Beruflich Dokumente
Kultur Dokumente
100 Thoughts
Hochgeladen von
raju_pnOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
100 Thoughts
Hochgeladen von
raju_pnCopyright:
Verfügbare Formate
100 thoughts for the critical care practitioner in the new
millennium
Cory Franklin, MD
THOUGHTS ON MAKING 10. The patient who comes into the indication for positive pressure ventila-
DIAGNOSES ICU with a normal serum sodium and tion.
experiences hyponatremia or hypernatre- 20. Most patients receiving mechani-
1. Making a diagnosis is only impor- mia in the ICU is usually the victim of cal ventilation do not require paralyzing
tant as it relates to treating the patient or iatrogenesis. drugs. The ones that do rarely need pa-
providing a prognosis; do not chase a 11. Whenever confronted with an un- ralysis for ⬎48 hrs. Make a point on
diagnosis simply as an intellectual exer- usual drug overdose, draw two extra rounds of discontinuing paralytics as
cise. tubes of blood right away. Label and re- soon as possible, especially in patients
2. When a patient’s mental status de- frigerate them; you may need them later. with status asthmaticus receiving high
teriorates suddenly and unexpectedly in 12. In patients with severe, chronic dose corticosteroids.
the intensive care unit (ICU), first check hypoxemia and no obvious etiology, re- 21. When the issue is whether or not a
the chart. Look at the medicines the pa- member to take an occupational history. patient is septic, the most important
tient has been receiving as well as the Some of those patients were chronically question is “how sick is the patient?” If
recent orders. exposed to pulmonary toxins in their em- the patient is sick, begin antibiotics im-
3. There is no physical finding or lab ployment.
mediately; if the patient is not too sick,
abnormality in sepsis or pulmonary em- 13. Some diagnoses will not be made
wait and see how he or she progresses
bolism that is invariably present. This by you.
and what the results of cultures are.
includes fever in sepsis and hypoxemia in 22. The goal of antibiotic therapy in
pulmonary embolism. critically ill patients is to narrow cover-
THOUGHTS ON THERAPY
4. Feel the feet of a patient in shock—
age, not to broaden it. The general rule is
a patient with warm toes does not have 14. Maintain a healthy respect for air- that the initial antibiotic coverage should
cardiogenic shock. way problems—they are the greatest only be broadened when the patient is
5. Histories given by drug users are source of preventable disasters. clinically deteriorating.
unreliable. 15. There is no such thing as a medi- 23. There should only be one person in
6. When the patient’s arterial blood cation or a surgery completely without charge of a cardiac resuscitation. At the
gases tell you he is ill and you do not risk. Anyone who tells you otherwise is end of the resuscitation that person
think he is, remember one of two things fooling himself or herself.
is at work— either you’re wrong or the should thank everyone who participated
16. Avoid treating the heart rate of a whether or not the resuscitation was suc-
blood gases will improve. patient with sinus tachycardia. If you ab-
7. Most patients who carry a diagnosis cessful.
solutely feel you must treat, treat the 24. Not every patient who carries the
of “rule out pulmonary embolism” do not cause.
have a pulmonary embolism. The trick is diagnosis of delirium tremens is suffering
17. Nobody ever died of peripheral
figuring out which ones do. from delirium tremens. Be reasonably
edema. It took a while for it to accumu-
8. Soft tissue infections of the extrem- certain when you treat delirium tremens
late and it takes a while for it to disap-
ity should always receive a radiograph, that is what the patient has.
pear. Do not try to make it go away too
surgical consult, and culture of the outer fast. 25. New medications are being intro-
border of the wound. 18. The most difficult decision in a duced all the time. Make an effort to learn
9. The neurologic examination in the critically ill pregnant patient is generally about them but remember that it is bet-
ICU is different from the standard neuro- whether and when to deliver the baby. ter to know several medicines well than it
logic examination. Become familiar with This decision is best made in conjunction is to know many superficially.
how to do it. Do not call a neurology with the gynecologist, anesthesiologist, 26. Review a patient’s medications on
consult just for a good examination. and neonatologist all talking with you in rounds daily. Look for medications that
the same room. Unfortunately, the deci- can be discontinued and discontinue
sion is all too often not made that way. them.
19. Patients in shock who are in the 27. Osler called morphine “God’s Own
From the Medical Intensive Care Unit, Cook County stage of metabolic acidosis often cannot Medicine.” The uses it has in critical
Hospital, Chicago, IL.
