Beruflich Dokumente
Kultur Dokumente
Surg MCQ
Hochgeladen von
zhahmyOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Surg MCQ
Hochgeladen von
zhahmyCopyright:
Verfügbare Formate
1. The following are absorbable sutures a. Catgut b. Silk c. Polyamide (Nylon) d. Polyglyconate (Maxon) e.
Polyglactin (Vicryl)
Suture materials The purpose of a suture
to hold a wound together in good apposition until such time as the natural healing process is sufficiently well established to make the support from the suture material unnecessary and redundant.
Choice of a suture
Choice of suture depends on:
o o o o o
Properties of suture material Absorption rate Handling characteristics and knotting properties Size of suture Type of needle
Natural suture materials
Absorbable
o
Catgut - Plain or chromic
Non-Absorbable
o o o
Silk Linen Stainless Steel Wire
Synthetic suture materials
Absorbable
o o o o
Polyglycolic Acid (Dexon) Polyglactin (Vicryl) Polydioxone (PDS) Polyglyconate (Maxon)
Non-Absorbable
o o o
Polyamide (Nylon) Polyester (Dacron) Polypropylene (Prolene)
Absorbable suture are broken down by either:
Proteolysis (e.g. Catgut) Hydrolysis (e.g. Vicryl, Dexon)
Catgut
Made from the submucosa of sheep gastrointestinal tract Broken down within about a week Chromic acid delays hydrolysis Even so it is destroyed before many wounds have healed
Silk
Strong and handles well but induces strong tissue reaction Capillarity encourages infection causing suture sinuses and abscesses
Vicryl
Tensile strength
o o o
65% @ 14 days 40% @ 21 days 10% @ 35 days
Absorption complete by 70 days
Polydioxone
Tensile strength
o o o
70% @ 14 days 50% @ 28 days 14% @ 56 days
Absorption complete by 180 days
Common errors of suture use
Too many throws. Increases foreign body size. Causes stitch abscesses Intra-cuticular rather than subcuticular sutures causing hypertrophic scars Holding monofilament sutures with instruments reduces tensile strength by over 50% Holding butt of needle causes needle and suture breakage
2. Peutz Jeghers Syndrome a. Is an autosomal recessive condition b. Often presents with anaemia in childhood c. Is characterised by circumoral mucocutaneous pigmented lesions d. Is associated with adenomatous polyps of the small intestine e. Malignant change occurs in 2-3% of polyps
Benign colonic polyps
A polyp is a pedunculated lesion Not all polyps are tumours Not all polypoid tumours are benign Not all benign tumours are polypoid
3. Regarding peptic ulceration a. H. pylori is a gram-positive bacillus b. Duodenal is more common than gastric ulceration c. Zollinger-Ellison syndrome is associated with gastrin hyposecretion d. H2-blockers will heal 85-95% of duodenal ulcers in 8 weeks e. Triple therapy can eradicate H. pylori in 80% of patients in one week
4. Head Injuries a. More than 1 million people are seen in UK hospitals each year with head injuries b. Skull X-rays can exclude an intracerebral haematoma c. Raised intracranial pressure is associated with an increase in cerebral perfusion d. Cushing's response consists of a rise in blood pressure and fall in heart rate
e. Pupillary dilatation usually occurs on the same side as the intracerebral haematoma
5. During surgery on the submandibular gland a. An incision on the lower border of the mandible is safe b. The submandibular gland is seen to wrap around the posterior border of mylohyoid c. The facial artery and vein are divided as they course through the deep part of the gland d. The hypoglossal nerve is seen to loop under the submandibular duct e. Damage to the lingual nerve will cause loss of sensation to the posterior third of the tongue
6. Regarding pancreatic carcinoma a. 90% are ductal adenocarcinomas b. Less than 20% occur in the head of the gland c. The usual presentation is with pain, weight loss and obstructive jaundice d. Ultrasound has a sensitivity of 80-90% in the detection of the tumour e. Less than 20% of patients are suitable for curative surgery
7. Regarding the management of major trauma a. Deaths follow a trimodal distribution b. X-rays after the primary survey should be of AP Cervical spine, chest and pelvis c. Cardiac tamponade is characterised by raised BP, low JVP and muffled heart sounds d. Assessment of uncomplicated limb fractures should occur during the primary survey e. Deterioration of the casualty during the primary survey should lead to the secondary survey
