Beruflich Dokumente
Kultur Dokumente
Head Injury and Intracranial Hypertension
Hochgeladen von
mangsiatOriginaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Head Injury and Intracranial Hypertension
Hochgeladen von
mangsiatCopyright:
Verfügbare Formate
UTHSCSA
Pediatric Resident Curriculum for the PICU
HEAD INJURY AND INTRACRANIAL HYPERTENSIO
Pediatric Resident Curriculum for the PICU
HEAD INJURY
Major cause of morbidity and mortality in children Leading cause of death in children > 1 yr is trauma Head injuries responsible for most trauma deaths Adverse outcomes result from Primary injury Result of mechanical forces producing tissue deformation at the moment of injury Secondary ischemic injury Associated with post injury hypotension, hypoxemia, and intracranial hypertension
UTHSCSA
Pediatric Resident Curriculum for the PICU
ETIOLOGIES
Motor vehicle accidents Responsible for most severe head injuries Falls Usually in children < 4 yrs and usually mild Recreational activities Half of these are bicycle accidents Assault or nonaccidental trauma Most head injuries in kids < 1 yr are from NAT and falls
UTHSCSA
Pediatric Resident Curriculum for the PICU
ANATOMY
Uniquely susceptible to injury Brain Inelastic and noncompressible Has no internal support Cranium Rigid and unyielding after sutures fused Bony buttresses at anterior poles and temporal poles Membranous slings Falx cerebri compartmentalizes R and L hemispheres Tentorium separates infra- and supratentorial regions
UTHSCSA
Pediatric Resident Curriculum for the PICU
MECHANISM OF BRAIN INJURY
Brain is thrown against bony irregularities or membranous slings or compressed against these surfaces by Contact injury Head strikes or is struck by an object Acceleration/deceleration injury Violent head motion causes compressive, tensile, and shear strain in brain tissue
UTHSCSA
Pediatric Resident Curriculum for the PICU
COUP - CONTRECOUP INJURY
UTHSCSA
LifeArt: Williams & Wilkins http://www.lifeart.com
Pediatric Resident Curriculum for the PICU
TYPES OF PRIMARY INJURIES
Focal injuries Diffuse injuries Skull fracture Diffuse axonal Parenchymal injury contusion Diffuse vascular Parenchymal injury laceration Vascular injury resulting in hematoma (subdural, extradural, or parenchymal)
UTHSCSA
Pediatric Resident Curriculum for the PICU
SKULL FRACTURES
Most are uncomplicated Basilar skull fractures
Battles sign, raccoon eyes CSF rhinorrhea, CSF otorrhea possible Cranial nerve injury possible
Depressed skull fractures represent more severe injury
1/3 are associated with dural laceration 1/3 are associated with cortical laceration May require surgical elevation
UTHSCSA
Fracture crossing path of major vascular structure increases risk for significant bleeding
Middle meningeal artery Large dural sinus
Pediatric Resident Curriculum for the PICU
CONTUSION
Usually frontal or temporal lobe Small cortical vessels and neural tissue damaged Damaged vessels may thombose, leading to ischemia
UTHSCSA
WebPath: University of Utah http://www-medlib.med.utah.edu/WebPath/webpath.html
Pediatric Resident Curriculum for the PICU
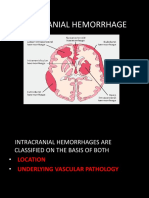
INTRACEREBRAL HEMORRHAGE
Usually frontal or temporal lobe Can be bilateral (contracoup injury) Can act as mass lesions and cause intracranial hypertension
UTHSCSA
Pediatric Resident Curriculum for the PICU
EPIDURAL HEMATOMA
Usually arterial in origin Between skull and dura, limited by suture lines Often from tear in middle meningeal artery Initial injury may seem minor, followed by lucid interval, then neurologic deterioration May expand rapidly and require emergency craniotomy
WebPath: University of Utah http://www-medlib.med.utah.edu/WebPath/webpath.html
UTHSCSA
Pediatric Resident Curriculum for the PICU
SUBDURAL HEMATOMA
Usually venous bleeding (bridging veins) On surface of cortex, beneath dura and outside arachnoid, not limited by suture lines. Typically requires greater force to produce than epidural hematoma Usually associated with severe parenchymal injury
WebPath: University of Utah http://www-medlib.med.utah.edu/WebPath/webpath.html
UTHSCSA
Pediatric Resident Curriculum for the PICU
. ...... . ..