Key Words: intensive care unit; critical care med- be stabilized unless mechanical ventila- care—pain control, sedation, treatment
icine tion is instituted. Progressive metabolic of pulmonary edema, reducing work of
Copyright © 2000 by Lippincott Williams & Wilkins acidosis in the patient with shock is an breathing—make it a drug every critical
3050 Crit Care Med 2000 Vol. 28, No. 8
care practitioner should know how to to see results after three consecutive tries 52. Some elderly doctors who have
use. of the same approach, leave it for some- never practiced critical care are really
one else to try. wise—learn who they are.
ON CATHETERS AND TUBES 38. Practicing critical care is like liv- 53. Some elderly doctors who have
ing life—it’s hard for everybody and never practiced critical care are not really
28. A patient receiving mechanical harder if you’re stupid. wise—learn who they are.
ventilation that had been quiet and sud- 39. When practicing critical care, it’s 54. There are three reasons to call a
denly becomes agitated should never be an advantage to be smart. But the best consultant—you need help or advice, you
sedated until the following have been critical care doctors are those who pay want to learn something, or you want the
checked: tube patency, breath sounds, attention to detail. Some smart critical consultant to observe the same phenom-
and oxygen saturation. Breaking this rule care doctors have never learned that. enon you are seeing.
will eventually lead to disaster. 40. Most people who work in the hos- 55. A good consultant sees a sick ICU
29. The four indications for endotra- pital are afraid of, or intimidated by, the patient more than once a day.
cheal intubation are to bypass an ob- ICU and everything that goes with it. It 56. Respect the consultant who wants
structed airway, to provide positive pres- can be a frightening place (think of your to learn from you.
sure, to provide airway protection, or to first time there). Your ability to practice 57. The two biggest mistakes inter-
provide tracheobronchial toilet. Be aware critical care lies in the fact you have over- nists make when consulting surgeons in
of what the indication is every time you come that fear and intimidation. the ICU is either believing everything
intubate a patient and always ask yourself 41. Do not practice critical care with they say or believing nothing they say—
if the indication is gone before you extu- an eye toward avoiding lawsuits. The best the opinion must be put in perspective
bate the patient. strategy for avoiding lawsuits is to work because the surgeon hasn’t been born
30. Any time any catheter is not func- hard, act in good faith, and establish a who is always right or always wrong.
tioning properly, the first question you good rapport with patients and families. 58. The biggest mistake surgeons
should ask is, “Does the patient need make when consulting internists in the
this?” JUDGMENT, SUCCESS, AND ICU is ignoring them, thus failing to lis-
31. Pulmonary artery catheters pro- FAILURE ten and occasionally learn because they
vide data, not judgment. believe internists suffer from paralysis
32. The doctor who tells you his pa- 42. Good judgment is based on expe- through analysis.
tient cannot be managed without a pul- rience and experience is based on bad 59. The surgeon who knows when not
monary artery catheter generally cannot judgment. to operate is just as valuable as the sur-
manage the same patient with a pulmo- 43. Savor your successes but do so geon who knows when to operate is.
nary artery catheter. It’s not a good idea quickly and then move on— dwelling on Sometimes more so.
to let people who are not familiar with them causes overconfidence.
the catheter tell you when to use it. 44. Learn from your failures but do so THE INTENSIVIST RELATING TO
33. In critically ill patients with pul- quickly and then move on— dwelling on NURSES AND OTHER ICU
monary problems who have pulmonary them causes indecision. PERSONNEL
artery catheters, always draw a mixed ve- 45. Some patients you think will get
60. Listen to the nurses and respect
nous sample from the pulmonary artery. better will get worse.
what they have to say. Like you, some-
Learn to calculate the pulmonary shunt 46. Some patients you think will get
times they’re right and sometimes they’re
and learn what it means. worse will get better.
wrong.
47. When you’re making decisions on
61. Learn the first name of the nurses
PRACTICING CRITICAL CARE rounds, put personal problems aside.
who work in the ICU and call those who
prefer it by their first names.