8. Regarding appendicitis a. The risk of developing the illness is greatest in childhood b. Mortality increases with age and is greatest in the elderly c. 20% of appendices are extraperitoneal in a retrocaecal position d. Faecoliths are present in 75-80% of resected specimens e. Appendicitis is a possible diagnosis in the absence of abdominal tenderness
9. Regarding stones in the gallbladder a. Cholesterol stones are the most common
b. Pigment stones are due increased excretion of polymerised conjugated bilirubin c. Are not a risk factor for the development of gallbladder carcinoma d. 90% of gallstones are radio-opaque e. A mucocele of the gallbladder is caused by a stone impacted in Hartmann's pouch
10. Stones in the common bile duct a. Are found in 30% of patients undergoing cholecystectomy (Without pre-op ERCP) b. Can present with Charcot's Triad c. Are suggested by an bile duct diameter >8mm on ultrasound d. ERCP, sphincterotomy and balloon clearance is now the treatment of choice e. If removed by exploration of the common bile duct the T-tube can be removed after 3 days
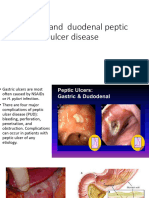
Peptic ulcer disease
Number of admissions for uncomplicated disease is falling Incidence of complications rated to NSAID use is increasing
Helicobacter pylori
H. pylori is gram-negative spiral flagellated bacterium Produces urease
Important in the aetiology of peptic ulcers and gastric cancer Found in:
o o o
Investigation
90% patients with duodenal ulceration 70% patients with gastric ulceration 60% patients with gastric cancer
The organism can be detected by Microscopy silver or Giemsa staining of antral biopsies Culture difficult and requires special culture techniques Rapid urease test colour changes due to change in pH
13
C or 14C breath test Ingested radioactive urea is broken down to carbon dioxide
Serology detected immunologically using an ELISA
Sensitivity and specificity of H. pylori diagnostic tests Test Rapid urease Culture Microscopy Carbon breath test Serology Sensitivity (%) 90 80 90 Specificity (%) 90-95 100 90
95
95
98
100
Medical management of peptic ulcer disease H2 Antagonists
65% healing at one month 85% healing at two months If stop treatment - 90% recurrence at 2 years If maintenance therapy - 20% recurrence at 5 years
Proton Pump inhibitors 90 - 100% healing at 2 months Low recurrence on long term maintenance
H. Pylori eradication 80% cured with dual or triple therapy Two weeks amoxycillin, metronidazole and omeprazole Short term recurrence rates low Long term recurrence rates are at present unknown Drugs have changed the need for ulcer surgery over last 20 years Admissions for elective surgery have significantly reduced The number of complications however remain unchanged May be increasing due to increased NSAID use in elderly
Bleeding and perforation still have mortality of >10%
History of peptic ulcer surgery Harberer (1882) - First gastric resection for benign ulcer Billroth (1885) - Billroth II Gastrectomy Von Fiselberg (1889) - 'Valve' to prevent bile reflux through gastroenterostomy Hofmeister (1896) & Polya (1911) - Retrocolic anastomosis Dragstedt (1943) - Truncal vagotomy Visick (1948) - Truncal vagotomy and drainage Johnson & Wilkinson (1970) - Highly selective vagotomy
Billroth I gastrectomy Originally described for the resection of distal gastric cancers Still used in gastric cancers if radical gastrectomy is inappropriate Later applied in the treatment of benign gastric ulcers Useful if ulcer situated high on the lesser curve or bleeding ulcer that requires resection Less effective than Polya Gastrectomy for duodenal ulcers
Billroth II / Polya gastrectomy Initially described for duodenal ulceration but rarely performed today Some form of vagotomy is the surgical treatment of choice for uncomplicated DU Occasionally used below a high gastric ulcer Ulcer invariably heals after surgery Useful in recurrent ulceration following previous vagotomy When constructing the anastomosis need to consider: Antecolic vs. retrocolic anastomosis Hofmeister valve so as direct bile in to the efferent loop Isoperistaltic vs. anteperistalitic anastomosis
