Beruflich Dokumente
Kultur Dokumente
Hematothorax
Hochgeladen von
mail junk0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
101 Ansichten15 Seitenyuhuu semoga membantu
Copyright
© © All Rights Reserved
Verfügbare Formate
PPTX, PDF, TXT oder online auf Scribd lesen
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenyuhuu semoga membantu
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
0 Bewertungen0% fanden dieses Dokument nützlich (0 Abstimmungen)
101 Ansichten15 SeitenHematothorax
Hochgeladen von
mail junkyuhuu semoga membantu
Copyright:
© All Rights Reserved
Verfügbare Formate
Als PPTX, PDF, TXT herunterladen oder online auf Scribd lesen
Sie sind auf Seite 1von 15
Hemotorax
Hemothorax is the presence of blood in the pleural space, specifically
when the hematocrit of the pleural fluid is greater than or equal to 50%
of that of the peripheral blood.
Etiology
• Hemothorax is a frequent manifestation of traumatic injury (blunt or
penetrating) to thoracic structures.
• Most cases of hemothorax arise from blunt mechanism with an
overall mortality of 9.4%.
• Non-traumatic causes are less common. Examples include iatrogenic,
lung sequestration, vascular, neoplasia, coagulopathies, and
infectious processes.
Traumatic Hemothorax
• Blood may enter the pleural space from injury to the chest wall,
diaphragm, lung, blood vessels, or mediastinum.
• On entering the pleural space, the blood coagulates rapidly, but,
presumably as a result of the physical agitation produced by
movement of the heart and lungs, the clot may be defibrinated,
rendering it liquid and unable to clot again.
• Loculation may develop early in the course of hemothorax.
Mechanism of Injury
The mechanisms of action that were predictive of significant thoracic
injury are
• motor vehicle accident greater than 35 mph,
• fall from more than 15 feet,
• pedestrian ejection of more than 10 feet,
• trauma with depressed level of consciousness.
Anamnesis
Important history components include
• chest pain,
• dyspnea,
• mechanism of injury (fall, direction, and speed),
• drug/alcohol use,
• comorbidities,
• surgical history,
• anticoagulation/antiplatelet therapies.
Physical Examination
Clinical findings of hemothorax are broad and may overlap with pneumothorax; these include
• respiratory distress,
• tachypnea,
• decreased or absent breath sounds,
• dullness to percussion,
• chest wall asymmetry,
• tracheal deviation,
• hypoxia,
• narrow pulse pressure,
• hypotension.
• Inspect the chest wall for signs of contusion, abrasions, "seat belt sign," penetrating injury,
paradoxical movement ("flail chest”), ecchymosis, deformities, crepitus, and point
tenderness.
• Distended neck veins are concerning for pneumothorax or pericardial tamponade but might
be absent in the setting of hypovolemia.
• Increased respiratory rate, effort, and use of accessory muscles may be signs of impending
respiratory failure.
Imaging
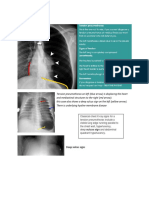
• Chest x-ray continues to be the initial diagnostic tool in the screening of traumatic
thoracic injuries.
• Chest x-ray reveals the presence of pleural fluid but does not prove it to be blood;
a preexisting pleural effusion would have an identical radiographic appearance.
• The CT scan is more sensitive than the chest radiograph in detecting
hemothoraces.
• CT scan of the chest is indicated for its ability to identify hemothorax, as well
as pneumothoraces, lung contusion, and bone fractures.
• Studies show that ultrasound is a superior diagnostic tool in detection of
traumatic thoracic injuries (e.g., pneumothorax and hemothorax)
• Ultrasound can detect as little as 20 ml of pleural fluid compared to 175 ml with
radiography, and is 100% sensitive for detecting effusions greater than 100 mL.
Physical Examination
The following physical findings should prompt the clinician to consider these
conditions:
• Distended neck veins → pericardial tamponade, tension pneumothorax, cardiogenic
failure, air embolism
• "Seat belt sign" → deceleration or vascular injury; chest wall contusion/abrasion
• Paradoxical chest wall movement → flail chest
• Facial/neck swelling or cyanosis → superior mediastinum injury with occlusion or
compression of superior vena cava (SVC)
• Subcutaneous emphysema → torn bronchus or lung parenchyma laceration
• Scaphoid abdomen → diaphragmatic injury with herniation of abdominal content
into the chest
• Excessive abdominal movement with breathing → chest wall injury
Treatment
• Minimal collection of blood (defined as less than 300 ml) in the
pleural cavity generally requires no treatment. Blood usually
reabsorbs throughout the course of several weeks.
