Beruflich Dokumente
Kultur Dokumente
Meconium Aspiration
Hochgeladen von
WitneyGrace0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
89 Ansichten23 SeitenNeonatal Emergencies
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenNeonatal Emergencies
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
89 Ansichten23 SeitenMeconium Aspiration
Hochgeladen von
WitneyGraceNeonatal Emergencies
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 23
Niyaha Abdulrahim
Witney Grace Agad
Trexie Alimpoos
Aliah Ali
MECONIUM
ASPIRATION
Mindanao State University – College of Medicine
Department of Internal Medicine
MECONIUM
• first intestinal discharge of the newborn infant
• sterile, thick, black-green, odorless material
• contains epithelial cells, desquamated skin, fetal hair, mucus,
fatty acids, bile, water, proinflammatory components and
even drug metabolites
MECONIUM ASPIRATION
• aspiration of meconium-stained amniotic fluid in utero
• caused by acute or chronic hypoxia and/or infection in utero
• cause airway obstruction, interfere gas exchange, air
trapping and inflammatory response
• MAS Hallmark: poor lung compliance, hypoxemia and
characteristic lung radiograph
INCIDENCE
• varies from 8-20% of all deliveries
• only 5% develop to MAS and >50% requires mechanical
ventilatory support
• very low among pre-terms (absence of enzyme-MOTILIN)
RISK FACTORS FOR MSAF
• Age of gestation (esp. postmaturity)- highest in those
AOG >41 weeks
• SGA
• Placental Insufficiency
• Fetal Distress
• Cord compression
• Low 5 minute APGAR Score
PATHOPHYSIOLOGY
HORMONAL STIMULATION
PARASYMPATHETIC NEURAL MATURATION
Factors: Fetal Distress and Vagal Stimulation
Cause:
1. Bronchiolar Edema
2. Narrowing of Small Airways
PATHOPHYSIOLOGY
END RESULT:
1. Respiratory Failure
2. Persistent Pulmonary
Hypertension
MSAF
CLINICAL MANIFESTATIONS
Features of Infants
1. Often there are signs of postmaturity
2. Respiratory distress evident at birth or in transition period
a. Significant perinatal asphyxia may cause:
• respiratory depression with poor respiratory effort
• decreased muscle tone
b. Presenting Manifestation
• High respiratory rate ranging from 60-100 cpm
• Cyanosis, retractions, grunting, nasal flaring, inc. AP diameter of chest
• Rales, ronchi or wheezing
MSAF
CLINICAL MANIFESTATIONS
Features of Infants
3. Meconium staining-proportional to length of exposure and
meconium concentration
• Umbilical cord staining – 15mins exposure to thick MSAF or 1hr to lightly
stained fluid
• Yellowing staining of nails – 4-6hrs of exposure
• Staining of vernix caseosa - ~12hrs
MSAF
CLINICAL MANIFESTATIONS
General Features of Amniotic Fluid
1. Appearance and Viscosity
• green-stained fluid to thick “pea soup” consistency
DIFFERENTIAL DIAGNOSIS
1.Transient Tachypnea of the Newborn
2.Neonatal Pneumonia
3.Congenital Heart Disease
4.CNS Insult
5.Respiratory Distress Syndrome
DIAGNOSIS
Laboratory Studies
1. Arterial Blood Gas
• Hypoxemia
• Respiratory alkalosis secondary to hyperventilation
• Respiratory acidosis secondary to airway obstruction,
atelectasis, pneumonitis
• Metabolic acidosis secondary to perinatal asphyxia
DIAGNOSIS
Imaging Studies
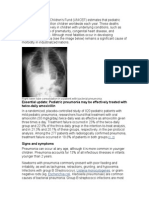
2. Chest Radiograph
• Hyperinflation of lung fields
• Flattened diaphragms
• Widened intercostal space
• Coarse, irregular patchy
infiltrates
• Central peri-hilar streaking
DIAGNOSIS
Cardiac Echocardiogram
1. Pulmonary Hypertension
2. Right to Left Atrial and Ductal Shunt
CBC and Blood Culture
Rule out and identify the cause of infection
MANAGEMENT
1. Prenatal Management
a. Identification of High-Risk Pregnancies
SAG, AOG, Hx of MSAF and Prolonged Labor
b. Monitoring during labor
Any signs of fetal distress
c. Amnioinfusion
With moderate or thick MSAF
MANAGEMENT
2. Delivery Room Management
a. Vigorous
Signs: spontaneous respirations, HR: >100 beats/min,
spontaneous movement and extremities on flexion
Management: Routine Care only should be provided
regardless of meconium consistency
suctioning
Initial steps in resuscitation: drying, warming, positioning
MANAGEMENT
2. Delivery Room Management
a. Depressed or Non-Vigorous
Signs: HR: <100bpm, airway obstruction (cyanotic and
gasping)
Management: intubated as quickly as feasible with
endotracheal tube connected to meconium trap aspirator
attached to wall suction at 100 mmHg.