DIFFUSE BRAIN INJURY
Diffuse axonal injury Usually from rapid acceleration/deceleration Shear forces disrupt small axonal pathways
After disruption, axons degenerate, fragment, then disappear The neurons then undergo Wallerian degeneration
Spectrum from mild to severe Diffuse vascular injury Microvasculature more resistant to shear than axons Results in multiple small hemorrhages throughout brain Usually seen in fatal head injuries
UTHSCSA
Pediatric Resident Curriculum for the PICU
SECONDARY ISCHEMIC BRAIN INJURY
Compounds the potential for adverse neurologic outcome Caused by: Post injury hypotension Hypoxemia Intracranial hypertension which impairs cerebral blood flow
UTHSCSA
Pediatric Resident Curriculum for the PICU
INTRACRANIAL HYPERTENSION
Vascular etiologies Vasogenic edema
BBB impaired, protein rich fluid leaks to ECF
Nonvascular etiologies Cytotoxic edema
Ionic gradients impaired and cells swell
Hyperemia
Occurs days 1 to 3 after injury
UTHSCSA
Obstructed venous drainage
Hydrostatic pressure increased, protein poor fluid leaks into ECF
Obstruction to CSF outflow Hematoma Osmotic brain edema
Decreased osmolality from iatrogenic hemodilution or SIADH
Pediatric Resident Curriculum for the PICU
INTRACRANIAL HYPERTENSION
Normal intracranial pressure:
Adults: < 10 mm Hg Infants/children: somewhat lower, depending on age
Elevated ICP impairs cerebral perfusion Risk for herniation with ICP > 40 mm Hg Herniation can occur at lower ICPs when mass lesion is present
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF HEAD INJURY
Goals of resuscitation and treatment is to minimize secondary ischemic brain injury by promoting and preserving cerebral perfusion
Prevent or treat post injury hypotension Prevent or treat hypoxemia and reduce oxygen demand of the brain Prevent or treat intracranial hypertension Avoid measures that decrease cerebral perfusion
UTHSCSA
Pediatric Resident Curriculum for the PICU
RESUSCITATION
A, B,Cs Major early risk is hypotension
Adequate fluid resuscitation to restore normal BP does NOT worsen neurologic outcome Avoid hypotonic fluids
Emergent airway control for
GCS 8 or less GSC 10 or less with abnormal head CT Rapid neurologic deterioration If needed for other injuries
UTHSCSA
Pediatric Resident Curriculum for the PICU
INTUBATION OF PATIENT WITH HEAD INJURY
Preserve cerebral oxygenation Maintain cerebral perfusion
Adequate analgesia and anxiolysis Avoid meds that increase ICP Avoid meds that cause hypotension Avoid Trendelenburg position
Avoid aggravating C spine injury
C-spine injuries in as many as 10% of head injury patients In-line axial stabilization by an assistant recommended
UTHSCSA
Pediatric Resident Curriculum for the PICU
DRUGS FOR RAPID SEQUENCE INTUBATION
Analgesia/sedation Neuromuscular blockade Fentanyl, etomidate Succinyl choline little effect on BP short acting Thiopental muscle fasciculations can decreases ICP but increase ICP can drop BP use with Anxiolysis defasciculating Midazolam dose of little effect on BP nondepolarizing Lidocaine IV Non depolarizing blunts vecuronium sympathetic longer acting and response to no increase in ICP intubation
UTHSCSA
Pediatric Resident Curriculum for the PICU
RULE OUT & PREVENT NEUROSURGICAL EMERGENCIES
Head CT as soon as possible Initial CT may be normal in severe head injury Repeat CT in 12 to 24 hours Moderate hyperventilation advisable during transport and initial evaluation If signs of impending herniation develop (lateralizing signs, pupil asymmetry) Hyperventilate Give mannitol