• If the patient is stable and has minimal respiratory distress, operative
intervention is not typically required.
• This group of patients can be treated by analgesia as needed and
observed with repeated imaging at 4 to 6 hours and 24 hours
Treatment
• Immediate life-threatening injuries require prompt intervention, such
as decompression needle thoracostomy, and/or emergent tube
thoracostomy for large pneumothoraces
• With an aseptic approach, the tube thoracostomy is placed
posteriorly towards gravity-dependent fluid, in the fourth or fifth
intercostal space between the anterior and mid-axillary line.
• The thoracostomy tube is then connected to a water seal and suction
to facilitate rapid drainage and prevent air leakage. Furthermore, tube
insertion provides for blood quantification to determine if surgical
intervention is needed.
Treatment
According to the literature, indications for surgical intervention (urgent
anterior thoracotomy) include:
• 1500 ml of blood drainage in 24 hours through the chest tube
• 300-500 ml/hour for 2 to 4 consecutive hours after chest tube insertion
• Great vessel or chest wall injury
• Pericardial tamponade
Referensi
• Staub LJ, Biscaro RRM, Kaszubowski E, Maurici R. Chest ultrasonography for
the emergency diagnosis of traumatic pneumothorax and haemothorax: A
systematic review and meta-analysis. Injury. 2018 Mar;49(3):457-466.
• Soni NJ, Franco R, Velez MI, Schnobrich D, Dancel R, Restrepo MI, Mayo PH.
Ultrasound in the diagnosis and management of pleural effusions. J Hosp
Med. 2015 Dec;10(12):811-6.
• Morley EJ, Johnson S, Leibner E, Shahid J. Emergency department
evaluation and management of blunt chest and lung trauma (Trauma
CME). Emerg Med Pract. 2016 Jun;18(6):1-20.
• https://www.sciencedirect.com/topics/nursing-and-health-
professions/hematothorax
• https://www.ncbi.nlm.nih.gov/books/NBK538219/
TERIMA KASIH
Treatment
• Perform initial resuscitation and management of a trauma patient
according to the ATLS protocol.
• Every patient should have two large bore IVs access, be placed on a
cardiac and oxygen monitor, and have a 12-lead EKG.
• Immediate life-threatening injuries require prompt intervention, such
as decompression needle thoracostomy, and/or emergent tube
thoracostomy for large pneumothoraces, and initial management of
hemothorax.
Das könnte Ihnen auch gefallen
- Referat HemothoraksDokument28 SeitenReferat HemothoraksitsmediNoch keine Bewertungen
- Penetrating Chest Trauma With Massive Hemothorax by A Small StoneDokument2 SeitenPenetrating Chest Trauma With Massive Hemothorax by A Small Stoneputri firda erlinaNoch keine Bewertungen
- Review ArdsDokument25 SeitenReview ArdsAdel HamadaNoch keine Bewertungen
- ARDS (Dr. Edi Nurtjahja - SP.P)Dokument23 SeitenARDS (Dr. Edi Nurtjahja - SP.P)Mirna Ayu Permata SariNoch keine Bewertungen
- Lung Abscess Handout PDFDokument3 SeitenLung Abscess Handout PDFTansanee MalivalayaNoch keine Bewertungen
- Ards 2Dokument7 SeitenArds 2LUCIBELLOT1Noch keine Bewertungen
- ARDSDokument81 SeitenARDSShanaz NovriandinaNoch keine Bewertungen
- PleurodesisDokument30 SeitenPleurodesisEliana Muis100% (1)
- Fat Embolism SyndromeDokument19 SeitenFat Embolism SyndromeFaizah AlmuhsinNoch keine Bewertungen
- DR Muhammed AslamDokument56 SeitenDR Muhammed AslamSef NengkoNoch keine Bewertungen
