Beruflich Dokumente
Kultur Dokumente
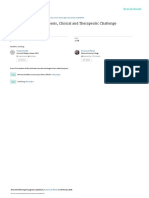
Fig. 2. View of Calcium: Sulphate Beads On Plain X-Ray Before Resorption
Hochgeladen von
Rade GrbićOriginalbeschreibung:
Originaltitel
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Fig. 2. View of Calcium: Sulphate Beads On Plain X-Ray Before Resorption
Hochgeladen von
Rade GrbićCopyright:
Verfügbare Formate
Evaluating the role of antibiotic-loaded calcium sulphate in the
treatment of
chronic osteomyelitis
6. Are there other suitable
Jack
Carruthers
1. Chronic osteomyelitis overview
4. What are the options?
Aetiology
Haematogenous seeding (rare in West); post-traumatic (especially in compound
fractures); infected foreign body.
Pathology
Bacterial entry into bone triggers an acute inflammatory response. Bacterial
virulence factors disrupt the blood supply, leading to the formation of a necrotic
sequestrum. The infection progresses to chronicity due to damaged skin,
abundant scarring, and impaired vascularity. Patient factors including
malnutrition, diabetes mellitus and smoking contribute to infection persistence.
Infection can spread to the soft tissues causing a discharging sinus.
Clinical features
Localised bone pain accompanied by erythema, and swelling. Sometimes there
are symptoms of systemic infection. A raised ESR and CRP can be present.
Diagnosis
Radiological features include: loss of trabecular architecture, osteopaenia,
scalloping of the inner surface of the bone cortex, periosteal involucrum
formation seen next to a radio-dense sequestrum. (1)
bioceramics?
PMMA beads
These were developed by Klemm in the 1970s (4). The delivery of antibiotics by
PMMA bead chains to the osteomyelitic cavity was demonstrated to be
in the order of 200 times that of systemic antibiotics (5). In rabbit
experimental models, treatment of osteomyelitis with PMMA beads
showed a 100% success rate at preventing infection recurrence (6).
Human studies by Nelson et al. demonstrated a reduction in the risk of
infection recurrence of 18% in patients treated with PMMA beads versus
conventional therapy (7). PMMA seemed to be the way forward; but a
major concern is that they require a second operation to remove.
Therefore, the focus is now on resorbable antibiotic carriers.
Collagen fleece
Although widely used and biodegradable, collagen fleece has numerous drawbacks. It is associated with seroma formation, and a recent study
demonstrated that it eluted 95% of its gentamicin in the first day (8).
5. Calcium sulphate
2. Current treatment rationale
Chronic osteomyelitis is primarily a surgical disease (2):
Debride the area of osteomyelitis.
Take no less than 5 microbiology samples for culture and sensitivity, and 3-5
histology samples.
Excise the area of necrotic bone, aiming for healthy bleeding bone at the cut
margins.
Dead-space management of the cavity, including antibiotic-loaded carriers.
Optional muscle flaps can promote revascularisation and healthy bone
formation, and provide soft-tissue coverage of the bone compartment.
Growth of new bone to fill the cavity can be encouraged by bone grafting and
osteoconductive bone graft substitutes.
Fig. 1. View of calcium sulphate
beads being introduced into a
debrided and excised cavity
(adapted from (13)).
3. Antibiotic-loaded carriers
What? Usually of an inert substance, they are loaded with broad-spectrum
antibiotics and placed into the excision cavity.
Why? They deliver high concentrations of antibiotics locally without the sideeffects of high-dose systemic antibiotics. In addition, they are important
in dead-space management, preventing haematoma formation. The
osteoconductive carriers act as bone graft substitutes, helping new bone
grow to fill the cavity (3).
Fig. 2. View of calcium
sulphate beads on plain Xray before resorption (10).
The first documented use of calcium sulphate, a
bioceramic, to treat bone infections was in 1842 by
Dreesmann (2). Since then, it has been loaded with
antibiotics to create a superior bone graft substitute
and is capable of effective dead-space management:
Antibiotic characteristics
Elution kinetics of many antibiotics, including
gentamicin, were investigated by Wichelhaus et al.
Calcium sulphate releases antibiotic over 10 days or
more in amounts well above the MIC of most
bacteria (9). It provides high local antibiotic
concentrations without systemic side-effects (10).
Resorbable
A prospective study into calcium sulphate pellet
treatment showed full resorption by 6 months posttreatment (10). This obviates the need for a second
operation to remove the dead-space filler.