UTHSCSA
Pediatric Resident Curriculum for the PICU
MONITORING OF INTRACRANIAL PRESSURE
Ventriculostomy catheter Catheter tip in frontal horn of lateral ventricle Can drain CSF Can be recalibrated as necessary Transducer tipped catheter Intraparenchymal or subdural Cannot drain CSF Cannot be recalibrated Exhibits drift in values measured over time
UTHSCSA
Pediatric Resident Curriculum for the PICU
MONITORING OF INTRACRANIAL PRESSURE
Indications
GCS < 8 after resuscitation Abnormal head CT Rapid neurologic deterioration
UTHSCSA
ICP monitoring is continued for as long as treatment of intracranial hypertension is required
Pediatric Resident Curriculum for the PICU
CEREBRAL PERFUSION PRESSURE
Can be determined from ICP and mean arterial pressure: CPP = MAP - ICP Calculated CPP does not reflect perfusion of entire brain CPP further decreased in areas of injury Factors that cause cerebral vasoconstriction without lowering MAP result in a falsely low calculated CPP
UTHSCSA
Pediatric Resident Curriculum for the PICU
CEREBRAL PERFUSION PRESSURE
Goal of therapy
CPP > 60 mm Hg if ICP < 22 mm Hg or CPP > 70 mm Hg if ICP > 22 mm Hg Lowering ICP while maintaining MAP will increase CPP Increasing MAP will increase CPP
UTHSCSA
Pediatric Resident Curriculum for the PICU
FACTORS AFFECTING INTRACRANIAL PRESSURE
Increases ICP hypercarbia hypoxia (pO2 < 50) seizures or shivering hyperthermia arousal pain, anxiety venous congestion fluid overload intrathoracic Decreases ICP hyperoxia hypothermia barbiturates hypocapnia via cerebral vasoconstrictio n lowers CPP and is undesirable
UTHSCSA
Pediatric Resident Curriculum for the PICU
EFFECT OF pCO2 and pO2 ON CBF AND CPP
Hypoxia increases CBF by vasodilation Hypercapnia increases CBF Hyperventilation and resulting hypocapnia decrease CBF Hyperventilation is useful to prevent impending herniation but will worsen secondary ischemic injury
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Head position Head elevated 30 degrees and midline Sedation and pain control Analgesic + anxiolytic Fentanyl, morphine, or propofol plus a benzodiazepine Continuous infusions or scheduled doses to maintain sedation Watch for and treat hypotension Seizure prophylaxis Phenytoin or phosphenytoin
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Neuromuscular blockade Facilitates mechanical ventilation and control of pCO2 Prevents shivering Use if movement increases ICP Temperature control A rise in temp of 1o C increases cerebral metabolic rate by 10%, increasing ICP by several mm Hg Maintain temp < 37.5 o C
Scheduled acetaminophen, body exposure, cooling blanket
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Osmotherapy with mannitol Decreases extracellular fluid in brain Intermittent doses for ICP spikes or scheduled if elevated ICP is persistent Adverse effects:
Hypernatremia, hypokalemia Hyperosmolality Hemodilution and drop in hematocrit Hypotension
UTHSCSA
Follow serum osmolality and Na Hold mannitol if serum osm > 320 mOsm/l
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Drainage of CSF
Possible if ventricular catheter is in place CSF drainage pressure usually set at 20 cm H2O CSF drains when ICP exceeds drainage pressure Ventricular catheters cannot be placed if cerebral edema has obliterated or significantly compressed ventricles
