Beruflich Dokumente
Kultur Dokumente
Allergic Skin
Hochgeladen von
Ryan Luqman HamdaniOriginalbeschreibung:
Copyright
Verfügbare Formate
Dieses Dokument teilen
Dokument teilen oder einbetten
Stufen Sie dieses Dokument als nützlich ein?
Sind diese Inhalte unangemessen?
Dieses Dokument meldenCopyright:
Verfügbare Formate
Allergic Skin
Hochgeladen von
Ryan Luqman HamdaniCopyright:
Verfügbare Formate
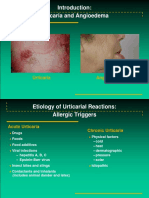
Introduction: Urticaria and Angioedema
Urticaria
Angioedema
Etiology of Urticarial Reactions: Allergic Triggers
Acute Urticaria
Drugs Foods
Chronic Urticaria
Food additives
Viral infections hepatitis A, B, C Epstein-Barr virus
Physical factors cold heat dermatographic pressure solar
Idiopathic
Insect bites and stings
Contactants and inhalants (includes animal dander and latex)
The Pathogenesis of Chronic Urticaria: Cellular Mediators
Histamine as a Mast Cell Mediator
Role of Mast Cells in Chronic Urticaria: Lower Threshold for Histamine Release
Cutaneous mass cell
Release threshold decreased by:
Cytokines & chemokines in the cutaneous microenvironment Antigen exposure Histamine-releasing factor Autoantibody Psychological factors
Release threshold increased by:
Corticosteroids Antihistamines Cromolyn (in vitro)
An Autoimmune Basis for Chronic Idiopathic Urticaria: Antibodies to IgE
Initial Workup of Urticaria
Patient history
Physical exam
Sinusitis Arthritis Thyroid disease Cutaneous fungal infections Urinary tract symptoms Upper respiratory tract infection (particularly important in children) Travel history (parasitic infection) Sore throat Epstein-Barr virus, infectious mononucleosis Insect stings Foods Recent transfusions with blood products (hepatitis) Recent initiation of drugs
Skin Eyes Ears Throat Lymph nodes Feet Lungs Joints Abdomen
Laboratory Assessment for Chronic Urticaria
Initial tests
CBC with differential Erythrocyte sedimentation rate Urinalysis
Possible tests for selected patients
Stool examination for ova and parasites Blood chemistry profile Antinuclear antibody titer (ANA) Hepatitis B and C Skin tests for IgE-mediated reactions
RAST for specific IgE Complement studies: CH50 Cryoproteins Thyroid microsomal antibody Antithyroglobulin Thyroid stimulating hormone (TSH)
Histopathology
Group 2:
Polymorphous perivascular infiltrate Neutrophils Eosinophils Mononuclear cells
Group 3:
Sparse perivascular lymphocytes
Urticaria Associated With Other Conditions
Collagen vascular disease (eg, systemic lupus erythematosus) Complement deficiency, viral infections (including hepatitis B and C), serum sickness, and allergic drug eruptions Chronic tinea pedis Pruritic urticarial papules and plaques of pregnancy (PUPPP) Schnitzlers syndrome
H1-Receptor Antagonists: Pros and Cons for Urticaria and Angioedema
First-generation antihistamines (diphenhydramine and hydroxyzine)
Advantages: Rapid onset of action, relatively inexpensive Disadvantages: Sedating, anticholinergic
Second-generation antihistamines (astemizole, cetirizine, fexofenadine, loratadine)
Advantages: No sedation (except cetirizine); no adverse anticholinergic effects; bid and qd dosing Disadvantages: Prolongation of QT interval; ventricular tachycardia (astemizole only) in a patient subgroup
Four-week Treatment Period: Fexofenadine HCl
Mean Pruritus Scores/Mean Number of Wheals/Mean Total Symptom Scores
An Approach to the Treatment of Chronic Urticaria
Treatment of Urticaria: Pharmacologic Options
