Beruflich Dokumente
Kultur Dokumente
040 - Bone Histology
Hochgeladen von
charlieholdenOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
040 - Bone Histology
Hochgeladen von
charlieholdenCopyright:
Verfügbare Formate
1. 2. 3. 4.
Milk teeth that are already erupted, or in the process of eruption Unerupted adult teeth at an early stage of formation Gingiva (gum) Alveolar bone of jaw
Gum and alveolar bone, kitten jaw 1. Gum - thick stratified squamous epithelium, with keratinized surface layer 2. Underlying dermal / connective tissue layer; highly cellular, containing numerous blood vessels 3. Alveolar bone; black arrowheads indicate surfaces where active bone formation by osteoblasts (layer of small dark purple cells) is occurring The bone matrix itself is stained pink.
The micrograph illustrates the dynamic cellular activity in this immature bone: The lower margin of the alveolar bone is being eroded by osteoclasts, the specialised multinucleate bone-resorbing cells (black arrows) to make way for the erupting tooth. Close by, however, bone is being deposited by rows of osteoblasts, the specialised bone-forming cells (white arrows), on surfaces facing away from the tooth. These dramatic cellular events probably occur as a result of upward pressure from the erupting tooth; similar events occur when orthodontists use the constant pressure provided by tooth braces to move teeth through the aveolar bone of juvenile or adult jaws.
This rapidly changing, immature bone is known as "woven bone"; it is widely distributed in growing animals (and humans!) and also occurs in the fracture callus that knits together broken bones in adults. This type of bone is essentially temporary; it is replaced eventually by lamellar bone, the adult form of bone.
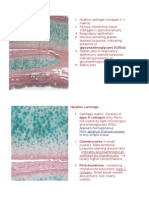
This is woven bone (rapidly produced, temporary bone) o Note the lack of internal structure to this woven bone matrix, and the haphazard arrangement of osteocytes embedded in it (which are large & round) Contrast with the micrographs of lamellar bone
1. Concave resorption pits (Howships lacunae) in bone matrix, excavated by large, multinucleated osteoclasts (stained purple) 2. Row of osteoblasts laying down new bone matrix (called "osteoid"). o The newly synthesised matrix essentially consists of tangle type 1 collage fibres o Osteoid is initially unmineralised (narrow, pale layer between cells and pink-stained matrix) 3. Some osteoblasts become buried in the accumulating bone matrix they are synthesising and differentiate into osteocytes; o Form an interconnecting network (of canaliculi), and are present throughout all living bone 4. Many small blood vessels are present in the stroma around the bone; osteoblast and osteoclast precursor cells are also present here.
1. 2. 3. 4.
Demineralised section of entire adult human finger bone N.B. There are no epiphyseal growth plates present in adult bone! Cortical bone (aka compact bone) Articular cartilage Tendon Marrow cavity, with bony trabeculae at epiphyses (subchondral bone at the end of the long bones is always trabecular)
1. Articular cartilage (hyaline cartilage) 2. Trabecular bone 3. Marrow cavity, mainly filled with adipocytes
1. Lamellar cortical bone. This apperance is the result of successive regular layers of bone matrix being deposited such that the orientation of the type 1 collagen fibres is different in each layer. The arrangement is analagous to plywood, and confers great strength / fracture resistance to the bone. Osteocytes (white arrowheads) tend to be sparesely & regularly distributed in adult bone (they are small and flattened)
2. Fibrous periosteum - containing type 1 collagen fibres (unmineralised), fibroblasts, osteoblast precursors, etc. 3. Marrow containing adipocytes and a few haemopoietic cells. High power view of periosteal surface, showing remodelling activity 1. Cavity (filled with small cells) excavated by large osteoclast o Multinucleated osteoclast (delineated by small white arrowheads)
Articular cartilage and subchondral bone 1. Matrix of articular (hyaline) cartilage (smooth articular surface indicated by black arrows) 2. Mineralised articular cartilage 3. Subchondral trabecular bone, surrounded mainly by adipocytes, with a few haemopoietic cells. With advancing age, the amount of yellow fatty marrow increases in adult bone.
