Beruflich Dokumente
Kultur Dokumente
SCOLIOSIS
Hochgeladen von
Espers Blues0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
82 Ansichten19 SeitenOriginaltitel
SCOLIOSIS.pptx
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
82 Ansichten19 SeitenSCOLIOSIS
Hochgeladen von
Espers BluesCopyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 19
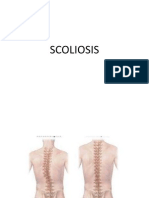
SCOLIOSIS
• A general spinal deformity characterized by
lateral curvatures and vertebral rotation.
• It may be associated with a fixed structural
curve or reducible functional curve.
• Correlation with discomfort is unclear, but low
back pain is usually the initial symptom.
• It is related to curve severity and usually
begins at the convexity.
PATHOLOGY
The Scoliosis Research Society
(SRS) has defined a medically significant frontal plane curve
(scoliosis) as any curve which is greater or equal to 10 degrees,
with or without a rotatory component (3). The definition of
a pathological sagittal plane curve is less settled. The spine is
“balanced” in the sagittal plane along a plumb line dropped
from the center of C7 to the sacral promontory (4). This balance
can be influenced by the position of the head and neck,
as well as the pelvis and lower limbs. This dynamic balance
may help explain some of the outstanding controversy about
pathological sagittal curves.
normal range of thoracic kyphosis to be 20 to 40 degrees,
others
(1) give the range as 30 to 50 degrees. Fon et al. (6) have
shown that kyphosis increases about 4 to 5 degrees over
childhood
to the end of adolescence. Kyphosis is also known to
increase with aging. The SRS has agreed that normal thoracic
kyphosis ranges from 20 to 50 degrees. The range of normal
for lumbar lordosis is even wider. Jackson and McManus (7)
found the mean lordosis to be 59 degrees. Vaz et al. (8) found
a mean lumbar lordosis of 46.5 degrees, with a range from 26
to 76 degrees. The SRS has agreed (4) that normal lumbar
lordosis can range from 31 to 79 degrees, depending on
measurement
technique
Clinical features
• Right thoracic curve Most common; the apex can
typically be seen at T7 or T8.
• Double major curve Right thoracic with a left
lumbar curve; little cosmetic deformity.
• Lumbar curve Left lumbar curves are greater than
right lumbar curves.
• Thoracolumbar curve Less cosmetic deformity
than thoracic curve, may have rib and flank
distortion.
• Left thoracic curve Rare; may be associated with
spinal cord abnormalities.
IMAGING
• X-rays help establish diagnosis and prognosis.
–– Follow-up x-rays will depend on skeletal maturity, patient age, and degree
of
curvature.
–– Younger patients with rapidly progressing curves warrant earlier x-ray
follow-up.
• Rotation (Figure 4–176)
–– Pedicle portion estimates the amount of vertebral rotation on the PA view.
–– Grading: 0 (no rotation) to 4 (complete pedicle rotation out of view).
• Curve: Cobb angle (Figure 4–177)
–– An angle formed by the perpendicular lines drawn from the endplates of
the most tilted
proximal and distal vertebrae to measure the scoliotic curve.
ETIOLOGY
Idiopathic Most common
• Infantile Birth to 3 years: associated with congenital defects
• Juvenile 4 years to 10 years; high risk of curve progression
• Adolescent Most common; 10 years to maturity; high risk
of progression
Congenital May be due to an early embryologic
developmental defect
• Open Caused by myelomeningocele
• Closed May be associated with neurologic deficits
Associated with a wedged vertebra, hemivertebra,
congenital bar, or block vertebrae
Neuromuscular
Certain neuromuscular disorders may have a rapid curve
progression with associated pulmonary and spinal cord
complications
TABLE 34.1 Types of Scoliosis and Typical Ages
of OnsetPathophysiological Typeof Scoliosis Typical
Age of Onset
• Idiopathic Infancy to adolescence
• Neuromuscular Childhood to adolescence
• Bone or ligamentous dysfunction Childhood
• Traumatic/posttraumatic All ages
• Infectious or neoplastic All ages
• Degenerative Middle age to seniors
Treatment
Degree of angulation
• Observation <20°
• Bracing 20° to 40°
• Surgery >40° (>35° for neuromuscular diseases)
Conservative
• –– Rehabilitation program
• –– Bracing
■■ Prevents worsening of the curvature but does not correct scoliosis.