Antihistamines, others
First-generation H1 Second-generation H1 Antihistamine/decongestant combinations Tricyclic antidepressants (eg, doxepin) Combined H1 and H2 agents
Corticosteroids
Severe acute urticaria avoid long-term use use alternate-day regimen when possible Avoid in chronic urticaria (lowest dose plus antihistamines might be necessary)
Beta-adrenergic agonists
Epinephrine for acute urticaria (rapid but short-lived response) Terbutaline
Miscellaneous
PUVA Hydroxychloroquine Thyroxine
Atopic Dermatitis: Acute, Subacute, and Chronic Lesions
Acute Cutaneous Lesions
Erythematous, intensely pruritic papules and vesicles Confined to areas of predilection cheeks in infants antecubital popliteal
Subacute Cutaneous Lesions
Erythema excoriation, scaling Bleeding and oozing lesions
Chronic Lesions
Excoriations with crusting Thickened lichenified lesions Postinflammatory hyperpigmentation Nodular prurigo
Atopic Dermatitis: Physical Distribution by Age Group
Immune Response in Atopic Dermatitis
Markedly elevated serum IgE levels
Peripheral blood eosinophilia
Highly complex inflammatory responses > IgE-dependent immediate hypersensitivity Multifunctional role of IgE (beyond mediation of specific mast cell or basophil degranulation) Cell types that express IgE on surface monocyte/macrophages Langerhans cells mast cells basophils
Atopic Dermatitis: Tests to Identify Specific Triggers
Skin prick testing for specific environmental and/or food allergens RAST, ELISA, etc, to identify serum IgE directed to specific allergens in patients with extensive cutaneous involvement Tzanck smear for herpes simplex
KOH preparation for dermatophytosis
Grams stain for bacterial infections Culture for antibiotic sensitivity for staphylococcal infection; supplement with bacterial cultures
Cultures to support tests bacterial, viral, or fungal
Topical Corticosteroids
Ranked from high to low potency in 7 classes Group 1 (most potent): betamethasone dipropionate 0.05% Group 4 (intermediate potency): hydrocortisone valerate 0.2% Group 7 (least potent): hydrocortisone hydrochloride 1% Local side effects: Development of striae and atrophy of the skin, perioral dermatitis, rosacea Systemic effects: Depend on potency, site of application, occlusiveness, percentage of body covered, length of use May cause adrenal suppression in infants and small children if used long term
Antihistamines and Other Treatments
Standard Treatment
Oral antihistamines to relieve itching Moisturizer to minimize dry skin Topical corticosteroids
Hard-to-manage Disease
Antibiotics Coal tar preparations (antipruritic and anti-inflammatory) Wet dressings and occlusion Systemic corticosteroids UV light therapy Hospitalization
Das könnte Ihnen auch gefallen
- Urticaria and AngioedemaDokument20 SeitenUrticaria and AngioedemaAhmad KusayiriNoch keine Bewertungen
- Hypersensitivity Disorders: Parameth Thiennimitr, M.D., PH.DDokument44 SeitenHypersensitivity Disorders: Parameth Thiennimitr, M.D., PH.DChaht RojborwonwitayaNoch keine Bewertungen
- 8 Hypersensitivity 03Dokument30 Seiten8 Hypersensitivity 03Mighty ExperienceNoch keine Bewertungen
- Staphylococcus & StreptococcusDokument100 SeitenStaphylococcus & StreptococcusFahim NadvyNoch keine Bewertungen
- Immunity, Autoimmunity - QsDokument5 SeitenImmunity, Autoimmunity - QsMaedehNoch keine Bewertungen
- 11 PsoriasisDokument69 Seiten11 PsoriasisRazane AbouzaidNoch keine Bewertungen
