Beruflich Dokumente
Kultur Dokumente
Malaria
Hochgeladen von
Mich Tolentino0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
130 Ansichten31 SeitenMalaria is a disease of the blood that is caused by the Plasmodium parasite. The parasite is transmitted from person to person by a particular type of mosquito. Female Anopheles mosquito is the only mosquito that transmits malaria.
Originalbeschreibung:
Originaltitel
Malaria.pptx
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenMalaria is a disease of the blood that is caused by the Plasmodium parasite. The parasite is transmitted from person to person by a particular type of mosquito. Female Anopheles mosquito is the only mosquito that transmits malaria.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
130 Ansichten31 SeitenMalaria
Hochgeladen von
Mich TolentinoMalaria is a disease of the blood that is caused by the Plasmodium parasite. The parasite is transmitted from person to person by a particular type of mosquito. Female Anopheles mosquito is the only mosquito that transmits malaria.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 31
MALARIA
#17 Gales,Bea Trixia
#18 Gepulango, Ethel Princess
The word malaria comes from 18th century
Italian mala meaning "bad" and aria meaning "air".
the term was first used by Dr. Francisco Torti, Italy,
when people thought the disease was caused by foul
air in marshy areas.
Malaria is a disease of the blood that is caused by the
Plasmodium parasite, which is transmitted from
person to person by a particular type of mosquito.
THE ANOPHELES MOSQUITO
The female Anopheles mosquito is the only mosquito
that transmits malaria.
Serve as the vector that carries and transfers the
infectious agent (Plasmodium)
primarily bites between the hours of 9pm and 5am,
which is why sleeping under a mosquito net at night is
such an important method of prevention.
Plasmodium falciparum - the most serious form of the
disease. It is most common in Africa, especially sub-
Saharan Africa.
Plasmodium vivax - milder form of the disease,
generally not fatal. This species is most commonly
found in Asia, Latin America, and parts of Africa.
Plasmodium malariae - milder form of the disease,
generally not fatal. known to stay in the blood of some
people for several decades.
Plasmodium ovale. - rarely found outside Africa or the
western Pacific islands. Symptoms are similar to those
of P. vivax.
Plasmodium knowlesi -causes malaria in macaques but
can also infect humans.occurs in certain forested areas
of South-East Asia.
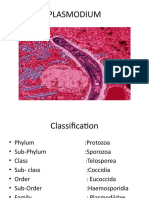
Kingdom Protista
Subkingdom Protozoa
Phylum Apicomplexa
Class Sporozoasida
Order Eucoccidiorida
Family Plasmodiidae
Genus Plasmodium
Species falciparum, malariae, ov
ale, vivax
The morphology of P. knowlesi parasites in human
infections:
closely resembled those of P. falciparum in the early
trophozoite stage
and P. malariae in the later stages of the erythrocytic
cycle.
Malaria commonly occur s in Central America, South America,
Caribbean, Africa, and Asia
The Malaria Control Program has categorized these 79 provinces based on the
5-year average .This helps the program in prioritizing resources in Categories A
& B provinces. Out of the 79 provinces, 57 are malaria endemic provinces. In
2007, 6 provinces have been added in the list of Category D provinces.
Involves two hosts,
Human and Anopheles
mosquitoes
The disease is transmitted
to humans when an
infected female
Anopheles mosquito bites
a person and injects the
malaria parasites
(sporozoites) into the
blood.
Sporozoites travel through
the bloodstream to the
liver, mature, and
eventually infect the
human red blood cells.
While in red blood cells,
the parasites again develop
until a mosquito takes a
blood meal from an
infected human and
ingests human red blood
cells containing the
parasites.
Then the parasites reach
the Anopheles mosquitos
stomach and eventually
invade the mosquito
salivary glands.
When an Anopheles
mosquito bites a human,
these sporozoites complete
and repeat the complex
Plasmodium life cycle.
Incubation means the time between becoming infected
and the appearance of symptoms. This generally
depends on the type of parasite:
P. falciparum - 9 to 14 days
P. vivax - 12 to 18 days
P. ovale - 12 to 18 days
P. malariae - 18 to 40 days
However, incubation periods can vary from as short as
7 days, to several months for P. vivax and P. ovale.
The first symptoms include fever, headache and
vomiting. . It is extremely uncommon for malaria to
cause skin lesions or rash.
If not treated within 24 hours, P. falciparum malaria
can progress to severe illness often leading to death.
Children with severe malaria
frequently develop one or more
of the following symptoms:
severe anaemia, respiratory
distress in relation to metabolic
acidosis, or cerebral malaria.
