Beruflich Dokumente
Kultur Dokumente
Scaling Up Laboratory Testing Capacity in The Context of Managing Emerging Pandemic Lessons Learned From Scaling Up SARS-COV-2 Testing in Rwanda
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Scaling Up Laboratory Testing Capacity in The Context of Managing Emerging Pandemic Lessons Learned From Scaling Up SARS-COV-2 Testing in Rwanda
Copyright:
Verfügbare Formate
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Scaling up Laboratory Testing Capacity in the
Context of Managing Emerging Pandemic:
Lessons Learned from Scaling Up
SARS-COV-2 Testing in Rwanda
Emil Ivan1,3,7, Patrick Gad Iradukunda2,3, Pierre Gashema1,3, Angelique Ingabire 3, Alice Kabanda3, Enatha Mukantwari3, Anicet
Rucogoza3, Jules Christian Ishimwe3, Kamwesiga Julius4, Emile Musoni3, Shema Eliah1,7
Tafadzwa Dzinamarira5, Eugene Mutimura6
1
Rwanda Biomedical Center, National Reference Laboratory Division and College of Medicine and Health Sciences,
University of Rwanda, Kigali, Rwanda
2
London School of Hygiene and Tropical Medicine, University of London, London, UK
3
Rwanda Joint Task Force COVID-19, Department of Biomedical Services, National Reference Laboratory Division, Rwanda
Biomedical Center, Kigali, Rwanda
4
AIDS Healthcare Foundation (AHF), Kigali, Rwanda
5
Department of Public Health Medicine, School of Nursing and Public Health,
University of KwaZulu-Natal, Durban, 4001, South Africa
6
National Council Science and Technology (NCST), Kigali Rwanda
7
Homeland Initiative (HLI), Kigali, Rwanda
Corresponding author: Alternative corresponding author:
Emil Ivan, PhD Patrick Gad Iradukunda
Rwanda Biomedical Center , Rwanda Joint Task Force COVID-19, Department of
National Reference Laboratory Division and College of Biomedical Services, National Reference Laboratory
Medicine and Health Sciences, Division, Rwanda Biomedical Center, Kigali, Rwanda.
University of Rwanda, Kigali, Rwanda
Abstract: The coronavirus disease 2019 (COVID-19) has population and government goodwill; research-based
challenged health systems globally. In low and middle- actions that included adopting a pooling strategy;
income countries, a unique challenge ensuring the optimized use of available human resources; and the use
widespread testing that is critical to the response toward of limited resource funding models to support the
the pandemic has persisted. The pandemic has established health system governance structure. Initially,
accentuated the need for rapid scale-up of real-time the national reference laboratory was the only testing site
polymerase chain reaction (RT-PCR), a molecular testing for COVID-19; however, later, the country implemented
technique that was often used for research purposes only, decentralized testing, setting up COVID-19 testing
especially in limited-resource settings. Rwanda is a low- centers countrywide. In this article, we highlight the
income country that has managed to scale up RT-PCR lessons learned from the Rwandan COVID-19 laboratory
laboratory testing capacity by 15-fold within the first testing response to guide effective laboratory response in
four-month of the COVID-19 pandemic. limited-resource settings.
Rwanda has been in line with the measures to We recommend an appropriate epidemic response
contain COVID-19 even before 14th March 2020, when algorithm to be developed to classify cases based on
the first case of COVID-19 was detected. Due to the epidemiological, clinical, and laboratory information in
transmission of the infection, the scale-up was line with diagnosis methods and sustain quality.
immediately in place, relying on public, private, non-
governmental, and voluntary students from universities Keywords: COVID-19, LABORATORY, DIAGNOSTICS,
to boost the surveillance of the pandemic in the SCALING UP, RT-PCR, RWANDA
population. In COVID-19 testing, this scale-up relied on
IJISRT21FEB179 www.ijisrt.com 339
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
I. INTRODUCTION ➢ The Overview of clinical laboratories and setting up
national COVID-19 testing in Rwanda
The novel Coronavirus (nCOVID-19), also commonly The Rwandan clinical laboratory and quality network
known as SARSCOV-2, was first reported in the city of follows a top-down supervision framework providing
Wuhan in China by the end of December 2019(1), but it has services adjusted to the decentralized health system. The
now spread throughout the world with varying impact. Rwanda National Reference (NRL) entered in World health
Scientists are still learning about the disease which was first organization's quality improvement steps, also called
linked with animals and its substantial impact on one Stepwise Laboratory Improvement Process Towards
health(2). The disease spreads from person to person through Accreditation in the Africa Region (SLIPTA), in July 2009
infected air droplets that are projected during sneezing and and benefited from the Strengthening Laboratory
coughing. It can also be transmitted when humans contact Management Toward Accreditation (SLMTA) program(12).
hands or surfaces containing the virus and touch their eyes, The country laboratory was also focusing on quality
nose, or mouth with the contaminated hands(3). improvement through the strategic health plan of July 2009,
which aimed to strengthen quality starting with four referral
The World health organization (WHO) Director- hospitals and the National Referral Laboratory(13). The NRL
General has consistently advised governments and all is an ISO 15189 accredited facility(14).
ministries of health to fight the COVID-19 pandemic through
widespread testing, contact tracing, and real-time response Pre-COVID-19 molecular testing in Rwanda was
tactic model(4). Despite the novel vaccines being mainly in monitoring people living with HIV/AIDS (PLWH),
acknowledged by Stringent Regulatory Authorities and patients with Chronic Hepatitis B Virus, and Chronic
efforts of COVAX to distribute the vaccine evenly across the Hepatitis C Virus. Due to the HIV monitoring program
world, there remain operational and global rational implementation and treatment for all, different laboratories
distribution challenges, especially in Low and Middle- were equipped with semi-automated molecular instruments
Income Countries (LMICs)(5). This implies that testing (COBAS CAPsTM and Abbott m2000 platforms) and trained
laboratories remain the cornerstone of managing the staff. When COVID-19 broke out in Rwanda, the Rwanda
pandemic through early detection to identify new cases and Forensic Laboratory provided technical expertise and
their contacts through active surveillance to minimize the provided support to the NRL to set up a national COVID-19
transmission of the virus in LMICs. testing site.