- 22 Hypersenitivity & AutoimmuneDokument53 Seiten22 Hypersenitivity & AutoimmuneAnonymous Bh6y0TuVHiNoch keine Bewertungen
- Staphylococci: Streptococcus PyogenesDokument20 SeitenStaphylococci: Streptococcus PyogenesPharmacy2015100% (2)
- Infection: Dr. Mehrunnisa Umar Assistant Professor Department of MedicineDokument57 SeitenInfection: Dr. Mehrunnisa Umar Assistant Professor Department of MedicinedrusmanjamilhcmdNoch keine Bewertungen
- Main Allergens Diagnosis of Allergic Diseases - Skin Prick Tests 2022Dokument52 SeitenMain Allergens Diagnosis of Allergic Diseases - Skin Prick Tests 2022SePeHR SHNoch keine Bewertungen
- Infections in Immunocompromised Host CHRI ClassDokument26 SeitenInfections in Immunocompromised Host CHRI Classmmkavitha98Noch keine Bewertungen
- Hypersensitivity Canvas2022Dokument23 SeitenHypersensitivity Canvas2022Muharem MemushiNoch keine Bewertungen
- 14 Hypersensitive ReactionsDokument32 Seiten14 Hypersensitive ReactionsrahuldhodapkarNoch keine Bewertungen
- 8 Hypersensitivity 03Dokument30 Seiten8 Hypersensitivity 03Khurshid HassanNoch keine Bewertungen
- Lect.12 - Immunologic and Endocrine Alterations in ChildrenDokument61 SeitenLect.12 - Immunologic and Endocrine Alterations in ChildrenlouradelNoch keine Bewertungen
- Juvenile Rheumatoid ArthritisDokument30 SeitenJuvenile Rheumatoid ArthritisAnonymous dFSZ2k2IUNoch keine Bewertungen
- Patofis 9 Alergi, Pseudoalergi, Rhematoid Arthritis, Ghout - NEWDokument42 SeitenPatofis 9 Alergi, Pseudoalergi, Rhematoid Arthritis, Ghout - NEWDea NaswaniyahNoch keine Bewertungen
- StaphylococciDokument73 SeitenStaphylococcishahbaz100% (5)
- 8 Hypersensitivity 03Dokument30 Seiten8 Hypersensitivity 03anzoltNoch keine Bewertungen
- Respiratory Tract MicrobiologyDokument68 SeitenRespiratory Tract Microbiologysultan khabeebNoch keine Bewertungen
- Gram Positive Cocci: Two GeneraDokument31 SeitenGram Positive Cocci: Two GeneraGeorgeNecoară100% (1)
- HypersensitivityDokument85 SeitenHypersensitivityAlina LubnaNoch keine Bewertungen
- Cornell Notes: TopicDokument4 SeitenCornell Notes: TopicLeahCongrehillaNoch keine Bewertungen
- Sigal Immuno DeficiencyDokument61 SeitenSigal Immuno DeficiencyClaire HendersonNoch keine Bewertungen
- Management of Septic ShockDokument33 SeitenManagement of Septic ShockswatisinghnigeriaNoch keine Bewertungen
- Adult Allergic/Hypersensitivity Disorders 2014 PHYSIOLOGIC OVERVIEW: ANTIBODIES React With Allergens byDokument9 SeitenAdult Allergic/Hypersensitivity Disorders 2014 PHYSIOLOGIC OVERVIEW: ANTIBODIES React With Allergens byRye AnchNoch keine Bewertungen
- Slides of Fever 3Dokument52 SeitenSlides of Fever 3Selly SelNoch keine Bewertungen
- Drugs Acting On The Immune SystemDokument33 SeitenDrugs Acting On The Immune SystemAnonymous iG0DCOf100% (1)
- Glo Me Rulo NephritisDokument74 SeitenGlo Me Rulo NephritisnewtypeNoch keine Bewertungen
- Hyper SensitivityDokument37 SeitenHyper Sensitivityash ashNoch keine Bewertungen
- Unit 10Dokument45 SeitenUnit 10amirahaliNoch keine Bewertungen
- Nursing Management of A Client With Immunological Disorders: M.N Priyadarshanie BSC in NursingDokument47 SeitenNursing Management of A Client With Immunological Disorders: M.N Priyadarshanie BSC in NursingClarissa Cabudoc OronosNoch keine Bewertungen
- Anaphylaxis ReactionDokument27 SeitenAnaphylaxis ReactiongusriaNoch keine Bewertungen
- 14 超敏反应Dokument32 Seiten14 超敏反应Jennifer DixonNoch keine Bewertungen