Osteoconductivity
Immunofluorescence studies demonstrated that both
osteoblasts and osteoclasts could adhere to a
calcium sulphate scaffold (11). Chang showed that
patients achieved full weight bearing status 3
months post-treatment for chronic osteomyelitis,
suggesting sufficient bone in-growth (12). Recently,
Franceschini et al. used X-rays 12 months post-op to
show that calcium sulphate Herafill beads, used at
the NOC, provide support for undisturbed reossification of the tibia, proving it to be an effective
bone graft substitute (13).
Infection control
In goat-models of tibial chronic osteomyelitis,
tobramycin-impregnated calcium sulphate beads
loaded into the dead-space prevented recurrence of
Current research into bioceramics including calcium sulphate have aimed to
optimise their osteoconductivity. Options other than calcium sulphate include
tricalcium phosphate (TCP) and silicated calcium phosphate (Si-CaP). A
comparative study by Hing et al. showed that calcium sulphate is resorbed too
quickly to provide a smooth continuum between resorption and adsorption of
bone. Indeed, the osteoconductive kinetics of Si-CaP were superior,
demonstrating re-vascularisation and bone apposition over 3-6 weeks (17).
7. Caveats to calcium sulphate use
The limits of osteoconductivity?
The osteoconductivity of calcium sulphate has been called into question in a
number of studies, not least Hing et al. Stubbs showed that while calcium
sulphate provided support for some bone in-growth, it did not result in complete
filling of the defect before total resorption (18). Moreover, the pattern of bone
in-growth in calcium sulphate is sporadic rather than gradual.
Inflammation?
High rates of resorption may result in microparticle-induced inflammation. The
resulting acidic environment favours osteoclast action and further degradation
of the ceramic (19). However, numerous studies challenge this contention, and
anecdotally, the NOC has not encountered this problem.
8. Conclusions: the future
Calcium sulphate fulfils the primary goal for the treatment of any disease:
patient satisfaction. Ultimately, it is a tool which allows patients to achieve an
infection-free fully functional bone or joint.
Calcium sulphate can only be improved. Recent experiments have combined
calcium sulphate with hydroxyapatite (HA) to improve biocompatibility and
osteoconductivity. Both Stubbs et al. and Rauschmann et al. highlighted
superior bone graft properties in calcium sulphate-HA composite carriers (18,
20). Adding a silicon component could enhance its ability to stimulate bone
metabolism (17).Combining calcium sulphate with mesenchymal stem cells to
promote new bone formation and stem cell osteogenic differentiation may be the
next step (21).
9. References
(1)
(2)
(3)
(4)
(5)
(6)
(7)
(8)
(9)
(10)
(11)
(12)
(13)
(14)
(15)
(16)
(17)
(18)
(19)
(20)
(21)
Berendt, A., Chapter 41: Acute and chronic osteomyelitis, In Cohen, J. et al., Infectious Diseases, volume one, Mosby Elsevier, p.p. 445-456.
Parsons, B. and E. Strauss, Surgical management of chronic osteomyelitis, The American Journal of Surgery, 188, 57S-66S (2004).
El-husseiny, M. et al., Biodegradable antibiotic delivery systems, The Journal of Bone and Joint Surgery, 93-B, 151-157 (2011).
Klemm, K. W., Gentamicin-PMMA chains (Septopal chains) for the local antibiotic treatment of chronic osteomyelitis, Reconstructive Surgery and Traumatology, 20, 11-35 (1988).
Wahlig, H. et al., The release of gentamicin from PMMA beads: an experimental and pharmacokinetic study, The Journal of Bone and Joint Surgery, 60-B, 270 (1978).
Evans, R. P. and C. L. Nelson, Gentamicin-impregnated PMMA beads compared with systemic antibiotic therapy in the treatment of chronic osteomyelitis, Clinical Orthopaedics and Related Research, 295,
37-42 (1993).
Nelson, C. L. et al., A comparison of gentamicin-impregnated polymethylmethacrylate bead implantation to conventional parenteral antibiotic therapy in infected total hip and knee arthroplasty, Clinical
Orthopaedics and Related Research, 295, 96-101 (1993).
Srensen, T. S., et al., Rapid release of gentamicin from collagen sponge: in vitro comparison with plastic beads, Acta Orthopaedica Scandinavica, 61, 353-361 (1990).
