Beruflich Dokumente
Kultur Dokumente
Cutaneous Abscess Furuncles and Carbucles
Hochgeladen von
azmmatgowher_12192660 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
62 Ansichten25 SeitenABOUT CUTANEOUS ABSCESS AND TREATMENT
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenABOUT CUTANEOUS ABSCESS AND TREATMENT
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
62 Ansichten25 SeitenCutaneous Abscess Furuncles and Carbucles
Hochgeladen von
azmmatgowher_1219266ABOUT CUTANEOUS ABSCESS AND TREATMENT
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 25
CUTANEOUS ABSCESS
FURUNCLES AND
CARBUCLES
DR AZMMAT GOWHER KHAN
A cutaneous abscess is a
localized collection of pus
in the skin and may occur
on any skin surface.
Cutaneous abscesses tend to
form in patients with bacterial
overgrowth, antecedent trauma
(particularly when a foreign
body is present), or
immunologic or circulatory
compromise
Symptoms and Signs
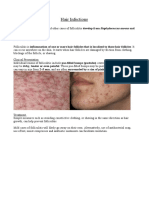
Cutaneous abscesses are painful, tender, indurated,
and sometimes erythematous.
They vary in size, typically 1 to 3 cm in length, but
sometimes much larger.
Initially the swelling is firm; later, as the abscess
“points,” the overlying skin becomes thin and feels
fluctuant. The abscess may then spontaneously drain.
Local cellulitis, lymphangitis, regional
lymphadenopathy, fever, and leukocytosis are variable
accompanying features.
ETIOLOGY
Bacteria causing cutaneous abscesses are
typically indigenous to the skin of the
involved area.
For abscesses on the trunk, extremities,
axillae, or head and neck, the most common
organisms are Staphylococcus aureus and
streptococci.
In recent years, methicillin-resistant S.
aureus(MRSA) has become a more common
cause.
.
Abscesses in the perineal (ie, inguinal,
vaginal, buttock, perirectal) region contain
organisms found in the stool, commonly
anaerobes or a combination of aerobes and
anaerobes.
Carbuncles and furuncles are follicle-based
cutaneous abscesses with characteristic
features
Diagnosis
Examination
Gram stain and culture
to identify MRSA
Diagnosis is usually obvious by
examination. Gram stain and
culture are recommended,
primarily to identify MRSA
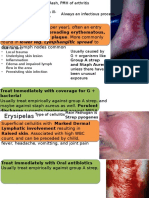
Treatment
Incision and drainage
Antibiotics
Some small abscesses resolve without
treatment, coming to a point and draining.
Warm compresses help accelerate the
process.
Incision and drainage are indicated when
significant pain, tenderness, and swelling
are present
It is unnecessary to await fluctuance. Under
sterile conditions, local anethesia is given as
either a lidocaine injection or a freezing
spray
Patients with large, extremely painful abscesses may
benefit from IV sedation and analgesia during
drainage.
A single puncture with the tip of a scalpel is often
sufficient to open the abscess.
After the pus drains, the cavity should be bluntly
probed with a gloved finger or curette to clear
loculations, and then irrigated with 0.9% saline
solution.
Some clinicians pack the cavity loosely with a gauze
wick that is removed 24 to 48 h later.
Local heat and elevation may hasten resolution of
inflammation
Antibiotics are unnecessary unless the patient has
signs of systemic infection, cellulitis, multiple
abscesses, immunocompromise, or a facial abscess in
the area drained by the cavernous sinus.
In these cases, empiric therapy should be started with
a drug active against MRSA
(eg,trimethoprim/sulfamethoxazole, clindamycin; for
severe infection, vancomycin) pending results of
bacterial culture.
Furuncles and Carbuncles
Furuncles also known as boils are skin abscesses
caused by staphylococcal infection, which involve a hair
follicle and surrounding tissue.
Carbuncles are clusters of furuncles connected
subcutaneously, causing deeper suppuration and
scarring.