In the surge to fight the novel coronavirus outbreak, As the COVID-19 response in Rwanda evolved, the
LMICs are characterized by inadequate laboratory capacity NRL built capacity through staff training, procurement, and
for diagnosing the disease (6, 7). Nasopharyngeal and availing testing infrastructure. In this respect, a forecast of
oropharyngeal specimens have been used to detect SARS- reagents and consumables was done. Worldwide, a growing
CoV-2 RNA (the causal agent of COVID-19) using real-time SARS-CoV-2 Diagnostic Technology Landscape explored
reverse transcription-polymerase chain reaction (RT- molecular and serology assays(15). However, despite the
PCR)(8). Other approaches that include serological testing (9) ever-increasing market, some of these platforms were still
and sophisticated approaches such as scent dog identification under validation and may not have allowed countries to
of samples to detect COVID-19 have also been employed as urgently respond appropriately for a stable and reliable
of December 2020(10). national testing strategy.
Medical laboratories in LMICs face different challenges Presently, NRL uses Real-Time Polymerase Chain
to satisfy infrastructure, equipment, human resources, and Reaction for SARS-CoV-2 testing. It uses both semi-
stockpiles of required reagents and supplies despite the automated platforms, the ABI 7500 (fast and standard), Bio-
introduced Africa Medical Supplies Platform(6). Rwanda has Rad CFX96, Rotor-Gene, ABI Quant studio 5 and a fully
been well-reputed over handling the COVID-19 pandemic so automated platform, Cobas 6800 (Roche). Also, SARSCOV-
far(11). Considering the overall data from April to November 2 Gene Xpert from Cepheid is used for emergency cases. The
2020 samples tested, thus this review will highlight the key satellite laboratories use Abbott m2000 and Bio-Rad CFX96.
lessons learned from testing COVID-19 in Rwanda while The equipment facilitated widespread testing of individuals at
setting up and decentralizing the RT-PCR testing capacity in risk of the COVID-19 infection and contact tracing of index
Rwanda to increase the testing capacity and the accessibility cases. Further, Rwanda utilized the existing equipment to
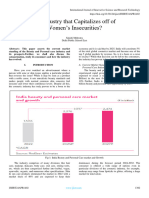
to laboratory results. The Figure-1 describes the tests support COVID-19 testing for other countries like the Central
conducted by the site in September 2020 and comparable African Republic(16).
extract for all samples from April- November, and a regional
testing capacity analysis.
IJISRT21FEB179 www.ijisrt.com 340
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Fig 1: Shows list of testing sites by volume for September 2020
The NRL uses a Detection kit for 2019 Novel services for the community thus supporting the surveillance
Coronavirus kits (2019-nCoV) RNA (PCR Fluorescence and quick management of SARSCOV-2 patients. By
Probing) from DaAn® Gene Co Ltd based on detection of N- September 2020, the national reference laboratory was able
gene and ORF1ab. Besides, for quality control of results to gain the average test capacity of 1500 samples of RT-PCR
purposes, the Rwanda reference laboratory uses Germany- per day, and together all the ten satellite laboratories were
made technology (TIB-MOLBIOL® GmbH Berlin) as testing 2500 samples per day at minimum. The testing
detection and confirmation kits with high sensitivity and
specificity to detect COVID-19 for E-gene and RNA workflow was established, giving results at an average
dependent RNA polymerase (RdRP) on the 7500 ABI® FAST turnaround time of 24 hours. Negative results were submitted
Machine. The machine has a test capacity of producing 768 to individuals, and the surveillance team informed them how
COVID-19 test results within 24 hours. to take appropriate protective measures. Positive SARSCOV-
2 was submitted to the surveillance team every evening to
➢ Setting up the RT-PCT Laboratories and results reporting immediately evacuate the patients to the selected treatment
mechanisms centers and trace the contact to reduce transmission risk.
Rwanda's national COVID-19 testing algorithm
recommends using RT-PCR to detect and confirm COVID- ➢ Training activities
19. This increases confidence between tested positive and Training activities involved a developed module by
negative from suspected samples critical for contact tracing. senior lab scientists to junior scientists and involved sample
Under the national reference laboratory's coordination and collection, sample transport, sample registration, sample
stewardship, ten new testing laboratories were established reception, processing, RNA extraction procedures,
and accredited to test for SARSCOV-2 countrywide as amplification, and reporting standard operating procedures to
illustrated in figure-1. The result reporting was in one return laboratory results on time. We trained 35 individuals
reporting system unilaterally validated through the health per week to master these procedures and generated a team of
management information system (HMIS-DHS2®) and was trainers, and in total, 350 volunteered technicians were
used for data management of COVID-19 patients on a daily trained to be involved in the testing and reporting of
basis. SARSCOV-2 methods in two months, and the capacity was
adequate to have a pool of skilled individuals for all sites. We
➢ Diagnostic testing capacity for SARSCOV-2 want to point out key lessons learned by implementing the
As demonstrated (Figure 2), shows the increasing pandemic scale-up and SARSCOV-2 laboratories in Rwanda
testing capacity and scaling up more testing sites increased (January –September 2020).
