Beruflich Dokumente
Kultur Dokumente
The Relationship of Endodontic-Periodontic Lesions
Hochgeladen von
Pam FNOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
The Relationship of Endodontic-Periodontic Lesions
Hochgeladen von
Pam FNCopyright:
Verfügbare Formate
In Remembrance
In Remembrance of James H.S. Simon
The Relationship of Endodontic–Periodontic Lesions
James H.S. Simon, AB, DDS,* Dudley H. Glick, BS, DDS,† and Alfred L. Frank, DDS‡
*Chief, Endodontic Section, V.A. Hospital, Long Beach, Cal-
ifornia and Clinical Assistant Professor of Endodontics, Univer-
sity of Southern California. †Clinical Professor of Endodontics,
University of Southern California. ‡Clinical Professor of
T he correlation of endodontic and periodontic radicular lesions has aroused
controversy and confusion inasmuch as dentists have become increasingly
more aware of the relationship between the attachment apparatus and the
Endodontics, University of Southern California. pulp. This article will offer a classification of these lesions based on their
Reprinted in its entirety from Simon JHS, Glick DH, Frank possible etiology, diagnosis and prognosis of treatment. Only by careful diag-
AL. The relationship of endodontic-periodontic lesions. J Perio-
dontol. 1972;43(4):202–8. Copyright ª American Academy of nosis and proper classification can the most effective treatment plan be
Periodontology. Reproduced with permission of American selected.
Academy of Periodontology. Although others (2, 3, 4, 5) have classified these lesions in varying degrees, we can
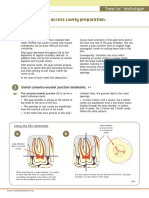
0099-2399/$ - see front matter theoretically delineate five types of lesion formation that are interrelated (Figure 1).
Copyright ª 2013 American Association of Endodontists.
http://dx.doi.org/10.1016/j.joen.2013.02.006
These will be discussed individually.
Primary Endodontic Lesions
Clinically, these lesions may appear concurrently with drainage from the gingival
sulcus area and/or swelling in the buccal attached gingiva. Although the patient may be
aware of minimal discomfort, pain is not usually present. An initial clinical impression is
that these are of periodontic origin. However, they are periodontic only in that they pass
through the periodontal ligament area. In reality, they are fistulas resulting from pulpal
disease.
Radiographically, different levels of bone loss may be apparent depending on
the avenue of fistulation. The necrotic pulp may cause a fistulous tract from the apex
through the periodontium along the mesial or distal root surface, to exit at the
cervical line. This appears as a radiolucency along the entire root length
(Figure 2a, Figure 3, Figure 4). This is not a totally dark radiolucent area, instead
a greyish, bony matrix may be visible. These lesions may occur on any maxillary or
mandibular tooth.
Fistulation can also occur from the apex into the bifurcation area which, radio-
graphically, creates the appearance of periodontal involvement. A similar radiographic
appearance may result from continual pulpal irritation through an accessory canal
(6, 7) which opens into the bifurcation area (Figure 2b & Figure 5). Diagnostically,
one should be suspicious of a pulpally induced lesion when the crestal bone level
on the mesial and distal appears relatively normal and only the bifurcation area is
radiolucent.
Figure 1. The clinical interrelationship of these five types of lesions is readily apparent.
JOE — Volume 39, Number 5, May 2013 Endo.–Perio. Lesions e41
In Remembrance
Figure 2. (a) Endodontic Lesions. The pathway of fistulation is evident through the periodontal ligament from the apex or a lateral canal. (b) Fistulation through
the apex or a lateral canal may cause bifurcation involvement. (c) Primary Endodontic Lesion with Secondary Periodontic Involvement. The existing pathway as in 2a
is shown but with the passage of time periodontitis with calculus formation begins at the cervical area. (d) Periodontic Lesions. This is the progression of peri-
odontitis to apical involvement. Note the vital pulp. (e) Primary Periodontic Lesion with Secondary Endodontic Involvement. The primary periodontic involvement at
the cervical margin and the resultant pulpal necrosis once the lateral canal is exposed to the oral environment result in this picture. (f) “True” Combined Lesions.