Wichelhaus, T. A. et al., Elution characteristics of vancomycin, teicoplanin, gentamicin and clindamycin from calcium sulphate beads, Journal of Antimicrobial Chemotherapy, 48, 117-119 (2001).
McKee, L. et al., The use of an antibiotic-impregnated, osteoconductive, bioabsorbable bone substitute in the treatment of infected long bone defects: early results of a prospective trial, Journal of Orthopaedic
Trauma, 16, 622-627 (2002).
Sidqui, M. et al., Osteoblast adherence and resorption activity of isolated osteoclasts on calcium sulphate hemihydrate, Biomaterials, 16, 1327-1332 (1995).
Chang, W. et al., Adult osteomyelitis: debridement versus debridement plus Osteoset T pellets, Acta Orthopaedica Belgica, 73, 238-243 (2007).
Franceschini, M. et al., Treatment of a chronic recurrent fistulised tibial osteomyelitis: administration of a novel antibiotic-loaded bone substitute combined with a pedicular muscle flap sealing, European
Journal of Orthopaedic Surgery and Traumatology, Published online (2012).
Thomas, D. B. et al., Tobramycin-impregnated calcium sulphate prevents infection in contaminated wounds, Clinical Orthopaedics and Related Research, 441, 366-371 (2005).
Nelson, C. L. et al., The treatment of experimental osteomyelitis by surgical debridement and the implantation of calcium sulfate tobramycin pellets, Journal of Orthopaedic Research, 20, 643-647 (2002).
Bouillet, R. et al., Traitement de losteomylite chronique en milieu africain par implants de pltre impregne dantibiotiques, Acta Orthopaedica Belgica, 55, 2-11 (1989).
Hing, K. A. et al., Comparative performance of three ceramic bone graft substitutes, The Spine Journal, 7, 475-490 (2007).
Stubbs, D. et al., In vivo evaluation of resorbable bone graft substitutes in a rabbit tibial defect model, Biomaterials, 25, 5037-5044 (2004).
Lu, J. et al., Relationship between bioceramics sintering and micro-particles-induced cellular damages, Journal of Materials Science: Materials in Medicine, 15, 361-365 (2004).
Rauschmann, M. A. et al., Nanocrystalline hydroxyapatite and calcium sulphate as biodegradable composite carrier material for local delivery of antibiotics in bone infections, Biomaterials, 26, 2677-2684
(2005).
Ueng, S. W. et al., Biodegradable alginate antibiotic beads, Clinical Orthopaedics and Related Research, 380, 250-259 (2000).
Das könnte Ihnen auch gefallen
- Biochemical Markers of Bone Metabolism PPT LectureDokument89 SeitenBiochemical Markers of Bone Metabolism PPT LectureNeil Vincent De AsisNoch keine Bewertungen
- 03 Bone Non-Neoplastic Part-1Dokument52 Seiten03 Bone Non-Neoplastic Part-1dryunusaqNoch keine Bewertungen
- Hydroxyapatite Ceramic Coating For Bone Implant FixationDokument60 SeitenHydroxyapatite Ceramic Coating For Bone Implant FixationCerita KitaNoch keine Bewertungen
- Article PDFDokument5 SeitenArticle PDFLauren LimNoch keine Bewertungen
- Osseteointegration of Dental ImplantDokument24 SeitenOsseteointegration of Dental ImplantFajar Kusuma Dwi KurniawanNoch keine Bewertungen
- Bone Tissue Enginering Hope Vs HypeDokument7 SeitenBone Tissue Enginering Hope Vs Hypecollin samuelNoch keine Bewertungen
- NJMS 14 125Dokument5 SeitenNJMS 14 125dreneanastriNoch keine Bewertungen
- Tesla BookDokument23 SeitenTesla BookKhaled Al GhaebNoch keine Bewertungen
- Masquelet InjuryDokument8 SeitenMasquelet Injurydrets70Noch keine Bewertungen
