Beruflich Dokumente
Kultur Dokumente
Sinul
Hochgeladen von
Cucos Natalia0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
109 Ansichten38 SeitenThis document provides an overview of breast anatomy relevant to plastic surgery. It describes the borders and components of the breast, including parenchyma, Cooper's ligaments, the nipple-areolar complex, vascular supply, lymphatics, innervation, and associated musculature. Gynecomastia, the enlargement of male breast tissue, is also briefly discussed.
Originalbeschreibung:
breast
Originaltitel
sinul
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenThis document provides an overview of breast anatomy relevant to plastic surgery. It describes the borders and components of the breast, including parenchyma, Cooper's ligaments, the nipple-areolar complex, vascular supply, lymphatics, innervation, and associated musculature. Gynecomastia, the enlargement of male breast tissue, is also briefly discussed.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
109 Ansichten38 SeitenSinul
Hochgeladen von
Cucos NataliaThis document provides an overview of breast anatomy relevant to plastic surgery. It describes the borders and components of the breast, including parenchyma, Cooper's ligaments, the nipple-areolar complex, vascular supply, lymphatics, innervation, and associated musculature. Gynecomastia, the enlargement of male breast tissue, is also briefly discussed.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 38
Breast ( anatomy, reduction,
tuberous breast deformity,
gynecomastia)
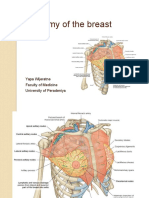
Anatomy for plastic surgery of the breast
Parenchymal borders:
• Superior border: clavicle
• Medial border: sternum
• Inferior border: inframammary
fold
• Lateral border: anterior border
of the latissimus dorsi
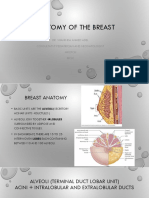
Parenchyma
• The functioning parenchyma produces milk in the post-partum
period. Adipose tissue comprises a significant amount of the
breast volume, representing 50–70% of the breast volume.
• With age and the hormonal changes of menopause, the
glandular tissue of the breast involutes, increasing the adipose
to parenchymal tissue ratio.
• The Cooper’s ligaments provide
numerous interconnections between
the deep and superficial fascial layers.
These ligaments pass through ad
invest in the breast parenchyma
securing to the pectoralis fascia. With
attenuation of these support structures,
breast ptosis will develop.
Nipple areola complex
• The nipple areola complex is the primary
landmark of the breast.
• The nipple itself may project as much as
≥1 cm, with a diameter of approximately
4–7 mm.
• The areola consists of pigmented skin
surrounding the nipple proper and is on
average approximately 4.2–4.5 cm in
diameter.
• The areola consists of keratinized,
stratified epithelium and contains not only
the lactiferous sinus openings, but also
sebaceous glands and the Montgomery
glands.
• Deep to the nipple and areolar there are
smooth muscle fibers which are arranged
circumferentially and radially. These
fibers are attached to the thick
connective tissue of the areola and are
responsible for nipple erection.
Vascularity
• The breast has a rich vascular supply
from multiple arterial sources.
• The primary arterial supply includes
three main sources: the internal
mammary perforators, lateral thoracic
artery and the anterolateral intercostal
perforators.
• Additional arterial supply includes the
thoracoacromial artery and its perforators
and the vessels of the serratus anterior.
• The internal mammary perforators enter
the superior medial portion of the breast
via the second through sixth intercostal
spaces. The second and third perforators
are the predominant of these perforating
vessels. Because of their larger caliber
the second or third perforators are the
preferred recipient vessels for free tissue
reconstruction using the internal
mammary perforators.
• Supplying the superolateral aspect
of the breast is the lateral thoracic
or external mammary artery. This
vessel is a primary branch of the
axillary artery and enters the
breast after passing around the
lateral border of the pectoralis
major muscle at the inferior aspect
of the axilla. It distributes its
branches in the upper outer
quadrant of the breast.
• The lateral intercostal vessels
represent an additional important
blood supply of the breast. The
lateral breast receives anterior
intercostal arteries from the third
through sixth interspaces. These
vessels perforate the serratus
anterior just lateral to the pectoral
border. Lateral intercostal vessels
enter the breast at the anterior
margin of the latissimus dorsi to
supply the lateral breast and
overlying skin.
• Medial intercostal perforators are
responsible for direct supply of the
inferior central portion of the breast
inferior to the nipple areolar
complex.