They are smaller and more superficial than
subcutaneous abscesses
Both furuncles and carbuncles may affect healthy
young people but are more common in the obese,
the immunocompromised (including those
with neutrophil defects), the elderly, and possibly
those with diabetes.
Clustered cases may occur among those living in
crowded quarters with relatively poor hygiene or
among contacts of patients infected with virulent
strains.
Predisposing factors include bacterial
colonization of skin or nares,
hot and humid climates, and occlusion
or abnormal follicular anatomy (eg,
comedones in acne).
Methicillin-resistant Staphylococcus
aureus(MRSA) is a common cause.
Furuncles are common on the neck, breasts, face, and
buttocks.
They are uncomfortable and may be painful when
closely attached to underlying structures (eg, on the
nose, ear, or fingers).
Appearance is a nodule or pustule that discharges
necrotic tissue and sanguineous pus.
Carbuncles may be accompanied by fever and
prostration
Treatment
Drainage
Often antibiotics
effective against MRSA
Abscesses are incised and drained
. Intermittent hot compresses are used to
facilitate drainage.
Antibiotics, when used, should be effective
against MRSA, pending culture and
sensitivity test results.
In afebrile patients, treatment of a single
lesion < 5 mm requires no antibiotics.
If a single lesion is ≥ 5 mm, an oral
antibiotic is given for 5 to 10 days
Systemic antibiotics are also
need for
Lesions < 5 mm that do not
resolve with drainage
Evidence of expanding cellulitis
Immunocompromised patients
Patients at risk of endocarditis
Furuncles frequently recur and can be
prevented by applying liquid soap
containing either chlorhexidine gluconate
with isopropyl alcohol or 2 to 3%
chloroxylenol and by giving maintenance
antibiotics over 1 to 2 mo.
Patients with recurrent furunculosis should
be treated for predisposing factors such as
obesity, diabetes, occupational or industrial
exposure to inciting factors, and nasal
carriage of S. aureus or MRSA colonization.
THANK YOU
Das könnte Ihnen auch gefallen
- Pediatric ECG Survival Guide - 2nd - May 2019Dokument27 SeitenPediatric ECG Survival Guide - 2nd - May 2019Marcos Chusin MontesdeocaNoch keine Bewertungen
- CellulitisDokument39 SeitenCellulitisMary Jhane Villanueva50% (4)
- Christianity and Mental Health WEB VERSIONDokument64 SeitenChristianity and Mental Health WEB VERSIONWorld Religion NewsNoch keine Bewertungen
- 2017 - The Science and Technology of Flexible PackagingDokument1 Seite2017 - The Science and Technology of Flexible PackagingDaryl ChianNoch keine Bewertungen
- Infectious DermatosesDokument41 SeitenInfectious DermatosesJuma SammyNoch keine Bewertungen
- Cutaneous and Superficial Abscesses: Key Practice PointsDokument10 SeitenCutaneous and Superficial Abscesses: Key Practice PointsFofiuNoch keine Bewertungen
- Integument - Self StudyDokument4 SeitenIntegument - Self Studystudyhard001Noch keine Bewertungen
- Skin and Soft Tissue Infection InfoDokument4 SeitenSkin and Soft Tissue Infection InfoPresura Andreea IulianaNoch keine Bewertungen
- Skin InfectionsDokument5 SeitenSkin InfectionsKiara GovenderNoch keine Bewertungen