CPAP or mechanical ventilation may be applied
MANAGEMENT
2. Management of newborn with meconium aspiration
a. General Management
Maintain a neutral thermal environment
Minimal handling protocol
Minimal adequate blood pressure and perfusion
Correct any metabolic abnormalities
Sedation
Gavage Feeding or Parenteral Nutrition
MANAGEMENT
2. Management of newborn with meconium aspiration
a. Respiratory Management
Pulmonary Toilet
Arterial Blood Gas Assessment
Oxygen Monitoring
Chest Radiograph
Antibiotic Coverage –Broad Spectrum
Mechanical Ventilation
Surfactant
Inhaled Nitric Oxide or Sildenafil
PROGNOSIS
• Complications are common and associated with
significant mortality
1. Meconium Aspiration Syndrome (due to hypoxia)
Global developmental delay
Cerebral palsy
Autism
Persistent Pulmonary Hypertension (15-30% mortality)
Pneumothorax and Pneumomediastinum
PROGNOSIS
• Complications are common and associated with
significant mortality
2. Prolonged Mechanical Ventilation
Bronchopulmonary dysplasia
Chronic lung disease
Warrants Long-term Follow-up
Das könnte Ihnen auch gefallen
- Meconium Aspiration Syndrome: Walter Otieno Consultant PaediatricianDokument27 SeitenMeconium Aspiration Syndrome: Walter Otieno Consultant PaediatricianMalueth AnguiNoch keine Bewertungen
- Poisoning in ChildrenDokument11 SeitenPoisoning in ChildrenAndriana HalfienNoch keine Bewertungen
- Abnormal OBDokument34 SeitenAbnormal OBLawrence NemirNoch keine Bewertungen
- Febrile Seizure Case FileDokument4 SeitenFebrile Seizure Case Filehttps://medical-phd.blogspot.comNoch keine Bewertungen
- Preterm Prelabour Rupture of MembranesDokument12 SeitenPreterm Prelabour Rupture of MembranesSeptiany Indahsari DjanNoch keine Bewertungen
- Transient Tachypnea of NewbornsDokument16 SeitenTransient Tachypnea of NewbornsSelena Marie0% (1)
- Tropical Splenomegaly SyndromeDokument12 SeitenTropical Splenomegaly SyndromeSaidAandySaida100% (1)
- Benign Ovarian TumorsDokument38 SeitenBenign Ovarian Tumorssimi yNoch keine Bewertungen
- Infants Diabetic MothersDokument17 SeitenInfants Diabetic MothersJaya PrabhaNoch keine Bewertungen
- Fanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsVon EverandFanconi Anemia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNoch keine Bewertungen
- HypertensionDokument6 SeitenHypertensionTj Kevin P-DoctorNoch keine Bewertungen
- Neonatal Jaundice DrkumarDokument44 SeitenNeonatal Jaundice Drkumarvasu_5iveNoch keine Bewertungen
- Top 93 Nursing SkillsDokument25 SeitenTop 93 Nursing SkillsericNoch keine Bewertungen
- Standard Treatment of Pyelonephritis in Pregnancy.4Dokument5 SeitenStandard Treatment of Pyelonephritis in Pregnancy.4Maria Fe Esperanza MadambaNoch keine Bewertungen
- PreeclampsiaDokument14 SeitenPreeclampsiaHenny NovitasariNoch keine Bewertungen
- Respiratory DistressDokument11 SeitenRespiratory DistressHina MasoodNoch keine Bewertungen