- Clinical and Radiographic of Marginal Periimplant Tissue Stability After Buccal Defect Regeneration Using Porous Titanium GranuDokument12 SeitenClinical and Radiographic of Marginal Periimplant Tissue Stability After Buccal Defect Regeneration Using Porous Titanium GranuDrMohamed AssadawyNoch keine Bewertungen
- J Tissue Eng Regen Med - 2014 - Detsch - The Role of Osteoclasts in Bone Tissue EngineeringDokument17 SeitenJ Tissue Eng Regen Med - 2014 - Detsch - The Role of Osteoclasts in Bone Tissue EngineeringVinícius Gabriel da SilvaNoch keine Bewertungen
- Complications in The Use of The Mandibular Body, Ramus and Symphysis As Donor Sites in Bone Graft Surgery. A Systematic ReviewDokument9 SeitenComplications in The Use of The Mandibular Body, Ramus and Symphysis As Donor Sites in Bone Graft Surgery. A Systematic ReviewBrenda Carolina Pattigno ForeroNoch keine Bewertungen
- Wallace, Maxillary Sinus AugmentationDokument16 SeitenWallace, Maxillary Sinus AugmentationChin-lungHsiehNoch keine Bewertungen
- Chapter 17 2Dokument106 SeitenChapter 17 2Zamir PaezNoch keine Bewertungen
- Kim2017 PDFDokument12 SeitenKim2017 PDFYashu GvNoch keine Bewertungen
- BR 04 03 0374Dokument5 SeitenBR 04 03 0374Anastasia EkaNoch keine Bewertungen
- Implant-Bone IntegrationDokument14 SeitenImplant-Bone IntegrationADanAlfaNoch keine Bewertungen
- Bone Tissue EngineeringDokument9 SeitenBone Tissue EngineeringKevinNoch keine Bewertungen
- Nanofibrous Substrates For Bone Tissue Biomimetic Hydroxyapatite-Containing CompositeDokument18 SeitenNanofibrous Substrates For Bone Tissue Biomimetic Hydroxyapatite-Containing CompositespsudharsansNoch keine Bewertungen
- Chapter VIDokument17 SeitenChapter VIsteigmannNoch keine Bewertungen
- Bone Graft Substitutes in Periodontal and Peri-Implant Bone RegenerationDokument4 SeitenBone Graft Substitutes in Periodontal and Peri-Implant Bone RegenerationKamila BencosmeNoch keine Bewertungen
- 2366-Article Text-6003-1-10-20190926Dokument8 Seiten2366-Article Text-6003-1-10-20190926Hugo MoralesNoch keine Bewertungen
- Craniofacial Bone Grafting Wolff's Law RevisitedDokument13 SeitenCraniofacial Bone Grafting Wolff's Law RevisitedR KNoch keine Bewertungen
- Histologic Comparison of Biologic Width Around Teeth Versus Implants: The Effect On Bone PreservationDokument5 SeitenHistologic Comparison of Biologic Width Around Teeth Versus Implants: The Effect On Bone PreservationPaul CerdaNoch keine Bewertungen
- Srep 17134Dokument13 SeitenSrep 17134Affan Nadeem QaziNoch keine Bewertungen
- Clinical Application of Scaffolds For Cartilage Tissue EngineeringDokument17 SeitenClinical Application of Scaffolds For Cartilage Tissue EngineeringikulNoch keine Bewertungen
- 1 s2.0 S0846537114001156 MainDokument7 Seiten1 s2.0 S0846537114001156 MainhilalNoch keine Bewertungen
- Bone Regeneration in DentistryDokument5 SeitenBone Regeneration in Dentistryclaudia360Noch keine Bewertungen
- ImplantDokument46 SeitenImplantMosica VladNoch keine Bewertungen
- Dental Implant OsseointegrationDokument12 SeitenDental Implant Osseointegrationdrgayen6042Noch keine Bewertungen
- 5 SmartBone 2019 Paper Tibial Plateu FracturesDokument11 Seiten5 SmartBone 2019 Paper Tibial Plateu FracturesachmadaNoch keine Bewertungen
- Influence of A Novel Surface of Bioactive Implants On OsseointegrationDokument14 SeitenInfluence of A Novel Surface of Bioactive Implants On OsseointegrationalinagaxiolaariasNoch keine Bewertungen
