).16 Despite rated with the American Society of Neuroradiology,
differences in degeneration, the pain measurement in the the American Society of Spine Radiology, the Society
treatment group was about the same immediately after of Interventional Radiology, and the Society of
surgery and at the 2-year follow-up appointment, indi- Neurointerventional Surgery to produce a practice
cating that the treated patients’ advanced adjacent disk parameter for vertebral augmentation.24 The docu-
degeneration did not weaken the clinical outcomes of ment defines vertebral augmentation as percutaneous
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 315
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
techniques used to stabilize a vertebral body, and it 70% of a vertebra has been compressed, an insufficient
deals primarily with vertebroplasty and kyphoplasty. amount of bone remains in which the procedure can
In the document, which has been renamed as a take place.2 Young patients with healthy bones who
practice parameter and revised in 2014, the authoring have a vertebral compression fracture from an accident
committee described the indications and timing for should not have vertebral augmentation. Their bones
when augmentation is warranted after the first line of are able to heal more readily than those of elderly
treatment for vertebral compression fractures, medi- patients, and no data on the long-term effects of verte-
cal therapy, fails. Typically, medical therapy for verte- broplasty or kyphoplasty exist. 4 These procedures also
bral compression fractures is deemed as failed when a are not meant for patients with scoliosis or kyphosis
patient has pain that persists at a level that leads to the caused by diseases other than osteoporosis, nor for
patient not being ambulatory for periods as long as 24 patients with herniated disks or spinal stenosis. 4
hours, even though the patient is receiving pain control
from analgesics. In other cases, a patient cannot toler- Alternative Augmentation Procedures
ate physical therapy, or therapy to relieve pain from New bioactive cements that can induce bone devel-
weakened or fractured vertebral bodies leads to adverse opment have been introduced to the marketplace.24 One
effects such as confusion, oversedation, or constipation. of these is CORTOSS (Orthovita), a composite that
Patients who have augmentation procedures should be has resin and bioactive glass fibers in it; patients who
symptomatic and have fractures confirmed by imaging have been treated with this cement have had fewer sub-
or vertebral bodies confirmed as weakened by tumors. sequent vertebral compression fractures. 6 Another new
Prevention of future fractures is not considered an cement additive is radiopaque strontium. In studies,
appropriate indication for the procedures.24 strontium has been shown to prompt new bone devel-
The practice parameters also clarify several contrain- opment and prevent bone resorption; the substance’s
dications to vertebral augmentation. Patients who have radiopaque properties can improve its visibility under
osteomyelitis (active infection) of the affected vertebra image guidance for cement injection.25
should not have the procedure. A systemic infection New tools also have been developed in recent years.
(septicemia) also is considered a contraindication, as is An expandable polymer bone tamp called SKy Bone
allergy to cement or contrast materials. Patients with Expander (Disc-O-Tech Medical Technologies Ltd)
certain clotting disorders that cannot be corrected with uses a polymer instead of a balloon to expand a defined
medications prior to or during the procedure should not cavity during the procedure. 6,31
have vertebral augmentation. A new technique called radiofrequency-targeted ver-
Other possible contraindications should be consid- tebral augmentation modifies the kyphoplasty proce-
ered by physicians recommending vertebral augmenta- dure.25 The physician directs warm, viscous polymethyl
tion to relieve symptoms in patients with compression methacrylate using radiofrequency activation through
fractures. Some patients have pain that extends beyond an osteotome (chisellike instrument) into the middle
local vertebral pain that is unrelated to the vertebral third of the vertebral body. The radiofrequency-activated
collapse. Pathology such as extension of a tumor into cement does not harden prematurely and improves pre-
the spinal canal or a fracture fragment compromising cision of delivery. Further research is needed for radio-
the spinal canal could contraindicate augmentation. frequency injection of bone cement.25
Further, some patients improve with medical therapy Vesselplasty is an additional modification of kypho-
during preparation for augmentation.24 plasty that involves leaving a balloon in the patient’s
Physicians also must consider whether an individual vertebra to minimize the risk of cement leakage. 6 A
patient can tolerate anesthesia if required, along with 2013 article published the results of vesselplasty to treat
a patient’s cardiac and pulmonary reserve, which must tumor-associated vertebral compression fractures in 9
be considered for the procedure length, anesthesia, and patients. None of the patients experienced cement leak-
the prone position typically used for the procedure.1 If age and their pain and disability improved significantly
316 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
despite initially having fractures that caused major pos- At the time of the actual or sham procedure, most
terior wall deficiency. A limitation of the study was its participants’ fractures were chronic (the average
small sample size.32 age of fractures was 4 to 5 months for the Kallmes
Another procedure uses VerteLift (SpineAlign et al study and 2 months for the Buchbinder et al
Medical Inc), a nitinol (nickel-titanium alloy) device. study) as opposed to acute ( 4 weeks old) when
A compressed nitinol cage is inserted into the verte- vertebroplasty is thought to be the most effective.