the national testing capacity and access to PCR testing
IJISRT21FEB179 www.ijisrt.com 341
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Fig 2: Scaling up the COVID-19 testing capacity for decentralized testing sites
II. LESSON LEARNED FROM COVID-19 Although several researchers and institutions have
TESTING IN RWANDA. acknowledged pooling, there is evidence that some limited
resource countries have not yet adopted the method, and
➢ Lesson 1: Promotion of research/evidence-based uncertainty remains high due to the result reliance gap
actions to inform implementation estimated by CDC with ≥85% percent positive agreement
Rwanda’s testing capacity for COVID-19 increased (PPA) and limited researches(23, 24). However, the method
from 200 samples per day to more than 1500 samples per day had a limitation of being useful in a low prevalence setting.
(Fig 1). Due to the tracing and surveillance system, the Therefore, setting-up new testing sites and decentralizing
number depended on the surge in cases and the clusters of hot testing to the hot spot areas closed the gap, making the
spot areas of COVID-19. This ensured smooth and productive pooling strategy more effective by site consideration.
surveillance of the virus and building on already existing
laboratory, sentinel, and disease surveillance systems. The In spite of the limited resources, Rwanda has
backbone of the surveillance has been acknowledged for contributed to the SARS-CoV-2 genomes by uploading nine
handling outbreak(17). Moreover, strengthening the health sequenced copies(25). However, as other LMICs, Rwanda
research system (HRS) and implementing the research has been left behind to track the new COVID-19 variants that
outcome provides efficient management of outbreak (18). originated from United Kingdom (UK), Brazil, and South
Africa(26). Since 3rd December 2021, COVID-19 cases have
Through research, Rwanda adopted the pooling strategy consistently risen from 17 new cases to 336 new cases as of
to scale up testing capacity increasing 15 folds from mid- 26th January 2021, and the mortality rate increased
March to mid-July with a daily capacity of more than 7,000 dramatically, with Rwanda reporting up to nine COVID-19
tests per day when the hot spot clusters increased(19). On 4th related death in a single day(27, 28). Thus, this strongly
September 2020, Rwanda tested 0.43 per 1,000 population, demonstrates the need for surveillance and investigating the
making it the fourth country with the highest testing coverage new COVID-19 variants to guide policy.
in Africa after Morocco (0.60 per 1,000), Namibia (0.57 per
1,000), and Lybia (0.46 per 1,000)(20). More importantly, ➢ Lesson 2: Optimizing Staff productivity
from 15th April to 30th June 2020, Rwanda was among the Apart from being the cornerstone of quality health care,
leading three low-income countries (LICs) with high daily the medical laboratory is a complex, rapidly evolving sector
COVID-19 testing per 1000 population, from the 1st July requiring a wide range of skilled workforce competent to use
until 16th August 2020. Rwanda becomes the first LIC with the novel technology on the market in consideration to stock
the highest daily testing capacity and later until 10th and resource availability(29). In the context of SARS_COV2
September 2020 when there was a significant reduction in diagnosis at NRL, on average, in a two-hour-long manual
tested cases due to a low positivity rate (from 230 daily cases extraction environment, 45 well-trained laboratory staff
as of 20th September 2020 to less than 20 cases as of 10th directly involved in extraction and amplification were able to
September 2020), Rwanda continued to be among the leading run the laboratory for twenty-four hours to amplify 3000
three LICs with high testing capacity and a reputable COVID- samples with a fluent and quality turnaround time. This
19 testing profile in LMICs(21, 22). implies a staff workload ratio of 15 for 1000 samples to run a
IJISRT21FEB179 www.ijisrt.com 342
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
RT PCR SARS-COV2 test for efficiency purposes. By optimizing the utilization existence platforms can contribute
adopting pooling in a low prevalence period, the productivity significantly.
could even be doubled(19). Countrywide, considering the
staffs directly involved in extraction and amplification, in Table 1: Required supplies for setting up testing in
September 2020, 73 staffs tested 86,086 samples with an September,2020
average of 2870 tests daily.