Current surgical options Indications for surgical treatment of duodenal ulceration are:
Intractability Haemorrhage Perforation Obstruction
Aims of surgery are:
To cure the ulcer diathesis with The lowest risk of recurrence and complications
Surgical options for duodenal ulceration Operations for duodenal ulceration reduce acid production by the stomach Cephalic phase reduced by vagotomy Antral phase reduced by antrectomy May require gastric drainage procedure to overcome effects of vagotomy on gastric drainage
Open surgical procedures Truncal vagotomy and pyloroplasty Truncal vagotomy and gastrojejunostomy Truncal vagotomy and antrectomy Highly selective vagotomy Anterior seromyotomy and posterior truncal vagotomy
Laparoscopic peptic ulcer operations
Thoracoscopic truncal vagotomy and pyloric stretch Truncal vagotomy and pyloric stretch Highly selective vagotomy Posterior truncal vagotomy and selective anterior vagotomy Posterior truncal vagotomy and anterior seromyotomy
Post gastrectomy complications Percentage Recurrent ulceration Diarrhoea Dumping Bilious vomiting Iron deficiency anaemia B12 deficiency Folate deficiency
16 14 10
12
14 32
Post vagotomy complications Percentage Diarrhoea Dumping Bilious vomiting Bibliography 2 2 <2
Classification of large bowel polyps
Epithelial
o o o o o o o
Juvenile polyps
Adenomas - tubular, villous, tubulovillous Metaplastic polyps
Mesodermal Lipoma Leiomyoma Haemangioma
Hamartoma Juvenile polyps Peutz-Jeghers syndrome
Commonest form of polyp in children Can occur throughout large bowel but are most common in the rectum Usually present before 12 years Present with Prolapsing lump or rectal bleeding Not pre-malignant Treated by local endoscopic resection
Peutz-Jeghers syndrome Rare familial disorder Circumoral pigmentation and intestinal polyps Polyps found throughout gut but most common in the small intestine
Presents in childhood with bleeding, anaemia or intussusception Polyps can become malignant
Metaplastic polyps
Small plaques approximately 2 mm in diameter Pathogenesis unknown Not pre-malignant
Adenomas Benign epithelial neoplasm They are pre-malignant Risk of malignancy increases with size Malignancy more common in villous rather than tubular lesions
Most adenomas are asymptomatic 10% of population over 45 years have adenomatous polyps If do become symptomatic usually present with bleeding, mucous discharge or prolapse Villous adenomas may produce hypokalaemia but this is rare Diagnosis is often by sigmoidoscopy or colonoscopy Full colonoscopy essential to exclude other lesions Treatment is by transanal excision or colonoscopic snaring Patients require regular colonoscopic surveillance
Familial adenomatous polyposis Aetiological factor in 1% of colorectal cancers Its is an autosomal dominant Due to mutation on long arm of chromosome 5 Mutation induces proliferation of mucosa throughout GI tract Develop colonic polyps in teens or early 20s Untreated progresses to cancer by 30s Screening by rigid or flexible sigmoidoscopy
Safe alternative to colonoscopy as rectal sparing rarely seen Start late teens and continue until 40 yrs and polyp free. Extra-colonic manifestations:
o o o o o o o o
Osteomas. epidermoid cysts = Gardeners Syndrome Gastroduodenal polyps Desmoid tumours Congenital hypertrophy of retinal pigmented epithelium
Surgical options: Panproctocolectomy and ileostomy Restorative panproctocolectomy Subtotal colectomy and ileorectal anastomosis NB will require surveillance of rectal stump
Hereditary non-polyposis colorectal cancer syndrome
Accounts for 5-10% of colorectal cancers Results in mainly right sided cancers Increased risk of other gastrointestinal, urological and gynaecological malignancy Diagnosed by having 3 affected relatives, in 2 generations and one patient <50 years Recommend to start colonoscopic screening starting 5 years before youngest affected relative.
Bibliography Campbell W J, Spence R A J, Parks T G. Familial adenomatous polyposis. Br J Surg 1994; 81: 1722 - 33.