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Second tier therapies for intracranial hypertension refractory to sedation, muscle relaxation, osmotherapy, and moderate hypothermia:
barbiturate coma induced hypertension decompressive craniotomy hypothermia
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Barbiturate coma ICP control is the principal endpoint EEG burst suppression is a useful guide to optimal barbiturate dosage
Pentobarbital 10mg/kg followed by infusion at 1 mg/kg/hr, titrated to effect May give additional boluses during infusion for acute spikes in ICP Moderate doses cause sluggishly reactive pupils while large doses may cause mid position to 5 mm nonreacting pupils Watch for hypotension
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Induced hypertension Inotropes to increase MAP, even beyond normal for age, to achieve an optimal CPP
Dopamine Norepineprine
Rise in ICP in tandem with a rise in MAP implies total loss of autoregulation and is a poor prognostic sign Decompressive craniotomy Large portion of cranium removed to allow room for brain to swell and minimize ischemia Dura must be opened as well
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF INCREASED ICP
Hypothermia Core body temp of 32o to 33o C Reduced cerebral metabolic activity, reducing ICP Also has cytoprotective effects Adverse effects Arrythmias Coagulopathies Hypokalemia Increased risk of infection
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Respiratory
Maintain normocapnia
Hyperventilation only appropriate during early diagnosis and management or if herniation is impending
Maintain oxygenation PEEP to maintain alveolar recruitment
ARDS, neurogenic pulmonary edema frequent complications Hypoxemia has more deleterious effects on brain than modest venous congestion caused by PEEP PEEP of 5 to 10 cm H2O not shown to have detrimental effect on neurologic outcome pO2 > 100 is optimal
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Cardiovascular Maintain normal blood pressure Hypotension significantly reduces CPP Inotropes if necessary to maintain normal BP Induced hypertension if necessary Gastrointestinal Stress gastritis prophylaxis with H2 blocker Jejunal feeds to maintain healthy intestinal mucosa and prevent bacterial translocation from gut
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Fluids, Electrolytes, Nutrition
Goal is NORMOVOLEMIA Total fluid intake should be @ 100% maintenance Bolus as necessary to achieve normal CVP Avoid hypotonic fluids Lactated Ringers and 0.9% saline w/ 20 mEq KCl/l are good choices for maintenance fluids Follow electrolytes closely Avoid hyponatremia Mannitol can cause electrolyte abnormalities Watch for SIADH, diabetes insipidus,
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Fluids, electrolytes, nutrition
Provide calories to meet metabolic demands of patient Increased metabolic demands during acute phase of injury Heavily sedated, relaxed, cooled patient has decreased metabolic demands Enteral feedings via nasojejunal catheter preferable to TPN if gut deemed to be healthy Avoid hyperglycemia Associated with poor neurologic outcome Watch serum glucose closely if dextrose containing fluids used
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Renal
Place foley for strict Is and Os
Hematologic
