Beruflich Dokumente
Kultur Dokumente
Anti Ischemia Drugs
Hochgeladen von
ckasapOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Anti Ischemia Drugs
Hochgeladen von
ckasapCopyright:
Verfügbare Formate
Anti-Ischemic Drugs: A compilation from Levis lecture, baby Katzung, and some Lilly/Costanzo.
(Not all of ischemic heart disease though.) If you understand this slide and know where the different drugs fit in, you are in decent shape.
3 types of ANGINA (chest pain due to oxygen shortage in the heart) Classic (effort, stress, atherosclerotic) Variant (at rest, angiospastic, -- Prinzmetal) Unstable (thrombotic) use antipatelet therapy too Determinants of Cardiac Oxygen demand: Different sources describe the oxygen demand/supply problem in different terms, but the main determinants are the same. Katzung describes it as a function of fiber tension. (kind of weird)
Preload: blood volume. Sympathetic activity increases preload due to increased venous tone Afterload: arterial blood pressure due to sympathetic outflow Inc Heart Rate increases demand and reduces supply: 1) at fast HR, fibers spend more time (proportionally) at systolic tension levels. 2) Less diastole = less time for coronary blood flow.
Contractility: increased ejection time = increased oxygen requirement
Costanzo describes it as cardiac work, and notes two categories: volume work and pressure work. Pressure work is MUCH more costly in terms of myocardial oxygen demand than, say, exercise. (think chronic hypertension, aortic stenosis.) Lillys notes 3 main contributors to myocardial O2 demand: (closest to Levi)
Increased wall stress (systolic and diastolic)
--Diastolic depends on preload (look at the chart, what physiologically alters preload? Venous capacitance) function of blood volume and venous tone --Systolic depends on afterload (what alters this? Peripheral resistance, heart rate, heart force, ejection time. Think of: Hypertension, aortic stenosis)
Heart rate see Katzung
Contractilitity see Katzung above
These determinants of myocardial O2 demand/supply will frame the pharmacologic strategy! Two main strategies: Vasodilate (increase Os delivery) or Cardiac Depress(reduce demand) Vasodilators include: Nitrates and Calcium Channel blockers Cardiac depressants include Calcium Channel blockers and Beta Blockers ** which calcium channel blocker depends on which class they vary! Surgical strategy: Revascularization (stents, CABG) In unstable angina, use urgent angioplasty, main focus is on anti-platelet therapy to prevent clotting but that is outside the scope of this lecture/chapter. Levis 3 types of Anti-anginal Drugs Nitrites and Nitrates Ca2+-channel Blockers -Blockers Nitrites and Nitrates PK Nitrates have: Poor <20% oral bioavailability by first pass metabolism (hepatic organic nitrate reductase denitrates it) Admin sublingual, bypass first pass and achieve fast therapeutic plasma levels Duration of Action: short, 15-30 min Sublingual doe limited by adverse efx such as: syncope, headache May give buccal/transdermal preparation for longer duration of action Nitrites are esters of nitrous acid Nitrates are esters of nitric acid They both release NO in vascular smooth muscle cells
Half life: un-denitrated is 2-8 min Hepatic metabolite is up to 3 h Excretion by kidney The efx are dose dependent. Sm dose venule dilation (desireable) Med dose arteries (do not want) High dose artioles and capillary sphincters (do not want) Effective for vasospasm!
MOA: denitration of nitrates in VSM cells by mito ALDH (aldehyde) causes release of nitric oxide (NO) NO stims sol GC Intracellular efx of cGMP are PI hydrolysis, Ca seq, dec Ca sensitivity Effect is vasorelaxation by dephosphorylation of myosin light chain phosphatase. Identical to nitroprusside MOA. End result is VSM relaxation. Note: people w/ ALDH -/- suffer no ill efx of NO OD!
Organ system Efx of NO: Cardiovascular:
peripheral venodilation reduced cardiac size, reduced CO through reduced preload arteriolar dilation reduced afterload
main effect is reduced O2 demand!!! Increased coronary flow may play a role, but is thought to be secondary. It DOES relax SMC of epicardial cor art and reduce vasospasm in var angina
Other organs: Relxes sm muscle of bronchi, GI, GU tracts, no other sig efx. Toxicities: tachycardia from baroreceptor reflex, orthostatic hypotension and syncope from venodilation, throbbing headache from meningeal artery vasodilation. NitrItes may also cause methemoglobinemia at high blood concentrations (cyanide antidote) NitrAtes do not cause methemoglobinemia., but do cause tolerance headaches (Monday disease.)