34. Critical illness goes on 24 hrs a THE INTENSIVIST RELATING TO 62. When you walk into the ICU, you
day, 7 days a week. But because no one THE NONINTENSIVIST have an agenda. The nurses have an
can be with the patient all the time, the
agenda. Your goal should be to make the
best critical care practitioners are those 48. Some doctors believe only those in
agenda they are pursuing and the agenda
who can anticipate problems and delegate their specialty can practice critical care.
you are pursuing the patient’s agenda.
a coherent treatment plan to others. Un- Recognize that there are good critical
63. Nurses and house officers never
like the emergency room, the ICU doesn’t care practitioners in many specialties.
call in the middle of the night to give you
lend itself well to shift work. There are also bad critical care practitio-
good news.
35. Any time you make a critical deci- ners in many specialties. It’s the singer,
64. The most underappreciated mem-
sion right before leaving the hospital, not the song.
ber of the ICU is usually the ward secre-
telephone an hour or two later to check 49. When dealing with other people in
tary.
up. the ICU, say what you mean and mean
65. The respiratory therapist is a close
36. When confronted with a difficult what you say, but pick your spots.
second.
ICU decision, if you’re not sure what to 50. Occasionally, doing the right thing
do, it’s usually a good idea to do nothing. in the ICU means making people upset.
THOUGHTS ON RESPECT FOR
Eventually it will become apparent what 51. Exchange notes frequently with
PATIENT AND FAMILIES
course to take. the physicians in the emergency room.
37. Try a new technique or therapeutic Teach them what you know and learn 66. The hardest thing you’ll ever do in
approach at least once a month. If you fail what they know. critical care medicine is to notify a family
Crit Care Med 2000 Vol. 28, No. 8 3051
of a family member’s unexpected death. general wards or in the emergency de- Given two patients with a blood urea ni-
Nothing else is remotely as difficult. partment who should be in the ICU. Make trogen of 100, one who developed the
67. If a patient who is being mechan- an effort to find them and make sure they problem in a week and the other who
ically ventilated is alert and awake, make get to the ICU. developed the problem over 20 yrs, the
an effort to talk with him or her on 79. The sickest group of patients in the first will generally appear far more ill
rounds. hospital is in the ICU; the next sickest than the second.
68. If a patient who is being mechan- group are the ones who have been trans- 87. Trends are more important than
ically ventilated is not alert and awake, ferred out of the ICU. Keep an eye on single values.
assume that the patient can hear and them. 88. An improvement in renal function
understand what you say on rounds. 80. If you ask a nurse, house officer, or is one of the surest signs a critically ill
69. Urge patients who survived after patient how a critically ill patient is doing patient is getting better.
being very sick in the ICU to visit the ICU and they say, “the same as yesterday,” 89. Informed consent usually is not.
at least once in the next year after they go keep in mind that every patient is either 90. As a wise economist once opined,
home from the hospital. Take a picture of better or worse than yesterday. It may “Data are not facts.”
them with the staff. These visits boost simply not be within the ability of the 91. “Facts are not information.”
everyone’s morale. person to discriminate. Eventually it will 92. “Information is not truth.”
70. Occasionally, when making rounds become obvious. 93. “Truth is not knowledge.”
on a patient likely to die, recall how you 81. In almost every case, it is possible 94. “Knowledge is not wisdom.”
felt when a close relative of yours died. If to keep house officer presentations of 95. As you gain experience in the ICU,
you’ve never had a close relative die, ask new patients to ⱕ5 mins. Have the house you will learn answers to more questions.
someone who has. officers use as few lab values as possible That is the good news. The bad news is
71. Every so often, call the ICU late in during the presentation. that you will also learn there are a greater
the evening. If it takes more than 2 mins 82. The patient who can sit in a chair, number of questions that do not have
for you to make contact with a human eat by himself, and oxygenates adequately answers and that the number of those
voice, make a point of notifying someone via nasal cannula is usually ready to be questions that do not have answers never
about this. Imagine how patients’ fami- transferred out of the ICU. stops growing. Think of it as an infinite
lies feel hearing the phone keep ringing. 83. The patient with a drug overdose jigsaw puzzle where the best you can do
72. Whenever possible, try to individ- who comes to the ICU alive will almost is fit an occasional piece.
ualize the visiting hours for the patient. certainly survive. The three main causes
The posted visiting hours will not be con- of death once the patient is in the ICU are CLOSING QUOTES FOR THE
venient for every family. delayed toxic effect of the drug, aspiration INTENSIVIST
73. Whenever possible, encourage pneumonia, and a repeat suicide attempt
families to become involved in the care of in the hospital (which is preventable). 96. Lao Tzu’s statement that “a jour-
patients. Have them bring food the pa- 84. To avoid burnout, every critical ney of a thousand miles must begin with
tient likes. See if they can assist the care practitioner should do something in a single step” also applies to caring for
nurses in giving baths. Letting a family medicine besides critical care. Surgeons complicated critically ill patients.