- Surgical Infections 025203Dokument80 SeitenSurgical Infections 025203Gracie KathyNoch keine Bewertungen
- DERMATOLOGY QuinterDokument177 SeitenDERMATOLOGY QuinterstaceyatienoomaNoch keine Bewertungen
- DermatologyDokument4 SeitenDermatologyZain Ul AbidinNoch keine Bewertungen
- Scabies 1Dokument25 SeitenScabies 1pmNoch keine Bewertungen
- P.S Very Nice!! May Pa-Picture Si Mayora!:D: FolliculitisDokument7 SeitenP.S Very Nice!! May Pa-Picture Si Mayora!:D: FolliculitisBea SartoNoch keine Bewertungen
- Diseases of External EarDokument19 SeitenDiseases of External EarMohamed Khaled TahaNoch keine Bewertungen
- Abses DMDokument19 SeitenAbses DMAngel MakinNoch keine Bewertungen
- Bacterial Skin Infections - Course VIIIDokument37 SeitenBacterial Skin Infections - Course VIIIAngelie PedregosaNoch keine Bewertungen
- Impetigo: Idowu O. A RN, M.SCDokument15 SeitenImpetigo: Idowu O. A RN, M.SCDebby Love GoodluckNoch keine Bewertungen
- Seminar 13Dokument10 SeitenSeminar 13TusharNoch keine Bewertungen
- BIOL 07 NotesDokument4 SeitenBIOL 07 NotesAdam MoncktonNoch keine Bewertungen
- Incision & Drainage of Abscess Group 9 4bDokument5 SeitenIncision & Drainage of Abscess Group 9 4bGUDISELA ramyaNoch keine Bewertungen
- Pressure UlcersDokument38 SeitenPressure UlcersRadwa EbedNoch keine Bewertungen
- Cellulitis - Biology Science Fair Project IdeasDokument4 SeitenCellulitis - Biology Science Fair Project IdeasEPFO AKURDINoch keine Bewertungen
- Biology Investigatory ProjectDokument16 SeitenBiology Investigatory ProjectpreranaNoch keine Bewertungen
- DR - Ali's Uworld Notes For Step 2 CKDokument19 SeitenDR - Ali's Uworld Notes For Step 2 CKuyesNoch keine Bewertungen
- Tinea Cruris Imp Points With ReferencesDokument35 SeitenTinea Cruris Imp Points With ReferencesSyed Saqib AliNoch keine Bewertungen
- N11 Chan Chloe Micropara 103 Compilation of Microbial Diseases Final RequirementDokument46 SeitenN11 Chan Chloe Micropara 103 Compilation of Microbial Diseases Final RequirementCHLOE CATHERINE CHANNoch keine Bewertungen
- Derm Quick ReviewDokument124 SeitenDerm Quick ReviewRohit NalamasuNoch keine Bewertungen
- Benign Vulvar Lesions: DR Sally Sayed El-Tawab Lecturer of Gyne-Oncology Alexandria UniversityDokument34 SeitenBenign Vulvar Lesions: DR Sally Sayed El-Tawab Lecturer of Gyne-Oncology Alexandria Universitysalah subbahNoch keine Bewertungen
- Skin and Soft Tissue Infectons 1Dokument51 SeitenSkin and Soft Tissue Infectons 1AISHWARYA T DNoch keine Bewertungen
- Cutaneous InfectionsDokument148 SeitenCutaneous InfectionsPratzNoch keine Bewertungen
- Veterinary Clinics: Management of Specific Skin WoundsDokument18 SeitenVeterinary Clinics: Management of Specific Skin WoundsGuadalupe Cristina Chuchón CáceresNoch keine Bewertungen
- Communicable Diseases of The Skin and EyeDokument37 SeitenCommunicable Diseases of The Skin and Eyemonica claritoNoch keine Bewertungen
- Incision and DrainageDokument33 SeitenIncision and DrainagemathisyncNoch keine Bewertungen
- Viral Wart - DermNet NZDokument6 SeitenViral Wart - DermNet NZMudassar SattarNoch keine Bewertungen
- Superficial Fungal Infections of The Skin VoiceoverDokument67 SeitenSuperficial Fungal Infections of The Skin VoiceoverMedo JT100% (1)
