Beruflich Dokumente
Kultur Dokumente
Decreased Urine Out Put
Hochgeladen von
Hila Amalia0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
71 Ansichten11 Seitenurologi
Copyright
© © All Rights Reserved
Verfügbare Formate
PPT, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenurologi
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
71 Ansichten11 SeitenDecreased Urine Out Put
Hochgeladen von
Hila Amaliaurologi
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 11
Artak Labadzhyan
Mini-Lecture Powerpoints
1/30/12
Definition of decreased urine output
(oliguria)
Questions to consider when first presented
with oliguria
Recognizing causes of oliguria
Focused review of history and physical
Management of oliguria
Recognizing life threatening complications
Oliguria = Urine output <400cc/day
(<20cc/hr)
Another def: urine output <0.5ml/kg/hr
Anuria = no urine output
Can signify complete mechanical obstruction of
bladder outlet or a blocked Foley
Does the pt have a foley catheter?
NO
YES
FLUSH FOLEY CATHETER
WITH 30-50CC NS
OBTAIN PVR (w/ US or cath
[will provide urine sample])
URINE OUTPUT IMPROVED?
PVR 100? ( 50 in younger pts)
YES
FOLEY LIKELY
CLOGGED
WITH
SEDIMENT
NO
PROCEDE
WITH
FURTHER
MANAGEMENT
YES
START FOLEY
& PROCEDE W/
FURTHER
MANAGEMENT
NO
PROCEED
WITH
FURTHER
MANAGEMENT
Consider the pathophysiology/causes of decreased
urine output. Three categories of causes:
Prerenal:
Volume depletion/dehydration/inadequate fluid
maintenance/Infection/sepsis
Reduced cardiac output
ICU setting: mechanical ventilation can also lead to low cardiac
output
Drugs
Does the pt have liver cirrhosis
Intrarenal:
ATN
ICU settings: Circulator shock, severe sepsis, multiorgan failure
AIN
Renal artery thrombosis/Emboli (septic [endocarditis]
Postrenal:
B/l ureteric obstruction (stones, clots, tumors, fibrosis)
Bladder outlet obstruction (BPH, tumors/retroperitoneal
mass, clots)
Foley catheter obstruction
Review chart to look for clues that may elicit
etiology (see previous slide)
History (sepsis, CHF, tumors, renal failure
etc)
Meds: diuretics, ace,
aminoglycosides/vancomycin, iv contrast,
NSAIDs
Old Labs: BUN/Cr (ratio); urine lytes; blood
cultures; vanco trough levels
Obtain new vitals, including orthostatics
Look for:
Jaundice
Crackles, pleural effusion
JVP, CVP if pt has central line
Especially useful in ICU for pt with central line:
for example a CVP of 2 can be good evidence
for hypovolemia
Palpate Kidneys and Bladder
Prostate/Cervical Exam
Rash
If not already done, order basic electrolytes,
CMP (monitor changes in Cr/GFR), and urine
studies (U/A, Na, BUN, Cr), to further help
classify etiology
Adjust/replace/discontinue and nephrotoxic
agents. Also, renally dose the non-toxic
meds
Early recognition and intervention of
potential life threatening complications
(direct or indirect causes e.g. renal
failure) is essential
Hyperkalemia: obtain EKG if elevated
CHF/Pulmonary Edema
Metabolic acidosis; Uremia (encephalopathy,
pericarditis)
Advanced complications of above may require
dialysis
Prerenal:
Treat underlying cause
If volume depleted (see physical exam): NS boluses
(500-1000ml fluid challenges) can repeat until
response (but need to monitor for fluid overload)
Avoid/be very cautious about giving lasix (again
investigation of underlying cause should drive this
decision).
Postrenal:
Treat underlying cause
Initiate Foley catheter (clear/flush catheter if already
in place)
Obtain Renal Ultrasound to assess for upper urinary
tract problems
Intrarenal:
Treat underlying causes (e.g. sever sepsis/shock)
Verify urine output w/ definition of oliguria in mind.
If pt has a Foley catheter, flushing Foley is a good initial
step. If no Foley, a PVR can help assess the need for
Foley.
A focused chart review along with a focused history and
physical can help clue in on the pathophysiology
including pre-renal/intrinsic/post-renal causes.
Recognizing life threatening complications (e.g.
hyperkalemia, acidosis, uremia) is an essential
component of acute/early management.
Decreased urine output does NOT mean lasix deficiency.
Administering lasix may actually exacerbate problem.
However very specific causes may require lasix.
Fluid boluse(s) is a good initial step (be very cautious in
CHF).
Ultimately, regardless of pathophysiology, treating
underlying cause is key for both acute and long term
management.
