Beruflich Dokumente
Kultur Dokumente
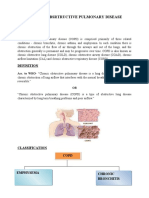
COPD
Hochgeladen von
pkm bungamas0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
43 Ansichten11 SeitenOriginaltitel
COPD.ppt
Copyright
© © All Rights Reserved
Verfügbare Formate
PPT, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
43 Ansichten11 SeitenCOPD
Hochgeladen von
pkm bungamasCopyright:
© All Rights Reserved
Verfügbare Formate
Als PPT, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 11
When performing spirometry, measure:
• Forced Vital Capacity (FVC) and
• Forced Expiratory Volume in one second
(FEV1)
Calculate the FEV1/FVC ratio
Spirometric results are expressed as %
Predicted using appropriate normal
values for the person’s sex, age, and
height.
Patients with COPD typically show a
decrease in both FEV1 and FEV1 /FVC.
The degree of spirometric abnormality
generally reflects the severity of COPD.
However, both symptoms and spirometry
should be considered when developing an
individulized management strategy for
each patient.
Classivication of COPD by Severity
Stage 0: At Risk – Chronic cough and sputum production;
lung function is still normal.
Stage I: Mild COPD – Mild airflow limitation (FEV1
/FVC<7% but FEV1≥80% predicted) and usually, but not
always, chronic cough and sputum production.
At this stage, the individual may not be aware that
his or her lung function is abnormal.
Stafe II: Moderate COPD – Worsening airflow
limitation (5%≤FEV1< 80% predicted), and usually the
progression of symptoms, with shortness of breath
typically developing on exertion.
Stage III: Severe COPD – Further worsening of airflow
limitation (30% ≤ FEV1<50% predicted), increased
shortness of breath, and repeated exacerbation which
have an impact on patients’ quality fo life.
• Exacerbations of symptoms, which have an impact on a patient’s
qulity of life and prognosis, are especially seen in patients with
FEV1 < 50% predicted.
Stage IV: Very Severe COPD – Severe airflow limitation
(FEV1 < 30% predicted) or the presence of chronic
respiratory failure. Patients may have very severe (stage
IV) COPD even if the FEV1 is > 30% predicted,
whenever these complications are present.
At this stage, quality of life is very appreciably impaired and
exacerbations may be life-threatening.
Differential Diagnosis: A Major differential
diagnosis is asthma. In some patients with
chronic asthma, a clear distinction from
COPD is not possible using current
imaging and physiological testing
techniques. In these patients, current
management is similar to that asthma.
Other potential diagnoses are usually
easier to distinguish from COPD (Figure
3).
Figure 3: Differential Diagnosis of COPD
Diagnosis Sugestiove Features*
COPD Onset in mid-life.
Symptoms slowly progressive.
Long smoking history
Dispnea during exercise
Largely irreversible airflow limitation
Asthma Onset early in life (often childhood).
Symptoms vary from day to day
Symptoms at night/early morning
Allergy, rhinitis, and/or eczema also present.
Largely reversible airflow limitation.
Congestive heart failure Fine basilar crackles on auscultation
Chest X-ray show dilated heart, pulmonary edema.
Pulmonary function tests indicate volume restriction,
not airflow limitation.
Bronchiectasis Large volumes of purulent sputum.
Commonly associated with bacterial infection.
Coarse crackles/clubbing on auscultation.
Chest X-ray/CT show bronchial dilation, bronchial
wall thickening.
Tuberculosis Onset all ages
Chest X-ray show lung infiltrate or nodular lesions
Microbiological confirmation
High local prevalence of tuberculosis
*these features tend to be characteristic of
the respective disease, but do not occur in
every case. For example, a person who
has never smoked may develop COPD
(especially in the developing world, where
other risk factors may be more important
than cigarette smoking); asthma may
develop in adult and even elderly patients.
Components of Care:
A COPD management program
The qoals of COPD management iclude:
Prevent disease progression
Relieve symptoms
Improve exercise tolerance
Improve health status
Prevent and treat complications
Prevent and treat exacerbations
Reduce mortality
Prevent or minimize side effects from treatmen.
Cessation of cigarette smoking should be included
as a goal throughout the management program.
These GOALS can be achieved through
implementation of a COPD management
program with four components:
1. Assess and monitor disease
2. Reduce risk factors
3. Manage stable COPD
4. Manage exacerbations
Component 1: Assess and Monitor Disease
A detailed medical history of a new patient known or
thought to have COPD should assess:
Exposure to risk factors, including intensity and duration.