- ScabiesDokument3 SeitenScabiesMuthi AdilahNoch keine Bewertungen
- ScabiesDokument4 SeitenScabiesGenita Savitri EkandariNoch keine Bewertungen
- Fungal Skin Infections ملزمةDokument6 SeitenFungal Skin Infections ملزمةعبدالرحمن طارق عبدالله صالحNoch keine Bewertungen
- Maryville NURS 623 ExamDokument14 SeitenMaryville NURS 623 ExamWizzardNoch keine Bewertungen
- Candidiasis (Candidosis)Dokument17 SeitenCandidiasis (Candidosis)h8j5fnyh7dNoch keine Bewertungen
- Skin Disorders KKKDokument8 SeitenSkin Disorders KKKjhcacbszkjcnNoch keine Bewertungen
- Fungal InfectionsDokument9 SeitenFungal InfectionsCoral Srinivasa RamaluNoch keine Bewertungen
- Parasitic InfestationDokument37 SeitenParasitic Infestation051 DhinakarNoch keine Bewertungen
- Infantile Perineal Protrusion.: ChildhoodDokument4 SeitenInfantile Perineal Protrusion.: Childhoodcahaya tinggiNoch keine Bewertungen
- Tubkut Srilanka JournalDokument7 SeitenTubkut Srilanka JournalMusdalifah MimousNoch keine Bewertungen
- CarbunclesDokument15 SeitenCarbunclesMr DanielNoch keine Bewertungen
- Dermatological Conditions KOROS E.k-1Dokument107 SeitenDermatological Conditions KOROS E.k-1victorNoch keine Bewertungen
- Overview of Skin InfectionsDokument53 SeitenOverview of Skin Infectionsadamu mohammadNoch keine Bewertungen
- Bact InfcDokument54 SeitenBact Infciamazk1000Noch keine Bewertungen
- Continuing Medical Education: Amanda M M Oakley MBCHB Fracp DiphealinfDokument4 SeitenContinuing Medical Education: Amanda M M Oakley MBCHB Fracp DiphealinfCarol SantosNoch keine Bewertungen
- Infections of The Skin 2Dokument42 SeitenInfections of The Skin 2Kathleen Daban RagudoNoch keine Bewertungen
- Psoriasis: Posted: 02 Aug 2010 11:18 PM PDTDokument5 SeitenPsoriasis: Posted: 02 Aug 2010 11:18 PM PDTScamb TrekNoch keine Bewertungen
- Bact InfcDokument54 SeitenBact Infciamazk1000Noch keine Bewertungen
- Breast Infection: By: Dr. Ahmed Mukhtar ElkhatimDokument16 SeitenBreast Infection: By: Dr. Ahmed Mukhtar ElkhatimRachid LacNoch keine Bewertungen
- Abscess Incision and Drainage Part 2Dokument1 SeiteAbscess Incision and Drainage Part 2rahmaNoch keine Bewertungen
- Furunculosis (Boils) & Carbuncles: Essentials of DiagnosisDokument10 SeitenFurunculosis (Boils) & Carbuncles: Essentials of DiagnosisarbazNoch keine Bewertungen
- Superficcial MycosisDokument6 SeitenSuperficcial MycosisIM CTNoch keine Bewertungen
- Wound UlcersDokument42 SeitenWound UlcersMohammad Husni BanisalmanNoch keine Bewertungen
- Skin Pediatric NotesDokument8 SeitenSkin Pediatric NotesNursyNurseNoch keine Bewertungen
- Herpes - RomeroDokument9 SeitenHerpes - RomeroJanine Mae MacaraigNoch keine Bewertungen
- Sebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsVon EverandSebaceous Cyst, A Simple Guide To The Condition, Treatment And Related ConditionsBewertung: 5 von 5 Sternen5/5 (1)
- Steel and Timber Design: Arch 415Dokument35 SeitenSteel and Timber Design: Arch 415Glennson BalacanaoNoch keine Bewertungen
- Motion and Time: Check Your Progress Factual QuestionsDokument27 SeitenMotion and Time: Check Your Progress Factual QuestionsRahul RajNoch keine Bewertungen