In adults, multi-organ
involvement is also frequent. In
malaria endemic areas, persons
may develop partial immunity,
allowing asymptomatic
infections to occur.
Demonstration of the parasites in peripheral blood is
important to a diagnosis
Several effective methods of diagnosis have been
developed:
Fluorescent dye staining
DNA probe specific for P. falciparum
PCR diagnostics
ELISA detection of P. falciparum antigen
WHO recommends that all cases of suspected malaria be
confirmed using parasite-based diagnostic testing (either
microscopy or rapid diagnostic test) before administering
treatment. These tests take less than 30 minutes to
perform.
Rapid tests can detect proteins called antigens that are
present in Plasmodium. However, the reliability of rapid
tests varies significantly from product to product. Thus, it
is recommended that rapid tests be used in conjunction
with microscopy.
the polymerase chain reaction (PCR) ,which detects
malaria DNA. Because this test is not widely available, it is
important not to delay treatment while waiting for results.
According to the CDC, the following drugs are commonly
used for treating malaria:
artemether-lumefantrine (Coartem)
atovaquone-proguanil (Malarone)
chloroquine
clindamycin (used in combination with quinine)
doxycycline (used in combination with quinine)
mefloquine (Lariam)
quinidine
quinine
artesunate
Most medications are available only as tablets or pills.
Intravenous treatment with quinidine may be needed
in severe malaria or when the patient cannot take oral
medications.
Patients with P. vivax or P. ovale may not be completely
cured by the above medications, even though the
symptoms resolve. This is because the parasites can
hide in the liver. A medication called primaquinine is
used to eradicate the liver form, but this drug cannot
be given to people who are deficient in an enzyme
called G6PD.
The best available treatment, particularly for P.
falciparum malaria, is artemisinin-based combination therapy
(ACT).
Artemether-lumefantrine: Coartem as the 1st line treatment of
uncomplicated P. falciparum cases, followed by Primaquine on
the 4th day of treatment.
Treatment of severe P.falciparum is a combination therapy of
quinine ampule/tablet plus any of the following antibiotics:
Tetracycline, Doxycycline or Clindamycin.
P. vivax cases are treated with Chloroquine for 3 days and
Primaquine for 14 days
PfSPZ, an unusual experimental malaria vaccine, developed
by Sanaria Inc. of Rockville, Maryland, USA, has shown
great promise in an early-stage clinical trial.
Trial researchers said the vaccine may provide 100%
protection against malaria infection in healthy adults.It is
said that PfSPZ has the best result for a malaria vaccine so
far.
. It uses weakened forms of the whole, immature
"sporozoite" phase of the parasite, and not an assortment
of parasite proteins to induce an immune response.
On October 10th, 2013, that a large-scale Phase III African
trial using the experimental malaria vaccine RTS,S
continued protecting young children up to 18 months after
vaccination.
The trial showed that RTS,S reduced cases of clinical
malaria in young children by 46% after the first vaccine,
compared to children of the same aged (5-17 months) who
received a control vaccine.
Babies aged six to twelve weeks had a 27% lower clinical
malaria incidence.
Vector control is the main way to reduce malaria
transmission at the community level
Two forms of vector control are effective in a wide range of
circumstances.
Insecticide-treated mosquito nets (ITNs)
Long-lasting insecticidal nets (LLINs) are the preferred form of ITNs
for public health distribution programmes.
The most cost effective way to achieve this is through provision of free
LLINs, so that everyone sleeps under a LLIN every night.
Indoor spraying with residual insecticides
Indoor residual spraying (IRS) with insecticides is a powerful way to
rapidly reduce malaria transmission. Its full potential is realized when
at least 80% of houses in targeted areas are sprayed. Indoor spraying is
effective for 36 months, depending on the insecticide used and the
type of surface on which it is sprayed.
Longer-lasting forms of existing IRS insecticides, as well as new classes
of insecticides for use in IRS programmes, are under development.
Antimalarial medicines can also be used to prevent
malaria:
For travellers, malaria can be prevented through
chemoprophylaxis, which suppresses the blood stage
of malaria infections, thereby preventing malaria
disease.
WHO recommends intermittent preventive treatment
with sulfadoxine-pyrimethamine for pregnant women
living in high transmission areas, at each scheduled
antenatal visit after the first trimester.
In 2012, WHO recommended Seasonal Malaria
Chemoprevention as an additional malaria prevention
strategy for areas of the Sahel sub-Region of Africa.
administration of monthly courses of amodiaquine
plus sulfadoxine-pyrimethamine to all children under
5 years of age during the high transmission season.