The two separate lesions are heading to a coalescence which forms the “true” combined lesion.
Another possibility results from fistulation through an accessory Primary Endodontic Lesions With Secondary
canal some distance from the apex on the mesial or distal which resem- Periodontic Involvement
bles an infra-bony pocket. (Figure 2a and Figure 6).
After a period of time if this primary endodontic problem
It must be pointed out that if fistulation occurs on the buccal or
remains untreated, it may then become secondarily involved
lingual aspect and is superimposed over the tooth root, a radiolucency with periodontal breakdown. Plaque may begin to form at the
may not appear on the radiograph. This also could be true of upper gingival margin which could result in a periodontitis (Figure 2c
molars where the palatal root screens the view of the trifurcation & Figure 7). The treatment and prognosis of the tooth are altered
area. Thus it is imperative that a gutta percha or silver cone be inserted when a probe or explorer encounters plaque or calculus. This
into the fistulous tract and x-rayed to determine the origin of the lesion. tooth now requires both endodontic and periodontic therapy.
However, when the pulp does not respond to an electric vitalometer or The prognosis depends on the periodontal therapy, assuming
thermal tests; it is evident a necrotic pulp may be the offender. In addi- the endodontic procedures are adequate. With endodontic
tion, when probing, a minimal amount of calculus or plaque formation therapy alone, only part of the lesion may heal which indi-
is encountered. In reality, these are not periodontic lesions but rather cates the presence of secondary periodontic involvement. In
fistulas of endodontic origin. They will heal with endodontic therapy general, healing of the endodontically induced areas may be
alone. anticipated.
Figure 3. The rather typical radiographic appearance on the distal is evident. Six month recall shows the radiolucency almost healed. Note the bony stroma visible
on the distal.
e42 Simon et al. JOE — Volume 39, Number 5, May 2013
In Remembrance
Figure 5. Radiographic bifurcation involvement is readily visible. Since the
pulp was necrotic only endodontic therapy was performed. Complete radio-
graphic healing is apparent nine months later. Note lateral canal opening
into the bifurcation.
Primary Periodontic Lesions
These lesions are caused by periodontal disease. Periodontitis
gradually progresses unchecked along the root surface until the
apical region is reached (Figure 2d & Figure 8). Occlusal trauma
may or may not be superimposed in these lesions. Diagnosis is based
Figure 4. Demonstrates the same radiographic appearance as on the on the usual periodontic test procedures. Probing usually reveals
distal of the molar. However, only endodontic therapy is required to calculus for varying lengths along the root surface and the pulp
accomplish healing. responds vitally to endodontic testing procedures. The diagnostician
JOE — Volume 39, Number 5, May 2013 Endo.–Perio. Lesions e43
In Remembrance
Figure 6. The mesial radiolucency on the first bicuspid resembles an infra- Figure 7. This was initially diagnosed as a primary endodontic lesion.
bony pocket. Since the pulp was nonvital, endodontic therapy was completed. However, on 3 year follow-up examination only partial healing is seen radio-
The lateral canal that showed on the post-operative x-ray was not anticipated. graphically. On probing the distal aspect calculus was encountered and the
However, in spite of a poorly condensed filling, healing of both the mesial and diagnosis of secondary periodontitis was made.
periapical areas occurred.
must also be aware of the radiographic appearance of periodontal lesion. The prognosis in this situation depends wholly upon the effi-
disease associated with developmental radicular anomalies (8). Sug- cacy of periodontal therapy.