N Item Item/pack Qty/ pack/box/
Rwanda Biomedical Center, in collaboration with or box month items
Rwanda Joint Task Force for COVID-19, which was initiated 1 Extraction Kit 1 605 605
in the early pandemic period leads response, boosted staff
output. Testing centers got an opportunity of welcoming 2 Amplification 1 280 280
skilled and well-trained personnel for technical assistance in Kits DaN
Covid-19 testing. The staff from public institutions 3 Amplification 1 70 70
(University of Rwanda, public institutions, and public Kits BGI
hospitals) and private sectors (World Health Organization, 4 Cryovials 1,5ml 100 60000 600
Local and international Non-governmental Organization,
5 Tips 1000µl 100 86400 864
Project San Francisco) come together through public and
private institutions partnerships to enforce the response 6 Tips 20µl 100 33600 336
during the pandemic. Professional associations' role was also 7 Tips 10µl 100 13440 134
noticed whereby; the association of biomedical technologists
in Rwanda (ATEBIR) nominated supporting staff among 8 Tips 100µl 100 7680 77
their members. This existing partnership helped NRL and
other testing sites continue delivering other laboratory 9 Tips 200µl 100 27840 278
services amid staff capacity requirements. 10 Ethanol 5 60 12
➢ Lesson 3: Laboratory resources optimization 11 PCR Tubes 100 4000 40
Rwandan COVID-19 laboratory response was
characterized by the utilization of testing platform resources 12 Plates sealer 1 4 4
and was leveraged to increase COVID-19 testing capacity. 13 Plate standard 1 2 2
Assuring the continuous availability of COVID-19 reagents
and other suppliers was a major consideration. Due to the 14 Covid-19 Ag for 50 7531 151
pooling influence, 86,086 tests that were tested countrywide validation
required 605 extraction kits, 208 DaAn Gene Co Ltd
amplification kits for screening and 70 BGI amplification kits ➢ Lesson 4: Training and decentralization of molecular
for confirmation. The pooling approach to scale up testing in testing
asymptomatic patients has been acknowledged by U.S Food Pre-COVID-19, Rwanda Biomedical Centre (RBC)
and Drugs Authority (FDA) with ≥85% positive collaborated with the WHO to provide training for the staff in
agreement(23). More importantly, given the mode the sample collection of a highly contagious outbreak such as
transmission of COVID-19, safety conditions required Ebola, and as a result, many health staff was trained across
enforcement despite the existing global shortage of PPEs. the country for sample collection, packaging, transportation
Tables 1 and 2 summarize the list of needed reagents, PPE and analysis(30). These trainings were enforced by rigid
consumables, and equipment for tested 86,086 samples in preparedness on COVID-19 simulation conducted
September 2020. countrywide in different health settings to boost the staff's
knowledge towards COVID-19 testing and preparedness.
Rwanda benefited from Abbott m-2000 testing platform
in different laboratories across the country to decentralize Two weeks after COVID-19 emerged in Rwanda, the
testing based on the surge in cases and the specific need of need for staffing was highly acknowledged, and the National
testing in an identified area. Based on the financial reference Laboratory Division had volunteers who were
requirement of PCR-testing, the approach to COVID-19 trained during preparedness and were ready to get involved.
testing in each part of the country may change due to many Also, civil servants with relevant experience and a
factors; however, it's crucial to expand the capacity to test background in molecular and laboratory testing were placed
individuals to maximize public effort health measures. on secondment to facilitate the testing and sampling of
Furthermore, when countries are in the process of lift COVID-19. Due to the sporadic cases of COVID-19 in other
measures to contain the virus, the disease's incidence rate will regions other than Kigali, there was a need to enforce the
likely increase. Countries with limited physical resources and molecular testing laboratories used to test HIV viral load,
human capacity are specifically requested to prioritize testing Hepatitis B Virus (HBV), and Hepatitis C Virus (HCV) Viral
to understand the disease burden. Thus pooling strategy and Load for supporting COVID-19 testing.
IJISRT21FEB179 www.ijisrt.com 343
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
Table 2: Staff Personal Protective equipment needs for ➢ Lesson 5: The role of laboratory continuous quality
setting up testing improvement, accreditation, and laboratory information
system standardization
N Item Item/pack Qty pack/box/
or box items National reference laboratory had been already enrolled
1 Masks N95 20 2778 139 in the accreditation system and at the time the first case of
2 Mask KF94 5 275 55 COVID-19 was detected in Rwanda(31). The laboratory has
3 Surgical Masks 50 8488 170 been Sassessed and waiting for an accreditation certificate
from the accrediting body. This was another side of quality
4 Face Shield 10 482 48 encouragement and laboratory staff were motivated to work
5 Clean all 6 317 53 hard while adhering to the quality standards. The PPE were
6 Lab Coats 100 3704 37 adequately availed to allow the staff to work with safety
7 Gloves 100 32416 324 standards (table1). In addition to the lessons, the laboratory
information system (LIS) was functional and operational so it
8 Autoclave waste big 50 447 9 was adopted for capturing COVID-19 data. It was later
9 Autoclave waste 50 343 7 changed and adopted to the health management information
small system (HMIS) that is part of the District Health Information
10 Hand Sanitizer 0.5 100.5 201 Software 2 (DHS2) web-based and fully tangled to the
11 Bleach 0.5 49.5 99 surveillance investigation form of the COVID-19 case and
12 Permanent marker 12 110 9 contact information. This responded to the call for health
informatics response required (32). This is another lesson that
13 Pens 50 600 12 COVID-19 activated in our laboratory information system
14 Soap 1 4 4 that strengthened our operations and improved the testing and
reporting procedures in Rwanda.
However, in some settings, such as Kirehe District ➢ Lesson 6: Efficient use of funds and donation
Hospital, where the setting site for COVID-19 for the South- As a LMIC, Rwanda used government funds and gained
East was settled, there was no existing molecular-based support from partners to scale up COVID-19 testing to
testing and using the East African Community (EAC) Mobile increase the detection rate and monitor activities. In
Laboratory Network to intervene in epidemic outbreak particular, Rwanda had also received other donations,
response like Dengue. Ebola, COVID-19 testing site was including SARS-COV-2 RT-PCR testing kits from Jack ma
initiated in Kirehe. The employees benefited from onsite and Alibaba foundation for testing COVID-19 and Rapid
training and mentorship during the process. Using BIO-RAD diagnostic tests, including personal protective equipment and
CFX96 Cycler, Kirehe became a testing site running up to hand sanitizers of all types. All together was necessary at the
500 tests daily, facilitating monitoring the cross-border truck initial stages of the pandemic when the purchase of kits was
drivers surveillance of COVID-19 in the Southeast region. complicated at the time of global lockdown. Through were
Figure 2 and 3 show the scaling up of decentralized testing structured systems that monitor government funds, the
sites and a trend of COVID-19 testing by decentralized country has managed to handle the corruption in the COVID-
testing sites.
