Beruflich Dokumente
Kultur Dokumente
ACLS ACS Algorithm New
Hochgeladen von
sambo100%(1)100% fanden dieses Dokument nützlich (1 Abstimmung)
119 Ansichten3 SeitenThis document provides guidelines for the assessment, treatment, and management of patients presenting with chest discomfort suggestive of ischemia. It outlines the steps emergency medical services and emergency department staff should take including monitoring vitals, administering oxygen and medications like aspirin and nitroglycerin, obtaining an ECG, and notifying the hospital. Upon arrival at the emergency department, further assessment and testing is done along with initiating treatments depending on whether ST elevation, ST depression, or normal ECG findings are present. Guidelines are provided for management of STEMI, high-risk UA/NSTEMI, and low-risk patients.
Originalbeschreibung:
algoritma acls acs
Copyright
© © All Rights Reserved
Verfügbare Formate
PPT, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenThis document provides guidelines for the assessment, treatment, and management of patients presenting with chest discomfort suggestive of ischemia. It outlines the steps emergency medical services and emergency department staff should take including monitoring vitals, administering oxygen and medications like aspirin and nitroglycerin, obtaining an ECG, and notifying the hospital. Upon arrival at the emergency department, further assessment and testing is done along with initiating treatments depending on whether ST elevation, ST depression, or normal ECG findings are present. Guidelines are provided for management of STEMI, high-risk UA/NSTEMI, and low-risk patients.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
100%(1)100% fanden dieses Dokument nützlich (1 Abstimmung)
119 Ansichten3 SeitenACLS ACS Algorithm New
Hochgeladen von
samboThis document provides guidelines for the assessment, treatment, and management of patients presenting with chest discomfort suggestive of ischemia. It outlines the steps emergency medical services and emergency department staff should take including monitoring vitals, administering oxygen and medications like aspirin and nitroglycerin, obtaining an ECG, and notifying the hospital. Upon arrival at the emergency department, further assessment and testing is done along with initiating treatments depending on whether ST elevation, ST depression, or normal ECG findings are present. Guidelines are provided for management of STEMI, high-risk UA/NSTEMI, and low-risk patients.
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 3
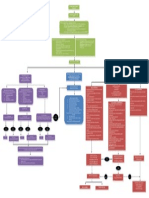
Chest discomfort suggestive of ischemia
EMS assessment and care and hospital preparation:
• Monitor, support ABCs. Be Prepared to provide CPR and defibrillation
• Administer oxygen, aspirin, nitroglycerin, and morphine if needed
• If availabe, obtain 12-lead ECG; if ST-elevation:
• Notify receiving hospital with transmission or interpretation
• Begin fibrinolytic chechlist
• Notified hospital should mobilize hospital resources to respond to STEMI
Immediate ED assessment (<10 min) Immediate ED general treatment
- Check vital signs; evaluate oxygen saturation - Morphine IV if pain relieved by nitroglycerin
- Establish IV access - Oxygen at 4 L/min; maintain 0, sat > 90%
- Obtain/review 12-lead ECG - Nitrogycerin sublingual, spray, or IV
- Perform brief, targeted history, physical exam - Aspirin 160 to 325 mg (if not given by EMS)
- Review/complete fibrinolytic checklist; check
- Containdication (table 1)
- Obatain initial cardaic marker levels; initial electrolyte
and coagulation studies
- Obtain portable chest x-ray (< 30 min)
Review initial 12-lead ECG
ST elevation or new or ST-depression or dynamic T-wave inversion; Normal or nondiagnostik
presumably new LBBB; strongly strongly suspicious for ischemia changes in ST segement or T
suspicious for injury High-Risk Unstable Angina/ wave
Non-ST-Elevation MI (UA/NSTEMI Intermediate/Low-Risk UA
ST-Elevation MI (STEMI)*
Start adjunctive treatment as Start adjunctive treatments as Develop high or