member provide mouth care is one of the and anesthesiologists should keep a hand 97. Remember Shakespeare’s words
easiest and most fulfilling tasks there is. in the operating room. Internists should from Julius Caesar, “Of all the wonders
74. Make a point to say hello to the see some non-critical care patients. that I have yet heard, it seems most
patients who are being discharged from strange that men should fear; seeing that
the ICU that day. ICU KOANS—CLINICAL AND death, a necessary end, will come when it
75. As a physician in the ICU, your role will come.”
OTHER
is to be the patient’s advocate. Sometimes 98. Pay heed Hamlet’s advice to Hora-
you are the patient’s only advocate. 85. All intensivists should realize that tio, “There are more things in heaven and
in critical illness, the heart and lungs earth than are dreamt of in your philos-
BRIEF SUGGESTIONS essentially function as one unit. An insult ophy.”
to one will tax the reserve of the other. 99. Remember Cromwell’s famous ad-
76. When in doubt, wash your hands. Those with the best reserve are most monition in a Letter to the Church of
77. If you do not know how, learn to likely to survive. Those with chronic dis- Scotland, “I beseech you, think it possible
read an anesthesia operative record. ease of one are least likely to survive an you may be mistaken.”
Learn why your patient who went to the acute insult to the other. 100. Nearly 2,500 yrs ago Hippocrates
operating room received the anesthetic 86. The loss of reserve of any organ wrote, “Life is short, the art long, timing
regimen that he or she did. system is tolerated differently if the insult is exact, experience treacherous, judg-
78. There are usually one or two pa- is chronic than if the insult is acute. In ment difficult.” An amazingly apt descrip-
tients in the hospital who are on the chronic disease, other organs can adapt. tion of critical care today.
3052 Crit Care Med 2000 Vol. 28, No. 8
Das könnte Ihnen auch gefallen
- ICU Scoring Systems A Complete Guide - 2020 EditionVon EverandICU Scoring Systems A Complete Guide - 2020 EditionNoch keine Bewertungen
- Registered Professional Nurse: Passbooks Study GuideVon EverandRegistered Professional Nurse: Passbooks Study GuideNoch keine Bewertungen
- Set 1Dokument62 SeitenSet 1Alyssa MontimorNoch keine Bewertungen
- Proofed - Nurs 3020 Final EvaluationDokument9 SeitenProofed - Nurs 3020 Final Evaluationapi-313199824Noch keine Bewertungen
- MidtermDokument15 SeitenMidtermapi-400034813Noch keine Bewertungen
- Proofed - Nurs 3021 Final EvaulDokument20 SeitenProofed - Nurs 3021 Final Evaulapi-313199824Noch keine Bewertungen
- Objectives May Be Used To Support Student Reflection, Although The List of Indicators Is NotDokument14 SeitenObjectives May Be Used To Support Student Reflection, Although The List of Indicators Is Notapi-456466614Noch keine Bewertungen
- Sample Questions Nursing ReviewDokument4 SeitenSample Questions Nursing ReviewJenny TorredaNoch keine Bewertungen
- Final EvaluationDokument17 SeitenFinal Evaluationapi-603938769Noch keine Bewertungen
- CCM Study Guide Foundations of NursingDokument46 SeitenCCM Study Guide Foundations of NursingAlexandra BrowneNoch keine Bewertungen
- NURS 421 NCLEX Kaplan Final Exam Predictor TestDokument64 SeitenNURS 421 NCLEX Kaplan Final Exam Predictor TestabbieNoch keine Bewertungen