- Drugs in The Neonatal Unit: 1 Julia PettyDokument5 SeitenDrugs in The Neonatal Unit: 1 Julia PettyMarjoNoch keine Bewertungen
- 68 Abnormal PeuperiumDokument44 Seiten68 Abnormal PeuperiumGodsonYeboah-AwudziNoch keine Bewertungen
- Perinatal Asphyxia - Outline of Pathophysiology and Recent Trends in ManagementDokument31 SeitenPerinatal Asphyxia - Outline of Pathophysiology and Recent Trends in Managementokwadha simionNoch keine Bewertungen
- Φ PathophysiologyDokument4 SeitenΦ PathophysiologyMariah AshooriyanNoch keine Bewertungen
- Rle Neonate DrugsDokument13 SeitenRle Neonate DrugsLhara Vhaneza CuetoNoch keine Bewertungen
- Febrile SeizuresDokument11 SeitenFebrile SeizuresLita Al AmudiNoch keine Bewertungen
- MeaslesDokument23 SeitenMeaslesadwait marhattaNoch keine Bewertungen
- Obstetrics Case PresentationDokument27 SeitenObstetrics Case PresentationMahaprasad sahoo 77Noch keine Bewertungen
- Neonatal SepsisDokument51 SeitenNeonatal SepsisAngelo Del VentoNoch keine Bewertungen
- FBCDokument14 SeitenFBCJane GarciaNoch keine Bewertungen
- Neonatal PneumoniaDokument16 SeitenNeonatal Pneumoniaelyuchan100% (1)
- Essential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinDokument54 SeitenEssential Update: Pediatric Pneumonia May Be Effectively Treated With Twice-Daily AmoxicillinYostesara Maurena SantosaNoch keine Bewertungen
- Seminar 2 (Paeds)Dokument31 SeitenSeminar 2 (Paeds)Jonathan YeohNoch keine Bewertungen
- Airway Emergencies: ORL PostingDokument58 SeitenAirway Emergencies: ORL PostingKimberlyLaw95Noch keine Bewertungen
- Asthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDokument26 SeitenAsthmatic Attack: Miriti M.D Masters of Clinical Medicine Accidents and Emergency Facilitator: DR Simba DR MburuguDennis MiritiNoch keine Bewertungen
- Maternal InfectionsDokument31 SeitenMaternal InfectionsJane Ann AlolodNoch keine Bewertungen
- Peads NotesDokument18 SeitenPeads Notesechofox11Noch keine Bewertungen
- 4.3 LP 5 Hypovolemic Shock - PPSXDokument40 Seiten4.3 LP 5 Hypovolemic Shock - PPSXCamelia A. ParuschiNoch keine Bewertungen
- Bronchial AsthmaDokument21 SeitenBronchial AsthmashaitabliganNoch keine Bewertungen
- Haematinic Deficiencies (Iron, Vit B12 and Folate)Dokument7 SeitenHaematinic Deficiencies (Iron, Vit B12 and Folate)Francesca Li100% (1)
- Monitoring The Progress of Labor: Marissa Villacarlos Nualla, MD, Fpogs, Fpsuog Mcu-College of MedicineDokument58 SeitenMonitoring The Progress of Labor: Marissa Villacarlos Nualla, MD, Fpogs, Fpsuog Mcu-College of MedicineRozzie ReyesNoch keine Bewertungen
- Amniotic Band SyndromeDokument47 SeitenAmniotic Band SyndromeNazrul Islam JhinukNoch keine Bewertungen
- Surgical Problems in PregnancyDokument37 SeitenSurgical Problems in PregnancyCodillia CheongNoch keine Bewertungen
- Abruptio Placenta B-1Dokument29 SeitenAbruptio Placenta B-1drsachinhNoch keine Bewertungen