bra after a space has been drilled out with a coaxial Failure to include vertebroplasty for fractures
manual drill. Once in place, the cage is opened and caused by malignancies.
filled with polymethyl methacrylate.25 The technique Failure to compare vertebroplasty to medical
has demonstrated effectiveness in preventing future therapy options.
vertebral height loss, and no cement leakage has been Additional research published since 2009 addresses
observed.25 the continuing discussion regarding treatment options
Finally, the Kiva VCF Treatment System for vertebral compression fractures. The VERTOS IV is
(Benvenue Medical) is a coillike nitinol insert filled an ongoing trial that compares vertebroplasty to a sham
with cement to maintain the latticelike, spongy bone procedure. 37 Study results are expected in late 2014;
architecture of the vertebra and raise the endplates. A however, the information was unavailable prior to publi-
study comparing the device (n 26) to kyphoplasty cation of this Directed Reading article. 38
(n 26) in patients with osteoporotic vertebral com- In 2013, Van Meirhaeghe et al published a report that
pression fractures found that the Kiva system required compared patients undergoing kyphoplasty (n 149) to
less procedure time, produced fewer subsequent frac- patients undergoing medical therapy (n 151) and found
tures, and resulted in about the same rate of cement that the patients who had kyphoplasty reported a better
leakage as the kyphoplasty procedures. 33 The reduc- quality of life and less pain than those who underwent
tion in subsequent vertebral compression fractures medical therapy only.20 Patients who received vertebral
could be attributed to the lower volume of cement augmentation had significantly greater restoration of their
required to fill the coils (2.2-2.6 mL) compared to kyphotic angulation and vertebral height. The authors
kyphoplasty (4.7-7.5 mL). The increased volume used also noted that mounting evidence supports kyphoplasty
in kyphoplasty possibly equates to more force applied and vertebroplasty as more cost-effective than medical
to the adjacent vertebrae. 33 treatment,20 perhaps because patients who have received
augmentation have fewer subsequent visits to their physi-
Medical Therapy vs Augmentation cians because of back pain.25
Vertebroplasty, kyphoplasty, and nonsurgical A study published by Kim et al in 2013 surveyed
approaches currently are used to manage vertebral 430 patients in Korea whose osteoporotic vertebral
compression fractures. Determining which approach is compression fractures had been managed either medi-
optimal for each patient can present clinical challenges. cally (63%) or with vertebroplasty (37%). 39 The authors
In 2009, research articles that compared vertebroplasty found no significant difference between the 2 groups’
to a feigned surgery (sham procedure) were published scores for patients’ self-reported pain assessment or dis-
by Buchbinder et al and Kallmes et al in the New ability. In addition, 75% of patients from both groups
England Journal of Medicine.34,35 Each trial concluded were satisfied with their treatment outcomes.