Das könnte Ihnen auch gefallen
- Fluid and Electrolytes for Nursing StudentsVon EverandFluid and Electrolytes for Nursing StudentsBewertung: 5 von 5 Sternen5/5 (12)
- Renal ReviewDokument23 SeitenRenal ReviewRaven Atisha100% (1)
- Intestinal Obstruction: Zeeshan Razzaq MRCS Ire, MRCS Ed, MRCS Eng Colorectal RegistrarDokument61 SeitenIntestinal Obstruction: Zeeshan Razzaq MRCS Ire, MRCS Ed, MRCS Eng Colorectal Registraraini natashaNoch keine Bewertungen
- Intestinal ObstructionDokument52 SeitenIntestinal ObstructionAsfandyar Khan100% (2)
- Ascites, A Simple Guide To The Condition, Treatment And Related ConditionsVon EverandAscites, A Simple Guide To The Condition, Treatment And Related ConditionsNoch keine Bewertungen
- Necessary Elements of A Dermatologic History and Physical Evaluation PDFDokument9 SeitenNecessary Elements of A Dermatologic History and Physical Evaluation PDFkyle31Noch keine Bewertungen
- Genito Urinary SystemDokument106 SeitenGenito Urinary Systemnursereview88% (8)
- Medical and Surgical NursingDokument4 SeitenMedical and Surgical NursingCrystal Ann Monsale TadiamonNoch keine Bewertungen
- Acute Renal FailureDokument30 SeitenAcute Renal FailureJerinNoch keine Bewertungen
- Genitourinary System: Billy Ray A. Marcelo, RNDokument35 SeitenGenitourinary System: Billy Ray A. Marcelo, RNDarell M. BookNoch keine Bewertungen
- Anatomy and Introduction CKD KidneyDokument39 SeitenAnatomy and Introduction CKD KidneySwatin ShettyNoch keine Bewertungen
- Epidemiology of Infectious DiseasesDokument69 SeitenEpidemiology of Infectious Diseasesmus zaharaNoch keine Bewertungen
- Renal Nursing - HandoutDokument16 SeitenRenal Nursing - HandoutJoms Kim Mina100% (3)
- DehydrationDokument14 SeitenDehydrationReimer LaquihuanacoNoch keine Bewertungen
- Grand Rounds Facial Nerve ParalysisDokument86 SeitenGrand Rounds Facial Nerve ParalysisA170riNoch keine Bewertungen
- Acute Biologic CrisisDokument143 SeitenAcute Biologic CrisisAprylL22100% (5)
- Urinary Catheter Placement For Feline ObstructionDokument6 SeitenUrinary Catheter Placement For Feline ObstructionWilliam ChandlerNoch keine Bewertungen
- Acute Renal Failure Nursing Care PlanDokument15 SeitenAcute Renal Failure Nursing Care PlanRanusha AnushaNoch keine Bewertungen
- Acute Renal FailureDokument13 SeitenAcute Renal FailureGlorianne Palor100% (2)
- Internal Medicine Boot Camp Sessions M. JunaidDokument21 SeitenInternal Medicine Boot Camp Sessions M. Junaidmjmd246Noch keine Bewertungen
- Chole CystitisDokument61 SeitenChole CystitisPlain GerlNoch keine Bewertungen
- Epigastric Pain AssignmentDokument3 SeitenEpigastric Pain AssignmentLauren EnglerNoch keine Bewertungen
- Alteration in Urinary System - ppt22222Dokument117 SeitenAlteration in Urinary System - ppt22222yen1988Noch keine Bewertungen
- Chronic Renal FailureDokument26 SeitenChronic Renal FailurePriya GandhiNoch keine Bewertungen
- Gagal GinjalDokument75 SeitenGagal GinjalAndi HeriantoNoch keine Bewertungen
- Acute Abdomen: Part I: Intestinal Obstruction/Bowel Infarction/ Constipation (And How To Assess and Initiate Management)Dokument63 SeitenAcute Abdomen: Part I: Intestinal Obstruction/Bowel Infarction/ Constipation (And How To Assess and Initiate Management)Rumana IslamNoch keine Bewertungen
- Acute Renal Failure Lecture 1 Critical Care NursingDokument52 SeitenAcute Renal Failure Lecture 1 Critical Care NursingDina Rasmita100% (2)
- Genito Urinary SystemDokument8 SeitenGenito Urinary SystemPinky CuaresmaNoch keine Bewertungen
- Acute Renal Failure8Dokument35 SeitenAcute Renal Failure8Andrew MidaNoch keine Bewertungen