Fig 3: The Trends in COVID-19 testing for decentralized testing sites
IJISRT21FEB179 www.ijisrt.com 344
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
19 era, which has been a challenge in developing countries, to everyone in need. Future work should utilize scaling up
resulting in miss use (24). testing capacity to prepare ground for vaccine efficacy studies
before and after its roll out to monitor progress in limited
❖ Limitations/Challenges and bottlenecks during the scale- resource setting.
up process:
• Insufficient physical and human resources in the ACKNOWLEDGEMENT
laboratory to support new high demand of work: despite
the additional work and increased demand, the human We acknowledge the efforts of Rwanda Biomedical
resources were not proportionally increased to stand the Center and Ministry for Health in Rwanda’s efforts to contain
testing demand in all facilities and testing needed in the COVID-19. This research received no specific grant from any
community. funding agency in the public, commercial, or not-for-profit
sectors.
• Low engagement of private sector to support the testing
needs of several entertainment groups need of testing We would also like to acknowledge contribution of
before gathering such as football and school opening and Belamo NIYIGENA, CYIZA Jean D’Amour Joly and Joseph
conferences and meetings, these required access to private Hakizimana all from Rwanda Joint Task Force COVID-19,
testing facilities to meet demand and exiting guidelines Rwanda Biomedical Center, Ministry of Health, and
were not yet in place for proper coordination to control Kigali, Rwanda
transmission of the virus to control community
transmission. Cite as: Ivan, E., Iradukunda, P. G., Gashema, P., Ingabire,
A., Kabanda, A., … & Mutimura, E. (2021). Scaling up
• Insufficient laboratory and clinical research funding to laboratory testing capacity in the context of managing
sustain the health infrastructure for motivating researchers emerging pandemic: lessons learned from scaling up SARS-
and local scientists to generate new knowledge for COV-2 testing in Rwanda. International Journal of Scientific
SARSCOV-2 from a multidisciplinary team. Research in Science, Engineering and Technology, 6(2), 340-
346
• Inadequate sequencing capacity for new strains of REFERENCES
SARSCOV-2 emerging/ reported in UK, USA, South
Africa, and Nigeria, and other countries. Capacity to [1]. Zhu H, Wei L, Niu P. 2020. The novel coronavirus
monitor new variants/strains is still lacking resources. outbreak in Wuhan, China. Glob Heal Res Policy
https://doi.org/10.1186/s41256-020-00135-6.
• Supply and consumables usually a challenge to get on [2]. CDC. COVID-19 and Animals | CDC.
time, and a variety of supplies are needed for RT-PCR, https://www.cdc.gov/coronavirus/2019-ncov/daily-
and delivery lead time is critical while dealing with life-coping/animals.html.
emergencies and pandemic; there is a challenge of [3]. Africa CDC. COVID-19 – Africa CDC.
procurement and funds alignment with existing https://africacdc.org/disease/covid-19/.
procurement regulations for competitive tendering. [4]. WHO. WHO Director-General’s opening remarks at
the media briefing on COVID-19 - 12th October
III. CONCLUSION 2020. https://www.who.int/director-
general/speeches/detail/who-director-general-s-
The need for rapid response to contain the propagation opening-remarks-at-the-media-briefing-on-covid-19-
of a pandemic is not questionable. Laboratory testing has 12-october-2020.
played a role in identifying pandemic cases in the community [5]. Covax announces additional deals to access
and continuing to be the reliable approach to guide promising covid-19 vaccine candidates; plans global
surveillance. Given the limited physical and human resources rollout starting q1 2021.
in developing countries, early research-based actions to drive https://www.who.int/news/item/18-12-2020-covax-
the effective utilization of resources and funds might be announces-additional-deals-to-access-promising-
prioritized to boost the laboratory response during covid-19-vaccine-candidates-plans-global-rollout-
SARSCOV-2 outbreak and might be extrapolated to other starting-q1-2021.
SARS-like respiratory disease outbreak management in the [6]. Nkengasong JN, Yao K, Onyebujoh P. 2018.
future. Constant Continuous training of the scientific Laboratory medicine in low-income and middle-
workforce is essential to ensure that staff is not overwhelmed income countries: progress and challenges. Lancet.
by new pandemic workload. The information system [7]. Munster VJ, Koopmans M, van Doremalen N, van
technology is critical to digitalize all the laboratory reporting Riel D, de Wit E. 2020. A Novel Coronavirus
information, provide timely feedback, and feed data science Emerging in China — Key Questions for Impact
for policy action. A constant and continuous research Assessment. N Engl J Med
approach in the pandemic period is vital to elucidate new https://doi.org/10.1056/nejmp2000929.
testing methods that give results in short time and [8]. World Health Organization. 2020. Laboratory testing
decentralization of test at point of care is important to test and for 2019 novel coronavirus (2019-nCoV) in
control the pandemic before vaccine is introduced and availed suspected human cases. WHO - Interim Guid.
IJISRT21FEB179 www.ijisrt.com 345
Volume 6, Issue 2, February – 2021 International Journal of Innovative Science and Research Technology
ISSN No:-2456-2165
[9]. Peeling RW, Wedderburn CJ, Garcia PJ, Boeras D, [21]. Daily COVID-19 tests per thousand people.
Fongwen N, Nkengasong J, Sall A, Tanuri A, https://ourworldindata.org/grapher/daily-tests-per-
Heymann DL. 2020. Serology testing in the COVID- thousand-people-smoothed-7-
19 pandemic response. Lancet Infect Dis. day?tab=chart&stackMode=absolute&time=earliest..