The vision of the Malaria Control Program is a malaria-free
Philippines by 2020. Strategies of the MCP include the
following:
1) Early diagnosis and prompt treatment
2) Vector control insecticide-treated mosquito net as main
vector control strategy, complemented by indoor residual
spraying
3) early management and disease surveillance
4) monitoring and evaluation drug and insecticide
resistance monitoring; drug quality monitoring (pilot study
to determine the baseline profile); Quality Assurance for
microscopy (GF sites) and Philippine Malaria Information
System at the provincial level.
Health services, including malaria control program
has been devolved to the local government units
(Local GovernmentCode of 1991).
The Department of Health has further undergone
reorganization to address its new role and mandate
under a decentralized set-up. The functions of the
DOH are policy formulation, advocacy, program
development, standard setting, technical assistance,
regulation and monitoring.
Gardner, MJ; Hall, N; Fung, E; White, O; Berriman, M; Hyman, RW; Carlton, JM; Pain, A;
Nelson, KE (2002). "Genome sequence of the human malaria parasite Plasmodium
falciparum". Nature 419 (6906): 498
511.Bibcode:2002Natur.419..408G.doi:10.1038/nature01097.PMID 12368864.
World Heath Organization http://www.who.int/mediacentre/factsheets/fs094/en/
Taxonomical Classification http://www. Msu.edu/course/zol/316/ pspptax.htm
Spread of malaria signs and symptoms http://www.cambodiafirstclinic.com/malaria/
Malaria in the Philippines
http://www.actmalaria.net/downloads/pdf/info/2008/Philippines%20Malaria%20Count
ry%20Profile%202008.pdf
Types of Malaria http://www.medicalnewstoday.com/articles/150670.php
Malaria http://www.emedicinehealth.com/malaria/page2_em.htm
Morphological Classification of Plasmodium
http://www.tulane.edu/`wiser/protozoology/notes/pl_sp.html
Morphological Classification of P.
knowlesihttp://www.ncbi.nlm.nih.gov/pmc/articles/PMC2676309/
Das könnte Ihnen auch gefallen
- Shoe Dog: A Memoir by the Creator of NikeVon EverandShoe Dog: A Memoir by the Creator of NikeBewertung: 4.5 von 5 Sternen4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Von EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Bewertung: 4 von 5 Sternen4/5 (98)
- BIOCHEM With AnswerDokument16 SeitenBIOCHEM With AnswerMich TolentinoNoch keine Bewertungen
- TX Non PharmacologicalDokument1 SeiteTX Non PharmacologicalMich TolentinoNoch keine Bewertungen
- Treatment INDDokument1 SeiteTreatment INDMich TolentinoNoch keine Bewertungen
- Solucionario Fenomenos de Transporte - Bird PDFDokument175 SeitenSolucionario Fenomenos de Transporte - Bird PDFAbi67% (6)
- Pacquiao Spouses vs. Commissioner on Internal Revenue tax case analysisDokument1 SeitePacquiao Spouses vs. Commissioner on Internal Revenue tax case analysisMich TolentinoNoch keine Bewertungen
- 2 LipidDokument48 Seiten2 LipidAshraf Rios KhaterNoch keine Bewertungen
- PX CDokument1 SeitePX CMich TolentinoNoch keine Bewertungen
- Hethics Prelims: Principles Premises To The Existence of Moral Principles. There Are Some Particular Moral TruthsDokument1 SeiteHethics Prelims: Principles Premises To The Existence of Moral Principles. There Are Some Particular Moral TruthsMich TolentinoNoch keine Bewertungen
- Swine FluDokument52 SeitenSwine FluMich TolentinoNoch keine Bewertungen
- TermsDokument1 SeiteTermsMich TolentinoNoch keine Bewertungen
- Gastritis CLNPHRDokument27 SeitenGastritis CLNPHRMich TolentinoNoch keine Bewertungen
- TermsDokument1 SeiteTermsMich TolentinoNoch keine Bewertungen
- Kaoru Ishikawa 2Dokument3 SeitenKaoru Ishikawa 2Mich Tolentino100% (1)
- Bahay Tsinoy PDFDokument2 SeitenBahay Tsinoy PDFMich TolentinoNoch keine Bewertungen
- Mising SOAP and ReferenceDokument26 SeitenMising SOAP and ReferenceMich TolentinoNoch keine Bewertungen
- Ethics For Pharmacistsch4 PDFDokument14 SeitenEthics For Pharmacistsch4 PDFMich TolentinoNoch keine Bewertungen