• Venous drainage of the breast is via
two systems. The subdermal venous
plexus above the superficial fascia is
quite variable and represents the
superficial system. The veins arise
from the periareolar venous plexus
within the parenchyma, the
superficial systems anastomose with
the deep system. The deep system
parallels the arterial supply with the
veins paired to their respective
arteries. Venous perforators following
the internal mammary perforators
drain via the internal mammary vein
to the innominate vein. The lateral
thoracic veins drain via the azygos
vein into the superior vena cava.
• Vascular anatomy is also of importance with regard to the recipient site for microvascular
anastomosis when free tissue transfer is used for breast reconstruction.
• The thoracodorsal vessels have been used, particularly when the reconstruction is immediately
postmastectomy. The thoracodorsal artery is often small (<2 mm) and may have insufficient flow.
The axillary vessels can be technically difficult for the assistant, since they must operate across
the chest. In addition, the axillary system may limit flap movement and shaping the breast.
• The use of the internal mammary vessels as a recipient site facilitates shaping the medial portion
of the breast. However, the technique requires partial rib resection and eliminates the opportunity
for a potential coronary artery bypass graft.
• The internal mammary vessel may be preferred in delayed cases, especially in patients who
have had adjuvant radiation, as dissection of axillary vessels can be very difficult.
Lymphatics
• The predominance of lymph
drainage of the breast is via the
interlobular lymphatic vessels to the
subareolar plexus. Lymph is
directed toward the axillary lymph
nodes.
• This drainage is parallel to the
venous drainage of the breast.
Lateral lymphatics course around
the edge of the pectoralis major
toward the pectoral lymph nodes.
Additional lymphatics course
through the pectoral muscles to the
apical lymph nodes. From the
axillary lymph nodes, lymph drains
into the subclavian and
supraclavicular lymph nodes.
Innervation
• Sensory innervation has three
major nerve distributions which
include the anterior lateral
intercostals, the medial intercostals,
and the cervical plexus.
• The anterior rami of the lateral
cutaneous nerves of the
intercostals provide sensation to
the lateral portion of the breast
extending to and including the
nipple areolar complex. The breast
demonstrates a dermatomal pattern
derived from the anterolateral and
anteromedial branches of the
intercostal nerves (T3–T5).
• Branches of the cervical plexus
provide the superior medial sensory
innervation.
• Intercostal segmental nerves
contribute the remainder of the
breast sensation and can be
considered the primary sensory
nerves. The third through sixth
anterolateral intercostal nerves pass
through the interdigitations of the
serratus muscles to enter the lateral
aspect of the breast.
• Along the medial border of the
breast, the second through sixth
anteromedial intercostal nerves
enter the breast parenchyma
alongside the internal mammary
perforating vessels. These sensory
nerves provide innervation to the
medial breast and nipple areolar
complex.1
Musculature
• The muscles directly
associated with the breast
include the pectoralis major,
serratus anterior, external
oblique and the superior
portion of the rectus
abdominis
Pectoralis major
• Origin- medial clavicle and lateral
sternum
• Insertion- on the humerus
• Blood suplly: toracoacromial artery;
intercostal perforators from the internal
mammary artery
• Inervation: medial and lateral anterior
thoracic nerves
• Action: flex; adduct and rotate the arm
medially.
• The pectoralis major is extremely
important in both aesthetic and
reconstructive breast surgery, since
it provides muscle coverage for the
breast implant
Serratus anterior
• Origin is the outer surface of the upper borders of
the first through eighth ribs
• Insertion is on the deep surface of the scapula
• Vascular supply is derived equally from the
lateral thoracic artery and branches from the
thoracodorsal artery
• The long thoracic nerve serves to innervate the
serratus anterior, which acts to rotate the
scapula, raising the point of the shoulder and
drawingthe scapula forward toward the body.
• Because the serratus anterior underlies the
lateral aspect of the breast, in aesthetic surgery,
blunt elevation of the pectoralis major laterally
inadvertently elevates a small portion of the
serratus muscle. To completely cover the implant
with muscle in reconstructive surgery, often the
serratus anterior must be elevated sharply to
obtain a sufficient muscle layer to provide
coverage.
Rectus abdominis
• Origin at the crest of the pubis
and interpubic ligament to its
insertion at the xiphoid process
and cartilages of the fifth through
seventh ribs.