■■ Worn 23 hours a day until spinal growth is completed.
■■ Weaning off can begin when radiographs display signs of maturity, and curves are
stable.
■■ Patients should be evaluated at 2- to 3-year intervals
Tipe :
Milwaukee brace High thoracic curves (apex at T8)
Low profile TLSO Lower thoracic, thoracolumbar, and lumbar curves (apex below T8)
• Surgical
–– Spinal procedures are indicated for scoliosis
with:
■■ Relentless progression.
■■ >40° curvature in the skeletally immature,
>50° in the skeletally mature, <35° in
Neuromuscular diseases, or progressive loss of
pulmonary function.
ANAMNESA
The first clue to the etiology of the deformity will be
the age of onset. If the scoliosis presents at or soon
after birth, it is more likely to be associated with a
congenital bony deformity or inherited disease
involving the neuromuscular system. If the scoliosis
begins in late childhood or adolescence, it is likely
to be idiopathic. Spinal deformity that begins in
young adulthood is most likely due to trauma or
infection; in middle age or later, it is likely to be
associated with degenerative disk or joint disease
and/or osteoporosis.
It is also important to determine if the onset of the curve
is associated with any acute problem such as trauma or infection.
The degree of curvature and how fast the size of the curve
increases also offer insights into etiology. An underlying
neuromuscular or ligamentous condition may promote quicker
progression. Children within their adolescent growth spurt
may have greater progression due to the rate of overall growth.
Progression in an older adult may be an indicator of poor bone
health.
Although pain is associated with spinal deformity in adults, it
is uncommon in children
and adolescents (13) and obligates the physiatrist to search
for underlying pathologies including neoplasm or infection.
Similar to other pain-evoking conditions, details about the
quality, intensity, and temporal and spatial parameters of the
pain will help distinguish among bony, soft-tissue–based, and
neuromuscular-based pain. Cardiopulmonary dysfunction
is the most serious morbidity of spinal deformity. Therefore,
questions about fatigability, shortness of breath, palpitations,
and decrease in endurance must be included in the history.
Any suggestion of cardiopulmonary dysfunction should lead
to a more rapid and aggressive workup.
It is important to inquire about the symptoms of central
nervous system dysfunction. Problems with loss of balance or
falls may indicate a coordination problem such as is seen in
cerebellar syndromes. Complaints of muscle spasms may indicate
spasticity. Conversely, complaints of weakness or sensory
loss may indicate peripheral nervous and/or muscle pathology.
Reports of frequent joint sprains may indicate the presence of
a condition associated with ligamentous laxity. In children and
adolescents, it is important to obtain a history of developmental
milestones. Indication of delay in any of the developmental
spheres—social/behavioral, communication and cognition,
fine motor, gross motor—may provide clues to the presence
of an underlying syndrome.
Since spinal deformity may be initiated or
exacerbated by conditions affecting other areas
of the body, the physiatrist should ask about
conditions that may affect the lower limbs, such
as a history of hip dislocation or leg length
discrepancy, and even conditions associated
with asymmetry of the upper limbs and head.