- Gallium and Silicon Synergistically Promote Osseointegration of Dental Implant in Patients With OsteoporosisDokument19 SeitenGallium and Silicon Synergistically Promote Osseointegration of Dental Implant in Patients With OsteoporosisMughalNoch keine Bewertungen
- Biomedicine & Pharmacotherapy: Zhou-Shan Tao, Wan-Shu Zhou, Hong-Guang Xu, Min YangDokument11 SeitenBiomedicine & Pharmacotherapy: Zhou-Shan Tao, Wan-Shu Zhou, Hong-Guang Xu, Min YangrosanaNoch keine Bewertungen
- Arslan, Elif Ekiz, Melis Sardan Cimenci, Cagla Eren Can, Nura - Protective Therapeutic Effects of Peptide Nanofiber and HyDokument42 SeitenArslan, Elif Ekiz, Melis Sardan Cimenci, Cagla Eren Can, Nura - Protective Therapeutic Effects of Peptide Nanofiber and HyPearlin HameedNoch keine Bewertungen
- Untitled 4Dokument15 SeitenUntitled 4Satya AsatyaNoch keine Bewertungen
- Tissue-Engineered Bone RegenerationDokument5 SeitenTissue-Engineered Bone RegenerationElsa GonçalvesNoch keine Bewertungen
- SCAFFOLDS COMBINED WITH STEM CELLS AND GROWTH FACTORS IN RECONSTRUCTION OF LARGE BONE DEFECTS. Rodolfo Capanna, Pietro de BiaseDokument7 SeitenSCAFFOLDS COMBINED WITH STEM CELLS AND GROWTH FACTORS IN RECONSTRUCTION OF LARGE BONE DEFECTS. Rodolfo Capanna, Pietro de BiaseNuno Craveiro LopesNoch keine Bewertungen
- 10 1002@cap 10141Dokument25 Seiten10 1002@cap 10141Karla Yaneth Cardoza PeñaNoch keine Bewertungen
- Maturo GenesisDokument7 SeitenMaturo GenesisHanny HoneyyNoch keine Bewertungen
- Ajtr0009 3200Dokument13 SeitenAjtr0009 3200iam_ca2Noch keine Bewertungen
- Implant Platforn SwitchingDokument6 SeitenImplant Platforn SwitchingJeary VargasNoch keine Bewertungen
- Bone and Connective TissueDokument20 SeitenBone and Connective TissueKarka PalmaNoch keine Bewertungen
- Bone Regeneration: Current Concepts and Future Directions: Review Open AccessDokument10 SeitenBone Regeneration: Current Concepts and Future Directions: Review Open AccessBianca Ionela DraganNoch keine Bewertungen
- Biology of Rotator Cuff HealingDokument10 SeitenBiology of Rotator Cuff HealingRaeni Dwi PutriNoch keine Bewertungen
- Brandusa 1Dokument7 SeitenBrandusa 1Iacob RoxanaNoch keine Bewertungen
- Pharmaceutical Nano TechnologyDokument20 SeitenPharmaceutical Nano TechnologyHarishNoch keine Bewertungen
- Ridge Preservation Using Composite AlloplasticDokument8 SeitenRidge Preservation Using Composite Alloplasticarun perioNoch keine Bewertungen
- Occlusal Overload With Dental Implants: A ReviewDokument5 SeitenOcclusal Overload With Dental Implants: A ReviewEmre TezulasNoch keine Bewertungen
- 17 2.1 去铁胺对骨质疏松小鼠骨血管和骨量的协同保护作用。Dokument8 Seiten17 2.1 去铁胺对骨质疏松小鼠骨血管和骨量的协同保护作用。YilinNoch keine Bewertungen
- Journal - 620 Stress-Diversion Surface SDS Dental Implant OriginalDokument28 SeitenJournal - 620 Stress-Diversion Surface SDS Dental Implant OriginalHamdani NurdinNoch keine Bewertungen
- Shapiro 2020Dokument4 SeitenShapiro 2020Alejandra LorancaNoch keine Bewertungen
- Osseointegration of Dental ImplantsDokument164 SeitenOsseointegration of Dental ImplantsjubinNoch keine Bewertungen
- Immediate Loading FaizDokument85 SeitenImmediate Loading FaizDrrksundar KumarNoch keine Bewertungen
- Review Paper An Overview of Scaffolds FoDokument5 SeitenReview Paper An Overview of Scaffolds FoHSE INTECHNoch keine Bewertungen
- Recurrent Giant Cell Tumour of Distal Tibia: Case Report and Review of The LiteratureDokument4 SeitenRecurrent Giant Cell Tumour of Distal Tibia: Case Report and Review of The LiteratureAMBS ABMS JMAANoch keine Bewertungen