• It acts to compress the abdomen
and flex the spine
• When placing an implant for
breast reconstruction, in
attempting to achieve complete
coverage with muscle, the rectus
fascia must often be elevated to
place the implant sufficiently
caudal.
External oblique
• Its origin is from the lower eight ribs, and its insertion
is along the anterior half of the iliac crest and the
aponeurosis of the linea alba from the xiphoid to the
pubis
• It acts to compress the abdomen, flex and laterally
rotate the spine, and depress the ribs.
• Elevated along with the rectusabdominis fascia to
provide inferior coverage of the breast implant during
reconstructive surgery
• In aesthetic surgery, placement of the implant
inferiorly is usually not below these fascial
attachments. If the implant is placed behind the
fascia, the implant often “rides too high” and may
result in a “double bubble” effect, wherein the breast
parenchyma slides over and off the implant
Gynecomastia
Gynecomastia
• Gynecomastia is enlargement of the male breast
and is caused by an increase in ductal tissue,.
stroma, and/or fat. Most frequently, the changes
occur at the time of hormonal change: infancy,
adolescence, and old age.
• The most common cause of gynecomastia is
unknown (idiopathic).
• In all three age groups (neonatal, adolescent,
and older men), gynecomastia appears to be
related to either an increase in estrogens, a
decrease in androgens, or a deficit in androgen
receptors.
• The incidence of gynecomastia rises again in
older men (age > 65 years).
COMMON CAUSES OF GYNECOMASTIA
DIAGNOSIS
PATHOLOGY
• A careful history and physical examination
• Three types of gynecomastia is the most important part of any workup
have been described: florid, for gynecomastia.
fibrous, and intermediate. The
6
• The history notes the time of onset of the
gynecomastia, symptoms associated with
florid type is characterized by an the gynecomastia, drug use.
increase in ductal tissue and • Physical examination includes assessment
vascularity. of the breast gland and includes the nature
of the tissue, isolated masses, and
• The fibrous type has more tenderness. The thyroid is evaluated for
stromal fibrosis with few ducts. enlargement. The testes are examined for
asymmetry, masses, enlargement, or
• The intermediate type is a atrophy.
mixture of the two. • Laboratory evaluation is based on the
findings of the history and physical
examination
CLASSIFICATION
Simon, Hoffman, and Kahn divided gynecomastia into four grades:
1
grade 1: small enlargement, no skin excess
grade 2 a: moderate enlargement, no skin excess
b: moderate enlargement with extra skin
grade 3: marked enlargement with extra skm
Letterman and Schuster' created a classification system based on the
type of correction:
1: intra-areolar incision with no excess skin
2: intra-areolar incision with mild redundancy corrected with
excision of skin
through a superior periareolar scar
3: excision of chest skin with or without shifting the nipple.
Rohrich et al.,in a paper discussing the utility of ultrasound-assisted liposuction
in the treatment of gynecomastia, developed the following classification
grade I: minimal hypertrophy (<250 g of breast tissue) without ptosis
grade II: moderate hypertrophy (250 to 500 g of breast tissue) without ptosis
grade III: severe hypertrophy (>500 g breast tissue) with grade I ptosis
grade IV: severe hypertrophy with grade II or III ptosis
TREATMENT OF GYNECOMASTIA
• The goal of surgery is:
- to remove the excess breast tissue and skin,
- ensure adequate positioning of the nipple-areola complex,
- ensure symmetry between the breasts and chest wall,
- to avoid significant scarring
• Most fibrous or solid Simon stage 1 or 2a lesions are treated
with surgical excision or more recently, in selected cases, with
ultrasonic liposuction:with sharp tip cannulas, power-assisted
liposuction, or ultrasound-assisted liposuction.
• If surgical excision is chosen, a periareolar incision is
performed.
• The skin incision is placed at the junction of the areola and skin.
• After the incision is made, a cuf of tissue 1 to 1.5 an in
thickness is preserved directly deep to the nipple/areola
complex. This maneuver prevents postoperative nipple/areola
depression or adherence of the nipple/areola to the chest wall.
• When liposuction is unsuccessful at
removing all of the tissue required to
achieve a good result, the pull-through
technique is added.
• In this technique, either the lateral or
periareolar incision is opened slightly
(about 1.5 em) and the residual tissue is
grasped. The tissue is pulled out through
the wound and removed with scissors or
electrocautery. The pull-through
resection is performed until the desired
contour is achieved.