Articular cartilage and subchondral bone This image illustrates very clearly the transition from unmineralised articular cartilage to mineralised articular cartilage to bone The wavy line separating mineralised from unmineralised cartilage is known as the "tidemark zone"; this advances towards the articular surface with increasing age. 1. Matrix of unmineralised articular (hyaline) cartilage 2. Matrix of mineralised articular (hyaline) cartilage 3. Matrix of subchondral bone - note typical adult lamellar structure Chondrocytes, arranged in small clusters, in both unmineralised and mineralised cartilage Osteocytes in bone
Periosteal surface of adult bone 1. Blood vessel channels (contrast with avascular cartilage) 2. Periosteal bone apposition - note layer of osteoblasts which lines the bone (underneath arrowheads) 3. Lamellar cortical bone 4. Fibrous periosteum 5. Complex of blood vessels (with nerves?) in mixed fibrous / fatty connective tissue Transverse section of cortical bone from human finger Note this is cortical bine so must be the diaphysis of the finger (the epiphysis would instead show trabecular subchondral bone). The bone was not demineralised or stained The section clearly illustrates the complex (Haversian) remodelling activity in adult cortical bone. Cortical bone consists of longditudinal units osteons (Haversian) Each osteon consists of concentric lamellae surrounding a central blood vessel 1,2,3,4: Osteonal (Haversian) systems. Some of the channels have blood residues present (blood vessels run in the centre of these channels). Systems 1 and 2 can be seen to be partly obliterating systems 3 and 4 - the result of remodelling. Therefore systems 1 and 2 are more recent - evidenced also by their larger lumens - not yet fully filled with concentric bone layers.
The white arrowheads the spaced osteocytes
indicate regularly that
interconnect with each other (black, spidery projections) and ramify throughout living bone This network of cells enables contact between the central blood vessel channel and other part of the osteon. It is thought that this arrangement may function in sensing & responding to mechanical strain. (Contrast with chondrocytes in cartilage which do not interconnect)
Osteoporosis:
Left: Low power scanning electron microscope image showing a sawn section down through the body of the third lumbar vertebra of a normal 30 year-old woman. Vertebral body = trabecular bone The marrow has been removed and no cells are visible - only the "naked" bone surfaces. Thick, regular, interconnecting plates of trabecular bone are evident. In engineering terms, this is a strong, rigid structure that can withstand the stresses and strains encountered in normal life. Right: Low power scanning electron microscope image of a sawn section through the body of the third lumbar vertebra of a 71 year-old woman. Osteoporosis is evident in this image. Contrast with the bone from the 30 year old: the thick, interconnecting plates of trabecular bone have been eroded to thin, spindly rods in the 71 year old. This is a mechanically inadequate structure that could fracture with minimal trauma (eg sitting down with a bump). Spinal osteoporosis leads to compression fractures, height loss and the classic "dowager's hump" often seen in elderly women. Osteoporotic bone: The severe erosion of the vertical bone rod in the foreground can be seen to have resulted from osteoclastic action - the surface is covered with resorption pits.
If this process had continued, this trabecular element would have been lost completely. Most osteoporosis is thought to result from osteoclast over-activity (osteoclastic resorbtion > osteoblastic formation) The swelling at the top of the vertical bone rod could possibly be part of a microfracture callus from an earlier trauma. SELF ASSESMENT QUIZ
7) Resting line: between newly formed bone, and older, resting bone.
1) Youngest 2) Middle 3) Oldest 4) = Haversian canal
1) Osteocyte 2) Canaliculi
3) Lamellae
YOUNGER Haversian osteons of cortical tissue: Have larger central lumens Are obliterating older osteons.