Nitrate Drug Interactions: with sildenafil (Viagra.) Nitrates increase production of cGMP, and sildenafil blocks PDE5 (which degrades cGMP) combo eft is dangerous hypoperfusion of organs from too much VSM relaxation!
Random facts from Levi lecture on PDE inhibitors:
1/2 Lives: sildenafil and vardenafil ~4 hr; tadalafil ~17.5 hr. Mild Vasodilators, minimal effect on BP Contraindicated with nitrate use Contraindicated with -blocker use Safe with antihypertensive medications
Other uses of PDE inhibition include: pulmonary hypertension In pulmonary hypertension, you have:
Decreased endothelial NO production decreased PA vasodilation, decreased PA remodeling Increased PDE5 activity in SMC and PDE3 in RV reduced PA vasodilation, rediced RV ionotropy
Calcium channel blockers Mech of action
Block L type calcium channels only, so does not interfere with hormonal release or neurotransmission, which employ other ca channels. Decrease intracellular calcium --> decrease muscle contractility. The effect may be either to vasodilator or to reduce cardiac contractility. Diff agents have diff spectrum of efx.
3 classes of calcium channel blockers Phenylalkylamine (verapamil) Benzothiazepine (diltiazem) Dihydroperidine (nifedipine)
QuickTime and a decompressor are needed to see this picture.
Effective for both stable and unstable angina.
For stable angina, the main MOA is to reduce O2 demand. Increases exercise tolerance and delays onset. For unstable angina, the main MOA is to increase O2 delivery, but also reduce demand and vasospasm For variant angina, the eft is to reduce vasospasm Also used in hypertension, supra ventricular tachycardia, migraine, preterm labor, stroke, and raynauds.
Dose dependent response: the clinical range is at the vasodilation dose. w/ inc dose you incur reduced heart contractility and reduced SAN. Specifically: Toxicities Constipation, edema, nausea, flushing, dizziness. More serious include congestive heart failure, av block, sa node depression. More common in verapamil Ethan dihydropyridines. Bepridil may induce torsade de points. Beta blockers must know: (propranolol, metoprolol, carvedilol) Competitive -- antagonize the -effects of catecholamines on heart, vessels, bronchi etc. Selective -- B2 v B1 v alpha (B1 is cardio-selective) need to fill this in for your 3 drugs Specifice -- don t antagonize cardiac stimulation and vasodilatation elicited by agents other than agonists SAR of -Blockers Goals in creating a -blocker: a) keep affinity for R, b) abolish intrinsic activity (as agonist, you want an antagonist) Thus, keep side chain, but substitute ring. Moa decrease cAmp decrease PKA activity, phosphorylate what? --? Decrease Ca intracellular concentration PROPRANOLOL At 50-100 ng/ml in humans propranolol will: 4. Lower plasma renin activity 3. Display anti-arrhythmic effects 2. Inhibit exercise tachycardia 1. Alleviate angina symptoms Summary of Effects Beneficial: decreased heart rate, cardiac force, blood pressure. Detrimental efx: increased heart size, longer ejection period. Asthma! (b/c of non-selectivity)
Clinical use Prophylactic tx of angina only. useful in acute setting. Ineffective against vasospasm but useful in exertional angina. Useful in combo w nitrates bc it prevents tachycardia and increased cardiac force induced by nitrates. Specific types: BETA-BLOCKER GENERATIONS 1st: Blanket or non-selective (1- + 2-blockers)(propranolol etc.) 2nd: Cardio-selective (1-blockers)(atenolol, metoprolol etc.) 3rd: Vasodilating properties (pindolol, carvedilol etc.) Mixed - and -blockers (labetalol) T1/2: 9 min (esmolol) to ~24 hr (nadolol) Lipid/water solubility influences route of elimination
QuickTime and a decompressor are needed to see this picture.
Nice Summary of all 3 classes of anti-Ischemics MOA:
QuickTime and a decompressor are needed to see this picture.