that patients with osteoporosis-associated vertebral Kim et al’s findings were similar to the findings of
compression fractures who had vertebroplasty did not Buchbinder et al and Kallmes et al, but Kim et al sup-
benefit from the procedure compared with patients ported vertebroplasty for certain patients, such as those
who underwent the sham procedure. These conclusions who are elderly and have both osteoporotic fractures
elicited a debate, including claims of the following flaws and chronic lung diseases. Kim et al also expressed
with the studies1,36: a need for more patients to defend against vertebral
Small sample sizes. compression fractures with medication that inhibits or
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 317
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
delays osteoporosis, stating that 87% of their study’s strength has been shown to have a higher significance
patients had not taken any preventive medications in maintaining quality of life than other influential fac-
before the first vertebral compression fracture, 35% of tors such as kyphotic angle and bone mineral density.1
which occurred without trauma. 39 Physicians and therapists must carefully choose
In 2012, Papanastassiou et al published the results of weight-bearing exercises for patients with compression
a literature review that included 27 studies, each with at fractures and osteoporosis, ensuring that the exercise
least 20 patients who were involved in prospective mul- does not overstrain the spine and cause a new fracture.1
tiarm studies comparing kyphoplasty, vertebroplasty, or One study found that postmenopausal women who
medical therapy. The authors found the following40: performed abdominal flexion exercises had an 89%
Pain relief was superior for patients receiving ver- rate of additional fractures associated with the exercise,
tebral augmentation compared with those who compared with just 16% who experienced additional
had medical therapy only. fractures after performing back extension exercises.1
No difference in pain relief was seen between Wong and McGirt recommended isometric contrac-
patients who had vertebroplasty and kyphoplasty. tion of paraspinal muscles and weight-bearing exercises
More subsequent fractures occurred in the group for the upper body. They also recommended the spinal
managed with no augmentation (22%) compared proprioception extension exercise dynamic (developed
with those having vertebral augmentation (11%). by Mehrsheed Sinaki) that can be performed twice
Kyphoplasty resulted in greater kyphosis reduc- daily for 20 minutes each.1 Women with osteoporosis
tion (4.88) than vertebroplasty (1.78). who participated in the workout during a study con-
Quality of life scores were better for patients ducted by Sinaki et al reported less back pain, more
undergoing kyphoplasty than for those who had back strength, and a reduced risk of falling or fear of
vertebroplasty. falling. Computer analysis of the study’s participants
Kyphoplasty was associated with fewer incidents confirmed that they had improved gait and posture.1
of cement extravasation than was vertebroplasty. Yoga is an additional option to help patients with
Augmentation within 7 weeks of incurring a osteoporosis avoid inactivity that can lead to progres-
vertebral compression fracture provided the best sive bone loss. Benefits of yoga include strengthening
results vs waiting longer. of the trunk muscles to support vertebrae, improved
In 2012, Ma et al came to similar conclusions after balance, and loosening of hip extensors to address tight
the authors conducted a literature search and graded hamstrings and prevent hyperkyphosis. In a 2013 arti-
the quality of studies, including a randomized trial and cle, authors Smith and Boser noted that yoga teachers
11 nonrandomized trials for a total of 1081 patients. 41 should pay careful attention to clients with osteoporosis
The authors concluded that both kyphoplasty and ver- because flexion and twisting motions can cause ver-
tebroplasty are safe and effective techniques for osteo- tebral compression fractures. 42 Their literature review
porotic vertebral compression fractures and that kypho- found that patients with osteoporosis could benefit
plasty is slightly better for patients with large kyphosis from strengthening their spinal extensor muscles and
angles, vertebral fissures, breaks in the posterior edge of improve their posture by doing gentle prone or standing
a vertebral body, and significant vertebral height loss. 41 yoga postures. Individuals with severe hyperkyphosis
who cannot perform these postures with a straight
Prevention spine should remain in supine positions without weight-
Because osteoporosis is the main cause of vertebral bearing spinal movements.
compression fractures, gentle exercises to strengthen
the bones might help prevent fractures and have been Conclusion
the subject of many studies. Improved back extension Vertebral compression fractures are a problem-
strength and lumbar mobility are important for post- atic, underdiagnosed condition affecting millions of
menopausal women with osteoporosis. Back extension Americans each year. Radiologic technologists play a
318 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
CE
Directed Reading
Dewar
pivotal role in helping to identify these fractures and 8. Burge R, Dawson-Hughes B, Solomon DH, Wong JB,
assist physicians in determining appropriate manage- King A, Tosteson A. Incidence and economic burden of
ment of symptoms. Medical imaging also is critical to osteoporosis-related fractures in the United States, 2005-
2025. J Bone Miner Res. 2007;22(3):465-475. doi:10.1359
image guidance for vertebral augmentation and the
/jbmr.061113.
patient’s follow-up radiologic assessment.