- LeukorrheaDokument29 SeitenLeukorrheaThorsang Chayovan100% (1)
- Management of Tuberculosis: A guide for clinicians (eBook edition)Von EverandManagement of Tuberculosis: A guide for clinicians (eBook edition)Noch keine Bewertungen
- Clinical Packet OBDokument7 SeitenClinical Packet OBLiza Jean BakerNoch keine Bewertungen
- Pregnancy Induced Hypertension: DefinitionDokument7 SeitenPregnancy Induced Hypertension: Definitionkristine hinaresNoch keine Bewertungen
- Gyne Past Papers Update 5Dokument139 SeitenGyne Past Papers Update 5Misbah KaleemNoch keine Bewertungen
- Case AppendicitisDokument30 SeitenCase AppendicitisSarahNoch keine Bewertungen
- Threatened AbortionDokument1 SeiteThreatened AbortionKEn PilapilNoch keine Bewertungen
- Protein Calorie MalnutritionDokument97 SeitenProtein Calorie Malnutritionnshaikh56Noch keine Bewertungen
- Ophthalmia NeonatorumDokument19 SeitenOphthalmia NeonatorumJisha Annie JohnNoch keine Bewertungen
- PnemoniaDokument38 SeitenPnemoniaArjumand AliNoch keine Bewertungen
- Heavy Menstrual BleedingDokument29 SeitenHeavy Menstrual BleedingsanjupainNoch keine Bewertungen
- Pediatric Asthma PDFDokument12 SeitenPediatric Asthma PDFzie_luph_taz13Noch keine Bewertungen
- Rubella and PregnancyDokument6 SeitenRubella and PregnancyKABERA RENENoch keine Bewertungen
- Diarrhea: WHO and IMCI GuidelinesDokument37 SeitenDiarrhea: WHO and IMCI GuidelinesJohn Christopher LucesNoch keine Bewertungen
- Placenta PreviaDokument33 SeitenPlacenta PreviamidoNoch keine Bewertungen
- Pre and Post PregnancyDokument23 SeitenPre and Post PregnancyJitendra ChaudharyNoch keine Bewertungen
- Hypothyroidism in PregnancyDokument29 SeitenHypothyroidism in PregnancyhanaddulNoch keine Bewertungen
- The Abnormal PuerperiumDokument25 SeitenThe Abnormal PuerperiumMartijn JohanNoch keine Bewertungen
- Ectopic Pregnancy - OMDokument9 SeitenEctopic Pregnancy - OMrheindNoch keine Bewertungen
- Case Presentation (IM)Dokument31 SeitenCase Presentation (IM)WitneyGraceNoch keine Bewertungen
- Lumbar PunctureDokument27 SeitenLumbar PunctureWitneyGrace100% (1)
- IV AccessDokument19 SeitenIV AccessWitneyGraceNoch keine Bewertungen
- Bone Marrow ExtractionDokument19 SeitenBone Marrow ExtractionWitneyGraceNoch keine Bewertungen
- Written Assignment Unit 2 - HS 2212Dokument5 SeitenWritten Assignment Unit 2 - HS 2212bnvjNoch keine Bewertungen
- 8. 학생 핸드북 (영문)Dokument33 Seiten8. 학생 핸드북 (영문)Eylül GülcemalNoch keine Bewertungen
- 3M Disposable Filtering Facepiece Respirator Fitting Poster English and SpanishDokument2 Seiten3M Disposable Filtering Facepiece Respirator Fitting Poster English and SpanishTrunggana AbdulNoch keine Bewertungen
- Full Employee ReportDokument3 SeitenFull Employee ReportXYZNoch keine Bewertungen
- RNA Columns NaOH Treatment RegenerationDokument7 SeitenRNA Columns NaOH Treatment RegenerationVageeshbabu HanurNoch keine Bewertungen