Coagulopathy common with head injuries Brain derived thromboplastin activator substances released Follow PT/PTT or DIC screens Blood component replacement if evidence of active bleeding or if surgical intervention anticipated Maintain normal hematocrit to optimize oxygen delivery
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Endocrine
DIABETES INSIPIDUS Complete or partial failure of ADH secretion from shearing of pituitary stalk Polyuria, hypernatremia, urine osm < plasma osm Treatment: Run maintenance fluids @ 100% Replace urine output cc for cc with dextrosecontaining fluids Continuous vasopressin infusion or DDAVP (subQ or intranasal) q 12 to 24 hrs
UTHSCSA
Pediatric Resident Curriculum for the PICU
MANAGEMENT OF OTHER SYSTEMS
Endocrine
CEREBRAL SALT-WASTING ANP-like substance released from brain, inducing natriuresis and diuresis SIADH Elevated level of ADH inappropriate for prevailing osmotic or volume stimuli Hyponatremia, hypo-osmolality, urine osm > plasma osm, high urine Na Treatment is water restriction
UTHSCSA
Pediatric Resident Curriculum for the PICU
SUMMARY
Identify and treat primary brain injury
Rule out neurosurgical emergency
Minimize secondary ischemic brain injury by promoting cerebral perfusion
Maintain normovolemia and adequate BP Maintain normal electrolytes and euglycemia Maintain normocapnia and adequate oxygenation Avoid factors that increase ICP Treat intracranial hypertension
UTHSCSA
Das könnte Ihnen auch gefallen
- Special - NCLEX - Exam - Jakarta - Students - PDF Filename UTF-8''Special NCLEX Exam - Jakarta StudentsDokument23 SeitenSpecial - NCLEX - Exam - Jakarta - Students - PDF Filename UTF-8''Special NCLEX Exam - Jakarta Studentsrizqi100% (1)
- Ob - Gyne FinalDokument36 SeitenOb - Gyne FinalsyringomyeliaNoch keine Bewertungen
- Psych NBME Form 4Dokument2 SeitenPsych NBME Form 4Christine CassidyNoch keine Bewertungen
- Collection and Transport of Histopathology SpecimensDokument38 SeitenCollection and Transport of Histopathology SpecimensOmair Riaz100% (3)
- Head Injury and Intracranial HypertensionDokument43 SeitenHead Injury and Intracranial HypertensiondenekeNoch keine Bewertungen
- Head Injury 2Dokument47 SeitenHead Injury 2drvishal bhattNoch keine Bewertungen
- Head Trauma: Will/Grundy EMS 2009 2 Trimester May CMEDokument100 SeitenHead Trauma: Will/Grundy EMS 2009 2 Trimester May CMESytrose Morales100% (1)
- Head Trauma Brain InjuryDokument54 SeitenHead Trauma Brain Injurymirzabb1Noch keine Bewertungen
- Pediatric Neuro AnesthesiaDokument108 SeitenPediatric Neuro AnesthesiaGemechis Akuma WayyesaNoch keine Bewertungen
- Hypoxic Ischemic EncephalopathyDokument78 SeitenHypoxic Ischemic EncephalopathyUmesh SinghNoch keine Bewertungen
- Head Injuries 2015Dokument41 SeitenHead Injuries 2015jimmyNoch keine Bewertungen
- 2.1 - Increased Intracranial PressureDokument45 Seiten2.1 - Increased Intracranial PressureRose AnnNoch keine Bewertungen
- Management of Client With Neurologic Trauma Anatomy of The CraniumDokument17 SeitenManagement of Client With Neurologic Trauma Anatomy of The CraniumGoldie Reroma GelagaNoch keine Bewertungen
- Cerebrovascula R AccidentDokument31 SeitenCerebrovascula R Accidenttorr123Noch keine Bewertungen
- Head Injury: Tsegazeab Laeke, MD, FCS (ECSA) August 1,2018Dokument38 SeitenHead Injury: Tsegazeab Laeke, MD, FCS (ECSA) August 1,2018Amanuel AyladoNoch keine Bewertungen