CORE KNOWLEDGE
Give brief explanations of the following terms (a few words only for each): (a) osteoblast bone-forming cell (b)osteocyte ex-osteoblast embedded in matrix -communication via canaliculi (c) osteoclast bone-resorbing (destroying) cell, usually multinucleate (d)osteoid newly deposited, unmineralised bone matrix (e) lamellar bone highly organised bone, deposited in discrete layers, each with differing collagen fibre orientation (like plywood) (f) woven bone rapidly produced, immature bone with random collagen fibre organisation; replaced by lamellar bone (g)trabecular (cancellous) bone 3-d meshwork of bone; open, sponge-like arrangement (but not soft!), eg in vertebral
bodies, ends of long bones (h)cortical bone dense bone, eg in shafts of long bones (i) Haversian system (osteon) concentric layers of bone around a blood vessel (bulk of cortical bone) -run parallel to long axis of bone (j) bone remodelling co-ordinated activity of osteoclasts and osteoblasts to replace or modify areas of bone that might be damaged, redundant or weak 2. What is intramembranous ossification? (see CORE KNOWLEDGE: CARTILAGE for comparison with endochondral ossification) Intramembranous ossification: de novo bone formation by osteoblasts -eg mandible and vault of skull 3. Describe the key structural components of bone matrix Organic component: type 1 collagen fibres (>90%); balance is mixture of small proteins including osteocalcin, osteopontin, osteonectin, plus growth factors including TGF, IGFs. Inorganic component: hydroxyapatite -Ca10(PO4)6(OH)2 4. What is osteoporosis? Who gets it and why? Bone loss due to imbalance of resorption/formation; remaining bone normal but mechanically inadequate fractures. Seen at high turnover sites (trabecular bone) -vertebrae & femoral neck. Age-related, common in post-menopausal women (<50% suffer in UK). Main causes oestrogen deficiency + declining mechanical stimulation (ie exercise). 5. Briefly describe two other bone diseases Rickets / osteomalacia: osteoid fails to mineralise due to vitamin D deficiency bendy bones deformity Paget's disease: many large, over-active osteoclasts (? viral cause) rapid, uncontrolled bone remodelling deformity.
6. Which hormones are thought to be important in regulating bone turnover? Parathyroid hormone (PTH) - turnover 1,25-dihydroxyvitamin D - turnover (calcitonin) - OC activity gonadal steroids: estrogens, androgens
Das könnte Ihnen auch gefallen
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (587)
- 009 - Reproductive HistologyDokument10 Seiten009 - Reproductive HistologycharlieholdenNoch keine Bewertungen
- 044 - Bone DisordersDokument7 Seiten044 - Bone DisorderscharlieholdenNoch keine Bewertungen
- 20 - Histology of The Nervous SystemDokument6 Seiten20 - Histology of The Nervous SystemcharlieholdenNoch keine Bewertungen
- 016 - Skeletal Muscle HistologyDokument4 Seiten016 - Skeletal Muscle HistologycharlieholdenNoch keine Bewertungen
- 005 - Cartilage HistologyDokument13 Seiten005 - Cartilage HistologycharlieholdenNoch keine Bewertungen
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (73)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (119)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- 6/27/2019 NO NAMA BARANG QTY UOM Batch EDDokument8 Seiten6/27/2019 NO NAMA BARANG QTY UOM Batch EDRedCazorlaNoch keine Bewertungen
- HouseflyDokument16 SeitenHouseflyRitu Puri50% (2)
- Angels Bridging Angels Bridging Angels Bridging Angels Bridging Gaps Gaps Gaps GapsDokument13 SeitenAngels Bridging Angels Bridging Angels Bridging Angels Bridging Gaps Gaps Gaps Gapsapi-251664135Noch keine Bewertungen