Physchiatric clinical examination
• assessment of pain, strength, endurance, sensation,
balance (in sitting and standing), coordination, range of
motion,reflexes,mobility, and dressing skills. Leg length
discrepancy should be assessed,
• The surface anatomy should be viewed in both prone
and side lying. If the patient can sit, then the spine
must be seen in sitting. If he or she can stand, even
with support, then the spine must be viewed in
standing. If there is concern about leg length
discrepancy and/or pelvic asymmetry, the spine should
also be viewed in standing with leveling blocks under
the foot on the “short” side and the depth
• the examiner should look at the shapeof the
rib cage for prominence or humping (Adam’s
forward bending test
negative positif
Das könnte Ihnen auch gefallen
- Frozen ShoulderDokument44 SeitenFrozen ShoulderEspers BluesNoch keine Bewertungen
- Herniated Nucleus Pulposus (HNP)Dokument21 SeitenHerniated Nucleus Pulposus (HNP)Kaye100% (1)
- Scoliosis (Curved Spine)Dokument7 SeitenScoliosis (Curved Spine)Chow Mun FaiNoch keine Bewertungen
- Femoral Neck FracturesDokument8 SeitenFemoral Neck FracturesMorshed Mahbub AbirNoch keine Bewertungen
- Low BackDokument7 SeitenLow BackMuhammad FahmyNoch keine Bewertungen
- Week 3 - PCPDokument3 SeitenWeek 3 - PCPapi-479754549100% (1)
- Week 6 - PCPDokument6 SeitenWeek 6 - PCPapi-479754549Noch keine Bewertungen
- Spinal Cord InjuryDokument39 SeitenSpinal Cord InjuryrahatNoch keine Bewertungen
- Orthopath Final ReviewDokument16 SeitenOrthopath Final ReviewharrischoeNoch keine Bewertungen
- ScoliosisDokument25 SeitenScoliosisshanel18100% (1)
- Joint DislocationsDokument35 SeitenJoint DislocationsfhmanshoriNoch keine Bewertungen
- Rehabilitation of Cerebral Palsy & Motor DelayDokument49 SeitenRehabilitation of Cerebral Palsy & Motor DelayasloocltNoch keine Bewertungen
- Spine Examination: Mario Johan Heryputra 11.2012.208Dokument29 SeitenSpine Examination: Mario Johan Heryputra 11.2012.208Mario Johan Heryputra100% (1)
- Spine Fractures and Spinal Cord InjuryDokument54 SeitenSpine Fractures and Spinal Cord InjuryAloy PudeNoch keine Bewertungen
- DR - Rieva Kuliah 7 November - 2018Dokument38 SeitenDR - Rieva Kuliah 7 November - 2018Nisrina100% (1)
- Pediatric OrthopedicsDokument28 SeitenPediatric OrthopedicsEdwin OkonNoch keine Bewertungen
- Cervical Radiculopathy, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandCervical Radiculopathy, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Sasaran Indikator Dan Pengukuran Mutu Klinik - 1Dokument61 SeitenSasaran Indikator Dan Pengukuran Mutu Klinik - 1Arief Jatmiko100% (2)
- Week 1 and 2 PCP Workbook QuestionsDokument4 SeitenWeek 1 and 2 PCP Workbook Questionsapi-479717740100% (1)
- Cervical SpondylosisDokument9 SeitenCervical SpondylosisNurHidayah Borhanudin100% (1)
- Cerebral Palsy Revalida FormatDokument10 SeitenCerebral Palsy Revalida FormatChelsea CalanoNoch keine Bewertungen
- Elbow Special TestDokument4 SeitenElbow Special TestEllaiza Astacaan100% (1)
- Avascular Necrosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandAvascular Necrosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBewertung: 4 von 5 Sternen4/5 (2)
- Orthopedic History Taking: DR - Kholoud Al-ZainDokument30 SeitenOrthopedic History Taking: DR - Kholoud Al-ZainKaizar EnnisNoch keine Bewertungen
- Spine: HistoryDokument6 SeitenSpine: HistorySham SundarNoch keine Bewertungen