arman and Sugarman (9) have raised the question of diagnosis on
teeth with full coverage. In this instance the test cavity is extremely
useful. A small hole is drilled through the crown and into the dentin Primary Periodontic Lesions With Secondary
with a highspeed #½ or #2 round burr, without the use of local Endodontic Involvement
anesthesia. The positive reaction to cutting dentin without coolants As periodontal lesions progress toward the apex, lateral or acces-
often will confirm a vital pulp. This is indicative of a periodontal sory canals may be exposed to the oral environment which can lead to
e44 Simon et al. JOE — Volume 39, Number 5, May 2013
In Remembrance
Figure 8. This is the reverse situation as in Figure 4. It is the opposite side of the same patient. This case went on to ultimate failure because of misdiagnosis. As the
records showed this to have a vital healthy pulp, this was purely a periodontal problem.
necrosis of the pulp (10) (Figure 2e). In addition, pulpal necrosis can 14) suggests that an interrelationship does exist once the integrity of
result from periodontal procedures where the blood supply, through an the dentinal tubules is violated. Further research in this area is
accessory canal or the apex is severed by a curette. definitely indicated.
These primary periodontal lesions with secondary endodontic
involvement may be radiographically indistinguishable from primary
endodontic lesions with secondary periodontic involvement. Teeth “True” Combined Lesions
undergoing periodontal therapy that do not respond as anticipated, These lesions occur where an endodontically induced periapical
should be pulp tested. It may be that the previously vital tooth is now lesion exists on a tooth that is also periodontally involved. The radio-
necrotic. Again the prognosis depends on the periodontal therapy graphic infra-bony defect is created when these two entities meet and
once the endodontic therapy has been solved. Periodontal treatment merge somewhere along the root surface. (Figure 2f & Figure 9).
alone will not suffice in the presence of a pulpally involved tooth. Ultimately, the clinical and radiographic picture is indistinguishable
Recently, there has been research to determine the relationship from the other two lesions that are secondarily involved. Periapical heal-
between periodontal and pulpal disease. Mazur and Massler, 1964 ing may be anticipated following successful endodontic therapy. The
(11), found no correlation between the severity of periodontal disease periodontic aspects then may or may not respond to periodontal treat-
and the status of the pulp. However, recent studies by others (12, 13, ment, depending on the severity of involvement.
Figure 9. The lesion involving the cuspid was diagnosed as a “true” combined lesion. The tooth was both supererupted and lingually tipped. The cuspid had
endodontic therapy including attempts at an autogenous bone marrow transplant. In spite of everything healing in the endodontic area occurred.
JOE — Volume 39, Number 5, May 2013 Endo.–Perio. Lesions e45
In Remembrance
It is interesting to note that a similar radiographic appearance may 3. Begin JF. Perio-Endo Considerations: Combined Therapy. Royal Canadian Dent
result from a vertically fractured tooth. If a fistula is present, it may be Corps Quarterly 1968;9:1–5.
4. Oliet S, Pollock S. Classification and Treatment of Endo-Perio Involved Teeth. Phila
necessary to lay a flap to help determine the exact etiology. A fracture Co Dent Soc Bulletin 1968;34:12–6.
that has penetrated to the pulp with resultant necrosis, also can be 5. Simon P, Jacobs P. The So-Called Combined Periodontal Pulpal Problem. Dent
labelled a "true" combined lesion. Clinics of NA 1969;13:45–53. W. B. Saunders Co.
6. Seltzer S, Bender IB, Zonti M. The Interrelationship of Pulp and Periodontal
Disease. OS, OM, and OP 1963;16:1474–90.
7. Winter GB, Kramer IRH. Changes in Periodontal Membrane and Bone Following
Summary Experimental Pulpal Injury in Deciduous Molar Teeth in Kittens. Arch Oral Biol
We have presented an etiologic classification of endodontic and 1965;10:279–89.
periodontic lesions. To better recognize, understand and treat these 8. Simon JH, Glick DH, Frank AL. Predictable Endodontic and Periodontic Failures as
a Result of Radicular Anomalies. OS, OM, and OP 1971;31:823–6.
problems, we have discussed their diagnosis and prognosis from a clin- 9. Sugarman MM, Surgarman EF. The Differential Diagnosis of Periodontic-
ical standpoint in order to explain the success or failure that follows Endodontic Problems. J Alabama Dent Assoc 1969;53:16–24.
treatment. 10. Rubach WC, Mitchell DF. Periodontal Disease, Accessory Canals, and Pulp Pathosis.