indicated (see text for Yes
indicated (see text for intermediate risk
contraindications) contraindications) criteria (tables 3,4)
•Clopidogrel
Do not delay reperfusion or
•Nitroglycerin
- Clopidogrel •B-adrenergic receptor blockers
troponin-positive
- -adrenergic reseptor blockers •Heparin (UFH or LMWH) No
- Heparin (UFH or LMWH) •Glycoprotein IIb/IIIa inhibitor
Consider admission to ED
>12 chest pain unit orto
hours monitored bed in ED
Time from onset of Admit to monitored bed
Assess risk status Follow:
symptoms < 12 hours? • Serial cardiac marker
<12 hours (including troponin)
• Repeat ECG/continous ST
Reperfusion strategy: High-risk patient : segment
Therapy defined by patients and •Refractory ischemic chest pain monitoring
center criteria (table 2) •Recurrent/persistent ST deviation • Consider stress test
- Be aware of reperfusion goals: •Ventricular tachycardia
•Hemodynamic instability
•Door-to-ballon inflation
•Signs of pump failure Yes
(PCI) goal of 90 min •Early invasive strategy, including Develop high or intermediate
•Door-to-needle catheterization and revascularization risk criteria or
(fibrinolysis) goal of 30 min for shock within 48 hours of an AMI troponin-positive
- Continue adjunctive therapies Continue ASA, heparin, and other
and: therapies as indicated No
•ACE inhibitor/ARB
•ACE inhibitors/angiotensi
•HMG CoA reductase inhibitor (statin If no evidence of ischemia or
receptor blockers (ARB) therapy)
within 24 hours of symptom infarction can discharge with
Not at high risk: cardiology to risk-
anset stratify follow-up
•HMG CoA reductase
Das könnte Ihnen auch gefallen
- Algorithm-ACLS ACS 200806 1Dokument1 SeiteAlgorithm-ACLS ACS 200806 1Kavya Shree100% (1)
- Acute Coronary SyndromeDokument7 SeitenAcute Coronary SyndromePuskesmas Pinang JayaNoch keine Bewertungen
- ACS Algorithm 2016 PDFDokument1 SeiteACS Algorithm 2016 PDFrabin1994Noch keine Bewertungen
- Kegawatan Jantung - MeDokument41 SeitenKegawatan Jantung - MeNam Min BinNoch keine Bewertungen
- Acute Coronary Syndrome / Acute Myocardial Infarction AlgorithmDokument37 SeitenAcute Coronary Syndrome / Acute Myocardial Infarction Algorithmjitendra magarNoch keine Bewertungen
- COVID-19 TREATMENT ADULT Algorithm 4.3.20Dokument10 SeitenCOVID-19 TREATMENT ADULT Algorithm 4.3.20luizfelipenobresc5492100% (1)
- TachycardiaDokument12 SeitenTachycardiaPuskesmas Pinang JayaNoch keine Bewertungen
- Ynhhs - Covid-19 Treatment Adult Algorithm 4.3.20Dokument10 SeitenYnhhs - Covid-19 Treatment Adult Algorithm 4.3.20Ren SNoch keine Bewertungen
- Acute Coronary Syndrome / Acute Myocardial Infarction AlgorithmDokument37 SeitenAcute Coronary Syndrome / Acute Myocardial Infarction AlgorithmHan OWNoch keine Bewertungen
- How To Stratify The Risk and When To Refer: NsteacsDokument28 SeitenHow To Stratify The Risk and When To Refer: NsteacsRatna TambaNoch keine Bewertungen
- Handbook of AnesthesiologyDokument176 SeitenHandbook of AnesthesiologyarmelzahfauziNoch keine Bewertungen
- Current Clinical Strategies: Handbook of AnesthesiologyDokument180 SeitenCurrent Clinical Strategies: Handbook of AnesthesiologydramaganaNoch keine Bewertungen
- Chest Pain System - DisorderDokument1 SeiteChest Pain System - DisorderAA DDNoch keine Bewertungen
- Tto COVID-19 TREATMENT ADULT AlgorithmDokument13 SeitenTto COVID-19 TREATMENT ADULT Algorithmmissbear100% (1)
- Acute Coronary Syndromes - HandoutDokument4 SeitenAcute Coronary Syndromes - Handoutapi-641524095Noch keine Bewertungen
- NSTEMI Management: MHAM-College of MedicineDokument14 SeitenNSTEMI Management: MHAM-College of MedicineMykki Gigi NateNoch keine Bewertungen
- Acute Coronary Syndrome - YMDokument64 SeitenAcute Coronary Syndrome - YMNirwanaNoch keine Bewertungen
- Chest Pain Investigations and ManagementDokument4 SeitenChest Pain Investigations and ManagementYY_1992Noch keine Bewertungen
- Ventura County Medical Center: Mi Thrombolysis, Management ofDokument3 SeitenVentura County Medical Center: Mi Thrombolysis, Management ofblackcat657Noch keine Bewertungen