- Strategies in Reconstruction of The Atrophic MaxillaDokument19 SeitenStrategies in Reconstruction of The Atrophic MaxillaEmil CorreaNoch keine Bewertungen
- 3D Culture of Osteoblast-Like Cells by Unidirectional or Oscillatory Flow For Bone Tissue EngineeringDokument9 Seiten3D Culture of Osteoblast-Like Cells by Unidirectional or Oscillatory Flow For Bone Tissue EngineeringLiu WenNoch keine Bewertungen
- Bisht2021 Article AdvancesInTheFabricationOfScafDokument23 SeitenBisht2021 Article AdvancesInTheFabricationOfScafOxy Dental Clinic MakassarNoch keine Bewertungen
- Bonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonDokument19 SeitenBonegraftingforimplant Surgery: Ladi Doonquah,, Pierre-John Holmes,, Laxman Kumar Ranganathan,, Hughette RobertsonJason LeeNoch keine Bewertungen
- Advanced 3D Magnetic Scaffolds For Tumor-Related BDokument30 SeitenAdvanced 3D Magnetic Scaffolds For Tumor-Related BCristina BancilaNoch keine Bewertungen
- Www.techTools.net - Www.thumperDC.comDokument1 SeiteWww.techTools.net - Www.thumperDC.comRade GrbićNoch keine Bewertungen
- 11LongChap78 Osteomyelitis PDFDokument14 Seiten11LongChap78 Osteomyelitis PDFMusculus PopliteusNoch keine Bewertungen
- Read Me!Dokument2 SeitenRead Me!Rade GrbićNoch keine Bewertungen
- Iftiarticleosteomyelitis PDFDokument11 SeitenIftiarticleosteomyelitis PDFRade GrbićNoch keine Bewertungen
- Week 5: Primary HemostasisDokument37 SeitenWeek 5: Primary HemostasisRade GrbićNoch keine Bewertungen
- Suicidal Attempts During The First Episode Psychosis: Ramunė Mazaliauskienė, Alvydas NavickasDokument4 SeitenSuicidal Attempts During The First Episode Psychosis: Ramunė Mazaliauskienė, Alvydas NavickasRade GrbićNoch keine Bewertungen
- Basic Facts About SchizophreniaDokument48 SeitenBasic Facts About SchizophreniaringbellsNoch keine Bewertungen
- ThrombosisDokument38 SeitenThrombosisDiana PanaitNoch keine Bewertungen
- Bleeding Disorders and TM 2014Dokument84 SeitenBleeding Disorders and TM 2014Rade GrbićNoch keine Bewertungen
- Paper WFMHDokument5 SeitenPaper WFMHRudianto AhmadNoch keine Bewertungen
- HemostasisDokument58 SeitenHemostasisRade GrbićNoch keine Bewertungen
- Fracturi de Coloana Cervicala, Toracala Si LombaraDokument770 SeitenFracturi de Coloana Cervicala, Toracala Si Lombaracomir2002100% (3)
- RSN 2016 Iss 84 MckinleyDokument5 SeitenRSN 2016 Iss 84 MckinleyRade GrbićNoch keine Bewertungen
- Skizofrenia 2 PDFDokument40 SeitenSkizofrenia 2 PDFIcvanBryliantNoch keine Bewertungen
- Sub Acute and Chronic OsteomielitisDokument26 SeitenSub Acute and Chronic OsteomielitisRade GrbićNoch keine Bewertungen
- Manejo de La EsquizofreniaDokument71 SeitenManejo de La Esquizofreniahp937Noch keine Bewertungen
- bdf0 PDFDokument25 Seitenbdf0 PDFRade GrbićNoch keine Bewertungen
- FINAL Depressive Disorders CD JUL2014Dokument5 SeitenFINAL Depressive Disorders CD JUL2014Rade GrbićNoch keine Bewertungen
- Psihijatrijski I Pravni Aspekti Prisilne Psihijatrijske HospitalizacijeDokument4 SeitenPsihijatrijski I Pravni Aspekti Prisilne Psihijatrijske HospitalizacijeRade Grbić100% (1)
- Bone and Joint InfectionDokument77 SeitenBone and Joint InfectiontitotamaNoch keine Bewertungen
- Tested and WorkingDokument1 SeiteTested and WorkingRade GrbićNoch keine Bewertungen
- Antioxidant in OsteoporosisDokument282 SeitenAntioxidant in OsteoporosisNisful Lail J. ANoch keine Bewertungen