9. Kondo KL. Osteoporotic vertebral compression fractures
and vertebral augmentation. Semin Intervent Radiol. 2008;
25(4):413-424. doi:10.1055/s-0028-1103000.
Cherie Dewar, BS, is a freelance medical writer and 10. Fourney DR, Schomer DF, Nader R, et al. Percutaneous ver-
president of Hummingbird Medical Communications. She has tebroplasty and kyphoplasty for painful vertebral body frac-
written a previous Radiologic Technology Directed Reading tures in cancer patients. J Neurosurg. 2003;98(1 suppl):21-30.
and contributed to ASRT Scanner. Dewar specializes in 11. Aebi M. Spinal metastasis in the elderly [published online
writing and editing patient education materials, manuscripts, ahead of print September 23, 2003]. Eur Spine J. 2003;12
pharmaceutical marketing material, drug dossiers, and (suppl 2):S202-213.
meeting summaries. She is the president-elect of the American 12. Anselmetti GC, Bernard J, Blattert T, et al. Criteria for the
appropriate treatment of osteoporotic vertebral compression
Medical Writers Association’s mid-Atlantic chapter. fractures. Pain Physician. 2013;16(5):E519-E530.
Reprint requests may be mailed to the American Society 13. Cho JH, Shin SI, Lee JH, Yeom JS, Chang BS, Lee CK.
of Radiologic Technologists, Communications Department, Usefulness of prone cross-table lateral radiographs in verte-
at 15000 Central Ave SE, Albuquerque, NM 87123-3909, bral compression fractures. Clin Orthop Surg. 2013;5(3):195-
or e-mailed to communications@asrt.org. 201. doi:10.4055/cios.2013.5.3.195.
© 2015 American Society of Radiologic Technologists 14. Jang JS, Kim DY, Lee SH. Efficacy of percutaneous vertebro-
plasty in the treatment of intravertebral pseudarthrosis asso-
References ciated with noninfected avascular necrosis of the vertebral
1. Wong CC, McGirt MJ. Vertebral compression fractures: a body. Spine (Phila PA 1976). 2003;28(14):1588-1592.
review of current management and multimodal therapy. J 15. Aggarwal A, Salunke P, Shekhar BR, et al. The role of mag-
Multidiscip Healthc. 2013;6:205-214. doi:10.2147/JMDH netic resonance imaging and positron emission tomography-
.S31659. computed tomography combined in differentiating benign
from malignant lesions contributing to vertebral compression
2. Harvard Women’s Health Watch. Treating osteoporotic frac-
fractures. Surg Neurol Int. 2013;4(suppl 5):S323-S326.
tures of the spine. http://www.health.harvard.edu/newslet
ters/Harvard_Womens_Health_Watch/2008/December 16. Qian J, Yang H, Jing J, et al. The early stage adjacent disc
/Treating_osteoporotic_fractures_of_the_spine. Published degeneration after percutaneous vertebroplasty and kypho-
December 2008. Accessed March 1, 2014. plasty in the treatment of osteoporotic VCFs. PLoS One.
2012;7(10):e46323. doi:10.1371/journal.pone.0046323.
3. Moore KL, Dalley AF. Back (chapter 4). In: Sun B, Scogna K,
Glazer J, Odyniec C, eds. Clinically Oriented Anatomy. 5th ed: 17. National Library of Medicine. Drugs, supplements, and herbal
Lippincott Williams & Wilkins; 2006: http://dermatologic information. MedlinePlus. http://www.nlm.nih.gov/medline
.com.ar/4.htm. Accessed February 16, 2014. plus/druginformation.html. Accessed September 10, 2014.
18. Bisphosphonates (marketed as Actonel, Actonel+Ca, Aredia,
4. Radiological Society of North America. Vertebroplasty &
Boniva, Didronel, Fosamax, Fosamax+D, Reclast, Skelid, and
kyphoplasty. RadiologyInfo.org. http://www.radiologyinfo
Zometa) Information. U.S. Food and Drug Administration
.org/en/info.cfm?pg=vertebro. Reviewed August 5, 2013.