[10]. Jendrny P, Schulz C, Twele F, Meller S, Von 2020-09-
Köckritz-Blickwede M, Osterhaus ADME, Ebbers J, 10&country=BGD~CIV~COD~ETH~GHA~KEN~
Pilchová V, Pink I, Welte T, Manns MP, Fathi A, MDG~MWI~MRT~MOZ~MMR~NPL~NGA~PAK
Ernst C, Addo MM, Schalke E, Volk HA. 2020. Scent ~RWA~SEN~SSD~TGO~TUN~UGA~ZMB~ZWE
dog identification of samples from COVID-19 ®ion=Africa.
patients - A pilot study. BMC Infect Dis [22]. COVID-19 |.
https://doi.org/10.1186/s12879-020-05281-3. https://www.rbc.gov.rw/index.php?id=707.
[11]. World Health Organization. COVID-19 in Rwanda: [23]. US Food DA. 2020. Pooled Sample Testing and
A country’s response | WHO | Regional Office for Screening Testing for COVID-19. US Food Drugs
Africa. https://www.afro.who.int/news/covid-19- Adm (2020).
rwanda-countrys-response. [24]. Dzinamarira T, Mukwenha S, Bschons RE, Cuadros
[12]. WHO. 2015. WHO Guide for the Stepwise DF, Mhlanga G, Musuka G, Eghtessadi R, Cuadros
Laboratory Improvement Prcess Towards DF, Mhlanga G, Musuka G. 2020. COVID-19
Accreditation in the African Region (SLIPTA). response in Zimbabwe: A Call for Urgent Scale-up of
[13]. Health-Rwanda M of. 2009. Health Sector Strategic Testing to meet National Capacity. Clin Infect Dis.
Plan. Heal (San Fr 1–98. [25]. Lu L, Lycett S, Ashworth J, Mutapi F, Woolhouse M.
[14]. Ndihokubwayo JB, Maruta T, Ndlovu N, Moyo S, 2021. What are SARS-CoV-2 genomes from the
Yahaya AA, Coulibaly SO, Kasolo F, Turgeon D, WHO Africa region member states telling us? BMJ
Abrol AP. 2016. Implementation of the World Health Glob Heal. BMJ Publishing Group.
Organization regional office for Africa Stepwise [26]. Mahase E. 2021. Covid-19: What new variants are
Laboratory Quality Improvement Process Towards emerging and how are they being investigated? BMJ
Accreditation. Afr J Lab Med 5:1–8. 372:n158.
[15]. Brooks ZC, Das S. 2020. COVID-19 Testing: Impact [27]. Update COVID-19 30 December 2020 | WHO |
of Prevalence, Sensitivity, and Specificity on Patient Regional Office for Africa.
Risk and Cost. Am J Clin Pathol 154:575–584. https://www.afro.who.int/news/update-covid-19-30-
[16]. Umviligihozo G, Mupfumi L, Sonela N, Naicker D, december-2020.
Obuku EA, Koofhethile C, Mogashoa T, Kapaata A, [28]. Update COVID-19 24 January 2021 | WHO |
Ombati G, Michelo CM, Makobu K, Todowede O, Regional Office for Africa.
Balinda SN. 2020. Sub-Saharan Africa preparedness https://www.afro.who.int/news/update-covid-19-24-
and response to the COVID-19 pandemic: A january-2021.
perspective of early career African scientists. [29]. Bennett A, Garcia E, Schulze M, Bailey M, Doyle K,
Wellcome Open Res Finn W, Glenn D, Holladay EB, Jacobs J, Kroft S,
https://doi.org/10.12688/wellcomeopenres.16070.2. Patterson S, Petersen J, Tanabe P, Zaleski S. 2014.
[17]. Brownson RC, Burke TA, Colditz GA, Samet JM. Building a Laboratory Workforce to Meet the Future.
2020. Reimagining Public Health in the Aftermath of Am J Clin Pathol 141:154–167.
a Pandemic. Am J Public Health 110:1605–1610. [30]. Ogunleye OO, Basu D, Mueller D, Sneddon J, Seaton
[18]. Yazdizadeh B, Majdzadeh R, Ahmadi A, Mesgarpour RA, Yinka-Ogunleye AF, Wamboga J, Miljković N,
B. 2020. Health research system resilience: lesson Mwita JC, Rwegerera GM, Massele A, Patrick O,
learned from the COVID-19 crisis. Heal Res Policy Niba LL, Nsaikila M, Rashed WM, Hussein MA,
Syst. BioMed Central Ltd. Hegazy R, Amu AA, Boahen-Boaten BB, Schellack
[19]. Mutesa L, Ndishimye P, Butera Y, Souopgui J, N, Rampamba EM, et al. Response to the Novel
Uwineza A, Rutayisire R, Musoni E, Rujeni N, Corona Virus (COVID-19) Pandemic Across Africa:
Nyatanyi T, Ntagwabira E, Semakula M, Successes, Challenges, and Implications for the
Musanabaganwa C, Nyamwasa D, Ndashimye M, Future. Front Pharmacol 11:1.
Ujeneza E, Mwikarago IE, Muvunyi CM, Mazarati [31]. Rusanganwa V, Gahutu JB, Nzabahimana I,
JB, Nsanzimana S, Turok N, Ndifon W. 2020. A Ngendakabaniga JMV, Hurtig A-K, Evander M.
strategy for finding people infected with SARS-CoV- 2018. Clinical Referral Laboratories in Rwanda. Am
2: optimizing pooled testing at low prevalence. arXiv. J Clin Pathol 150:240–245.