Past medical history, including asthma, allergy, sinusitis or nasal
polyps, respiratory infection, and other respiratory diseases
Family history of COPD or other chronic respiratory disease
Pattern of symptom development.
History of exacerbations or previous hospitalizations for
respiratory disorder.
Presence of co morbidities, such as heart disease and rheumatic
disease, that may also contribute to restriction of activity
Appropriateness of current medical treatments.
Impact of disease on patient’s life, including limitation of activity;
missed work and economic impact; effect on family routines; and
feelings of depression or anxiety.
Social and family support available to the patient.
Possibilities fro reducing risk factors, especially smoking
cessation.
Das könnte Ihnen auch gefallen
- Asthma: Symptoms, Treatments, and Medication for Asthma and BronchitisVon EverandAsthma: Symptoms, Treatments, and Medication for Asthma and BronchitisNoch keine Bewertungen
- (Chronic Obstructive Pulmonary Disease) : Kelompok DDokument31 Seiten(Chronic Obstructive Pulmonary Disease) : Kelompok DErwin BawonoNoch keine Bewertungen
- 1.chronic Illness Overview and COPDDokument12 Seiten1.chronic Illness Overview and COPDOmar IzzoNoch keine Bewertungen
- COPDDokument38 SeitenCOPDMuhammad SulfikarNoch keine Bewertungen
- COPD Diet: A Beginner's 3-Week Step-by-Step Guide to Managing COPD Symptoms, With Curated Recipes and a Meal PlanVon EverandCOPD Diet: A Beginner's 3-Week Step-by-Step Guide to Managing COPD Symptoms, With Curated Recipes and a Meal PlanNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinDokument39 SeitenChronic Obstructive Pulmonary Disease (COPD) : Assistant Professor:Tong JinEINSTEIN2DNoch keine Bewertungen
- Asthma-COPD Overlap SyndromeDokument38 SeitenAsthma-COPD Overlap SyndromeSanjay NavaleNoch keine Bewertungen
- Copd-1 2023Dokument38 SeitenCopd-1 2023grim reaperNoch keine Bewertungen
- Copd and PneuDokument38 SeitenCopd and Pneuprogramgrabber100% (1)
- Asma Dan Penyakit Paru Obstruktif KronisDokument34 SeitenAsma Dan Penyakit Paru Obstruktif KronisAtikah ArifahNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD) : Diagnosis and ManagementDokument19 SeitenChronic Obstructive Pulmonary Disease (COPD) : Diagnosis and ManagementtiaranindyNoch keine Bewertungen
- Seminar (A5) - 1Dokument35 SeitenSeminar (A5) - 1mohamed6j19Noch keine Bewertungen
- The EssayDokument33 SeitenThe EssayAnonymous bLaVaKSbdBNoch keine Bewertungen
- COPD Case Pres2Dokument29 SeitenCOPD Case Pres2Kelly Queenie Andres100% (2)
- Copd PDFDokument28 SeitenCopd PDFDarawan MirzaNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD) : Assistant Sukhonos NDokument17 SeitenChronic Obstructive Pulmonary Disease (COPD) : Assistant Sukhonos NRayan Rayan darwishNoch keine Bewertungen
- Copd Case StudyDokument6 SeitenCopd Case StudyChrischia Yvonne GualbertoNoch keine Bewertungen
- K10 - Copd 2011Dokument47 SeitenK10 - Copd 20111e23e2ewNoch keine Bewertungen
- A Case Presentation On Chronic Obstructive Disease (COPD)Dokument18 SeitenA Case Presentation On Chronic Obstructive Disease (COPD)Harvey T. Dato-onNoch keine Bewertungen
- COPDDokument11 SeitenCOPDSherree HayesNoch keine Bewertungen
- #6 Copd 11 PDFDokument11 Seiten#6 Copd 11 PDFOmar BasimNoch keine Bewertungen
- DR: Adel Hamada: Bronchial Asthma and COPD Similarities AND DifferencesDokument20 SeitenDR: Adel Hamada: Bronchial Asthma and COPD Similarities AND DifferencesAdel HamadaNoch keine Bewertungen
- Description: Back To TopDokument21 SeitenDescription: Back To Toprovergzz88Noch keine Bewertungen
- Nur 111 Session 1 Sas 1Dokument8 SeitenNur 111 Session 1 Sas 1Zzimply Tri Sha UmaliNoch keine Bewertungen