- Bronchiectasis: Prepared By: Michelle TamorDokument17 SeitenBronchiectasis: Prepared By: Michelle TamorMichelle TamorNoch keine Bewertungen
- Pneumothorax FinalDokument62 SeitenPneumothorax FinalmithramuruganNoch keine Bewertungen
- Lecture Secondary TuberculosisDokument78 SeitenLecture Secondary TuberculosisslyfoxkittyNoch keine Bewertungen
- Copd PDFDokument28 SeitenCopd PDFDarawan MirzaNoch keine Bewertungen
- Tension PneumothoraxDokument5 SeitenTension PneumothoraxKay BristolNoch keine Bewertungen
- Tension PneumothoraxDokument9 SeitenTension PneumothoraxFadilla Rizki PutriNoch keine Bewertungen
- PneumothoraxDokument43 SeitenPneumothoraxSravani KanchiNoch keine Bewertungen
- Diagnosis and Management of Shock: Dr. Nurkhalis, SPJP, FihaDokument51 SeitenDiagnosis and Management of Shock: Dr. Nurkhalis, SPJP, FihaHilmaNoch keine Bewertungen
- Chest Tube ManagementDokument27 SeitenChest Tube ManagementIanne Merh100% (2)
- COPDDokument73 SeitenCOPDBroken OreosNoch keine Bewertungen
- Restrictive Lung DiseaseDokument32 SeitenRestrictive Lung DiseaseSalman Khan100% (1)
- Chronic Obstructive Pulmonary Disease: Olivia Faye J Listanco IM Resident January 21, 2016Dokument52 SeitenChronic Obstructive Pulmonary Disease: Olivia Faye J Listanco IM Resident January 21, 2016FayeListancoNoch keine Bewertungen
- Pharmacotherapy For COPD: Prepared ByDokument35 SeitenPharmacotherapy For COPD: Prepared ByYogi RavalNoch keine Bewertungen
- Interstitial Lung Disease Diffuse Parenchymal Lung DiseaseDokument59 SeitenInterstitial Lung Disease Diffuse Parenchymal Lung Diseaseapi-19641337Noch keine Bewertungen
- Update in Diagnosis and Management of Interstitial Lung DiseaseDokument8 SeitenUpdate in Diagnosis and Management of Interstitial Lung DiseaseTimothy23 SiregarNoch keine Bewertungen
- Eff Pleura & PneumothoraxDokument69 SeitenEff Pleura & PneumothoraxUswatun Hasanah RINoch keine Bewertungen
- COPD NotesDokument38 SeitenCOPD NotesKudingLimMingYaoNoch keine Bewertungen
- Diagnostic Thoracoscopy (VATS) in Lung CancerDokument18 SeitenDiagnostic Thoracoscopy (VATS) in Lung CancerlmdarlongNoch keine Bewertungen
- Understanding Mechanical Ventilation: Jennifer Zanni, PT, DSCPT Johns Hopkins HospitalDokument52 SeitenUnderstanding Mechanical Ventilation: Jennifer Zanni, PT, DSCPT Johns Hopkins HospitalDeepa BhattacharjeeNoch keine Bewertungen
- Hypovolemic ShockDokument2 SeitenHypovolemic ShocklarklowNoch keine Bewertungen
- CopdDokument74 SeitenCopdSardor AnorboevNoch keine Bewertungen
- Acute Limb IschemicDokument32 SeitenAcute Limb IschemicAnanda YulianNoch keine Bewertungen
- Acute Respiratory Failure: R. Bhakialakshmi M.Sc. Nursing 2 Year PSG College of NursingDokument31 SeitenAcute Respiratory Failure: R. Bhakialakshmi M.Sc. Nursing 2 Year PSG College of NursingassumptaNoch keine Bewertungen
- 13Lec-Approach To Neonates With Suspected Congenital InfectionsDokument56 Seiten13Lec-Approach To Neonates With Suspected Congenital InfectionsMinerva Stanciu100% (1)
- PleurodesisDokument6 SeitenPleurodesisKlit TongNoch keine Bewertungen
- CopdDokument29 SeitenCopdRidha SyahputraNoch keine Bewertungen
- AtelectasisDokument28 SeitenAtelectasisShikha Acharya100% (1)
- Cor PulmonaleDokument8 SeitenCor PulmonaleAymen OmerNoch keine Bewertungen
- 06prof. Riwanto-Abdominal Compartment SyndromeDokument41 Seiten06prof. Riwanto-Abdominal Compartment SyndromeTanujaa Venugopal100% (1)