Das könnte Ihnen auch gefallen
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (121)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (895)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Raza's ECGDokument45 SeitenRaza's ECGcozmoxxxNoch keine Bewertungen
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
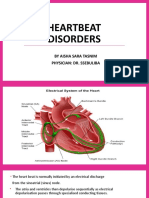
- Heartbeat Disorders: by Aisha Sara Tasnim Physician: Dr. SsebulibaDokument31 SeitenHeartbeat Disorders: by Aisha Sara Tasnim Physician: Dr. SsebulibaNinaNoch keine Bewertungen
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- ASE Reference Book PDFDokument68 SeitenASE Reference Book PDFrentedmule00Noch keine Bewertungen
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (73)
- NCP Ineffective Cerebral Tissue Perfusion STROKEDokument3 SeitenNCP Ineffective Cerebral Tissue Perfusion STROKEMa. Elaine Carla TatingNoch keine Bewertungen
- Cardiology - Corrected AhmedDokument23 SeitenCardiology - Corrected AhmedHanadi UmhanayNoch keine Bewertungen
- EKGDokument137 SeitenEKGGbariel100% (3)
- CARDIOVASDokument18 SeitenCARDIOVASVikash KushwahaNoch keine Bewertungen
- DefibrillationDokument11 SeitenDefibrillationAli Al-AhmedyNoch keine Bewertungen
- ArrhythmiaDokument25 SeitenArrhythmiad_94Noch keine Bewertungen
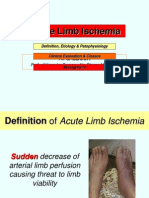
- Acute Limb Ischemia SiteDokument23 SeitenAcute Limb Ischemia Sitedokteraan100% (2)
- DLL Circulatory SystemDokument3 SeitenDLL Circulatory SystemJoiemmy Sumedca Bawengan Gayudan100% (1)
- Cut HeartDokument1 SeiteCut HeartckasapNoch keine Bewertungen
- Molly Toxicity Clinical CaseDokument2 SeitenMolly Toxicity Clinical CaseckasapNoch keine Bewertungen
- ROS ChecklistDokument2 SeitenROS Checklistmindful33Noch keine Bewertungen
- Drug Interactions in PatientsDokument2 SeitenDrug Interactions in PatientsckasapNoch keine Bewertungen
- GI MotilityDokument2 SeitenGI MotilityckasapNoch keine Bewertungen
- Mine ScoreDokument7 SeitenMine ScoreCharlys RhandsNoch keine Bewertungen
- Print 2 PDFDokument6 SeitenPrint 2 PDFfk unswagatiNoch keine Bewertungen
- Blood Pressure by Height & AgeDokument4 SeitenBlood Pressure by Height & AgeAzmi Muliatua PanjaitanNoch keine Bewertungen
- RatnaDokument3 SeitenRatnaAkram KastiranNoch keine Bewertungen
- Biomedical Engineering Biomedizinische TechnikDokument10 SeitenBiomedical Engineering Biomedizinische TechnikJayanthi ThiruvengadamNoch keine Bewertungen
- 15 - CCLS - PharmacologyDokument32 Seiten15 - CCLS - PharmacologyVENKATESH RAMSALINoch keine Bewertungen
- Cardiovascular SystemDokument40 SeitenCardiovascular SystemDouglas Jacques100% (1)
- Operator's Manual - CNAP Monitor 500Dokument119 SeitenOperator's Manual - CNAP Monitor 500evgenyNoch keine Bewertungen
- 2021 AHA ASA Guideline For The Prevention of Stroke in Patients With Stroke and TIA Clinical UpdateDokument43 Seiten2021 AHA ASA Guideline For The Prevention of Stroke in Patients With Stroke and TIA Clinical UpdateLê Thị HươngNoch keine Bewertungen
- Say No To Code Blue, Say YesDokument36 SeitenSay No To Code Blue, Say YesTheodorus PY PranotoNoch keine Bewertungen
- Perfusion Concept MapDokument1 SeitePerfusion Concept Mapapi-639782898Noch keine Bewertungen
- VT Guidelines PDFDokument74 SeitenVT Guidelines PDFgabrimarteNoch keine Bewertungen
- Second Degree Av Block Type 1 (Mobitz I or Wenckebach)Dokument1 SeiteSecond Degree Av Block Type 1 (Mobitz I or Wenckebach)christine louise bernardoNoch keine Bewertungen
- Calcium ScanDokument3 SeitenCalcium ScanStepyn SalvadorNoch keine Bewertungen
- Fact Sheet On HypertensionDokument1 SeiteFact Sheet On HypertensionMichael Vance Boctot100% (1)
- Golden First Minute 2Dokument9 SeitenGolden First Minute 2meliaNoch keine Bewertungen
- In Partial Fulfillment of The Requirements in Biological ScienceDokument11 SeitenIn Partial Fulfillment of The Requirements in Biological ScienceGodfrey Loth Sales Alcansare Jr.Noch keine Bewertungen
- Nursing Care Plan For Myocardial InfarctionDokument7 SeitenNursing Care Plan For Myocardial InfarctionRocelyn CristobalNoch keine Bewertungen