J Periodont 1965;36:34–8.
11. Mazur B, Massler M. Influence of Periodontal Disease on the Dental Pulp. OS, OM,
and OP 1964;17:592–603.
References 12. Stahl SS. Pathogenesis, of Inflammatory Lesions in Pulp and Periodontal Tissues.
1. Schilder, H., The Relationship of Periodontics to Endodontics, Transactions of the Periodontics 1966;4:190–6.
Third International Conference on Endodontics (Louis I. Grossman, editor), 13. Seltzer S, Bender IB, Nazimov H, et al. Pulpitis-Induced Interradicular Periodontal
University of Pennsylvania, Philadelphia, 1963. Changes in Experimental Animals. J Periodont 1967;38:124–9.
2. Amen CR. When is the Condition of the Pulp an Important Consideration in Peri- 14. Stallard RE. Periodontal Disease and Its Relationship to Pulpal Pathology. Am Inst, of
odontal Disease? Periodontal Abstract 1967;15:7–8. Oral Biology Annual Meeting 1967;197–203.
e46 Simon et al. JOE — Volume 39, Number 5, May 2013
Das könnte Ihnen auch gefallen
- Clinical Data Management Ensures Trial IntegrityDokument39 SeitenClinical Data Management Ensures Trial IntegrityBhavana Alapati100% (4)
- Gingival Enlargement Causes, Classification and GradingDokument49 SeitenGingival Enlargement Causes, Classification and Gradingdhwanit31100% (1)
- Cairo Clasificaion ResecionDokument7 SeitenCairo Clasificaion ResecionMartty BaNoch keine Bewertungen
- Dentoalveolar Surgery PDFDokument146 SeitenDentoalveolar Surgery PDFdrzana78100% (2)
- Sympton Relief in Palliative Care PDFDokument300 SeitenSympton Relief in Palliative Care PDFdjsalman25% (4)
- Prevalence and Extent of Long Oval Canals in The Apical ThirdDokument5 SeitenPrevalence and Extent of Long Oval Canals in The Apical Thirddr.samiNoch keine Bewertungen
- Mixed AnxietyDokument2 SeitenMixed Anxietyarif rhNoch keine Bewertungen
- The Impact of Music Therapy On Mental HealthDokument5 SeitenThe Impact of Music Therapy On Mental Healthapi-561468026Noch keine Bewertungen
- Strategic Planning in Healthcare: Benefits, Process and ImplementationDokument7 SeitenStrategic Planning in Healthcare: Benefits, Process and Implementationalodia_farichaiNoch keine Bewertungen
- JIAP July 2011 - Guided Tissue Regeneration - A Decision-Making ModelDokument8 SeitenJIAP July 2011 - Guided Tissue Regeneration - A Decision-Making ModelLouis HutahaeanNoch keine Bewertungen
- Elements of A Comprehensive Community DiagnosisDokument6 SeitenElements of A Comprehensive Community DiagnosisAila Hinlog100% (8)
- Odontogenic Cysts Summary Chart: Radicular Cyst (Periapical Cyst)Dokument4 SeitenOdontogenic Cysts Summary Chart: Radicular Cyst (Periapical Cyst)ML90Noch keine Bewertungen
- An Atlas of Head & Neck Surgery Vol1 4 Ed PDFDokument829 SeitenAn Atlas of Head & Neck Surgery Vol1 4 Ed PDFRaphaela Travassos100% (3)
- 35133OPDH2EDokument358 Seiten35133OPDH2EDodo AlvaNoch keine Bewertungen
- New Classification For Periodontal Diseases 2017 PDFDokument367 SeitenNew Classification For Periodontal Diseases 2017 PDFblokolbNoch keine Bewertungen