- 099 - Acute Renal Failure - Di PDFDokument2 Seiten099 - Acute Renal Failure - Di PDFSetiya Dini LarasatiNoch keine Bewertungen
- Dialysis: Presented By: Pallavi Shukla Khushbu RathoreDokument15 SeitenDialysis: Presented By: Pallavi Shukla Khushbu RathoreKrishnaBihariShuklaNoch keine Bewertungen
- Balance Cairan Final.Dokument41 SeitenBalance Cairan Final.Niqko Bayu PrakarsaNoch keine Bewertungen
- Gangguan Ginjal AkutDokument29 SeitenGangguan Ginjal Akutb3djo_76Noch keine Bewertungen
- Indications of Dialysis in Acute Renal Failure (ARF)Dokument3 SeitenIndications of Dialysis in Acute Renal Failure (ARF)Tariku GelesheNoch keine Bewertungen
- Diarrhea and DehydrationDokument12 SeitenDiarrhea and DehydrationnikprovNoch keine Bewertungen
- Renal Disorders 1Dokument73 SeitenRenal Disorders 1Kyla PamaNoch keine Bewertungen
- Renal PhysiologyDokument5 SeitenRenal PhysiologyJayricDepalobosNoch keine Bewertungen
- What Causes Fluid Overloa1Dokument5 SeitenWhat Causes Fluid Overloa1Norine_Barrios_2887Noch keine Bewertungen
- Diagnostic TestsDokument5 SeitenDiagnostic TestsCristina L. JaysonNoch keine Bewertungen
- Acute Renal FailureDokument3 SeitenAcute Renal FailureJimae Rose BaculaNoch keine Bewertungen
- Aki NotesDokument10 SeitenAki NotesGennel Mae GarovilloNoch keine Bewertungen
- SimulationDokument5 SeitenSimulationJessFriend100% (1)
- Emskfjek-Intravenous IV Fluid Prescribing in AdultsDokument14 SeitenEmskfjek-Intravenous IV Fluid Prescribing in AdultsAli SemajNoch keine Bewertungen
- Acute Renal Failure & Chronic Renal FailureDokument38 SeitenAcute Renal Failure & Chronic Renal FailureArti GondNoch keine Bewertungen
- Hyperkalaemia: See Also BackgroundDokument6 SeitenHyperkalaemia: See Also BackgroundamaliaNoch keine Bewertungen
- Fluid Student 2012Dokument43 SeitenFluid Student 2012Sara Ilyas KhanNoch keine Bewertungen
- An Interesting Case When Proper Clnical Evaluation Matters MostDokument48 SeitenAn Interesting Case When Proper Clnical Evaluation Matters MostDr. KENNETH N. ORIMMANoch keine Bewertungen
- Pedoman Tatalaksana Sindrom Koroner Akut 2015Dokument29 SeitenPedoman Tatalaksana Sindrom Koroner Akut 2015Vittorio bagscenterNoch keine Bewertungen
- Fluid and Electrolytes: Robert Mcintyre, Jr. Associate Professor of Surgery University of Colorado Health Sciences CenterDokument54 SeitenFluid and Electrolytes: Robert Mcintyre, Jr. Associate Professor of Surgery University of Colorado Health Sciences CenterWilliam Yap WLNoch keine Bewertungen
- CirrhosisDokument10 SeitenCirrhosisJames FlanneryNoch keine Bewertungen
- General Clinical ManifestationsDokument17 SeitenGeneral Clinical ManifestationsYohannis AsefaNoch keine Bewertungen
- Renal FailureDokument11 SeitenRenal FailureRashed ShatnawiNoch keine Bewertungen
- Renal Replacement Therapy HandoutDokument4 SeitenRenal Replacement Therapy HandoutAsdzxcNoch keine Bewertungen
- GIT Bleeding PSIKDokument28 SeitenGIT Bleeding PSIKYanto RiyantoNoch keine Bewertungen
- Alterations in Fluid VolumeDokument4 SeitenAlterations in Fluid VolumeRichmund Earl GeronNoch keine Bewertungen
- Brain Dump NUR 213 FINALDokument37 SeitenBrain Dump NUR 213 FINALkelsey jackson100% (1)
- Acute Kidney Injury and Chronic Kidney DiseaseDokument44 SeitenAcute Kidney Injury and Chronic Kidney DiseaseshihochanNoch keine Bewertungen
- Gallstone Disease and Acute CholecystitisDokument21 SeitenGallstone Disease and Acute CholecystitisTheresia Merdeka PutriNoch keine Bewertungen