- Modified Barthel Index (Shah Ver.)Dokument4 SeitenModified Barthel Index (Shah Ver.)Chia Yuan Lin100% (6)
- Prolapsed Disc SignsDokument14 SeitenProlapsed Disc SignsMartin Sage100% (1)
- Primary and Secondary Adhesive Capsulitis Etiology, Stages, Signs, Tests and ManagementDokument8 SeitenPrimary and Secondary Adhesive Capsulitis Etiology, Stages, Signs, Tests and ManagementVanessa Yvonne Gurtiza100% (1)
- Trochanteric Bursitis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandTrochanteric Bursitis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- Spine Special Test RoeDokument9 SeitenSpine Special Test RoeElijah Quiano100% (1)
- Perthes Disease: by Dr. Abdul Karim Postgraduate Resident Orthopedic Surgery Pgmi/Lgh. Lahore PakistanDokument68 SeitenPerthes Disease: by Dr. Abdul Karim Postgraduate Resident Orthopedic Surgery Pgmi/Lgh. Lahore Pakistandrakkashmiri50% (2)
- ShoulderDokument51 SeitenShoulderIts LaraNoch keine Bewertungen
- Elbow Anatomy & Biomechanics - Shoulder & Elbow - OrthobulletsDokument10 SeitenElbow Anatomy & Biomechanics - Shoulder & Elbow - OrthobulletsShashank VermaNoch keine Bewertungen
- Perthes Disease: A Rare Childhood Hip ConditionDokument4 SeitenPerthes Disease: A Rare Childhood Hip ConditionMohamed HamoodNoch keine Bewertungen
- Ankel Heel PainDokument51 SeitenAnkel Heel PainMeno Ali100% (1)
- Scoliosis: Spinal Curvature, KyphoscoliosisDokument3 SeitenScoliosis: Spinal Curvature, Kyphoscoliosisiamweena17Noch keine Bewertungen
- Sachs Sentence Test1Dokument4 SeitenSachs Sentence Test1Angela Mae100% (1)
- Adolescent Idiopathic ScoliosisDokument29 SeitenAdolescent Idiopathic ScoliosisfenskaNoch keine Bewertungen
- Scoliosis: Aka: Idiopathic Scoliosis, Adolescent ScoliosisDokument12 SeitenScoliosis: Aka: Idiopathic Scoliosis, Adolescent ScoliosisLei Coloma SissonNoch keine Bewertungen
- Project Management British English TeacherDokument4 SeitenProject Management British English TeacherАнастасия МицковскаяNoch keine Bewertungen
- Ielts Speaking Part One Long Short Answers PDFDokument7 SeitenIelts Speaking Part One Long Short Answers PDFKaran JariwalaNoch keine Bewertungen
- Get It Up 1 - DAP AnDokument18 SeitenGet It Up 1 - DAP AnAndreea EliescuNoch keine Bewertungen
- TB Spine OrthopedicsDokument34 SeitenTB Spine OrthopedicsHafizah HoshniNoch keine Bewertungen
- Sample Statement of Purpose Computer Engineering (SOP)Dokument1 SeiteSample Statement of Purpose Computer Engineering (SOP)theonlybbb86% (7)
- Sprengel's ShoulderDokument21 SeitenSprengel's ShoulderNahayo Xavier100% (1)
- What Is PolymyositisDokument24 SeitenWhat Is PolymyositisAshraf MobyNoch keine Bewertungen
- Orthopedic examination techniques and common conditionsDokument226 SeitenOrthopedic examination techniques and common conditionsMandisa Ndlovu Tenego0% (1)
- Prosthetic GaitDokument33 SeitenProsthetic GaitDibyendu DuttaNoch keine Bewertungen
- Soft tissue injury treatment RICEDokument2 SeitenSoft tissue injury treatment RICEDenis Edem Dzebre100% (1)
- Fractures of Spine and Pelvis2007Dokument70 SeitenFractures of Spine and Pelvis2007api-19916399Noch keine Bewertungen
- Periarthritis Shoulder By: DR - Sindhu.MPT (Ortho)Dokument39 SeitenPeriarthritis Shoulder By: DR - Sindhu.MPT (Ortho)Michael Selvaraj100% (1)
- Elbow TraumaDokument62 SeitenElbow Traumadrcoolcat2000Noch keine Bewertungen
- Knee Special Test FinallllllDokument19 SeitenKnee Special Test FinallllllElijah QuianoNoch keine Bewertungen