• All patients are treated with compression
garments for at least 1 month
COMPLICATIONS
• Complications include inadequate resection, overresection, excess
skin, complex scars, hematoma, seroma, partial nipple necrosis, suture
line dehiscence, pain, loss of nipple sensation, and infection.
• Potential risks of ultrasonic liposuction include thermal burns and skin
necrosis, because one of the byproducts of ultrasonic energy is heat.
• This is avoided by using cool towels over the skin and avoiding
superficial planes near the skin surface.
TUBEROUS BREAST
DEFORMITY
• Tuberous breast deformity describes a spectrum of aberrant breast
morphology first reported by Rees and Aston
• There are several features of the tuberous breast that are important to
identify before management. These include a constricted base,
contraction of the skin envelope, relative micromastia, enlarged
diameter of the nipple-areola complex and herniation of breast
parenchyma through the nipple-areola complex.
• Although the exact etiology has not
been elucidated, it is generally
accepted that this disorder has an
embryologic origin.Most reports have
speculated that the superficial
investing fascia of the breast is
abnormal and constricted at the base
of the breast. This constriction at the
base and deficiency at the areola is
responsible for the reduced base
diameter and areolar herniation
Classification
Von Heimburg:
Type 1: hypoplasia of the lower
medial quadrant
Type II: hypoplasia of the lower
medial and lateral quadrants
with sufficient skin in the
subareolar area
Type III: hypoplasia of the lower
medial and lateral quadrants
with a deficiency of the
subareolar skin
Type IV: severe breast constriction
with minimal breast base
Grolleau Classification
Type 1: lower medial quadrant deficiency
• Type II: lower medial and lateral quadrant deficiency
Type Ill: deficiency of all four quadrants
Treatment
• The goals of surgery are to restore volume to the hypoplastic breast(s),
expand the lower pole by releasing the tethering fibrous attachments or
bands between the breast parenchyma and deep fascial and pectoralis
muscle and also between the breast parenchyma and skin, and where
necessary reduce the areola size and recess the herniated breast tissue.
• The Mandrekas technique is
illustrated. (Above, left) A
periareolar approach is
advocated. (Above, center)
The dissection proceeds in
the subcutaneous plane to
the pectoral fascia. (Above,
right) The dissection
continues to the desired
inframammary fold. (Below,
left) The inferior pole of the
breast is exteriorized, and the
constrictive band is divided
vertically. (Below, right)
Finally, the areola is reduced,
and the breast is recontoured
Das könnte Ihnen auch gefallen
- SinulDokument86 SeitenSinulCucos NataliaNoch keine Bewertungen
- Anatomy of The Pectoral RegionDokument42 SeitenAnatomy of The Pectoral Regionomotayojane21Noch keine Bewertungen
- Anatomy Screeningcervix by DR. VACHASPATIDokument52 SeitenAnatomy Screeningcervix by DR. VACHASPATIOshydh PojnNoch keine Bewertungen
- Anatomy of The UterusDokument21 SeitenAnatomy of The UterusSalman KhanNoch keine Bewertungen
- P. Cavity: (Female Reproductive Organs)Dokument38 SeitenP. Cavity: (Female Reproductive Organs)SAKARIYE MAXAMEDNoch keine Bewertungen
- Anatomical Considerations During G-Laparoscopic SurgeryDokument28 SeitenAnatomical Considerations During G-Laparoscopic SurgeryMahia RahmanNoch keine Bewertungen
- Abdominal Wall and HerniaDokument35 SeitenAbdominal Wall and HerniaMohammad BanisalmanNoch keine Bewertungen