Questions 11-20 11. Regarding crystalloid solutions a. Normal saline contains 154 mmol sodium and 154 mmol of chloride b. 3 litres of dextrose saline in a day will provide 90 mmol of sodium c. 2 grams of potassium chloride is equal to 57 mmol of the salt d. Hartmann's solution contains calcium and bicarbonate e. The daily maintenance potassium requirement of a 40 Kg woman is about 40 mmol
12. Regarding colloid solutions a. Human albumin has a molecular weight of 69 kDa b. Albumin has a half life in the circulation of about 15 hours c. Gelatins (e.g. Haemaccel) are polysaccharides with a MW of about 35 kDa d. Dextrans reduce platelet aggregation and can induce anaphylaxis e. 6% Hydroxylethyl Starch (HES) is synthetic polysaccharide derived from amylopectin
13. Central parenteral nutrition a. Is a hypo-osmolar solution b. Typically contains 14-16g nitrogen as D-amino acids c. Typically contains about 250g glucose d. Is associated with metabolic disturbances in about 5% patients e. Can induce derangement of liver function tests
14. Solitary thyroid nodules a. Are more prevalent in women b. In the adult population less than 10% are malignant c. More than 50% of scintigraphically cold nodules are malignant d. The risk of a hot module being malignant is negligible e. Should be surgically removed in all patients
15. Regarding abdominal wall hernias a. Almost 100,000 hernia operations are performed annually in the United Kingdom b. 20% of inguinal hernias are indirect c. In women inguinal hernias are as common as femoral hernias d. The mortality assocaited with strangulation is over 10% e. The mortality has reduced dramatically over the past 30 years
16. The femoral canal a. Lies lateral to the femoral vein b. Has the inguinal ligament as its anterior border c. Has the lacunar ligament as its lateral border d. Has the pectineal ligament as its posterior border e. Contains the lymph node of Cloquet
17. Intermittent claudication
a. Affects less than 1% of men over the age of 50 years b. At 5 years 10% of claudicants will have progressed to an amputation c. At 5 years 20% of claudicants will have died from ischaemic heart disease d. Is usually associated with an ankle / brachial pressure index (ABPI) > 0.7 e. Is associated with a fall in the ABPI on exercise with delayed recovery
18. The pathology of ulcerative colitis a. Shows full thickness inflammation b. The rectum is almost always involved c. 10% patients have terminal ileal disease d. Enterocutaneous or intestinal fistulae are common e. The serosa is usually normal
19. Regarding surgery for ulcerative colitis a. 30% patients with total colitis will require surgery within 5 years b. Panproctocolectomy and pouch formation is appropriate as an emergency operation c. Pouches can be fashioned as 'S' 'J' or 'W' loops d. Over 90% patients with a pouch have perfect continence e. With a pouch the mean stool frequency is about 6 times per day
20. Regarding benign breast disease
a. Cyclical mastalgia is the commonest reason for referral to the breast clinic b. Fibroadenomas are derived from the breast lobule c. Lactational breast abscesses are usually due to Staph aureus d. Duct ectasia is more common in smokers e. Atypical lobular hyperplasia is associated with an increased risk of breast cancer
Das könnte Ihnen auch gefallen
- Surgical Tutor MCQDokument2 SeitenSurgical Tutor MCQfreeuser3100% (8)
- 1 - The Following Are Absorbable SuturesDokument15 Seiten1 - The Following Are Absorbable SuturesKhaled ShaheenNoch keine Bewertungen
- Pathogens: Hepatic AbscessDokument8 SeitenPathogens: Hepatic Abscessalberto cabelloNoch keine Bewertungen
- Mcq's With Key Surgery - BDokument7 SeitenMcq's With Key Surgery - BSiraj Ul Islam50% (2)