Web site. http://www.fda.gov/drugs/drugsafety/postmarket
Accessed March 1, 2014.
drugsafetyinformationforpatientsandproviders/ucm101551
5. Ensrud KE, Schousboe JT. Vertebral fractures. N Engl J Med. .htm. Updated September 1, 2011. Accessed September 9, 2014.
2011;364(17):1634-1642. doi:10.1056/NEJMcp1009697.
19. Understanding osteoporosis medications. eMedicineHealth
6. Alexandru D, So W. Evaluation and management of vertebral Web site. http://www.emedicinehealth.com/understand
compression fractures. Perm J. 2012;16(4):46-51. ing_osteoporosis_medications/page7_em.htm. Accessed
7. Briggs AM, Geig AM, Hodges PW. Paraspinal muscle control September 10, 2014.
in people with osteoporotic vertebral fracture. Eur Spine J. 20. Van Meirhaeghe J, Bastain L, Boonen S, Ranstam J, Tillman
2007;16(8):1137-1144. doi:10.1007/s00586-006-0276-8. JB, Wardlaw D. A randomized trial of balloon kyphoplasty
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 319
CE
Directed Reading
Diagnosis and Treatment of Vertebral Compression Fractures
and nonsurgical management for treating acute vertebral patients - preliminary results. Rofo. 2013;185(4):340-350.
compression fractures: vertebral body kyphosis correc- doi:10.1055/s-0032-1330443.
tion and surgical parameters. Spine. 2013;38(12):971-983. 33. Otten LA, Bornemnn R, Jansen TR, et al. Comparison of
doi:10.1097/BRS.0b013e31828e8e22. balloon kyphoplasty with the new kiva VCF system for the
21. Malmros B, Mortensen L, Jensen MB, Charles P. Positive treatment of vertebral compression fractures. Pain Physician.
effects of physiotherapy on chronic pain and performance in 2013;16(5):E505-E512.
osteoporosis. Osteoporos Int. 1998;8(3):215-221. 34. Buchbinder R, Osborne RH, Ebeling PR, et al. A randomized
22. Bennell KL, Matthews B, Greig A, et al. Effects of an exercise trial of vertebroplasty for painful osteoporotic vertebral frac-
and manual therapy program on physical impairments, func- tures. N Engl J Med. 2009;361(6):557-568. doi:10.1056/NEJ
tion and quality-of-life in people with osteoporotic vertebral Moa0900429.
fracture: a randomised, single-blind controlled pilot trial. 35. Kallmes DF, Comstock BA, Heagerty PJ, et al. A randomized
BMC Musculoskelet Disord. 2010;11:36. trial of vertebroplasty for osteoporotic spinal fractures. N Engl
23. Papaioannou A, Adachi JD, Winegard K, et al. Efficacy of J Med. 2009;361(6):569-579. doi:10.1056/NEJMoa0900563.
home-based exercise for improving quality of life among 36. Kinkade S, Stevermer JJ. Vertebroplasty for osteoporotic frac-
elderly women with symptomatic osteoporosis-related verte- ture? Think twice. J Fam Pract. 2009;58(12):654-656.
bral fractures. Osteoporos Int. 2003;14(8):677-682. 37. Firanescu C, Lohle PN, de Vries J, et al. A randomised sham
24. American College of Radiology. ACR–ASNR–ASSR–SIR– controlled trial of vertebroplasty for painful acute osteopo-
SNIS practice parameter for the performance of vertebral rotic vertebral fractures (VERTOS IV). Trials. 2011;12:93.
augmentation. http://www.acr.org/~/media/ACR/Docu 38. Spinal News International. VERTOS IV study uses strict
ments/PGTS/guidelines/Vertebral_Augmentation.pdf. inclusion criteria. http://www.spinalnewsinternational.com
Amended 2014. Accessed March 1, 2014. /sn-features/spinal-news---features/vertos-iv-study-uses
25. Yimin Y, Zhiwei R, Wei M, Jha R. Current status of percu- -strict-inclusion-criteria. Published January 9, 2014. Accessed
taneous vertebroplasty and percutaneous kyphoplasty--a March 22, 2014.
review. Med Sci Monit. 2013;19:826-836. doi:10.12659/MSM 39. Kim KW, Cho KJ, Kim SW, Lee SH, An MH, Im JH. A
.889479. nation-wide, outpatient-based survey on the pain, disabil-
26. Gray DT, Hollingworth W, Onwudiwe N, Deyo RA, Jarvik ity, and satisfaction of patients with osteoporotic vertebral
JG. Thoracic and lumbar vertebroplasties performed in US compression fractures. Asian Spine J. 2013;7(4):301-307.