[20]. Daily COVID-19 tests per thousand people, 4th [32]. Reeves JJ, Hollandsworth HM, Torriani FJ, Taplitz
September, 2020. R, Abeles S, Tai-Seale M, Millen M, Clay BJ,
https://ourworldindata.org/grapher/daily-tests-per- Longhurst CA. 2020. Rapid response to COVID-19:
thousand-people-smoothed-7- Health informatics support for outbreak management
day?stackMode=absolute&time=2020-09- in an academic health system. J Am Med Informatics
04&country=RWA~KEN~ZAF~MAR~UGA~ZWE Assoc https://doi.org/10.1093/jamia/ocaa037.
~ZMB~TUN~COD~ETH~NAM~MOZ~NGA~SEN
~SSD®ion=Africa.
IJISRT21FEB179 www.ijisrt.com 346
Das könnte Ihnen auch gefallen
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (74)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- Rubrics For Competency Based ExamsDokument3 SeitenRubrics For Competency Based ExamsrajtanniruNoch keine Bewertungen
- Zikes - Jaaha - 2012 - Bilateral Ventriculocordectomy Via Ventral Approach For LAR PARDokument11 SeitenZikes - Jaaha - 2012 - Bilateral Ventriculocordectomy Via Ventral Approach For LAR PARranderson1972Noch keine Bewertungen
- Impact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaDokument6 SeitenImpact of Stress and Emotional Reactions due to the Covid-19 Pandemic in IndiaInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Utilization of Waste Heat Emitted by the KilnDokument2 SeitenUtilization of Waste Heat Emitted by the KilnInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Detection and Counting of Fake Currency & Genuine Currency Using Image ProcessingDokument6 SeitenDetection and Counting of Fake Currency & Genuine Currency Using Image ProcessingInternational Journal of Innovative Science and Research Technology100% (9)
- Entrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisDokument10 SeitenEntrepreneurial Creative Thinking and Venture Performance: Reviewing the Influence of Psychomotor Education on the Profitability of Small and Medium Scale Firms in Port Harcourt MetropolisInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- An Overview of Lung CancerDokument6 SeitenAn Overview of Lung CancerInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Ambulance Booking SystemDokument7 SeitenAmbulance Booking SystemInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Designing Cost-Effective SMS based Irrigation System using GSM ModuleDokument8 SeitenDesigning Cost-Effective SMS based Irrigation System using GSM ModuleInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Unmasking Phishing Threats Through Cutting-Edge Machine LearningDokument8 SeitenUnmasking Phishing Threats Through Cutting-Edge Machine LearningInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Digital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaDokument10 SeitenDigital Finance-Fintech and it’s Impact on Financial Inclusion in IndiaInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Auto Tix: Automated Bus Ticket SolutionDokument5 SeitenAuto Tix: Automated Bus Ticket SolutionInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Effect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictDokument13 SeitenEffect of Solid Waste Management on Socio-Economic Development of Urban Area: A Case of Kicukiro DistrictInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Computer Vision Gestures Recognition System Using Centralized Cloud ServerDokument9 SeitenComputer Vision Gestures Recognition System Using Centralized Cloud ServerInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Predictive Analytics for Motorcycle Theft Detection and RecoveryDokument5 SeitenPredictive Analytics for Motorcycle Theft Detection and RecoveryInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Study Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoDokument6 SeitenStudy Assessing Viability of Installing 20kw Solar Power For The Electrical & Electronic Engineering Department Rufus Giwa Polytechnic OwoInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Forensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsDokument12 SeitenForensic Advantages and Disadvantages of Raman Spectroscopy Methods in Various Banknotes Analysis and The Observed Discordant ResultsInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- An Industry That Capitalizes Off of Women's Insecurities?Dokument8 SeitenAn Industry That Capitalizes Off of Women's Insecurities?International Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Cyber Security Awareness and Educational Outcomes of Grade 4 LearnersDokument33 SeitenCyber Security Awareness and Educational Outcomes of Grade 4 LearnersInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Factors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaDokument6 SeitenFactors Influencing The Use of Improved Maize Seed and Participation in The Seed Demonstration Program by Smallholder Farmers in Kwali Area Council Abuja, NigeriaInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Parastomal Hernia: A Case Report, Repaired by Modified Laparascopic Sugarbaker TechniqueDokument2 SeitenParastomal Hernia: A Case Report, Repaired by Modified Laparascopic Sugarbaker TechniqueInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Blockchain Based Decentralized ApplicationDokument7 SeitenBlockchain Based Decentralized ApplicationInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Insights Into Nipah Virus: A Review of Epidemiology, Pathogenesis, and Therapeutic AdvancesDokument8 SeitenInsights Into Nipah Virus: A Review of Epidemiology, Pathogenesis, and Therapeutic AdvancesInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Implications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewDokument6 SeitenImplications of Adnexal Invasions in Primary Extramammary Paget's Disease: A Systematic ReviewInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Impact of Silver Nanoparticles Infused in Blood in A Stenosed Artery Under The Effect of Magnetic Field Imp. of Silver Nano. Inf. in Blood in A Sten. Art. Under The Eff. of Mag. FieldDokument6 SeitenImpact of Silver Nanoparticles Infused in Blood in A Stenosed Artery Under The Effect of Magnetic Field Imp. of Silver Nano. Inf. in Blood in A Sten. Art. Under The Eff. of Mag. FieldInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Smart Health Care SystemDokument8 SeitenSmart Health Care SystemInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Visual Water: An Integration of App and Web To Understand Chemical ElementsDokument5 SeitenVisual Water: An Integration of App and Web To Understand Chemical ElementsInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Air Quality Index Prediction Using Bi-LSTMDokument8 SeitenAir Quality Index Prediction Using Bi-LSTMInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Predict The Heart Attack Possibilities Using Machine LearningDokument2 SeitenPredict The Heart Attack Possibilities Using Machine LearningInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Compact and Wearable Ventilator System For Enhanced Patient CareDokument4 SeitenCompact and Wearable Ventilator System For Enhanced Patient CareInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Smart Cities: Boosting Economic Growth Through Innovation and EfficiencyDokument19 SeitenSmart Cities: Boosting Economic Growth Through Innovation and EfficiencyInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Parkinson's Detection Using Voice Features and Spiral DrawingsDokument5 SeitenParkinson's Detection Using Voice Features and Spiral DrawingsInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- Test Bank For Comprehensive Health Insurance 3rd Edition by VinesDokument15 SeitenTest Bank For Comprehensive Health Insurance 3rd Edition by Vinestrangdatif0Noch keine Bewertungen
- Data of Doctors in TexasDokument54 SeitenData of Doctors in TexasAdnanNoch keine Bewertungen
- Sex Ed PresentationDokument20 SeitenSex Ed Presentationapi-399914198Noch keine Bewertungen
- Dental Hygiene EssayDokument13 SeitenDental Hygiene Essayapi-3173047210% (1)
- DineshPonraj 1808165 - 05 00 - 1Dokument4 SeitenDineshPonraj 1808165 - 05 00 - 1revanth kumarNoch keine Bewertungen
- ISOPP Standards of Practice - Safe Handling of CytotoxicsDokument104 SeitenISOPP Standards of Practice - Safe Handling of CytotoxicsprovaoralNoch keine Bewertungen
- Report - For MaamDokument7 SeitenReport - For MaamSherchen Antonio-CortesNoch keine Bewertungen
- Aceclofenac Efficacy and Safety Vs DiclofenacDokument6 SeitenAceclofenac Efficacy and Safety Vs DiclofenacpdelaxNoch keine Bewertungen
- Abortions in Dairy Cows PDFDokument4 SeitenAbortions in Dairy Cows PDFransinghNoch keine Bewertungen
- Children's Health ProblemsDokument14 SeitenChildren's Health ProblemsAyro Business CenterNoch keine Bewertungen
- Drug Decriminalisation in Portugal Setting The Record StraightDokument10 SeitenDrug Decriminalisation in Portugal Setting The Record StraightGabriel Mota GalaNoch keine Bewertungen
- Sip Survey 2goDokument4 SeitenSip Survey 2goMichael P. CelisNoch keine Bewertungen
- Lawsuit Against Small Smiles Dental Center Aka Alabany Access Dental Center Et. Al.Dokument52 SeitenLawsuit Against Small Smiles Dental Center Aka Alabany Access Dental Center Et. Al.DebHgnNoch keine Bewertungen
- NURSING CARE PLAN-disturbed Sleep PatternDokument2 SeitenNURSING CARE PLAN-disturbed Sleep PatternJinnijinniNoch keine Bewertungen
- Training Curriculum On Drug Addiction Counseling - Chapter 5Dokument139 SeitenTraining Curriculum On Drug Addiction Counseling - Chapter 5Pinj Blue100% (1)
- Bronchiolitis in Infants and Children - Upto-Date 2015Dokument15 SeitenBronchiolitis in Infants and Children - Upto-Date 2015Gerardo MansillaNoch keine Bewertungen
- Medical Helminthology Introduction PDFDokument13 SeitenMedical Helminthology Introduction PDFfaiz0% (1)
- 4 - CatheterizationDokument20 Seiten4 - Catheterizationkirstenfrancine28Noch keine Bewertungen
- Housekeeping ManualDokument22 SeitenHousekeeping ManualWe Care Facility Management ServicesNoch keine Bewertungen
- Tuberculous MeningitisDokument34 SeitenTuberculous MeningitisLuvi PujiNoch keine Bewertungen
- Via Zis 1991Dokument2 SeitenVia Zis 1991drvivek reddyNoch keine Bewertungen
- Pressure Ulcer Prevention in Long Term CareDokument6 SeitenPressure Ulcer Prevention in Long Term CareambariyantoNoch keine Bewertungen
- ComprehensiveUnifiedPolicy TBDokument159 SeitenComprehensiveUnifiedPolicy TBallan14_reyesNoch keine Bewertungen
- Serum Albumin Level Adjusted With C-Reactive Protein Predicts Hemodialysis Patient SurvivalDokument9 SeitenSerum Albumin Level Adjusted With C-Reactive Protein Predicts Hemodialysis Patient Survivalmelda lestari haidirNoch keine Bewertungen
- Hahnemann S., Chronic DisDokument167 SeitenHahnemann S., Chronic Dishompat100% (1)
- Network Lists in UAE - Mar 2015Dokument93 SeitenNetwork Lists in UAE - Mar 2015Kamran KhanNoch keine Bewertungen
- NCP 1edited With ConstiDokument3 SeitenNCP 1edited With ConstiKizza SaavedraNoch keine Bewertungen
- Paediatric Triage ToolDokument32 SeitenPaediatric Triage Toolwellnessbywanda1Noch keine Bewertungen