- Variasi Normal Rongga MulutDokument18 SeitenVariasi Normal Rongga MulutRafi Kusuma Ramdhan SukonoNoch keine Bewertungen
- Oral Wound Healing: Cell Biology and Clinical ManagementVon EverandOral Wound Healing: Cell Biology and Clinical ManagementHannu LarjavaNoch keine Bewertungen
- Aggressive Periodontitis inDokument5 SeitenAggressive Periodontitis inOctavian CiceuNoch keine Bewertungen
- Tips On Access Cavity Preparation.: How To' TechniqueDokument4 SeitenTips On Access Cavity Preparation.: How To' TechniqueGoran TosicNoch keine Bewertungen
- Black Triangle PDFDokument4 SeitenBlack Triangle PDFzinniaNoch keine Bewertungen
- Diagnosis of Pulp and Periradicular Disease 2012Dokument75 SeitenDiagnosis of Pulp and Periradicular Disease 2012keelerketo13Noch keine Bewertungen
- Effect of Gingival Biotype On Orthodontic TreatmenDokument8 SeitenEffect of Gingival Biotype On Orthodontic Treatmensolodont1Noch keine Bewertungen
- Evaluation of Third MolarsDokument6 SeitenEvaluation of Third Molarsapi-265532519Noch keine Bewertungen
- AggressiveDokument55 SeitenAggressiveSaima KhanNoch keine Bewertungen
- Case Report Fissure SealantDokument8 SeitenCase Report Fissure SealantrespikNoch keine Bewertungen
- Jurnal Scalling Dan Root PlaningDokument17 SeitenJurnal Scalling Dan Root PlaningJesicaNoch keine Bewertungen
- Surgical Periodontal TherapyDokument11 SeitenSurgical Periodontal TherapyGonzalo Becerra LeonartNoch keine Bewertungen
- Modern Healthcare ArchitectureDokument15 SeitenModern Healthcare ArchitectureKanak YadavNoch keine Bewertungen
- Odontogenic Keratocyst: - Jayalakshmi Preetha Meyyanathan CRIDokument48 SeitenOdontogenic Keratocyst: - Jayalakshmi Preetha Meyyanathan CRIJayalakshmi PreethaNoch keine Bewertungen
- Aggressive Periodontitis KalpsDokument59 SeitenAggressive Periodontitis Kalpskalpanagokul44Noch keine Bewertungen
- Traumatic FibromaDokument3 SeitenTraumatic FibromaDiana FitriNoch keine Bewertungen
- Contemporary ExodontiaDokument8 SeitenContemporary ExodontiaEmilio RodríguezNoch keine Bewertungen
- Bulk Fill Resin RestorationDokument18 SeitenBulk Fill Resin RestorationNuningK93Noch keine Bewertungen
- Restoring Posterior Tooth with Semidirect TechniqueDokument4 SeitenRestoring Posterior Tooth with Semidirect Techniquemartariwansyah100% (1)
- Longevity of Posterior Composite RestorationDokument15 SeitenLongevity of Posterior Composite Restorationvrana23Noch keine Bewertungen
- ChronicPerio 16 12 14Dokument39 SeitenChronicPerio 16 12 14vsdeepsNoch keine Bewertungen
- Generalized Aggressive Periodontitis in Preschoolers: Report of A Case in A 3-1/2 Year OldDokument6 SeitenGeneralized Aggressive Periodontitis in Preschoolers: Report of A Case in A 3-1/2 Year OldDyah Wulan RamadhaniNoch keine Bewertungen
- Klasifikasi Impaksi Caninus Rahang Atas Pada Pemeriksaan Radiograf Panoramik Dan CBCT Sebagai Penunjang OdontomyDokument8 SeitenKlasifikasi Impaksi Caninus Rahang Atas Pada Pemeriksaan Radiograf Panoramik Dan CBCT Sebagai Penunjang OdontomyRahmi WastriNoch keine Bewertungen