- Angelman Syndrome - Identification and ManagementDokument10 SeitenAngelman Syndrome - Identification and ManagementFajar YuniftiadiNoch keine Bewertungen
- Seminar and Topic ObjectivesDokument2 SeitenSeminar and Topic ObjectivesNeyo KatalbasNoch keine Bewertungen
- Procedure Checklist On OxygenationDokument2 SeitenProcedure Checklist On OxygenationKhatlen BagaresNoch keine Bewertungen
- Assisting For Endotracheal IntubationDokument16 SeitenAssisting For Endotracheal IntubationSREEDEVI T SURESH100% (1)
- South Asian AnthropologistDokument8 SeitenSouth Asian AnthropologistVaishali AmbilkarNoch keine Bewertungen
- Core CompetencyDokument9 SeitenCore CompetencyCharm BarinosNoch keine Bewertungen
- Advancements in The Bbutilization of Azolla Anabaena System in RelationDokument17 SeitenAdvancements in The Bbutilization of Azolla Anabaena System in Relationryana_soesantieNoch keine Bewertungen
- Brain Tumors - KY Cancer RegistryDokument45 SeitenBrain Tumors - KY Cancer RegistryMohammad Galih PratamaNoch keine Bewertungen
- OpdscheduleDokument14 SeitenOpdscheduleSrinidhi ChandraguthiNoch keine Bewertungen
- ProVari ManualDokument16 SeitenProVari ManualPatrickNoch keine Bewertungen
- 429-Article Text-1894-2-10-20210715Dokument12 Seiten429-Article Text-1894-2-10-20210715Ziya AstgaNoch keine Bewertungen
- 80020120LITPDFDokument37 Seiten80020120LITPDFPraistonNoch keine Bewertungen
- QUARTER 3 WEEK 3 English For Academic and PPDokument11 SeitenQUARTER 3 WEEK 3 English For Academic and PPCharmaine PearlNoch keine Bewertungen
- MSDS PDFDokument5 SeitenMSDS PDFdang2172014Noch keine Bewertungen
- Meditation ScriptDokument9 SeitenMeditation Scriptapi-361293242100% (1)
- Countryside in Figures 2019 Parañaque City PDFDokument282 SeitenCountryside in Figures 2019 Parañaque City PDFJaimee Ruth LiganNoch keine Bewertungen
- 21.JMM Promotion and Management, Inc. vs. Court of AppealsDokument3 Seiten21.JMM Promotion and Management, Inc. vs. Court of AppealsnathNoch keine Bewertungen
- UrethralstricturesDokument37 SeitenUrethralstricturesNinaNoch keine Bewertungen
- Golf Proposal 09Dokument7 SeitenGolf Proposal 09nrajentranNoch keine Bewertungen
- JHU Press Fall 2013 CatalogDokument99 SeitenJHU Press Fall 2013 CatalogjhupressNoch keine Bewertungen
- 5 Cover Letter Samples For Your Scientific ManuscriptDokument11 Seiten5 Cover Letter Samples For Your Scientific ManuscriptAlejandra J. Troncoso100% (2)
- Assisting Delivery Name: - Grade: - Year and Section: - DateDokument5 SeitenAssisting Delivery Name: - Grade: - Year and Section: - DateCrisia Jane LotaNoch keine Bewertungen
- Becky Ortiz ResumeDokument1 SeiteBecky Ortiz ResumeBecky OrtizNoch keine Bewertungen
- Di Specials. 2Dokument2 SeitenDi Specials. 2Ravindhar reddyNoch keine Bewertungen
- COSWPDokument7 SeitenCOSWPjquanNoch keine Bewertungen