Medicare enrollees, 2001-2005. JAMA. 2007;298(15):1760- doi:10.4184/asj.2013.7.4.301.
1762. 40. Papanastassiou ID, Phillips FM, Van Meirhaeghe J, et al.
27. Harvard Health Publications. Osteoporosis: A guide to prevention Comparing effects of kyphoplasty, vertebroplasty, and
and treatment. Boston, MA: Harvard Medical School; 2010. non-surgical management in a systematic review of random-
28. Satre TJ, Mackler L, Birch JT Jr. Clinical inquiries. Who ized and non-randomized controlled studies. Eur Spine J.
should receive vertebroplasty? J Fam Pract. 2006;55(7): 2012;21(9):1826-1843.
637-638. 41. Ma XL, Xing D, Ma JX, Xu WG, Wang J, Chen Y. Balloon
29. Chung SE, Lee SH, Kim TH, Yoo KH, Jo BJ. Renal cement kyphoplasty versus percutaneous vertebroplasty in treating
embolism during percutaneous vertebroplasty [published osteoporotic vertebral compression fracture: grading the
online ahead of print December 14, 2005]. Eur Spine J. 2006; evidence through a systematic review and meta-analysis. Eur
15(suppl 5):590-594. doi:10.1007/s00586-005-0037-0. Spine J. 2012;21(9):1844-1859.
30. Machikanti L, Pampati V, Hirsch JA. Analysis of utiliza- 42. Smith EN, Boser A. Yoga, vertebral fractures, and osteo-
tion patterns of vertebroplasty and kyphoplasty in the porosis: research and recommendations. Int J Yoga Therap.
Medicare population. J NeuroIntervent Surg. 2013;5:467-472. 2013;23(1):17-23.
doi:10.1136/neurintsurg-2012-010337.
31. Seel EH, Davies EM. A biomechanical comparison of kypho-
plasty using a balloon bone tamp versus an expandable poly-
mer bone tamp in a deer spine model. J Bone Joint Surg Br.
2007;89(2):253-257.
32. Klingler JH, Sircar R, Deininger MH, Scheiwe C, Kogias E,
Hubbe U. Vesselplasty: A new minimally invasive approach
to treat pathological vertebral fractures in selected tumor
320 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
Directed Reading Quiz
15801-02
1.0 Category A+ credits
Original Expiration Date:
Feb. 28, 2017* Diagnosis and Treatment of
Renewed through
Mar. 1, 2020*
Vertebral Compression Fractures
To earn continuing education credit:
Take this Directed Reading quiz online at asrt.org/drquiz.
Or, transfer your responses to the answer sheet on Page 326 and mail to:
Processing Center, 2908 Stewart Creek Blvd., Charlotte, NC 28216.
New and rejoining members are ineligible to take DRs from journal issues published prior to their most recent join date
unless they have purchased access to the quiz from the ASRT. To purchase access to other quizzes, go to asrt.org/store.
* Your answer sheet for this Directed Reading must be received in the ASRT office on or before this date.
Some quizzes are renewed and the expiration date extended. Check online at asrt.org/drquiz or
call Member Services at 800-444-2778.
Read the preceding Directed Reading and choose the answer that is most correct based on the article.
1. A vertebral compression fracture is best described 3. The ______ is the oval-shaped structure attached
as a ______ bone. anteriorly to the vertebral arch that protects the
a. snapped spinal cord.
b. condensed a. superior end plate
c. ruptured b. vertebral body
d. shattered c. inferior end plate
d. spinal nerve
2. An adult vertebra is made up of which of the
following? 4. Most vertebral compression fractures occur in the
1. vertebral body ______ region of the vertebral column.