- D. Preparing The Medication For Bolus AdministrationDokument17 SeitenD. Preparing The Medication For Bolus AdministrationseanNoch keine Bewertungen
- NRSG 2221 Skills Mastery 1 Skills ChecklistDokument2 SeitenNRSG 2221 Skills Mastery 1 Skills ChecklistNi CaoNoch keine Bewertungen
- 2011 Understanding Pharmacology Essentials For Medication SafetyDokument1 Seite2011 Understanding Pharmacology Essentials For Medication SafetygloriyaNoch keine Bewertungen
- Anatomical Orientation QuizDokument1 SeiteAnatomical Orientation QuizUna Furtiva LacrimaNoch keine Bewertungen
- CH 32Dokument8 SeitenCH 32Elizabeth PetersenNoch keine Bewertungen
- Dysrhythmia TestsDokument3 SeitenDysrhythmia TestsKimberly WhitesideNoch keine Bewertungen
- BSC 2085 Anatomy and Physiology NCLEX Final Exam Predictor Study Guide (Verified and Correct Answers, 200 Questions Secure Highscore) Latest 2021Dokument131 SeitenBSC 2085 Anatomy and Physiology NCLEX Final Exam Predictor Study Guide (Verified and Correct Answers, 200 Questions Secure Highscore) Latest 2021abbieNoch keine Bewertungen
- Focus Pharmacology Essentials Health Professionals 3rd Moini Test BankDokument8 SeitenFocus Pharmacology Essentials Health Professionals 3rd Moini Test BankRaadqqqNoch keine Bewertungen
- Intro To Nursinhjcfnhgg - Exam 2 Concepts - Modules 5-8Dokument53 SeitenIntro To Nursinhjcfnhgg - Exam 2 Concepts - Modules 5-8GovindSoniNoch keine Bewertungen
- Question Quiz 1Dokument6 SeitenQuestion Quiz 1Alejandro Daniel Landa MoralesNoch keine Bewertungen
- Handout NSNA Student PresentationDokument14 SeitenHandout NSNA Student PresentationlisaNoch keine Bewertungen
- The Skeletal SystemDokument10 SeitenThe Skeletal SystemAarchi SinghNoch keine Bewertungen
- StudentreportviewerDokument14 SeitenStudentreportviewerapi-403691564100% (1)
- TXTDokument356 SeitenTXTJec AmracNoch keine Bewertungen
- Final 2010 High Yield Supporting Students Book1Dokument114 SeitenFinal 2010 High Yield Supporting Students Book1api-278384508Noch keine Bewertungen
- Chapter 46: Nursing Management: Renal and Urologic Problems Test BankDokument13 SeitenChapter 46: Nursing Management: Renal and Urologic Problems Test BankPrince K. TaileyNoch keine Bewertungen
- 13 Musculoskeletal System - ATFDokument20 Seiten13 Musculoskeletal System - ATFipek terimNoch keine Bewertungen
- Fundamentals of Nursing: Intuitive Nursing/ Primitive Nursing/ Instinctive NursingDokument21 SeitenFundamentals of Nursing: Intuitive Nursing/ Primitive Nursing/ Instinctive NursingDaren Guno LinatocNoch keine Bewertungen
- NURS 6630 Midterm ExamDokument18 SeitenNURS 6630 Midterm ExamNelson MandelaNoch keine Bewertungen
- Q&A Random - 6Dokument10 SeitenQ&A Random - 6api-3818438100% (1)
- Robinson Mejia Preceptor Evaluation of StudentDokument1 SeiteRobinson Mejia Preceptor Evaluation of Studentapi-418543464Noch keine Bewertungen
- Competency Appraisal Safety ExamDokument61 SeitenCompetency Appraisal Safety ExamRubz BulquerinNoch keine Bewertungen
- Biochemistry: Molecules of LifeDokument20 SeitenBiochemistry: Molecules of Lifeapi-464344582Noch keine Bewertungen
- CHAPTER 02 Pharmacology Test BankDokument5 SeitenCHAPTER 02 Pharmacology Test BankseeryneNoch keine Bewertungen
- SAQ Short Form 2006Dokument1 SeiteSAQ Short Form 2006Hanan DaghashNoch keine Bewertungen
- Pharmacology Syllabus Bio 408 Sum 2017Dokument6 SeitenPharmacology Syllabus Bio 408 Sum 2017Grafika DiahNoch keine Bewertungen
- Q&A Health Promotion MaintenanceDokument10 SeitenQ&A Health Promotion Maintenanceapi-3818438100% (1)