- IndianJDentSci92126-1778286 045622Dokument8 SeitenIndianJDentSci92126-1778286 045622Debora NatalynaNoch keine Bewertungen
- Pathologies of CementumDokument61 SeitenPathologies of CementumKoyyalamudi PrudhviNoch keine Bewertungen
- BURNING MOUTH SYNDROME REVIEWDokument26 SeitenBURNING MOUTH SYNDROME REVIEWMariatun Zahro NasutionNoch keine Bewertungen
- Bystrom & Sundqvist 1985Dokument7 SeitenBystrom & Sundqvist 1985doutormarcielNoch keine Bewertungen
- Banerjee - 2018 - Selective Removal of Carious DentinDokument16 SeitenBanerjee - 2018 - Selective Removal of Carious DentinAli Al-QaysiNoch keine Bewertungen
- Lecture 4 Diagnosis of Dental CariesDokument12 SeitenLecture 4 Diagnosis of Dental CariesDt omarNoch keine Bewertungen
- TUTORIAL IN ENGLISH Blok 12Dokument7 SeitenTUTORIAL IN ENGLISH Blok 12Ifata RDNoch keine Bewertungen
- Save the natural tooth or place an implant ? A Periodontal decisional criteria to perform a correct therapy. Ricci, Ricci & Ricci. The International Journal of Periodontics & Restorative Dentistry, 2011; 31, 29-37. .pdfDokument10 SeitenSave the natural tooth or place an implant ? A Periodontal decisional criteria to perform a correct therapy. Ricci, Ricci & Ricci. The International Journal of Periodontics & Restorative Dentistry, 2011; 31, 29-37. .pdfanonimoNoch keine Bewertungen
- Teknik Frenectomy Miller 2020Dokument4 SeitenTeknik Frenectomy Miller 2020yufita fitrianiNoch keine Bewertungen
- Pulp Capping Provides Lowest Incidence of Bacterial Microleakage and Pulp InflammationDokument7 SeitenPulp Capping Provides Lowest Incidence of Bacterial Microleakage and Pulp InflammationamandaNoch keine Bewertungen
- Tooth Mobility: A Review: Dr. Prerna Kataria Dr. Vishal Arya Dr. Lavina Taneja AryaDokument3 SeitenTooth Mobility: A Review: Dr. Prerna Kataria Dr. Vishal Arya Dr. Lavina Taneja Aryaanusha guptaNoch keine Bewertungen
- Orofacial Pain Classification and ManagementDokument16 SeitenOrofacial Pain Classification and ManagementMat MatttNoch keine Bewertungen
- Chronic and Aggressive PeriodontitisDokument46 SeitenChronic and Aggressive PeriodontitisMoola Bharath ReddyNoch keine Bewertungen
- REVIEW - The Microtensile Bond TestDokument12 SeitenREVIEW - The Microtensile Bond TestElmer Acevedo0% (1)
- DiagnosisDokument51 SeitenDiagnosisRamya ChowdaryNoch keine Bewertungen
- Molar Incisor Hypomineralization Prevalence PatterDokument9 SeitenMolar Incisor Hypomineralization Prevalence PatterAndreea Andrei AndreeaNoch keine Bewertungen
- Operkulektomi Herlambang, Devina, Asya, AlinDokument3 SeitenOperkulektomi Herlambang, Devina, Asya, AlinHerlambang PrasetyoNoch keine Bewertungen
- Dense Bone Island: Temuan Insidental Pada Radiograf PanoramikDokument4 SeitenDense Bone Island: Temuan Insidental Pada Radiograf PanoramikFransiski HoNoch keine Bewertungen
- Exodontia in Pediatric Dental Patient: 1 Pediatrics For Dentistry C-IDokument50 SeitenExodontia in Pediatric Dental Patient: 1 Pediatrics For Dentistry C-IVincent SerNoch keine Bewertungen
