Beruflich Dokumente
Kultur Dokumente
OS 213 RESP 1 #26 Pathology, Bronhiectasis, Bronchitis
Hochgeladen von
2012Originalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
OS 213 RESP 1 #26 Pathology, Bronhiectasis, Bronchitis
Hochgeladen von
2012Copyright:
Verfügbare Formate
PULMONARY OS 213
BLOCK B
Trans 26 |
PRECEPTORS Exam 2
OUTLINE The figure shows a marked inflammation of
the bronchi and bronchiolar walls. The inflammatory
I. CASE 1: BRONCHIECTASIS cells are seen as dark blue nuclei under the mucosal
II. CASE 2: CHRONIC BRONCHITIS lining. The right portion of this bronchiole shows
III. CASE 3: DIFFUSE ALVEOLAR epithelial erosion. There is exudate in the lumen.
DAMAGE Acute inflammatory cells, especially PMNs, are also
present, although evidence of chronic inflammation is
also likely to be present.
QUESTIONS
CASE 1: BRONCHIECTASIS
1. What are the underlying conditions associated with
A case of a 20 year old patient who bronchiectasis?
presented with recurrent fever and productive cough.
Sputum gradually became copious, foul and purulent. Bronchiectasis is caused by conditions that
Initial PE includes bronchial breath sounds on the predispose to chronic necrotizing infections and
peripheral lung fields; and bibasal crackles. consequent destruction of muscle and elastic support
tissue of bronchi and bronchioles. The most common
conditions are:
a. Bronchial obstruction (tumors; foreign
bodies), diffuse obstructive airway
diseases (atopic asthma; chronic
bronchitis)
b. Congenital or hereditary conditions
(congenital bronchiectasis; cystic
fibrosis)
c. Necrotizing or suppurative pneumonias.
2. What processes are necessary for the
development of bronchiectasis?
a. Persistent obstruction
b. Superimposed infection
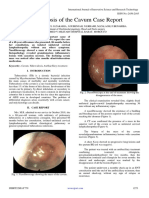
Figure 1. Cut section of the left lung 3. What type of inflammatory cells are present?
Compare with asthma.
Bronchiectasis is the permanent dilation of
bronchi and bronchioles and is secondary to cycles of • Acute inflammatory cells, especially
obstruction and infection. Note the inflamed left main PMNs, are present, although evidence of
stem bronchus in figure 1. It gives rise to branches in chronic inflammation is also likely to be
the left lower lobe that has been opened to present.
demonstrate that they extend nearly to the pleural • By comparison, in asthma, the
surface in this specimen. The diameters of the two inflammatory cells are composed of
opened bronchial branches in the lower lobe are CD4+ lymphocytes, eosinophils, mast
each greater than the diameter of the bronchus from cells, and a few neutrophils.
which they originate, indicating the severity of
bronchial dilation.
CASE 2: CHRONIC BRONCHITIS
A case of a 62 year old chain-smoker who
presented with persistent cough with daily sputum
production for almost 10 months each year since
1999. Occasionally, patient spat blood-tinged sputum,
but no consult was done until patient had dyspnea,
fever, and palpitations. Initial PE revealed cyanosis,
dynamic precordium and diffuse crackles on both
lungs.
Figure 2. Section from a bronchiole.
August 3, 2006 Rrrr… Page 1 of 3
PULMONARY OS 213
BLOCK B
Trans 26 |
PRECEPTORS Exam 2
airways, chronic inflammation of the airways
(predominantly lymphocytes) and hypertrophy of the
submucosal glands in the trachea and bronchi.
2. How does the mucous gland hyperplasia in
chronic bronchitis differ from that in a typical case of
asthma?
In typical allergic asthma, which also has
mucous gland hyperplasia, the bronchial wall has an
inflammatory infiltrate in which eosinophils are
prominent. There is also hypertrophy and hyperplasia
of smooth muscle cells in asthma.
Figure 3. Trachea and the main bronchi 3. What is the Reid Index?