- Code of Ethics For PharmacistsDokument4 SeitenCode of Ethics For PharmacistsMich TolentinoNoch keine Bewertungen
- PX CDokument1 SeitePX CMich TolentinoNoch keine Bewertungen
- RX 1 10Dokument9 SeitenRX 1 10Mich Tolentino0% (1)
- Asssss PB 2 PDFDokument2 SeitenAsssss PB 2 PDFMich TolentinoNoch keine Bewertungen
- Philippine Pharmaceutical Marketing and Self-MedicationDokument16 SeitenPhilippine Pharmaceutical Marketing and Self-MedicationMich TolentinoNoch keine Bewertungen
- Home Medication ManagementDokument1 SeiteHome Medication ManagementMich TolentinoNoch keine Bewertungen
- RX 18 20 PDFDokument13 SeitenRX 18 20 PDFMich TolentinoNoch keine Bewertungen
- UST Hospital Prescriptions SummaryDokument5 SeitenUST Hospital Prescriptions SummaryMich Tolentino100% (1)
- Evaluating - The - Clinical Literature - PPSXDokument51 SeitenEvaluating - The - Clinical Literature - PPSXMich TolentinoNoch keine Bewertungen
- Drug Information Resources - PPSXDokument28 SeitenDrug Information Resources - PPSXMich TolentinoNoch keine Bewertungen
- Hethics Prelims: Principles Premises To The Existence of Moral Principles. There Are Some Particular Moral TruthsDokument1 SeiteHethics Prelims: Principles Premises To The Existence of Moral Principles. There Are Some Particular Moral TruthsMich TolentinoNoch keine Bewertungen
- Math30 Thu Lecture 01Dokument11 SeitenMath30 Thu Lecture 01Mich TolentinoNoch keine Bewertungen
- Compact Pharmaceutical Corporation PDFDokument2 SeitenCompact Pharmaceutical Corporation PDFMich TolentinoNoch keine Bewertungen
- 4F ProductInsert Tolentino, MDokument2 Seiten4F ProductInsert Tolentino, MMich TolentinoNoch keine Bewertungen
- Never Split the Difference: Negotiating As If Your Life Depended On ItVon EverandNever Split the Difference: Negotiating As If Your Life Depended On ItBewertung: 4.5 von 5 Sternen4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceVon EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceBewertung: 4 von 5 Sternen4/5 (890)
- Grit: The Power of Passion and PerseveranceVon EverandGrit: The Power of Passion and PerseveranceBewertung: 4 von 5 Sternen4/5 (587)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeVon EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeBewertung: 4 von 5 Sternen4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingVon EverandThe Little Book of Hygge: Danish Secrets to Happy LivingBewertung: 3.5 von 5 Sternen3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureVon EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureBewertung: 4.5 von 5 Sternen4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryVon EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryBewertung: 3.5 von 5 Sternen3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerVon EverandThe Emperor of All Maladies: A Biography of CancerBewertung: 4.5 von 5 Sternen4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersVon EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersBewertung: 4.5 von 5 Sternen4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealVon EverandOn Fire: The (Burning) Case for a Green New DealBewertung: 4 von 5 Sternen4/5 (73)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaVon EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaBewertung: 4.5 von 5 Sternen4.5/5 (265)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyVon EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyBewertung: 3.5 von 5 Sternen3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnVon EverandTeam of Rivals: The Political Genius of Abraham LincolnBewertung: 4.5 von 5 Sternen4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreVon EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreBewertung: 4 von 5 Sternen4/5 (1090)
- The Unwinding: An Inner History of the New AmericaVon EverandThe Unwinding: An Inner History of the New AmericaBewertung: 4 von 5 Sternen4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Von EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Bewertung: 4.5 von 5 Sternen4.5/5 (119)