- Health Promotion and MaintenanceDokument6 SeitenHealth Promotion and Maintenanceapi-3818438Noch keine Bewertungen
- Safe Use of InsulinDokument44 SeitenSafe Use of InsulinGhada HusseinNoch keine Bewertungen
- 1020 Final EvaluationDokument9 Seiten1020 Final Evaluationapi-456466614Noch keine Bewertungen
- Self-Assessment Vital SignsDokument2 SeitenSelf-Assessment Vital SignscarlyNoch keine Bewertungen
- Nursing exam questions and answersDokument12 SeitenNursing exam questions and answersJagveer ChauhanNoch keine Bewertungen
- Concept MapDokument6 SeitenConcept Mapapi-499028250Noch keine Bewertungen
- Chart Notes-Megan JolmaDokument5 SeitenChart Notes-Megan Jolmaapi-317575833Noch keine Bewertungen
- Comprehensive Elsevier Price List June 2012 Subject-WiseDokument47 SeitenComprehensive Elsevier Price List June 2012 Subject-WiseMatin Ahmad KhanNoch keine Bewertungen
- ATI DRUG TABLES Module4 Respiratory Glucocorticoids InhalationDokument1 SeiteATI DRUG TABLES Module4 Respiratory Glucocorticoids InhalationnoeyeshaveseenNoch keine Bewertungen
- Ashleigh Cole Canadian Ota Pta Fieldwork Evaluation Form - Durham College 2016-2017Dokument14 SeitenAshleigh Cole Canadian Ota Pta Fieldwork Evaluation Form - Durham College 2016-2017api-395143739Noch keine Bewertungen
- Push 3Dokument2 SeitenPush 3Sandeep SharmaNoch keine Bewertungen
- Caremark Drug ListDokument10 SeitenCaremark Drug ListRahul DocNoch keine Bewertungen
- Nursing Guide to Bowel Disorder DrugsDokument7 SeitenNursing Guide to Bowel Disorder DrugsMarcela VeraNoch keine Bewertungen
- Medical-Surgical Nursing-3Dokument23 SeitenMedical-Surgical Nursing-3slsNoch keine Bewertungen
- NCLEX 15 WK 1critical ThinkingDokument2 SeitenNCLEX 15 WK 1critical ThinkingNikita TamrakarNoch keine Bewertungen
- Initial Approach to Trauma LectureDokument74 SeitenInitial Approach to Trauma LectureOjambo FlaviaNoch keine Bewertungen
- Blank Letter of Recommendation GenericDokument1 SeiteBlank Letter of Recommendation Genericapi-457505993Noch keine Bewertungen
- CCHIT Certified 2011 Ambulatory EHR Test Script 20100326Dokument121 SeitenCCHIT Certified 2011 Ambulatory EHR Test Script 20100326Zeeshan Ahmed KhanNoch keine Bewertungen
- Health Assessment Finals Review Flashcards - QuizletDokument92 SeitenHealth Assessment Finals Review Flashcards - QuizletViea Pacaco SivaNoch keine Bewertungen
- General Pharmacology - Sources of Drugs and Routes of AdministrationDokument48 SeitenGeneral Pharmacology - Sources of Drugs and Routes of AdministrationDhriti Brahma78% (9)
- Self Assessment - Midterm 2016Dokument11 SeitenSelf Assessment - Midterm 2016api-341527743Noch keine Bewertungen
- Ventilation Servo-I With Nava Neurally Controlled VentilationDokument14 SeitenVentilation Servo-I With Nava Neurally Controlled Ventilationraju_pnNoch keine Bewertungen
- 64-65 RiceDokument2 Seiten64-65 RiceyatishksNoch keine Bewertungen
- V7 CompleteDokument1.162 SeitenV7 Completeraju_pnNoch keine Bewertungen
- Ipod Nano 5th Gen UserGuideDokument104 SeitenIpod Nano 5th Gen UserGuideAnand BabuNoch keine Bewertungen
- Tool and Resource Evaluation TemplateDokument4 SeitenTool and Resource Evaluation Templatetimie_reyesNoch keine Bewertungen
- 2014 AHA/ACC Guidelines for Managing NSTE-ACSDokument46 Seiten2014 AHA/ACC Guidelines for Managing NSTE-ACSEmmieNoch keine Bewertungen
- 4 5953781827192751296Dokument119 Seiten4 5953781827192751296Ridha Afzal100% (1)