The figure shows that the trachea in the mid- It is the ratio of the thickness of the mucous
upper field is hyperemic, and the bifurcation and main gland layer to the thickness of the wall between the
stem bronchi contain mucopurulent exudate. The epithelium and the cartilage. The normal ratio is 0.4.
underlying epithelium is also inflamed. This picture It is increased in chronic bronchitis.
may occur in chronic bronchitis and a superimposed
infection. However, one may also see this picture as
part of an acute inflammatory process in a patient CASE 3: DIFFUSE ALVEOLAR DAMAGE
dying of acute pneumonia. Remember that chronic
bronchitis is a clinical term.
A case of a 52 year old diabetic, with a
history of cerebral infarct and with left-sided
residuals, who was diagnosed to have community
acquired pneumonia on admission. Patient was
admitted for 6 days and was apparently improved on
discharge. At home, patient developed high grade
fever, body malaise and recurrence of productive
cough. Home medications were continued and
consult was done only 5 days later. Patient already
presented with difficulty of breathing and was
subsequently re-admitted. At the wards, patient was
hypotensive, tachypneic and febrile. Intubation was
done due to sudden respiratory distress and
cyanosis. Chest x-ray showed diffuse bilateral
Figure 4. Section of the bronchial wall. alveolar infiltration. Despite resuscitative efforts,
patient demised on the 2nd hospital day.
The histological section reveals that there are
changes typical of chronic bronchitis. The bronchial
epithelium is partially denuded in some regions but
squamous metaplasia is present in others. The
basement membrane is thickened and the mucosal
vessels are engorged and dilated. A moderate
number of plasmacytes and lymphocytes are present
in the submucosa and the gland layer which is
markedly enlarged and composes almost half of the
wall thickness of the bronchus. Majority of the galnds
are mucous in character. The glands and ducts are
dilated and filled with mucinous secretion containing
desquamated cells and inflammatory cells.
QUESTIONS
Figure 5. Lung section, scanning view.
1. What is your diagnosis? Bases?
The diagnosis is chronic bronchitis. It is a The figure shows diffused infiltration by
clinical term referring to a persistent cough with inflammatory cells with loss of alveolar architecture.
sputum production for at least three months in two There are areas revealing collection of pink
consecutive years. amorphous material and hyalinized deposits. Most
Characteristic features supporting this areas have necrotic debris with admixed neutrophils.
diagnosis are hypersecretion of mucous in the large
August 3, 2006 Rrrr… Page 2 of 3
PULMONARY OS 213
BLOCK B
Trans 26 |
PRECEPTORS Exam 2
3. Enumerate the composition of the hyaline
membrane seen in the histologic sections.
The waxy hyaline membranes lining the
alveolar walls consist of fibrin-rich edema fluid mixed
with the cytoplasmic and lipid remnants of necrotic
epithelial cells.
4. What pathologic finding is central to the
development of ARDS?
Diffuse damage to the alveolar capillary
walls. Neutrophils are thought to play an important
role in the pathogenesis of acute lung injury and
Figure 6. Lung section, HPO. ARDS. In contrast, the respiratory distress in
newborns is initiated by deficiency in pulmonary
The figure show damaged alveolar wall with surfactant.
fibrin rich hyaline material lining it.
GREETINGS
QUESTIONS
Dave: Oh my God, I have already reached the
1. What is your histologic diagnosis? saturation point, shet, when it comes to writing
greetings. I can’t feel any excitement anymore. This
Diffuse alveolar damage, representing the is so weird for it’s the only thing that I look forward to
usual underlying pathologic change of the clinically during transcribing but I think, this probable pathology
defined Adult Respiratory Distress Syndrome. is just secondary to the toxicity inflicted by the shet
thing called “pulmo”. Shet. Shet. Shet. Nevertheless,
2. Can the exact etiology be determined by the I have to occupy the remaining space. Sayang
microscopic findings alone? naman. JOJO, we love you still. Pulmo lang ang shet,
youre still gorgeous and “the best. Thanks Joguel for
No. The morphologic changes are non- lending us your flash. Salamat talaga. Hi BioDil
specific. DAD is best viewed as the pathologic end- people. Jorel, happy birthday uli, hope nagustuhan
result of acute alveolar injury caused by a variety of mo ang mga flowers and butterflies na pinaghirapan
insults and initiated by different mechanisms. nmin ni JOJO. Bea, babayaran na kita, sorry, antagal
kasi ni Vince magbayad. Orm, bagay pala kayo ni
3. What is the likely cause in this case? What other Bea, hehe. Chelle, salamat sa copy nung samplex
conditions can cause these findings? and SGD thingy. John, congrats! Unit 2B people,
magtipid na daw tayo sa kuryente sabi ni Rikka,
Sepsis, diffuse pulmonary infections, gastric hehe. Sorry, madami ako kasalanan in connection
aspiration, and mechanical trauma are responsible with the high kuryente natin. Sandee, ate mahal
for more than 50% of cases of ARDS. Other possible talaga kita. Kathy, minsan shet ka no, hehe, pero
causes include: girl….shet ka talaga, hehe, love you Kathy. Tara,
• Injuries: (pulmonary contusion; mahirap talagang gumamit ng laptop mo, hitech shet.