- Economies of Scale in European Manufacturing Revisited: July 2001Dokument31 SeitenEconomies of Scale in European Manufacturing Revisited: July 2001vladut_stan_5Noch keine Bewertungen
- Sample A: For Exchange Students: Student's NameDokument1 SeiteSample A: For Exchange Students: Student's NameSarah AuliaNoch keine Bewertungen
- Understanding SIP RE-INVITEDokument6 SeitenUnderstanding SIP RE-INVITESK_shivamNoch keine Bewertungen
- CrisisDokument13 SeitenCrisisAngel Gaddi LarenaNoch keine Bewertungen
- Gastric Emptying PresentationDokument8 SeitenGastric Emptying Presentationrahul2kNoch keine Bewertungen
- Laboratory Methodsin ImmnunologyDokument58 SeitenLaboratory Methodsin Immnunologyadi pNoch keine Bewertungen
- Conductivity MeterDokument59 SeitenConductivity MeterMuhammad AzeemNoch keine Bewertungen
- PCI Bank V CA, G.R. No. 121413, January 29, 2001Dokument10 SeitenPCI Bank V CA, G.R. No. 121413, January 29, 2001ademarNoch keine Bewertungen
- Tangazo La Kazi October 29, 2013 PDFDokument32 SeitenTangazo La Kazi October 29, 2013 PDFRashid BumarwaNoch keine Bewertungen
- Political and Institutional Challenges of ReforminDokument28 SeitenPolitical and Institutional Challenges of ReforminferreiraccarolinaNoch keine Bewertungen
- DLP No. 10 - Literary and Academic WritingDokument2 SeitenDLP No. 10 - Literary and Academic WritingPam Lordan83% (12)
- BRAC BrochureDokument2 SeitenBRAC BrochureKristin SoukupNoch keine Bewertungen
- (Methods in Molecular Biology 1496) William J. Brown - The Golgi Complex - Methods and Protocols-Humana Press (2016)Dokument233 Seiten(Methods in Molecular Biology 1496) William J. Brown - The Golgi Complex - Methods and Protocols-Humana Press (2016)monomonkisidaNoch keine Bewertungen
- Syllabus Biomekanika Kerja 2012 1Dokument2 SeitenSyllabus Biomekanika Kerja 2012 1Lukman HakimNoch keine Bewertungen
- MSC in Healthcare Management (Top-Up) Degree From ARU - Delivered Online by LSBR, UKDokument19 SeitenMSC in Healthcare Management (Top-Up) Degree From ARU - Delivered Online by LSBR, UKLSBRNoch keine Bewertungen
- Materials System SpecificationDokument14 SeitenMaterials System Specificationnadeem shaikhNoch keine Bewertungen
- FPSCDokument15 SeitenFPSCBABER SULTANNoch keine Bewertungen
- Charles P. Jones, Investments: Analysis and Management, Eleventh Edition, John Wiley & SonsDokument20 SeitenCharles P. Jones, Investments: Analysis and Management, Eleventh Edition, John Wiley & SonsRizki AuliaNoch keine Bewertungen
- ListeningDokument2 SeitenListeningAndresharo23Noch keine Bewertungen
- Lista Agentiilor de Turism Licentiate Actualizare 16.09.2022Dokument498 SeitenLista Agentiilor de Turism Licentiate Actualizare 16.09.2022LucianNoch keine Bewertungen
- All Zone Road ListDokument46 SeitenAll Zone Road ListMegha ZalaNoch keine Bewertungen
- RESO NO. 4 - LANYARD FinalDokument1 SeiteRESO NO. 4 - LANYARD FinalsharonleefulloNoch keine Bewertungen
- Recent Cases On Minority RightsDokument10 SeitenRecent Cases On Minority RightsHarsh DixitNoch keine Bewertungen
- Session Guide - Ramil BellenDokument6 SeitenSession Guide - Ramil BellenRamilNoch keine Bewertungen
- Tour Guiding and Escort Services - 301Dokument95 SeitenTour Guiding and Escort Services - 301Zane 19531Noch keine Bewertungen