- Uterus Fallopian Tube and OvaryDokument35 SeitenUterus Fallopian Tube and Ovaryvijaya pranaviNoch keine Bewertungen
- Lec.1.Anatomy of PregnancyDokument53 SeitenLec.1.Anatomy of PregnancyManal AsadNoch keine Bewertungen
- Anatomy of GIT For PCII Students..Dokument106 SeitenAnatomy of GIT For PCII Students..AMANUEL HABTEWOLDNoch keine Bewertungen
- Female Genital OrgansDokument40 SeitenFemale Genital OrgansShimmering MoonNoch keine Bewertungen
- Anatomy of Breast: DR Ram Manohar Lohia Institute of Medical Sciences, LucknowDokument103 SeitenAnatomy of Breast: DR Ram Manohar Lohia Institute of Medical Sciences, LucknowMohammad Ahmad AyasrahNoch keine Bewertungen
- Anatomy of Fallopian Tube & OvaryDokument89 SeitenAnatomy of Fallopian Tube & OvaryAsma AijazNoch keine Bewertungen
- Surgical-ANATOMY OF Anterior Abdominal WallDokument83 SeitenSurgical-ANATOMY OF Anterior Abdominal WallSyed Irfan ArifNoch keine Bewertungen
- Anatomy of The Breast1Dokument13 SeitenAnatomy of The Breast1Shahinda Ahmed AdelNoch keine Bewertungen
- AnatDokument45 SeitenAnatRinxas VerinxtNoch keine Bewertungen
- Breast Anatomy With Clinical CorrelationDokument27 SeitenBreast Anatomy With Clinical CorrelationDionix Cruz100% (2)
- Anatomy and Physiology of The VaginaDokument74 SeitenAnatomy and Physiology of The VaginaRacquel BurrowesNoch keine Bewertungen
- Breast AnatomyDokument15 SeitenBreast Anatomyvarun100% (1)
- Anterolateral Abdominal Wall and Abdominal IncisionsDokument42 SeitenAnterolateral Abdominal Wall and Abdominal IncisionsSamar AhmadNoch keine Bewertungen
- Abdomen and Abdominal WallDokument40 SeitenAbdomen and Abdominal WallAlex ChagalaNoch keine Bewertungen
- Embryology and Functional Anatomy of The BreastDokument20 SeitenEmbryology and Functional Anatomy of The BreastseidkeNoch keine Bewertungen
- Abdominal Region Part 2Dokument58 SeitenAbdominal Region Part 2Swati LataNoch keine Bewertungen
- Breast - Mammary GlandDokument16 SeitenBreast - Mammary GlandEniola DaramolaNoch keine Bewertungen
- Uterus and Ovary UltrasoundDokument144 SeitenUterus and Ovary Ultrasoundisicheipraise3Noch keine Bewertungen
- Anatomy of Female Reproductive SystemDokument68 SeitenAnatomy of Female Reproductive SystemdodoNoch keine Bewertungen
- 4rd Lecture - AbdomenDokument26 Seiten4rd Lecture - AbdomenZainab Jamal SiddiquiNoch keine Bewertungen
- Anatomy and Embryology of Bladder: Dr. Deepesh Kalra Institute of Urology Madras Medical College, ChennaiDokument33 SeitenAnatomy and Embryology of Bladder: Dr. Deepesh Kalra Institute of Urology Madras Medical College, ChennaiFatima Zahra Rahim ArchiNoch keine Bewertungen
- 4) Mammary Gland 220413 Upnm2Dokument22 Seiten4) Mammary Gland 220413 Upnm2AaronMaroonFive100% (1)
- Maternal Anatomy WilliamsDokument60 SeitenMaternal Anatomy WilliamsZari Novela100% (2)
- Female Genital Organs.Dokument18 SeitenFemale Genital Organs.Shimmering MoonNoch keine Bewertungen
- Topography Femoral RegionDokument40 SeitenTopography Femoral RegionmonaNoch keine Bewertungen
- Perineal TearsDokument49 SeitenPerineal TearsvisakhaNoch keine Bewertungen
- Vagina Anat, Episiotomy and MGMT of Cervical TearDokument50 SeitenVagina Anat, Episiotomy and MGMT of Cervical TearCapricious BibekNoch keine Bewertungen
- Intro Lab Anatomi Rps (2024)Dokument117 SeitenIntro Lab Anatomi Rps (2024)Jason Maxwell mcguireNoch keine Bewertungen
- Abdominal WallDokument56 SeitenAbdominal WallAHMAD KHANNoch keine Bewertungen
- PT Physiology of PuerperiumDokument14 SeitenPT Physiology of PuerperiumPragati BholeNoch keine Bewertungen