- PT Case: Copd Exacerbation: DedicationDokument10 SeitenPT Case: Copd Exacerbation: DedicationDianaLopezBorjaNoch keine Bewertungen
- Seminar (GA5)Dokument59 SeitenSeminar (GA5)mohamed6j19Noch keine Bewertungen
- DR Ambreen Shams NephrologistDokument58 SeitenDR Ambreen Shams NephrologistAamer NaeemNoch keine Bewertungen
- Anaesthesia and CopdDokument7 SeitenAnaesthesia and CopdAshish PandeyNoch keine Bewertungen
- Bronchoobstrustive SyndromeDokument32 SeitenBronchoobstrustive SyndromeCk Kma67% (3)
- Case Study Sem 6Dokument42 SeitenCase Study Sem 6radicalmpNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument29 SeitenChronic Obstructive Pulmonary DiseasesivaNoch keine Bewertungen
- Copd by Musa Afridi 17-029Dokument6 SeitenCopd by Musa Afridi 17-029Essa AfridiNoch keine Bewertungen
- Astm ErsDokument9 SeitenAstm ErsAdrian RomanNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDokument12 SeitenChronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDiana Jalaynie S. SambolawanNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDokument12 SeitenChronic Obstructive Pulmonary Disease (COPD) Is A Condition ofDiana Jalaynie S. SambolawanNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument23 SeitenChronic Obstructive Pulmonary DiseaseLe RobertNoch keine Bewertungen
- Asthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaDokument7 SeitenAsthma: Chronic Inflammation of The Airways. The Hyper-Responsive Airways Typical of AsthmaRaj PaulNoch keine Bewertungen
- Merged 37Dokument21 SeitenMerged 37abdulkreemsalem4Noch keine Bewertungen
- COPD SlidesDokument27 SeitenCOPD SlidesMelito Vergara IINoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease: Laily Hidayati, S.Kep., NS., M.KepDokument55 SeitenChronic Obstructive Pulmonary Disease: Laily Hidayati, S.Kep., NS., M.KepGlory Stefanny NorotumilenaNoch keine Bewertungen
- Practice EamDokument35 SeitenPractice EamMYKRISTIE JHO MENDEZNoch keine Bewertungen
- Diagnosis of COPDDokument36 SeitenDiagnosis of COPDdrhrshitjainNoch keine Bewertungen
- Description: Chronic Bronchitis EmphysemaDokument16 SeitenDescription: Chronic Bronchitis EmphysemaJay-ar Zars0% (1)
- Patient Prep: Follow Guidelines On P. 65 of Clinical PacketDokument4 SeitenPatient Prep: Follow Guidelines On P. 65 of Clinical PacketKatherine AmbrosiaNoch keine Bewertungen
- Chronic Obsrtructive Pulmonary DiseaseDokument11 SeitenChronic Obsrtructive Pulmonary Diseasepreeti sharmaNoch keine Bewertungen
- CopdDokument47 SeitenCopdNingshesil Ny HermantNoch keine Bewertungen
- 70, - H 35 - H 2 - O N, L T: T: E G D - Develop A Self Management PlanDokument11 Seiten70, - H 35 - H 2 - O N, L T: T: E G D - Develop A Self Management PlanjljoioiuNoch keine Bewertungen
- Chronic Obstructive Pulmonary DiseaseDokument8 SeitenChronic Obstructive Pulmonary DiseaseYessamin Paith RoderosNoch keine Bewertungen
- Obstructive Pulmonary DiseasesDokument42 SeitenObstructive Pulmonary Diseasesbessan alfqeatNoch keine Bewertungen
- Case Study Sem 6Dokument41 SeitenCase Study Sem 6Mohd HarizNoch keine Bewertungen
- Bronkitis 2Dokument12 SeitenBronkitis 2Lucky PuspitasariNoch keine Bewertungen
- Asthma ApproachDokument7 SeitenAsthma ApproachpNoch keine Bewertungen
- Chronic Obstructive Pulmonary Disease (COPD)Dokument21 SeitenChronic Obstructive Pulmonary Disease (COPD)MudrekaNoch keine Bewertungen
- 4 Bronchial AsthmaDokument9 Seiten4 Bronchial Asthmashanfiza_92Noch keine Bewertungen
- COPD Student Lec DR Atef Alkarn 6-2022Dokument42 SeitenCOPD Student Lec DR Atef Alkarn 6-2022mohamed albnaNoch keine Bewertungen
- Copd in Primary CareDokument27 SeitenCopd in Primary CarerobyalfNoch keine Bewertungen