- Ec FistulaDokument2 SeitenEc Fistulasachn doshiNoch keine Bewertungen
- SplitPDFFile 801 To 1000Dokument200 SeitenSplitPDFFile 801 To 1000Shafan ShajahanNoch keine Bewertungen
- Choledochal Cyst: SymposiumDokument3 SeitenCholedochal Cyst: SymposiumRegi Anastasya MangiriNoch keine Bewertungen
- Kevin Ooi and Shing W Wong: IdemiologyDokument16 SeitenKevin Ooi and Shing W Wong: IdemiologyIbrar KhanNoch keine Bewertungen
- Obstructive Jaundice A Clinical StudyDokument7 SeitenObstructive Jaundice A Clinical StudyAnisah Maryam DianahNoch keine Bewertungen
- Gastrointestinal MCQDokument25 SeitenGastrointestinal MCQLương Thế Đoàn100% (2)
- in The Workup On A Patient For Possible Appendicitis, CT Scanning Should Be PerformedDokument9 Seitenin The Workup On A Patient For Possible Appendicitis, CT Scanning Should Be PerformedDr-Mohammad Ali-Fayiz Al TamimiNoch keine Bewertungen
- NEET SS January 2022 MCh GI Surgery RecallDokument58 SeitenNEET SS January 2022 MCh GI Surgery RecallRajhan 410Noch keine Bewertungen
- ColorectalDokument69 SeitenColorectalOstazNoch keine Bewertungen
- Surgery-6th-Year-2016 MCQSDokument26 SeitenSurgery-6th-Year-2016 MCQSAbdullah Matar BadranNoch keine Bewertungen
- 2 Gastric and Duodenal Peptic Ulcer Disease 2Dokument35 Seiten2 Gastric and Duodenal Peptic Ulcer Disease 2rayNoch keine Bewertungen
- Colonic DiseasesDokument28 SeitenColonic DiseasesMICHAEL SAKALANoch keine Bewertungen
- General Surgery Board RevieDokument69 SeitenGeneral Surgery Board RevieFadi Alkhassawneh88% (8)
- IntestineDokument31 SeitenIntestineMohamed SolimanNoch keine Bewertungen
- Esophagus Surgery Part 3A ReviewDokument8 SeitenEsophagus Surgery Part 3A ReviewJam JamaNoch keine Bewertungen
- 6 13Dokument3 Seiten6 13Shawn Gaurav JhaNoch keine Bewertungen
- Enfermedad Ácido-PépticaDokument10 SeitenEnfermedad Ácido-PépticaDoris Santiago FloresNoch keine Bewertungen
- San Pablo Colleges Medical Center case presentation on cholelithiasisDokument43 SeitenSan Pablo Colleges Medical Center case presentation on cholelithiasisMary Rose LinatocNoch keine Bewertungen
- Surgical Management For Gastric Ulcer PerforationDokument48 SeitenSurgical Management For Gastric Ulcer PerforationFauziaNoch keine Bewertungen
- Radiology 2Dokument15 SeitenRadiology 2Muhammed lotfiNoch keine Bewertungen
- Peptic and Other Benign UlcersDokument31 SeitenPeptic and Other Benign Ulcersmomi311Noch keine Bewertungen
- 1Dr - Mamoun JamousDokument258 Seiten1Dr - Mamoun JamousMohammad BanisalmanNoch keine Bewertungen
- Absite Master PileDokument23 SeitenAbsite Master PileJames JosephNoch keine Bewertungen
- AntrectomyDokument15 SeitenAntrectomyOhana S.Noch keine Bewertungen
- Best operative approach for choledochal cyst MCQ quizDokument19 SeitenBest operative approach for choledochal cyst MCQ quizKarem MaaliNoch keine Bewertungen
- Billroth I & II Procedure GuideDokument5 SeitenBillroth I & II Procedure GuideRoxieparkerNoch keine Bewertungen
- Key WordsDokument28 SeitenKey WordsChriz CoolNoch keine Bewertungen
- Mcqs Mock Exams For General Surgery Board ExamDokument7 SeitenMcqs Mock Exams For General Surgery Board ExamSergiu CiobanuNoch keine Bewertungen
- C. A Patient Who Withdraw Normally, But Can't Localize A Painful Stimuli, Has A Score of 5 On Motor Response Part of Glasgow Coma ScaleDokument13 SeitenC. A Patient Who Withdraw Normally, But Can't Localize A Painful Stimuli, Has A Score of 5 On Motor Response Part of Glasgow Coma ScaleDr-Mohammad Ali-Fayiz Al TamimiNoch keine Bewertungen
- P2 F2019Dokument9 SeitenP2 F2019marwaNoch keine Bewertungen
- 1 Surgery McqsDokument29 Seiten1 Surgery McqsSherlockHolmesSez50% (6)
- Colo Rectal CarcinomaDokument10 SeitenColo Rectal CarcinomaA.R. MendozaNoch keine Bewertungen