- Revisit of Male & Female Genital Tracts Semester VIIDokument50 SeitenRevisit of Male & Female Genital Tracts Semester VIIDr. AyshaNoch keine Bewertungen
- 07 - Uterus, Uterine Tubes, OvariesDokument52 Seiten07 - Uterus, Uterine Tubes, Ovariesck4realNoch keine Bewertungen
- AnatomicallyDokument3 SeitenAnatomicallyAjayDeep NallabothulaNoch keine Bewertungen
- CBL 2Dokument20 SeitenCBL 2Hammad AkramNoch keine Bewertungen
- Anatomy of Uterus and Vagina and PudendumDokument38 SeitenAnatomy of Uterus and Vagina and Pudendumgugus aminaNoch keine Bewertungen
- Female PerineumDokument27 SeitenFemale Perineumkaartikey dubeNoch keine Bewertungen
- Anterior Abdominal Wall& Inguinal Canal 2023Dokument26 SeitenAnterior Abdominal Wall& Inguinal Canal 2023GanapathyGaneshNoch keine Bewertungen
- Ca BreastDokument64 SeitenCa Breastadina.batajuNoch keine Bewertungen
- Perineum and UG TriangleDokument27 SeitenPerineum and UG TriangleAbiola NerdNoch keine Bewertungen
- Maternal AnatomyDokument96 SeitenMaternal AnatomyIbnu RahmanNoch keine Bewertungen
- UntitledDokument7 SeitenUntitledDania Ibraheem100% (1)
- Student Name: ALI HASSAN RAZA STUDENT I D: 2018304027Dokument6 SeitenStudent Name: ALI HASSAN RAZA STUDENT I D: 2018304027Sayed AsifNoch keine Bewertungen
- Perineum AnatomyDokument23 SeitenPerineum Anatomyrohitrohillapalwal999Noch keine Bewertungen
- Anatomy of Pregnancy NewDokument42 SeitenAnatomy of Pregnancy NewZaroon Abdullah KhanNoch keine Bewertungen
- Relations of ThoraxDokument28 SeitenRelations of ThoraxAnigha PrasadNoch keine Bewertungen
- Anatomy and PhysiologyDokument3 SeitenAnatomy and PhysiologyJade AltarejosNoch keine Bewertungen
- Inguinal Canal: DR - Lubna NazliDokument28 SeitenInguinal Canal: DR - Lubna NazliAhmed AminNoch keine Bewertungen
- UterusDokument34 SeitenUterushammad992Noch keine Bewertungen
- Urinary Bladder, Rectum and Anal CanalDokument34 SeitenUrinary Bladder, Rectum and Anal CanalIbe ClementNoch keine Bewertungen
- Uterus 1Dokument13 SeitenUterus 1shrutik91Noch keine Bewertungen
- Female Reproductive SystemDokument40 SeitenFemale Reproductive SystemSAYMABANUNoch keine Bewertungen
- Female Reproductive System (Yuni)Dokument36 SeitenFemale Reproductive System (Yuni)Ayi Abdul BasithNoch keine Bewertungen
- Essentials of Plastic Surgery, 2nd EditionDokument1.351 SeitenEssentials of Plastic Surgery, 2nd EditionIcleanu Alexandru84% (19)
- (Mebooksfree Net) Cor&pro&pla&sur&nel&buc&2nd PDFDokument527 Seiten(Mebooksfree Net) Cor&pro&pla&sur&nel&buc&2nd PDFCucos Natalia100% (1)
- Amputation Stumps H. E.: Harding Langdale-Kelham, London, EnglandDokument3 SeitenAmputation Stumps H. E.: Harding Langdale-Kelham, London, EnglandCucos NataliaNoch keine Bewertungen
- Menstrual Disorders Associated With Thyroid Dysfunction: Ramya M. R., Parvathavarthini, Darshan Savery, R. SankareswariDokument5 SeitenMenstrual Disorders Associated With Thyroid Dysfunction: Ramya M. R., Parvathavarthini, Darshan Savery, R. SankareswariCucos NataliaNoch keine Bewertungen
- Essentials of Plastic Surgery, 2nd EditionDokument1.351 SeitenEssentials of Plastic Surgery, 2nd EditionIcleanu Alexandru84% (19)
- PH Water On Stability PesticidesDokument6 SeitenPH Water On Stability PesticidesMontoya AlidNoch keine Bewertungen
- T2T - One - U12 - Grammarworksheet - 1 Should For Advice PDFDokument1 SeiteT2T - One - U12 - Grammarworksheet - 1 Should For Advice PDFGrissellNoch keine Bewertungen
- TG - Health 3 - Q3Dokument29 SeitenTG - Health 3 - Q3LouieNoch keine Bewertungen
- Intimate TemporalitiesDokument12 SeitenIntimate TemporalitiesmittentenNoch keine Bewertungen