- 5.a Missing IncisorDokument4 Seiten5.a Missing IncisormirfanulhaqNoch keine Bewertungen
- Aulia Rizqi Niami - J2a017048 - Skenario 4Dokument29 SeitenAulia Rizqi Niami - J2a017048 - Skenario 4Aulia Rizqi NiamiNoch keine Bewertungen
- Working LengthDokument67 SeitenWorking LengthnishthaNoch keine Bewertungen
- Traumatic Injuries Notes 22nk8pfDokument16 SeitenTraumatic Injuries Notes 22nk8pfAmee PatelNoch keine Bewertungen
- Mucogingival Deformities: Ni Made Ista PrestiyantiDokument55 SeitenMucogingival Deformities: Ni Made Ista Prestiyantiista prestiyantiNoch keine Bewertungen
- Decoronation of An Ankylosed Permanent Incisor: Alveolar Ridge Preservation and Rehabilitation by An Implant Supported Porcelain CrownDokument4 SeitenDecoronation of An Ankylosed Permanent Incisor: Alveolar Ridge Preservation and Rehabilitation by An Implant Supported Porcelain CrownJuan Carlos MeloNoch keine Bewertungen
- Endo Perio2Dokument9 SeitenEndo Perio2Fernando CordovaNoch keine Bewertungen
- Computerized Occlusal Analysis As An Alternative Occlusal IndicatorDokument6 SeitenComputerized Occlusal Analysis As An Alternative Occlusal IndicatorMariana RaduNoch keine Bewertungen
- Traumatic UlcersDokument25 SeitenTraumatic UlcersHina MahessarNoch keine Bewertungen
- Dental stains: Causes, types and treatmentDokument30 SeitenDental stains: Causes, types and treatmentArtur Radvanszki100% (1)
- Papila DentalDokument6 SeitenPapila DentalFedor Rivas MedinaNoch keine Bewertungen
- Kanker MulutDokument2 SeitenKanker MulutHamba AllahNoch keine Bewertungen
- 1 - The Periodontal PocketDokument54 Seiten1 - The Periodontal Pocketdrdkdk7Noch keine Bewertungen
- Manejo de Periodontitis PerpupebralDokument6 SeitenManejo de Periodontitis PerpupebralPam FNNoch keine Bewertungen
- Other Words - Learningproduct - Sep14 - 18Dokument7 SeitenOther Words - Learningproduct - Sep14 - 18Pam FNNoch keine Bewertungen
- Alveolarosteitis Andosteomyelitis Ofthejaws: Peter A. KrakowiakDokument13 SeitenAlveolarosteitis Andosteomyelitis Ofthejaws: Peter A. KrakowiakPam FNNoch keine Bewertungen
- Complications of 3rd Molar SurgeryDokument12 SeitenComplications of 3rd Molar Surgeryhamad_kayani_774954Noch keine Bewertungen
- Orthopedic Treatment ManageDokument63 SeitenOrthopedic Treatment ManagePam FNNoch keine Bewertungen
- Ortopedia Caso ClinicoDokument6 SeitenOrtopedia Caso ClinicoPam FNNoch keine Bewertungen
- The Maryland Bridge Retainer: A Modi Fication of A Maryland BridgeDokument4 SeitenThe Maryland Bridge Retainer: A Modi Fication of A Maryland BridgePam FNNoch keine Bewertungen
- The Role of Orthodontics in The Repair of PDFDokument6 SeitenThe Role of Orthodontics in The Repair of PDFPam FNNoch keine Bewertungen
- The Role of Orthodontics in The Repair of PDFDokument6 SeitenThe Role of Orthodontics in The Repair of PDFPam FNNoch keine Bewertungen
- The Role of Orthodontics in The Repair of PDFDokument6 SeitenThe Role of Orthodontics in The Repair of PDFPam FNNoch keine Bewertungen