near drowning; fat embolism; burns; Mel R, miss na kita, din a tayo nakakapagusap. Atrio,
ionizing radiation) I salute you, buti ka pa, napagod na sa CLOSET,
• Inhaled irritants: (oxygen toxicity; yung iba, kahit hypoxemic at cyanotic na, CLOSETA,
smoke; irritant gasses and pa din…Kakapagod nun, but I respect them, echoz!
chemicals) HeHe. Val, uy girl, salamat sa pagtanggap ng work,
• Chemical injury: (heroin or mahal talaga kita. Dala ka ng car sa med mission ha.
methadone overdose; Pasakay Please! Maqi, Mai, and Mia, thanks sa mga
aspirin; barbiturate conversations hehe, Maqi, dakila ka talagang
overdose; paraquat) negastar. Iaia and Glai, sorry medyo maingay ako ha.
Binky, hay ang boobs talagang nagpupumiglas hehe.
• Hematologic conditions: (multiple
Go lang ng Go girl. Kris, salamat sa pagpapainvade
transfusions; DIC)
ng unit nyo. Siena, ang sarap ng pulvoron mo. Sa
• Pancreatitis mga BOYs na nagbigay ng flower kay JOrella, thank
• Uremia you. Pinasaya nyo ang bading. HehE. Geno and
• Cardiopulmonary bypass Odessa, basta.Hehe.
• Hypersensitivity reactions:
organic solvents, drugs
August 3, 2006 Rrrr… Page 3 of 3
Das könnte Ihnen auch gefallen
- 6th Central Pay Commission Salary CalculatorDokument15 Seiten6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- 6th Central Pay Commission Salary CalculatorDokument15 Seiten6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Diseases of The Anus Rev#1CDokument77 SeitenDiseases of The Anus Rev#1C2012Noch keine Bewertungen
- Holy Basil: Natural Remedy For StressDokument4 SeitenHoly Basil: Natural Remedy For StressOmar Katalanisch100% (1)
- Review Lectures Forlu6: Basic Eye Exam Common Opd Complaints Common Er Cases PharmacologyDokument110 SeitenReview Lectures Forlu6: Basic Eye Exam Common Opd Complaints Common Er Cases Pharmacologyupmed2012block9Noch keine Bewertungen
- ++serrapeptase The Miracle EnzymeDokument2 Seiten++serrapeptase The Miracle EnzymeabazanNoch keine Bewertungen
- Anatomy and Physiology CopdDokument15 SeitenAnatomy and Physiology CopdAssenav May100% (3)
- Medical Mnemonic Sketches : Pulmonary DiseasesVon EverandMedical Mnemonic Sketches : Pulmonary DiseasesNoch keine Bewertungen
- Book Based: Etiology: Tubercle Bacilli Precipitating Factors Predisposing FactorsDokument7 SeitenBook Based: Etiology: Tubercle Bacilli Precipitating Factors Predisposing FactorsIrish EspinosaNoch keine Bewertungen
- PulmDokument11 SeitenPulmNia IarajuliNoch keine Bewertungen
- Miasms Chart - PDF VersionDokument1 SeiteMiasms Chart - PDF Versionsergiomiguelgomes992369% (16)
- NCM 118 - Lesson 2 (COPD)Dokument6 SeitenNCM 118 - Lesson 2 (COPD)Bobby Christian DuronNoch keine Bewertungen
- Bronchoscopy and Esophagoscopy A Manual of Peroral Endoscopy and Laryngeal SurgeryVon EverandBronchoscopy and Esophagoscopy A Manual of Peroral Endoscopy and Laryngeal SurgeryBewertung: 5 von 5 Sternen5/5 (1)
- Physiotherapy Practice Guidelines For COPDDokument35 SeitenPhysiotherapy Practice Guidelines For COPD健康生活園Healthy Life Garden100% (1)
- CIE A Level Biology - Gas ExchangeDokument14 SeitenCIE A Level Biology - Gas ExchangeSaraNoch keine Bewertungen