- Her Body and Other Parties: StoriesVon EverandHer Body and Other Parties: StoriesBewertung: 4 von 5 Sternen4/5 (821)
- Frequently Asked Questions (Faqs) : What Is Malaria?Dokument3 SeitenFrequently Asked Questions (Faqs) : What Is Malaria?Dummy1 AccountNoch keine Bewertungen
- Malaria Management Asep MCU FinalDokument65 SeitenMalaria Management Asep MCU FinalTommy JunaidiNoch keine Bewertungen
- JKJJDokument11 SeitenJKJJJesseJamesNoch keine Bewertungen
- Jurnal PDFDokument7 SeitenJurnal PDFAjeng WidyastutiNoch keine Bewertungen
- Surveilans FilariasisDokument12 SeitenSurveilans Filariasisesti syafaahNoch keine Bewertungen
- CDC - Malaria - About Malaria - HistoryDokument5 SeitenCDC - Malaria - About Malaria - Historyapi-286232916Noch keine Bewertungen
- Plasmodium Parasite Life Cycle and SpeciesDokument36 SeitenPlasmodium Parasite Life Cycle and SpeciesHibaaq AxmedNoch keine Bewertungen
- ProtozoaDokument18 SeitenProtozoaKathleen RagudoNoch keine Bewertungen
- Pathogenesis of MalariaDokument2 SeitenPathogenesis of MalariaAde YonataNoch keine Bewertungen
- Factors Linked to Dengue Fever IncidenceDokument9 SeitenFactors Linked to Dengue Fever IncidenceNhana NhanottNoch keine Bewertungen
- MalariaDokument28 SeitenMalariaArthur Samuel ShavaniNoch keine Bewertungen
- Penyelidikan Kejadian Luar Biasa (KLB) Demam Chikungunya Di Kelurahan Talawaan Kab. Minahasa Utara Provinsi Sulawesiu UtaraDokument12 SeitenPenyelidikan Kejadian Luar Biasa (KLB) Demam Chikungunya Di Kelurahan Talawaan Kab. Minahasa Utara Provinsi Sulawesiu UtaraRena SajaNoch keine Bewertungen
- 4 SporozoaDokument42 Seiten4 SporozoaFranz SalazarNoch keine Bewertungen
- Evidence-Based Case Report Ceftriaxone Verus Penicillin For Treatment of Leptopspirosis in AdultsDokument7 SeitenEvidence-Based Case Report Ceftriaxone Verus Penicillin For Treatment of Leptopspirosis in AdultsWinson JosNoch keine Bewertungen
- Materi MalariaDokument29 SeitenMateri MalariaRudy Arindra WijayaNoch keine Bewertungen
- Malaria Situation in India: Dr. Neeraj Dhingra Additional Director & Head Malaria Division, NVBDCP Dghs Mohfw IndiaDokument21 SeitenMalaria Situation in India: Dr. Neeraj Dhingra Additional Director & Head Malaria Division, NVBDCP Dghs Mohfw IndiaMJ SolNoch keine Bewertungen
- Hist 2021-2022Dokument364 SeitenHist 2021-2022Ade HanityaNoch keine Bewertungen
- Developing Whole PersonDokument10 SeitenDeveloping Whole Personarun sivaNoch keine Bewertungen
- ElephantiasisDokument13 SeitenElephantiasisrhimineecat71Noch keine Bewertungen
- Brugia timori Epidemiology and Life CycleDokument6 SeitenBrugia timori Epidemiology and Life CycleNurul Farhana IsmailNoch keine Bewertungen
- Malaria Treatment Guidelines WHO 2010Dokument211 SeitenMalaria Treatment Guidelines WHO 2010emc27Noch keine Bewertungen
- Kemampuan Predasi Ikan Kepala Timah Aplocheilus Panchax Jantan Dan Betina Terhadap Larva Nyamuk Aedes AegyptiDokument5 SeitenKemampuan Predasi Ikan Kepala Timah Aplocheilus Panchax Jantan Dan Betina Terhadap Larva Nyamuk Aedes AegyptiAesthetic GirlNoch keine Bewertungen
- Dengue FeverDokument28 SeitenDengue Fevercooky maknaeNoch keine Bewertungen
- Malaria Se Bachne Ke 10 Upay Malaria Prevention Tips in HindiDokument2 SeitenMalaria Se Bachne Ke 10 Upay Malaria Prevention Tips in HindiGovindNoch keine Bewertungen
- MalariaDokument4 SeitenMalarianafrabNoch keine Bewertungen
- Markell and Voges Medical Parasitology 9th Ed PDFDokument487 SeitenMarkell and Voges Medical Parasitology 9th Ed PDFariana praditaNoch keine Bewertungen
- National Vector Borne Disease ControlDokument12 SeitenNational Vector Borne Disease ControlSutirtho MukherjiNoch keine Bewertungen
- PlasmodiumDokument15 SeitenPlasmodiumanil singhNoch keine Bewertungen
- 02 Dr. Anung Sugihantono, M.kesDokument15 Seiten02 Dr. Anung Sugihantono, M.kesratna ayu lestariNoch keine Bewertungen
- 12 DBD Malaria PKP 2018 TetapDokument24 Seiten12 DBD Malaria PKP 2018 TetapNugrah HilmiNoch keine Bewertungen