- KP 3.2.5.4 Rachitis - Vit D Ricketsia - OsteomalaciaDokument72 SeitenKP 3.2.5.4 Rachitis - Vit D Ricketsia - OsteomalaciaMuhammad Mirdho ArfiNoch keine Bewertungen
- Osteopenia & Osteoporosis - Basic Science - Orthobullets PDFDokument5 SeitenOsteopenia & Osteoporosis - Basic Science - Orthobullets PDFMelAcostaNoch keine Bewertungen
- Basic Concepts of Growth and DevelopmentDokument40 SeitenBasic Concepts of Growth and DevelopmentMonojit Dutta100% (1)
- JAAOS - Volume 11 - Issue 01 January & February 2003Dokument77 SeitenJAAOS - Volume 11 - Issue 01 January & February 2003kenthepaNoch keine Bewertungen
- Pros Lec 1Dokument15 SeitenPros Lec 1ريام الموسويNoch keine Bewertungen
- Osteoporosis: Disease SummaryDokument10 SeitenOsteoporosis: Disease SummaryHohai ConcepcionNoch keine Bewertungen
- Chapter 5 The Skeletal SystemDokument47 SeitenChapter 5 The Skeletal SystemOlalekan OyekunleNoch keine Bewertungen
- Porose Gravidez e Puerperio 2021Dokument15 SeitenPorose Gravidez e Puerperio 2021Ben-Hur AlbergariaNoch keine Bewertungen
- Nanophase Ceramics: The Future Orthopedic and Dental Implant MaterialDokument42 SeitenNanophase Ceramics: The Future Orthopedic and Dental Implant MaterialDario Bejarano RojasNoch keine Bewertungen
- Full PDFDokument6 SeitenFull PDFChuco HarrisonNoch keine Bewertungen
- Introduction To OrthopaedicsDokument40 SeitenIntroduction To OrthopaedicsAnonymous 9zN5Ag8iee50% (2)
- Calcium Metabolism - WordDokument40 SeitenCalcium Metabolism - WordVineela ChowdaryNoch keine Bewertungen
- DenosumabDokument2 SeitenDenosumabMahdy AlShammariNoch keine Bewertungen
- Case Osteoarthritis NewDokument33 SeitenCase Osteoarthritis NewQueenie P. Manalo67% (3)
- B. Cyclophtsphamide C. Oprelvekin (For Thrombocytopenia) : Chlamydia Treated by ADELA (AzithromycinDokument28 SeitenB. Cyclophtsphamide C. Oprelvekin (For Thrombocytopenia) : Chlamydia Treated by ADELA (AzithromycinEmadSamirNoch keine Bewertungen
- Chapter 44 Alteration in Musculoskeletal FunctionDokument11 SeitenChapter 44 Alteration in Musculoskeletal FunctionromiNoch keine Bewertungen
- NCM 116 Midterm PDFDokument130 SeitenNCM 116 Midterm PDFPonciana PasanaNoch keine Bewertungen
- Hypercalcemia in Dogs Emergent Care Diagnostics and TreatmentsDokument8 SeitenHypercalcemia in Dogs Emergent Care Diagnostics and Treatmentstarilubis277Noch keine Bewertungen
- Trauma IçerikDokument32 SeitenTrauma Içerikkocaeli ortopediNoch keine Bewertungen
- Endokrin (1) - TerkunciDokument25 SeitenEndokrin (1) - TerkuncihafizauliaNoch keine Bewertungen
- Quizlet EndoDokument17 SeitenQuizlet EndoemmaNoch keine Bewertungen
- Presented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsDokument21 SeitenPresented by Dr. K. M. Rukhshad Asif Zaman Khan Department of Orthodontics and Dentofacial OrthopaedicsRukshad Asif Jaman KhanNoch keine Bewertungen
- Bone Biomechanics - AgingDokument59 SeitenBone Biomechanics - AgingpupuliciouzNoch keine Bewertungen
- Chemistry Project On Estimation of Contant of Bone Ash PDFDokument9 SeitenChemistry Project On Estimation of Contant of Bone Ash PDFPooja BhagwatNoch keine Bewertungen
- Secondary OsteoporosisDokument22 SeitenSecondary OsteoporosisBenny Chris TantoNoch keine Bewertungen
- Assessment of Bone Turnover Markers in Stages of Facture HealingDokument8 SeitenAssessment of Bone Turnover Markers in Stages of Facture Healingijmb333Noch keine Bewertungen
- Renal PhysioDokument140 SeitenRenal Physioarturo quevedoNoch keine Bewertungen