- Chapter 24 Management of Patients With Chronic Pulmonary DisordersDokument3 SeitenChapter 24 Management of Patients With Chronic Pulmonary DisordersPeej Reyes100% (1)
- BronchitisDokument11 SeitenBronchitisRenuka Sivaram100% (2)
- Bronchiectasis OkDokument60 SeitenBronchiectasis OkImmanuelNoch keine Bewertungen
- Medical Progress: Review ArticleDokument11 SeitenMedical Progress: Review ArticlemayaNoch keine Bewertungen
- Covid DiagnosticDokument44 SeitenCovid DiagnosticFrancesco De PalmaNoch keine Bewertungen
- Acquired Bronchiectasis: AbcessDokument14 SeitenAcquired Bronchiectasis: AbcessAhmed GaberNoch keine Bewertungen
- Abnormal Chest FindingsDokument5 SeitenAbnormal Chest FindingsAbishek Prince100% (1)
- 2.BE PathogenesisDokument7 Seiten2.BE PathogenesisJaya Semara PutraNoch keine Bewertungen
- BRONCHIECTASISDokument2 SeitenBRONCHIECTASISKaren Mae PadillaNoch keine Bewertungen
- BronchiectasisDokument4 SeitenBronchiectasisCitrusNoch keine Bewertungen
- THE So-Called Middle Lobe Syndrome: LeegaardDokument3 SeitenTHE So-Called Middle Lobe Syndrome: LeegaardHari PrasadNoch keine Bewertungen
- A Bronchographic Sign of Chronic: Bronchitis'Dokument4 SeitenA Bronchographic Sign of Chronic: Bronchitis'Ziyan NafisahNoch keine Bewertungen
- Diagnostic Evaluation of BronchiectasisDokument16 SeitenDiagnostic Evaluation of BronchiectasisAinun Jariah MuliadiNoch keine Bewertungen
- BronchopneumoniaDokument14 SeitenBronchopneumoniaCaitlynNoch keine Bewertungen
- Chronic Bronchitis and BronchiectasisDokument3 SeitenChronic Bronchitis and BronchiectasisMuhammad Dimas HaryokoNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument2 SeitenChronic Obstructive Pulmonary DiseaseShrestha AnjivNoch keine Bewertungen
- Chapter 15 Respiratory System (2nd Edition)Dokument54 SeitenChapter 15 Respiratory System (2nd Edition)vs7ksgrj8pNoch keine Bewertungen
- BronchiolitisDokument9 SeitenBronchiolitisretnomardiyantiNoch keine Bewertungen
- Emphysema Chronic Bronchitis BronchiectasisDokument7 SeitenEmphysema Chronic Bronchitis BronchiectasisFortin BerryNoch keine Bewertungen
- Lung AbscessDokument20 SeitenLung AbscessSAMOEINoch keine Bewertungen
- 长沙医学院 国际教育学院 Pathology (病理学)Dokument57 Seiten长沙医学院 国际教育学院 Pathology (病理学)Ichsan FajriNoch keine Bewertungen
- Div Clsis An Update Onvestigation DivDokument4 SeitenDiv Clsis An Update Onvestigation DivAshwinNoch keine Bewertungen
- 11 Full PDFDokument3 Seiten11 Full PDFPriyaNoch keine Bewertungen
- (PTL) 10 Pulmonary PathologyDokument51 Seiten(PTL) 10 Pulmonary Pathologyjohnderice.mojares.medNoch keine Bewertungen
- Pathology of Respiratory SystemDokument61 SeitenPathology of Respiratory SystemIngeNoch keine Bewertungen
- Une Dyspnee Aigue Revelatrice Dun Syndrome de Mounier-Kuhn: A Propos Dun Cas Et Revue de LitteratureDokument6 SeitenUne Dyspnee Aigue Revelatrice Dun Syndrome de Mounier-Kuhn: A Propos Dun Cas Et Revue de LitteratureIJAR JOURNALNoch keine Bewertungen
- Organizing Pneumonia Following Covid19 PneumoniaDokument4 SeitenOrganizing Pneumonia Following Covid19 PneumoniaKhangNoch keine Bewertungen