- Universal Algorithm (According To The European Conference 2000)Dokument11 SeitenUniversal Algorithm (According To The European Conference 2000)Pawan MishraNoch keine Bewertungen
- Acute Kidney Injury: DR Hodan Ahmed Dept of Pediatrics and Child Health Amoud Medical School, AUDokument32 SeitenAcute Kidney Injury: DR Hodan Ahmed Dept of Pediatrics and Child Health Amoud Medical School, AUMohamoud MohamedNoch keine Bewertungen
- MCI One Pager Version 1.0 Oct 2020Dokument1 SeiteMCI One Pager Version 1.0 Oct 2020naval730107Noch keine Bewertungen
- Hip Resurfacing Expectations and LimitationsDokument4 SeitenHip Resurfacing Expectations and LimitationsCristian BenayNoch keine Bewertungen
- Foensic Vol-1 BookDokument149 SeitenFoensic Vol-1 Booksayenshan0205Noch keine Bewertungen
- FC Continuous Education Microcredentials July 2021 (3354)Dokument9 SeitenFC Continuous Education Microcredentials July 2021 (3354)Luis Peralta GuzmanNoch keine Bewertungen
- DNRDokument1 SeiteDNRabiangdanNoch keine Bewertungen
- Approach To Nursing Assessment 1Dokument5 SeitenApproach To Nursing Assessment 1Taiye OkondoNoch keine Bewertungen
- Pediatrics PDFDokument33 SeitenPediatrics PDFChellapandyaNoch keine Bewertungen
- Ludwig Heinrich Bojanus (1776-1827) On Gall's Craniognomic System, Zoology - UnlockedDokument20 SeitenLudwig Heinrich Bojanus (1776-1827) On Gall's Craniognomic System, Zoology - UnlockedJaime JaimexNoch keine Bewertungen
- FDG PET - CT-based Response AssessmentDokument17 SeitenFDG PET - CT-based Response AssessmentHelen MejiaNoch keine Bewertungen
- Rachael Stanton Resume Rachael Stanton LVT 1 2Dokument2 SeitenRachael Stanton Resume Rachael Stanton LVT 1 2api-686124613Noch keine Bewertungen
- Daftar PustakaDokument2 SeitenDaftar PustakaErick PrasetyaNoch keine Bewertungen
- Down Screen Proposal For Health Screen at Thyrocare AmitDokument19 SeitenDown Screen Proposal For Health Screen at Thyrocare AmitSwatiSuranaNoch keine Bewertungen
- 1st Floor No 105 Above Raymonds Opp Medical College Koti: SHARMA Bpo SupportDokument4 Seiten1st Floor No 105 Above Raymonds Opp Medical College Koti: SHARMA Bpo SupportMK Musthafa GudalurNoch keine Bewertungen
- Stylohyoid LigamentDokument4 SeitenStylohyoid LigamentArindom ChangmaiNoch keine Bewertungen
- Dengue Outbreak Declared in CaviteDokument5 SeitenDengue Outbreak Declared in CaviteDoc AlexNoch keine Bewertungen
- Permintaan Lab 2023Dokument9 SeitenPermintaan Lab 2023imanNoch keine Bewertungen
- CXL Te Istanbul 2011Dokument59 SeitenCXL Te Istanbul 2011Ana_BiosooftNoch keine Bewertungen
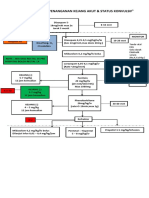
- Algoritma Penanganan Kejang AkutDokument1 SeiteAlgoritma Penanganan Kejang AkutEwa ClaudiaNoch keine Bewertungen
- Maklumat Vaksinasi: Vaccination DetailsDokument2 SeitenMaklumat Vaksinasi: Vaccination DetailsNORFADHLI ARIFNoch keine Bewertungen
- HEPADNAVIRIDAEDokument14 SeitenHEPADNAVIRIDAEnur qistina humaira zulkarshamsiNoch keine Bewertungen
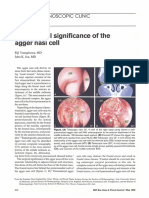
- Agger NasiDokument3 SeitenAgger NasiDr Saikat SahaNoch keine Bewertungen
- AJHP Pharmacy Forecast 2018-3Dokument32 SeitenAJHP Pharmacy Forecast 2018-3tpatel0986Noch keine Bewertungen
- Mangalam Drugs ReportDokument1 SeiteMangalam Drugs ReportBKSNoch keine Bewertungen
- GMMMC Sukkur MbbsDokument6 SeitenGMMMC Sukkur MbbsSherazAhmedNoch keine Bewertungen
- Blood CirculationDokument42 SeitenBlood CirculationAshu kumar100% (1)
- Practice Worksheet Class XiiDokument7 SeitenPractice Worksheet Class XiiManjusha NayakNoch keine Bewertungen
- Inappropriate Sinus TachycardiaDokument23 SeitenInappropriate Sinus TachycardiaOnon EssayedNoch keine Bewertungen