- Sefcik Ashley Resume 2018Dokument1 SeiteSefcik Ashley Resume 2018api-394215168Noch keine Bewertungen
- Student study on family health and pregnancy in rural ZimbabweDokument3 SeitenStudent study on family health and pregnancy in rural ZimbabweTubocurareNoch keine Bewertungen
- Eyelid Eversion and Inversion Causes and TreatmentsDokument17 SeitenEyelid Eversion and Inversion Causes and TreatmentsmanognaaaaNoch keine Bewertungen
- Geriatric Nursing MidtermDokument67 SeitenGeriatric Nursing MidtermMadeline N. Gerzon100% (2)
- Efficacy of Transpalatal Arch As An Anchorage Rein PDFDokument7 SeitenEfficacy of Transpalatal Arch As An Anchorage Rein PDFOana CostanNoch keine Bewertungen
- HAADStatisticsEng2013 PDFDokument91 SeitenHAADStatisticsEng2013 PDFHitesh MotwaniiNoch keine Bewertungen
- Resume 101: Write A Resume That Gets You NoticedDokument16 SeitenResume 101: Write A Resume That Gets You Noticedgqu3Noch keine Bewertungen
- Reflection Paper-Culture, Spirituality, and InstitutionsDokument4 SeitenReflection Paper-Culture, Spirituality, and Institutionsapi-359979131Noch keine Bewertungen
- ANATOMY AND PHYSIOLOGY of RabiesDokument5 SeitenANATOMY AND PHYSIOLOGY of RabiesDavid CalaloNoch keine Bewertungen
- Bls - Fbao - First AidDokument172 SeitenBls - Fbao - First AidMaria Regina Castro Gabriel100% (1)
- Functional Foods and Nutraceuticals-ModeDokument18 SeitenFunctional Foods and Nutraceuticals-ModediahNoch keine Bewertungen
- PMLS ReviewerDokument26 SeitenPMLS ReviewerEkoy TheRealNoch keine Bewertungen
- Science Chapter on ReproductionDokument4 SeitenScience Chapter on ReproductionAnita GargNoch keine Bewertungen
- Respiratory Physiology AnswersDokument4 SeitenRespiratory Physiology AnswersRamya100% (2)
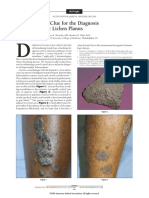
- A Novel Visual Clue For The Diagnosis of Hypertrophic Lichen PlanusDokument1 SeiteA Novel Visual Clue For The Diagnosis of Hypertrophic Lichen Planus600WPMPONoch keine Bewertungen
- Group 9 - Dental FluorosisDokument37 SeitenGroup 9 - Dental Fluorosis2050586Noch keine Bewertungen
- Chapter 6 DiscussionDokument3 SeitenChapter 6 DiscussionyughaNoch keine Bewertungen
- A Client With A Brain Tumor: Nursing Care PlanDokument1 SeiteA Client With A Brain Tumor: Nursing Care Planshabatat2002Noch keine Bewertungen
- Effects of Pulmonary Rehabilitation On Physiologic and Psychosocial Outcomes in Patients With Chronic Obstructive Pulmonary DiseaseDokument10 SeitenEffects of Pulmonary Rehabilitation On Physiologic and Psychosocial Outcomes in Patients With Chronic Obstructive Pulmonary DiseaseElita Urrutia CarrilloNoch keine Bewertungen
- Aghamohammadi Et Al 2016 WEB OF SCIENCE Integrative Cancer TherapiesDokument9 SeitenAghamohammadi Et Al 2016 WEB OF SCIENCE Integrative Cancer Therapiesemmanuelle leal capelliniNoch keine Bewertungen
- Reading ComprehensionDokument42 SeitenReading Comprehension14markianneNoch keine Bewertungen
- Martial Arts SecretsDokument4 SeitenMartial Arts SecretsGustavoRodriguesNoch keine Bewertungen
- Dengulata KosamDokument3 SeitenDengulata KosamChina SaidaNoch keine Bewertungen
- PR Menarini PDX Ab RBCDokument2 SeitenPR Menarini PDX Ab RBCvyasakandarpNoch keine Bewertungen
- Fin e 222 2018Dokument143 SeitenFin e 222 2018Gnana SekarNoch keine Bewertungen
- UrinalysisDokument43 SeitenUrinalysisJames Knowell75% (4)
- Chapter Three Research Methodology Study DesignDokument3 SeitenChapter Three Research Methodology Study Designotis2ke9588Noch keine Bewertungen