- ACLS Algorithms SlideDokument26 SeitenACLS Algorithms SlidehrsoNoch keine Bewertungen
- Acs CCS 2021 KLDokument52 SeitenAcs CCS 2021 KLPitchya WangmeesriNoch keine Bewertungen
- NTSEMI and Unstable Angina ANdreaDokument17 SeitenNTSEMI and Unstable Angina ANdreaandreaNoch keine Bewertungen
- Acs With New Stemi GuidelineDokument35 SeitenAcs With New Stemi Guidelinematmin07Noch keine Bewertungen
- CCS - Handbook of Anesthesiology (2005)Dokument180 SeitenCCS - Handbook of Anesthesiology (2005)Rojelle LezamaNoch keine Bewertungen
- M10 Standards MVD Management DR C AtkinsDokument26 SeitenM10 Standards MVD Management DR C Atkinsveterinaria87Noch keine Bewertungen
- Myocardial Infarction Concept MapDokument7 SeitenMyocardial Infarction Concept Mapkarelclarke629280% (5)
- Advanced Cardiac Life SupportDokument37 SeitenAdvanced Cardiac Life SupportRoy Acosta GumbanNoch keine Bewertungen
- Dr. Rony M Santoso - ACS From Diagnosis To Long Term Treatment - Focus On Oral AntiplateletDokument25 SeitenDr. Rony M Santoso - ACS From Diagnosis To Long Term Treatment - Focus On Oral AntiplateletluckyariadneeNoch keine Bewertungen
- Arrhythmias EmergencyDokument10 SeitenArrhythmias EmergencyNITACORDEIRONoch keine Bewertungen
- Algorithm 1: Initial Evaluation and Management: Symptoms of Possible ACSDokument6 SeitenAlgorithm 1: Initial Evaluation and Management: Symptoms of Possible ACSNenyNoch keine Bewertungen
- EHC ED Critical Care Induced Hypothermia ProtocolDokument4 SeitenEHC ED Critical Care Induced Hypothermia ProtocolmaddythedocNoch keine Bewertungen
- Management of Common Cases in Emergency MedicineDokument55 SeitenManagement of Common Cases in Emergency MedicinemonpyitharNoch keine Bewertungen
- Controlling Heart Rate And/or RhythmDokument3 SeitenControlling Heart Rate And/or RhythmDaia DaiaNoch keine Bewertungen
- Controlling Heart Rate And/or RhythmDokument3 SeitenControlling Heart Rate And/or RhythmDaia DaiaNoch keine Bewertungen
- Atrial Fibrillation - Student ResidencyDokument6 SeitenAtrial Fibrillation - Student Residencyapi-404356063Noch keine Bewertungen
- Clinical Pathway StrokeDokument8 SeitenClinical Pathway StrokedjizhieeNoch keine Bewertungen
- Chest PainDokument5 SeitenChest PainAndrei MurariuNoch keine Bewertungen
- ST-Elevation Myocardial Infarction (Stemi) : Present byDokument29 SeitenST-Elevation Myocardial Infarction (Stemi) : Present byReema AlamriNoch keine Bewertungen
- QTC Flow Diagram With Medications Final Dec 17 A3 With LogosDokument1 SeiteQTC Flow Diagram With Medications Final Dec 17 A3 With LogosMelissa MurilloNoch keine Bewertungen
- Cardio BBDokument73 SeitenCardio BBايات عبدالرحمنNoch keine Bewertungen
- CCU HandoverDokument9 SeitenCCU Handoverapi-192342497Noch keine Bewertungen
- Management of Acute Coronary Syndrome / NSTEMI: Purpose of The GuidelineDokument7 SeitenManagement of Acute Coronary Syndrome / NSTEMI: Purpose of The GuidelineSahera Nurhidayah NasutionNoch keine Bewertungen
- CCU Clinical GuidelinesDokument63 SeitenCCU Clinical GuidelinesHAMMYER ALROKHAMINoch keine Bewertungen
- Af NoteDokument6 SeitenAf NoteMohammed SadoonNoch keine Bewertungen
- AMI CP EnglishDokument1 SeiteAMI CP EnglishNovema AsharNoch keine Bewertungen
- Treatment of Prolonged SeizuresDokument1 SeiteTreatment of Prolonged SeizuresAhmad ShukriNoch keine Bewertungen
- ACS LectureDokument55 SeitenACS LectureAyunda AlmiradaniNoch keine Bewertungen
- Acs 2023 Part 4 Presentation VersionDokument38 SeitenAcs 2023 Part 4 Presentation Versionapi-668470097Noch keine Bewertungen
- P ('t':'3', 'I':'669636497') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Dokument56 SeitenP ('t':'3', 'I':'669636497') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Muna NadiNoch keine Bewertungen
- 12 Hours: Continue To Monitor: High-Risk NSTEACSDokument1 Seite12 Hours: Continue To Monitor: High-Risk NSTEACSMeita ReligiaNoch keine Bewertungen
- Orthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingVon EverandOrthopedic Inpatient Protocols: A Guide to Orthopedic Inpatient RoundingNoch keine Bewertungen