- TB of Spine Diagnosis and TreatmentDokument13 SeitenTB of Spine Diagnosis and Treatmentzoha hassan100% (1)
- Pediatric Hip Dysplasia Case StudyDokument13 SeitenPediatric Hip Dysplasia Case Studyapi-349474075Noch keine Bewertungen
- Special Tests For Elbow and ForearmDokument3 SeitenSpecial Tests For Elbow and ForearmAllyza PenaNoch keine Bewertungen
- Pott's Disease NCPDokument30 SeitenPott's Disease NCPmrscribd12Noch keine Bewertungen
- Cervical Radiculopathy Clinical PresentationDokument9 SeitenCervical Radiculopathy Clinical PresentationItai IzhakNoch keine Bewertungen
- Low Back Pain Pearls of WisdomDokument33 SeitenLow Back Pain Pearls of WisdomNaveed KhanNoch keine Bewertungen
- S Pondy Lolis ThesisDokument13 SeitenS Pondy Lolis ThesisFadlu Manaf100% (1)
- SpondylosisDokument20 SeitenSpondylosisLiza Puspita SariNoch keine Bewertungen
- MusculoskeletalDokument119 SeitenMusculoskeletalEdissa PangilinanNoch keine Bewertungen
- LaminectomyDokument5 SeitenLaminectomyanon_931797817Noch keine Bewertungen
- Coxa VaraDokument3 SeitenCoxa VaraMd Ahsanuzzaman PinkuNoch keine Bewertungen
- Biomechanics of The ElbowDokument16 SeitenBiomechanics of The ElbowAsmaa Ahmad SharawyNoch keine Bewertungen
- Juvenile Rheumatoid Arthritis: Dorothy W. Wortmann, MDDokument38 SeitenJuvenile Rheumatoid Arthritis: Dorothy W. Wortmann, MDLavi GoyalNoch keine Bewertungen
- Fracture Neck of FemurDokument18 SeitenFracture Neck of FemurPraganesh VarshneyNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument33 SeitenChronic Obstructive Pulmonary DiseaseEspers BluesNoch keine Bewertungen
- Frozen ShoulderDokument44 SeitenFrozen ShoulderEspers BluesNoch keine Bewertungen
- COPD Classification and TreatmentDokument10 SeitenCOPD Classification and TreatmentlolNoch keine Bewertungen
- Diet DiabetesDokument2 SeitenDiet DiabetesEspers BluesNoch keine Bewertungen
- Lifestyle PDFDokument19 SeitenLifestyle PDFEspers BluesNoch keine Bewertungen
- Balance evaluation tools for stroke patientsDokument17 SeitenBalance evaluation tools for stroke patientsEspers BluesNoch keine Bewertungen
- Stroke in South Asia PDFDokument7 SeitenStroke in South Asia PDFEspers BluesNoch keine Bewertungen
- Stroke in Saudi PDFDokument5 SeitenStroke in Saudi PDFEspers BluesNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument33 SeitenChronic Obstructive Pulmonary DiseaseEspers BluesNoch keine Bewertungen
- Stroke in South Asia PDFDokument7 SeitenStroke in South Asia PDFEspers BluesNoch keine Bewertungen
- Progressing Haemorhagic Stroke PDFDokument18 SeitenProgressing Haemorhagic Stroke PDFEspers BluesNoch keine Bewertungen
- Managemen Stroke PDFDokument6 SeitenManagemen Stroke PDFEspers BluesNoch keine Bewertungen
- Role of OTs and PTs in stroke preventionDokument11 SeitenRole of OTs and PTs in stroke preventionEspers BluesNoch keine Bewertungen
- Role of OTs and PTs in stroke preventionDokument11 SeitenRole of OTs and PTs in stroke preventionEspers BluesNoch keine Bewertungen
- Balance evaluation tools for stroke patientsDokument17 SeitenBalance evaluation tools for stroke patientsEspers BluesNoch keine Bewertungen
- 54 Factors Known To Cause False Positives PDFDokument4 Seiten54 Factors Known To Cause False Positives PDFDiani ArisandhiNoch keine Bewertungen
- OA Genu Support SlideDokument71 SeitenOA Genu Support SlideEspers BluesNoch keine Bewertungen
- OA Genu Support SlideDokument71 SeitenOA Genu Support SlideEspers BluesNoch keine Bewertungen