2. vertebral arch a. cervical
3. spinous process b. thoracolumbar
c. sacral
a. 1 and 2 d. coccygeal
b. 1 and 3
c. 2 and 3 5. What is the predominant cause of vertebral
d. 1, 2, and 3 compression fractures?
a. trauma
b. cancer
c. osteoporosis
d. infection
continued on next page
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 321
Directed Reading Quiz
6. A T-score between 21 and 22.5 is defined by the 11. A ______ % decrease in vertebral height is needed
World Health Organization as: to diagnose a vertebral compression fracture.
a. osteoarthritis. a. 10
b. osteomalacia. b. 15
c. osteoporosis. c. 20
d. osteopenia. d. 25
7. Which of the following are risk factors for 12. Which imaging examination can help determine
developing a vertebral compression fracture? the condition of the spinal ligamentous complex
1. chronic obstructive pulmonary disease and inform a surgical or interventional team of a
2. impaired eyesight fracture’s stability?
3. obesity a. lateral radiograph
b. MR short tau inversion recovery
a. 1 and 2 c. helical CT scan
b. 1 and 3 d. nuclear medicine bone scan
c. 2 and 3
d. 1, 2, and 3 13. When a patient is ready, performing gentle exercises
such as swimming or walking is recommended.
8. Which of the following is not an effect of severe a. true
kyphosis? b. false
a. pulmonary impairment
b. protruding abdomen 14. What could happen if a patient wears a brace for
c. back sores more than 3 months?
d. poor nutrition a. weakened core muscles
b. tightened back muscles
9. Which part of the population is most likely to c. additional vertebral compression fractures
experience a vertebral compression fracture? d. altered posture
a. men
b. postmenopausal women 15. Before vertebral augmentation, which type of
c. African American women imaging is used to confirm a vertebral compression
d. young adults fracture and display possible disk, spinal cord, or
soft tissue involvement?
10. Which diagnostic imaging examination is used a. lateral radiograph
most often to diagnose vertebral compression b. MR scan
fractures? c. CT scan
a. lateral radiograph d. nuclear medicine bone scan
b. magnetic resonance (MR) scan
c. computed tomography (CT) scan
d. nuclear medicine bone scan
continued on next page
322 RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3
Directed Reading Quiz
16. According to the article, during a vertebroplasty,
the lateral and anteroposterior fluoroscopic images
should display the ______ clearly for trocar
position.
a. intravertebral foramen
b. balloon
c. pedicles
d. spreader
17. Which contrast agent is most often used in the
cement for vertebroplasty or kyphoplasty?
a. barium sulfate
b. tantalum powder
c. tungsten
d. zirconium dioxide
18. The chances of restoring vertebral height are best
when kyphoplasty is performed ______ the
vertebral compression fracture occurrence.
a. within 3 weeks of
b. within 3 months of
c. after 3 months have passed since
d. after 6 months have passed since
19. According to the American College of Radiology
and collaborating societies, which is not an
indication for vertebral augmentation?
a. failure of medical therapy to ease symptoms
b. vertebral bodies weakened by neoplasm
c. symptomatic fracture
d. prevention of future fractures
20. Patients with herniated disks and scoliosis can be
treated with kyphoplasty or vertebroplasty.