- Module. Immunity - Infection Fall 2019Dokument44 SeitenModule. Immunity - Infection Fall 2019Christyl RealreconizerealNoch keine Bewertungen
- Lecture 21 - HypersensitivityDokument25 SeitenLecture 21 - Hypersensitivityapi-3703352100% (2)
- Hypersensitivity: DR - Bimal ChauhanDokument45 SeitenHypersensitivity: DR - Bimal Chauhantajir cetajirNoch keine Bewertungen
- Farmakologi Obat Pada Reaksi HipersensitivitasDokument59 SeitenFarmakologi Obat Pada Reaksi HipersensitivitasTitip Elia GustamiNoch keine Bewertungen
- Lecture 11 Hypersensitivity ReactionsDokument41 SeitenLecture 11 Hypersensitivity ReactionsAakashNoch keine Bewertungen
- Karaganda State Medical University: Department of Pathological PhysiologyDokument23 SeitenKaraganda State Medical University: Department of Pathological PhysiologyPraveen NayakNoch keine Bewertungen
- Anafilaksis PDFDokument27 SeitenAnafilaksis PDFAvicenna_MSC100% (1)
- Connective Tissue Disease LectureDokument99 SeitenConnective Tissue Disease Lectureconfuzzledfreak100% (1)
- Food IntoleranceDokument95 SeitenFood IntoleranceShirin Syailandira100% (2)
- Questions ExplanationDokument63 SeitenQuestions ExplanationnomintmNoch keine Bewertungen
- Introduction To Pathology Infectious DiseasesDokument37 SeitenIntroduction To Pathology Infectious DiseasesNirav PatelNoch keine Bewertungen
- Basic Skin Immunology 2011Dokument22 SeitenBasic Skin Immunology 2011krishnappanramu100% (1)
- Drug AllergyDokument61 SeitenDrug Allergyadysti100% (1)
- Anaphylaxis ReactionDokument27 SeitenAnaphylaxis Reactionmau tauNoch keine Bewertungen
- Week 2 Chapter 10: Alterations in Immune FunctionDokument55 SeitenWeek 2 Chapter 10: Alterations in Immune FunctionAshley Diane HenryNoch keine Bewertungen
- Hypersensitivity Rev BWDokument34 SeitenHypersensitivity Rev BWGuhanNoch keine Bewertungen
- Cutaneous Lupus Erythematosus: SGD B3Dokument41 SeitenCutaneous Lupus Erythematosus: SGD B3Che Haniff100% (2)
- Hypersensitivity: Presenter:Prateema Gill Moderater: Dr. Niti SinghalDokument25 SeitenHypersensitivity: Presenter:Prateema Gill Moderater: Dr. Niti SinghalAvi VermaNoch keine Bewertungen
- Disorders of Immunity EditedDokument62 SeitenDisorders of Immunity EditedJustine NyangaresiNoch keine Bewertungen
- Nursing Care of Clients With Allergic DisordersDokument12 SeitenNursing Care of Clients With Allergic Disordersbwee bweeNoch keine Bewertungen
- Hypersensitivity Reactions: Prakash Nagarkatti, Ph.D. E-Mail: Pnagark@uscmed - Sc.edu)Dokument7 SeitenHypersensitivity Reactions: Prakash Nagarkatti, Ph.D. E-Mail: Pnagark@uscmed - Sc.edu)anon_60614972Noch keine Bewertungen
- Reviewofprimary ImmunodeficiencydiseasesDokument58 SeitenReviewofprimary Immunodeficiencydiseasespriti adsulNoch keine Bewertungen
- Behaviour Aspect in Allergic Disease: Prof. Dr. Dr. Endang Sutedja, SPKK (K)Dokument43 SeitenBehaviour Aspect in Allergic Disease: Prof. Dr. Dr. Endang Sutedja, SPKK (K)elmacitaNoch keine Bewertungen
- Autoimmune DiseaseDokument38 SeitenAutoimmune DiseaseGustiandari FidhyaNoch keine Bewertungen
- Chapter 13:: Basic Principles of Immunologic Diseases in Skin (Pathophysiology of Immunologic/Inflammatory Skin Diseases)Dokument7 SeitenChapter 13:: Basic Principles of Immunologic Diseases in Skin (Pathophysiology of Immunologic/Inflammatory Skin Diseases)S FznsNoch keine Bewertungen
- Special Operations Forces Medical HandbookVon EverandSpecial Operations Forces Medical HandbookBewertung: 4.5 von 5 Sternen4.5/5 (2)