- Abdominal Compartment Syndrome: By: Adel Ghuloom, MD Lubna Kamaldien, MDDokument42 SeitenAbdominal Compartment Syndrome: By: Adel Ghuloom, MD Lubna Kamaldien, MDnanang anacardia Subagyo100% (1)
- COPD SlidesDokument27 SeitenCOPD SlidesMelito Vergara IINoch keine Bewertungen
- Suppurative Lung Diseases: DR Faisal Moidunny Mammu Department of PaediatricsDokument39 SeitenSuppurative Lung Diseases: DR Faisal Moidunny Mammu Department of PaediatricsFaisal MoidunnyNoch keine Bewertungen
- Acute Lung Injury/Acute Respiratory Distress Syndrome: Deepak Mulajker, Vasu Vardhan, AK NagpalDokument6 SeitenAcute Lung Injury/Acute Respiratory Distress Syndrome: Deepak Mulajker, Vasu Vardhan, AK NagpalDeepak MulajkerNoch keine Bewertungen
- 2023.2024chronic Obstructive Pulmonary DiseaseDokument17 Seiten2023.2024chronic Obstructive Pulmonary Diseasesameh EidNoch keine Bewertungen
- Pneumocystis Carinii PneumoniaDokument16 SeitenPneumocystis Carinii PneumoniaHera HeraNoch keine Bewertungen
- Diagnosis of PneumoconiosisDokument55 SeitenDiagnosis of PneumoconiosiselsaNoch keine Bewertungen
- Endotracheal Intubation: Oleh: Dr. Natalia Rasta M Pembimbing: Dr. Eko Widya, Sp. EMDokument22 SeitenEndotracheal Intubation: Oleh: Dr. Natalia Rasta M Pembimbing: Dr. Eko Widya, Sp. EMNatalia RastaNoch keine Bewertungen
- FOM STUDY GUIDE 3rd Block 1Dokument3 SeitenFOM STUDY GUIDE 3rd Block 1Bernadine Cruz Par100% (1)
- Description of DiseaseDokument10 SeitenDescription of DiseaseRajaNoch keine Bewertungen
- Ccam N Bps Management PDFDokument9 SeitenCcam N Bps Management PDFEthan AmalNoch keine Bewertungen
- Lung AbscessDokument25 SeitenLung AbscessIskandar HasanNoch keine Bewertungen
- Efusi Pleura TBDokument35 SeitenEfusi Pleura TBAlfina Aulia RizkiNoch keine Bewertungen
- Acute Respiratory Distress SyndromeDokument3 SeitenAcute Respiratory Distress SyndromedindayantNoch keine Bewertungen
- 3 - Flail ChestDokument3 Seiten3 - Flail ChestKrishna Chaitanya GovardhanamNoch keine Bewertungen
- Journal StrokeDokument5 SeitenJournal StrokeRika Sartyca IlhamNoch keine Bewertungen
- Acute Respiratory FailureDokument34 SeitenAcute Respiratory FailureStuDIEng100% (1)
- Pulmonary HypertensionDokument26 SeitenPulmonary Hypertensionakoeljames8543Noch keine Bewertungen
- Torso TraumaDokument37 SeitenTorso TraumaFiza MushtaqNoch keine Bewertungen
- Chest Injury and Its TypesDokument14 SeitenChest Injury and Its TypesKoochi PoojithaNoch keine Bewertungen
- HemothoraxDokument27 SeitenHemothoraxShreyasi AnkushNoch keine Bewertungen
- Acquired Microcephaly: Causes, Patterns, Motor and IQ Effects, and Associated Growth ChangesDokument8 SeitenAcquired Microcephaly: Causes, Patterns, Motor and IQ Effects, and Associated Growth Changesmail junkNoch keine Bewertungen
- KHI Fact Sheet Template Aug 2014Dokument1 SeiteKHI Fact Sheet Template Aug 2014mail junkNoch keine Bewertungen
- Pengaruh Asfiksia Terhadap Ukuran Lingkar Kepala Anak Usia 6 Bulan - 2 Tahun Di Rumah Sakit Umum Provinsi Nusa Tenggara BaratDokument9 SeitenPengaruh Asfiksia Terhadap Ukuran Lingkar Kepala Anak Usia 6 Bulan - 2 Tahun Di Rumah Sakit Umum Provinsi Nusa Tenggara Baratmail junkNoch keine Bewertungen
- Hubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouDokument6 SeitenHubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouIsmi NfNoch keine Bewertungen