- Lacunar Infarct and SyndromesDokument40 SeitenLacunar Infarct and Syndromeslovelots1234100% (1)
- Anesthetic Management of Intracranial Aneurysms R-MasriDokument66 SeitenAnesthetic Management of Intracranial Aneurysms R-MasriadheNoch keine Bewertungen
- Tbi Case PresentationDokument22 SeitenTbi Case PresentationNinaNoch keine Bewertungen
- CT ScanLesson VIDokument60 SeitenCT ScanLesson VILalaine De JesusNoch keine Bewertungen
- Traumatic Head InjuriesDokument50 SeitenTraumatic Head InjuriesVasudha BuddyNoch keine Bewertungen
- Askep Pasien Dengan Stroke ShareDokument48 SeitenAskep Pasien Dengan Stroke ShareIntan Pertiwi EdisonNoch keine Bewertungen
- Neurological SupportDokument26 SeitenNeurological Supporticu ciruasNoch keine Bewertungen
- WEEK 12 Diagnostics Altered PerceptionDokument131 SeitenWEEK 12 Diagnostics Altered PerceptionEMBER MARIE SAYMANNoch keine Bewertungen
- Brain Injury Dr. Shema Dr. MuyimboDokument58 SeitenBrain Injury Dr. Shema Dr. MuyimboTIMOTHY MUYIMBONoch keine Bewertungen
- Head TraumaDokument32 SeitenHead TraumacokarisaNoch keine Bewertungen
- Head InjuryDokument100 SeitenHead Injurywafaazulkifli100% (4)
- Management OF Head Injury: DR Echebiri, PDokument26 SeitenManagement OF Head Injury: DR Echebiri, PLuther ThengNoch keine Bewertungen
- Head Injury: Anthony G. Hillier, D.O. St. John West Shore Emergency Medicine ResidentDokument45 SeitenHead Injury: Anthony G. Hillier, D.O. St. John West Shore Emergency Medicine Residentsgod34Noch keine Bewertungen
- Anesthesia For Neurosurg2Dokument42 SeitenAnesthesia For Neurosurg2Praveen RamasamyNoch keine Bewertungen
- Stroke: A.K.A. Cerebrovascular Accident (CVA) & Brain AttackDokument81 SeitenStroke: A.K.A. Cerebrovascular Accident (CVA) & Brain AttackNovianty GliceriaNoch keine Bewertungen
- Cerebrovascular AccidentDokument31 SeitenCerebrovascular AccidentRam ReddyNoch keine Bewertungen
- Neurologic Trauma: Traumatic Brain InjuryDokument18 SeitenNeurologic Trauma: Traumatic Brain InjuryPearl Raiza Hadani100% (1)
- Head Trauma: Dr. Andy Wijaya, SpemDokument20 SeitenHead Trauma: Dr. Andy Wijaya, SpemThomas AlbertNoch keine Bewertungen
- Tekanan Intra KranialDokument31 SeitenTekanan Intra KranialUtari DzayNoch keine Bewertungen
- Head - Spinal - Injury SC1Dokument48 SeitenHead - Spinal - Injury SC1Jujhar BoparaiNoch keine Bewertungen
- Patho StrokeDokument14 SeitenPatho StrokeKyla R. PinedaNoch keine Bewertungen
- Lesson 5 - Altered PerceptionDokument10 SeitenLesson 5 - Altered PerceptionSTEFFANIE VALE BORJANoch keine Bewertungen
- Cns Pathology: Cerebral InfarctionDokument24 SeitenCns Pathology: Cerebral InfarctionElvisNoch keine Bewertungen
- 5A. Traumatic Brain InjuriesDokument242 Seiten5A. Traumatic Brain InjuriesMajed AlamiNoch keine Bewertungen
- SHORT CASE 1 Epidural HematomaDokument30 SeitenSHORT CASE 1 Epidural HematomaNurmalinda MappapaNoch keine Bewertungen
- Pharm Care in Stroke-1Dokument45 SeitenPharm Care in Stroke-1Achmad Triwidodo AmoeNoch keine Bewertungen
- Emed - Special Resuscitation Situations (Doc Vito)Dokument55 SeitenEmed - Special Resuscitation Situations (Doc Vito)Princess Cate MercadoNoch keine Bewertungen
- Emed - Special Resuscitation Situations (Doc Vito)Dokument55 SeitenEmed - Special Resuscitation Situations (Doc Vito)Princess Cate MercadoNoch keine Bewertungen
- Cerebral EdemaDokument40 SeitenCerebral EdemaMithun GorreNoch keine Bewertungen