- COPDDokument23 SeitenCOPDUsamaNoch keine Bewertungen
- Topic 2 COPD and AsthmaDokument18 SeitenTopic 2 COPD and AsthmaCaitlynNoch keine Bewertungen
- Beginner To Intermediate Yoga-DYWMDokument6 SeitenBeginner To Intermediate Yoga-DYWMGeraldine QuintanaNoch keine Bewertungen
- Top Communicable Diseases in The Philippines 2019Dokument4 SeitenTop Communicable Diseases in The Philippines 2019Nicole cuencosNoch keine Bewertungen
- Illness BehaviorsDokument2 SeitenIllness BehaviorsJoi Ezra JumamilNoch keine Bewertungen
- Benign Malignant: Malignant Transformation: Retrovirus (RNA Virus)Dokument3 SeitenBenign Malignant: Malignant Transformation: Retrovirus (RNA Virus)ChiNoch keine Bewertungen
- Truscreen Cervical Screening SystemDokument39 SeitenTruscreen Cervical Screening SystemVyacheslav PilyaevNoch keine Bewertungen
- CompleteBloodCounts NORMAL VALUEDokument4 SeitenCompleteBloodCounts NORMAL VALUEWoro Hapsari Wahyuningrum100% (1)
- Polypharmacy in Elderly PatientsDokument7 SeitenPolypharmacy in Elderly PatientsMariana RibeiroNoch keine Bewertungen
- Post-Traumatic Stress Disorder Symptoms, ScreeningDokument4 SeitenPost-Traumatic Stress Disorder Symptoms, ScreeningDaniel RobertNoch keine Bewertungen
- 06 Feminist TherapyDokument26 Seiten06 Feminist TherapyPiter AriwijayaNoch keine Bewertungen
- Chapter 8. Vaginal and Vulvovaginal DisordersDokument22 SeitenChapter 8. Vaginal and Vulvovaginal DisordersMonica CiorneiNoch keine Bewertungen
- Theories of Counselling 5033: EducationDokument10 SeitenTheories of Counselling 5033: EducationheymuraliusNoch keine Bewertungen
- Heart AttackDokument12 SeitenHeart AttackPaul NeedhamNoch keine Bewertungen
- Drug DoseDokument23 SeitenDrug DoserajNoch keine Bewertungen
- 180-Day Exclusivity TrackerDokument4.005 Seiten180-Day Exclusivity Trackershah777Noch keine Bewertungen
- Clinical Pathway DengueDokument4 SeitenClinical Pathway Denguedr. Albertus S.ANoch keine Bewertungen
- Ijm 6 263Dokument6 SeitenIjm 6 263Nurlina NurdinNoch keine Bewertungen
- 21st Century Cures ActDokument312 Seiten21st Century Cures ActStephen LoiaconiNoch keine Bewertungen
- Morning Report Psychiatric DepartmentDokument51 SeitenMorning Report Psychiatric DepartmentaldensmagdalenaNoch keine Bewertungen
- Poster Presentations: 2009 The Authors Journal Compilation 2009 Blackwell Verlag GMBH - Mycoses, 52 (Suppl. 1), 29-123Dokument95 SeitenPoster Presentations: 2009 The Authors Journal Compilation 2009 Blackwell Verlag GMBH - Mycoses, 52 (Suppl. 1), 29-123Flávio VianiNoch keine Bewertungen
- AsthmaDokument2 SeitenAsthmaNaeem ZubairNoch keine Bewertungen
- Career Interest Profiler ReflectionDokument2 SeitenCareer Interest Profiler Reflectionapi-478464529Noch keine Bewertungen
- Anaesthetic Drugs Cheat SheetsDokument2 SeitenAnaesthetic Drugs Cheat SheetsPkern100% (3)
- Ah Chiropractic Billing GuideDokument8 SeitenAh Chiropractic Billing GuideHariharan SivaramagopalakrishnanNoch keine Bewertungen
- TitleDokument8 SeitenTitleBerms Flares FasoyNoch keine Bewertungen
- EcmoDokument81 SeitenEcmoBasantkumar SinghNoch keine Bewertungen
- Pearls in PPCDokument5 SeitenPearls in PPCRajinder Kumar BassanNoch keine Bewertungen
- Effects of Computer AddictionDokument11 SeitenEffects of Computer AddictionErich Trinidad33% (3)
- Management of Breast DisordersDokument17 SeitenManagement of Breast Disorderskhadzx100% (2)
- Bursitis Hip Exercises For Pain ReliefDokument8 SeitenBursitis Hip Exercises For Pain ReliefMark BeechNoch keine Bewertungen
- Kantar Article (2012) PsychopathologyDokument3 SeitenKantar Article (2012) PsychopathologyShelby Jones-StachnikNoch keine Bewertungen