- Calista Roy LuigiDokument22 SeitenCalista Roy LuigiLuigi Prada GuzmanNoch keine Bewertungen
- ATLS ProtocoloDokument21 SeitenATLS Protocoloedgarjavier65100% (2)
- Dengue Disease Spectrum Among Infants in The 2001 Dengue Epidemic in Chennai, Tamil Nadu, IndiaDokument3 SeitenDengue Disease Spectrum Among Infants in The 2001 Dengue Epidemic in Chennai, Tamil Nadu, IndiaReju VijayandranNoch keine Bewertungen
- Reporting and Learning Systems for Medication ErrorsDokument7 SeitenReporting and Learning Systems for Medication ErrorsNoor KevNoch keine Bewertungen
- Drug Development: FDA's Definition of A New DrugDokument11 SeitenDrug Development: FDA's Definition of A New DrugSophie MendezNoch keine Bewertungen
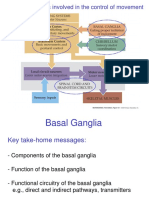
- Neural Structures Involved in The Control of MovementDokument68 SeitenNeural Structures Involved in The Control of MovementSAYAN NAGNoch keine Bewertungen
- Freud, Unconscious ExplorerDokument5 SeitenFreud, Unconscious ExplorerRyder Blue Holmes WilsonNoch keine Bewertungen
- DocumentationDokument11 SeitenDocumentationjoyveeNoch keine Bewertungen
- Anatomy and Types of ScoliosisDokument18 SeitenAnatomy and Types of ScoliosisVanessa Yvonne GurtizaNoch keine Bewertungen
- Chronic Suppurative Otitis MediaDokument4 SeitenChronic Suppurative Otitis MediarchristoverNoch keine Bewertungen
- Shock Power PointDokument24 SeitenShock Power PointmarwaNoch keine Bewertungen
- Healthcare Solutions-CooperDokument188 SeitenHealthcare Solutions-Cooper7alejandro7Noch keine Bewertungen
- A HOFFER Review Niacin The Real StoryDokument2 SeitenA HOFFER Review Niacin The Real StoryAna Lu100% (1)
- Medical Devices by FacilityDokument60 SeitenMedical Devices by FacilityjwalitNoch keine Bewertungen
- MCMI-IV Interpretive Report - 6856501 - 20180509033028436 PDFDokument10 SeitenMCMI-IV Interpretive Report - 6856501 - 20180509033028436 PDFChristianJ.Rodriguez100% (1)
- NeuVision 900 Operation+ManualDokument169 SeitenNeuVision 900 Operation+ManualRafael Salazar100% (1)
- Best Homeopathic RemediesDokument24 SeitenBest Homeopathic RemediesDrUday SrivastavaNoch keine Bewertungen
- Total Gastrectomy - Options For The Restoration of Gastrointestinal Continuity PDFDokument6 SeitenTotal Gastrectomy - Options For The Restoration of Gastrointestinal Continuity PDFJorge SalinasNoch keine Bewertungen
- THE HR Chronicle - November'19Dokument8 SeitenTHE HR Chronicle - November'19DrSwati Jayant PawarNoch keine Bewertungen
- The Lady With the LampDokument2 SeitenThe Lady With the LampBella RettobNoch keine Bewertungen
- Guillian-Barre Syndrome: Renalyn Galache Gladys Gegare BSN-3BDokument18 SeitenGuillian-Barre Syndrome: Renalyn Galache Gladys Gegare BSN-3BGLadys GegareNoch keine Bewertungen
- Heat Stroke: Causes, Symptoms, TreatmentDokument21 SeitenHeat Stroke: Causes, Symptoms, TreatmentHelloNoch keine Bewertungen
- Avi Kremer Case AnalysisDokument2 SeitenAvi Kremer Case AnalysisSurya BakshiNoch keine Bewertungen
- Acquired Brain en Una Tienda de LibrosDokument428 SeitenAcquired Brain en Una Tienda de Libroslig100% (1)
- Meningitis Beyond Neonatal AgeDokument57 SeitenMeningitis Beyond Neonatal AgeTilahun Kegne100% (2)
- 8 Emergency Formative Clinical Evaluation ChecklistDokument1 Seite8 Emergency Formative Clinical Evaluation Checklistمهند الرحيليNoch keine Bewertungen
- ArrowDokument12 SeitenArrowcelestialionNoch keine Bewertungen