- Intracranial Pressure (Icp) : Mohd Roslee Bin Abd GhaniDokument25 SeitenIntracranial Pressure (Icp) : Mohd Roslee Bin Abd GhaniSaha DirllahNoch keine Bewertungen
- Interference With Function Because of Vascular ConditionsDokument34 SeitenInterference With Function Because of Vascular Conditionsfrenee aradanasNoch keine Bewertungen
- Stroke, Inc IcpDokument6 SeitenStroke, Inc IcpJojo JustoNoch keine Bewertungen
- Increased Intracranial Pressure: T. Dawkins 19 - 64 2018Dokument14 SeitenIncreased Intracranial Pressure: T. Dawkins 19 - 64 2018okaciaNoch keine Bewertungen
- Management of Stroke: Dr. Isnaniah, Sp. SDokument80 SeitenManagement of Stroke: Dr. Isnaniah, Sp. SchintyamontangNoch keine Bewertungen
- Cranio Cerebral TraumaDokument10 SeitenCranio Cerebral TraumaAlexandrutzu356Noch keine Bewertungen
- HEAD INJURY (Trauma Kepala) DR - AgusDokument53 SeitenHEAD INJURY (Trauma Kepala) DR - AgusSetyo RahmanNoch keine Bewertungen
- Head InjuryDokument9 SeitenHead InjuryRaveen mayiNoch keine Bewertungen
- Intracranial HemorrhageDokument75 SeitenIntracranial HemorrhageDea DNoch keine Bewertungen
- Dr. Tommy SP - BS - Head Trauma Webinar Dr. TMYDokument30 SeitenDr. Tommy SP - BS - Head Trauma Webinar Dr. TMYOctafiani Trikartika DarimanNoch keine Bewertungen
- Traumatic Brain Injury and Cerebral ResuscitationDokument56 SeitenTraumatic Brain Injury and Cerebral ResuscitationsyahirNoch keine Bewertungen
- Meningitis: O Highly Contagious People at RiskDokument3 SeitenMeningitis: O Highly Contagious People at RiskJulx0Noch keine Bewertungen
- Head Trauma: Dr. Nasir Lamhot, Sp. BSDokument31 SeitenHead Trauma: Dr. Nasir Lamhot, Sp. BSYohannes KurniawanNoch keine Bewertungen
- Traumatic Brain Injury (TBI)Dokument48 SeitenTraumatic Brain Injury (TBI)Alaa OmarNoch keine Bewertungen
- IcpDokument30 SeitenIcpalia nanohanoNoch keine Bewertungen
- Chapter 62 Stroke Study GuideDokument4 SeitenChapter 62 Stroke Study GuideValerie BarrNoch keine Bewertungen
- 25 26. Operasi Neurologi IDokument75 Seiten25 26. Operasi Neurologi IMagfira Al HabsyiNoch keine Bewertungen
- Head Injury 5Dokument68 SeitenHead Injury 5drvishal bhattNoch keine Bewertungen
- Assessment of Racchimedular Injury by NursingVon EverandAssessment of Racchimedular Injury by NursingNoch keine Bewertungen
- STROKE: Handbook with activities, exercises and mental challengesVon EverandSTROKE: Handbook with activities, exercises and mental challengesNoch keine Bewertungen
- Pixma E510-E610 DLDokument2 SeitenPixma E510-E610 DLmangsiatNoch keine Bewertungen
- BrosurDokument2 SeitenBrosurAbuNoch keine Bewertungen
- Traumatic Brain Injury: National Institute of Neurological Disorders and Stroke National Institutes of HealthDokument53 SeitenTraumatic Brain Injury: National Institute of Neurological Disorders and Stroke National Institutes of HealthmangsiatNoch keine Bewertungen
- Icd 10 Cm/PcsDokument4 SeitenIcd 10 Cm/Pcsmuhammad maulana67% (6)
- Wap54g V3-Qig Combo W Eu de FR Ug WebDokument293 SeitenWap54g V3-Qig Combo W Eu de FR Ug WebBedest CakepNoch keine Bewertungen
- Head Injury ManagementDokument2 SeitenHead Injury ManagementWaiwit ChotchawjaruNoch keine Bewertungen
- Sample Employment Application FormDokument4 SeitenSample Employment Application Formapi-296940651Noch keine Bewertungen
- The Faces of Alzheimer'S Disease Self-Portraits by William Utermohlen UtermohlenDokument42 SeitenThe Faces of Alzheimer'S Disease Self-Portraits by William Utermohlen UtermohlenmangsiatNoch keine Bewertungen