- Simple Past Story 1Dokument7 SeitenSimple Past Story 1Ummi Umarah50% (2)
- Upanikhat-I Garbha A Mughal Translation PDFDokument18 SeitenUpanikhat-I Garbha A Mughal Translation PDFReginaldoJurandyrdeMatosNoch keine Bewertungen
- High Court Judgment On Ex Party DecreeDokument2 SeitenHigh Court Judgment On Ex Party Decreeprashant pathakNoch keine Bewertungen
- Mission Veng 29th, 2019Dokument4 SeitenMission Veng 29th, 2019Lasky ChhakchhuakNoch keine Bewertungen
- Incremental Analysis 2Dokument12 SeitenIncremental Analysis 2enter_sas100% (1)
- PDFDokument50 SeitenPDFWalaa RaslanNoch keine Bewertungen
- Qsen CurriculumDokument5 SeitenQsen Curriculumapi-280981631Noch keine Bewertungen
- Africanas Journal Volume 3 No. 2Dokument102 SeitenAfricanas Journal Volume 3 No. 2Gordon-Conwell Theological Seminary100% (2)
- Comparative Analysis of Levis Wrangler & LeeDokument10 SeitenComparative Analysis of Levis Wrangler & LeeNeelakshi srivastavaNoch keine Bewertungen
- Sancticity AllDokument21 SeitenSancticity AllJames DeHart0% (1)
- IJONE Jan-March 2017-3 PDFDokument140 SeitenIJONE Jan-March 2017-3 PDFmoahammad bilal AkramNoch keine Bewertungen
- 5 Reported Speech - T16-6 PracticeDokument3 Seiten5 Reported Speech - T16-6 Practice39 - 11A11 Hoàng Ái TúNoch keine Bewertungen
- Conspicuous Consumption-A Literature ReviewDokument15 SeitenConspicuous Consumption-A Literature Reviewlieu_hyacinthNoch keine Bewertungen
- SSP ReviwerDokument40 SeitenSSP ReviwerRick MabutiNoch keine Bewertungen
- Introduction, Case StudyDokument56 SeitenIntroduction, Case StudyLeanna Cantanero67% (3)
- Pi 100 Book ReviewDokument10 SeitenPi 100 Book ReviewBianca CacnioNoch keine Bewertungen
- Sales Plan: Executive SummaryDokument13 SeitenSales Plan: Executive SummaryaditiNoch keine Bewertungen
- Speaking C1Dokument16 SeitenSpeaking C1Luca NituNoch keine Bewertungen
- Acid Base AnswersDokument4 SeitenAcid Base Answersapi-232466940Noch keine Bewertungen
- BreadTalk - Annual Report 2014Dokument86 SeitenBreadTalk - Annual Report 2014Vicky NeoNoch keine Bewertungen
- Robbins Ob14 PPT 11Dokument27 SeitenRobbins Ob14 PPT 11daneshnedaieNoch keine Bewertungen
- Birnbaum - 2006 Registration SummaryDokument14 SeitenBirnbaum - 2006 Registration SummaryEnvironmental Evaluators Network100% (1)
- Fundamentals of Biochemical Engineering Dutta Solution ManualDokument6 SeitenFundamentals of Biochemical Engineering Dutta Solution Manualhimanshu18% (22)
- Mushoku Tensei Volume 2Dokument179 SeitenMushoku Tensei Volume 2Bismillah Dika2020Noch keine Bewertungen
- Commercial LawDokument61 SeitenCommercial LawthebfilesNoch keine Bewertungen
- ) Mark Scheme (Results) January 2019: Pearson Edexcel International GCSE in Mathematics A (4MA1) Higher Tier Paper 1HRDokument22 Seiten) Mark Scheme (Results) January 2019: Pearson Edexcel International GCSE in Mathematics A (4MA1) Higher Tier Paper 1HRNewtonNoch keine Bewertungen
- Hermeneutical Phenomenology and Human Enviroment SystemDokument12 SeitenHermeneutical Phenomenology and Human Enviroment SystemAllen Rose Buenaflor BuenoNoch keine Bewertungen
- Possessive Adjectives 3Dokument1 SeitePossessive Adjectives 3RAMIRO GARCIA CANCELANoch keine Bewertungen
- Songs of KabirDokument342 SeitenSongs of KabirSant MatNoch keine Bewertungen
- Final Draft Investment Proposal For ReviewDokument7 SeitenFinal Draft Investment Proposal For ReviewMerwinNoch keine Bewertungen