- Tutorial Class 4: Finders As Bailee Right of A Bailee General LienDokument26 SeitenTutorial Class 4: Finders As Bailee Right of A Bailee General Lienchirag jainNoch keine Bewertungen
- Budget ProposalDokument1 SeiteBudget ProposalXean miNoch keine Bewertungen
- Laws and Policies of Fertilizers SectorDokument12 SeitenLaws and Policies of Fertilizers Sectorqry01327Noch keine Bewertungen
- Sikarep® Microcrete-4: Product Data SheetDokument2 SeitenSikarep® Microcrete-4: Product Data Sheetsidharthsud28Noch keine Bewertungen
- Value Chain AnalaysisDokument100 SeitenValue Chain AnalaysisDaguale Melaku AyeleNoch keine Bewertungen
- Bon JourDokument15 SeitenBon JourNikolinaJamicic0% (1)
- Index-Formal Spoken Arabic Dialogue - Al Kitaab Based - MSA - From Langmedia Five CollegesDokument5 SeitenIndex-Formal Spoken Arabic Dialogue - Al Kitaab Based - MSA - From Langmedia Five CollegesD.ElderNoch keine Bewertungen
- Exam Questions AZ-304: Microsoft Azure Architect Design (Beta)Dokument9 SeitenExam Questions AZ-304: Microsoft Azure Architect Design (Beta)Deepa R NairNoch keine Bewertungen
- IsaiahDokument7 SeitenIsaiahJett Rovee Navarro100% (1)
- Internship Report On A Study of The Masterbranding of Dove: Urmee Rahman SilveeDokument45 SeitenInternship Report On A Study of The Masterbranding of Dove: Urmee Rahman SilveeVIRAL DOSHINoch keine Bewertungen
- Rotation and Revolution of EarthDokument4 SeitenRotation and Revolution of EarthRamu ArunachalamNoch keine Bewertungen
- IKEA AyeshaDokument41 SeitenIKEA AyeshaAYESHAREHMAN100Noch keine Bewertungen
- Venue:: Alberta Electrical System Alberta Electrical System OperatorDokument48 SeitenVenue:: Alberta Electrical System Alberta Electrical System OperatorOmar fethiNoch keine Bewertungen
- Review of Related LiteratureDokument9 SeitenReview of Related LiteratureMarion Joy GanayoNoch keine Bewertungen
- Garden Club of Virginia RestorationsDokument1 SeiteGarden Club of Virginia RestorationsGarden Club of VirginiaNoch keine Bewertungen
- Lunch Hour Meetings: Kiwanis Mission:: - Officers & Directors, 2018-2019Dokument2 SeitenLunch Hour Meetings: Kiwanis Mission:: - Officers & Directors, 2018-2019Kiwanis Club of WaycrossNoch keine Bewertungen
- Trainee'S Record Book: Technical Education and Skills Development Authority (Your Institution)Dokument17 SeitenTrainee'S Record Book: Technical Education and Skills Development Authority (Your Institution)Ronald Dequilla PacolNoch keine Bewertungen
- Manual StereoDokument29 SeitenManual StereoPeter Mac RedNoch keine Bewertungen
- Earnings Statement: Hilton Management Lane TN 38117 Lane TN 38117 LLC 755 Crossover MemphisDokument2 SeitenEarnings Statement: Hilton Management Lane TN 38117 Lane TN 38117 LLC 755 Crossover MemphisSelina González HerreraNoch keine Bewertungen
- New Count The DotsDokument1 SeiteNew Count The Dotslin ee100% (1)
- PDF - Unpacking LRC and LIC Calculations For PC InsurersDokument14 SeitenPDF - Unpacking LRC and LIC Calculations For PC Insurersnod32_1206Noch keine Bewertungen
- Bus Organization of 8085 MicroprocessorDokument6 SeitenBus Organization of 8085 MicroprocessorsrikrishnathotaNoch keine Bewertungen
- Hirarc Form: 1. Hazard Identification 2. Risk Analysis 3. Risk ControlDokument2 SeitenHirarc Form: 1. Hazard Identification 2. Risk Analysis 3. Risk ControlQurratulain Syarifuddinzaini100% (1)
- James Ellroy PerfidiaDokument4 SeitenJames Ellroy PerfidiaMichelly Cristina SilvaNoch keine Bewertungen
- Pre Joining Guidelines For InfosysDokument21 SeitenPre Joining Guidelines For InfosysGokul0% (2)
- Powerpoints 4 4up8Dokument9 SeitenPowerpoints 4 4up8Ali KalyarNoch keine Bewertungen