- (23933356 - Romanian Journal of Rhinology) Mucocele of The Middle Turbinate - A Rare Entity PDFDokument4 Seiten(23933356 - Romanian Journal of Rhinology) Mucocele of The Middle Turbinate - A Rare Entity PDFGeorge Razvan DascalescuNoch keine Bewertungen
- Etiology: 1. Compare Lobar Pneumonia With Lobular Pneumonia On The ListDokument3 SeitenEtiology: 1. Compare Lobar Pneumonia With Lobular Pneumonia On The Listselam kalayuNoch keine Bewertungen
- Tuberculosis of The Cavum Case ReportDokument3 SeitenTuberculosis of The Cavum Case ReportInternational Journal of Innovative Science and Research TechnologyNoch keine Bewertungen
- BronchitisDokument40 SeitenBronchitisJAMES NYIRENDANoch keine Bewertungen
- Lung Abscess Handout PDFDokument3 SeitenLung Abscess Handout PDFTansanee MalivalayaNoch keine Bewertungen
- Concept MapDokument4 SeitenConcept MapMersiya SarapuddinNoch keine Bewertungen
- (Materi Dr. Heny) PneumoniaDokument86 Seiten(Materi Dr. Heny) PneumoniaFathiyah SalsabilaNoch keine Bewertungen
- Key Points: Diagnostic Imaging in Adult Non-Cystic Fibrosis BronchiectasisDokument8 SeitenKey Points: Diagnostic Imaging in Adult Non-Cystic Fibrosis BronchiectasisAmirah SilinoNoch keine Bewertungen
- Raut 2018Dokument4 SeitenRaut 2018nesrine ninaNoch keine Bewertungen
- TB RadiologyDokument15 SeitenTB RadiologyNathania PutriNoch keine Bewertungen
- Bronkiektasis: DOSEN: Dr. Merari Panti Astuti, SP - Rad Satrianti Totting (42170175)Dokument43 SeitenBronkiektasis: DOSEN: Dr. Merari Panti Astuti, SP - Rad Satrianti Totting (42170175)quinnNoch keine Bewertungen
- 1 Lung AbscessDokument51 Seiten1 Lung AbscessЕвгений ХанькоNoch keine Bewertungen
- Bacillus Cereus Bacteremia and Meningoen PDFDokument4 SeitenBacillus Cereus Bacteremia and Meningoen PDFdr israrNoch keine Bewertungen
- Bronko PneumoniaDokument33 SeitenBronko PneumoniaNurul Hidayati SyarahNoch keine Bewertungen
- 5.3.2.1 Pulmonary infection-นพ.อภิชาติ ตันตระวรศิลป์Dokument85 Seiten5.3.2.1 Pulmonary infection-นพ.อภิชาติ ตันตระวรศิลป์golfntwsxNoch keine Bewertungen
- DifferentialsDokument7 SeitenDifferentialsStewart Garneth Reston RancesNoch keine Bewertungen
- Suppurative Desease of Lungs and PleuraDokument26 SeitenSuppurative Desease of Lungs and PleuraGarima SahuNoch keine Bewertungen
- Post-Tuberculous Bronchiectasis: Indications For Surgical TreatmentDokument2 SeitenPost-Tuberculous Bronchiectasis: Indications For Surgical TreatmentJaya Semara PutraNoch keine Bewertungen
- Diffuse Pulmonary DiseasesDokument19 SeitenDiffuse Pulmonary DiseasessivaNoch keine Bewertungen
- 16 Organizing Pneumonia - Libre PathologyDokument4 Seiten16 Organizing Pneumonia - Libre PathologyfadoNoch keine Bewertungen
- Patient Based PathophysiologyDokument2 SeitenPatient Based PathophysiologyDeinielle Magdangal RomeroNoch keine Bewertungen
- TxBookofTB 2ndeditDokument10 SeitenTxBookofTB 2ndeditalukoNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease: Iman Galal, MDDokument60 SeitenChronic Obstructive Pulmonary Disease: Iman Galal, MDYan Sheng HoNoch keine Bewertungen
- Pneumonia: or Generalized Patchy InfiltrateDokument3 SeitenPneumonia: or Generalized Patchy InfiltrateizyanzatiNoch keine Bewertungen