a. true
b. false
RADIOLOGIC TECHNOLOGY, January/February 2015, Volume 86, Number 3 323
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5795)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1091)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- ADULT TRUMA FRCS Practice MCQsDokument112 SeitenADULT TRUMA FRCS Practice MCQsmonkeyzergNoch keine Bewertungen
- UKITE 07 AnswersDokument46 SeitenUKITE 07 AnswersJipin Gopi100% (1)
- Pediatric Orthopedic Surgical EmergenciesDokument237 SeitenPediatric Orthopedic Surgical EmergenciesOrlando Rodríguez Gavilanes100% (2)
- Principles in Fracture ManagementDokument60 SeitenPrinciples in Fracture ManagementNge NgeNoch keine Bewertungen
- POC NotesDokument3 SeitenPOC NotesJosef SuenoNoch keine Bewertungen
- 2006 @dentallib Pradip K Ghosh Synopsis of Oral and MaxillofacialDokument220 Seiten2006 @dentallib Pradip K Ghosh Synopsis of Oral and MaxillofacialVictor PerdomoNoch keine Bewertungen
- AOCMF Brochure ISS5 A4 04 LRDokument16 SeitenAOCMF Brochure ISS5 A4 04 LRDea Alberta SNoch keine Bewertungen
- Nomenklatur IBS Edit THTDokument291 SeitenNomenklatur IBS Edit THTriezki_pattikratonMDNoch keine Bewertungen
- Research Article: Epidemiology of Maxillofacial Fractures at A Teaching Hospital in Malaysia: A Retrospective StudyDokument11 SeitenResearch Article: Epidemiology of Maxillofacial Fractures at A Teaching Hospital in Malaysia: A Retrospective Studydr_nadheemNoch keine Bewertungen
- Roles of Trauma CT and Cta in Salvaging Threateaned or Mangled ExtremityDokument18 SeitenRoles of Trauma CT and Cta in Salvaging Threateaned or Mangled ExtremityJEAN CARLOS GALLO VALVERDENoch keine Bewertungen
- OsteosintesisDokument15 SeitenOsteosintesisNicolásNoch keine Bewertungen
- Case Study July 19Dokument2 SeitenCase Study July 19Vinay ShankerNoch keine Bewertungen
- 7 Sports InjuriesDokument33 Seiten7 Sports Injuriesapi-286702267Noch keine Bewertungen
- BSHM 55 - Lesson 9 & 10Dokument9 SeitenBSHM 55 - Lesson 9 & 10Yisu HimaaNoch keine Bewertungen
- Rao 2017Dokument2 SeitenRao 2017Guma KipaNoch keine Bewertungen
- Attending Osteomyelitis ModuleDokument9 SeitenAttending Osteomyelitis ModuleMrLarry DolorNoch keine Bewertungen
- SoK Ortho MedExDokument14 SeitenSoK Ortho MedExsharvindan subramaniamNoch keine Bewertungen
- Extensor Tendon Injuries in The HandDokument8 SeitenExtensor Tendon Injuries in The HandkenthepaNoch keine Bewertungen
- Musculosceletal Block: Prof - Dr.Dr. Bambang Pardjianto, SPB., Spbp-Re (K)Dokument32 SeitenMusculosceletal Block: Prof - Dr.Dr. Bambang Pardjianto, SPB., Spbp-Re (K)Irsyad Robani WNoch keine Bewertungen
- Orthopaedics Diagnosis & Therapy: Dr. Su Djie To Rante, M.Biomed, SP - OTDokument75 SeitenOrthopaedics Diagnosis & Therapy: Dr. Su Djie To Rante, M.Biomed, SP - OTDiana MarcusNoch keine Bewertungen
- 3.9 C.IM.07 Instructions For Use of Spinal Implants (R3-01.10.2018) ProsDokument2 Seiten3.9 C.IM.07 Instructions For Use of Spinal Implants (R3-01.10.2018) Prosibrahim kademogluNoch keine Bewertungen
- CT TractionDokument3 SeitenCT TractionLaira CañeteNoch keine Bewertungen
- Radius and UlnaDokument12 SeitenRadius and UlnaMauricio OjedaNoch keine Bewertungen
- Simple Future TenseDokument5 SeitenSimple Future TenseJULITANoch keine Bewertungen
- Orthopedic Surgery ReviewerDokument7 SeitenOrthopedic Surgery ReviewerAzria John DemetriNoch keine Bewertungen
- Treatment of Cominuted Acetabular Fractures Using Ilizarov Ligamentotaxis and Minimal Fixation. Nuno Craveiro LopesDokument3 SeitenTreatment of Cominuted Acetabular Fractures Using Ilizarov Ligamentotaxis and Minimal Fixation. Nuno Craveiro LopesNuno Craveiro Lopes100% (1)
- G11-Principles of External FixationDokument111 SeitenG11-Principles of External Fixationhello from the other side100% (1)
- Judo Ortho InjuriesDokument21 SeitenJudo Ortho InjuriesKritss ClaudiuNoch keine Bewertungen
- Orthopaedic SplintingDokument52 SeitenOrthopaedic SplintingandhitaNoch keine Bewertungen
- Osteopenia & Osteoporosis - Basic Science - Orthobullets PDFDokument5 SeitenOsteopenia & Osteoporosis - Basic Science - Orthobullets PDFMelAcostaNoch keine Bewertungen