- Pengaruh Hipoglikemia Pada Pasien Diabetes MelitusDokument8 SeitenPengaruh Hipoglikemia Pada Pasien Diabetes Melitusmail junkNoch keine Bewertungen
- Hubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouDokument6 SeitenHubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouIsmi NfNoch keine Bewertungen
- Pengaruh Hipoglikemia Pada Pasien Diabetes Melitus Tipe 2 Terhadap Kepatuhan Terapi Dan Kualitas HidupDokument8 SeitenPengaruh Hipoglikemia Pada Pasien Diabetes Melitus Tipe 2 Terhadap Kepatuhan Terapi Dan Kualitas Hidupilma adilla syahidaNoch keine Bewertungen
- Hubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouDokument6 SeitenHubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouIsmi NfNoch keine Bewertungen
- WHO Growth Chart Boy - Draft 01 - 1425701689Dokument54 SeitenWHO Growth Chart Boy - Draft 01 - 1425701689silentnewbie100% (1)
- Block 3.3 Sesi 3 Pathology of Urinary Tract: by Asdos 2011: Vetta Awe Eric Lily Fiko Ghana Ikal Linda May FahmiDokument96 SeitenBlock 3.3 Sesi 3 Pathology of Urinary Tract: by Asdos 2011: Vetta Awe Eric Lily Fiko Ghana Ikal Linda May Fahmimail junkNoch keine Bewertungen
- Hubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouDokument6 SeitenHubungan Lingkar Kepala Dan Perkembangan Bayi Di Poli Bayi & Tumbuh Kembang Rsup Prof. Dr. R. D. KandouIsmi NfNoch keine Bewertungen
- Travel Reservation April 16 For MISS NINDI DESHERA PUTRIDokument1 SeiteTravel Reservation April 16 For MISS NINDI DESHERA PUTRImail junkNoch keine Bewertungen
- Wellness and Wellness and Healthy Magazine Healthy MagazineDokument10 SeitenWellness and Wellness and Healthy Magazine Healthy Magazinealien babycutiehoneypieNoch keine Bewertungen
- Acquired Microcephaly: Causes, Patterns, Motor and IQ Effects, and Associated Growth ChangesDokument8 SeitenAcquired Microcephaly: Causes, Patterns, Motor and IQ Effects, and Associated Growth Changesmail junkNoch keine Bewertungen
- Pengaruh Asfiksia Terhadap Ukuran Lingkar Kepala Anak Usia 6 Bulan - 2 Tahun Di Rumah Sakit Umum Provinsi Nusa Tenggara BaratDokument9 SeitenPengaruh Asfiksia Terhadap Ukuran Lingkar Kepala Anak Usia 6 Bulan - 2 Tahun Di Rumah Sakit Umum Provinsi Nusa Tenggara Baratmail junkNoch keine Bewertungen
- This Is Your Presentation TitleDokument40 SeitenThis Is Your Presentation TitleArnold UrbinaNoch keine Bewertungen
- Cordelia SlidesCarnivalDokument40 SeitenCordelia SlidesCarnivalEnzo Alcívar ThomasNoch keine Bewertungen
- BroDokument14 SeitenBromail junkNoch keine Bewertungen
- WHO Growth Chart Girl - Draft 01 - 243678126Dokument52 SeitenWHO Growth Chart Girl - Draft 01 - 243678126silentnewbieNoch keine Bewertungen
- Tutorial Gizi Dasar 2015 UTK MHS Edit 23 Agustus 16Dokument8 SeitenTutorial Gizi Dasar 2015 UTK MHS Edit 23 Agustus 16mail junkNoch keine Bewertungen
- Lower LimbDokument7 SeitenLower Limbmail junkNoch keine Bewertungen
- Ham ADokument1 SeiteHam Araj1969Noch keine Bewertungen
- Review: The Changing Face of Pneumonia Maids PatientsDokument9 SeitenReview: The Changing Face of Pneumonia Maids Patientsmail junkNoch keine Bewertungen
- Hap Vap Guidelines 2016 PDFDokument51 SeitenHap Vap Guidelines 2016 PDFJerryEddyaPutraBoerNoch keine Bewertungen
- Ok TC FlotationDokument4 SeitenOk TC FlotationWilliam SalcedoNoch keine Bewertungen
- A Ongc HRM Summer ProjectDokument58 SeitenA Ongc HRM Summer ProjectAmit SunsaraNoch keine Bewertungen