- Exercises ConditionalsDokument13 SeitenExercises ConditionalsPam FNNoch keine Bewertungen
- Conceptual Map ConditionalsDokument2 SeitenConceptual Map ConditionalsPam FNNoch keine Bewertungen
- Comparision Chart ConditionalsDokument3 SeitenComparision Chart ConditionalsPam FNNoch keine Bewertungen
- Diagnostic Terms For Pulp Conditions - JoE 2009Dokument13 SeitenDiagnostic Terms For Pulp Conditions - JoE 2009Bicho Angel LisseaNoch keine Bewertungen
- Fibromyalgia: by Tara E. Dymon, Pharm.D., BCACPDokument14 SeitenFibromyalgia: by Tara E. Dymon, Pharm.D., BCACPAnggi CalapiNoch keine Bewertungen
- Example Nursing Thesis StatementDokument4 SeitenExample Nursing Thesis StatementTye Rausch100% (2)
- Eoi Medical TourismDokument9 SeitenEoi Medical TourismSHAH MOHAMMAD FAISAL CCBMDO 2021Noch keine Bewertungen
- Defining Patient ExperienceDokument15 SeitenDefining Patient ExperiencesanaaNoch keine Bewertungen
- Mental Health ResumeDokument6 SeitenMental Health Resumeafjwdudgyodbef100% (2)
- ANTIBIOTIC POLICY FOR Sassoon Hospital & BJGMC, PuneDokument32 SeitenANTIBIOTIC POLICY FOR Sassoon Hospital & BJGMC, Puneshah007zaadNoch keine Bewertungen
- Homoeopathy PosologyDokument27 SeitenHomoeopathy PosologyLakshmi Deepak INoch keine Bewertungen
- Health Emergency Kits Training 2019 PDFDokument33 SeitenHealth Emergency Kits Training 2019 PDFrema_rhere95Noch keine Bewertungen
- The Biting Facts About Fleas 38186 ArticleDokument6 SeitenThe Biting Facts About Fleas 38186 ArticleCabinet VeterinarNoch keine Bewertungen
- Case Management Assessment FormDokument13 SeitenCase Management Assessment Formiman diarNoch keine Bewertungen
- Medical Audit of Inpatient Medical Records in A Tertiary Care Hospital - January - 2022 - 1381401306 - 8501173Dokument3 SeitenMedical Audit of Inpatient Medical Records in A Tertiary Care Hospital - January - 2022 - 1381401306 - 8501173sanjay yadavNoch keine Bewertungen
- Folic AcidDokument2 SeitenFolic AcidShaira Richelle OmagapNoch keine Bewertungen
- NCM 113 Community Health Nursing LectureDokument4 SeitenNCM 113 Community Health Nursing LectureAngelica Kaye BuanNoch keine Bewertungen
- Senior Capstone Critical JudgementDokument6 SeitenSenior Capstone Critical Judgementapi-546967314Noch keine Bewertungen
- 100-6226-9 Level 2 Cert in Safe Handling in MedicinesDokument49 Seiten100-6226-9 Level 2 Cert in Safe Handling in MedicinesAndreea GheorghiuNoch keine Bewertungen
- Research Evidence PyramidDokument22 SeitenResearch Evidence PyramidSyifa SalsabilaNoch keine Bewertungen
- FNCPDokument1 SeiteFNCPapi-383235850% (2)
- Recommendation FormsDokument5 SeitenRecommendation FormsRezi Sabutanan AmerilaNoch keine Bewertungen
- Treatment For Complicated Grief State of The ScienDokument7 SeitenTreatment For Complicated Grief State of The SciendfvbnmjkioNoch keine Bewertungen
- 206 - Update-The Business of Anesthesiology - Leibowitz, AndrewDokument9 Seiten206 - Update-The Business of Anesthesiology - Leibowitz, Andrewyoshizzle129909Noch keine Bewertungen