- OA Genu Support SlideDokument71 SeitenOA Genu Support SlideEspers BluesNoch keine Bewertungen
- Mass Gen Shoulder Impingement Syndrome Patient Inormation Information and Exercises PDFDokument9 SeitenMass Gen Shoulder Impingement Syndrome Patient Inormation Information and Exercises PDFEspers BluesNoch keine Bewertungen
- OA Genu Support SlideDokument71 SeitenOA Genu Support SlideEspers BluesNoch keine Bewertungen
- Trigger FingerDokument13 SeitenTrigger FingerEspers BluesNoch keine Bewertungen
- European Project Semester MinorDokument3 SeitenEuropean Project Semester MinorIrving Delgado SilvaNoch keine Bewertungen
- LPU Student HandbookDokument164 SeitenLPU Student HandbookAngelique MancillaNoch keine Bewertungen
- Human Resources CertificateDokument16 SeitenHuman Resources CertificatejennyNoch keine Bewertungen
- Female Hindu PriestsDokument4 SeitenFemale Hindu PriestsHarivenugopalaNoch keine Bewertungen
- Individual Reflection 4Dokument4 SeitenIndividual Reflection 4Urvashi PuraniNoch keine Bewertungen
- Bryson Yurkemik: Employment ObjectiveDokument2 SeitenBryson Yurkemik: Employment Objectiveapi-345358688Noch keine Bewertungen
- SelfDokument2 SeitenSelfglezamaeNoch keine Bewertungen
- Unit Portfolio RubricDokument1 SeiteUnit Portfolio Rubricapi-262178636Noch keine Bewertungen
- ACTION PLAN IN GUIDANCE S.Y. 2021-2022Dokument2 SeitenACTION PLAN IN GUIDANCE S.Y. 2021-2022Maria Noly Villotes EntinoNoch keine Bewertungen
- Aliran SBP Tingkatan 4 Tahun 2015 & Laman Web Sekolah PDFDokument1 SeiteAliran SBP Tingkatan 4 Tahun 2015 & Laman Web Sekolah PDFPaul Chan C LNoch keine Bewertungen
- Intermediate Sample Pop Exam Paper 1Dokument10 SeitenIntermediate Sample Pop Exam Paper 1Анюта ЛіхванчукNoch keine Bewertungen
- Managing ServiceguardDokument534 SeitenManaging ServiceguardSagar BachalNoch keine Bewertungen
- Session Plan FBSDokument17 SeitenSession Plan FBSorabelle punoNoch keine Bewertungen
- GE 8 EthcsDokument22 SeitenGE 8 EthcsWilliam Soneja CalapiniNoch keine Bewertungen
- Visualization Without VisionDokument21 SeitenVisualization Without Vision11Dewi Meiliyan Ningrum dewimeiliyan.2020Noch keine Bewertungen
- Diaz - Science 1 - Learning Packet - Week 04Dokument6 SeitenDiaz - Science 1 - Learning Packet - Week 04Maloucel DiazNoch keine Bewertungen
- George ResumeDokument3 SeitenGeorge Resumeapi-287298572Noch keine Bewertungen
- 14JE000423-Rajat Kumar Jain - B.Tech (Computer Science and Engineering)Dokument2 Seiten14JE000423-Rajat Kumar Jain - B.Tech (Computer Science and Engineering)AshNoch keine Bewertungen
- Year 3 Civic Lesson Plan (September - Love) : Content StandardDokument1 SeiteYear 3 Civic Lesson Plan (September - Love) : Content StandardIdham HakimiNoch keine Bewertungen
- Mechanical Engineer ResumeDokument3 SeitenMechanical Engineer ResumeHimanshu ChauhanNoch keine Bewertungen
- 3 Schizophrenia AssessmentDokument36 Seiten3 Schizophrenia AssessmentArvindhanNoch keine Bewertungen
- OlanipekunDokument3 SeitenOlanipekunAnesu MasirahaNoch keine Bewertungen
- SCNN Scalogram-Based Convolutional Neural Network To Detect ObstructiveDokument12 SeitenSCNN Scalogram-Based Convolutional Neural Network To Detect ObstructiveDayana VieiraNoch keine Bewertungen
- ES 122-Engineering Drawing 2Dokument7 SeitenES 122-Engineering Drawing 2Ricson BondadNoch keine Bewertungen
- Junior HSE AssistantDokument2 SeitenJunior HSE AssistantMuhammad AdnanNoch keine Bewertungen