- Abdominal X-Rays PT 1Dokument20 SeitenAbdominal X-Rays PT 1sb medexNoch keine Bewertungen
- Behind The Knife’s Quick Hits for Anesthesia and SurgeryDokument19 SeitenBehind The Knife’s Quick Hits for Anesthesia and SurgeryMujahed LaswiNoch keine Bewertungen
- Behind The Knife’s Quick Hits for Anesthesia and SurgeryDokument24 SeitenBehind The Knife’s Quick Hits for Anesthesia and Surgerycusom34Noch keine Bewertungen
- Syrgery Mock 10Dokument8 SeitenSyrgery Mock 10Sergiu CiobanuNoch keine Bewertungen
- Syrgery Mock 10Dokument8 SeitenSyrgery Mock 10Sergiu CiobanuNoch keine Bewertungen
- Biliary Diseases: Dr. Wu Yang Dept. of Surgery The First Affiliated Hospital of Zhengzhou UniversityDokument42 SeitenBiliary Diseases: Dr. Wu Yang Dept. of Surgery The First Affiliated Hospital of Zhengzhou Universityapi-19916399Noch keine Bewertungen
- Jipmer 2013Dokument7 SeitenJipmer 2013revanth kallaNoch keine Bewertungen
- Acute Gyn 2 MCQDokument6 SeitenAcute Gyn 2 MCQzoya virjiNoch keine Bewertungen
- Surgery 2 PDFDokument93 SeitenSurgery 2 PDFBALAJI GKRRNoch keine Bewertungen
- Please Read Carefully and Choose The Best Answer:: A. TraumaDokument18 SeitenPlease Read Carefully and Choose The Best Answer:: A. Traumamotasem alsharifNoch keine Bewertungen
- Laryngeal CarcinomaDokument52 SeitenLaryngeal CarcinomaEjay Jacob Ricamara67% (3)
- DR Ashraf Gift To DR AlvaroDokument16 SeitenDR Ashraf Gift To DR AlvaroAhmed Saleh100% (1)
- Hematuria in AdultsDokument9 SeitenHematuria in AdultsTheddyon BhenlieNoch keine Bewertungen
- Guide to evaluating hematuria in adultsDokument9 SeitenGuide to evaluating hematuria in adultsTheddyon BhenlieNoch keine Bewertungen
- Absite 21 Answers - StomachDokument2 SeitenAbsite 21 Answers - Stomachsiriopa08Noch keine Bewertungen
- Obstructive Jaundice: Dr. SrinivasDokument52 SeitenObstructive Jaundice: Dr. SrinivasSahir100% (1)
- Choledocholithiasis ManagementDokument20 SeitenCholedocholithiasis ManagementNikoFebriRyandoNoch keine Bewertungen
- Multiple Choice Questions in Paediatric SurgeryVon EverandMultiple Choice Questions in Paediatric SurgeryBewertung: 1 von 5 Sternen1/5 (1)
- Colorectal Cancer: Diagnosis and Clinical ManagementVon EverandColorectal Cancer: Diagnosis and Clinical ManagementJohn H. ScholefieldNoch keine Bewertungen
- The Ileoanal Pouch: A Practical Guide for Surgery, Management and TroubleshootingVon EverandThe Ileoanal Pouch: A Practical Guide for Surgery, Management and TroubleshootingJanindra WarusavitarneNoch keine Bewertungen
- Carcinoid Syndrome, A Simple Guide To The Condition, Treatment And Related DiseasesVon EverandCarcinoid Syndrome, A Simple Guide To The Condition, Treatment And Related DiseasesNoch keine Bewertungen
- Fundamentals of Colitis: Pergamon International Library of Science, Technology, Engineering and Social StudiesVon EverandFundamentals of Colitis: Pergamon International Library of Science, Technology, Engineering and Social StudiesNoch keine Bewertungen
- Colorectal Surgery: Clinical Care and ManagementVon EverandColorectal Surgery: Clinical Care and ManagementBruce GeorgeNoch keine Bewertungen
- Complete Muscle ActionDokument11 SeitenComplete Muscle ActionkapczukNoch keine Bewertungen
- Mms For Household Uses-S.pardee-1Dokument7 SeitenMms For Household Uses-S.pardee-1Manny JorgeNoch keine Bewertungen
- Gamper (2013) Bad Ragaz (ECEBAT)Dokument14 SeitenGamper (2013) Bad Ragaz (ECEBAT)Blajiu BeatriceNoch keine Bewertungen
- Anti-Doping Presentation: A Resource For Cgas To Present To Athletes and Team OfficialsDokument20 SeitenAnti-Doping Presentation: A Resource For Cgas To Present To Athletes and Team OfficialsAjay Pal NattNoch keine Bewertungen