- Diffuse Lung Disease Caused by Cotton Fibre Inhalation But Distinct From ByssinosisDokument3 SeitenDiffuse Lung Disease Caused by Cotton Fibre Inhalation But Distinct From ByssinosisAnonymous h1XAlApsUNoch keine Bewertungen
- TarpaulinDokument1 SeiteTarpaulinJhoson Ige E. LaxamanaNoch keine Bewertungen
- Pneumonia, Pleuropneumonia, Lung Abscess, and Pleuritis: Radiographic Appearance of PneumoniaDokument9 SeitenPneumonia, Pleuropneumonia, Lung Abscess, and Pleuritis: Radiographic Appearance of PneumoniaEasti EmoraNoch keine Bewertungen
- Laporan Pendahuluan Asuhan Keperawatan Anak Pada Klien Dengan BronkhitisDokument14 SeitenLaporan Pendahuluan Asuhan Keperawatan Anak Pada Klien Dengan BronkhitisDicky Aris SetiawanNoch keine Bewertungen
- Med2 - 2.2.2.cystic FibrosisDokument4 SeitenMed2 - 2.2.2.cystic Fibrosisk6598jrx67Noch keine Bewertungen
- Ajon Codp Web CausationDokument3 SeitenAjon Codp Web Causationapi-383804230Noch keine Bewertungen
- Fa Step 1 ScheduleDokument5 SeitenFa Step 1 ScheduleDinesh DalviNoch keine Bewertungen
- Boards SyllabusDokument14 SeitenBoards Syllabus2012Noch keine Bewertungen
- General Recommendation ImmunizationDokument69 SeitenGeneral Recommendation Immunization2012Noch keine Bewertungen
- PCAP UpdatesDokument60 SeitenPCAP Updates2012Noch keine Bewertungen
- ADA Summary of Guidelines 2011Dokument7 SeitenADA Summary of Guidelines 2011IffatNaeemNoch keine Bewertungen
- Boards SyllabusDokument14 SeitenBoards Syllabus2012Noch keine Bewertungen
- Clin Tox Oral Vs IV ActylcysteineDokument19 SeitenClin Tox Oral Vs IV Actylcysteine2012Noch keine Bewertungen
- USMLEboardswhatworked 2008Dokument32 SeitenUSMLEboardswhatworked 20082012Noch keine Bewertungen
- CEBM Levels of EvidenceDokument2 SeitenCEBM Levels of Evidence2012100% (2)
- The Division of Plastic SurgeryDokument36 SeitenThe Division of Plastic Surgery2012Noch keine Bewertungen
- Glomerulonephritis Block A TransDokument7 SeitenGlomerulonephritis Block A Trans2012Noch keine Bewertungen
- Review of The Evidence For Herbal Medications and NutraceuticalsDokument5 SeitenReview of The Evidence For Herbal Medications and Nutraceuticals2012Noch keine Bewertungen
- Art of Med Trans Feb 28Dokument9 SeitenArt of Med Trans Feb 282012Noch keine Bewertungen
- CSAP Full 2002Dokument125 SeitenCSAP Full 20022012Noch keine Bewertungen
- SCOPING DOCUMENT For WHO Treatment Guidelines On Pain Related ToDokument10 SeitenSCOPING DOCUMENT For WHO Treatment Guidelines On Pain Related To2012Noch keine Bewertungen
- Pharma EvaluationDokument1 SeitePharma Evaluation2012Noch keine Bewertungen
- Test Blueprint For Final Exam 2008-2009 For 75 PtsDokument3 SeitenTest Blueprint For Final Exam 2008-2009 For 75 Pts2012Noch keine Bewertungen
- American Diabetes Association (ADA) gUIDELINESDokument43 SeitenAmerican Diabetes Association (ADA) gUIDELINESSamuel Rudolf Maranatha JulioNoch keine Bewertungen
- Organ Transplantation, Immunology and RejectionDokument2 SeitenOrgan Transplantation, Immunology and Rejection2012Noch keine Bewertungen