- At Home Activities Mathlink Cubes Big BuildersDokument7 SeitenAt Home Activities Mathlink Cubes Big BuildersdrchiNoch keine Bewertungen
- A Report On External Analysis of Construction in NepalDokument13 SeitenA Report On External Analysis of Construction in Nepalsubash upretiNoch keine Bewertungen
- Introduction On Photogrammetry Paul R WolfDokument33 SeitenIntroduction On Photogrammetry Paul R Wolfadnan yusufNoch keine Bewertungen
- Denel Dynamics Product Brochure PDFDokument36 SeitenDenel Dynamics Product Brochure PDFeggboy196967% (3)
- Ancient CivilizationsDokument9 SeitenAncient CivilizationsMarienne LaoNoch keine Bewertungen
- Feeg2003 L21Dokument9 SeitenFeeg2003 L21jiales225Noch keine Bewertungen
- Sustainability Schematic ReportDokument5 SeitenSustainability Schematic ReportsakhrNoch keine Bewertungen
- Method Statement For Boom Barrier Installation (Rev00) ELV2Dokument38 SeitenMethod Statement For Boom Barrier Installation (Rev00) ELV2balajiNoch keine Bewertungen
- Bravo Petroleum ProfileDokument8 SeitenBravo Petroleum ProfileJacob Thom ZiwahwaNoch keine Bewertungen
- Subcontracting Process in Production - SAP BlogsDokument12 SeitenSubcontracting Process in Production - SAP Blogsprasanna0788Noch keine Bewertungen
- Neo Neurophone Patrick FlanaganDokument2 SeitenNeo Neurophone Patrick FlanaganalexanderjfernandesNoch keine Bewertungen
- SBB Product NoteDokument3 SeitenSBB Product NoteFilipe MartinsNoch keine Bewertungen
- 10 Powerful Mudras and How To Use Them: 1. GyanDokument4 Seiten10 Powerful Mudras and How To Use Them: 1. GyanAkrithi Akrithi100% (1)
- Green Revolution: It's Acheivements and FailuresDokument24 SeitenGreen Revolution: It's Acheivements and FailuresSingh HarmanNoch keine Bewertungen
- Euroncap 2017 Audi q5 DatasheetDokument13 SeitenEuroncap 2017 Audi q5 DatasheetCosmin AnculiaNoch keine Bewertungen
- Stephane Moses The Angel of History Rosenzweig Benjamin Scholem PDFDokument196 SeitenStephane Moses The Angel of History Rosenzweig Benjamin Scholem PDFlivehuman100% (3)
- Harmonization of HR Policies - RoughDokument119 SeitenHarmonization of HR Policies - RoughFrancis SoiNoch keine Bewertungen
- 13 - Oxygen Removal From Boiler WaterDokument12 Seiten13 - Oxygen Removal From Boiler Waterarunkumar23101100% (1)
- Electrical Circuits 1 QPDokument7 SeitenElectrical Circuits 1 QPKitty MinogueNoch keine Bewertungen
- Neurology Condition Assessment Methods: Guillain-Barre Syndrome (GBS) Disability ScoreDokument15 SeitenNeurology Condition Assessment Methods: Guillain-Barre Syndrome (GBS) Disability ScoreMrinmayeeDeshmukhNoch keine Bewertungen
- Comic Book Paramhansa YoganandaDokument36 SeitenComic Book Paramhansa Yoganandaarjuna198986% (7)
- Specifications: Louie Jean Mabanag Ar - 3BDokument8 SeitenSpecifications: Louie Jean Mabanag Ar - 3BLouie Jean100% (1)
- Bruker d8 XRD TutoriallDokument16 SeitenBruker d8 XRD TutoriallravarNoch keine Bewertungen
- BJT Common Emitter Characteristics: Experiment 6Dokument5 SeitenBJT Common Emitter Characteristics: Experiment 6beesahNoch keine Bewertungen
- 8 - Precast Concrete Structures-Students PDFDokument17 Seiten8 - Precast Concrete Structures-Students PDFsitehabNoch keine Bewertungen
- English: Third Quarter - Module 3Dokument12 SeitenEnglish: Third Quarter - Module 3Anna Agravante-SulitNoch keine Bewertungen
- Honda Bikes and ScootersDokument6 SeitenHonda Bikes and ScootersShamrjit AgrahariNoch keine Bewertungen