- Alert Medical Series: Internal Medicine Alert I, II, IIIVon EverandAlert Medical Series: Internal Medicine Alert I, II, IIINoch keine Bewertungen
- Alert Medical Series: Emergency Medicine Alert I, II, IIIVon EverandAlert Medical Series: Emergency Medicine Alert I, II, IIINoch keine Bewertungen
- Amma Mobile InsuranceDokument1 SeiteAmma Mobile InsuranceANANTH JNoch keine Bewertungen
- Work Procedure For CCB Installation of Raised Floor 2Dokument13 SeitenWork Procedure For CCB Installation of Raised Floor 2ResearcherNoch keine Bewertungen
- Effects of Climate ChangeDokument10 SeitenEffects of Climate ChangeJan100% (1)
- Commodity FuturesDokument19 SeitenCommodity FuturesPrabhu G UmadiNoch keine Bewertungen
- Fem 3202-1 IntroductionDokument29 SeitenFem 3202-1 IntroductionRon ChongNoch keine Bewertungen
- Explorations in PersonalityDokument802 SeitenExplorations in Personalitypolz2007100% (8)
- 1 s2.0 S0149763418301957 MainDokument24 Seiten1 s2.0 S0149763418301957 MainjackNoch keine Bewertungen
- Z160-250 Instruction ManualDokument182 SeitenZ160-250 Instruction ManualNMA Industrial ServicesNoch keine Bewertungen
- 10893259-PIB 背钳弹簧保持架垫片落物事件Dokument2 Seiten10893259-PIB 背钳弹簧保持架垫片落物事件xlzyydf2015Noch keine Bewertungen
- Best WiFi Adapter For Kali Linux - Monitor Mode & Packet InjectionDokument14 SeitenBest WiFi Adapter For Kali Linux - Monitor Mode & Packet InjectionKoushikNoch keine Bewertungen
- Everything You Need to Know About Gas Metal Arc Welding (GMAWDokument31 SeitenEverything You Need to Know About Gas Metal Arc Welding (GMAWAhmetDuranCeyhanNoch keine Bewertungen
- Lesson Plan The Food: TH THDokument8 SeitenLesson Plan The Food: TH THFeraru FlorinNoch keine Bewertungen
- PGDHM SyllabusDokument34 SeitenPGDHM SyllabusankushlmpNoch keine Bewertungen
- Aquatic Ecology and LimnologyDokument96 SeitenAquatic Ecology and LimnologySale AlebachewNoch keine Bewertungen
- Solarizer Value, Spring & UltraDokument4 SeitenSolarizer Value, Spring & UltraEmmvee SolarNoch keine Bewertungen
- Unit 23 The Interior LandscapeDokument21 SeitenUnit 23 The Interior LandscapesNoch keine Bewertungen
- Duties and Responsibilities of Housekeeping Staff:-1) Executive Housekeeper/Director of HousekeepingDokument8 SeitenDuties and Responsibilities of Housekeeping Staff:-1) Executive Housekeeper/Director of HousekeepingsachinNoch keine Bewertungen
- HawkeyeDokument12 SeitenHawkeyeJanardhanam VaratharajanNoch keine Bewertungen
- Letter To Judge Anita Brody From Debra PykaDokument1 SeiteLetter To Judge Anita Brody From Debra PykaRobert LeeNoch keine Bewertungen
- Pnp-MemorandumDokument9 SeitenPnp-MemorandumraalphNoch keine Bewertungen
- Lab Report 1Dokument3 SeitenLab Report 1CarlEspantoNoch keine Bewertungen
- Blessed Are Those Who MournDokument7 SeitenBlessed Are Those Who MournPatrick MabbaguNoch keine Bewertungen
- Res Ipsa LoquiturDokument6 SeitenRes Ipsa LoquiturZydalgLadyz NeadNoch keine Bewertungen
- Traceability Summary - Supplies July 2015 - June 2016: PT Multimas Nabati Asahan, Kuala TanjungDokument4 SeitenTraceability Summary - Supplies July 2015 - June 2016: PT Multimas Nabati Asahan, Kuala TanjungAbu KhalidNoch keine Bewertungen
- 5 Ethiopian - National - Healthcare - Quality - and - Safety - Strategy - Final - Draft-July122021Dokument86 Seiten5 Ethiopian - National - Healthcare - Quality - and - Safety - Strategy - Final - Draft-July122021Kemal MahmoudNoch keine Bewertungen
- Reliance Tabletop SonicDokument20 SeitenReliance Tabletop SonicbrisaNoch keine Bewertungen
- Electrical: Mep Project Progress ReportDokument11 SeitenElectrical: Mep Project Progress ReportAvinash GuptaNoch keine Bewertungen
- Performance Task MidTerm Second Sem. AY 2022 2023Dokument2 SeitenPerformance Task MidTerm Second Sem. AY 2022 2023KZpathryn Jemimench AleurevNoch keine Bewertungen
- Viscometer Toki Sangyo - TV25 - 35Dokument12 SeitenViscometer Toki Sangyo - TV25 - 35Eddy CurrentNoch keine Bewertungen
- Vishal Seminar Report StrokeDokument40 SeitenVishal Seminar Report StrokeVishal kaushikNoch keine Bewertungen