- Patho Lab Trans - ButchDokument6 SeitenPatho Lab Trans - Butch2012Noch keine Bewertungen
- Renal Patho Lab 2 PART 1 ColoredDokument8 SeitenRenal Patho Lab 2 PART 1 Colored2012Noch keine Bewertungen
- Cancer Pain Relief Who 1998Dokument86 SeitenCancer Pain Relief Who 19982012100% (1)
- Trans Pulmopatho ColoredDokument8 SeitenTrans Pulmopatho Colored2012Noch keine Bewertungen
- Trans Glomerularpatho FinalDokument16 SeitenTrans Glomerularpatho Final2012100% (1)
- OS 214 - Renal Module - Imaging of The KUBDokument9 SeitenOS 214 - Renal Module - Imaging of The KUB2012Noch keine Bewertungen
- 434 OS 212 PictoTrans - Cutaneous SymptomatologyDokument51 Seiten434 OS 212 PictoTrans - Cutaneous Symptomatology2012Noch keine Bewertungen
- Hypo Ventilation SyndromesDokument22 SeitenHypo Ventilation SyndromesFer45Noch keine Bewertungen
- Degenerative Disc DiseaseDokument13 SeitenDegenerative Disc DiseaseSisuka CeritaNoch keine Bewertungen
- ATI Respiratory PowerpointDokument90 SeitenATI Respiratory PowerpointAnn KelseaNoch keine Bewertungen
- Dhudhi Badi ImportantDokument4 SeitenDhudhi Badi ImportantpoonamNoch keine Bewertungen
- STDTRT Guidelilne Essentialdruglist SA PHCDokument392 SeitenSTDTRT Guidelilne Essentialdruglist SA PHCAvinash Rangarajan100% (1)
- Presentation Science ScrapbookDokument16 SeitenPresentation Science ScrapbookJJ LimNoch keine Bewertungen
- Emphysema - PhysiopediaDokument1 SeiteEmphysema - PhysiopediaШеікх АбрарNoch keine Bewertungen
- BronchitisDokument3 SeitenBronchitisVenkatesan VidhyaNoch keine Bewertungen
- Dr. Blyden: Chronic Obstructive Pulmonary Disease (Copd)Dokument63 SeitenDr. Blyden: Chronic Obstructive Pulmonary Disease (Copd)Blyden NoahNoch keine Bewertungen
- Antitussives & MucolyticsDokument50 SeitenAntitussives & MucolyticsSaha DirllahNoch keine Bewertungen
- Beta 2 AgonistsDokument198 SeitenBeta 2 AgonistsLeonardo FerreiraNoch keine Bewertungen
- Imir Studyguide2014Dokument499 SeitenImir Studyguide2014Sam GhaziNoch keine Bewertungen
- In The Name of Allah, Most Gracious, Most MercifulDokument25 SeitenIn The Name of Allah, Most Gracious, Most Mercifulmnajeeb807196Noch keine Bewertungen
- CH 129: Lower Respiratory Tract Infections Self-Assessment Question-AnswersDokument2 SeitenCH 129: Lower Respiratory Tract Infections Self-Assessment Question-AnswersTop VidsNoch keine Bewertungen
- The Effects of SmokingDokument2 SeitenThe Effects of SmokingNino-prexy AcdalNoch keine Bewertungen
- Acute Bronchitis: Bjorn BuhagiarDokument4 SeitenAcute Bronchitis: Bjorn Buhagiaryulita kesumaNoch keine Bewertungen
- Nursing Care Plan: Group 1 Pangilinan Tadeo Sta. Maria Tecson Rivera SilvestreDokument8 SeitenNursing Care Plan: Group 1 Pangilinan Tadeo Sta. Maria Tecson Rivera SilvestreTADEO, Joyce B.Noch keine Bewertungen
- 06 Offline Module CourseDokument15 Seiten06 Offline Module CourseDylan Angelo AndresNoch keine Bewertungen
- Exam Tips PDFDokument32 SeitenExam Tips PDFKaarthigan RamaiahNoch keine Bewertungen
- Outbreak of Lung DiseaseDokument8 SeitenOutbreak of Lung DiseaseRowan MacLauchlinNoch keine Bewertungen
- English q4 w6Dokument63 SeitenEnglish q4 w6MARICEL SIBAYANNoch keine Bewertungen