- Icd 10 Cm/PcsDokument4 SeitenIcd 10 Cm/Pcsmuhammad maulana67% (6)
- 863lymphatic FilariasisDokument25 Seiten863lymphatic FilariasisShreya SinghalNoch keine Bewertungen
- Endocrinology Slides 2003 1119Dokument62 SeitenEndocrinology Slides 2003 1119mangsiatNoch keine Bewertungen
- Colour Atlas For MCCDokument80 SeitenColour Atlas For MCCpapaokey100% (3)
- EdemaDokument24 SeitenEdemamangsiatNoch keine Bewertungen
- About Arteriovenous Overview!!!Dokument7 SeitenAbout Arteriovenous Overview!!!Cj UritaNoch keine Bewertungen
- MS 21Dokument10 SeitenMS 21karenkaren09Noch keine Bewertungen
- Prevalence of Overhang Interproximal Amalgam RestorationsDokument4 SeitenPrevalence of Overhang Interproximal Amalgam RestorationsNaji Z. ArandiNoch keine Bewertungen
- Asuhan Keperawatan Pada Pasien Dengan Chronic Kidney DiseasesDokument24 SeitenAsuhan Keperawatan Pada Pasien Dengan Chronic Kidney DiseasestidaktahudiriNoch keine Bewertungen
- Maxillary Major ConnectorsDokument20 SeitenMaxillary Major ConnectorsRohan GroverNoch keine Bewertungen
- Pollock 2001Dokument14 SeitenPollock 2001Segura RojasNoch keine Bewertungen
- Suspension TherapyDokument39 SeitenSuspension TherapyFarrukh Shahzad100% (5)
- Disability Ahmed Refat 12 2012 121225021809 Phpapp02 PDFDokument81 SeitenDisability Ahmed Refat 12 2012 121225021809 Phpapp02 PDFRaghu NadhNoch keine Bewertungen
- KSRR 24 201Dokument7 SeitenKSRR 24 201Jesiree DizonNoch keine Bewertungen
- 1 March 2009 Dental Anatomy TestDokument15 Seiten1 March 2009 Dental Anatomy TestManish AggarwalNoch keine Bewertungen
- Arch-En-Design New Delhi / LucknowDokument12 SeitenArch-En-Design New Delhi / LucknowMC EstimationNoch keine Bewertungen
- FE ImbalanceDokument6 SeitenFE ImbalanceDonna CortezNoch keine Bewertungen
- SAAOL Heart Centre CaseDokument9 SeitenSAAOL Heart Centre CaseMunem ChowdhuryNoch keine Bewertungen
- Truncus ArteriosusDokument19 SeitenTruncus ArteriosusHijaz Al-YamanNoch keine Bewertungen
- 93 M Deatials PDFDokument5 Seiten93 M Deatials PDFRatna RoesardhyatiNoch keine Bewertungen
- Kuliah 8. Anestesi - Syok Dan Tata LaksananyaDokument63 SeitenKuliah 8. Anestesi - Syok Dan Tata LaksananyaDesi Suryani DewiNoch keine Bewertungen
- Lung Contusion & Traumatic AsphyxiaDokument17 SeitenLung Contusion & Traumatic AsphyxiaLady KeshiaNoch keine Bewertungen
- Ketoconazole: SampleDokument7 SeitenKetoconazole: SampleJuan PerezNoch keine Bewertungen
- ATPDDokument11 SeitenATPDsagar189Noch keine Bewertungen
- 6665 PDFDokument4 Seiten6665 PDFerindah puspowatiNoch keine Bewertungen
- Guidance For Industry Substantiation For Dietary Supplement Claims Made Under Section 403 (R) (6) of The Federal Food Drug and Cosmetic ActDokument18 SeitenGuidance For Industry Substantiation For Dietary Supplement Claims Made Under Section 403 (R) (6) of The Federal Food Drug and Cosmetic ActDeepa PatelNoch keine Bewertungen
- Benefits of Medical Expert SystemsDokument27 SeitenBenefits of Medical Expert Systemsrobertxxx100% (1)
- Acute Coronary Syndrome NCP 03Dokument6 SeitenAcute Coronary Syndrome NCP 03AgronaSlaughterNoch keine Bewertungen
- Barcelona 2014Dokument92 SeitenBarcelona 2014ckeshavaNoch keine Bewertungen
- AdenoidsDokument8 SeitenAdenoidsUjjawalShriwastavNoch keine Bewertungen
- Dr. Ameya PDFDokument2 SeitenDr. Ameya PDFdrameyaragnekarNoch keine Bewertungen