- Effect of Xylazine and Ketamine On Pulse Rate, Respiratory Rate and Body Temperature in DogDokument3 SeitenEffect of Xylazine and Ketamine On Pulse Rate, Respiratory Rate and Body Temperature in DogPrimyntNoch keine Bewertungen
- Local Anesthesia in Pediatric Dentistry Lecture Students 2009 MDokument88 SeitenLocal Anesthesia in Pediatric Dentistry Lecture Students 2009 MIoana DănilăNoch keine Bewertungen
- ENT Question PaperDokument12 SeitenENT Question Paperasokk40% (5)
- C C C C C C Is A Sudden Inflammation of The Gastric or Stomach Mucosa. It IsDokument4 SeitenC C C C C C Is A Sudden Inflammation of The Gastric or Stomach Mucosa. It IsAngelica LykaNoch keine Bewertungen
- SPOSI Final Members List 2015Dokument58 SeitenSPOSI Final Members List 2015Mukesh KumarNoch keine Bewertungen
- Disorders of The Thyroid Gland Harrison's Principles of Internal Medicine, 19eDokument21 SeitenDisorders of The Thyroid Gland Harrison's Principles of Internal Medicine, 19ePeterNoch keine Bewertungen
- Stress Management HandoutDokument8 SeitenStress Management HandoutBlasius DsouzaNoch keine Bewertungen
- Info Iec60479-1 (Ed4.0) BDokument23 SeitenInfo Iec60479-1 (Ed4.0) BHongNoch keine Bewertungen
- Adventure Therapy TimelineDokument2 SeitenAdventure Therapy TimelineChristine SherwoodNoch keine Bewertungen
- Pediatric Rehabilitation: Cerebral PalsyDokument133 SeitenPediatric Rehabilitation: Cerebral PalsyAlfredson Busto Ramirez100% (1)
- A A A A C C C C A A A A D D D D Eeee M M M M IIII C C C C S S S S C C C C IIII Eeee N N N N C C C C Eeee S S S SDokument3 SeitenA A A A C C C C A A A A D D D D Eeee M M M M IIII C C C C S S S S C C C C IIII Eeee N N N N C C C C Eeee S S S SnelisaNoch keine Bewertungen
- How To Start A Homestead No Matter Where You LiveDokument41 SeitenHow To Start A Homestead No Matter Where You LiveAndrea MarendaNoch keine Bewertungen
- 02-Clinical Study Leaflet FinalDokument4 Seiten02-Clinical Study Leaflet FinalFakeGNoch keine Bewertungen
- Renal Blood Flow and Glomerular Filtration Rate (GFRDokument23 SeitenRenal Blood Flow and Glomerular Filtration Rate (GFRRudinNoch keine Bewertungen
- Lesson Plan On PEMDokument5 SeitenLesson Plan On PEMgk57% (7)
- Laying Out Arnold Palmer HospitalDokument2 SeitenLaying Out Arnold Palmer HospitalazilaNoch keine Bewertungen
- 3) Buku Log Clinical Practice Record PERIOPERATIVE CAREDokument41 Seiten3) Buku Log Clinical Practice Record PERIOPERATIVE CAREAslam AssandakaniNoch keine Bewertungen
- Supra Ventricular Tachycardia in PregnancyDokument2 SeitenSupra Ventricular Tachycardia in PregnancylulzimkamberiNoch keine Bewertungen
- Hematology of RatDokument4 SeitenHematology of RatTunde LamidiNoch keine Bewertungen
- New Hospivac 350 VAC 350 V: Suction UnitsDokument2 SeitenNew Hospivac 350 VAC 350 V: Suction UnitsWidad Mardin Mas JayaNoch keine Bewertungen
- Sequelae of Injury To Anterior Teeth II PedoDokument40 SeitenSequelae of Injury To Anterior Teeth II PedoFourthMolar.comNoch keine Bewertungen
- Extractables and Leachables Testing Services - Vimta Labs Ltd.Dokument10 SeitenExtractables and Leachables Testing Services - Vimta Labs Ltd.Vimta Labs LtdNoch keine Bewertungen
- Stigma of HGDokument8 SeitenStigma of HGHarnila JaNoch keine Bewertungen
- HOSPITAL LISTINGDokument12 SeitenHOSPITAL LISTINGSiddharth KumarNoch keine Bewertungen
- Clinical Characteristics of Vaginitis and Effectiveness of Fenticonazole - An Observational Study From IndiaDokument8 SeitenClinical Characteristics of Vaginitis and Effectiveness of Fenticonazole - An Observational Study From IndiaEditor ERWEJNoch keine Bewertungen
- The KT/V by Ionic Dialysance: Interpretation Limits: Original ArticleDokument7 SeitenThe KT/V by Ionic Dialysance: Interpretation Limits: Original Articleahmed AlayoudNoch keine Bewertungen